Healthcare providers face mounting pressure to maintain financial stability while delivering quality patient care. The complexity of medical billing, insurance verification, claims processing, and regulatory compliance demands comprehensive solutions healthcare organizations can rely on to optimize revenue cycles. Modern revenue cycle management has evolved beyond basic billing services to encompass integrated strategies that address every touchpoint from patient registration through final payment collection.
Understanding the Scope of Solutions Healthcare
Solutions healthcare encompasses a broad spectrum of services designed to address operational, financial, and clinical challenges facing medical practices. These comprehensive approaches integrate multiple disciplines including revenue cycle management, compliance monitoring, technology implementation, and workflow optimization.
Revenue cycle management represents a critical component where solutions healthcare makes its most significant impact. Medical practices struggle with claim denials, slow reimbursements, and administrative burden that diverts resources from patient care. According to healthcare professionals seeking evidence-based resources, reliable information and systematic approaches are essential for improving operational outcomes.
Key Components of Effective Healthcare Solutions
Financial Performance Optimization includes medical billing accuracy, charge capture completeness, payment posting efficiency, and accounts receivable management. Each element directly impacts cash flow and practice sustainability.
Compliance and Risk Management addresses HIPAA requirements, payer policy adherence, coding accuracy, and audit preparedness. Non-compliance carries substantial financial penalties and reputational damage.
Technology Integration leverages electronic health records, practice management systems, clearinghouse connectivity, and analytics platforms. The right technology infrastructure enables solutions healthcare to function efficiently.
The Revenue Cycle Management Foundation
Revenue cycle management serves as the backbone of solutions healthcare for medical practices. This process begins when patients schedule appointments and continues through final payment reconciliation. Understanding each phase allows providers to identify improvement opportunities and implement targeted interventions.
The revenue cycle process in healthcare encompasses patient access, clinical documentation, charge capture, claims management, payment processing, and accounts receivable follow-up. Each stage requires specialized expertise and attention to detail.
Patient Access and Verification
Strong front-end processes set the foundation for successful reimbursement. Insurance eligibility verification confirms coverage before services are rendered, preventing downstream payment issues. Demographic accuracy ensures claims reach the correct payer without delays.
Registration staff must collect complete patient information including:
- Current insurance policy details and member identification
- Accurate demographic data matching insurance records exactly
- Authorization requirements for planned procedures
- Financial responsibility acknowledgment and payment arrangements
- Previous balance information requiring resolution
When practices verify medical insurance proactively, they reduce claim denials by 30-40% and improve patient satisfaction through transparent financial communication.
Claims Processing and Submission
Medical coding translates clinical documentation into billable charges using standardized code sets. Professional coders ensure services are represented accurately with appropriate CPT, ICD-10, and HCPCS codes. This precision directly affects reimbursement levels and compliance.
Claims must be submitted as clean claims in medical billing to avoid processing delays. Clean claim rates above 95% indicate strong coding accuracy and data quality controls. Each rejected claim requires rework, delaying payment and consuming staff resources.
| Claim Status | Processing Time | Payment Timeline | Rework Required |
|---|---|---|---|
| Clean Claim | 2-5 days | 14-21 days | None |
| Pending Claim | 7-14 days | 30-45 days | Minimal |
| Rejected Claim | Immediate return | 45-60+ days | Extensive |
| Denied Claim | Full processing | 60-90+ days | Appeal necessary |
Denial Management as a Solutions Healthcare Priority
Claim denials represent significant revenue leakage for healthcare providers. Industry studies indicate 5-10% of claims face initial denial, with 60-70% of denied claims never resubmitted. This abandoned revenue amounts to billions annually across the healthcare sector.
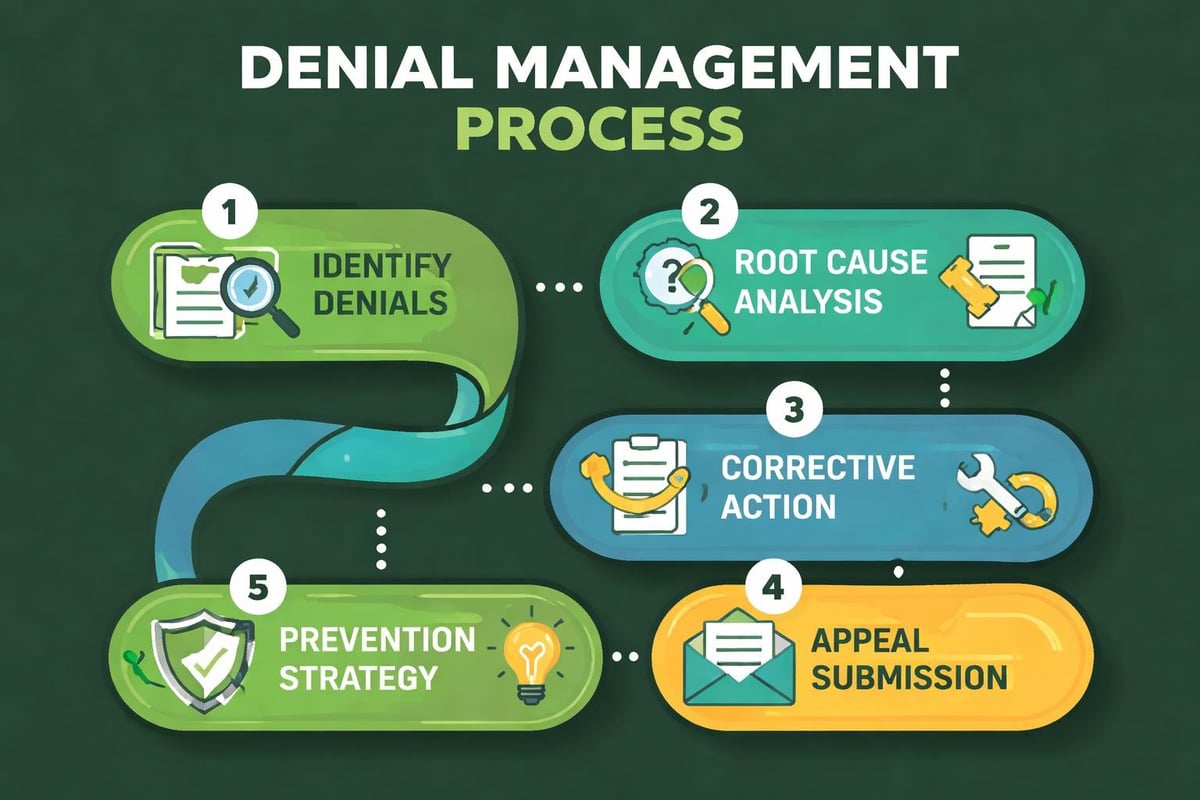
Effective denial management in medical billing requires systematic identification of denial patterns, root cause analysis, corrective action implementation, and appeal management. Solutions healthcare approaches treat denials as opportunities for process improvement rather than isolated incidents.
Common Denial Categories and Prevention
Eligibility and Authorization Denials occur when services are provided without confirming coverage or obtaining required pre-authorizations. Real-time verification systems and authorization tracking prevent most eligibility-related denials.
Coding and Documentation Denials result from insufficient documentation to support billed services, incorrect code selection, or missing modifiers. Regular coding audits and provider education address these issues proactively.
Timely Filing Denials happen when claims are submitted beyond payer deadlines, typically 90-365 days from service dates. Workflow monitoring and submission calendars ensure compliance with filing requirements.
Duplicate and Coordination of Benefits Denials involve claims submitted multiple times or without proper primary/secondary payer coordination. Robust claim scrubbing and payer sequencing logic prevent these denials.
Solutions healthcare providers implement denial prevention programs that include:
- Pre-service verification confirming coverage and authorization requirements before appointments
- Real-time claim edits identifying errors before electronic submission to payers
- Denial tracking dashboards monitoring trends by provider, payer, and denial reason
- Staff training programs addressing common errors specific to the practice specialty
- Appeal workflows ensuring timely, complete appeals for overturnable denials
Understanding how denial management improves cash flow helps practices prioritize these initiatives within broader operational strategies.
Technology's Role in Modern Solutions Healthcare
Healthcare technology has transformed revenue cycle management from manual, paper-based processes to automated, data-driven operations. Practice management systems, electronic health records, and specialized billing software create the infrastructure supporting solutions healthcare delivery.
Integration between clinical and financial systems eliminates duplicate data entry, reduces errors, and accelerates workflows. When documentation flows seamlessly from the EHR to billing systems, practices capture charges more completely and submit claims more quickly.
Essential Technology Components
Practice Management Systems handle scheduling, registration, billing, and reporting functions. These platforms serve as the operational hub for patient financial data and workflow management.
Clearinghouses validate claims against payer requirements before submission, identifying errors that would cause rejections. This intermediary layer significantly improves clean claim rates.
Analytics Platforms transform raw data into actionable insights about practice performance. Key performance indicators track days in accounts receivable, collection rates, denial percentages, and productivity metrics.
Patient Payment Portals facilitate online bill payment, payment plan management, and financial communication. These self-service tools improve patient satisfaction while accelerating collections.
Research into AI applications in healthcare demonstrates how emerging technologies will further enhance solutions healthcare through predictive analytics, automated coding assistance, and intelligent workflow optimization.
Compliance Requirements Driving Solutions Healthcare
Healthcare operates under stringent regulatory requirements affecting every aspect of revenue cycle management. HIPAA privacy and security rules govern patient information handling. Payer policies dictate coverage determinations and coding requirements. State and federal regulations establish billing standards and fraud prevention measures.
Solutions healthcare providers must maintain current knowledge of evolving regulations and implement compliant processes. Regular compliance audits identify gaps before they result in penalties or payment recoupment.
Critical Compliance Areas
HIPAA Privacy and Security protects patient health information through administrative, physical, and technical safeguards. Business associate agreements establish compliance responsibilities when vendors access protected data.
Coding Compliance requires accurate representation of services provided according to current code sets and payer guidelines. Upcoding, unbundling, and other improper practices carry severe penalties.
Billing Integrity demands truthful claim submission without fraudulent or abusive practices. False Claims Act violations can result in treble damages and exclusion from federal programs.
Documentation Requirements vary by service type and payer but universally require sufficient detail to support medical necessity and service level. Retrospective audits frequently focus on documentation adequacy.
| Compliance Area | Primary Regulation | Audit Frequency | Penalty Range |
|---|---|---|---|
| HIPAA Privacy | HIPAA Privacy Rule | Event-triggered | $100-$50,000 per violation |
| Coding Accuracy | Medicare rules, payer policies | Annual minimum | Repayment plus penalties |
| Billing Practices | False Claims Act, Anti-Kickback | Variable | $11,000-$23,000 per claim |
| Documentation | Medicare Conditions of Participation | 3-5 year cycle | Payment recoupment |
Specialized Solutions Healthcare by Practice Type
Different medical specialties face unique revenue cycle challenges requiring tailored solutions healthcare approaches. Primary care practices deal with high patient volumes and complex coding for evaluation and management services. Surgical specialties manage expensive implants, modifier usage, and global period billing.
Behavioral health providers navigate limited insurance coverage, complex authorization processes, and unique documentation requirements. Understanding medical billing for behavioral health helps these practices optimize reimbursement despite industry-specific challenges.
Primary Care Revenue Cycle Considerations
Primary care generates revenue primarily through evaluation and management services, preventive care visits, and ancillary services like immunizations and minor procedures. Accurate level of service coding significantly impacts reimbursement, yet documentation often fails to support higher-level codes.
Annual wellness visits represent valuable revenue opportunities when properly coded and documented. Knowing the annual wellness visit CPT code by age ensures correct billing for these preventive services.
Chronic care management programs provide additional revenue streams for primary care practices managing patients with multiple chronic conditions. These time-based services require tracking and documentation systems to support compliant billing.
Specialty Practice Unique Requirements
Surgical practices must manage complex modifier requirements, global period tracking, and implant billing. Solutions healthcare for these providers includes specialized coding expertise and systems supporting detailed charge capture.
Diagnostic imaging centers deal with technical and professional component billing, contrast agent coding, and prior authorization management. Revenue cycle solutions must accommodate split billing arrangements and modifier complexity.
Mental health and substance abuse treatment providers face unique challenges including limited sessions allowed, frequent prior authorization requirements, and stigma affecting patient payment. Specialized revenue cycle support addresses these behavioral health-specific issues.

Performance Metrics Measuring Solutions Healthcare Success
Quantifiable metrics enable healthcare providers to assess revenue cycle performance and identify improvement opportunities. Key performance indicators provide objective measurements of efficiency, effectiveness, and financial health.
Days in accounts receivable measures the average time between service delivery and payment collection. Industry benchmarks suggest 30-40 days for well-managed practices, though this varies by specialty and payer mix.
Essential Revenue Cycle KPIs
Net Collection Rate calculates the percentage of expected reimbursement actually collected after contractual adjustments. Rates above 95% indicate strong performance across verification, coding, and collections functions.
First Pass Resolution Rate tracks the percentage of claims paid upon initial submission without requiring corrections or appeals. This metric directly reflects coding accuracy and claim scrubbing effectiveness.
Denial Rate measures rejected and denied claims as a percentage of total submissions. Tracking denial rates by reason code, payer, and provider identifies specific improvement targets.
Patient Collection Rate compares patient responsibility collected to total patient responsibility billed. As patient financial responsibility increases, this metric becomes increasingly critical to practice financial health.
| Performance Metric | Target Range | Measurement Frequency | Primary Drivers |
|---|---|---|---|
| Days in AR | 30-40 days | Monthly | Claim submission speed, payer processing time, follow-up effectiveness |
| Net Collection Rate | 95-98% | Monthly | Coding accuracy, contract rates, collection effectiveness |
| Clean Claim Rate | 95-98% | Weekly | Data accuracy, coding quality, eligibility verification |
| Denial Rate | 5-8% | Weekly | Verification processes, coding accuracy, authorization management |
Understanding what affects healthcare revenue cycle analytics helps practices establish meaningful benchmarks and track progress toward financial goals.
Outsourcing Versus In-House Revenue Cycle Management
Healthcare providers must decide whether to manage revenue cycles internally or partner with specialized solutions healthcare vendors. Each approach offers distinct advantages and challenges depending on practice size, specialty, and internal capabilities.
In-house management provides direct control over processes, immediate access to staff, and integration with clinical workflows. However, it requires significant investment in staff salaries, benefits, training, technology, and ongoing management.
Evaluating Outsourcing Benefits
Professional revenue cycle management services offer specialized expertise, scalable resources, advanced technology platforms, and performance guarantees. These providers dedicate entire organizations to staying current with payer requirements, regulatory changes, and industry best practices.
Cost structure shifts from fixed salaries and benefits to variable fees based on collections. This arrangement aligns vendor incentives with practice financial performance and eliminates overhead for vacation, sick time, and turnover.
Working with experienced providers like those listed among top medical billing companies gives practices access to specialized expertise without internal hiring and training requirements.
Transparency and Communication remain critical when outsourcing revenue cycle functions. Providers should expect regular reporting, accessible account representatives, and collaborative problem-solving approaches.
Technology Integration must allow seamless data exchange between practice systems and vendor platforms. Cloud-based solutions facilitate real-time information sharing while maintaining security and compliance.
Performance Guarantees establish accountability through contractual metrics and service level agreements. Well-structured contracts include clean claim rate minimums, days in AR targets, and collection rate benchmarks.
Emerging Trends Shaping Solutions Healthcare
Healthcare revenue cycle management continues evolving in response to technological advancement, regulatory changes, and shifting reimbursement models. Practices must stay informed about emerging trends to maintain competitive advantages and financial stability.
Value-based reimbursement models shift focus from volume to quality and outcomes. These arrangements require enhanced data analytics, quality reporting, and risk management capabilities beyond traditional fee-for-service billing.
Artificial Intelligence and Automation
Machine learning algorithms now assist with coding suggestions, denial prediction, and payment variance identification. These technologies augment human expertise rather than replacing it, enabling staff to focus on complex issues requiring judgment and experience.
Robotic process automation handles repetitive tasks like eligibility verification, payment posting, and claim status checking. This automation reduces labor costs while improving accuracy and turnaround times.
Natural language processing extracts billable services from clinical documentation, improving charge capture completeness. This technology identifies procedures and diagnoses providers document but fail to bill.
Patient Financial Responsibility Growth
High-deductible health plans transfer increasing financial responsibility to patients. Practices must adapt collection strategies, implement price transparency tools, and offer flexible payment arrangements to maintain collection rates.
Point-of-service collection becomes essential as patient balances grow. Staff training in financial conversations, payment plan options, and empathetic collection approaches improves both collections and patient satisfaction.
Price transparency requirements now mandate that providers disclose cost estimates before services are delivered. Solutions healthcare must include tools and processes supporting compliant price estimation based on patient insurance and service mix.
Understanding resources like those provided through trusted medical information sources helps practices make informed decisions about emerging trends and industry changes.
Building a Sustainable Revenue Cycle Strategy
Long-term financial health requires strategic planning beyond day-to-day operational management. Successful practices assess current performance, identify improvement priorities, implement targeted interventions, and measure results continuously.
Comprehensive assessments evaluate people, processes, and technology across the entire revenue cycle. These reviews identify strengths to leverage and weaknesses requiring attention. External assessments provide objective perspectives practices may miss through internal review alone.
Strategic Implementation Framework
1. Current State Analysis documents existing workflows, performance metrics, technology utilization, and staff capabilities. This baseline establishes starting points for improvement initiatives.
2. Gap Identification compares current performance against industry benchmarks and internal goals. Prioritization focuses resources on areas with greatest financial impact.
3. Solution Design develops specific interventions addressing identified gaps. Solutions may include technology upgrades, process redesign, staff training, or outsourcing arrangements.
4. Implementation Planning establishes timelines, resource requirements, success metrics, and accountability structures. Phased approaches minimize disruption while delivering incremental improvements.
5. Performance Monitoring tracks key metrics against targets, identifies emerging issues, and validates intervention effectiveness. Continuous monitoring enables rapid course correction when needed.
Revenue cycle success requires ongoing attention rather than one-time fixes. Markets change, regulations evolve, and payer requirements shift constantly. Practices must maintain adaptive capabilities that respond to changing conditions while preserving operational stability.
Staying informed through reliable sources for health information and professional development ensures teams remain current with industry developments affecting revenue cycle management.
Selecting the Right Solutions Healthcare Partner
Practices considering outsourced revenue cycle management must evaluate potential partners carefully. The right relationship delivers measurable financial improvements, operational efficiency gains, and peace of mind that billing functions are handled professionally.
Experience within your specific specialty matters significantly. Payer requirements, coding nuances, and documentation standards vary substantially across medical specialties. Partners with relevant expertise deliver better results with shorter learning curves.
Evaluation Criteria for RCM Partners
Industry Experience and Reputation can be assessed through client references, case studies, industry recognition, and longevity. Established providers demonstrate proven methodologies and stable operations.
Technology Capabilities should include modern platforms, electronic data exchange, real-time reporting, and integration with major practice management and EHR systems. Technology enablement drives efficiency and accuracy.
Service Scope and Flexibility determines whether providers offer comprehensive services or specialized functions. Some practices need full-cycle support while others require targeted assistance with specific challenges like denials or credentialing.
Communication and Transparency establishes the foundation for successful partnerships. Accessible account management, regular reporting, and collaborative problem-solving approaches indicate client-focused service models.
Compliance and Security must include HIPAA compliance, business associate agreement execution, secure data handling, and regular security audits. Financial data security and patient privacy cannot be compromised.
Pricing Structure and Contract Terms should align costs with results through percentage-based fees or performance guarantees. Transparent pricing without hidden fees enables accurate cost-benefit analysis.
Exploring how the healthcare revenue cycle management industry operates helps practices understand standard service models and set appropriate expectations for vendor relationships.
Solutions healthcare represents an integrated approach to the financial and operational challenges facing medical practices today. By combining specialized expertise, advanced technology, and proven processes, comprehensive revenue cycle management delivers measurable improvements in reimbursement, efficiency, and compliance. Greenhive Billing Solutions provides tailored revenue cycle management services designed specifically for healthcare providers who need reliable partners to optimize financial performance. Our team of experienced professionals handles medical billing, verification, claims processing, and denial management with a commitment to transparency, compliance, and maximum reimbursements, allowing you to focus on delivering exceptional patient care.