Medical claims billing represents the financial backbone of healthcare delivery, connecting the services rendered by providers with the reimbursements received from payers. This complex process requires precision, compliance expertise, and a thorough understanding of regulatory requirements to ensure healthcare organizations maintain healthy cash flow. As healthcare providers face increasing pressure to optimize revenue while managing administrative costs, understanding the intricacies of medical claims billing becomes essential for sustainable practice operations.
Understanding the Medical Claims Billing Process
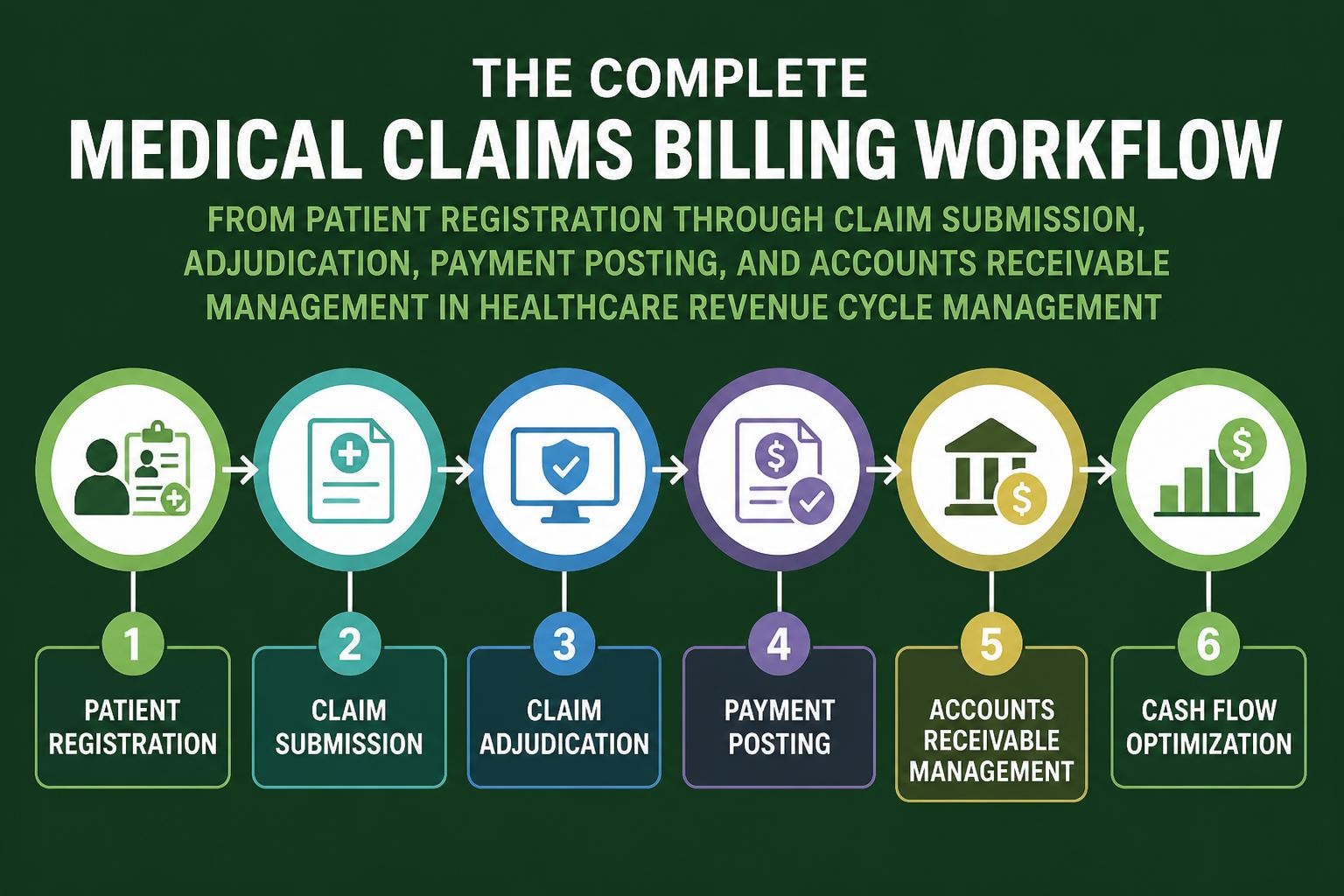
Medical claims billing encompasses the entire journey of transforming healthcare services into submitted claims and ultimately receiving payment from insurance companies or patients. This systematic approach begins the moment a patient schedules an appointment and continues through final payment reconciliation.
The foundation of successful medical claims billing starts with accurate patient registration and insurance verification. Before any service is rendered, administrative staff must collect comprehensive demographic information, confirm insurance coverage, and verify eligibility for specific procedures. This proactive step prevents claim denials and reduces the administrative burden of retroactive corrections.
Patient Registration and Eligibility Verification
Capturing accurate patient information during registration sets the stage for successful claims processing. Verification specialists confirm active insurance coverage, check benefit limits, and identify any pre-authorization requirements specific to planned procedures. This critical step significantly reduces downstream complications that could delay or prevent reimbursement.
Key elements of thorough patient registration include:
- Complete demographic details including current address and contact information
- Primary and secondary insurance policy information
- Verification of benefits and coverage limitations
- Identification of co-payment, deductible, and coinsurance responsibilities
- Documentation of authorization requirements for scheduled services
Documentation and Medical Coding Accuracy
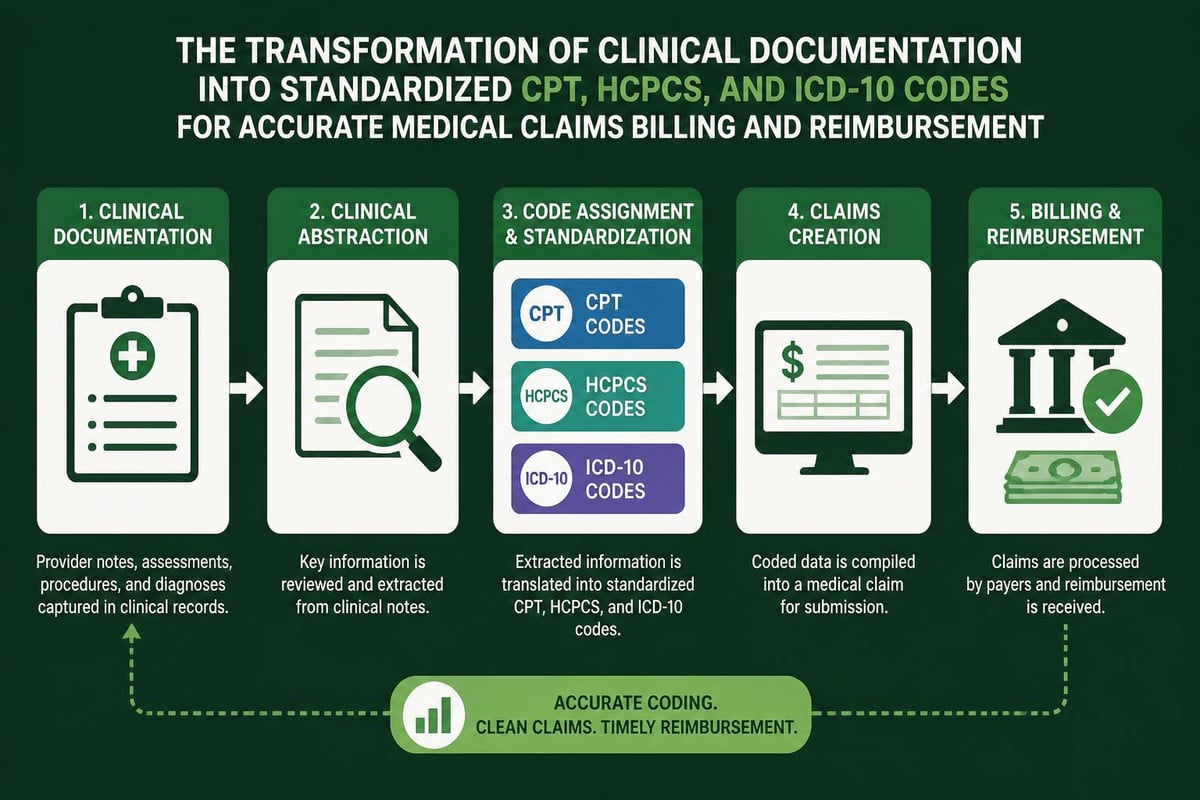
Once services are provided, clinical documentation becomes the foundation for medical claims billing. Providers must thoroughly document all services rendered, diagnoses established, and treatments administered during each patient encounter. This documentation then undergoes translation into standardized medical codes that payers recognize and process.
Professional medical coders review clinical documentation to assign appropriate CPT (Current Procedural Terminology), HCPCS (Healthcare Common Procedure Coding System), and ICD-10 (International Classification of Diseases) codes. The accuracy of this coding directly impacts reimbursement levels and claim acceptance rates. Understanding different types of medical coding helps practices ensure they receive appropriate compensation for services rendered.
The Role of Charge Capture
Charge capture represents the process of recording all billable services and procedures performed during patient care. Comprehensive charge capture ensures that practices bill for every service provided, maximizing legitimate revenue opportunities. Proper charge entry in medical billing prevents revenue leakage and supports accurate financial reporting.
Common charge capture challenges include:
- Missing charges for ancillary services or supplies
- Delayed entry of charges leading to timely filing issues
- Inconsistent documentation between providers
- Lack of integration between clinical and billing systems
Claims Submission and Electronic Processing
After coding completion, claims move into the submission phase where they transmit to insurance payers for adjudication. Modern medical claims billing relies heavily on electronic submission through clearinghouses that validate claim data before forwarding to payers. This electronic approach dramatically reduces processing time compared to traditional paper claims.
The medical billing process involves multiple checkpoints where claims undergo scrutiny for accuracy and compliance. Clearinghouses perform initial scrubbing to identify common errors such as invalid codes, missing information, or formatting issues. This preliminary review allows practices to correct problems before payers reject claims.
Clean Claims and First-Pass Resolution
A clean claim in medical billing contains complete and accurate information that allows payers to process it without requesting additional documentation. Achieving high clean claim rates significantly accelerates reimbursement timelines and reduces administrative costs associated with rework.
Industry benchmarks suggest successful practices achieve clean claim rates exceeding 95%. Reaching this threshold requires:
- Robust front-end verification processes
- Comprehensive coder training and education
- Regular auditing of submitted claims
- Effective use of billing software edit checks
- Continuous monitoring of payer-specific requirements
| Metric | Industry Average | Best-in-Class |
|---|---|---|
| Clean Claim Rate | 85-90% | 95%+ |
| Days in AR | 45-50 days | 30-35 days |
| Collection Rate | 95-96% | 98%+ |
| Denial Rate | 8-10% | <5% |
Adjudication and Payment Posting
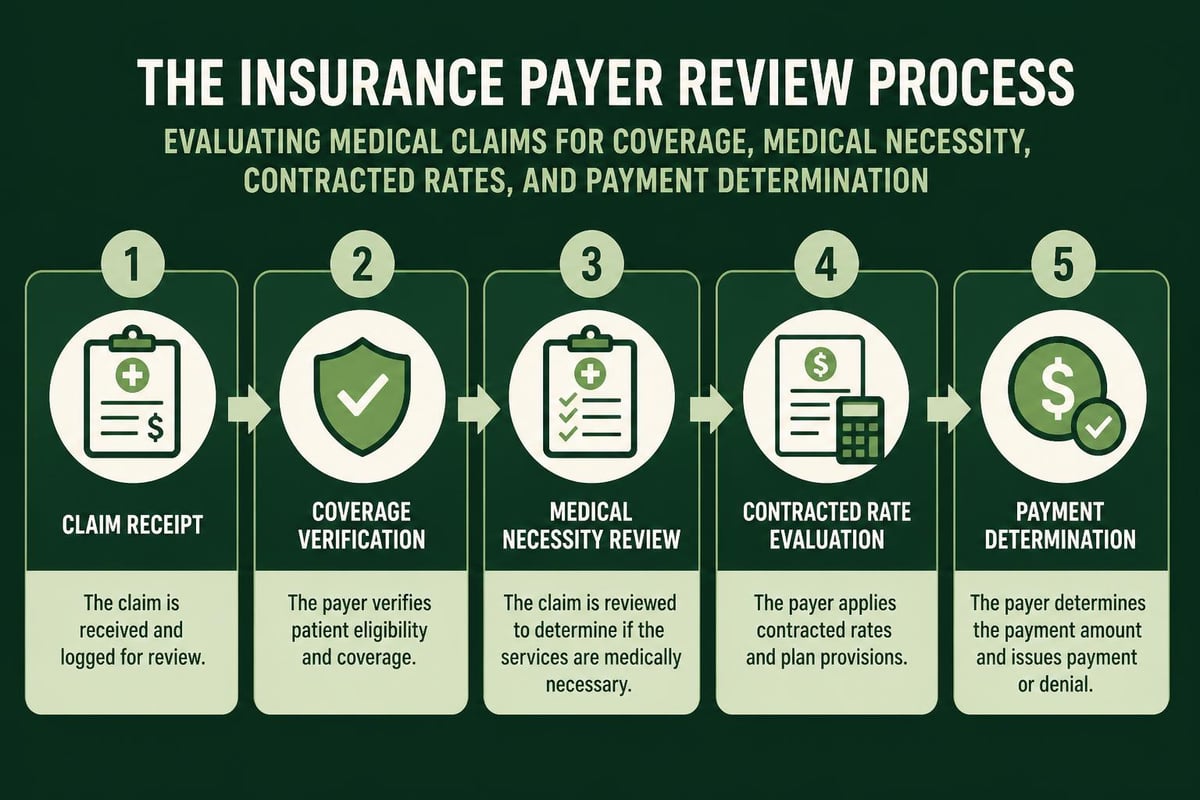
Once payers receive claims, they enter the adjudication phase where insurance companies review claims for medical necessity, coverage compliance, and pricing accuracy. Payers apply contracted fee schedules, check for coordination of benefits with other insurance, and determine the allowed amount for each service.
The adjudication process generates Electronic Remittance Advice (ERA) or Explanation of Benefits (EOB) documents detailing payment decisions. Understanding ERA in medical billing helps billing staff quickly identify which claims paid in full, which received partial payment, and which were denied.
Payment posting translates remittance information into the practice management system, crediting patient accounts and identifying remaining balances. Accurate payment posting enables effective accounts receivable management and ensures proper patient billing for their financial responsibility.
Managing Denials and Appeals
Despite careful preparation, some claims receive denials requiring additional work to secure payment. Denial management in medical billing represents a specialized function focused on understanding denial reasons, correcting claims, and appealing improper denials.
Common denial categories include:
- Technical denials resulting from coding errors or missing information
- Coverage denials when services fall outside policy benefits
- Medical necessity denials questioning the appropriateness of care
- Coordination of benefits denials requiring other insurance information
- Timely filing denials for claims submitted beyond payer deadlines
Successful practices establish systematic denial management workflows that categorize denials, assign responsibility for resolution, track appeal status, and analyze denial patterns to prevent recurrence.
Accounts Receivable Management
Medical claims billing extends beyond initial claim submission to include comprehensive accounts receivable follow-up. Managing AR in medical billing requires persistent monitoring of outstanding claims, proactive payer communication, and strategic escalation of delayed payments.
Effective AR management segments receivables by age, payer type, and claim status to prioritize collection efforts. Claims aging beyond 30 days require investigation to determine whether payers need additional information, claims were lost in processing, or denials require appeals.
Patient Collections and Billing
As high-deductible health plans increase patient financial responsibility, collecting patient balances becomes increasingly important for practice viability. Medical claims billing systems must accurately calculate patient portions after insurance adjudication and communicate balances clearly to patients.
Best practices for patient collections include:
- Collecting estimated patient responsibility at time of service
- Sending clear, itemized billing statements promptly
- Offering multiple payment methods including online portals
- Establishing payment plans for larger balances
- Maintaining compassionate communication about financial obligations
Compliance and Regulatory Requirements
Medical claims billing operates within a complex regulatory environment requiring strict adherence to federal and state regulations. HIPAA (Health Insurance Portability and Accountability Act) establishes privacy and security standards for protected health information used throughout the billing process.
Beyond HIPAA, practices must comply with payer-specific billing requirements, Medicare and Medicaid regulations, and fraud and abuse laws. The False Claims Act imposes severe penalties for knowingly submitting inaccurate claims, making compliance programs essential components of medical claims billing operations.
Understanding the RCM process helps practices establish comprehensive compliance frameworks that protect against regulatory violations while optimizing revenue capture. Regular compliance audits identify potential vulnerabilities before they result in penalties or payment recoupments.
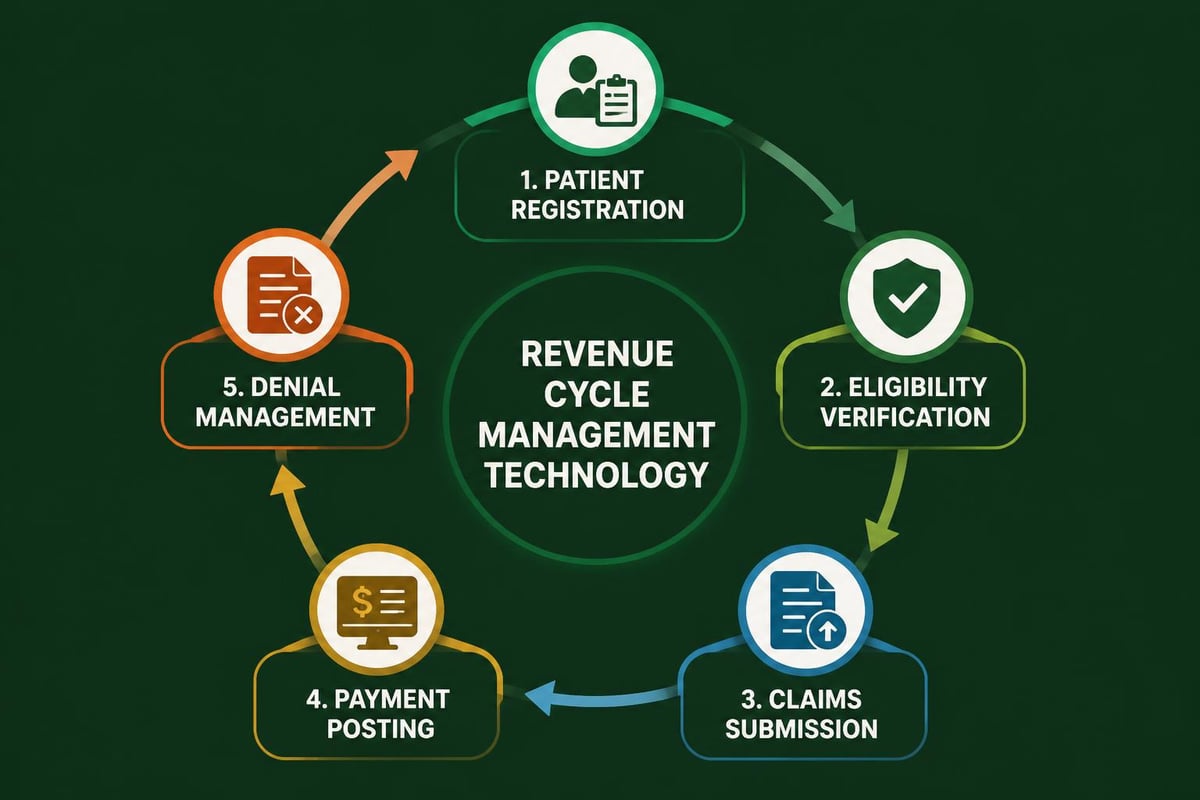
Technology and Automation in Modern Billing
Contemporary medical claims billing leverages sophisticated technology to streamline workflows and reduce manual intervention. Practice management systems integrate patient registration, scheduling, clinical documentation, coding, and billing into unified platforms that eliminate duplicate data entry and reduce errors.
Artificial intelligence and machine learning increasingly support medical claims billing by identifying coding opportunities, predicting denial likelihood, and automating routine tasks. These technologies allow billing professionals to focus expertise on complex cases requiring human judgment rather than repetitive administrative work.
| Technology | Benefit | Implementation Consideration |
|---|---|---|
| Electronic Claims Submission | Faster processing, reduced errors | Clearinghouse integration |
| Automated Eligibility Verification | Real-time coverage confirmation | API connectivity with payers |
| Claims Scrubbing Software | Error detection before submission | Regular rule updates |
| ERA Processing | Automated payment posting | Bank reconciliation workflows |
| Denial Management Platforms | Pattern identification | Staff training requirements |
Best Practices for Optimizing Revenue Cycle Performance
High-performing practices adopt structured approaches to medical claims billing that emphasize prevention over correction. Medical billing best practices focus on establishing workflows that minimize errors, accelerate cash flow, and maximize legitimate reimbursement.
Staff education and training represent foundational investments in billing excellence. Regular training keeps team members current on coding updates, payer policy changes, and regulatory requirements. Cross-training ensures workflow continuity when team members are unavailable.
Performance monitoring through key performance indicators enables data-driven decision-making. Tracking metrics such as clean claim rates, days in accounts receivable, collection percentages, and denial rates identifies improvement opportunities and measures intervention effectiveness.
Payer Relationship Management
Maintaining positive working relationships with insurance payers facilitates faster claims resolution and smoother appeals processing. Understanding payer-specific requirements, preferred communication channels, and escalation processes helps billing staff navigate complex payer organizations effectively.
Strategic payer management includes:
- Maintaining updated payer policy manuals and fee schedules
- Establishing direct contacts for claim inquiries
- Participating in payer education sessions and webinars
- Documenting payer-specific billing requirements
- Negotiating favorable contract terms during renewals
The Strategic Value of Outsourced Medical Claims Billing
Many healthcare providers partner with specialized revenue cycle management companies to handle medical claims billing functions. This strategic decision allows clinical teams to focus on patient care while billing experts manage the administrative complexities of revenue cycle operations.
Top medical billing companies bring specialized expertise, dedicated technology investments, and economies of scale that individual practices struggle to achieve independently. Outsourced billing typically delivers faster claims processing, higher collection rates, and reduced administrative overhead compared to in-house operations.
Professional billing services provide:
- Experienced coding and billing specialists
- Sophisticated technology platforms
- Comprehensive compliance programs
- Transparent reporting and analytics
- Scalability to accommodate practice growth
The transition to outsourced medical claims billing requires careful partner selection, thorough implementation planning, and ongoing performance monitoring to ensure service levels meet practice expectations and financial objectives.
Medical claims billing serves as the critical link between healthcare delivery and financial sustainability, requiring expertise in clinical documentation, medical coding, payer regulations, and technology systems. Success in this complex environment demands attention to detail, continuous education, and systematic processes that prevent errors while maximizing legitimate reimbursement. Greenhive Billing Solutions provides comprehensive revenue cycle management services that optimize medical claims billing performance for healthcare providers across the United States, delivering improved cash flow, reduced administrative burden, and transparent communication throughout the billing process. Partner with experienced professionals who understand the intricacies of medical claims billing and are committed to your practice's financial success.