Healthcare providers face mounting pressure to maintain financial stability while delivering quality patient care. The complexity of modern medical billing, insurance requirements, and regulatory compliance demands a comprehensive approach that addresses every aspect of the revenue cycle. Total rcm solutions have emerged as the definitive answer for practices seeking to optimize their financial performance while reducing administrative burden and ensuring consistent cash flow.
Understanding the Comprehensive Approach to Revenue Cycle Management
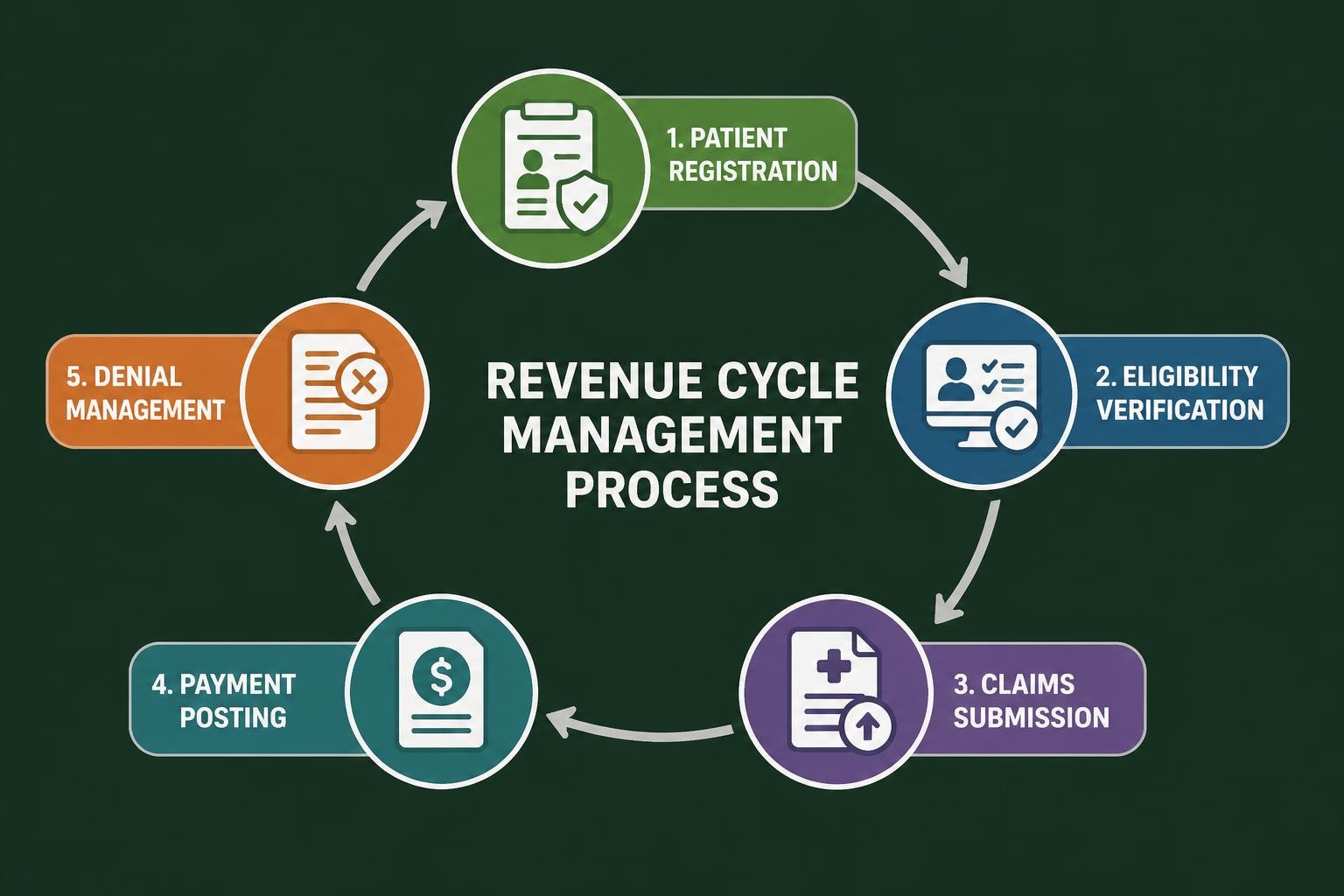
Total rcm solutions represent a holistic strategy that manages every phase of the patient financial journey, from initial scheduling through final payment reconciliation. Unlike fragmented services that address isolated components, a comprehensive approach integrates all revenue cycle functions into a seamless operation.
This integrated methodology encompasses patient registration, insurance eligibility verification, charge capture, coding, claims submission, payment posting, denial management, and patient collections. Each component connects to the others, creating a unified system that minimizes errors and maximizes reimbursement rates.
Key Components of Complete Revenue Cycle Management
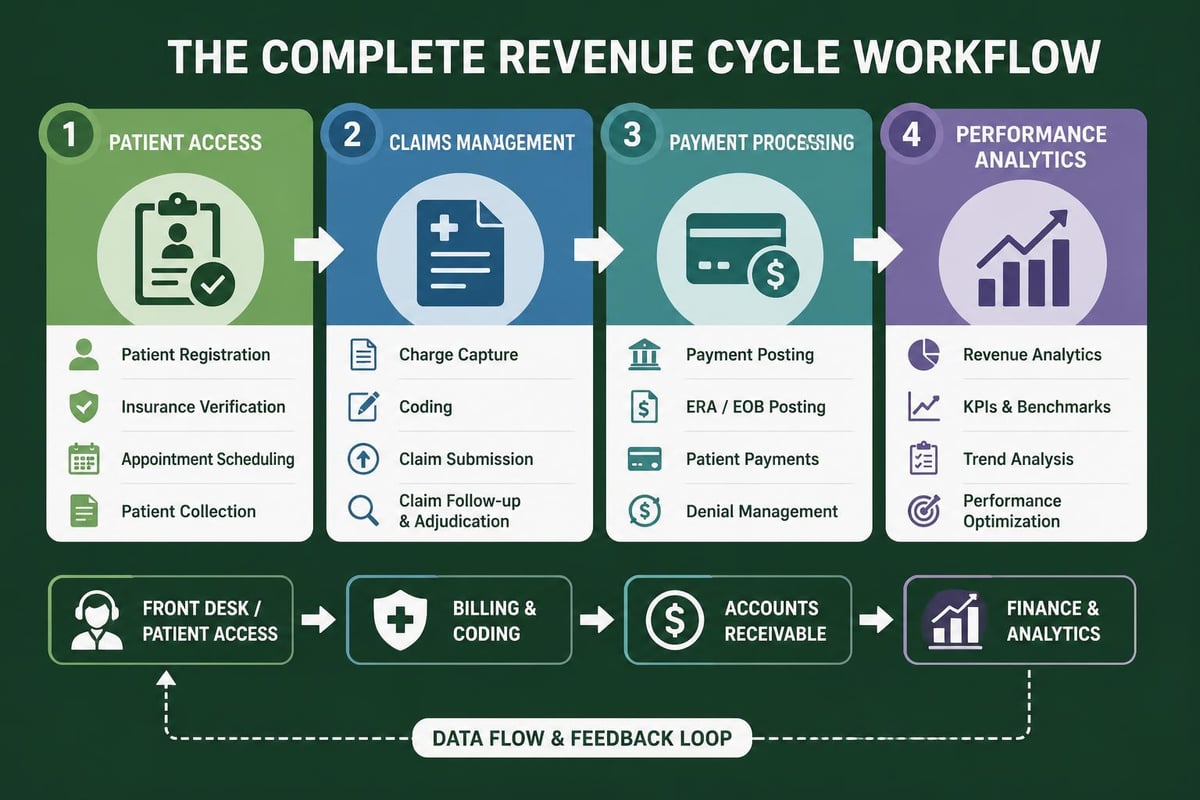
The foundation of total rcm solutions rests on several critical pillars:
- Front-end revenue cycle management: Patient scheduling, registration accuracy, insurance verification, and authorization management
- Mid-cycle operations: Accurate coding, charge capture, claims scrubbing, and timely submission
- Back-end processes: Payment posting, denial management, appeals, and patient billing
- Analytics and reporting: Performance monitoring, trend analysis, and strategic planning
- Compliance oversight: HIPAA adherence, regulatory updates, and audit preparation
Each element requires specialized expertise and dedicated attention. When these components work in harmony, practices experience reduced claim denials, faster payment cycles, and improved cash flow predictability.
The Financial Impact of Implementing Comprehensive RCM Services
Healthcare organizations implementing total rcm solutions typically observe measurable improvements across multiple financial metrics. Research demonstrates that comprehensive revenue cycle management can reduce claim denial rates by 15-25% while accelerating payment collection timeframes by 20-30%.
These improvements translate directly to the bottom line. A practice generating $3 million annually might recover an additional $150,000 to $300,000 through optimized revenue cycle processes. The return on investment becomes particularly evident when comparing internal billing costs against outsourced comprehensive solutions.
| Performance Metric | Before Total RCM | After Implementation | Improvement |
|---|---|---|---|
| First-pass claim acceptance rate | 82% | 96% | +14% |
| Days in accounts receivable | 48 days | 32 days | -33% |
| Collection rate | 91% | 97% | +6% |
| Denial rate | 12% | 4% | -67% |
The transformation extends beyond simple percentage improvements. Practices gain predictable revenue streams, reduced administrative overhead, and the freedom to focus resources on patient care rather than billing complexities. Understanding how denial management in medical billing improves cash flow becomes essential to maximizing these benefits.
Technology Integration and Automation Benefits
Modern total rcm solutions leverage advanced technology platforms that automate repetitive tasks while maintaining accuracy. Automated eligibility checks prevent scheduling patients without verified coverage. Intelligent claim scrubbing identifies errors before submission, reducing rejection rates.
According to current trends in revenue cycle management software, automation and advanced analytics are fundamentally transforming financial operations in healthcare. These technologies enable real-time visibility into revenue cycle performance, allowing proactive management rather than reactive problem-solving.
Electronic remittance advice (ERA) processing exemplifies this technological advantage. Understanding ERA in medical billing reveals how automated posting reduces manual entry errors and accelerates payment reconciliation.
Selecting the Right Total RCM Solutions Partner
Choosing a comprehensive revenue cycle management provider requires careful evaluation of capabilities, experience, and alignment with your practice's specific needs. Not all total rcm solutions offer identical services or deliver comparable results.
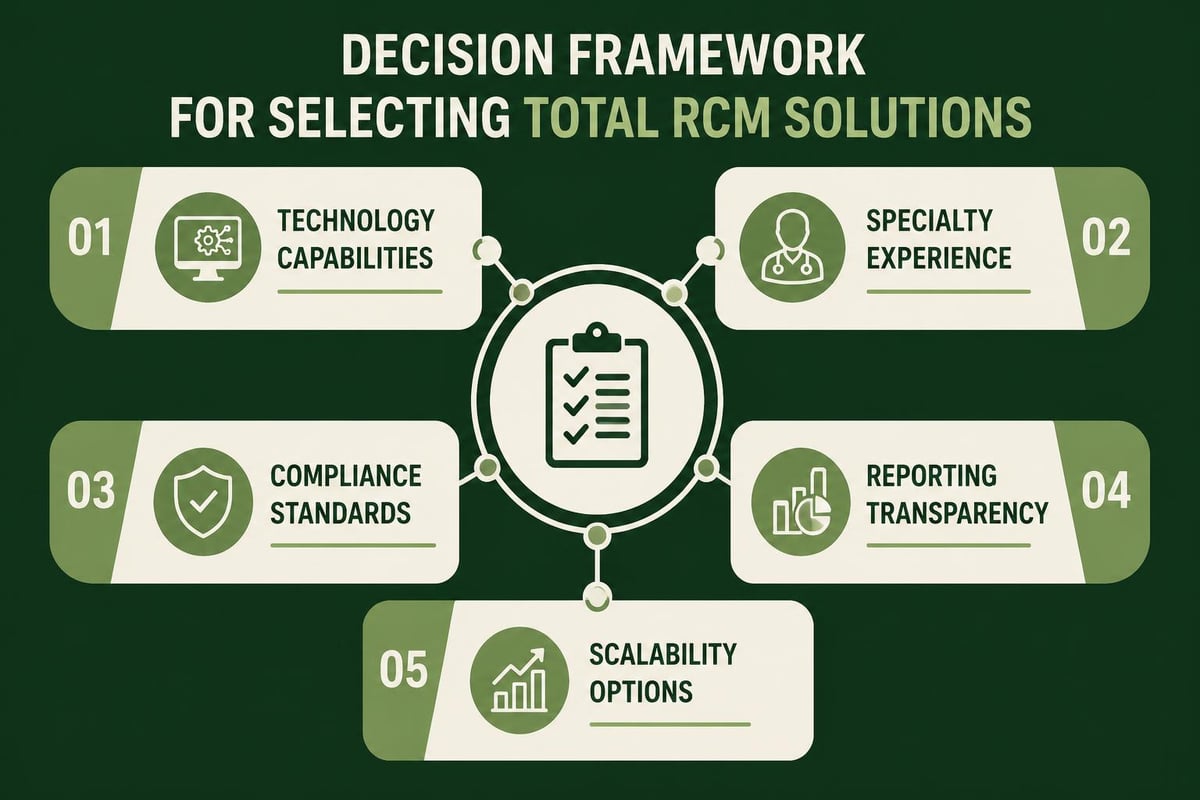
Critical evaluation criteria include:
- Specialty-specific expertise: Does the provider understand your specialty's unique coding requirements, payer policies, and reimbursement challenges?
- Technology infrastructure: What platforms and tools does the provider use, and how do they integrate with your existing practice management system?
- Transparency and reporting: How frequently will you receive performance reports, and what metrics are tracked?
- Compliance commitment: What processes ensure HIPAA compliance and data security?
- Scalability: Can the solution grow with your practice as patient volume increases?
The distinction between basic billing services and total rcm solutions becomes apparent during this evaluation. Comprehensive providers offer strategic partnership rather than transactional service delivery. They invest in understanding your practice's financial goals and develop customized approaches to achieve them.
Service Level Agreements and Performance Guarantees
Reputable providers of total rcm solutions establish clear service level agreements (SLAs) that define expected performance standards. These agreements should specify metrics such as claim submission timeframes, denial response times, and collection rates.
| Service Component | Standard SLA | Premium SLA |
|---|---|---|
| Clean claim submission | Within 48 hours | Within 24 hours |
| Denial management response | Within 5 business days | Within 2 business days |
| Patient inquiry response | Within 24 hours | Same business day |
| Monthly reporting delivery | By 10th of month | By 5th of month |
Performance guarantees demonstrate provider confidence and align incentives between your practice and the RCM partner. Some providers offer revenue guarantees or share savings arrangements that tie their compensation to your financial performance.
Overcoming Common Revenue Cycle Challenges
Healthcare practices encounter numerous obstacles that disrupt revenue cycle efficiency. Total rcm solutions address these challenges through specialized expertise and proven methodologies.
Frequent denial triggers include:
- Incorrect patient demographic information
- Missing or invalid authorization numbers
- Coding errors or lack of medical necessity documentation
- Timely filing violations
- Coordination of benefits mistakes
Each denial type requires specific intervention strategies. Demographic errors demand improved front-end registration processes and real-time eligibility verification. Authorization issues necessitate robust tracking systems and payer-specific protocols. Coding problems require ongoing education and quality assurance reviews.
Comprehensive denial management services systematically address root causes rather than merely processing appeals. This proactive approach reduces future denial frequency while recovering revenue from previously rejected claims.
Managing Payer Complexity and Contract Optimization
The proliferation of insurance plans, each with unique requirements and reimbursement rates, creates significant administrative complexity. Total rcm solutions maintain current knowledge of payer-specific policies, submission protocols, and appeal procedures across hundreds of insurance companies.
Contract analysis represents another valuable component. Expert review of payer contracts identifies underpayment patterns and negotiation opportunities. Many practices unknowingly accept reimbursement rates below their contracted amounts due to inadequate verification processes.
Implementing proper net revenue management strategies ensures that practices capture every dollar owed under existing contracts while building data to support future negotiations.
Staffing Considerations and Internal vs. Outsourced Models
Practices face a fundamental decision when implementing total rcm solutions: building internal capabilities versus partnering with specialized external providers. Each approach offers distinct advantages and challenges.
Internal billing department advantages:
- Direct control over processes and timelines
- Immediate access to billing staff for questions
- Cultural alignment with practice values
- No external vendor contracts or negotiations
Internal billing department challenges:
- Recruiting and retaining qualified billing professionals
- Ongoing training costs for regulatory changes
- Technology investment and maintenance
- Limited scalability during growth periods
- Vulnerability to staff turnover
External total rcm solutions eliminate many staffing headaches while providing access to deeper expertise. Specialized providers maintain teams of certified coders, billing specialists, and denial management experts who work exclusively on revenue cycle functions.
The cost comparison extends beyond simple salary calculations. Internal departments require office space, computers, software licenses, benefits, and ongoing education. External providers absorb these overhead costs while distributing them across multiple clients, creating economies of scale.
For practices evaluating medical billing services, the decision often hinges on practice size, growth trajectory, and leadership bandwidth for managing billing operations.
Compliance and Security in Total RCM Solutions
Healthcare revenue cycle management involves handling extraordinarily sensitive patient information, creating significant compliance obligations. Total rcm solutions must maintain rigorous security standards and demonstrate ongoing HIPAA compliance.
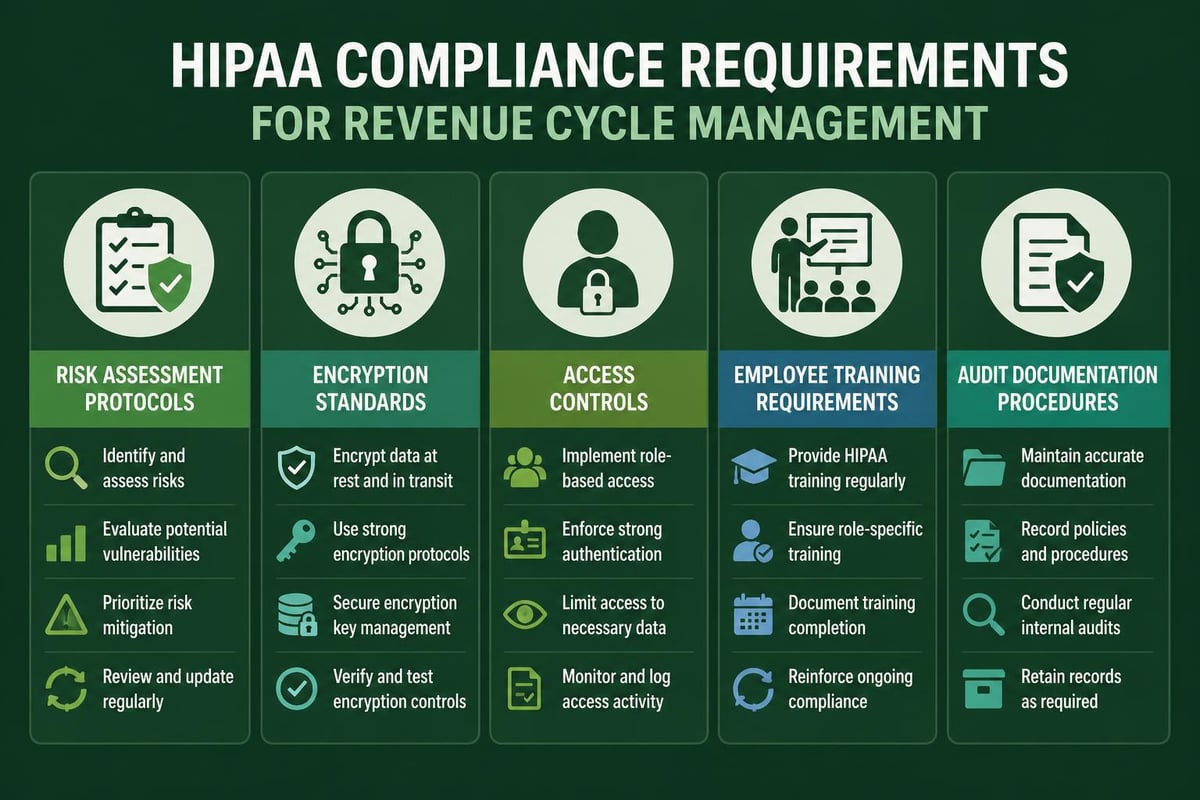
Essential compliance components include:
- Risk assessments: Regular evaluation of potential security vulnerabilities in all systems and processes
- Business associate agreements: Formal contracts defining data protection responsibilities
- Employee training: Ongoing education about privacy requirements and security protocols
- Encryption standards: Protection of data in transit and at rest using current encryption technology
- Audit trails: Comprehensive logging of all access to patient information
- Incident response plans: Documented procedures for addressing potential breaches
The consequences of compliance failures extend far beyond financial penalties. Reputation damage, patient trust erosion, and operational disruption can threaten practice viability. Partnering with providers who prioritize compliance reduces these risks substantially.
Understanding regulations such as the No Surprises Act, price transparency requirements, and evolving payer policies requires dedicated resources. Many comprehensive providers like those offering total RCM solutions include regulatory monitoring and process updates as standard service components.
Technology Platforms Supporting Comprehensive Revenue Cycle Management
The infrastructure underlying total rcm solutions has evolved dramatically with cloud computing, artificial intelligence, and advanced analytics. Modern platforms provide capabilities that were impossible just a few years ago.
Core technology features include:
- Real-time eligibility verification integrated with scheduling systems
- Automated charge capture linked to electronic health records
- Intelligent coding assistance with built-in compliance checks
- Predictive denial analytics identifying high-risk claims
- Automated payment posting with exception management
- Patient engagement portals for self-service billing
Integration represents a critical success factor. Total rcm solutions must connect seamlessly with existing practice management systems, electronic health records, and clearinghouses. APIs (application programming interfaces) enable data exchange without manual entry or file transfers.
Practices interested in top medical billing software should prioritize platforms that support comprehensive workflows rather than isolated functions. The best solutions provide end-to-end visibility from patient registration through payment reconciliation.
Analytics and Business Intelligence Capabilities
Data-driven decision making separates high-performing practices from those struggling with revenue cycle challenges. Total rcm solutions equipped with robust analytics capabilities transform raw billing data into actionable insights.
Comprehensive reporting should address multiple perspectives:
| Report Category | Key Metrics | Decision Support |
|---|---|---|
| Production | Charges by provider, procedure volume, relative value units | Capacity planning, provider productivity |
| Collections | Payments by payer, collection rates, aging analysis | Cash flow forecasting, payer negotiations |
| Denials | Denial rates by reason, payer, CPT code | Process improvement priorities, training needs |
| Compliance | Coding accuracy, documentation completeness, timely filing | Risk mitigation, audit preparation |
Advanced platforms employ predictive modeling to forecast revenue, identify collection risks, and prioritize account follow-up. Machine learning algorithms continuously improve accuracy by analyzing historical patterns and outcomes.
Patient Experience and Financial Communication
Total rcm solutions increasingly recognize that patient satisfaction extends beyond clinical care to include financial interactions. The billing experience significantly influences patient loyalty, online reviews, and referral patterns.
Modern patient engagement strategies include transparent cost estimates before service delivery, flexible payment options, and user-friendly billing statements. Digital communication channels-patient portals, text messaging, email-provide convenient alternatives to phone calls for billing inquiries.
The rise of high-deductible health plans has shifted financial responsibility to patients, making effective patient collections more critical. Comprehensive solutions address this challenge through early financial conversations, payment plan options, and compassionate collection approaches.
Practices offering services like prior authorization management understand that preventing surprise bills improves patient satisfaction while reducing collection complications.
Payment Plan Management and Financial Assistance
Total rcm solutions should include strategies for patients facing financial hardship. Structured payment plans make healthcare accessible while ensuring practices receive compensation for services rendered.
Effective payment plan programs feature:
- Clear eligibility criteria based on account balance and patient circumstances
- Automated payment processing through stored payment methods
- Flexible term options accommodating various financial situations
- Grace periods and modification procedures for patients experiencing hardship
- Integration with practice management systems for seamless tracking
Financial assistance programs demonstrate community commitment while addressing practical revenue cycle needs. Well-designed charity care policies establish qualifying criteria, required documentation, and approval processes that balance compassion with fiscal responsibility.
Measuring Success and Continuous Improvement
Implementing total rcm solutions represents the beginning of an ongoing optimization journey rather than a final destination. Continuous monitoring and refinement ensure sustained performance improvement and adaptation to changing healthcare dynamics.
Essential performance indicators include:
- Net collection rate: Percentage of allowed charges actually collected
- Days in accounts receivable: Average time from service delivery to payment receipt
- Clean claim rate: Percentage of claims paid on first submission
- Denial rate: Percentage of submitted claims rejected by payers
- Cost to collect: Total revenue cycle expenses as percentage of collections
- Patient satisfaction scores: Ratings specific to billing and financial interactions
Benchmarking against specialty-specific standards provides context for evaluating performance. What constitutes excellent performance in primary care may differ substantially from surgical specialties or diagnostic facilities.
Regular business reviews with your total rcm solutions provider should examine trends, identify opportunities, and establish improvement initiatives. Quarterly assessments allow sufficient time to observe pattern changes while maintaining momentum toward goals.
Practices seeking expertise in specialized areas like medical credentialing services benefit from providers who understand how credentialing timelines and payer enrollment impact revenue cycle performance.
Industry Trends Shaping Future Revenue Cycle Management
The healthcare landscape continues evolving rapidly, driven by regulatory changes, technological advancement, and shifting reimbursement models. Total rcm solutions must adapt to these trends to remain effective.
Emerging developments include:
- Value-based payment models replacing fee-for-service reimbursement
- Artificial intelligence automating coding, denial prediction, and payment posting
- Blockchain technology securing health information exchange
- Price transparency requirements increasing patient financial responsibility
- Telehealth integration creating new billing scenarios and compliance requirements
The transition toward value-based care fundamentally changes revenue cycle priorities. Success increasingly depends on care coordination, quality metrics, and risk management rather than volume maximization. Comprehensive providers help practices navigate these complexities while maintaining financial stability during the transition.
Organizations like Nimble Solutions demonstrate how specialized, tech-enabled approaches address the unique needs of specific healthcare sectors through intelligent insights and analytics.
Customization for Different Practice Sizes and Specialties
Total rcm solutions must accommodate tremendous variation across healthcare provider types. A solo practitioner's needs differ dramatically from those of a 50-physician multispecialty group. Similarly, cardiology billing requirements diverge significantly from mental health practice revenue cycles.
Practice size considerations:
- Solo and small practices (1-5 providers): Affordability, minimal disruption, quick implementation, personal service
- Medium practices (6-20 providers): Scalability, specialty-specific expertise, reporting capabilities, technology integration
- Large groups (20+ providers): Enterprise-level security, multi-location coordination, advanced analytics, dedicated account management
Specialty-specific expertise proves equally important. Understanding different types of medical coding reveals the complexity introduced by specialty variations in documentation requirements, coding guidelines, and payer policies.
Surgical specialties require expertise in global period billing, modifier usage, and ASC versus hospital billing distinctions. Mental health practices navigate unique challenges around session documentation, diagnosis coding, and payer authorization requirements. Primary care providers manage preventive service coding, chronic care management billing, and quality reporting programs.
Comprehensive providers maintain specialized teams with deep knowledge in specific medical specialties, ensuring accurate coding, appropriate reimbursement, and regulatory compliance unique to each field.
Implementing comprehensive revenue cycle management transforms practice financial performance through integrated processes, specialized expertise, and continuous optimization. Whether you choose to build internal capabilities or partner with external specialists, total rcm solutions provide the framework for sustainable growth and operational excellence. Greenhive Billing Solutions delivers tailored revenue cycle management services that address every aspect of your practice's financial operations, from eligibility verification through denial resolution. Our experienced team works within your existing systems to maximize reimbursements, reduce administrative burden, and ensure HIPAA-compliant processes that support your mission of delivering exceptional patient care.