The healthcare industry faces increasing pressure to maintain financial stability while delivering quality patient care. At the heart of this challenge lies the revenue cycle management framework, a systematic approach that determines how efficiently medical practices convert patient services into collected revenue. Understanding the rcm process is essential for healthcare providers seeking to optimize cash flow, reduce administrative burden, and ensure compliance with evolving regulations. This comprehensive guide examines the critical components of revenue cycle management and provides actionable strategies for healthcare organizations to improve their financial performance.
Understanding the Revenue Cycle Management Framework
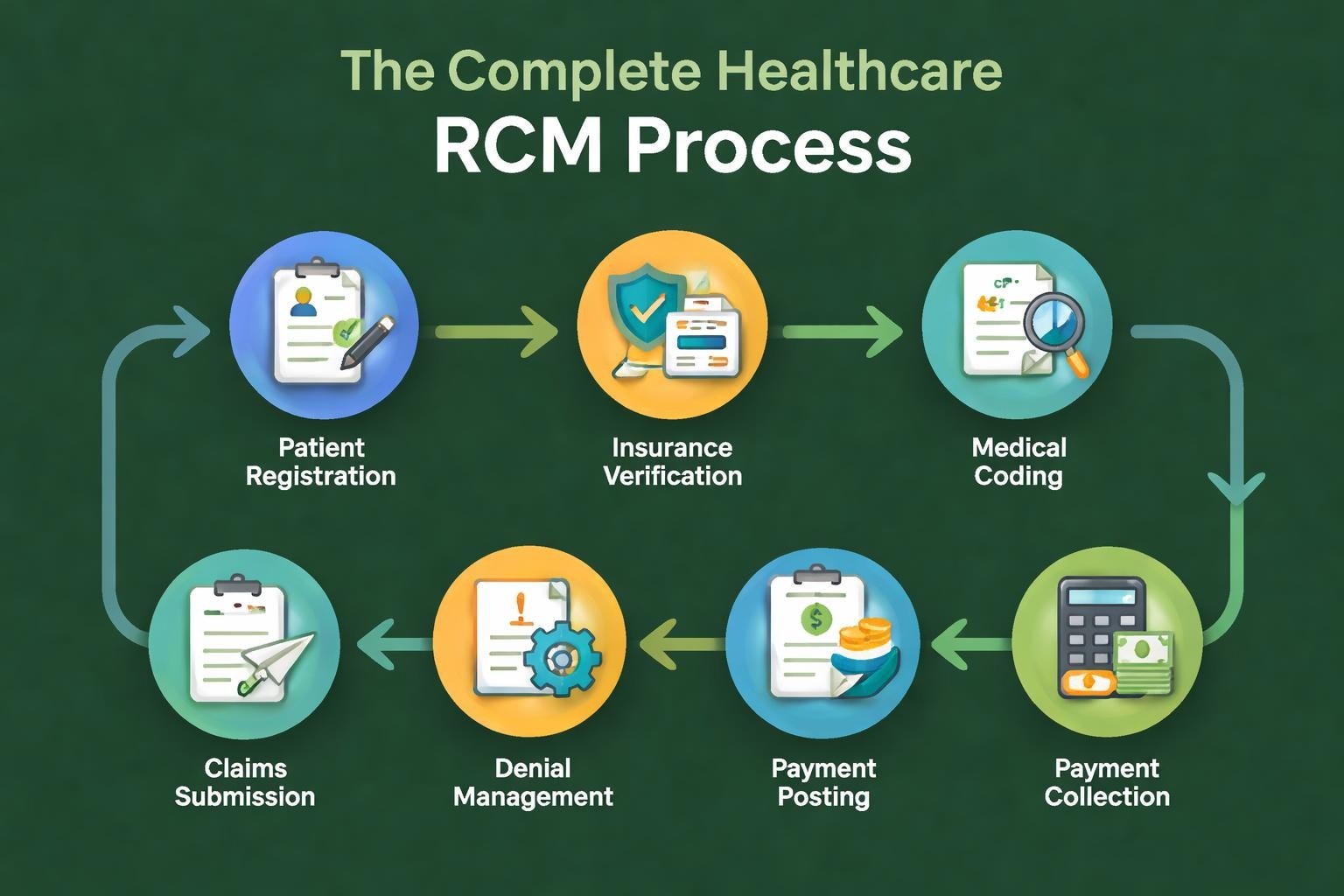
Revenue cycle management encompasses all administrative and clinical functions that contribute to the capture, management, and collection of patient service revenue. The rcm process begins the moment a patient schedules an appointment and continues through final payment collection and reconciliation. Each stage requires meticulous attention to detail, appropriate technology, and trained personnel to prevent revenue leakage.
Healthcare providers often underestimate the complexity involved in managing their revenue cycles effectively. The process involves multiple stakeholders, including front desk staff, clinical teams, billing specialists, coding professionals, and payer representatives. When any component of this ecosystem breaks down, the entire revenue stream suffers.
Core Components of the RCM Process
The rcm process consists of several interconnected stages that must function seamlessly together. These components include patient access management, charge capture, claims management, payment processing, and denial resolution. Each stage presents unique challenges and opportunities for optimization.
Patient access management establishes the foundation for successful revenue collection. This phase involves verifying patient demographics, confirming insurance eligibility, obtaining necessary authorizations, and collecting patient responsibility amounts. Errors at this stage cascade through the entire revenue cycle, resulting in delayed payments and increased denial rates.
Charge capture ensures that all billable services are documented and coded correctly. This requires close collaboration between clinical staff and billing departments to capture every procedure, supply, and service provided. Missing charges represent lost revenue that can never be recovered, making this stage critical for financial performance.
Step-by-Step Breakdown of the RCM Process
Step 1: Patient Registration and Scheduling
The rcm process initiates when patients schedule appointments or present for services. During this phase, staff members collect essential demographic information, verify insurance coverage, and confirm appointment details. Accurate data collection at this point prevents downstream complications.
Front desk personnel should verify several critical data points during registration:
- Patient full legal name matching insurance cards
- Current address and contact information
- Insurance policy numbers and group identifiers
- Primary care physician information
- Emergency contact details
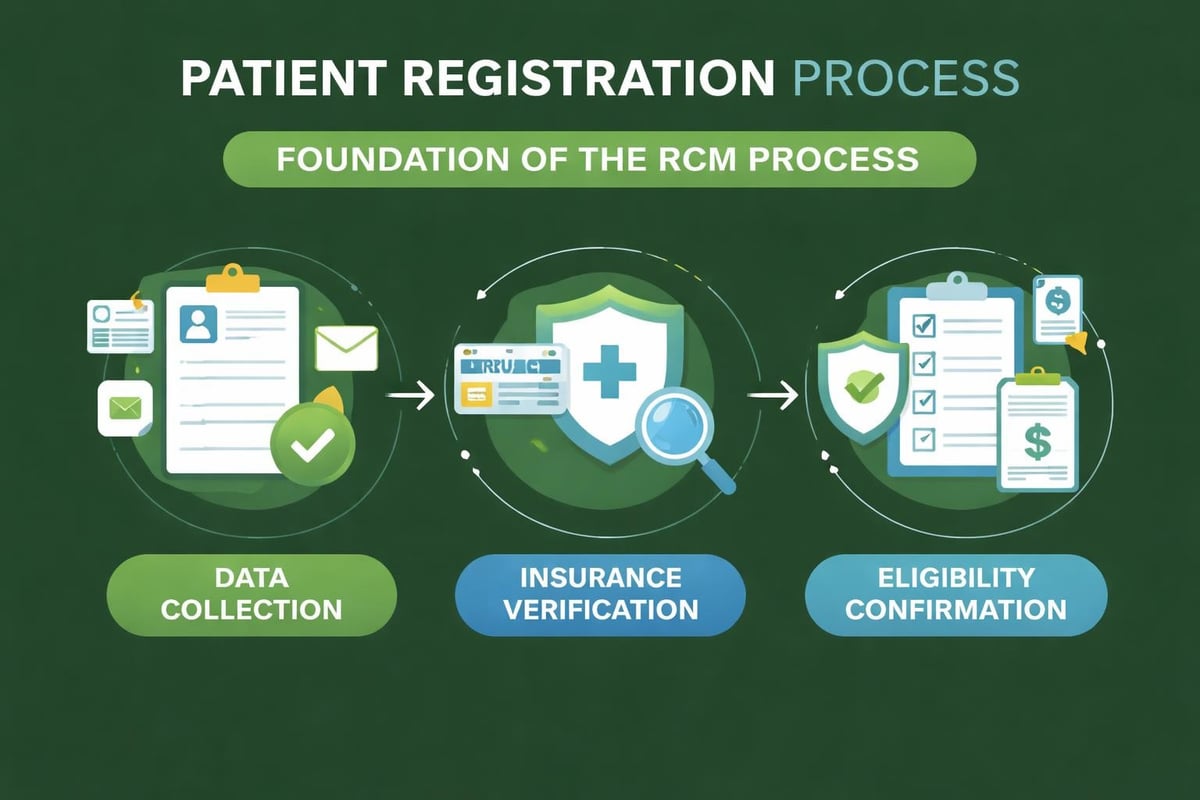
Step 2: Insurance Verification and Authorization
Before services are rendered, healthcare revenue cycle management requires confirmation of coverage and benefits. This verification process prevents claim denials due to inactive policies, incorrect subscriber information, or services not covered under the patient's plan. Implementing accurate NPI lookup best practices helps reduce errors during this crucial stage.
Thorough verification includes checking deductible amounts, copayment requirements, coinsurance percentages, and out-of-pocket maximums. For specialized procedures, obtaining prior authorization from payers becomes mandatory before rendering services.
| Verification Element | Purpose | Impact on Revenue |
|---|---|---|
| Active Coverage Status | Confirms patient has valid insurance | Prevents complete claim denials |
| Benefit Limits | Identifies service restrictions | Avoids unauthorized service denials |
| Prior Authorization | Secures payer approval for procedures | Eliminates medical necessity denials |
| Patient Responsibility | Calculates expected patient payment | Improves upfront collections |
Step 3: Charge Capture and Documentation
Once services are delivered, clinical documentation must accurately reflect all procedures performed, supplies used, and time spent with patients. The rcm process relies heavily on complete and precise documentation to support appropriate coding and billing.
Healthcare providers should implement processes that capture charges in real-time or as close to the point of service as possible. Delayed charge entry increases the risk of forgotten procedures and missed revenue opportunities. Electronic health record systems can facilitate automatic charge capture when properly configured.
Step 4: Medical Coding and Compliance
Professional medical coders translate clinical documentation into standardized diagnosis and procedure codes using ICD-10, CPT, and HCPCS code sets. This translation forms the language of healthcare billing and determines reimbursement amounts. Understanding different types of medical coding helps providers appreciate the complexity and importance of this stage.
The rcm process depends on coding accuracy for several reasons. Correct codes ensure appropriate reimbursement levels, support medical necessity, comply with payer requirements, and protect against audit risks. Coding errors, whether upcoding or undercoding, can result in lost revenue, compliance violations, and legal exposure.
Key coding considerations include:
- Specificity in diagnosis code selection
- Proper sequencing of primary and secondary diagnoses
- Accurate procedure code assignment
- Appropriate modifier usage to clarify services
- Compliance with payer-specific coding guidelines
Claims Submission and Management
Step 5: Claims Generation and Scrubbing
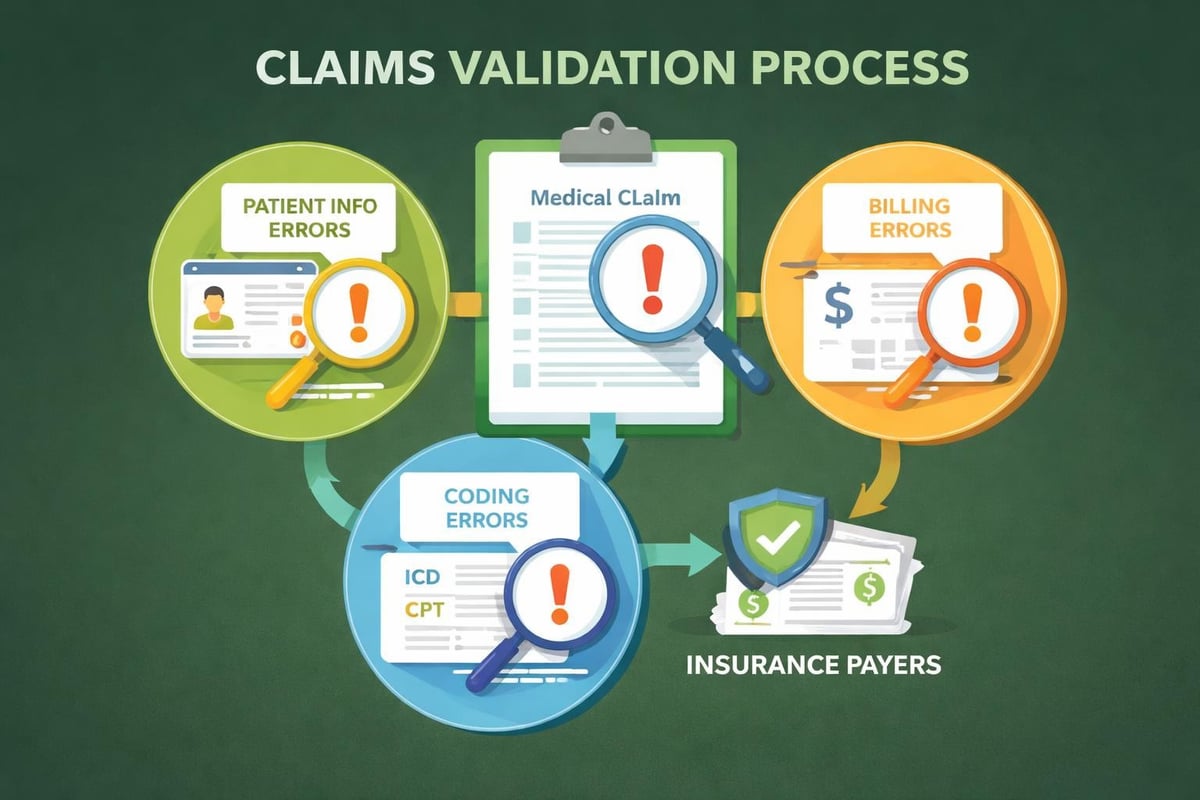
After coding completion, the rcm process moves to claims creation. Modern billing systems generate electronic claims automatically based on entered charges and codes. However, before submission to payers, claims should undergo thorough scrubbing to identify potential errors.
Claims scrubbing software analyzes submissions for common errors such as missing information, invalid code combinations, demographic mismatches, and compliance issues. Identifying and correcting these problems before submission significantly reduces denial rates and accelerates payment cycles. Medical claim submission services can streamline this complex process for busy practices.
Step 6: Electronic Claims Transmission
Clean claims are transmitted electronically to payers through clearinghouses or direct connections. The rcm process benefits enormously from electronic submission, which reduces processing time, minimizes lost claims, provides submission confirmation, and enables faster adjudication compared to paper submissions.
Most payers acknowledge claim receipt within 24-48 hours, allowing billing teams to track submission status and identify transmission failures quickly. This rapid feedback loop enables prompt correction and resubmission when necessary.
Step 7: Payment Posting and Reconciliation
As payers adjudicate claims, they issue explanation of benefits documents detailing approved amounts, adjustments, and patient responsibilities. The rcm process requires accurate payment posting to update patient accounts and maintain financial records.
Payment posting involves several critical tasks:
- Recording insurance payments to appropriate claims
- Applying contractual adjustments according to fee schedules
- Identifying and posting patient responsibility balances
- Recognizing and flagging underpayments or overpayments
- Reconciling posted payments against bank deposits
Accurate posting enables practices to monitor accounts receivable aging, identify collection opportunities, and recognize payment trends across different payers.
Denial Management and Appeals
Step 8: Denial Identification and Analysis
Despite best efforts, a percentage of claims receive denials or rejections from payers. The rcm process must include robust denial management capabilities to recover this revenue. Understanding how denial management improves cash flow helps practices prioritize this critical function.
Not all denials are equal. Some represent simple administrative errors easily corrected and resubmitted, while others require detailed appeals with supporting documentation. Effective denial management begins with categorizing denials by root cause to identify systemic issues requiring process improvements.
| Denial Category | Common Causes | Resolution Approach |
|---|---|---|
| Registration Errors | Incorrect patient information | Verify data and resubmit |
| Authorization Issues | Missing prior approvals | Obtain retroactive authorization if possible |
| Coding Problems | Invalid or unsupported codes | Review documentation and recode |
| Timely Filing | Missed submission deadlines | Appeal with proof of timely filing |
| Medical Necessity | Insufficient documentation | Submit additional clinical records |
Step 9: Appeals and Resubmission
For denials requiring appeals, the rcm process demands organized documentation, clear communication, and persistent follow-up. Successful appeals typically include detailed explanation letters, supporting clinical documentation, relevant coding guidelines, and payer policy references.
Time limits govern the appeals process, with most payers establishing strict deadlines for each appeal level. Missing these deadlines forfeits the opportunity to recover payment, making timely action essential for revenue preservation.
Patient Billing and Collections
Step 10: Patient Statement Generation
After insurance adjudication, remaining patient balances must be billed and collected. The rcm process extends beyond insurance payments to include patient responsibility amounts, which have grown substantially in recent years due to high-deductible health plans.
Effective patient billing requires clear, understandable statements that explain services received, insurance payments applied, adjustments made, and amounts owed. Transparency in billing communications reduces confusion, decreases payment delays, and improves patient satisfaction.
Best practices for patient statements include:
- Itemized service descriptions in plain language
- Clear explanation of insurance processing
- Multiple payment options and instructions
- Contact information for billing questions
- Payment plan availability for larger balances
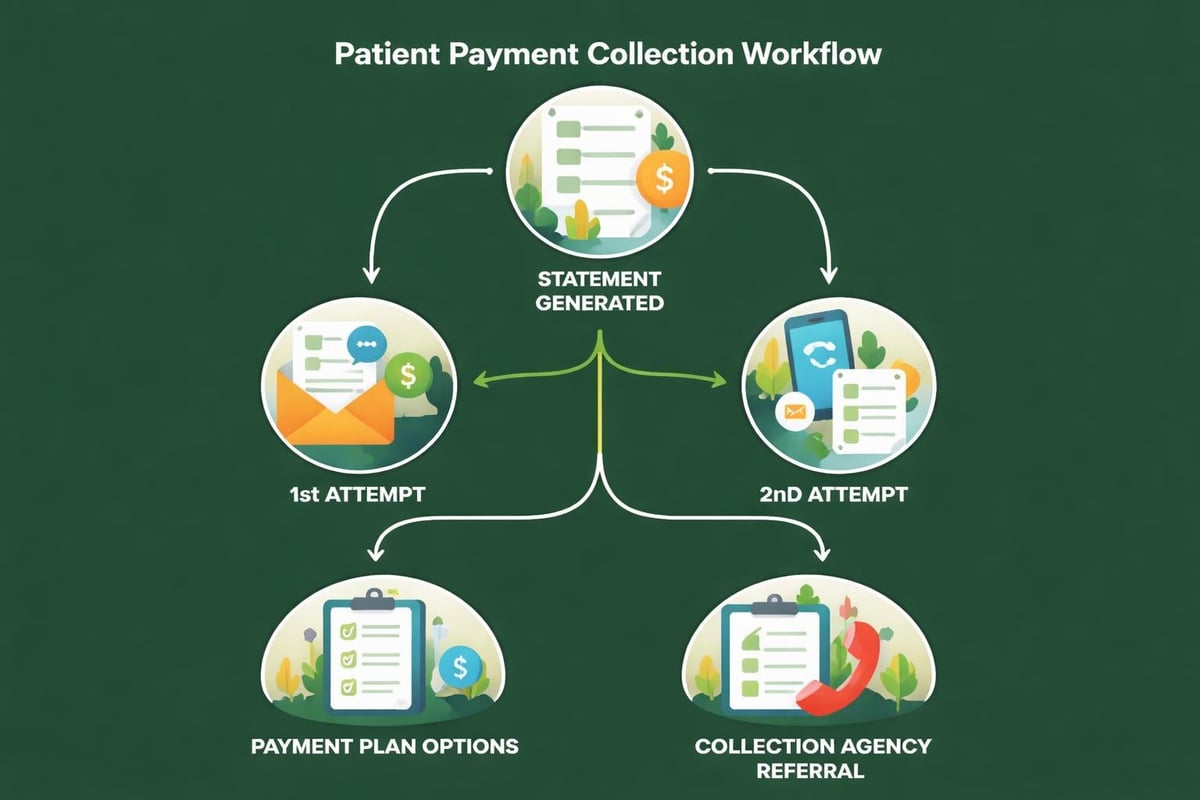
Step 11: Payment Collection and Follow-Up
The final stage of the rcm process involves collecting patient balances through various channels including online payments, phone payments, mail-in remittances, and in-person collections. Establishing clear collection policies and training staff in respectful collection communications maximizes recovery while maintaining patient relationships.
Progressive collection strategies typically involve multiple touchpoints at increasing intervals. Initial statements should be friendly reminders, while subsequent communications become more direct about payment expectations and consequences of non-payment.
Technology Integration in the RCM Process
Modern revenue cycle management relies heavily on integrated technology solutions. Practice management systems, electronic health records, billing software, and clearinghouse platforms must communicate seamlessly to support efficient workflows. The integration of AI and automation in RCM offers significant opportunities for improving efficiency and reducing errors.
Healthcare organizations evaluating medical billing software solutions should prioritize systems offering comprehensive functionality across all stages of the rcm process. Disconnected point solutions create data silos, duplicate data entry requirements, and increase error risks.
Essential Technology Features
Effective revenue cycle technology should support automated eligibility verification, real-time charge capture, intelligent claims scrubbing, electronic remittance processing, comprehensive reporting capabilities, and secure patient payment portals. These features reduce manual work, accelerate cash flow, and improve accuracy throughout the billing cycle.
Understanding Master Data Management principles helps organizations maintain data integrity across systems, ensuring consistent and accurate information flows through the entire rcm process.
Performance Measurement and Optimization
Successful revenue cycle management requires ongoing monitoring of key performance indicators that reveal process efficiency and financial health. The rcm process should be measured against industry benchmarks to identify improvement opportunities and track progress over time.
Critical RCM metrics include:
- Days in Accounts Receivable: Average time from service date to payment collection
- Clean Claim Rate: Percentage of claims paid upon initial submission
- Denial Rate: Percentage of claims denied by payers
- Collection Rate: Percentage of expected revenue actually collected
- Cost to Collect: Administrative expenses per dollar collected
| Metric | Industry Benchmark | Impact on Revenue |
|---|---|---|
| Days in A/R | 30-40 days | Slower cash flow beyond benchmark |
| Clean Claim Rate | 95% or higher | More staff time on rework |
| Denial Rate | Below 5% | Direct revenue loss and rework costs |
| Net Collection Rate | 95-99% | Revenue leakage from write-offs |
Regular analysis of these metrics reveals trends, highlights problem areas, and guides strategic decisions about process improvements, staff training needs, and technology investments. Organizations should establish monthly reporting routines that track metrics over time and compare performance across different providers, locations, or payer groups.
Compliance Considerations Throughout the RCM Process
Healthcare billing operates under extensive regulatory oversight requiring strict adherence to federal and state laws, payer policies, and ethical billing practices. The rcm process must incorporate compliance checkpoints at every stage to prevent fraud, abuse, and improper billing.
Key compliance areas include:
- HIPAA privacy and security requirements protecting patient information
- False Claims Act prohibitions against knowingly submitting incorrect claims
- Stark Law and Anti-Kickback Statute restrictions on financial relationships
- Coding accuracy requirements preventing upcoding and unbundling
- Timely filing obligations for claim submissions
Developing comprehensive compliance programs with regular training, internal audits, and clear policies protects organizations from legal exposure while ensuring ethical revenue cycle operations. Medical coding audit services provide objective assessment of coding accuracy and compliance adherence.
Common Challenges in the RCM Process
Healthcare providers face numerous obstacles in managing their revenue cycles effectively. Staffing shortages make it difficult to maintain experienced billing teams with specialized knowledge. Payer complexity creates confusion with varying requirements, fee schedules, and authorization rules across different insurance companies.
Regulatory changes require constant adaptation to new coding systems, billing rules, and compliance requirements. Technology limitations in legacy systems prevent automation and create inefficiencies. Patient collection challenges have intensified as out-of-pocket expenses have grown, making collection efforts more important yet more difficult.
Addressing these challenges requires strategic investments in people, processes, and technology. Many healthcare organizations partner with specialized revenue cycle management service providers to access expertise, technology, and economies of scale unavailable internally.
Best Practices for RCM Process Optimization
Healthcare organizations seeking to improve their revenue cycle performance should consider implementing several proven strategies. Front-end optimization through thorough patient access processes prevents downstream problems. Staff training ensures team members understand their roles in the larger revenue cycle and possess necessary skills.
Regular process audits identify inefficiencies, errors, and opportunities for improvement. Technology leverage through appropriate software and automation reduces manual work and accelerates workflows. Payer relationship management through regular communication and partnership approaches resolves issues more quickly.
Effective denial management services should be prioritized given the significant revenue at stake in denied claims. Organizations must develop systematic approaches to denial analysis, appeals, and prevention.
Strategic Considerations for Revenue Cycle Success
The rcm process continues to evolve as healthcare delivery models change, payment structures shift toward value-based arrangements, and technology advances create new capabilities. Forward-thinking healthcare organizations view revenue cycle management as a strategic function requiring executive attention and ongoing investment.
Successful practices align their revenue cycle operations with broader organizational goals, ensuring that billing processes support clinical excellence, patient satisfaction, and financial sustainability. This alignment requires regular communication between clinical leaders, financial managers, and operational staff.
Understanding the complete rcm process from patient registration through final payment collection enables healthcare providers to identify improvement opportunities, allocate resources effectively, and build sustainable financial operations. Organizations that master these fundamentals position themselves for success regardless of external pressures and market changes.
The complexity of modern healthcare billing demands specialized expertise, appropriate technology, and dedicated focus that many practices struggle to maintain internally. Comprehensive documentation throughout the RCM process outlined in industry guidance provides practical frameworks for implementation and optimization.
Mastering the rcm process requires attention to detail, appropriate technology, trained personnel, and systematic approaches across all stages from patient registration through final payment collection. Healthcare providers seeking to optimize their revenue cycles must invest in comprehensive solutions that address each component while maintaining compliance and supporting positive patient relationships. Greenhive Billing Solutions delivers specialized revenue cycle management services designed for healthcare providers who want to maximize collections, reduce administrative burden, and focus on patient care. Our experienced team handles everything from eligibility verification and claims processing to denial management and payment posting, ensuring your practice achieves optimal financial performance while maintaining HIPAA compliance and transparent communication throughout the billing cycle.