The landscape of medical in the US presents unique challenges for healthcare providers, particularly when managing the financial aspects of patient care. From navigating complex insurance requirements to ensuring regulatory compliance, medical practices face mounting pressure to maintain profitability while delivering quality care. Understanding the intricacies of revenue cycle management becomes essential for clinics, hospitals, and private practices that aim to sustain operations in an increasingly demanding environment. The financial health of healthcare organizations depends heavily on efficient billing processes, accurate coding, and strategic denial management.
The Current State of Healthcare Billing Infrastructure
Medical in the US operates within a multifaceted ecosystem where providers must balance patient care with financial sustainability. The Centers for Disease Control and Prevention (CDC) tracks healthcare utilization patterns that directly impact billing volumes and complexity. Healthcare organizations process millions of claims annually, each requiring precise documentation and adherence to payer-specific guidelines.
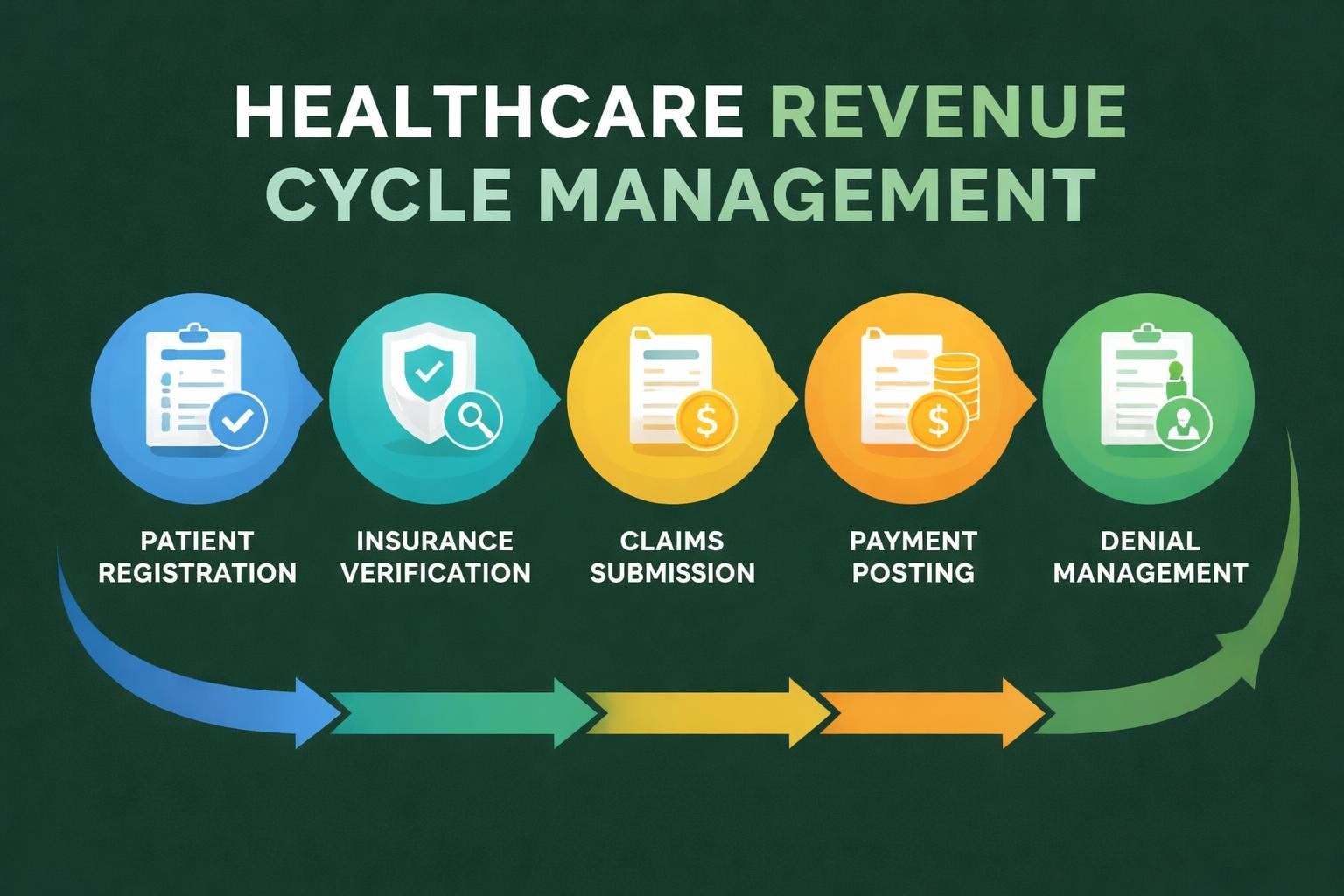
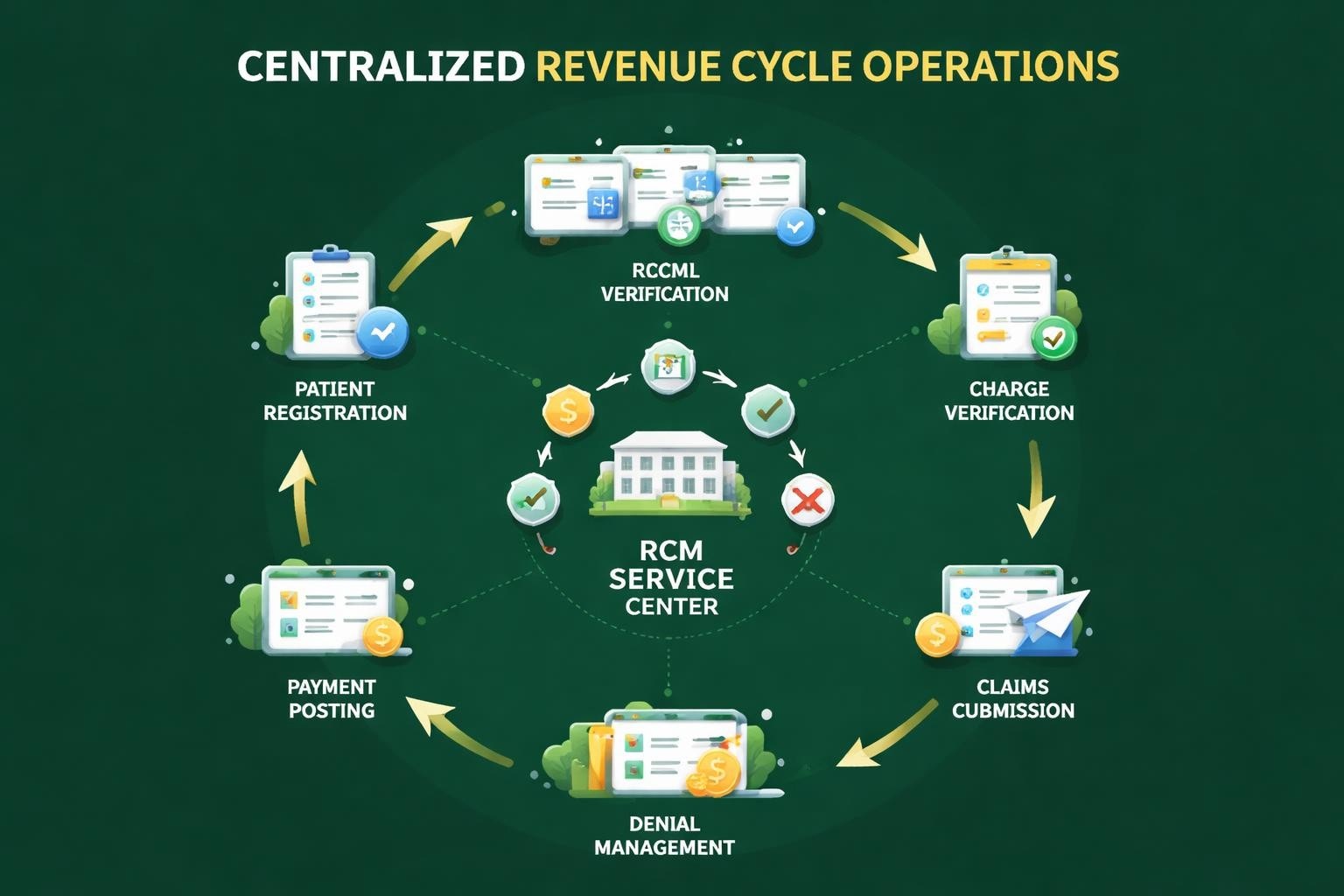
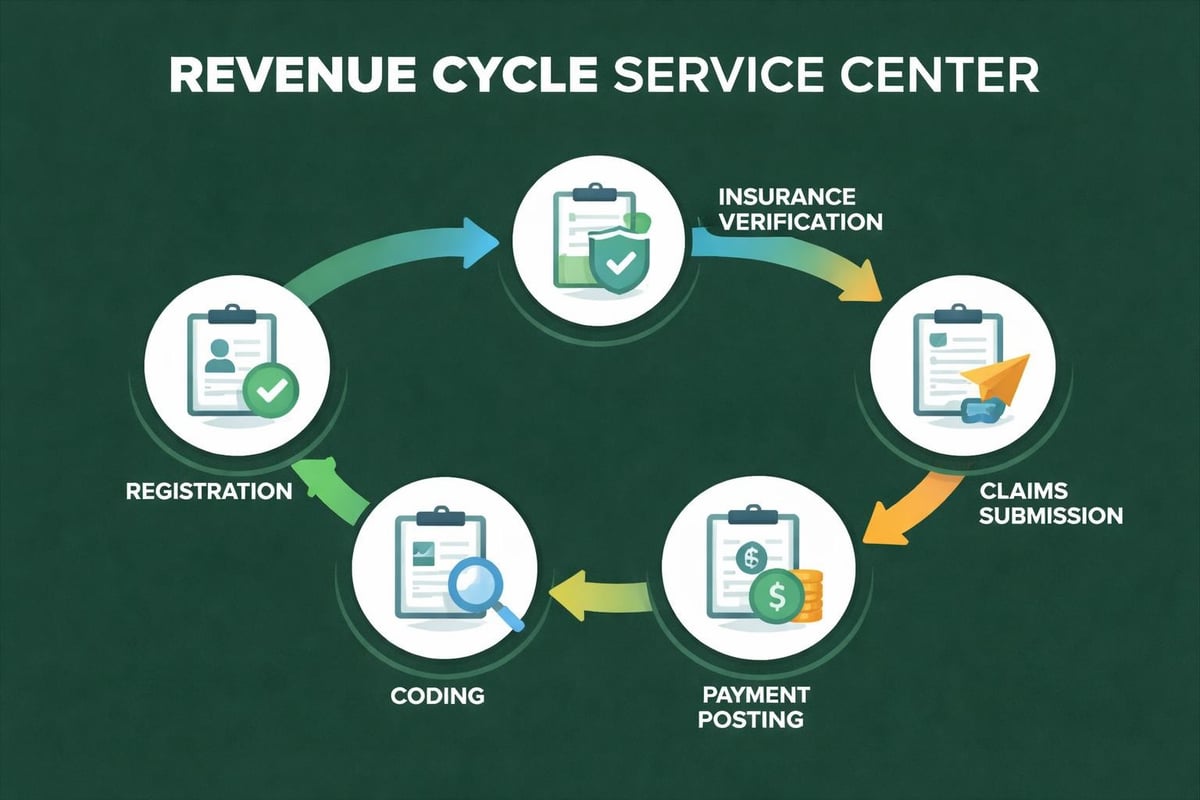
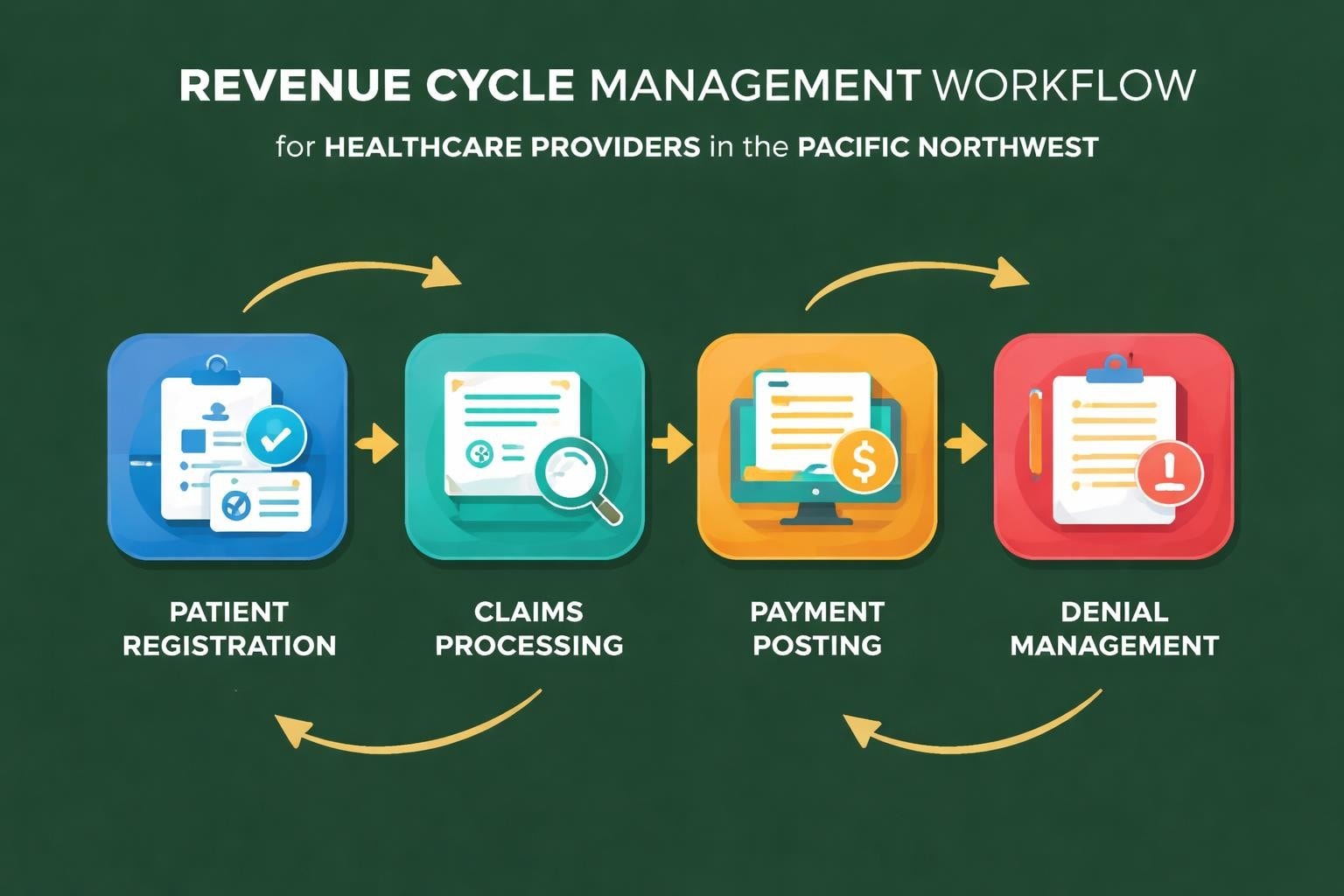
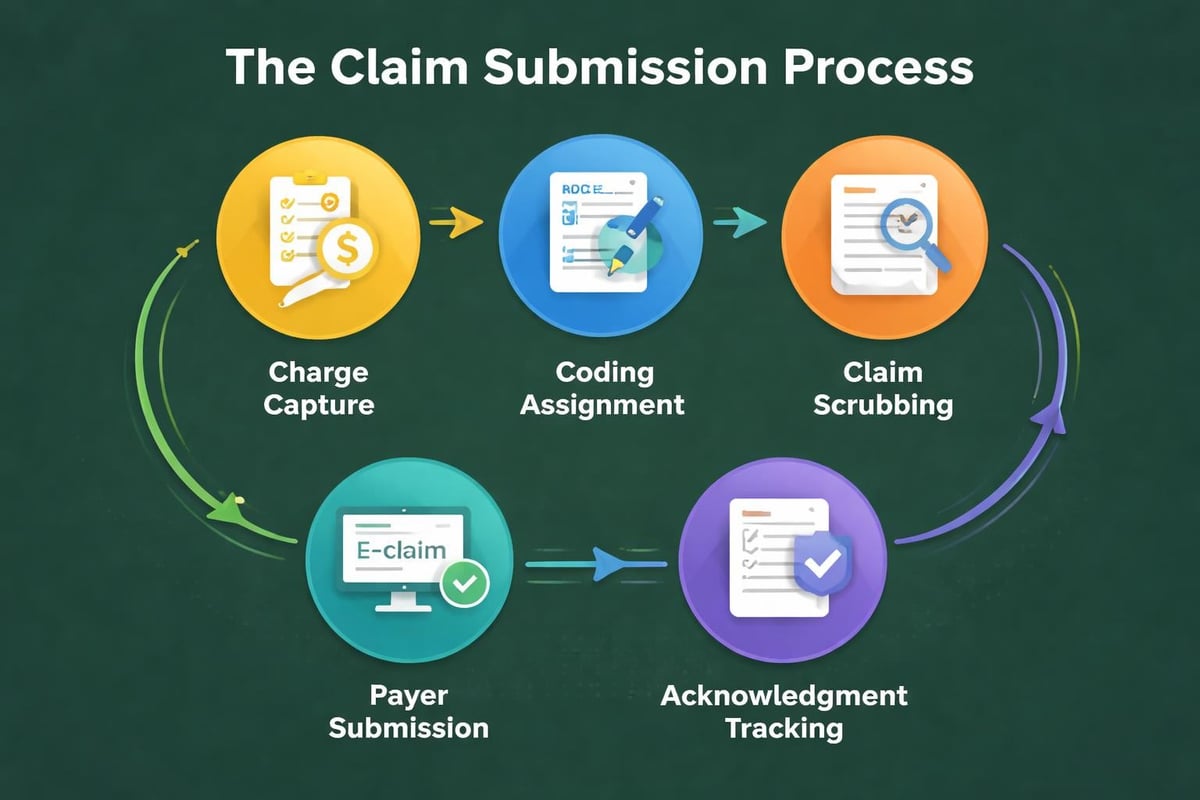
The revenue cycle begins the moment a patient schedules an appointment and extends through final payment collection. This cycle encompasses multiple touchpoints where errors can occur, leading to delayed reimbursements or outright denials. Providers must verify insurance eligibility, obtain prior authorizations, document services accurately, submit clean claims, and manage patient financial responsibilities.
Insurance Verification and Eligibility Challenges
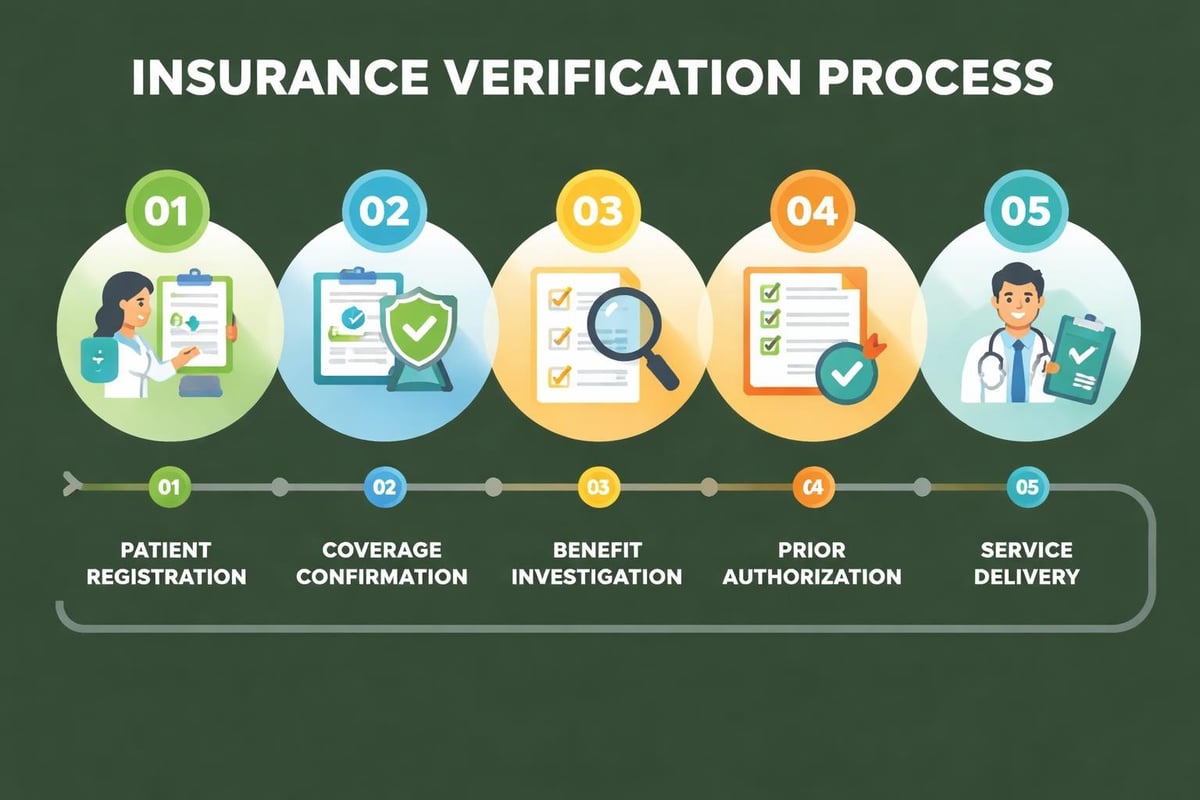
One of the earliest obstacles in medical in the US involves confirming patient coverage before services are rendered. Insurance eligibility verification prevents claim denials and reduces patient billing disputes. However, insurance plans vary significantly in their coverage policies, copayment structures, and deductible requirements.
Key verification elements include:
- Patient demographic accuracy
- Active coverage status
- Benefit limitations and exclusions
- Prior authorization requirements
- Copayment and deductible amounts
- Network participation status
Practices that neglect thorough insurance verification often face increased denial rates and delayed payments. Real-time eligibility checks have become standard practice, yet many providers still struggle with outdated systems or manual processes that introduce errors.
Coding Accuracy and Documentation Requirements
Medical in the US demands meticulous attention to coding standards that translate clinical services into billable claims. The American Medical Association (AMA) publishes Current Procedural Terminology (CPT) codes that providers use to describe medical services. Proper coding ensures appropriate reimbursement and reduces compliance risks.
Clinical documentation must support every code submitted on a claim. Insufficient documentation leads to denials, audits, and potential fraud allegations. Providers need comprehensive training on different types of medical coding systems including CPT, ICD-10-CM, and HCPCS Level II codes.
Common Coding Pitfalls
Healthcare organizations frequently encounter coding errors that compromise revenue. Undercoding leaves money on the table, while overcoding invites scrutiny and penalties. Mismatched diagnosis and procedure codes trigger automatic denials from payers.
| Error Type | Impact | Prevention Strategy |
|---|---|---|
| Unbundling | Incorrect payment, audit risk | Use appropriate bundling edits |
| Modifier misuse | Claim rejection | Train staff on modifier application |
| Outdated codes | Automatic denial | Implement regular code updates |
| Incomplete documentation | Delayed payment | Establish documentation protocols |
Understanding what CPT codes mean for insurance claims helps practices avoid these costly mistakes. Regular audits identify patterns that require corrective action.
Claims Submission and Processing Complexity
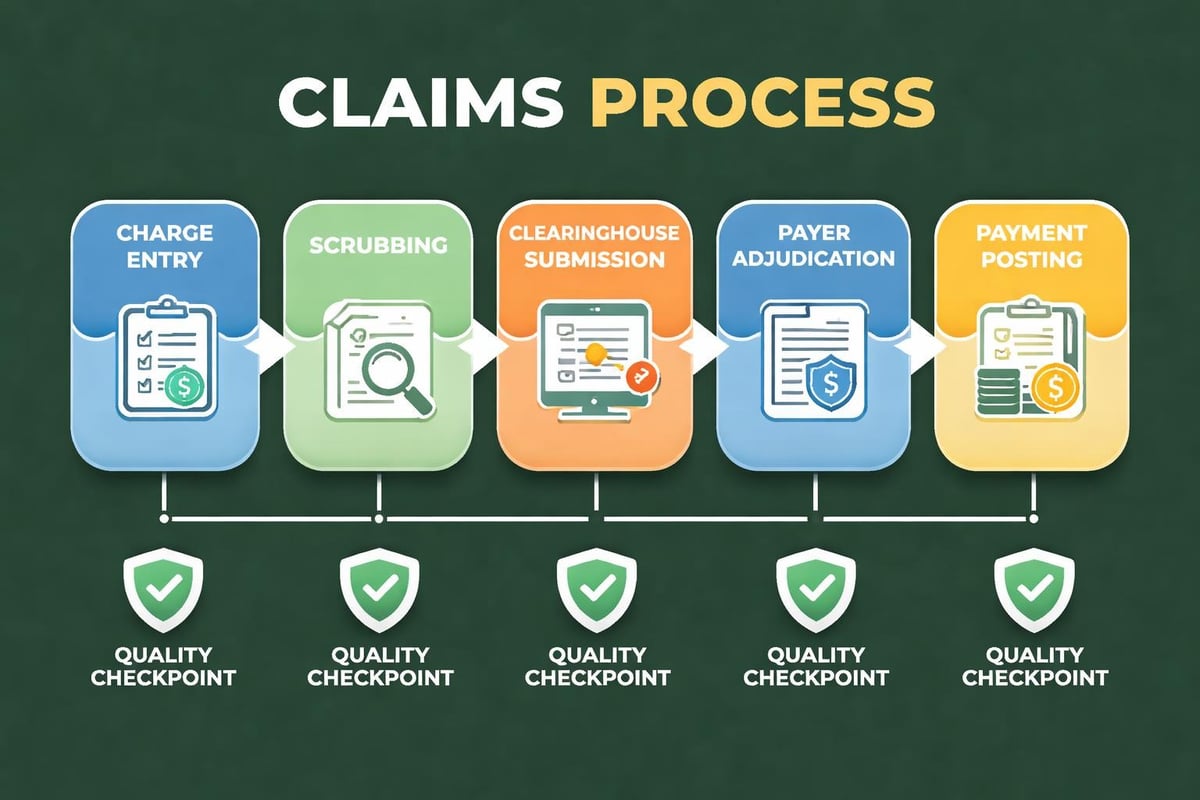
Medical in the US involves navigating diverse payer requirements during claims submission. Each insurance company maintains unique formatting rules, timely filing limits, and documentation standards. Electronic claims submission has streamlined many processes, yet errors still occur frequently.
Clean claims that contain no errors pass through payer systems without delays. Achieving high clean claim rates requires systematic quality checks before submission. Practices should target clean claim rates above 95% to maintain healthy cash flow.
Payer-Specific Requirements
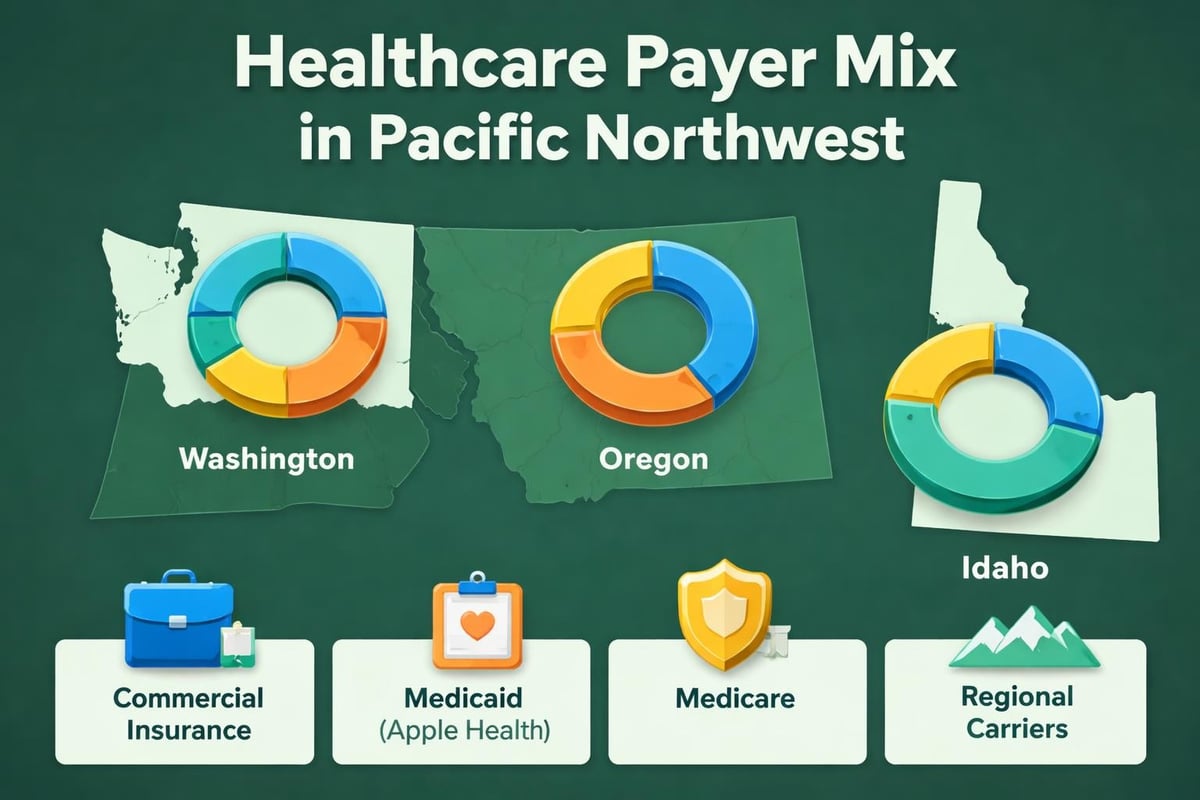
Commercial insurers, Medicare, Medicaid, and managed care organizations each impose distinct submission protocols. Medicare requires specific place of service codes and accepts only certain billing formats. Commercial payers may demand additional documentation or use proprietary coding systems.
Critical submission considerations:
- Timely filing deadlines – Most payers enforce strict submission windows ranging from 90 days to one year from the date of service
- Electronic formatting standards – HIPAA 837 transaction sets must comply with payer specifications
- Attachment protocols – Medical records and supporting documentation require specific submission methods
- Coordination of benefits – Multiple insurance coverage demands proper sequencing
Practices serving diverse patient populations must maintain expertise across multiple payer systems. The National Institutes of Health (NIH) conducts research on healthcare delivery systems that inform best practices in claims management.
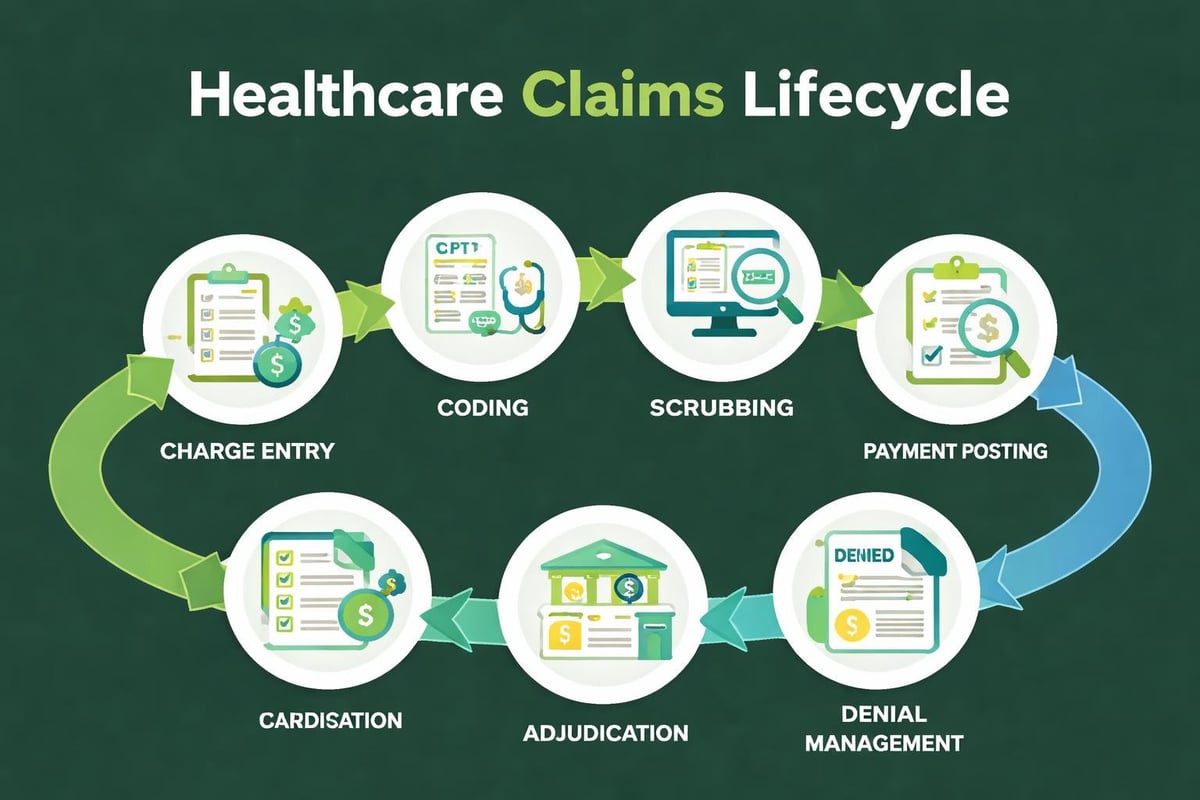
Denial Management and Appeals Strategy
Denial rates significantly impact the financial performance of medical practices in the US. Industry benchmarks suggest that 5-10% of claims receive initial denials, though many are recoverable through appeals. Effective denial management in medical billing improves cash flow and reduces revenue leakage.
Analyzing denial patterns reveals systemic issues requiring process improvements. Common denial reasons include missing information, authorization failures, timely filing violations, and medical necessity disputes. Each denial category demands specific resolution tactics.
Building an Effective Appeals Process
Successful appeals require organized documentation, clear communication, and persistent follow-up. Providers should establish standardized workflows for addressing different denial types. First-level appeals often involve simple corrections or additional documentation.
Step-by-step appeals approach:
- Categorize denials – Sort by denial reason, payer, and service type to identify trends
- Determine appeal viability – Assess whether the denial is worth the time investment based on claim value
- Gather supporting documentation – Compile medical records, authorization letters, and correspondence
- Draft compelling appeal letters – Clearly explain why the service was medically necessary and properly documented
- Submit within deadline – Most payers allow 30-180 days for first-level appeals
- Track outcomes – Monitor appeal success rates to refine strategies
Understanding how to appeal medical insurance denials empowers practices to recover rightfully owed revenue. Persistent follow-up on pending appeals prevents claims from aging beyond recovery.
Regulatory Compliance and Risk Management
Medical in the US operates under extensive federal and state regulations governing billing practices. HIPAA privacy rules, anti-kickback statutes, and False Claims Act provisions create substantial compliance obligations. Violations result in severe penalties including fines, exclusion from federal programs, and criminal prosecution.
Providers must implement comprehensive compliance programs that address billing accuracy, documentation standards, and fraud prevention. Regular training ensures staff understand regulatory requirements and organizational policies. Internal audits identify vulnerabilities before external reviewers discover them.
Key Compliance Areas
Healthcare organizations face scrutiny from multiple oversight entities including Medicare Administrative Contractors, commercial payer auditors, and government agencies. Maintaining compliant operations requires ongoing vigilance across various domains.
| Compliance Area | Primary Regulations | Risk Level |
|---|---|---|
| Coding accuracy | CPT, ICD-10, HCPCS guidelines | High |
| Documentation completeness | Medicare guidelines, payer policies | High |
| Privacy protection | HIPAA Privacy Rule | Critical |
| Security safeguards | HIPAA Security Rule | Critical |
| Billing integrity | False Claims Act, Anti-Kickback Statute | High |
Resources from Medical News Today provide updates on healthcare policy changes affecting billing practices. Staying informed about regulatory developments helps practices adapt proactively.
Financial Performance Metrics and Analytics
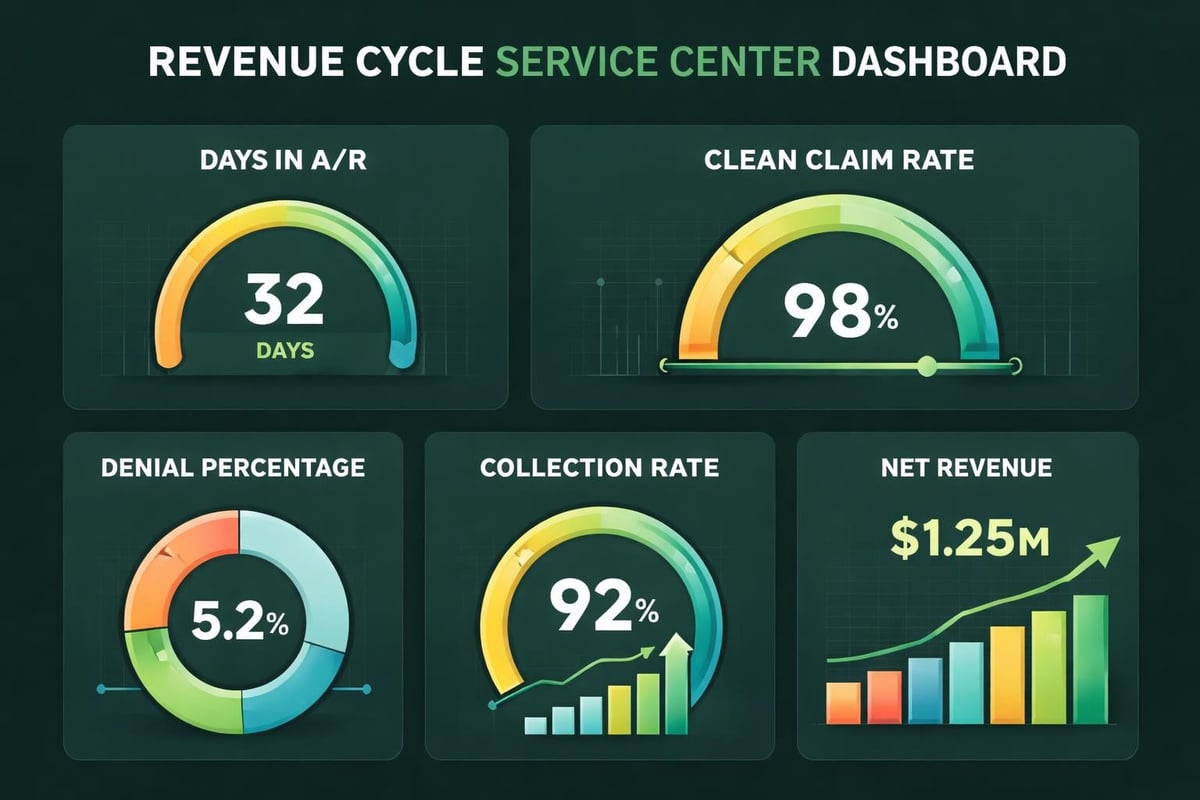
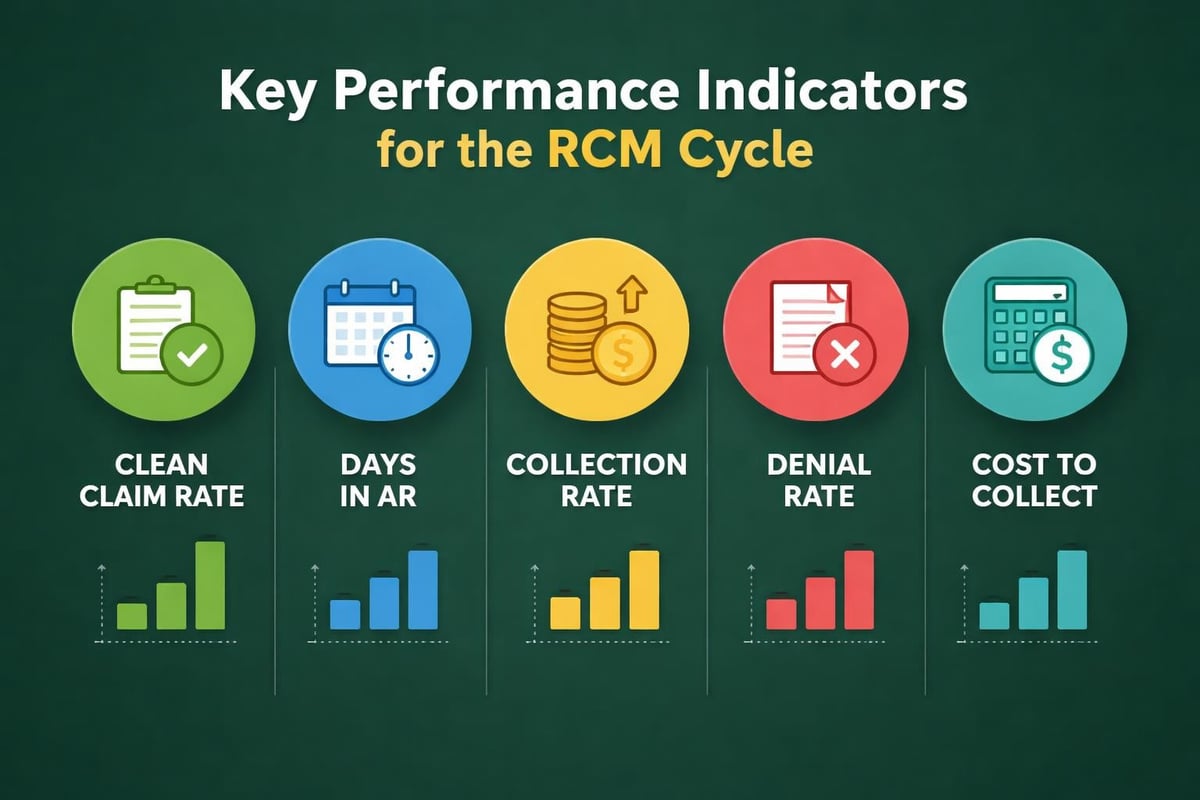
Successful management of medical operations in the US depends on tracking key performance indicators that reveal revenue cycle health. Days in accounts receivable, collection rates, and denial percentages provide insight into operational efficiency. Practices should establish benchmarks and monitor trends over time.
Healthcare revenue cycle analytics transform raw data into actionable insights. Dashboard reporting enables leadership to identify problems quickly and measure improvement initiatives. Regular financial reviews ensure the practice maintains profitability targets.
Essential Revenue Cycle Metrics
Healthcare providers should monitor multiple indicators across the revenue cycle continuum. Each metric illuminates specific aspects of financial performance and operational efficiency.
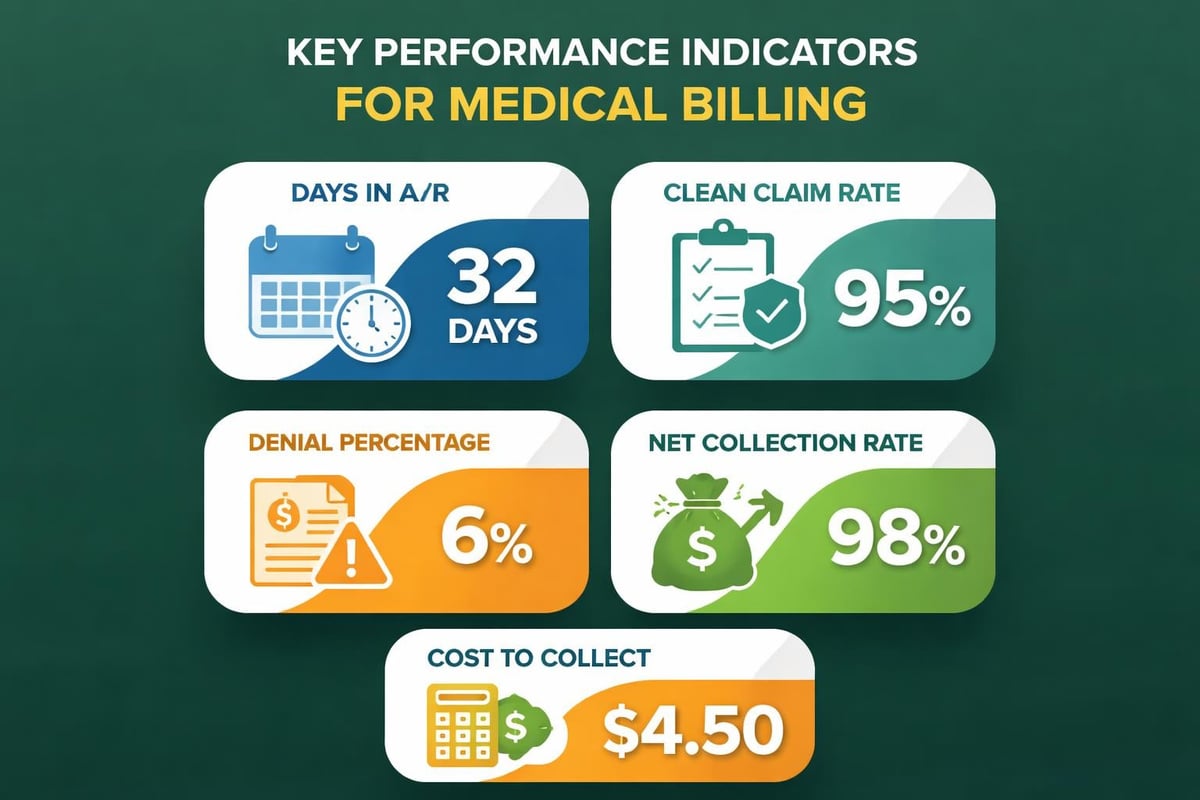
- Net collection rate – Percentage of collectible revenue actually received
- Days in A/R – Average time from service date to payment receipt
- Clean claim rate – Percentage of claims accepted without errors on first submission
- Denial rate – Percentage of claims denied by payers
- Cost to collect – Operational expenses per dollar collected
- Patient payment collection – Percentage of patient responsibility collected
Benchmarking against industry standards helps identify areas requiring attention. Practices performing below benchmarks should investigate root causes and implement corrective measures.
Technology Solutions and Outsourcing Considerations
Medical billing in the US increasingly relies on sophisticated software platforms that automate routine tasks and reduce errors. Practice management systems integrate scheduling, billing, and clinical documentation. Electronic health records facilitate coding accuracy through built-in decision support.
However, technology alone cannot solve all revenue cycle challenges. Many practices lack the internal expertise to maximize software capabilities or maintain current knowledge of billing regulations. The complexity of medical billing charges and evolving payer requirements overwhelms smaller organizations.
Evaluating Service Provider Partnerships
Healthcare providers increasingly partner with specialized revenue cycle management companies that offer comprehensive support. These partnerships allow practices to focus on clinical care while experts handle billing complexities. When evaluating potential partners, providers should assess several critical factors.
Selection criteria for RCM partners:
- Industry experience and healthcare specialization
- Technology platform capabilities and integration options
- Compliance track record and audit procedures
- Transparent reporting and communication practices
- Pricing structure and performance guarantees
- Client references and demonstrated results
Understanding medical billing costs helps practices evaluate the financial impact of outsourcing versus maintaining in-house operations. Research from PubMed includes studies on healthcare administrative efficiency that inform these decisions.
Payer Contract Negotiation and Management
The financial viability of medical practices in the US depends significantly on negotiated reimbursement rates with insurance companies. Contract terms dictate payment amounts, billing requirements, and dispute resolution procedures. Providers must approach negotiations strategically to secure favorable terms.
Many practices accept initial contract offers without negotiation, leaving substantial revenue potential unrealized. Understanding payer leverage points and market dynamics strengthens negotiating positions. Practices should analyze their patient mix, competitive positioning, and service differentiation.
Contract Review Essentials
Payer contracts contain complex provisions affecting revenue capture. Providers should scrutinize every clause before signing and periodically review existing agreements. Legal counsel specializing in healthcare contracts provides valuable guidance during negotiations.
| Contract Element | Considerations | Impact on Revenue |
|---|---|---|
| Fee schedules | Comparison to Medicare rates | Direct payment amount |
| Carve-outs | Services excluded from standard rates | Potential underpayment |
| Timely filing | Claim submission deadlines | Denial risk |
| Credentialing | Provider enrollment requirements | Payment eligibility |
| Termination clauses | Notice periods and conditions | Business continuity |
Effective revenue cycle billing requires ongoing contract management that identifies underpayment and enforces agreement terms. Regular rate analyses ensure contracts remain financially viable.
Specialized Service Line Considerations
Different medical specialties face unique billing challenges within the broader context of medical in the US. Behavioral health services encounter extensive prior authorization requirements and session limits. Surgical specialties navigate complex bundling rules and modifier applications.
Medical billing for behavioral health demands expertise in mental health parity regulations and telehealth billing codes. Specialty-specific knowledge ensures compliant billing and optimal reimbursement.
Urgent Care and Multi-Location Practices
Urgent care facilities operate under distinct billing parameters compared to traditional office practices. These high-volume operations require efficient workflows that maintain accuracy despite rapid patient turnover. Urgent care revenue cycle management addresses the unique challenges of extended hours, walk-in visits, and diverse payer mixes.
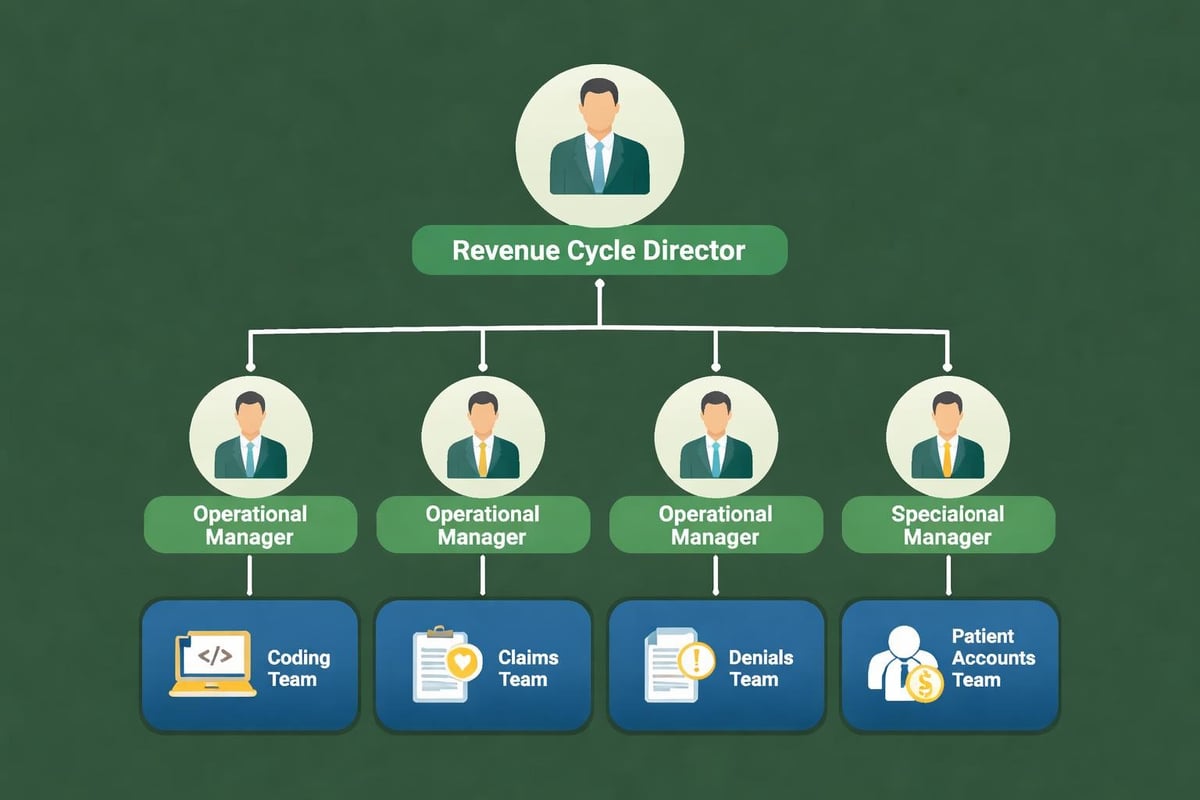
Multi-location practices face additional complexity coordinating billing across sites. Centralized billing operations improve consistency and efficiency. However, location-specific payer contracts and state regulations require careful management.
Patient Financial Responsibility and Collections
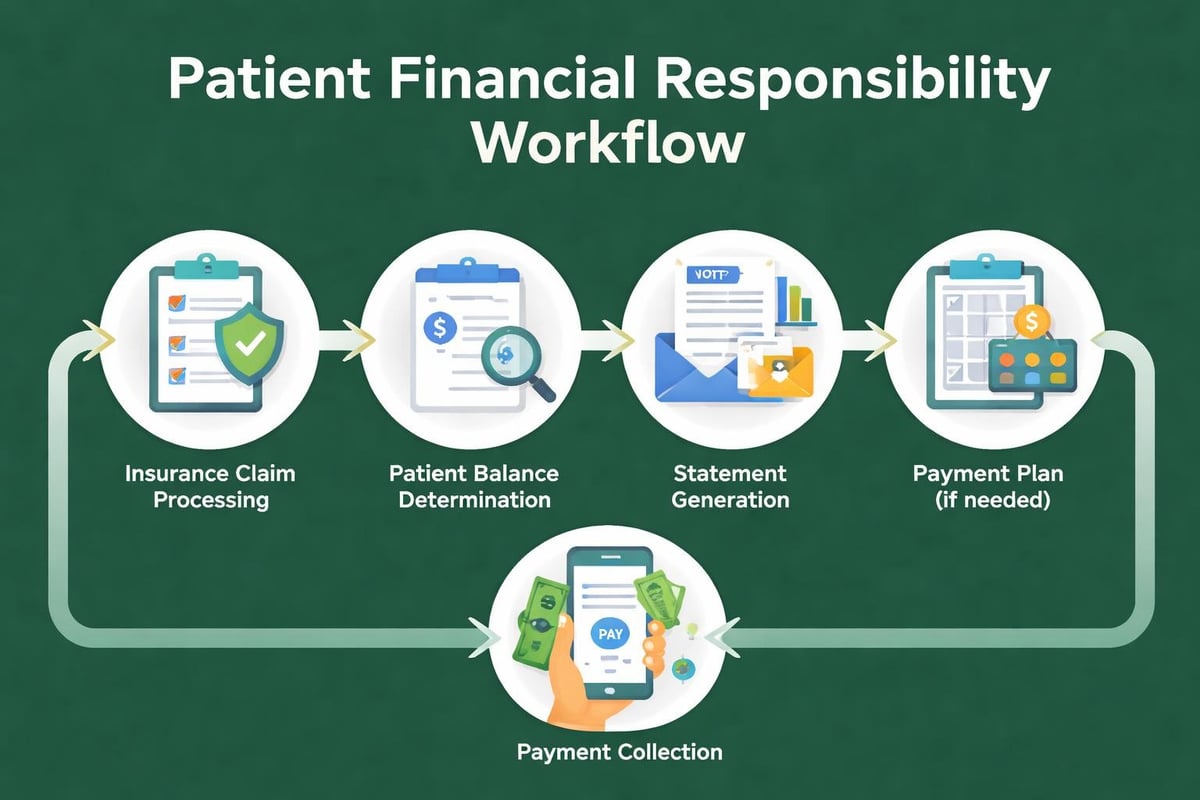
Medical in the US increasingly shifts costs to patients through higher deductibles and copayments. This trend creates collection challenges for providers accustomed to insurance-driven revenue. Practices must develop patient-friendly payment policies while maintaining cash flow.
Transparent communication about financial obligations improves collection rates. Providing cost estimates before service delivery reduces billing disputes. Offering payment plans accommodates patients facing financial hardship while ensuring revenue capture.
Best Practices for Patient Collections
Successful patient collection strategies balance financial needs with relationship preservation. Practices should establish clear policies applied consistently across all patients. Training front desk staff on financial conversations creates positive interactions.
Effective patient collection strategies:
- Collect at time of service – Point-of-service collections significantly improve overall collection rates
- Offer multiple payment methods – Credit cards, payment plans, and online portals increase convenience
- Send clear statements – Patient-friendly bills explain charges in understandable language
- Follow up promptly – Contact patients within 30 days of statement mailing
- Establish payment plans – Structured agreements accommodate patient budgets while securing commitments
- Know when to write off – Set thresholds for pursuing small balances or aged accounts
Resources from MedicineNet provide patient education materials that support informed financial discussions. Understanding patient perspectives improves collection outcomes.
Staff Training and Process Optimization
The human element remains critical despite technological advances in medical billing in the US. Well-trained staff who understand both clinical operations and billing requirements drive revenue cycle success. Ongoing education keeps teams current on regulatory changes and payer updates.
Cross-training staff across multiple revenue cycle functions creates operational flexibility. When team members understand how their work impacts downstream processes, they exercise greater care and accountability. Regular team meetings facilitate communication and problem-solving.
Developing Revenue Cycle Competency
Healthcare organizations should invest in structured training programs that build billing expertise. New hires require comprehensive onboarding covering organizational policies, software systems, and payer requirements. Experienced staff benefit from continuing education on regulatory updates and best practices.
Certification programs demonstrate professional competency and commitment to excellence. Organizations that support professional development retain skilled employees and improve performance outcomes. Understanding what you need to do medical billing and coding successfully guides individual career development and organizational hiring decisions.
Navigating the complexities of medical in the US requires strategic planning, operational excellence, and continuous adaptation to regulatory changes. Healthcare providers must balance clinical priorities with financial sustainability through efficient revenue cycle management. When internal resources prove insufficient to manage these demands, partnering with experienced professionals offers a viable solution. Greenhive Billing Solutions delivers comprehensive revenue cycle management services that help healthcare providers optimize reimbursements, reduce denials, and improve cash flow through expert billing support, claims processing, and denial management tailored to your practice's unique needs.