Healthcare operations encompass the complex coordination of clinical, administrative, and financial processes that keep medical practices running smoothly. From patient scheduling and resource allocation to revenue cycle management and compliance oversight, every operational decision impacts both patient outcomes and financial sustainability. For healthcare providers navigating increasingly complex regulatory requirements and reimbursement models, understanding how to optimize healthcare operations has become essential for long-term viability. Efficient operations translate directly to improved patient satisfaction, reduced administrative burden, and maximized revenue collection.
Understanding the Core Components of Healthcare Operations
Healthcare operations extend far beyond simple day-to-day task management. They represent the strategic orchestration of multiple interconnected systems designed to deliver quality patient care while maintaining financial health.
Clinical Workflow Management
Clinical workflows form the backbone of patient care delivery. These processes include appointment scheduling, patient intake, examination procedures, treatment protocols, and follow-up care coordination. When these workflows operate efficiently, providers can see more patients without compromising care quality.
Key clinical workflow elements include:
- Patient registration and demographic verification
- Medical history documentation and review
- Treatment planning and execution
- Care coordination between multiple providers
- Patient education and discharge planning
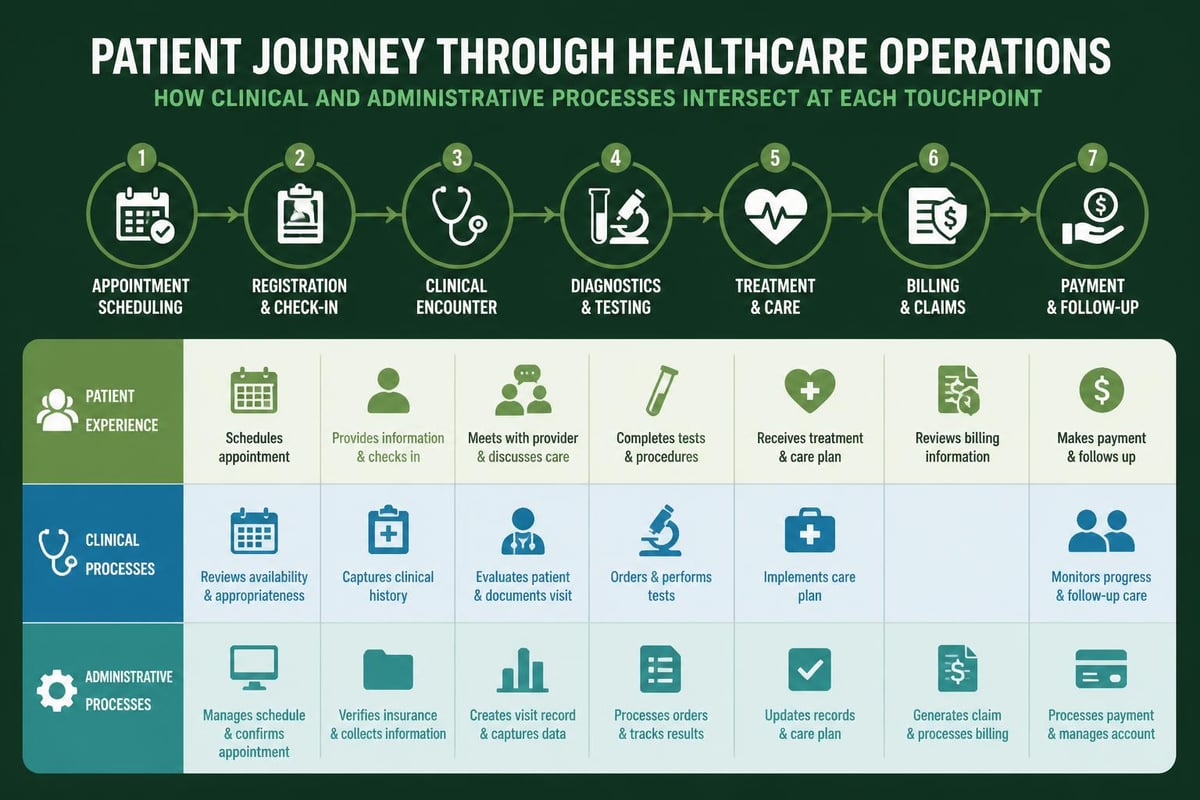
Streamlining clinical workflows requires continuous assessment of bottlenecks and inefficiencies. Many practices discover that seemingly minor process improvements, such as implementing electronic health records or optimizing exam room utilization, can yield significant productivity gains.
Administrative Process Optimization
Administrative functions support clinical operations by managing the business side of healthcare delivery. These processes ensure that practices maintain compliance, manage staff effectively, and handle the logistical requirements of running a medical facility.
| Administrative Function | Impact on Operations | Optimization Strategy |
|---|---|---|
| Staff scheduling | Ensures adequate coverage | Predictive scheduling based on patient volume |
| Inventory management | Reduces waste and stockouts | Just-in-time ordering systems |
| Facility management | Maintains safe, functional environment | Preventive maintenance programs |
| Compliance tracking | Prevents regulatory violations | Automated monitoring systems |
The application of data analytics in operations management has revolutionized how healthcare organizations approach administrative optimization, enabling data-driven decision-making across all operational domains.
Financial Operations and Revenue Cycle
Financial operations represent a critical component of healthcare operations, encompassing everything from insurance verification to final payment collection. The revenue cycle management process connects clinical services with financial outcomes, ensuring that providers receive appropriate reimbursement for the care they deliver.
Effective financial operations include:
- Insurance eligibility verification before patient appointments
- Accurate charge capture for all services provided
- Timely claims submission to payers
- Denial management and appeals for rejected claims
- Patient billing and collections for outstanding balances
Understanding what adjustments on medical bills mean helps practices identify revenue leakage and implement corrective measures. Many providers lose significant revenue simply because they lack systematic approaches to financial operations.
Operational Challenges Facing Healthcare Providers
Healthcare operations face unique challenges that distinguish them from other industries. The complexity of medical care, coupled with strict regulatory requirements and unpredictable patient volumes, creates operational hurdles that require specialized solutions.
Resource Allocation and Capacity Planning
Hospitals and medical practices must balance resource availability against fluctuating demand. Research on integrated planning approaches in hospitals demonstrates how simultaneous planning of operating rooms, beds, and staff enhances efficiency while maintaining care quality.
Effective resource allocation addresses:
- Physician and nursing staff scheduling to match patient volume patterns
- Equipment utilization to maximize return on investment
- Exam room and facility space optimization
- Supply chain management to prevent shortages
The core challenges in healthcare operations management often stem from the unpredictable nature of patient care needs combined with fixed resource constraints. Unlike manufacturing or retail, healthcare cannot simply turn away customers during peak periods.
Compliance and Regulatory Requirements
Healthcare operations must navigate an intricate web of federal, state, and local regulations. HIPAA compliance, quality reporting requirements, and payer-specific documentation standards add layers of complexity to operational processes.
Compliance considerations affecting operations:
- Patient privacy and data security protocols
- Clinical documentation requirements for reimbursement
- Quality measure reporting and value-based care metrics
- Accreditation standards and certification maintenance
- Billing and coding accuracy to prevent fraud allegations
The best practices for operational excellence in healthcare emphasize creating robust procedures that accommodate regulatory requirements without compromising efficiency.
Technology Integration Challenges
Modern healthcare operations increasingly depend on technology platforms that often struggle to communicate with each other. Electronic health records, practice management systems, billing software, and patient portals must work together seamlessly to support efficient operations.
Many practices face technology challenges including:
- Legacy systems that don't integrate with newer platforms
- Data silos that prevent comprehensive operational visibility
- High implementation costs for system upgrades
- Staff training requirements for new technologies
- Cybersecurity vulnerabilities as attack surfaces expand
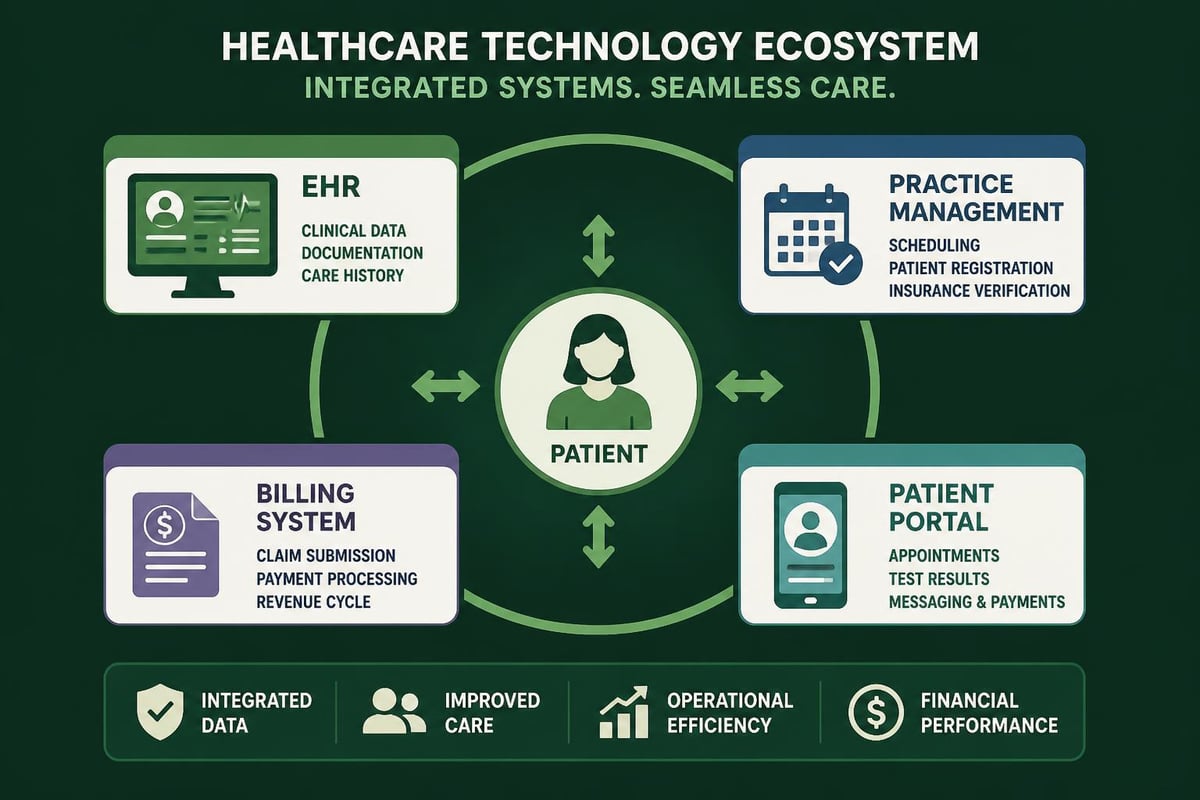
The emergence of Machine Learning Health Operations approaches offers new possibilities for optimizing complex healthcare processes through predictive analytics and automated decision support.
Strategic Approaches to Improving Healthcare Operations
Optimizing healthcare operations requires a systematic approach that addresses both immediate inefficiencies and long-term strategic goals. Successful practices implement continuous improvement methodologies tailored to healthcare's unique requirements.
Lean Methodology in Healthcare Settings
Lean principles, originally developed for manufacturing, translate effectively to healthcare operations when properly adapted. The core concept involves identifying and eliminating waste while maximizing value for patients.
Seven types of waste in healthcare operations:
- Waiting time for patients, staff, or information
- Overprocessing through redundant paperwork or unnecessary tests
- Inventory waste from expired supplies or overstocking
- Motion waste from inefficient facility layouts
- Defects requiring rework or corrections
- Overproduction of services not aligned with patient needs
- Underutilized talent and staff capabilities
Implementing lean healthcare operations starts with value stream mapping to identify where bottlenecks occur. Many practices discover that patients spend more time waiting than receiving actual care, indicating clear opportunities for improvement.
Process Standardization and Documentation
Standardizing clinical and administrative processes reduces variation, improves consistency, and facilitates training for new staff members. Well-documented procedures ensure that best practices become institutional knowledge rather than depending on individual expertise.
| Process Type | Standardization Benefits | Implementation Approach |
|---|---|---|
| Patient intake | Faster processing, fewer errors | Create standardized forms and checklists |
| Clinical documentation | Improved coding accuracy | Develop templates for common conditions |
| Billing procedures | Reduced claim denials | Establish verification protocols |
| Quality checks | Consistent care standards | Implement regular audits |
The importance of clean claims in medical billing demonstrates how standardization directly impacts financial outcomes. Practices that develop systematic approaches to charge capture and claims submission experience significantly lower denial rates.
Performance Metrics and Continuous Monitoring
What gets measured gets managed. Establishing key performance indicators for healthcare operations enables practices to track progress, identify emerging issues, and make data-driven decisions.
Critical operational metrics include:
- Patient access metrics: Time to appointment, wait times, schedule utilization
- Clinical efficiency indicators: Patient throughput, length of stay, treatment completion rates
- Financial performance measures: Days in accounts receivable, collection rates, denial percentages
- Staff productivity benchmarks: Patients per provider, revenue per full-time equivalent
- Quality indicators: Patient satisfaction scores, clinical outcomes, readmission rates
Research on intra-hospital patient transport illustrates how operational research methods can optimize specific healthcare processes through systematic measurement and modeling.
Revenue Cycle Integration Within Healthcare Operations
The revenue cycle represents where clinical operations meet financial sustainability. Effective integration ensures that the quality care providers deliver translates into appropriate reimbursement that sustains practice operations.
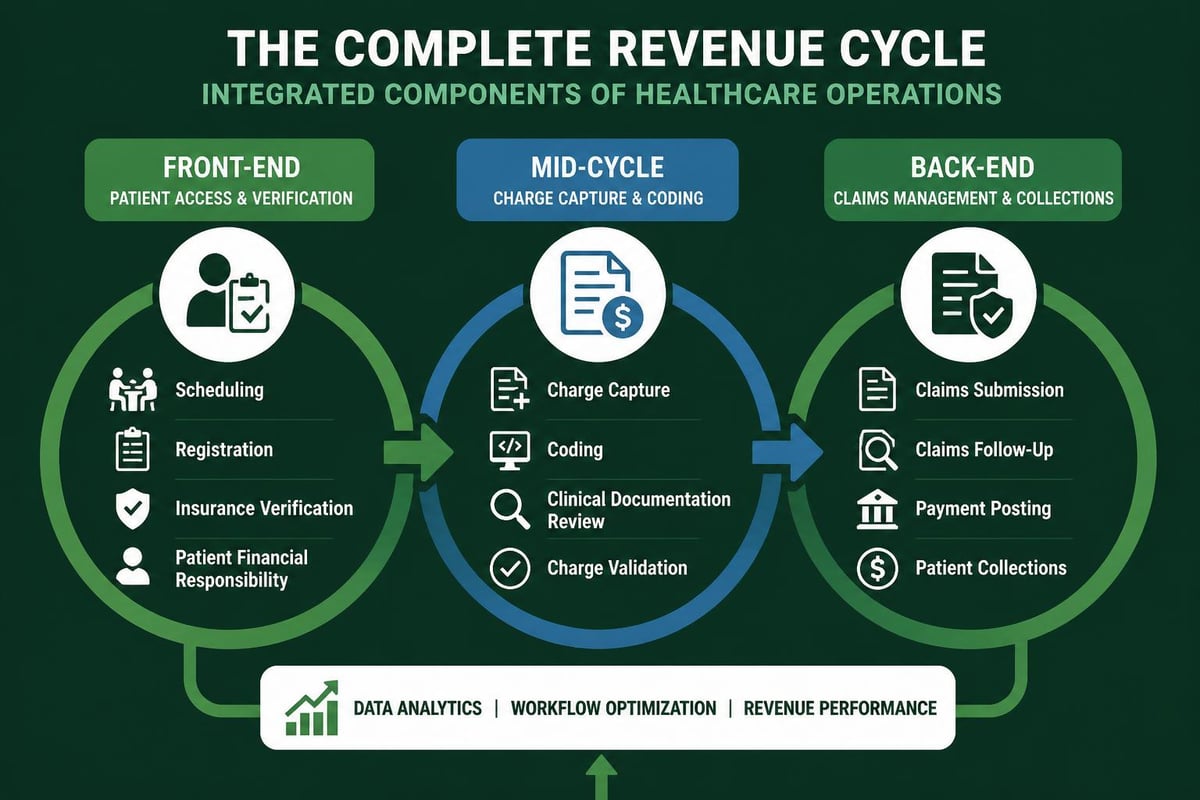
Front-End Revenue Cycle Operations
Front-end processes set the foundation for successful claims and payments. Insurance verification, benefit confirmation, and accurate patient demographic collection prevent downstream revenue disruptions.
Optimized front-end operations include:
- Real-time eligibility verification during scheduling
- Benefit investigation for planned procedures
- Prior authorization management for required services
- Upfront patient responsibility estimation and collection
- Accurate demographic and insurance information capture
Many practices underestimate the revenue impact of front-end accuracy. Understanding how to verify medical insurance effectively prevents claim denials and reduces rework throughout the revenue cycle.
Mid-Cycle Revenue Operations
Mid-cycle processes connect clinical service delivery with accurate charge capture and coding. This critical phase ensures that the documentation supports the services billed and that claims contain complete, accurate information.
Mid-cycle operational requirements:
- Charge capture systems integrated with clinical workflows
- Coding accuracy through proper documentation review
- Claim scrubbing to identify errors before submission
- Compliance checks against payer policies and regulations
Professional charge entry in medical billing requires understanding both clinical services and billing requirements. Errors at this stage cascade through the remaining revenue cycle, delaying payments and increasing administrative costs.
Back-End Revenue Cycle Operations
Back-end processes manage claims after submission, handling denials, posting payments, and collecting patient balances. Efficient back-end operations minimize days in accounts receivable and maximize collection rates.
| Back-End Function | Operational Impact | Best Practice |
|---|---|---|
| Denial management | Recovers rejected revenue | Root cause analysis and prevention |
| Payment posting | Maintains accurate financial records | Automated ERA processing |
| Patient collections | Improves cash flow | Clear billing statements and payment plans |
| Reconciliation | Ensures complete payment capture | Regular account reviews |
Effective denial management in medical billing requires both efficient appeals processes and systematic analysis to prevent recurrent denials. Practices that treat denials as operational failures rather than inevitable outcomes achieve superior financial performance.
Outsourcing as an Operational Strategy
Many healthcare providers discover that partnering with specialized service providers improves operational outcomes while allowing clinical staff to focus on patient care. Outsourcing revenue cycle functions has become an increasingly common strategy for optimizing healthcare operations.
When Outsourcing Makes Strategic Sense
Practices should consider outsourcing when internal operations consistently underperform industry benchmarks or when staff lacks specialized expertise. Revenue cycle management requires specific knowledge of payer requirements, coding regulations, and billing best practices that extend beyond clinical training.
Indicators that outsourcing may improve operations:
- Denial rates exceeding 10% of submitted claims
- Days in accounts receivable above 40 days
- Collection rates below 95% of expected reimbursement
- High staff turnover in billing positions
- Frequent compliance concerns or audit findings
- Lack of technology infrastructure for efficient processing
Working with top medical billing companies provides access to specialized expertise, established processes, and technology platforms without capital investment.
Maintaining Operational Control with External Partners
Successful outsourcing relationships maintain practice oversight while leveraging external expertise. Healthcare operations remain the provider's responsibility even when specific functions are delegated to service partners.
Effective outsourcing relationships include:
- Clear service level agreements defining performance expectations
- Regular reporting on operational and financial metrics
- Transparent communication about issues and opportunities
- Collaborative problem-solving for complex cases
- Continuous improvement initiatives to enhance outcomes
Understanding physician RCM requirements helps practices evaluate potential partners and establish productive working relationships that enhance rather than diminish operational control.
Technology's Evolving Role in Healthcare Operations
Technology continues transforming healthcare operations, creating new possibilities for efficiency while introducing implementation challenges. The most successful practices adopt technology strategically, focusing on solutions that address specific operational pain points.
Automation and Workflow Optimization
Automation eliminates repetitive manual tasks that consume staff time without adding clinical or operational value. From automated appointment reminders to robotic process automation for claims processing, technology reduces administrative burden.
High-value automation opportunities:
- Eligibility verification before appointments
- Claim scrubbing and error detection
- Payment posting from electronic remittance advice
- Prior authorization status checking
- Patient communication for scheduling and follow-up
Modern medical billing software solutions incorporate automation features that reduce manual intervention while improving accuracy and processing speed.
Data Analytics for Operational Insights
Analytics platforms transform operational data into actionable insights. Rather than simply tracking what happened, advanced analytics predict future trends and recommend operational adjustments.
Healthcare operations benefit from analytics in areas including:
- Patient volume forecasting for staffing decisions
- Revenue cycle bottleneck identification
- Payer performance comparison
- Provider productivity analysis
- Resource utilization optimization
Understanding healthcare revenue cycle analytics enables practices to shift from reactive to proactive operational management.
Interoperability and Information Exchange
Seamless information exchange between systems and organizations represents both a significant challenge and major opportunity for healthcare operations. True interoperability reduces duplicate data entry, prevents information gaps, and supports care coordination.
| Interoperability Level | Operational Benefit | Implementation Challenge |
|---|---|---|
| Foundational | Basic data exchange | Technical connectivity |
| Structural | Standardized formatting | Common data standards |
| Semantic | Shared understanding | Terminology mapping |
| Organizational | Cross-entity workflows | Business agreements |
The push toward interoperability promises to streamline healthcare operations by eliminating information silos that currently create operational friction and delays.
Workforce Considerations in Healthcare Operations
People ultimately execute healthcare operations, making workforce planning, training, and engagement critical operational success factors. Even the best processes and technologies fail without capable, motivated staff to implement them.
Cross-Training and Operational Flexibility
Cross-trained staff provide operational resilience, allowing practices to adapt to volume fluctuations, absences, and changing priorities. Rather than rigid role definitions, successful practices develop versatile team members who understand multiple operational functions.
Cross-training benefits include:
- Reduced vulnerability to unexpected staff absences
- Better understanding of how different operational functions connect
- Improved collaboration between departments
- Enhanced career development opportunities for staff
- Greater operational flexibility during volume peaks
Many practices discover that staff who understand both clinical and revenue cycle operations identify improvement opportunities that specialists miss.
Specialized Expertise for Complex Functions
While cross-training provides operational flexibility, certain healthcare operations functions require specialized expertise that justifies dedicated resources. Medical coding, denial management, and compliance oversight demand specific knowledge that comes from focused training and experience.
Functions benefiting from specialized staff:
- Medical coding: Requires certification and ongoing education
- Credentialing: Demands knowledge of complex payer requirements
- Compliance auditing: Needs understanding of regulatory frameworks
- Revenue cycle analytics: Benefits from data analysis expertise
- Denial appeals: Requires knowledge of appeals processes and medical necessity criteria
Understanding what billing and coding specialists do helps practices determine when to develop internal expertise versus partnering with external service providers.
Staff Engagement and Operational Culture
Engaged employees drive operational excellence through consistent execution, continuous improvement suggestions, and commitment to organizational goals. Healthcare operations suffer when staff view their roles as merely transactional rather than contributing to patient care outcomes.
Building operational culture requires:
- Clear communication about how operational efficiency supports patient care
- Recognition of process improvement contributions
- Involvement in operational decision-making
- Training opportunities for skill development
- Transparent performance feedback and coaching
Practices with strong operational cultures consistently outperform those that treat healthcare operations as separate from clinical mission.
Measuring Healthcare Operations Success
Defining and tracking success metrics ensures that operational initiatives deliver intended results. Without clear measurement frameworks, practices cannot distinguish effective improvements from wasted effort.
Financial Performance Indicators
Financial metrics provide objective measures of operational effectiveness. While not the only success indicators, financial performance reflects how well operations convert clinical services into sustainable revenue.
Key financial metrics for healthcare operations:
- Net collection rate (actual collections versus expected reimbursement)
- Days in accounts receivable (average time from service to payment)
- Claim denial rate (percentage of claims rejected on first submission)
- Cost to collect (operational expense per dollar collected)
- Revenue per provider (productivity measure)
These metrics should be tracked monthly and compared against both internal benchmarks and industry standards to identify performance gaps.
Operational Efficiency Measures
Efficiency metrics assess how well practices utilize resources to deliver care. These indicators reveal whether operations support or hinder clinical productivity.
| Efficiency Metric | Target Range | Operational Significance |
|---|---|---|
| Patient wait time | Under 15 minutes | Reflects scheduling and workflow efficiency |
| Exam room utilization | 70-80% | Indicates capacity optimization |
| Schedule fill rate | Above 90% | Measures access and scheduling effectiveness |
| Staff productivity | Varies by role | Assesses resource allocation |
Monitoring these metrics helps practices identify operational bottlenecks before they significantly impact financial performance or patient satisfaction.
Patient Experience Outcomes
Patient experience represents the ultimate measure of whether healthcare operations serve their intended purpose. Operations should facilitate rather than obstruct positive patient interactions with the healthcare system.
Patient experience indicators include:
- Appointment availability and scheduling convenience
- Wait time before being seen
- Ease of registration and check-in processes
- Clarity of billing statements and payment options
- Responsiveness to questions and concerns
Practices that optimize healthcare operations with patient experience in mind achieve both operational efficiency and higher satisfaction scores that increasingly influence reimbursement under value-based care models.
Optimizing healthcare operations requires balancing clinical excellence, operational efficiency, and financial sustainability across interconnected processes. By implementing systematic approaches to workflow management, revenue cycle integration, and performance measurement, healthcare providers can achieve superior outcomes while maintaining focus on quality patient care. Greenhive Billing Solutions specializes in comprehensive revenue cycle management services that streamline healthcare operations for medical practices across the United States. Our experienced team provides medical billing, claims processing, denial management, and insurance verification services designed to improve your practice's financial performance while allowing your clinical staff to focus on what they do best: caring for patients.