Healthcare providers face mounting administrative challenges as they navigate the complex landscape of payer enrollment and provider verification. Credentialing solutions have emerged as essential tools that enable practices to maintain compliance, accelerate revenue cycles, and ensure uninterrupted patient care. These comprehensive systems streamline the traditionally cumbersome process of verifying provider qualifications, managing documentation, and maintaining active status across multiple insurance networks. For revenue cycle management professionals, understanding the full scope of modern credentialing solutions is critical to optimizing financial performance and reducing administrative burden.
Understanding Modern Credentialing Solutions in Healthcare
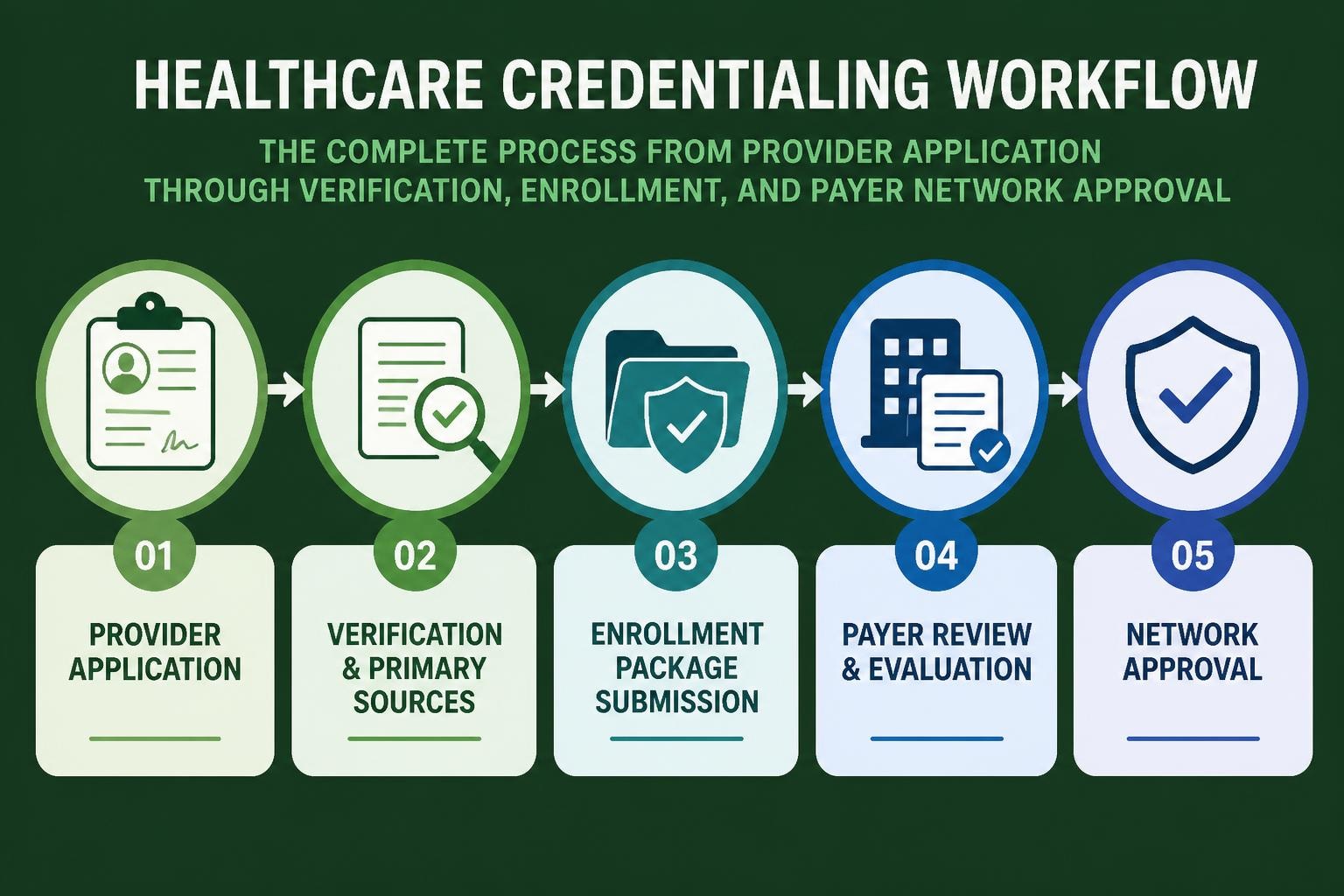
Credentialing solutions represent a systematic approach to collecting, verifying, and maintaining provider information required for participation in insurance networks and healthcare organizations. The credentialing process involves comprehensive documentation of education, training, licensure, and professional history to ensure providers meet established quality standards.
Core Components of Effective Systems
Modern credentialing solutions encompass several critical elements that work together to create efficient workflows:
- Primary source verification of education, training, and licensure credentials
- Automated data collection from standardized databases and provider attestations
- Real-time status tracking across multiple payer networks and organizations
- Compliance monitoring for expiring licenses, certifications, and documentation
- Privileging management for hospital-based and specialty care providers
These components integrate to reduce manual effort while maintaining the accuracy and completeness required by accrediting bodies. Organizations implementing robust credentialing solutions report significant reductions in enrollment timeframes and administrative costs.
The sophistication of credentialing solutions has evolved considerably in recent years. Provider enrollment that once required six to nine months can now be completed in significantly shorter timeframes through automated workflows and digital documentation management.
Benefits of Implementing Credentialing Solutions
Healthcare organizations that deploy comprehensive credentialing solutions experience measurable improvements across multiple operational metrics. These systems transform credentialing from a reactive administrative burden into a proactive revenue enabler.
Revenue Cycle Impact
The connection between credentialing efficiency and revenue performance is direct and substantial. Delays in provider enrollment translate immediately to lost revenue opportunities. When newly hired providers cannot bill insurance companies, practices absorb significant financial losses while continuing to incur salary and overhead expenses.
| Impact Area | Without Solutions | With Solutions |
|---|---|---|
| Enrollment Timeline | 120-180 days | 60-90 days |
| Administrative Hours | 40-60 hours/provider | 10-15 hours/provider |
| Documentation Errors | 15-25% | 3-5% |
| Re-credentialing Delays | 20-30% | Under 5% |
Credentialing solutions create value by accelerating the enrollment process, reducing errors that cause rejections, and ensuring continuous network participation. These improvements directly support net revenue management objectives by eliminating gaps in billing capability.
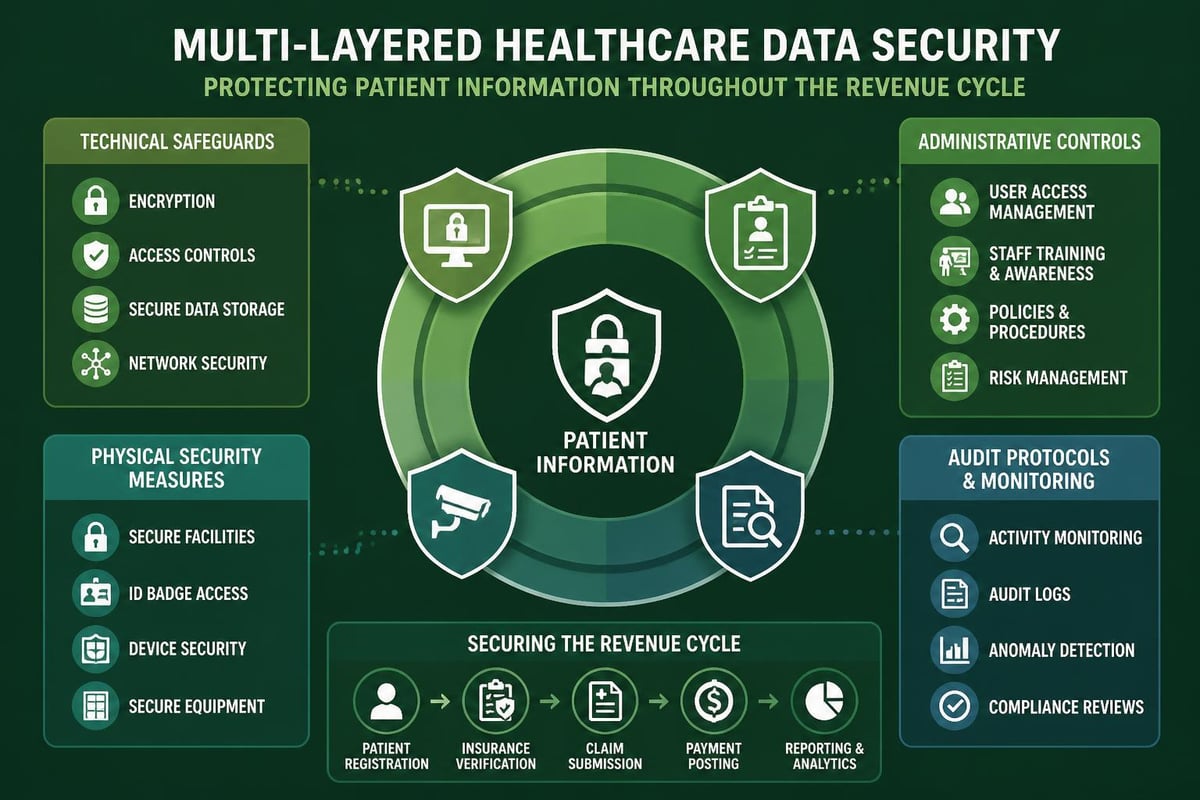
Compliance and Risk Mitigation
Healthcare organizations face substantial regulatory and accreditation requirements related to provider credentialing. The National Committee for Quality Assurance (NCQA) establishes rigorous standards that health plans and credentialing organizations must meet to maintain accreditation.
Credentialing solutions help organizations maintain compliance through:
- Standardized verification protocols that ensure consistent application of standards
- Automated expiration tracking that prevents lapses in licensure or certification
- Comprehensive audit trails documenting all verification activities
- Quality assurance workflows that flag incomplete or questionable information
- Integration with primary sources reducing reliance on provider-supplied documentation
Organizations utilizing advanced credentialing solutions demonstrate higher compliance rates during accreditation surveys and payer audits. The systematic approach reduces human error and ensures that verification activities meet current regulatory standards.
Key Features of Advanced Credentialing Solutions
The most effective credentialing solutions incorporate technologies and capabilities that address the full lifecycle of provider enrollment and maintenance. Understanding these features helps organizations evaluate potential systems and maximize their investment.
Centralized Database Management
Modern credentialing solutions maintain comprehensive provider databases that serve as single sources of truth for all credential information. These databases integrate with external systems to populate and verify data automatically, reducing manual entry and associated errors.
The CAQH credentialing suite represents one widely adopted approach, with over two million healthcare providers using these solutions to exchange professional information securely. This centralization eliminates redundant data entry and accelerates the verification process.
Automated Workflow Management
Credentialing involves numerous sequential steps, each with specific requirements and dependencies. Advanced solutions automate these workflows through:
- Task assignment and routing based on credential type and organizational role
- Status notifications alerting stakeholders to pending actions or approaching deadlines
- Document management systems organizing required attestations and supporting materials
- Integration with eligibility verification services and payer portals
- Escalation protocols for items requiring management attention
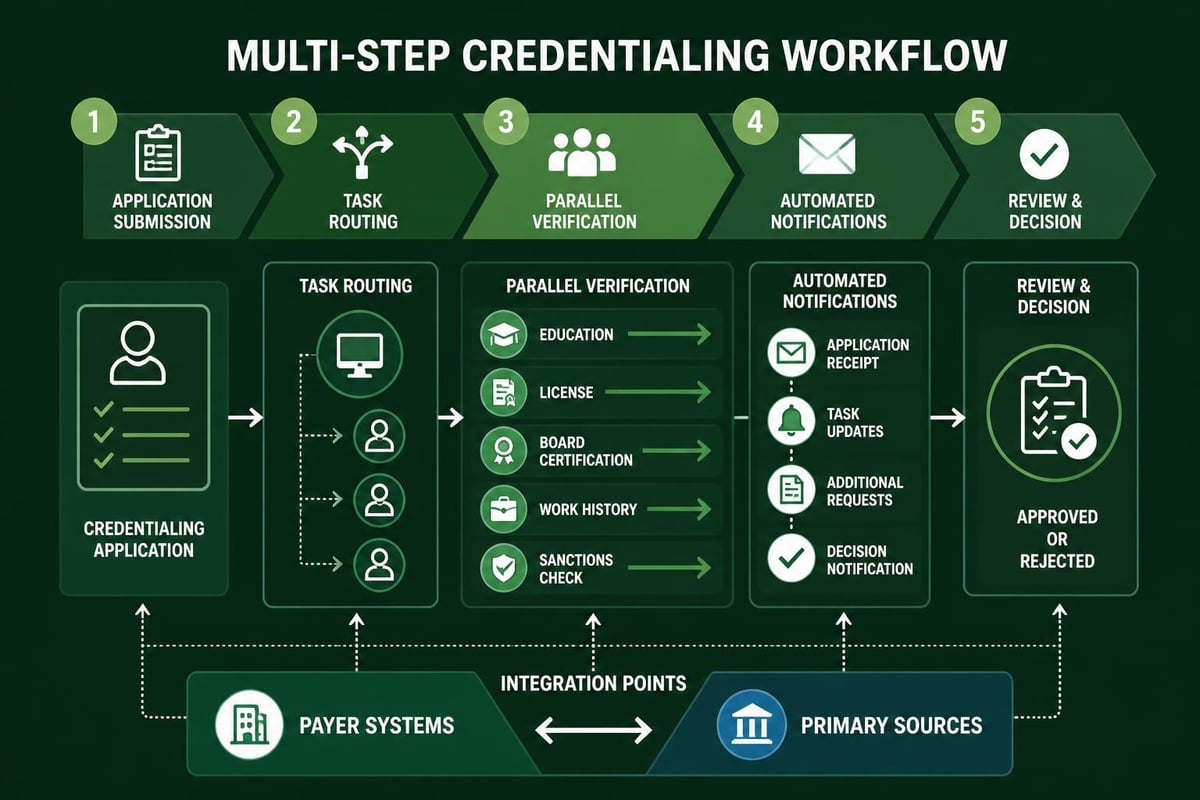
Workflow automation reduces credentialing cycle time by eliminating manual handoffs and ensuring that all required activities progress simultaneously rather than sequentially. Organizations implementing automated workflows report enrollment timeframe reductions of thirty to fifty percent.
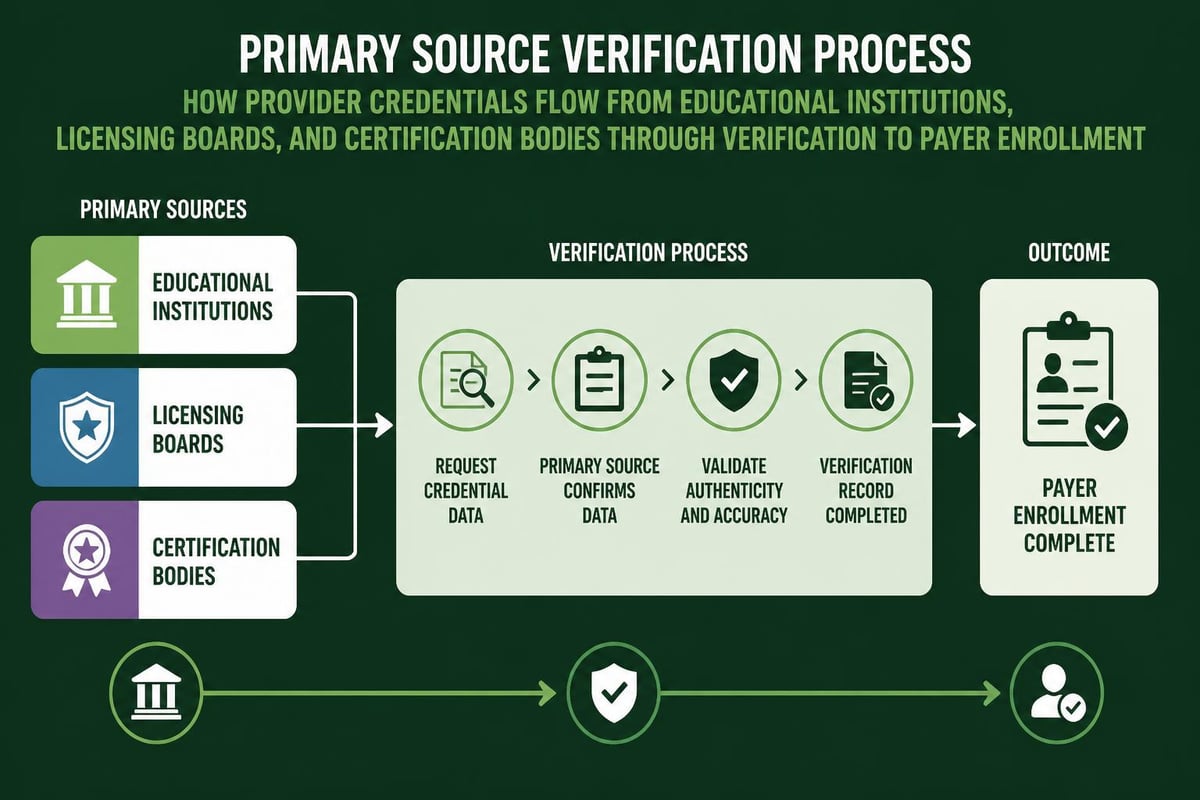
Primary Source Verification Technology
The foundation of credentialing quality rests on accurate verification of provider credentials through primary sources. Traditional manual verification involved phone calls, faxes, and mailed requests to educational institutions, licensing boards, and certification bodies.
Modern credentialing solutions leverage technology to streamline primary source verification:
| Verification Type | Traditional Method | Modern Solution |
|---|---|---|
| Medical Education | Mail request to school | Electronic verification through database |
| State Licensure | Phone/fax to board | Real-time API integration |
| Board Certification | Written request | Automated specialty board lookup |
| DEA Registration | Manual NPDB query | Integrated federal database access |
| Work History | Phone verification | Electronic employment verification |
These technological advances reduce verification timeframes from weeks to days while improving accuracy and creating verifiable audit trails. Solutions like VeriFide utilize advanced technologies to authenticate provider information efficiently.
Building Effective Credentialing Programs
Organizations seeking to optimize their credentialing processes must consider both technology implementation and program design. The most sophisticated credentialing solutions deliver limited value without proper organizational structure and governance.
Program Design Considerations
Effective credentialing program design addresses fundamental questions about organizational structure, resource allocation, and quality standards. Healthcare organizations must decide whether to manage credentialing internally, outsource to credential verification organizations, or adopt hybrid approaches.
Internal credentialing programs offer direct control and deep organizational integration but require significant staffing and expertise. Credential Verification Organizations (CVOs) provide specialized capabilities and economies of scale but introduce external dependencies. Many organizations adopt hybrid models, managing strategic elements internally while outsourcing routine verification activities.
Staffing and Expertise Requirements
Credentialing solutions require knowledgeable personnel who understand regulatory requirements, payer-specific criteria, and verification methodologies. Organizations must invest in:
- Certified credentialing specialists with relevant industry credentials
- Training programs ensuring staff remain current with changing standards
- Quality assurance personnel monitoring accuracy and completeness
- Technology administrators managing system configuration and optimization
The complexity of credentialing necessitates ongoing professional development. Staff members must understand nuances across multiple specialties, state regulations, and payer requirements to make appropriate verification decisions.
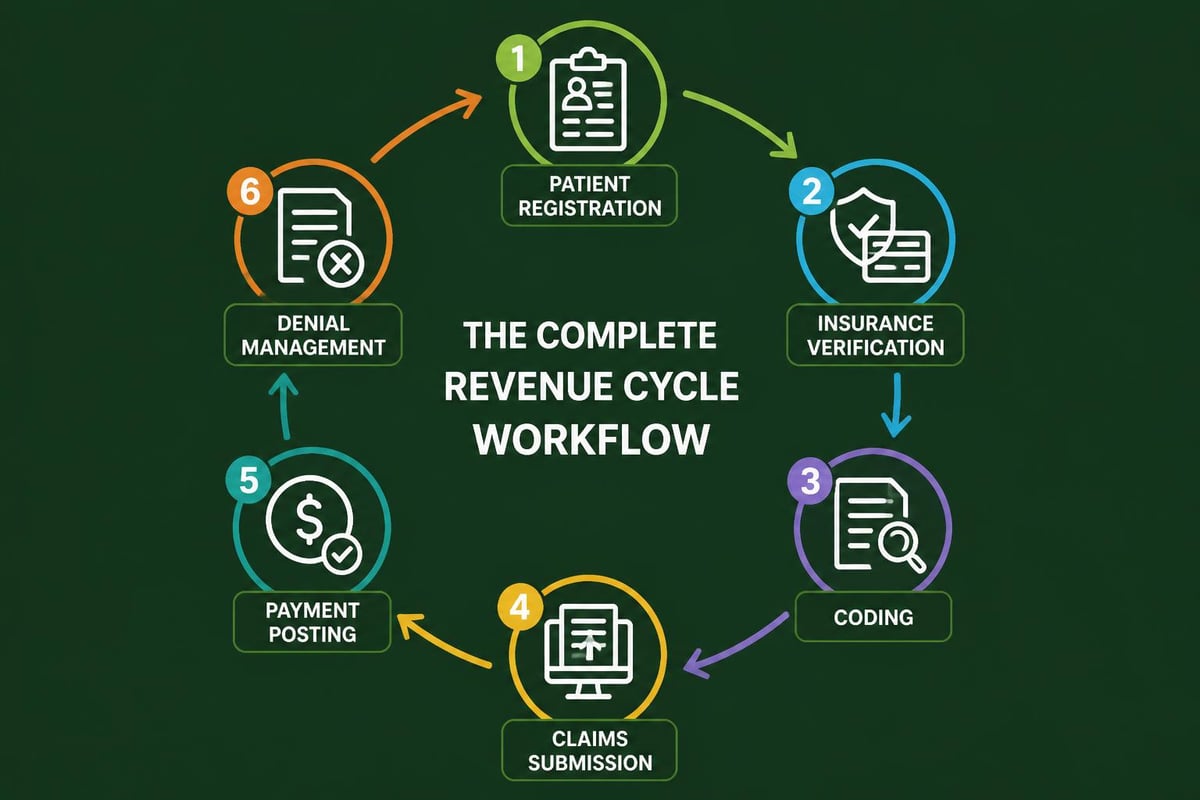
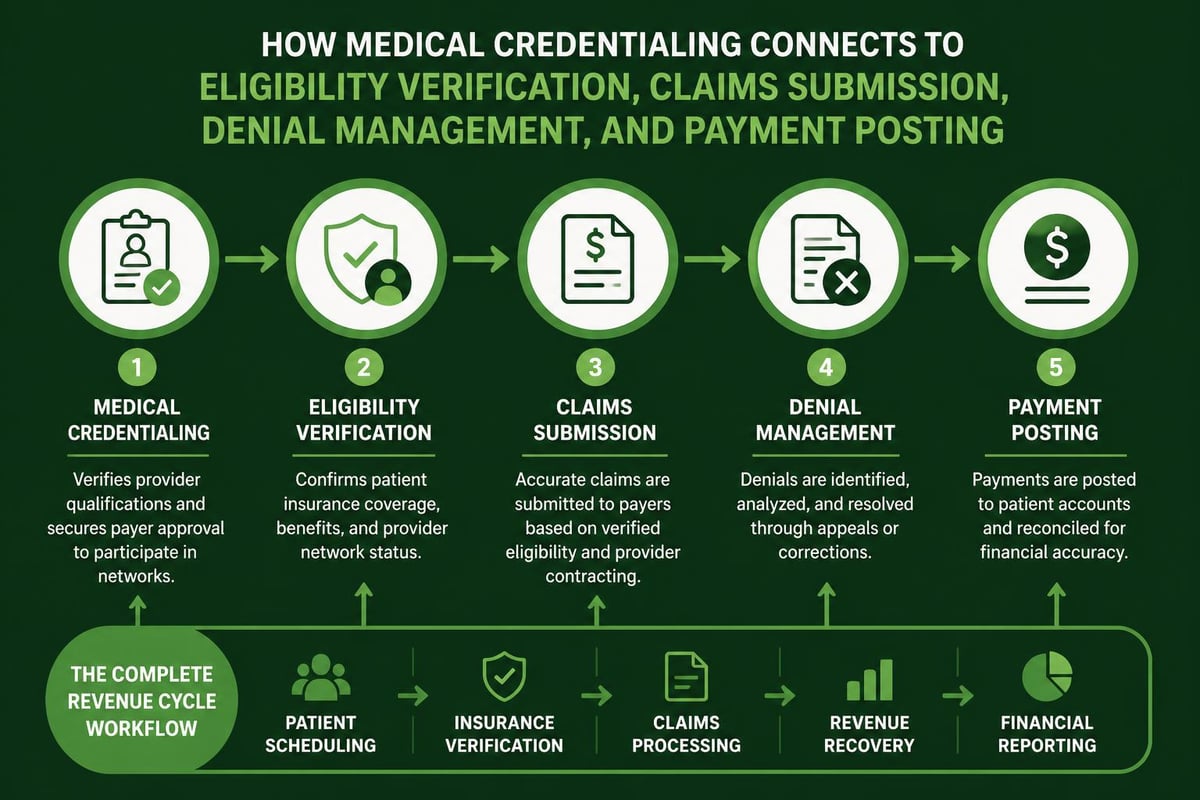
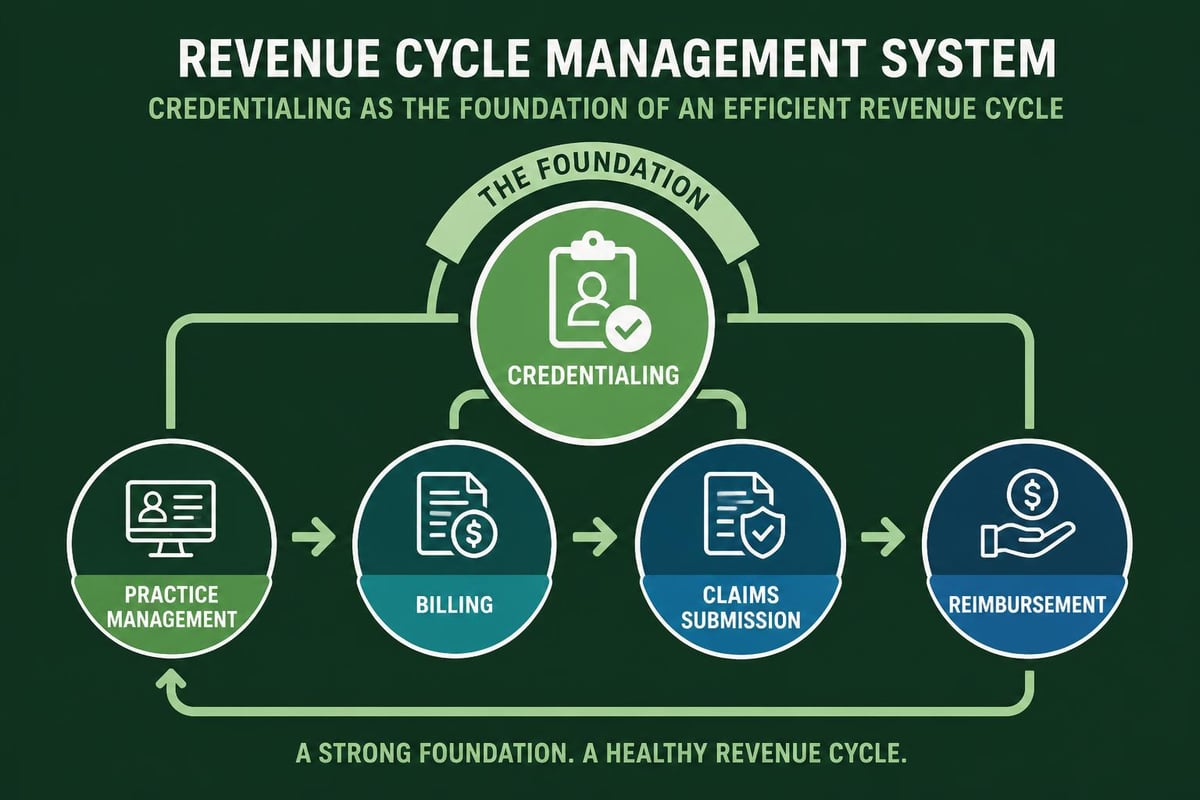
Integration with Revenue Cycle Management
Credentialing solutions function most effectively when integrated with broader revenue cycle management systems. This integration ensures that billing capabilities align with provider network participation status and prevents claims submission for services rendered by non-credentialed providers.
Key integration points include:
- Practice management systems that track provider participation by payer and location
- Medical billing services platforms that validate provider-payer relationships before claim submission
- Scheduling systems that prevent appointment booking before credential completion
- Reporting tools that monitor credentialing status as a revenue cycle metric
Organizations like Greenhive Billing Solutions recognize that credentialing represents a critical upstream component of revenue cycle optimization. When credentialing processes function efficiently, downstream activities like claims processing and payment posting proceed without interruption.
Credentialing Challenges and Solutions
Despite technological advances, healthcare organizations continue to face significant credentialing challenges. Understanding these obstacles and implementing appropriate solutions is essential for maintaining operational efficiency.
Common Credentialing Obstacles
Healthcare providers encounter numerous difficulties throughout the credentialing lifecycle:
- Lengthy enrollment timeframes delaying revenue generation for new providers
- Inconsistent payer requirements creating confusion and requiring customized approaches
- Incomplete or inaccurate documentation causing application rejections and delays
- Re-credentialing lapses resulting in network termination and billing disruptions
- Multi-state licensure complexity for telehealth and multi-location practices
These challenges compound when organizations manage credentialing through manual processes or outdated systems. The administrative burden diverts resources from patient care while creating financial risk through delayed or denied reimbursements.
Strategic Solutions and Best Practices
Organizations implementing comprehensive credentialing solutions address these challenges through systematic approaches:
Proactive Timeline Management
Successful organizations establish credentialing timelines that begin six months before anticipated provider start dates. This buffer accommodates unexpected delays while ensuring revenue-generating capability aligns with employment commencement. Automated reminders and milestone tracking prevent timeline drift.
Payer-Specific Documentation Libraries
Maintaining current documentation requirements for each payer network reduces submission errors and accelerates approval. Credentialing solutions should include customizable checklists and templates aligned with specific payer criteria. Regular communication with payer credentialing departments ensures requirement changes are captured promptly.
Quality Assurance Protocols
Implementing multi-level review processes catches errors before submission. Effective quality assurance includes peer review of completed applications, supervisory oversight of verification activities, and pre-submission audits against payer checklists. These processes improve first-pass approval rates and reduce costly rework.
Technology Trends Shaping Credentialing Solutions
The credentialing landscape continues to evolve as technology advances and industry requirements change. Forward-thinking organizations monitor emerging trends to maintain competitive advantages and operational efficiency.
Artificial Intelligence and Automation
Artificial intelligence applications are increasingly incorporated into credentialing solutions, automating routine decision-making and document review. Machine learning algorithms can:
- Extract relevant information from uploaded documents automatically
- Flag inconsistencies between provider attestations and verified data
- Predict potential application issues based on historical patterns
- Prioritize verification activities based on urgency and complexity
These capabilities allow credentialing specialists to focus on complex cases requiring professional judgment while routine applications progress automatically through standardized workflows.
Blockchain for Credential Verification
Blockchain technology offers potential solutions for credential verification challenges. Distributed ledger systems could create tamper-proof records of provider credentials, reducing verification burden and improving data accuracy. Early implementations focus on educational credentials and professional certifications, with broader healthcare applications under development.
Enhanced Data Interoperability
Industry initiatives promoting data standardization and exchange protocols are reducing friction in credentialing processes. Enhanced interoperability enables:
- Seamless data transfer between provider databases and payer systems
- Real-time credential status verification without manual queries
- Automated updates when credentials change or expire
- Unified provider directories accessible across multiple organizations
Organizations like NCQA-certified CVOs are adopting these standards to improve efficiency and reduce administrative burden across the healthcare ecosystem.
Continuous Credentialing Models
Traditional credentialing approaches rely on periodic re-credentialing cycles, typically every two to three years. Emerging continuous credentialing models leverage real-time data monitoring to identify credential changes as they occur. This approach reduces administrative burden while improving quality by catching issues immediately rather than at re-credentialing intervals.
Measuring Credentialing Solution Performance
Healthcare organizations must establish metrics to evaluate credentialing solution effectiveness and identify improvement opportunities. Performance measurement ensures that investments in credentialing technology and personnel deliver expected returns.
Key Performance Indicators
Effective credentialing performance measurement incorporates metrics across multiple dimensions:
| Metric Category | Specific Indicators | Target Benchmark |
|---|---|---|
| Efficiency | Average enrollment timeline | 60-75 days |
| Quality | First-pass approval rate | Above 90% |
| Compliance | Re-credentialing on-time completion | 100% |
| Financial Impact | Revenue delay due to credentialing | Under 2% of collections |
| Resource Utilization | Hours per provider application | 12-18 hours |
Organizations should track these metrics regularly and establish improvement initiatives when performance falls below benchmarks. Integration with revenue cycle reporting provides visibility into credentialing impact on overall financial performance.
Continuous Improvement Methodology
Leading organizations apply structured improvement methodologies to credentialing operations. Root cause analysis identifies underlying factors contributing to delays or errors. Process mapping reveals inefficiencies and redundancies in existing workflows. Stakeholder feedback from providers, payer representatives, and credentialing staff highlights pain points requiring attention.
Credentialing solutions supporting robust reporting and analytics enable data-driven improvement. Organizations can analyze patterns across provider types, payer networks, and geographic regions to identify targeted optimization opportunities. Similar to denial management in medical billing, systematic analysis of credentialing challenges yields actionable insights for performance improvement.
Selecting the Right Credentialing Solutions
Healthcare organizations evaluating credentialing solutions face numerous options ranging from comprehensive enterprise platforms to specialized point solutions. Selecting appropriate systems requires careful assessment of organizational needs, existing infrastructure, and strategic objectives.
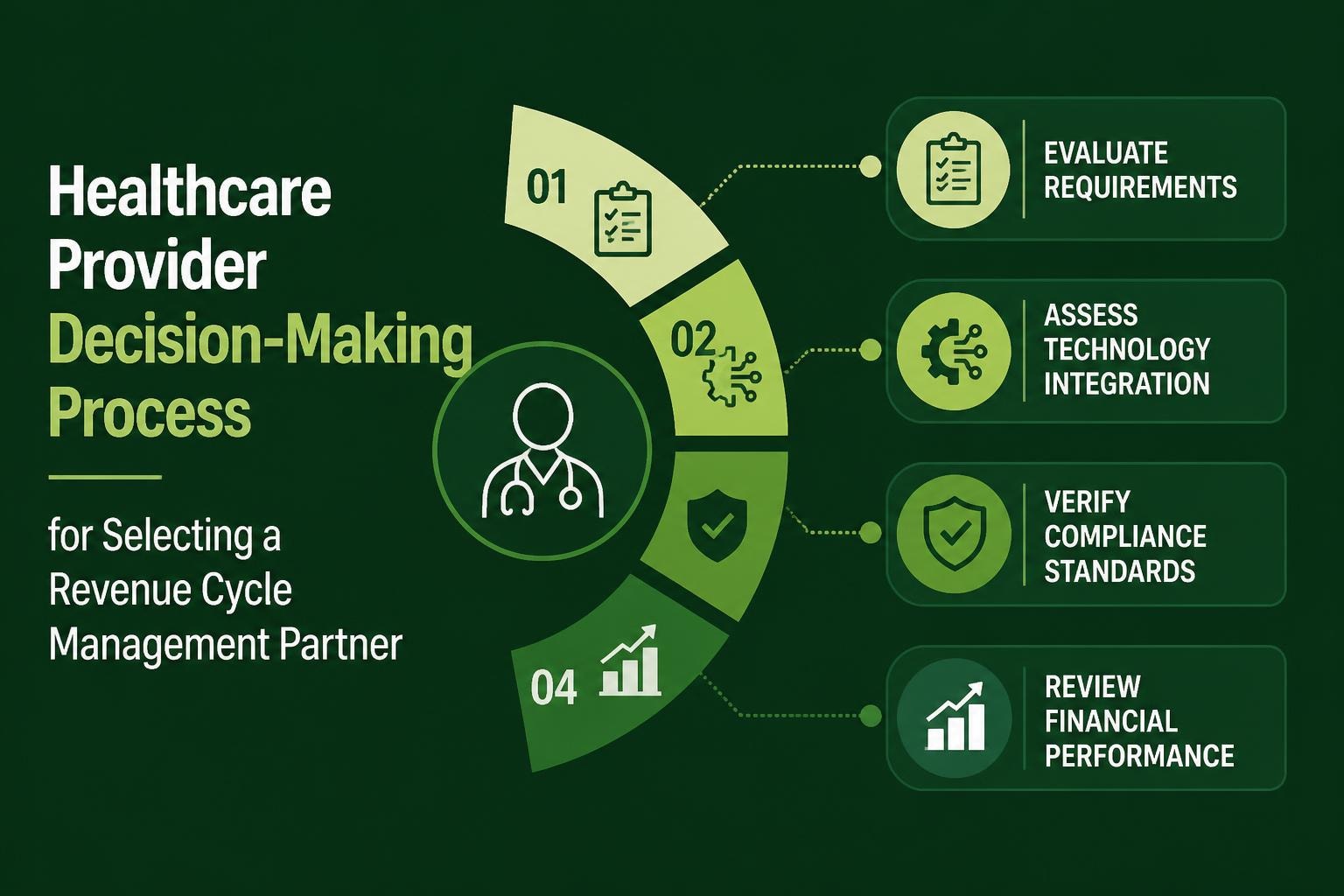
Evaluation Criteria
Organizations should assess potential credentialing solutions against comprehensive criteria:
- Functional completeness covering initial credentialing, re-credentialing, privileging, and ongoing monitoring
- Integration capabilities with existing practice management, billing, and HR systems
- Scalability to accommodate organizational growth and changing provider populations
- Vendor stability and support ensuring long-term viability and responsive assistance
- Compliance with industry standards including NCQA requirements and data security protocols
- User experience for both credentialing staff and provider applicants
- Reporting and analytics supporting performance measurement and improvement initiatives
- Total cost of ownership including licensing, implementation, training, and ongoing maintenance
Thorough evaluation prevents costly implementation failures and ensures selected solutions address actual organizational requirements rather than theoretical capabilities.
Implementation Best Practices
Successful credentialing solution implementation requires structured project management and organizational change management. Critical success factors include:
- Executive sponsorship ensuring adequate resources and organizational commitment
- Detailed workflow mapping documenting current processes and desired future states
- Comprehensive data migration planning to populate new systems accurately
- Phased rollout approaches reducing implementation risk and allowing course correction
- Extensive user training ensuring staff can leverage system capabilities effectively
Organizations should allocate sufficient time for implementation, typically three to six months for comprehensive solutions. Rushed implementations compromise data quality and user adoption, ultimately undermining the value of credentialing solutions.
Credentialing Solutions and Specialized Practice Needs
Different healthcare specialties and practice models present unique credentialing challenges requiring tailored approaches. Credentialing solutions must accommodate these variations while maintaining consistent quality standards.
Hospital-Based Providers and Privileging
Hospital credentialing extends beyond basic payer enrollment to include privileging decisions that determine specific procedures providers may perform. Credentialing solutions for hospitals must support:
- Delineation of privileges by specialty and procedure complexity
- Ongoing professional practice evaluation monitoring quality metrics
- Periodic privilege renewal based on activity and outcomes
- Integration with medical staff bylaws and committee structures
These requirements demand more sophisticated credentialing solutions than those used in office-based settings. Hospital systems often implement specialized applications designed specifically for medical staff services departments.
Multi-Location and Telehealth Considerations
Healthcare organizations operating across multiple states or providing telehealth services face complex licensure and credentialing requirements. Providers must maintain active licenses in each state where they provide services, whether physically or virtually. General credentialing information covers these special considerations.
Credentialing solutions supporting multi-state operations include:
- License tracking across all relevant jurisdictions with jurisdiction-specific renewal dates
- Automated notification of approaching expirations in any state
- Payer credentialing for telehealth-specific networks and arrangements
- State-specific primary source verification addressing varying requirements
Organizations expanding geographic reach or implementing telehealth programs must ensure their credentialing solutions accommodate these complexities. Failure to maintain required state licenses creates significant compliance risk and billing complications.
Ancillary Providers and Non-Physician Credentialing
Modern healthcare delivery relies increasingly on nurse practitioners, physician assistants, and other advanced practice providers. Credentialing solutions must address the unique requirements applicable to these provider types, including:
- Collaborative practice agreements and supervisory relationships
- State-specific scope of practice limitations
- Certification and specialty credentialing for APRNs
- Prescriptive authority verification and DEA registration
Payer credentialing for non-physician providers often presents additional challenges due to inconsistent network participation criteria. Comprehensive credentialing solutions track these provider-specific requirements and ensure compliance across all applicable dimensions.
Efficient credentialing solutions represent essential infrastructure for healthcare revenue cycle management, directly impacting provider enrollment timelines, compliance status, and financial performance. Organizations that implement comprehensive systems while establishing strong operational processes achieve measurable advantages in revenue capture and administrative efficiency. Greenhive Billing Solutions delivers expert medical credentialing services alongside comprehensive revenue cycle management, helping healthcare providers navigate complex enrollment requirements while optimizing reimbursement performance. Our experienced team manages the complete credentialing lifecycle using industry-standard platforms, ensuring your providers maintain uninterrupted network participation and billing capability.