Healthcare practices face increasing complexity when managing their financial operations. From patient registration through final payment, every touchpoint in the revenue cycle requires precision, compliance expertise, and strategic oversight. Medical revenue services provide specialized support for these critical financial functions, enabling healthcare providers to focus on patient care while ensuring optimal reimbursement and operational efficiency. Understanding how these services work and the value they deliver helps practices make informed decisions about their revenue cycle management strategy.
Understanding Medical Revenue Services
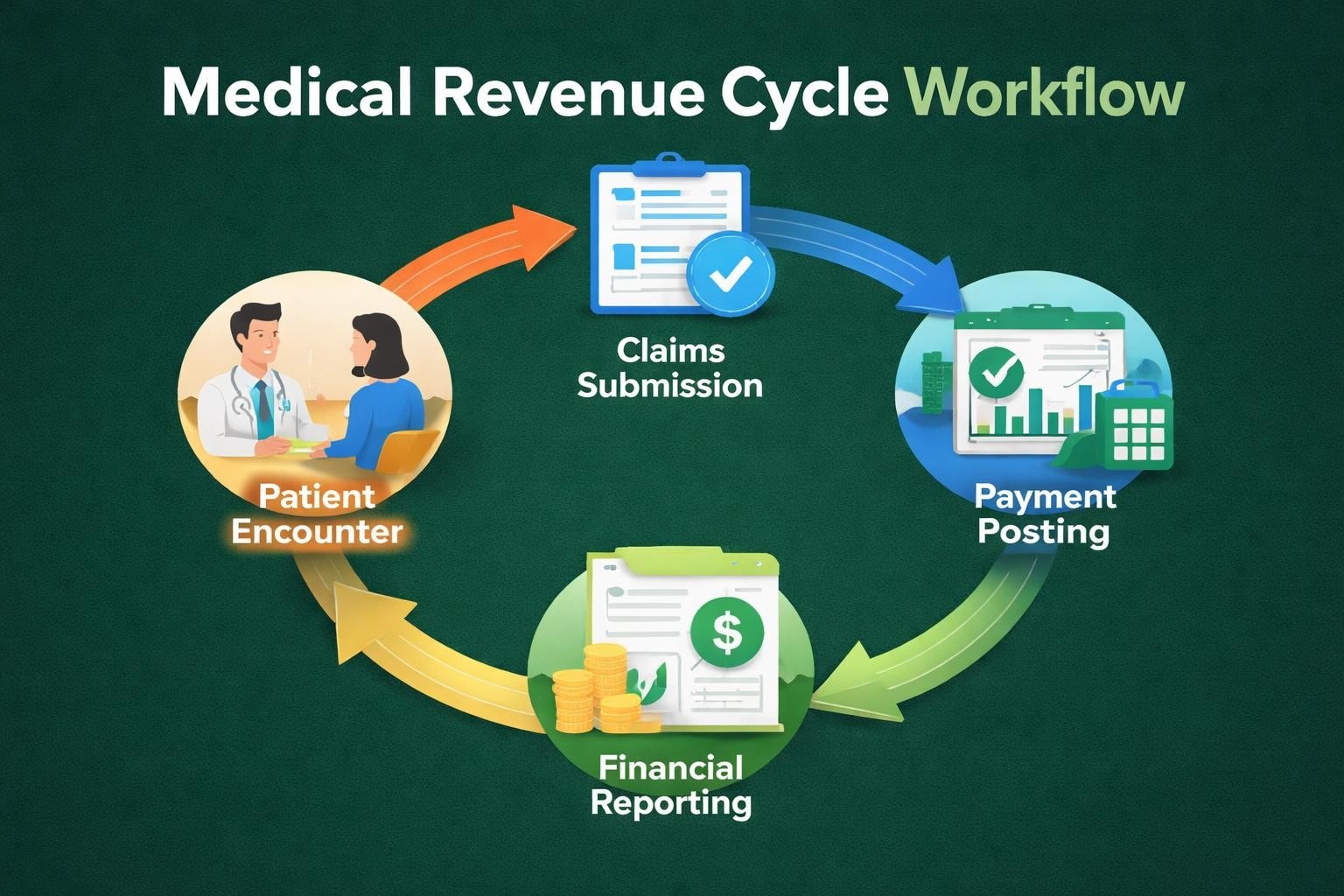
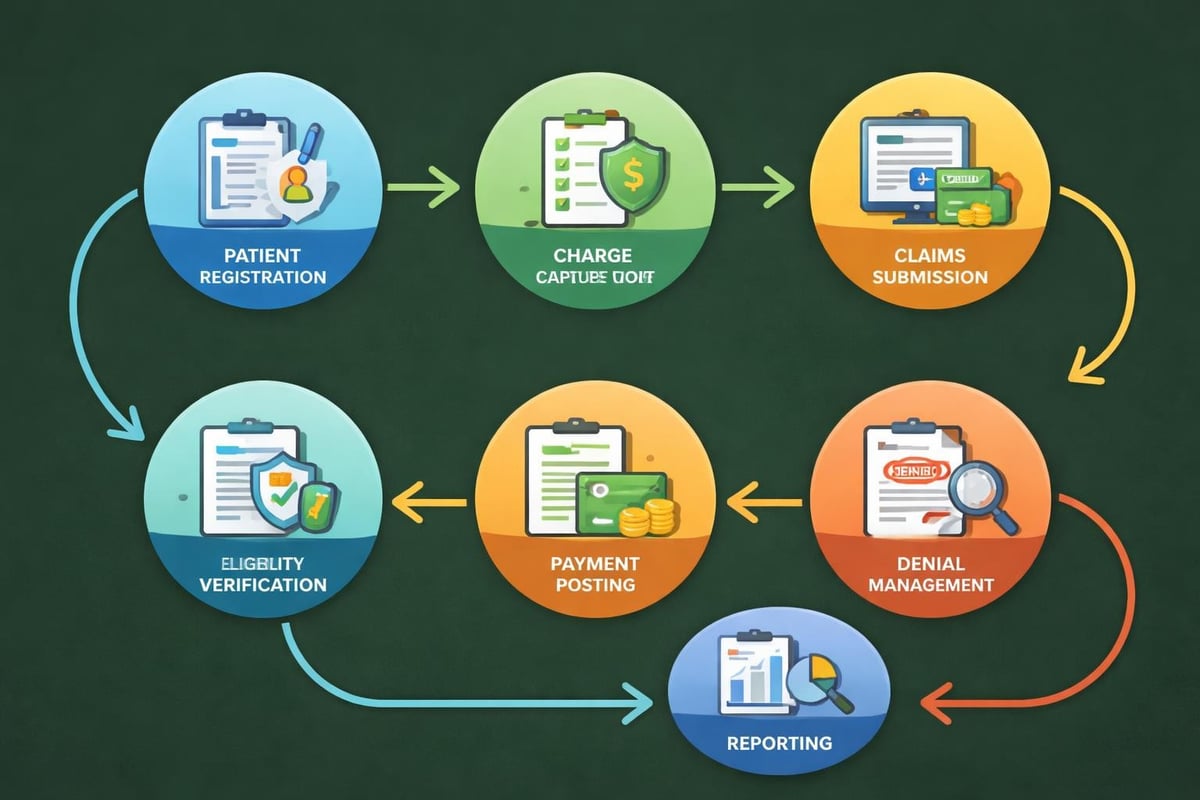
Medical revenue services encompass comprehensive management of the entire financial lifecycle for healthcare organizations. These services extend beyond basic billing to include patient eligibility verification, charge capture, claims submission, payment posting, denial management, and detailed financial reporting.
The primary objective of medical revenue services is maximizing revenue while minimizing administrative burden for healthcare providers. This involves navigating complex payer requirements, staying current with regulatory changes, and implementing best practices across all billing and collection activities.
Core Components of Revenue Service Solutions
Patient access and eligibility verification form the foundation of successful revenue capture. Before services are rendered, verification specialists confirm insurance coverage, identify patient responsibility, and obtain necessary authorizations. This proactive approach prevents claim denials and reduces billing surprises for patients.
Charge capture and coding ensure that all services provided are accurately documented and translated into billable claims. Professional coders apply current CPT, ICD-10, and HCPCS codes while adhering to payer-specific guidelines and CMS claims processing standards.
Medical revenue services also handle claims submission through electronic clearinghouses, monitoring for acceptance or rejection. When claims require correction, experienced specialists quickly identify issues and resubmit to minimize payment delays.
Benefits of Professional Revenue Service Support
Healthcare organizations partnering with specialized revenue service providers experience measurable improvements across multiple financial and operational metrics. These benefits directly impact practice profitability and sustainability.
| Benefit Category | Impact on Practice | Measurable Outcome |
|---|---|---|
| Cash Flow | Faster claim processing | 30-40% reduction in days in A/R |
| Collection Rate | Improved first-pass acceptance | 95%+ clean claim rate |
| Denial Rate | Proactive prevention | 50-70% fewer denials |
| Administrative Cost | Reduced overhead | Lower cost-to-collect ratio |
Enhanced Revenue Capture
Professional medical revenue services identify and capture revenue that might otherwise be lost due to coding errors, missed charges, or inadequate documentation. Experienced specialists review encounter data to ensure complete and accurate billing for all services rendered.
Compliance expertise reduces the risk of audits and penalties. Revenue service professionals stay current with changing regulations, payer policies, and coding updates, protecting practices from costly compliance violations.
Transparent reporting provides visibility into financial performance. Detailed analytics help practice administrators understand revenue trends, identify opportunities for improvement, and make data-driven decisions about their operations.
Key Processes Within Medical Revenue Services
Effective revenue management requires coordination across numerous interconnected processes. Each step must be executed correctly to ensure optimal financial outcomes.
Insurance Verification and Authorization
Before patient appointments, eligibility verification services confirm active coverage and benefits. This step identifies:
- Current insurance status and policy details
- Patient copay, deductible, and coinsurance amounts
- Coverage limitations or exclusions
- Prior authorization requirements for planned procedures
When authorization is required, specialists submit requests with complete clinical documentation, follow up on pending requests, and ensure approval before services are delivered.
Claims Submission and Management
Following patient encounters, medical claim submission services prepare and transmit claims electronically to insurance payers. This process involves:
- Charge review: Verifying that all services are captured with appropriate codes
- Claim scrubbing: Checking claims against payer-specific edits before submission
- Electronic transmission: Sending claims through secure clearinghouses
- Acknowledgment monitoring: Tracking acceptance or rejection status
- Correction and resubmission: Addressing rejected claims within 24-48 hours
Professional claim submission reduces errors and accelerates payment cycles, improving overall cash flow for healthcare practices.

Denial Management as a Critical Revenue Service
Claim denials represent one of the most significant challenges in healthcare revenue management. Medical revenue services include specialized denial management in medical billing to recover lost revenue and prevent future denials.
Common Denial Categories
Understanding denial patterns helps practices address systemic issues. The most frequent denial reasons include:
- Registration and eligibility errors: Incorrect patient demographic information or inactive insurance coverage
- Authorization issues: Missing or expired prior authorizations for procedures
- Coding problems: Incorrect, outdated, or unsupported procedure and diagnosis codes
- Timely filing: Claims submitted beyond payer-specific deadlines
- Medical necessity: Insufficient documentation to support the services billed
Strategic Denial Resolution
Effective denial management combines immediate resolution with long-term prevention strategies. When denials occur, revenue service specialists:
- Analyze denial reasons using remittance advice codes
- Determine appealability based on payer policies and claim details
- Gather supporting documentation including medical records and clinical notes
- Prepare and submit appeals within required timeframes
- Track appeal outcomes to measure success rates
Pattern analysis identifies recurring denial reasons, enabling process improvements that prevent similar denials in future claims. This proactive approach delivered through denial management services significantly improves overall collection rates.
Technology Integration in Medical Revenue Services
Modern revenue cycle management relies on sophisticated technology platforms to enhance efficiency and accuracy. Professional service providers leverage industry-standard software and systems to deliver optimal results.
Electronic Health Record Integration
Medical revenue services integrate seamlessly with existing practice management and EHR systems. This connectivity ensures:
- Real-time data access for billing specialists without duplicate entry
- Automated charge capture from clinical documentation
- Coordinated workflow between clinical and financial operations
- Comprehensive audit trails for compliance and quality assurance
Service providers adapt to the technology infrastructure already in place at healthcare organizations, working within client-owned systems and platforms. This flexibility eliminates the need for practices to change their existing software while still accessing expert revenue cycle support.
Advanced Analytics and Reporting
Sophisticated reporting and analytics capabilities transform raw billing data into actionable insights. Key performance indicators tracked through medical revenue services include:
| Metric | Purpose | Target Benchmark |
|---|---|---|
| Days in A/R | Measures collection speed | Under 35 days |
| Clean Claim Rate | First-pass acceptance | Above 95% |
| Net Collection Rate | Percentage of collectible revenue captured | 95-98% |
| Denial Rate | Claims requiring rework | Below 5% |
| Cost to Collect | Revenue cycle operational efficiency | 3-5% of collections |
Regular reporting keeps practice administrators informed about financial performance and highlights areas requiring attention.
Payment Posting and Reconciliation
Accurate payment posting services ensure that all payments from insurers and patients are correctly applied to patient accounts. This critical function within medical revenue services includes:
Insurance payment processing involves reviewing electronic remittance advice (ERA) and explanation of benefits (EOB) documents, posting payments to corresponding claims, recording contractual adjustments and write-offs, and identifying underpayments or overpayments.
Patient payment management tracks copays, deductibles, and coinsurance collected at time of service, posts payments received through mail or online portals, reconciles patient balances with insurance payments, and generates patient statements for outstanding balances.
Bank Reconciliation and Financial Accuracy
Daily reconciliation ensures that all posted payments match actual bank deposits. This verification process catches discrepancies early, maintains accurate financial records, supports practice accounting functions, and provides confidence in reported revenue figures.
Specialized Services for Different Practice Types
Medical revenue services adapt to the unique requirements of various healthcare specialties. Different practice types face distinct billing challenges that require specialized expertise.
Primary Care and Multi-Specialty Practices
Primary care providers handle high patient volumes with diverse payer mixes. Revenue services for these practices emphasize efficient patient flow, preventive care billing optimization, chronic care management coding, and value-based care program support.
Specialty Practice Requirements
Specialty practices require revenue service providers with deep knowledge of specialty-specific coding, common procedures and diagnosis patterns, and payer policies affecting their field. Whether supporting cardiology practices or surgical centers, specialized medical revenue services ensure accurate billing for complex procedures and appropriate modifier usage.
Small practices benefit particularly from outsourced revenue services because they gain access to professional expertise without maintaining full in-house billing departments. Solutions for medical billing services for small practices provide scalable support that grows with the practice.
Compliance and Security in Revenue Services
Healthcare financial operations must adhere to strict regulatory requirements. Professional medical revenue services maintain rigorous compliance standards across all activities.
HIPAA Compliance and Data Security
All revenue service operations must protect patient health information according to HIPAA privacy and security rules. This includes:
- Encrypted data transmission and storage
- Strict access controls and user authentication
- Regular security training for all personnel
- Business associate agreements with all service providers
- Comprehensive audit logging and monitoring
Regulatory Adherence
Beyond HIPAA, medical revenue services ensure compliance with numerous other regulations including Medicare and Medicaid billing rules, state-specific insurance requirements, anti-kickback and Stark Law provisions, and proper documentation standards.
Staying current with regulatory changes protects practices from audits, recoupments, and penalties while ensuring ethical billing practices across all payer types.
Credentialing and Provider Enrollment Support
Before revenue can be collected, healthcare providers must be properly credentialed with insurance payers. Medical credentialing services facilitate this complex process by managing initial applications, maintaining credential files, tracking expiration dates, and processing re-credentialing requirements.
Comprehensive medical revenue services include credentialing support to ensure providers remain in-network with all relevant payers, maximizing patient access and reimbursement rates.
Selecting the Right Revenue Service Partner
Healthcare organizations evaluating medical revenue services should consider several critical factors when choosing a partner. The right provider delivers measurable results while aligning with practice values and operational needs.
Evaluation Criteria
Experience and expertise in your specific practice type ensures the service provider understands your unique challenges. Review their track record with similar practices, specialty-specific knowledge, and client retention rates.
Technology capabilities determine operational efficiency. Assess their system integration abilities, reporting functionality, and adoption of industry best practices for electronic processing.
Transparency and communication build trust and enable collaboration. Quality providers offer regular performance reporting, accessible account management, and clear explanation of their processes and pricing.
Compliance commitment protects your practice. Verify their HIPAA compliance measures, staff training programs, and history of regulatory adherence.
Partnership Approach
The most effective medical revenue services operate as true partners rather than vendors. This partnership model includes collaborative problem-solving, proactive communication about issues and opportunities, investment in understanding your practice culture, and alignment with your long-term financial goals.
Organizations like those featured among top medical billing companies demonstrate these partnership qualities through consistent performance and client satisfaction.
Financial Impact and Return on Investment
Healthcare practices investing in professional medical revenue services typically see substantial financial returns that justify the partnership cost. The investment delivers value through multiple channels.
Revenue Increase Opportunities
Expert revenue management commonly increases practice revenue by 10-20% through improved clean claim rates, reduced denial write-offs, enhanced charge capture, accelerated cash flow, and decreased days in accounts receivable.
Cost Reduction Benefits
Beyond revenue increases, medical revenue services reduce operational costs by eliminating overhead for in-house billing staff, decreasing technology and training expenses, minimizing compliance risks and associated costs, and reducing administrative burden on clinical staff.
The combined effect of increased revenue and decreased costs delivers measurable ROI, often within the first few months of partnership. Practices gain financial stability while freeing resources to invest in patient care improvements and practice growth.
Regional Service Delivery Considerations
Medical revenue services adapt to regional variations in payer requirements, state regulations, and market dynamics. Providers serving practices across different states maintain expertise in location-specific billing requirements.
For example, practices in different regions benefit from specialized knowledge of local payer networks, whether they need medical billing services in California, medical billing services in Texas, or support in specific metropolitan areas. This geographic expertise ensures compliance with state-specific regulations while optimizing reimbursement based on regional payer contracts.
Future Trends in Medical Revenue Services
The healthcare revenue cycle continues evolving with technological advancement and regulatory change. Forward-thinking medical revenue services adapt to emerging trends that shape the industry.
Artificial intelligence and automation increasingly support routine tasks like eligibility verification, payment posting, and denial prediction. These technologies enhance efficiency while allowing human specialists to focus on complex problem-solving and strategic planning.
Value-based care models shift reimbursement from volume to outcomes, requiring revenue services to support quality reporting, risk adjustment coding, and alternative payment model administration.
Patient financial responsibility continues growing as high-deductible health plans become more common. Modern medical revenue services include enhanced patient communication, flexible payment options, and improved price transparency to support collection of patient balances.
Interoperability standards improve data exchange between systems, enabling more seamless integration of revenue cycle processes with clinical workflows and payer platforms.
Medical revenue services provide essential support for healthcare practices navigating the complex financial landscape of modern medicine. By partnering with experienced specialists, providers improve their revenue capture, reduce administrative burden, and gain confidence in their financial operations. Greenhive Billing Solutions delivers comprehensive revenue cycle management tailored to healthcare providers across the United States, combining expert staff, industry-standard technology, and a commitment to transparent partnership that drives measurable financial results for practices of all sizes.