Managing financial operations in healthcare requires precision, compliance, and strategic oversight. Accounts receivable medical billing represents one of the most critical components of revenue cycle management, directly impacting cash flow, financial stability, and operational sustainability. For healthcare providers across the United States, understanding how to optimize this process can mean the difference between thriving financially and struggling with unpaid claims. This comprehensive guide explores the essential elements of accounts receivable in medical billing, offering actionable strategies to improve collections, reduce aging claims, and enhance overall financial performance.
Understanding the Fundamentals of Accounts Receivable Medical Billing
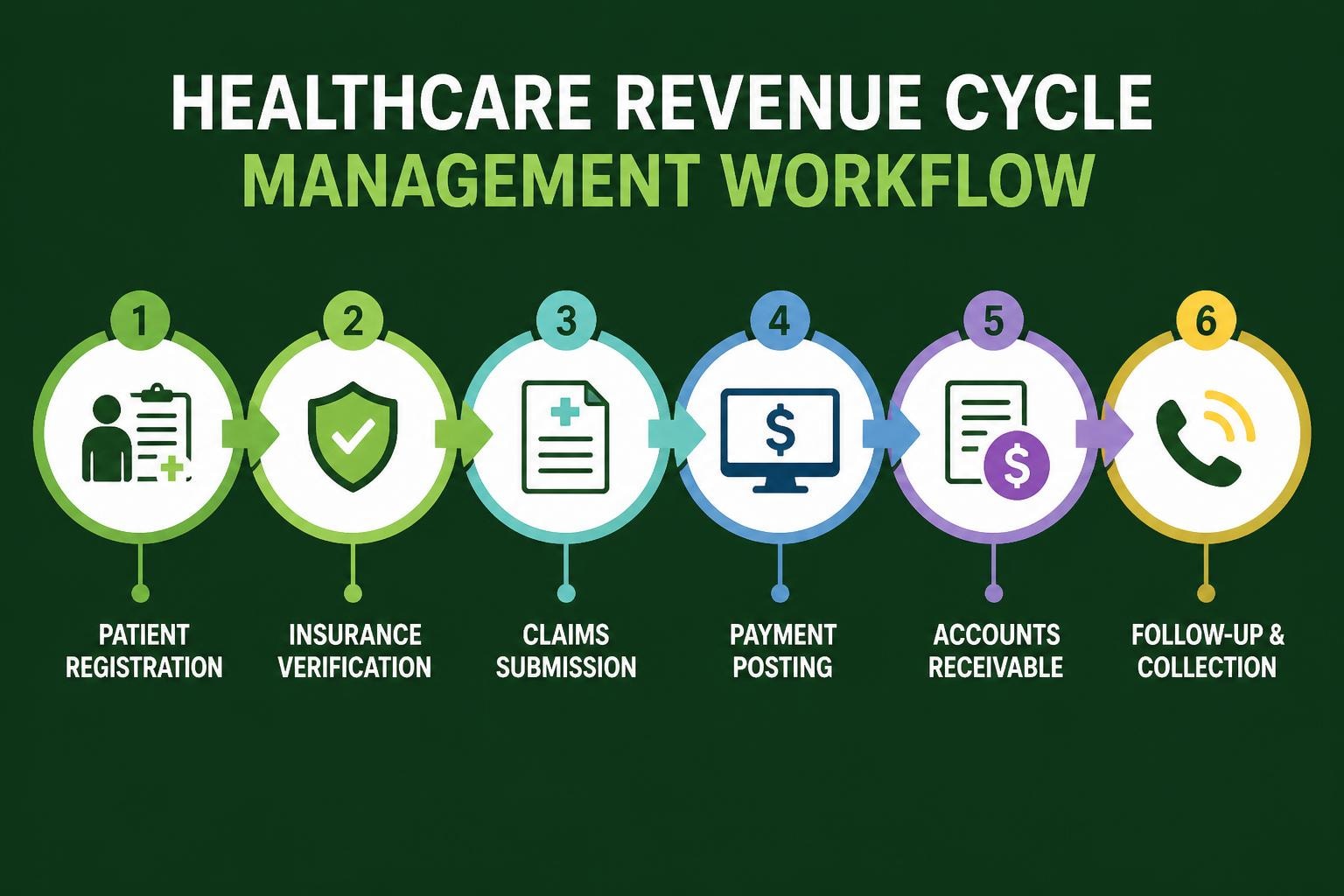
Accounts receivable medical billing encompasses all outstanding payments owed to healthcare providers for services rendered. This includes insurance payments, patient responsibilities, and any other balances not yet collected. Unlike traditional business receivables, medical billing accounts receivable involve complex interactions with multiple payers, strict regulatory requirements, and intricate coding systems.
The lifecycle of accounts receivable medical billing begins the moment a patient schedules an appointment and continues until all balances are fully collected or written off. This process involves insurance eligibility verification, accurate charge capture, proper coding, timely claim submission, payment posting, and diligent follow-up on unpaid balances.
Key Components of Medical Accounts Receivable
Primary elements include:
- Outstanding insurance claims awaiting payment
- Patient balances after insurance adjudication
- Denied claims requiring correction and resubmission
- Aging accounts categorized by time periods (30, 60, 90, 120+ days)
- Contractual adjustments from payer agreements
- Write-offs and bad debt
Healthcare providers must maintain detailed tracking of each component to identify bottlenecks, address payment delays, and implement corrective measures. The RCM process requires coordination across multiple departments, from front desk staff handling patient registration to billing specialists managing claim submissions and collections.
Common Challenges in Accounts Receivable Medical Billing
Healthcare organizations face numerous obstacles when managing accounts receivable medical billing. These challenges can significantly impact cash flow and require proactive strategies to overcome. Understanding common accounts receivable challenges provides the foundation for developing effective solutions.
Insurance Claim Denials and Rejections
Claim denials represent one of the most significant barriers to timely payment collection. Denials occur for various reasons, including:
- Incorrect or missing patient information
- Invalid procedure or diagnosis codes
- Lack of prior authorization
- Services not covered under patient's plan
- Timely filing limit violations
Each denied claim requires investigation, correction, and resubmission, consuming valuable staff time and delaying payment. Implementing robust denial management strategies reduces these occurrences and accelerates revenue collection.
Coding Errors and Documentation Issues
Medical coding accuracy directly affects accounts receivable medical billing performance. Errors in CPT codes, ICD-10 diagnoses, or modifiers lead to claim rejections, underpayments, or compliance risks. Healthcare providers must ensure coders stay current with annual code updates and payer-specific requirements.
Documentation deficiencies that impact AR include:
- Incomplete patient encounter notes
- Missing or inadequate clinical justification
- Failure to document medical necessity
- Inconsistencies between documentation and codes submitted
| Challenge Type | Impact on AR | Prevention Strategy |
|---|---|---|
| Claim Denials | 15-25% of initial submissions | Pre-submission claim scrubbing |
| Coding Errors | 5-10% revenue loss | Regular coder training and audits |
| Eligibility Issues | 3-7% claim rejections | Real-time verification systems |
| Documentation Gaps | 10-15% underpayments | Provider education programs |
Patient Payment Collection Difficulties
As patient financial responsibility increases through high-deductible health plans, collecting patient portions has become increasingly challenging. Many practices struggle with point-of-service collections, leading to higher accounts receivable balances and increased bad debt.
Managing accounts receivables for medical practices requires establishing clear payment policies, offering flexible payment options, and communicating financial expectations upfront.
Best Practices for Optimizing Accounts Receivable Medical Billing
Implementing strategic best practices transforms accounts receivable medical billing from a reactive process to a proactive revenue optimization system. Healthcare providers who adopt these approaches experience faster collections, reduced aging balances, and improved financial predictability.
Front-End Revenue Cycle Excellence
The foundation of effective accounts receivable medical billing begins before services are rendered. Front-end processes set the stage for clean claims and timely payments.
Critical front-end steps:
- Verify insurance eligibility and benefits before each appointment to confirm coverage and identify patient responsibilities
- Collect accurate demographic and insurance information to prevent claim rejections due to data errors
- Obtain necessary prior authorizations for procedures requiring payer approval
- Establish clear financial policies and communicate patient payment expectations
- Collect point-of-service payments including copays, deductibles, and previous balances
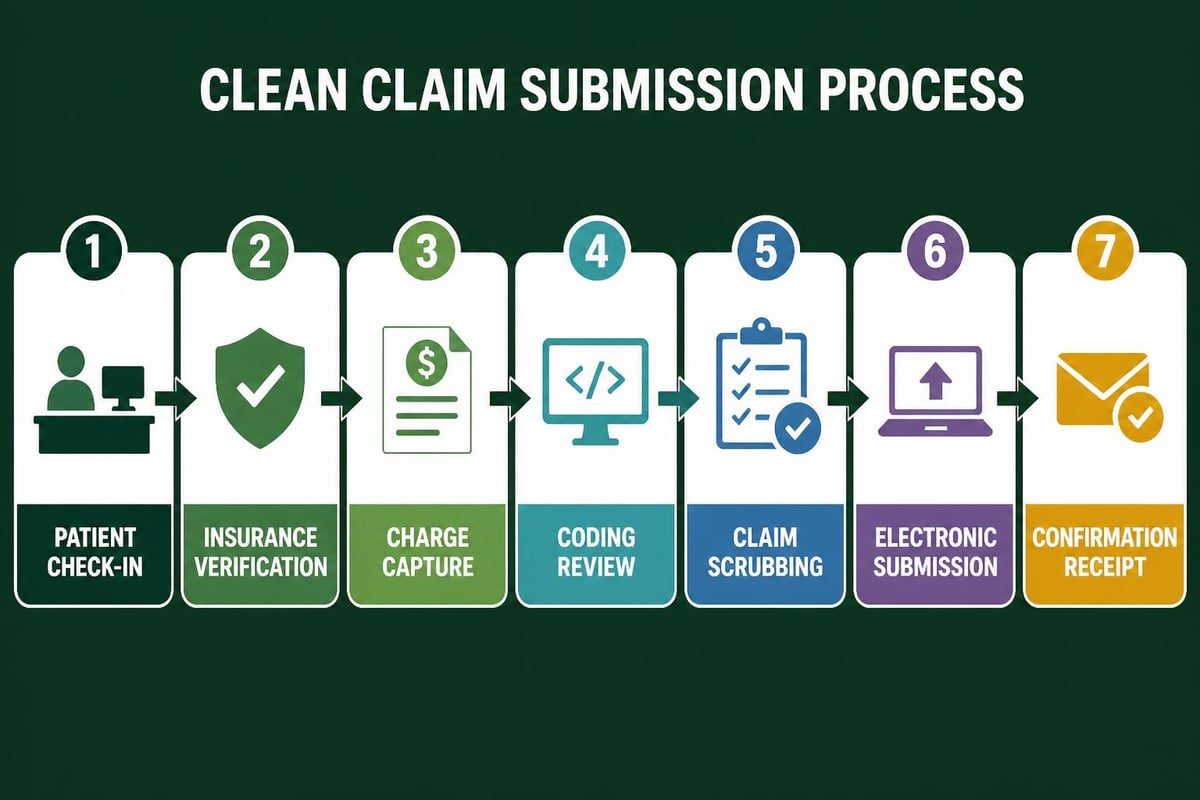
Streamlined Claims Submission Processes
Timely and accurate claim submission is essential for maintaining healthy accounts receivable medical billing metrics. Delays in submission create cash flow gaps and risk missing payer filing deadlines.
Healthcare providers should establish standardized workflows that include:
- Daily claim submission schedules rather than batch processing
- Automated claim scrubbing before submission to identify errors
- Electronic claim submission through clearinghouses
- Real-time claim status tracking
- Immediate attention to rejections and pended claims
Accounts Receivable Follow-Up Protocols
Systematic follow-up on unpaid claims separates high-performing practices from those with excessive aging balances. Strategies to improve medical billing accounts receivable emphasize the importance of consistent, organized follow-up activities.
Effective follow-up includes:
- Prioritizing claims by dollar amount and aging category
- Establishing payer-specific follow-up timelines
- Documenting all payer communications
- Escalating unresolved claims to supervisors
- Appealing denied claims with supporting documentation
Key Performance Indicators for Accounts Receivable Medical Billing
Monitoring specific metrics provides insight into accounts receivable medical billing health and identifies areas requiring improvement. Healthcare organizations should track these indicators regularly and establish benchmarks for performance.
Days in Accounts Receivable
This metric measures the average time between service delivery and payment receipt. The industry benchmark typically ranges from 30-40 days, though this varies by specialty and payer mix. Lower days in AR indicate efficient collections and healthy cash flow.
Calculation: (Total AR / Average Daily Charges) = Days in AR
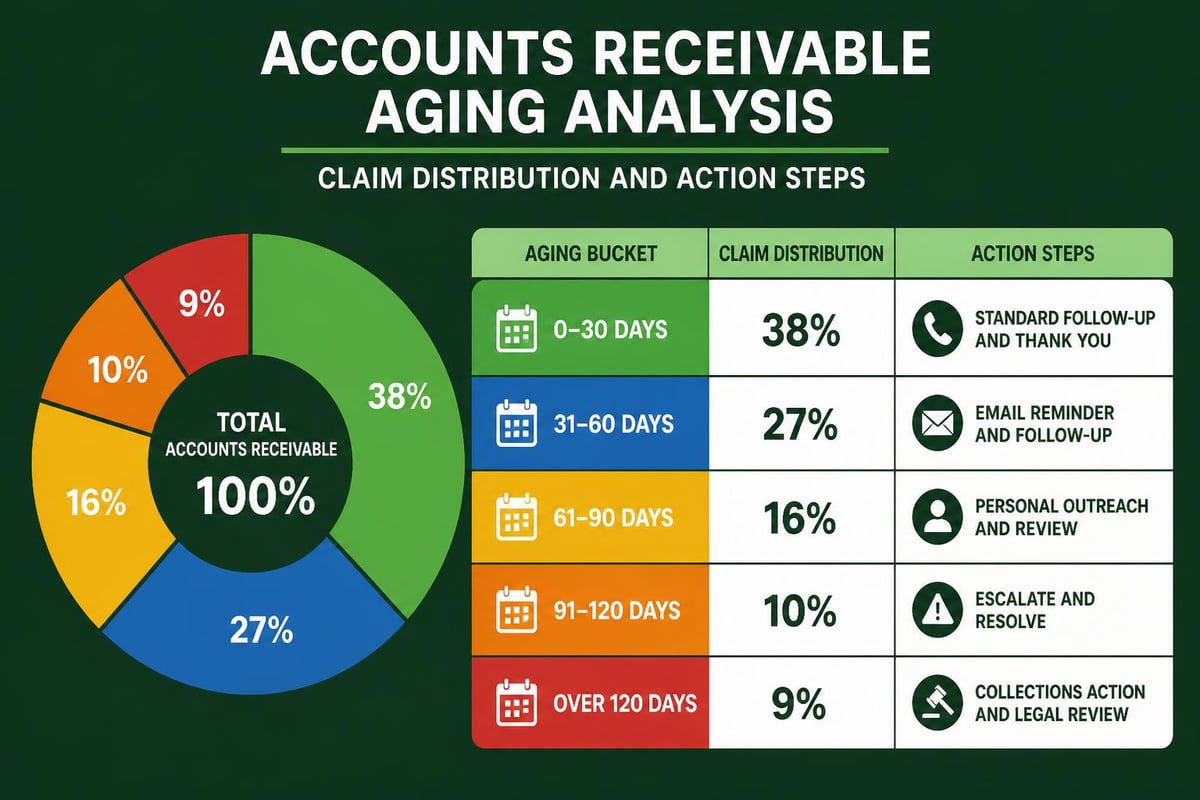
Accounts Receivable Aging Analysis
Breaking down receivables by aging categories reveals collection effectiveness and potential problem areas. A healthy AR distribution shows the majority of balances in the 0-30 day category, with minimal amounts aging beyond 90 days.
| Aging Category | Healthy Target | Action Required |
|---|---|---|
| 0-30 days | 60-70% of total AR | Standard follow-up |
| 31-60 days | 15-20% of total AR | Increased contact frequency |
| 61-90 days | 8-12% of total AR | Supervisor involvement |
| 91-120 days | 3-5% of total AR | Escalation to manager |
| 120+ days | Under 5% of total AR | Write-off consideration |
Clean Claim Rate
The percentage of claims paid on first submission without denials, rejections, or requests for additional information. Top-performing practices achieve clean claim rates above 95%, minimizing rework and accelerating payment.
Collection Rate
This metric measures the percentage of collectible revenue actually received. While 100% collection is unrealistic due to contractual adjustments and bad debt, best-in-class practices achieve 95-98% collection rates on available revenue.
Technology Solutions for Accounts Receivable Medical Billing
Modern revenue cycle management leverages technology to automate routine tasks, reduce errors, and provide real-time visibility into accounts receivable medical billing performance. Healthcare providers working with experienced RCM service providers benefit from access to industry-standard platforms and tools without the capital investment in proprietary software.
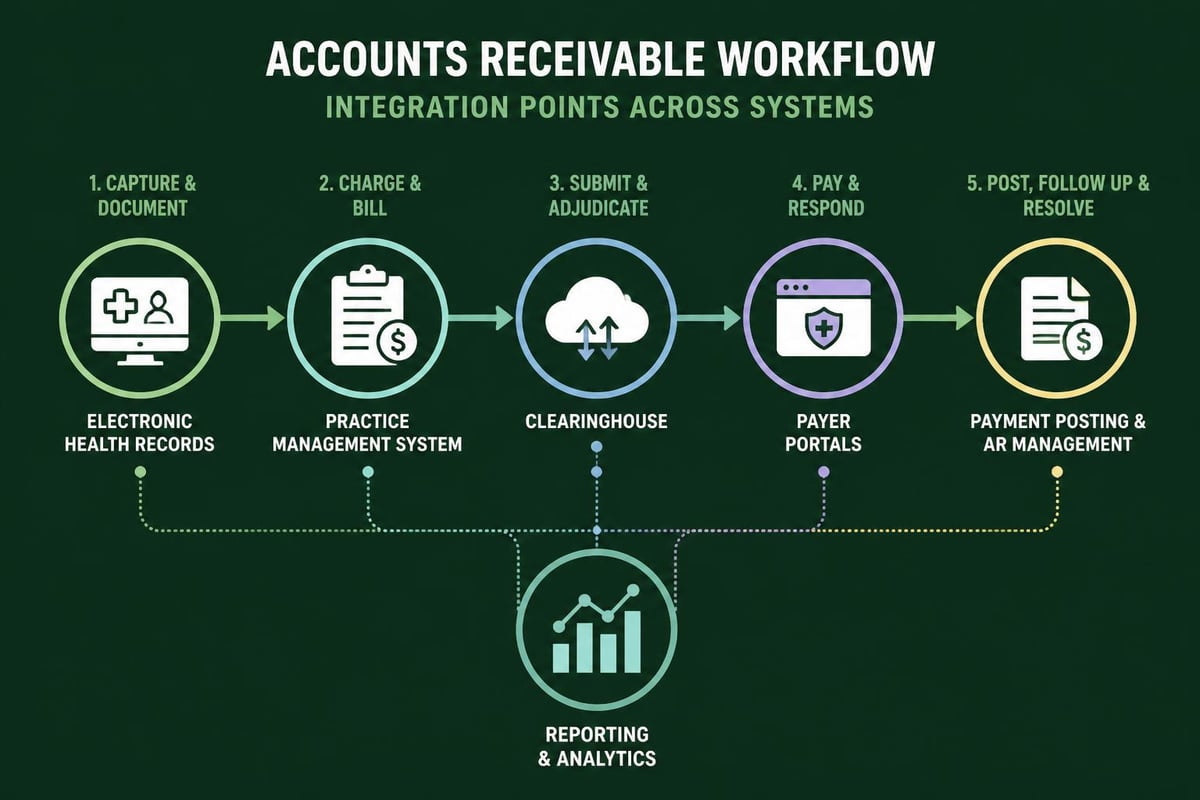
Practice Management and Billing Systems
Comprehensive practice management systems integrate scheduling, registration, billing, and collections into unified workflows. These platforms enable:
- Automated eligibility verification
- Electronic claim submission and tracking
- Payment posting automation
- Patient portal access for bill payment
- Reporting and analytics dashboards
When healthcare providers partner with specialized billing companies, they gain the advantages of enterprise-level systems operated by trained professionals who understand the nuances of accounts receivable medical billing.
Clearinghouse Integration
Electronic clearinghouses serve as intermediaries between healthcare providers and insurance payers, scrubbing claims for errors before submission and providing real-time claim status updates. This technology reduces rejection rates and accelerates the payment cycle.
Automation and Artificial Intelligence
Advanced automation streamlines accounts receivable medical billing by handling repetitive tasks and flagging anomalies for human review. AI-powered solutions can:
- Predict claim denial probability
- Recommend optimal follow-up timing
- Identify coding patterns associated with denials
- Prioritize work queues based on payment likelihood
- Generate patient payment plans based on financial indicators
Staff Training and Development for AR Excellence
Even the best technology cannot compensate for inadequately trained staff. Accounts receivable medical billing requires specialized knowledge spanning medical terminology, insurance policies, coding guidelines, and collection techniques.
Essential Competencies for Billing Staff
Healthcare organizations should invest in ongoing education covering:
Technical skills:
- Medical coding (CPT, ICD-10, HCPCS)
- Payer policies and billing requirements
- Practice management system proficiency
- Electronic remittance advice (ERA) interpretation
Soft skills:
- Professional communication with patients and payers
- Problem-solving and critical thinking
- Attention to detail and accuracy
- Time management and prioritization
Continuous Education Programs
The healthcare billing landscape evolves continuously with regulatory changes, payer policy updates, and coding revisions. Understanding accounts receivable challenges requires staying current with industry developments.
Organizations should establish regular training schedules including monthly coding updates, quarterly compliance reviews, and annual comprehensive education programs. Many healthcare providers find that partnering with specialized billing services provides access to dedicated professionals who maintain current certifications and expertise.
Strategies for Reducing Accounts Receivable Aging
Preventing claims from aging beyond 60 days significantly improves collection rates and cash flow. Common medical accounts receivable challenges often stem from delayed follow-up and inadequate aging management.
Proactive Claim Management
Rather than waiting for claims to age, implement proactive monitoring:
- Review all claims at 14 days post-submission if no response received
- Contact payers at 21 days for claims without payment or denial
- Escalate claims at 30 days to senior billing staff
- Initiate formal appeals at 45 days for unjustified denials
- Consider third-party collections at 120 days for patient balances
Payer-Specific Strategies
Each insurance company operates with unique policies, payment timelines, and claim submission requirements. Successful accounts receivable medical billing requires understanding these nuances and tailoring follow-up approaches accordingly.
Create payer profiles documenting:
- Standard payment timeframes
- Preferred contact methods (phone, portal, email)
- Common denial reasons and resolution strategies
- Appeal processes and required documentation
- Key contacts for complex issues
Patient Communication and Payment Plans
For patient responsibility balances, clear communication and flexible payment options improve collection rates while maintaining positive patient relationships. Healthcare accounts receivable management emphasizes the importance of patient-friendly billing practices.
Effective patient AR strategies include:
- Sending statements within 48 hours of insurance payment
- Offering online payment portals for convenience
- Providing payment plan options for large balances
- Making courtesy calls for balances over specific thresholds
- Using text and email reminders in addition to mailed statements
Denial Management Within Accounts Receivable
Denied claims directly impact accounts receivable medical billing performance by delaying payment and requiring additional resources for resolution. A comprehensive denial management program addresses both prevention and correction.
Root Cause Analysis
Understanding why claims are denied enables targeted prevention efforts. Track denial reasons by category:
| Denial Category | Common Causes | Prevention Strategy |
|---|---|---|
| Registration/Eligibility | Incorrect insurance info, expired coverage | Real-time verification at every visit |
| Authorization | Missing prior auth, services not covered | Authorization tracking system |
| Coding | Invalid codes, incorrect modifiers | Regular coder training and audits |
| Timely Filing | Late submission | Daily claim submission workflow |
| Medical Necessity | Insufficient documentation | Provider education on documentation |
Appeals Process
Well-documented appeals overturn a significant percentage of initial denials. Establish standardized appeal procedures including:
- Initial review within 3 business days of denial
- Collection of supporting documentation and medical records
- Preparation of clear, concise appeal letters
- Submission within payer deadlines
- Tracking and follow-up on appeal status
Denial Prevention Programs
Preventing denials is more cost-effective than appealing them. Implement pre-submission claim review processes that catch common errors before claims leave your practice. Many healthcare providers leverage medical coding audit services to identify patterns and improve accuracy.
Outsourcing Accounts Receivable Medical Billing Functions
Many healthcare providers partner with specialized revenue cycle management companies to optimize accounts receivable medical billing while allowing clinical staff to focus on patient care. This approach offers several advantages for practices of all sizes.
Benefits of Professional RCM Services
Specialized billing service providers bring expertise, technology access, and dedicated resources that may be difficult for individual practices to maintain internally:
Operational advantages:
- Reduced overhead costs compared to in-house billing departments
- Access to certified coding and billing specialists
- Advanced technology platforms without capital investment
- Scalability during practice growth or seasonal volume changes
- Reduced compliance risk through HIPAA-compliant processes
Financial benefits:
- Improved collection rates through specialized expertise
- Faster payment cycles with dedicated follow-up teams
- Reduced days in accounts receivable
- Lower denial rates through prevention programs
- Transparent reporting and analytics for financial decision-making
Selecting the Right RCM Partner
When evaluating potential billing service providers, healthcare organizations should assess several critical factors. Look for companies that demonstrate experience in your specific specialty, maintain transparent communication practices, and provide detailed performance reporting.
Key evaluation criteria include:
- Industry certifications and credentials
- Technology platform capabilities
- Client references and testimonials
- Service level agreements and guarantees
- Data security and HIPAA compliance measures
- Reporting frequency and detail
The Future of Accounts Receivable Medical Billing
The healthcare billing landscape continues evolving with technological advancements, regulatory changes, and shifting payment models. Understanding emerging trends helps healthcare providers prepare for future challenges and opportunities in accounts receivable medical billing.
Value-Based Care Impact
As healthcare shifts toward value-based reimbursement models, accounts receivable medical billing must adapt to track quality metrics, patient outcomes, and alternative payment arrangements. This transition requires enhanced data analytics and integration between clinical and financial systems.
Artificial Intelligence and Machine Learning
Advanced AI applications will increasingly automate routine billing tasks, predict denial probability, and optimize collection strategies. These technologies augment human expertise rather than replacing it, enabling billing professionals to focus on complex cases requiring judgment and negotiation skills.
Patient Financial Experience
With patients bearing greater financial responsibility, the line between traditional accounts receivable medical billing and consumer billing continues to blur. Healthcare providers must adopt patient-friendly billing practices including price transparency, flexible payment options, and simplified statements.
Emerging patient-centric approaches:
- Upfront cost estimates before service delivery
- Digital payment options including mobile apps
- Automated payment plans based on patient financial capacity
- Text and email communication preferences
- Integrated financial counseling services
Effective accounts receivable medical billing requires a combination of front-end accuracy, systematic follow-up, denial prevention, and ongoing performance monitoring. Healthcare providers who implement these strategies experience improved cash flow, reduced aging balances, and enhanced financial stability. Greenhive Billing Solutions delivers comprehensive revenue cycle management services that optimize every aspect of the billing process, from eligibility verification through final payment collection. Our team of certified professionals leverages industry-leading technology and best practices to improve your practice's financial performance while you focus on delivering exceptional patient care.