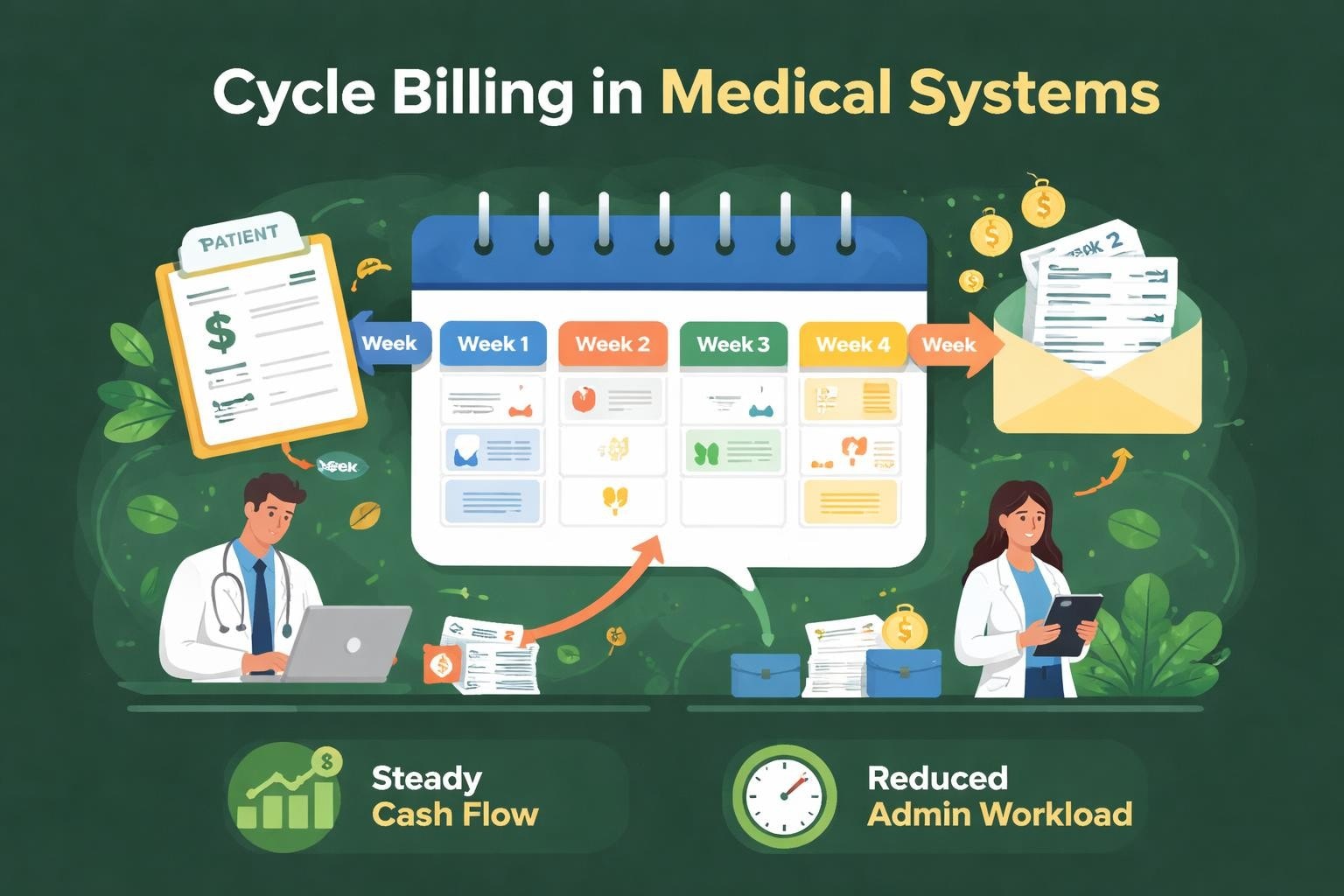
Healthcare providers face constant challenges managing their revenue cycles while delivering quality patient care. Among the various billing strategies available, cycle billing medical practices implement represents a powerful approach to maintaining consistent cash flow and reducing administrative burden. This method involves distributing billing statements throughout the month rather than sending all invoices on a single date, creating a more manageable workflow and improving collection rates.
Understanding Cycle Billing in Healthcare Revenue Management
Cycle billing medical systems divide patient accounts into groups and assign each group a specific billing date within the month. Instead of overwhelming billing departments with end-of-month statement runs, this approach distributes the workload evenly across thirty days.
The fundamental concept behind this billing methodology connects directly to operational efficiency. When practices send all statements on the first of each month, they create predictable bottlenecks in their revenue cycle. Staff members scramble to process thousands of statements simultaneously, patient inquiries flood phone lines during the same period, and payment processing becomes concentrated in specific weeks.
Key Components of Effective Cycle Billing Systems
A well-designed cycle billing medical framework includes several essential elements that work together to optimize revenue collection:
- Account segmentation based on patient demographics, insurance types, or alphabetical groupings
- Automated statement generation tied to predetermined billing cycles
- Tracking mechanisms to monitor which accounts belong to each billing cycle
- Integration with practice management systems for seamless data flow
- Compliance protocols ensuring HIPAA standards throughout the billing process
The medical billing cycle encompasses numerous steps, and cycle billing influences how practices manage the statement generation and collection phases.
Benefits That Transform Practice Financial Performance
Healthcare organizations implementing cycle billing medical strategies experience measurable improvements across multiple operational areas. The advantages extend beyond simple convenience, directly impacting financial health and patient relationships.
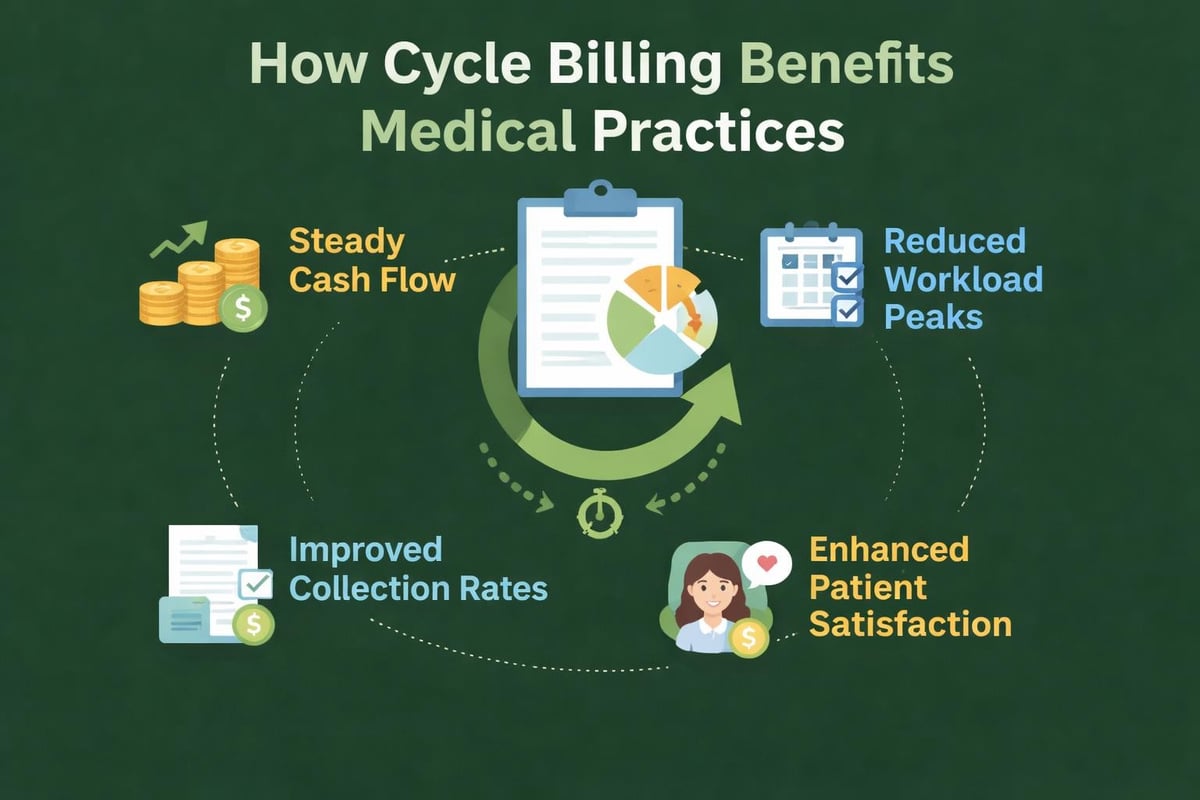
Steady Cash Flow Throughout the Month
Traditional billing creates feast-or-famine payment patterns. Cycle billing medical practices adopt generates predictable revenue streams by encouraging payments throughout the entire month rather than clustering them around specific dates.
Cash flow stability becomes particularly crucial for smaller practices with limited financial reserves. When revenue arrives consistently, practices can better manage:
- Payroll obligations
- Supply ordering schedules
- Equipment investments
- Emergency expenditures
- Operational expenses
This distribution effect helps practices maintain healthier working capital positions without relying on credit lines or delayed vendor payments.
Reduced Administrative Workload Peaks
Billing department staff members experience significantly lower stress levels when workloads remain consistent. The cycle billing medical approach eliminates the monthly crunch that traditionally characterizes healthcare billing operations.
| Traditional Billing | Cycle Billing Medical |
|---|---|
| All statements on day 1 | Statements distributed across 30 days |
| Staff overtime required monthly | Consistent staffing needs |
| Phone lines overwhelmed | Manageable inquiry volumes |
| Error rates increase under pressure | Quality maintained through balanced workload |
Organizations focused on healthcare revenue cycle management recognize that employee burnout directly correlates with billing errors and delayed collections.
Implementing Cycle Billing in Your Medical Practice
Transitioning to a cycle billing medical system requires careful planning and systematic execution. Practices cannot simply switch overnight without risking disruption to their revenue streams.
Step-by-Step Implementation Process
Step 1: Analyze Current Billing Patterns
Begin by examining existing billing cycles, payment trends, and staffing capabilities. Document when patients typically pay, which days generate the highest inquiry volumes, and how current processes handle statement generation.
Step 2: Design Account Segmentation Strategy
Determine how to divide patient accounts into billing cycles. Common approaches include:
- Alphabetical groupings (A-F on specific dates, G-L on others)
- Insurance type categories (commercial, Medicare, Medicaid, self-pay)
- Geographic zones for multi-location practices
- Patient account numbers or medical record numbers
Step 3: Configure Practice Management Systems
Most modern billing software supports cycle billing functionality. Work with your technology vendor to establish the necessary configurations, ensuring the system can automatically assign accounts to appropriate cycles and generate statements according to your schedule.
Step 4: Communicate Changes to Patients
Transparent communication prevents confusion when patients notice statement timing changes. Send advance notifications explaining the new billing schedule and what patients should expect regarding future statements.
Step 5: Train Staff on New Procedures
Ensure all team members understand the cycle billing medical framework, including how to respond to patient questions, process payments tied to specific cycles, and troubleshoot issues that arise during the transition.
The medical documentation and billing cycle requires precise coordination, and staff training becomes critical when implementing new methodologies.
Optimizing Cycle Billing for Maximum Revenue Impact
Once a cycle billing medical system operates successfully, practices can refine their approach to achieve even better results. Optimization focuses on analyzing performance metrics and adjusting parameters to improve collection rates.
Performance Metrics to Monitor
Tracking specific key performance indicators reveals whether cycle billing delivers expected benefits:
- Days in accounts receivable across different billing cycles
- Collection rates by cycle group
- Patient inquiry volumes distributed throughout the month
- Statement processing errors before and after implementation
- Staff overtime hours required for billing functions
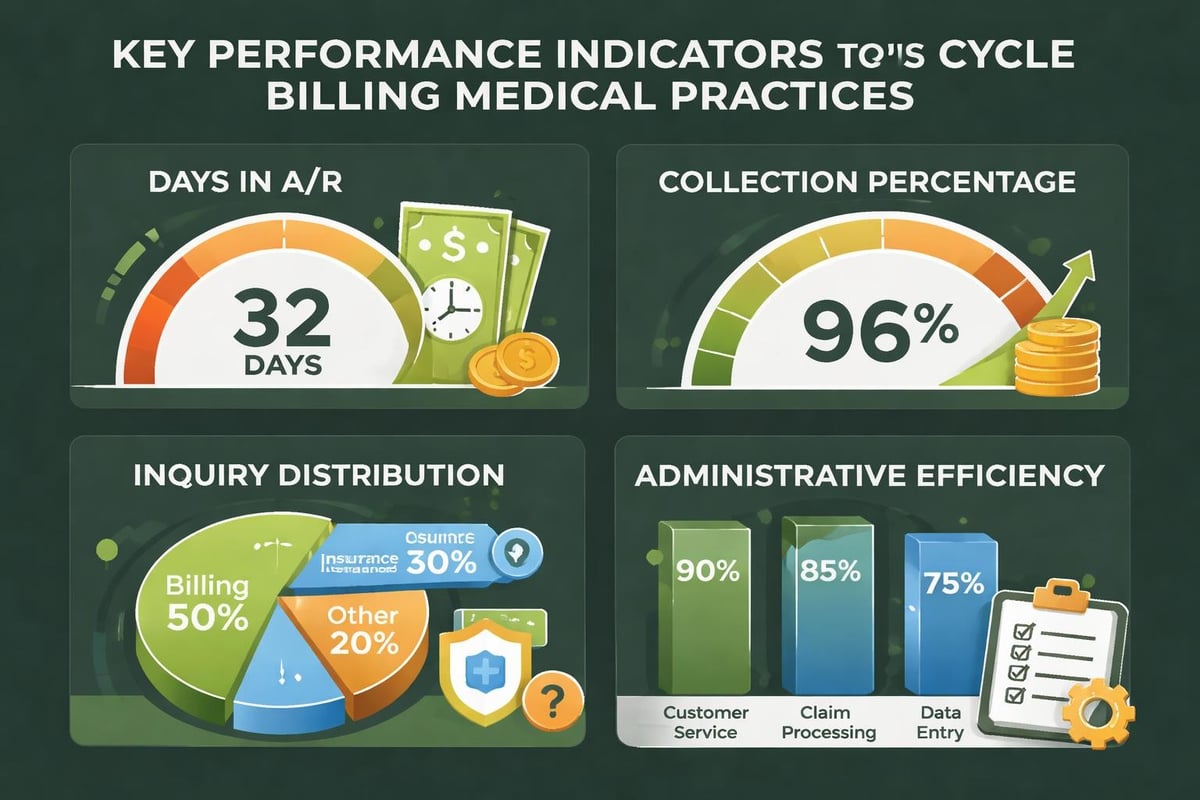
Practices should compare these metrics against baseline measurements taken before implementing cycle billing. Significant improvements validate the strategy, while stagnant numbers indicate adjustment opportunities.
Integration with Denial Management Processes
Cycle billing medical operations work most effectively when integrated with comprehensive denial management systems. Understanding denial management in medical billing helps practices coordinate their billing cycles with appeals processes and resubmission timelines.
When denials arrive throughout the month rather than concentrating around specific dates, staff members can address them more efficiently. This distributed workload allows for thorough investigation of each denial, increasing the likelihood of successful appeals and reducing revenue leakage.
Technology Considerations for Cycle Billing Success
Modern healthcare billing relies heavily on technology platforms that facilitate automated processes and reduce manual intervention. Cycle billing medical implementations depend on robust software capabilities.
Essential Software Features
Healthcare providers should verify their billing systems include these critical functionalities:
- Automated cycle assignment that categorizes new patients into appropriate billing groups
- Flexible scheduling options allowing practices to adjust cycle dates as needed
- Batch processing capabilities supporting efficient statement generation
- Integration with payment portals enabling patients to pay online regardless of billing cycle
- Comprehensive reporting tools tracking performance across all billing cycles
Organizations evaluating medical billing software for small businesses should prioritize platforms offering native cycle billing functionality rather than attempting workarounds with basic systems.
Data Security and Compliance
Protected health information flows through every aspect of the billing process. Cycle billing medical systems must maintain HIPAA compliance regardless of when statements generate or how patient data segments across different billing groups.
Security considerations include:
- Encrypted data transmission between systems
- Access controls limiting who can view or modify billing cycle assignments
- Audit trails documenting all changes to patient billing information
- Secure statement delivery whether through mail or electronic portals
- Backup procedures ensuring data preservation across all billing cycles
Professional revenue cycle management providers maintain stringent compliance protocols across all billing operations, protecting both practices and patients from data breaches.
Addressing Common Cycle Billing Challenges
Despite significant advantages, cycle billing medical practices adopt may encounter obstacles during implementation or ongoing operations. Recognizing these challenges early allows for proactive problem-solving.
| Challenge | Solution Approach |
|---|---|
| Patient confusion about statement timing | Clear communication materials and staff training |
| Uneven cycle distribution causing workload imbalances | Periodic analysis and rebalancing of account assignments |
| System limitations preventing full automation | Software upgrades or migration to more capable platforms |
| Coordination with insurance payment cycles | Strategic cycle assignment based on payer patterns |
| Regulatory compliance across different cycles | Standardized procedures applied uniformly to all cycles |
Managing Patient Expectations
Some patients expect statements on specific dates each month based on years of consistent billing patterns. When practices transition to cycle billing medical methodologies, temporary confusion may result.
Effective communication strategies include:
- Statement stuffers explaining the new billing schedule
- Website updates describing when patients in different groups will receive statements
- Phone scripts for staff members answering timing questions
- FAQ documents addressing common concerns
- Email notifications for patients enrolled in electronic communication
Transparency builds trust and reduces the volume of billing inquiries that could otherwise overwhelm customer service resources.
Financial Planning Benefits for Healthcare Organizations
Beyond operational advantages, cycle billing medical practices implement provides strategic financial planning benefits that strengthen long-term organizational health.
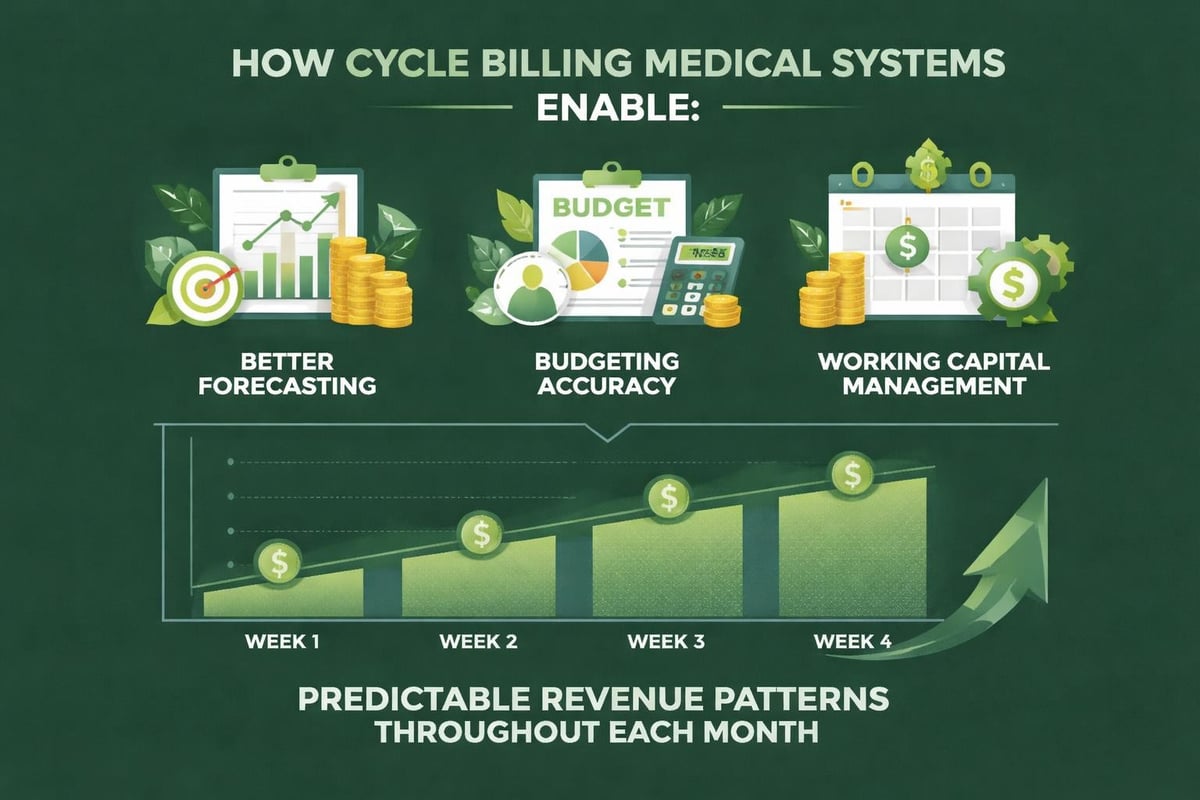
Improved Revenue Forecasting
When payments arrive consistently throughout each month, financial managers can develop more accurate revenue projections. This predictability supports:
- Cash flow modeling for expansion planning
- Loan applications demonstrating stable revenue patterns
- Vendor negotiations based on reliable payment capabilities
- Investment decisions supported by predictable working capital
- Budget development grounded in realistic income expectations
Healthcare organizations working with medical billing services often discover that professional revenue cycle management enhances forecasting accuracy through disciplined cycle billing implementation.
Enhanced Working Capital Management
Consistent cash inflows eliminate the need for expensive short-term financing arrangements that many practices use to bridge gaps between concentrated payment periods. Better working capital management translates directly to:
- Reduced interest expenses on credit lines
- Earlier payment discount opportunities with suppliers
- Stronger negotiating positions with vendors
- Greater financial flexibility during slow periods
- Improved creditworthiness for future financing needs
These financial benefits compound over time, creating measurable improvements in practice profitability and sustainability.
Coordinating Cycle Billing with Insurance Verification
Effective cycle billing medical strategies align statement distribution with insurance verification workflows. The relationship between these two revenue cycle components significantly impacts collection success.
Practices should coordinate eligibility verification services with their billing cycles to ensure accurate patient responsibility calculations before statements generate. This coordination prevents the need for corrected statements and reduces patient confusion about amounts owed.
Pre-Statement Verification Protocols
Establishing verification checkpoints before each billing cycle generates statements reduces errors and improves first-pass collection rates:
- Insurance eligibility confirmation within 48 hours of billing cycle date
- Benefit verification for high-dollar procedures before statement generation
- Coordination of benefits review for patients with multiple insurance policies
- Patient responsibility calculation based on current coverage information
- Balance verification against payment posting records
These protocols ensure statements reflect accurate patient obligations, reducing the likelihood of disputes and payment delays.
Measuring Long-Term Success of Cycle Billing Implementation
Evaluating whether cycle billing medical programs deliver sustained value requires ongoing assessment beyond initial implementation metrics.
Quarterly Performance Reviews
Establish regular review sessions examining:
Financial Indicators:
- Total collections compared to prior periods
- Days in accounts receivable trends
- Bad debt write-off percentages
- Collection cost per dollar collected
- Revenue cycle length from service to payment
Operational Metrics:
- Staff productivity measurements
- Overtime requirements
- Error rates in statement processing
- Patient inquiry volumes
- Statement generation costs
Patient Satisfaction Scores:
- Billing-related complaints
- Payment plan enrollment rates
- Online payment portal usage
- Survey responses regarding billing clarity
- Patient retention rates
Comprehensive assessment reveals whether cycle billing continues delivering expected benefits or requires refinement. Many practices discover that periodic adjustments to cycle assignments optimize performance as patient populations and payer mixes evolve.
Scaling Cycle Billing Across Growing Practices
Medical practices experiencing growth must ensure their cycle billing medical systems scale appropriately. What works for a single-location practice with 2,000 active patients may require modification when expanding to multiple locations or 10,000 patients.
Growth Accommodation Strategies
Adding billing cycles provides one scaling approach. Practices might begin with weekly billing cycles (four per month) and expand to daily cycles as patient volumes increase. This granular approach maintains manageable workloads even with substantial growth.
Technology upgrades often become necessary as practices scale. Entry-level billing systems may lack the sophisticated automation required for complex multi-location cycle billing operations. Investing in enterprise-grade platforms supports growth without compromising billing efficiency.
Outsourcing considerations emerge when internal resources cannot manage increased billing complexity. Professional revenue cycle management providers bring specialized expertise in managing high-volume cycle billing operations while maintaining accuracy and compliance.
Organizations exploring medical billing services for small practices often discover that outsourcing enables cycle billing implementation without significant internal resource investment.
Best Practices for Sustained Cycle Billing Excellence
Maintaining high performance requires ongoing attention to process refinement and staff development. Leading practices embrace continuous improvement methodologies applied to their cycle billing medical operations.
Documentation and Process Standardization
Create comprehensive procedure documentation covering:
- Cycle assignment protocols for new patients
- Exception handling procedures for unusual billing situations
- Quality control checkpoints before statement generation
- Patient communication scripts addressing cycle-related questions
- System troubleshooting guides for common technical issues
Standardized processes reduce variability and ensure consistent performance regardless of which staff members handle specific billing tasks.
Continuous Staff Training
Billing regulations, payer requirements, and best practices evolve constantly. Regular training sessions keep team members current on:
- Compliance updates affecting billing cycles
- New software features enhancing cycle management
- Patient communication techniques
- Error prevention strategies
- Performance optimization approaches
Investing in staff development directly improves billing accuracy and collection effectiveness across all cycles.
Patient Education Initiatives
Proactive patient education reduces confusion and improves payment compliance. Effective initiatives include:
- New patient orientation materials explaining billing cycles
- Portal demonstrations showing where to find statements online
- Payment option guides describing available payment methods
- Insurance coordination information helping patients understand their responsibilities
- Financial assistance program descriptions for patients experiencing hardship
Well-informed patients pay more promptly and require fewer customer service interactions, improving efficiency across the entire revenue cycle.
Cycle billing medical practices implement creates measurable improvements in cash flow consistency, administrative efficiency, and patient satisfaction while supporting better financial planning and scalability. The strategic distribution of billing statements throughout each month eliminates workflow bottlenecks and enables more predictable revenue patterns. Whether you're operating a small practice or managing a multi-location healthcare organization, professional expertise can help you implement and optimize cycle billing strategies tailored to your specific needs. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to maximize your practice's financial performance through proven methodologies including cycle billing implementation, claims processing, denial management, and eligibility verification, all backed by HIPAA-compliant processes and transparent communication.