Healthcare providers face mounting pressure to optimize revenue while delivering exceptional patient care. One critical yet often underestimated component of financial health is eligibility verification in medical billing. This foundational process ensures that insurance coverage is confirmed before services are rendered, preventing costly claim denials and reducing administrative burden. When executed correctly, eligibility verification safeguards revenue streams, enhances patient satisfaction, and establishes a solid foundation for the entire revenue cycle. For practices seeking to minimize write-offs and accelerate reimbursements, mastering this essential function has never been more important.
Understanding the Core Purpose of Insurance Verification
Eligibility verification in medical billing serves as the gateway between patient care and proper reimbursement. This process involves confirming that a patient's insurance coverage is active, determining which services are covered under their specific plan, and identifying any limitations or requirements such as prior authorizations. Without this critical step, providers risk delivering services that may not be reimbursed, leading to unexpected patient balances and strained relationships.
The verification process extends beyond simply confirming active coverage. Staff must identify the patient's deductible status, copayment amounts, coinsurance percentages, and benefit limitations. Understanding why eligibility and verification are the main pillars of medical billing helps practices appreciate how this function directly impacts financial performance.
Financial Impact on Revenue Cycle Performance
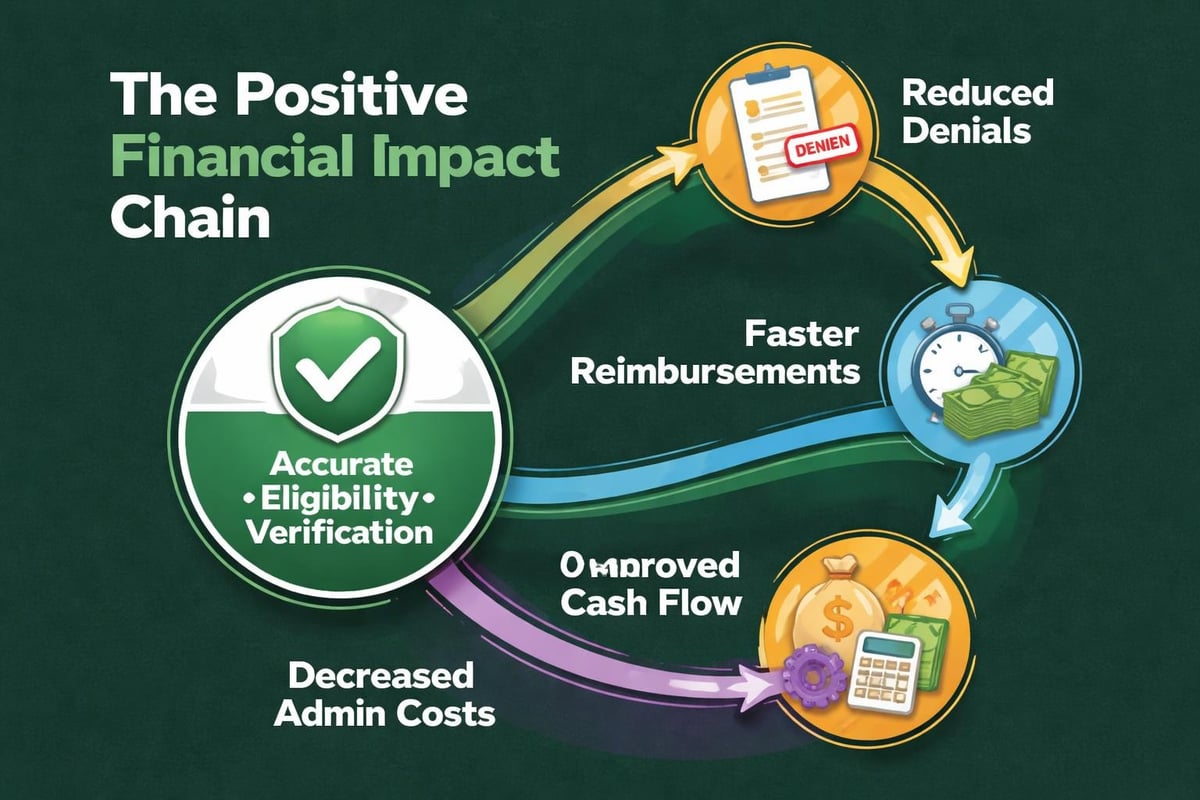
When eligibility verification in medical billing is performed accurately, practices experience measurable improvements across multiple financial metrics. Claim acceptance rates increase, denial rates decrease, and days in accounts receivable shrink. These outcomes directly correlate with improved cash flow and reduced administrative costs associated with reworking denied claims.
Key financial benefits include:
- Reduced claim denial rates by 20-30% on average
- Decreased time spent on appeals and resubmissions
- Improved patient payment collections through accurate cost estimates
- Lower write-off percentages from uncollectible balances
- Enhanced relationships with payers through accurate initial submissions
Practices that integrate robust denial management in medical billing strategies recognize that prevention begins with thorough verification protocols.
Essential Components of the Verification Process
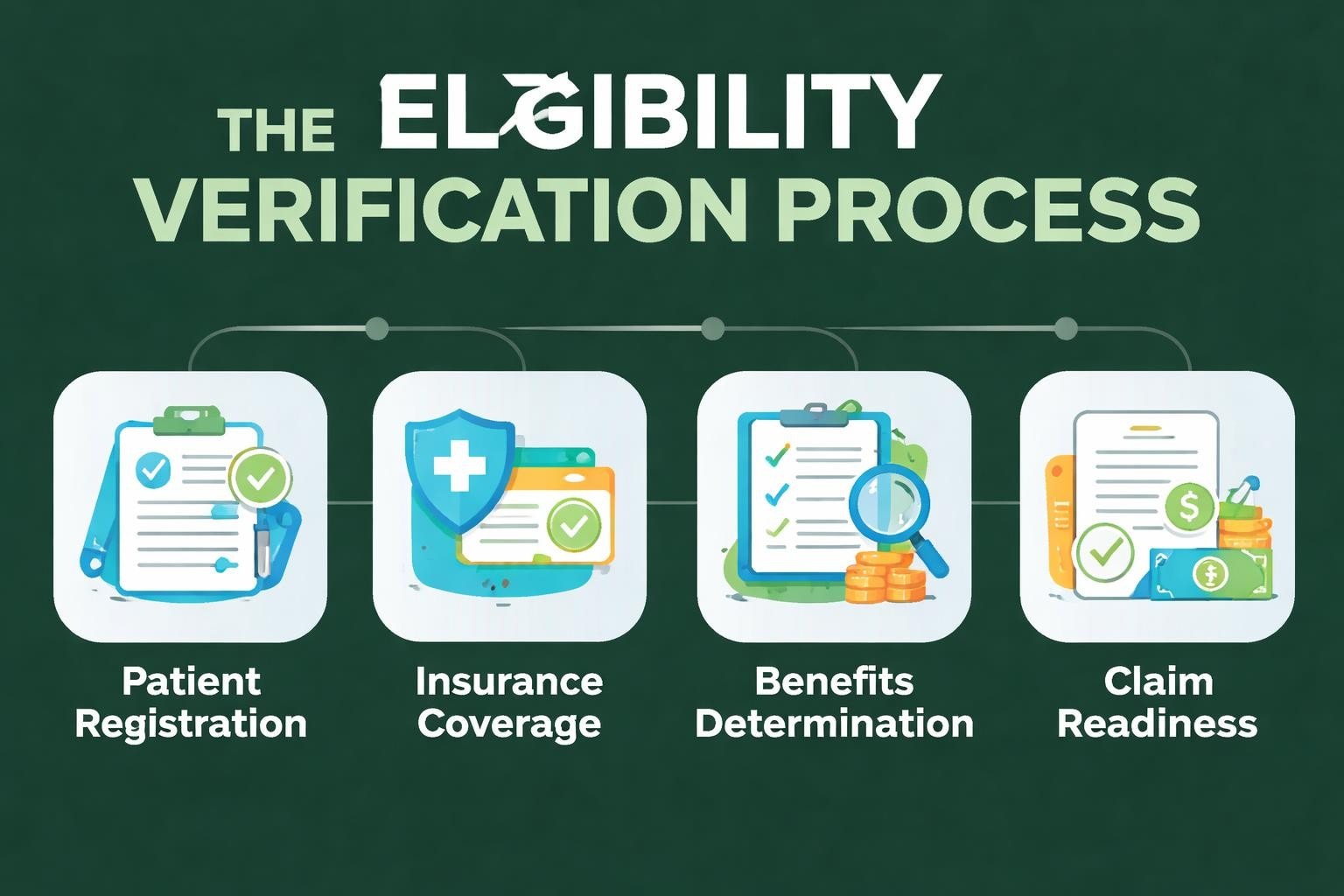
The eligibility verification process consists of several interconnected steps that must be completed systematically to ensure accuracy. Each component builds upon the previous one, creating a comprehensive understanding of the patient's coverage and benefits.
Step 1: Gathering Accurate Patient Information
The verification process begins at patient registration, where complete and accurate demographic and insurance information must be collected. This includes:
- Patient's full legal name as it appears on their insurance card
- Date of birth and social security number
- Current insurance carrier and policy number
- Subscriber information if the patient is a dependent
- Secondary insurance details if applicable
- Contact information for billing communications
Even minor discrepancies in this initial data collection can trigger claim rejections. Front desk staff must verify information directly from insurance cards and government-issued identification rather than relying solely on patient recall.
Step 2: Confirming Active Coverage Status
Once patient information is collected, the next critical step involves confirming that insurance coverage is active on the date of service. Coverage can be terminated for various reasons including non-payment of premiums, employment changes, or policy modifications. The eligibility verification process in medical billing must occur close to the appointment date to ensure accuracy.
Timing matters significantly. Verifying coverage too early may result in outdated information if the patient's status changes before their appointment. Conversely, verifying too late leaves insufficient time to address coverage issues or reschedule if necessary.
Step 3: Determining Covered Services and Benefits
Active coverage doesn't guarantee that specific services are covered under the patient's plan. This step requires investigating which procedures, treatments, and diagnostic tests are included in the patient's benefits package. Different plans have varying coverage levels for:
- Preventive care services
- Specialist consultations
- Diagnostic imaging and laboratory tests
- Surgical procedures
- Durable medical equipment
- Behavioral health services
Understanding these nuances helps practices set accurate patient expectations and avoid surprise bills that damage trust and complicate collections.
Common Verification Challenges and Solutions
Healthcare practices encounter numerous obstacles when performing eligibility verification in medical billing. Recognizing these challenges and implementing appropriate solutions strengthens the entire revenue cycle.
Technology Integration Issues
Many practices struggle with disconnected systems where patient scheduling software doesn't communicate effectively with verification platforms. This fragmentation creates redundant data entry, increases error rates, and consumes valuable staff time. Implementing integrated systems that automatically pull patient information and trigger verification workflows eliminates these inefficiencies.
| Challenge | Impact | Solution |
|---|---|---|
| Manual verification processes | High error rates, slow turnaround | Automated real-time verification systems |
| Outdated patient information | Claim denials, delayed payments | Regular database updates and verification |
| Incomplete benefit details | Unexpected patient balances | Comprehensive verification checklists |
| Staff training gaps | Inconsistent verification quality | Standardized protocols and ongoing education |
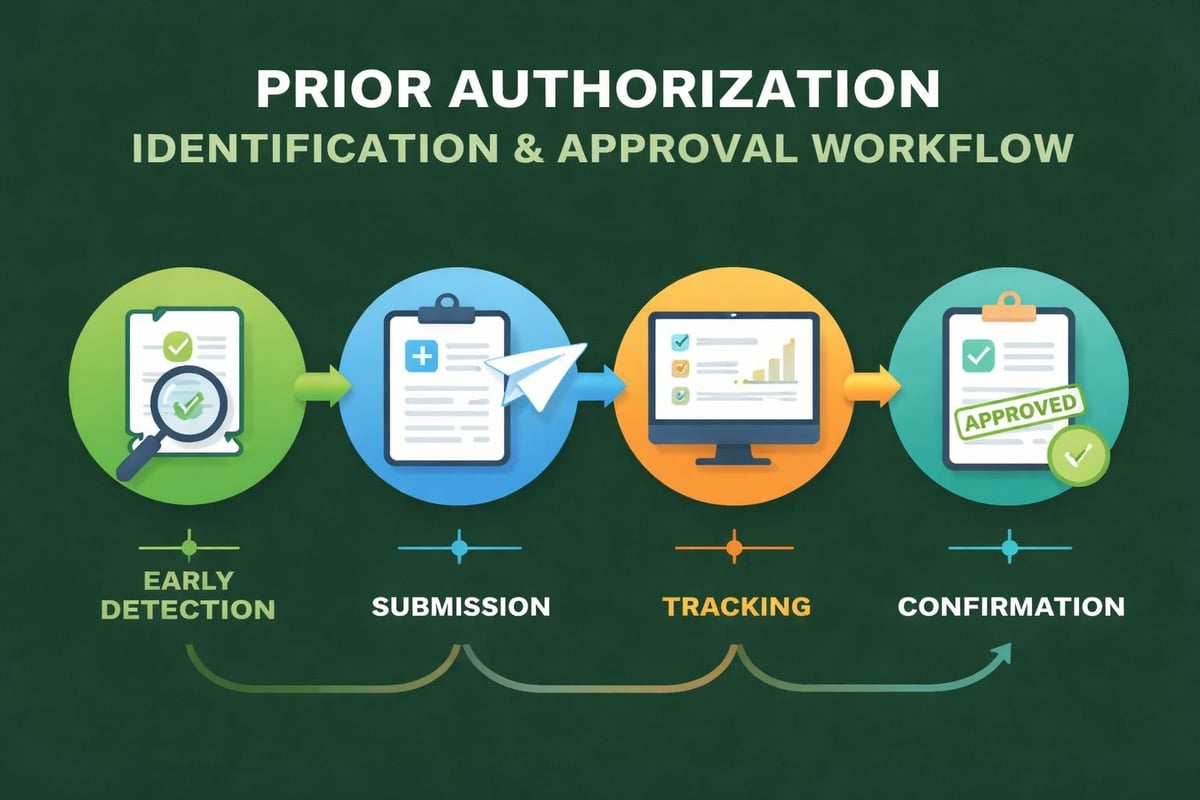
Managing Prior Authorization Requirements
Certain services require prior authorization from insurance carriers before being performed. Failure to obtain these approvals results in automatic claim denials, regardless of medical necessity. Effective verification processes identify prior authorization requirements early, allowing sufficient time to complete the approval process before scheduled appointments.
Staff should maintain updated lists of services commonly requiring authorization within each major payer contract. This proactive approach prevents last-minute cancellations and revenue disruptions.
Best Practices for Accurate Verification
Implementing standardized protocols for eligibility verification in medical billing transforms this function from a reactive task to a proactive revenue protection strategy. These best practices help practices achieve consistent, reliable results.
Establish Verification Timing Protocols
Different service types require different verification timelines. Establishing clear protocols ensures adequate time for addressing any coverage issues:
- Emergency services: Verify immediately upon patient stabilization
- Routine appointments: Verify 3-5 business days before scheduled service
- Scheduled procedures: Verify 7-10 business days in advance to allow for prior authorization
- Recurring services: Re-verify monthly or according to payer requirements
These timeframes provide sufficient buffer to resolve coverage problems, obtain necessary authorizations, or reschedule services if needed.
Document Everything Thoroughly
Comprehensive documentation protects practices during claim disputes and appeals. Staff should record:
- Date and time of verification
- Name of insurance representative spoken with
- Reference or confirmation numbers
- Specific benefits confirmed
- Any limitations or exclusions noted
- Prior authorization requirements and approval numbers
This documentation becomes critical evidence when payers dispute coverage or deny claims based on eligibility issues. Practices utilizing healthcare revenue cycle management strategies understand that thorough documentation supports successful appeals.
Implement Quality Assurance Measures
Regular audits of the verification process identify training opportunities, system gaps, and areas for improvement. Monthly reviews should examine:
- Verification completion rates
- Accuracy of information obtained
- Denials attributable to eligibility issues
- Time required to complete verifications
- Patient complaints related to billing surprises
These metrics reveal process weaknesses and guide targeted improvements that enhance overall revenue cycle performance.
The Role of Technology in Modern Verification
Technological advancement has revolutionized eligibility verification in medical billing, shifting from time-consuming phone calls to instantaneous electronic verification. Understanding available tools and their applications helps practices select appropriate solutions.
Real-Time Eligibility Verification Systems
Real-time verification platforms connect directly with payer databases, delivering instant confirmation of coverage and benefits. These systems dramatically reduce staff workload while improving accuracy by eliminating transcription errors and outdated information. The complete guide to insurance eligibility verification explores technological solutions that streamline this critical function.
Advantages of automated systems:
- Instant results available 24/7
- Reduced phone hold times and manual research
- Standardized data format across all payers
- Integration with practice management systems
- Audit trails documenting verification activities
Clearinghouse Integration
Many practices leverage clearinghouse services that consolidate verification functions across multiple payers. Rather than maintaining separate login credentials and processes for each insurance carrier, clearinghouses provide unified access through a single platform. This consolidation simplifies workflows and reduces the learning curve for staff members.
Addressing Common Verification Mistakes
Even experienced billing staff can fall victim to common errors that compromise verification effectiveness. Awareness of these pitfalls helps practices implement preventive measures. Learning from common mistakes in eligibility and benefits verification strengthens verification protocols.
Assuming Coverage Based on Previous Visits
Patient insurance status changes frequently due to employment transitions, policy modifications, or life events like marriage or divorce. Assuming that coverage remains unchanged from previous visits is a dangerous practice that leads to denied claims and unexpected patient balances. Every encounter requires fresh verification regardless of recent visit history.
Overlooking Secondary Insurance
Patients with multiple insurance policies require coordination of benefits to determine primary and secondary payer responsibility. Failing to identify and verify secondary coverage leaves money on the table and creates confusion about patient responsibility. Complete verification protocols must capture all active insurance policies.
Insufficient Detail on Benefit Limitations
Generic verification confirming "active coverage" provides inadequate protection against denials. Staff must drill deeper to understand specific benefit parameters including:
- Annual or lifetime maximums
- Visit limitations for certain service types
- Network restrictions and out-of-network penalties
- Waiting periods for specific procedures
- Benefit year reset dates
This detailed information enables accurate patient estimates and prevents unexpected denials after services are rendered. Practices focused on accurate eligibility and benefits verification understand how thoroughness reduces write-offs.
Training and Staff Development Considerations
The quality of eligibility verification in medical billing directly correlates with staff competency and training. Investing in comprehensive education programs yields measurable returns through improved accuracy and efficiency.
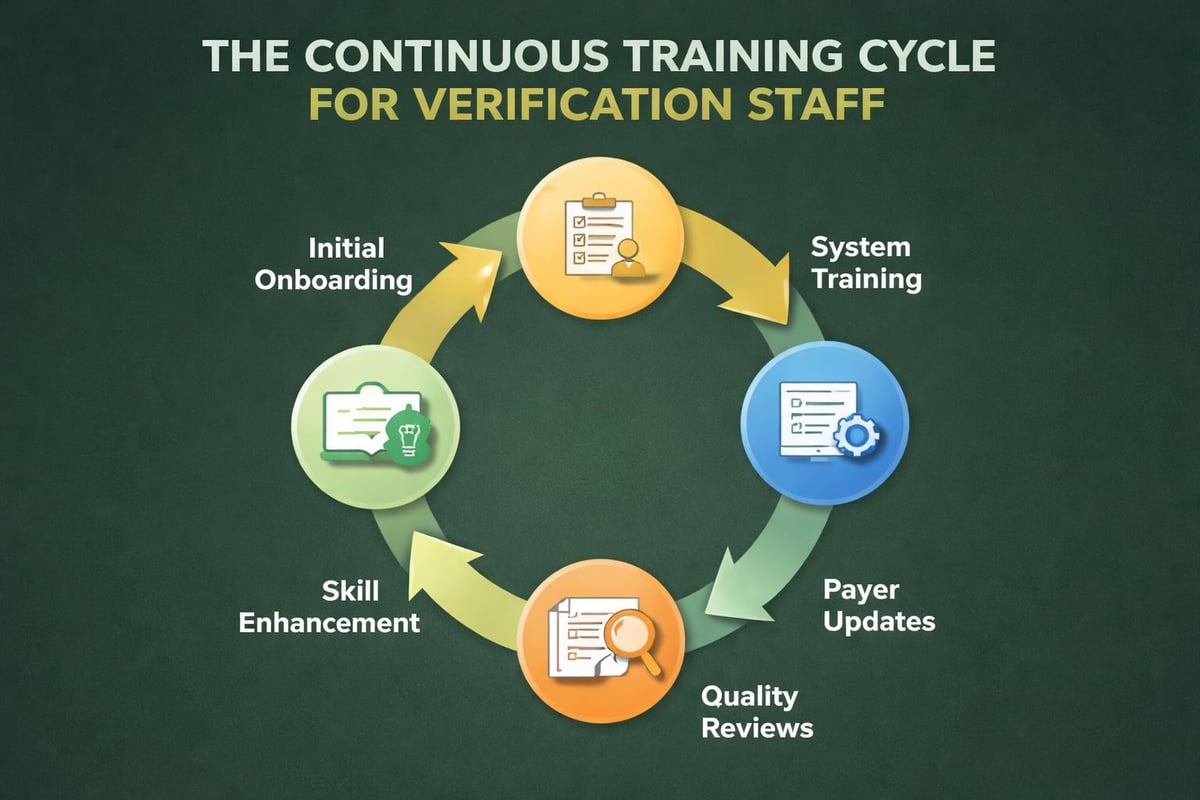
Initial Training Requirements
New staff members require structured onboarding that covers both technical skills and conceptual understanding. Effective training programs include:
- Insurance terminology and plan types
- Payer-specific verification requirements
- System navigation and data entry protocols
- Documentation standards and compliance requirements
- Communication skills for patient conversations about coverage
Role-playing exercises help staff practice difficult conversations about coverage limitations or high patient responsibility amounts.
Ongoing Education and Updates
The healthcare landscape evolves continuously, with payers modifying requirements, introducing new plan designs, and updating verification protocols. Regular training sessions keep staff current on these changes. Monthly team meetings should include updates on:
- New payer requirements or policy changes
- Recent denial trends and root causes
- Technology updates and system enhancements
- Best practice sharing among team members
- Regulatory changes affecting verification processes
Measuring Verification Effectiveness
Quantifying the performance of eligibility verification processes provides objective data for continuous improvement. Establishing key performance indicators helps practices monitor success and identify opportunities for enhancement.
Critical Metrics to Track
| Metric | Target Range | Significance |
|---|---|---|
| Verification completion rate | 98-100% | Ensures comprehensive coverage confirmation |
| Denial rate due to eligibility issues | Less than 2% | Indicates verification accuracy |
| Average verification time per patient | 3-5 minutes | Measures process efficiency |
| Prior authorization approval rate | 95-98% | Reflects thoroughness in identifying requirements |
| Patient complaint rate about billing surprises | Less than 1% | Shows effectiveness of patient communication |
These metrics should be reviewed monthly with trending analysis to identify patterns and guide process improvements.
Creating Accountability Systems
Assigning clear ownership for verification tasks ensures accountability and prevents missed verifications. Some practices designate specific team members for particular payer relationships, building expertise and efficiency. Others rotate responsibilities to maintain broad knowledge across the team. Regardless of approach, documented protocols and regular performance reviews maintain consistent quality standards.
Integration with Broader Revenue Cycle Functions
Eligibility verification in medical billing doesn't operate in isolation. Its effectiveness depends on seamless integration with other revenue cycle components. Understanding these connections optimizes overall financial performance.
Connection to Charge Entry and Coding
Accurate verification information informs proper charge entry and coding decisions. When staff understand coverage limitations and benefit structures, they can ensure that services are coded appropriately and billed to the correct payer. This connection between charge entry in medical billing and verification reduces coding-related denials.
Supporting Clean Claims Submission
The ultimate goal of eligibility verification is supporting clean claim submission that passes all payer edits on the first attempt. Complete and accurate verification data provides the foundation for claims that contain correct patient demographics, valid coverage information, appropriate authorization numbers, and accurate benefit coordination details.
When verification processes feed directly into claims submission workflows, practices experience dramatically higher first-pass acceptance rates and faster reimbursement cycles. This integration represents the seamless operation of an effective revenue cycle medical billing system.
Patient Communication and Transparency
Beyond the technical aspects of confirming coverage, eligibility verification in medical billing creates opportunities for meaningful patient engagement. Proactive communication about coverage and costs builds trust and improves collection rates.
Setting Accurate Financial Expectations
Armed with detailed verification information, front desk staff can provide patients with reliable estimates of their financial responsibility before services are rendered. This transparency allows patients to make informed decisions about their care and prepare financially for upcoming expenses.
Effective patient communication includes:
- Clear explanation of deductible status and remaining balance
- Copayment or coinsurance amounts for planned services
- Out-of-pocket maximums and current progress
- Available payment plans or financial assistance options
- Timeline for receiving statements after service
This upfront dialogue reduces billing complaints, improves collections, and strengthens patient relationships.
Handling Coverage Gaps Compassionately
When verification reveals coverage limitations or terminations, staff must communicate these findings with sensitivity and problem-solving focus. Rather than simply canceling appointments, effective teams explore alternatives such as payment plans, sliding fee scales, or assistance program referrals. This patient-centered approach balances financial responsibility with compassionate care.
Compliance and Regulatory Considerations
Eligibility verification processes must adhere to strict privacy and security regulations. Understanding compliance requirements protects practices from legal exposure and penalties.
HIPAA Privacy Standards
All verification activities involve protected health information and must comply with HIPAA privacy standards. Staff should verify patient identity before discussing coverage details, limit information sharing to the minimum necessary, and maintain secure documentation of all verification activities. Regular privacy training reinforces these critical protections.
State-Specific Requirements
Some states impose additional requirements on verification processes or patient notification about coverage limitations. Practices operating in multiple states must understand and comply with varying regulatory frameworks. Consulting with compliance experts ensures that protocols meet all applicable standards.
Vendor Selection for Verification Services
Practices unable to maintain robust in-house verification capabilities may partner with specialized service providers. Evaluating potential partners requires careful consideration of multiple factors.
Critical Evaluation Criteria
When assessing verification service vendors, practices should examine:
- Integration capabilities with existing practice management systems
- Payer network coverage and real-time connection reliability
- Turnaround time commitments and service level agreements
- Staff training and support provided
- Compliance certifications and security protocols
- Reporting capabilities and performance metrics
- Pricing structure and contract flexibility
Requesting references from similar-sized practices in comparable specialties provides valuable insights into vendor performance and reliability.
Effective eligibility verification in medical billing forms the cornerstone of healthy revenue cycle performance, preventing denials and ensuring practices receive appropriate reimbursement for services rendered. By implementing standardized protocols, leveraging technology, and maintaining rigorous staff training, healthcare providers can transform this essential function from administrative burden to strategic advantage. Greenhive Billing Solutions delivers comprehensive eligibility verification services as part of our integrated revenue cycle management offerings, helping practices across the United States maximize reimbursements while minimizing administrative complexity. Our experienced team works seamlessly with your existing systems to provide accurate, timely verification that protects your revenue and enhances patient satisfaction.