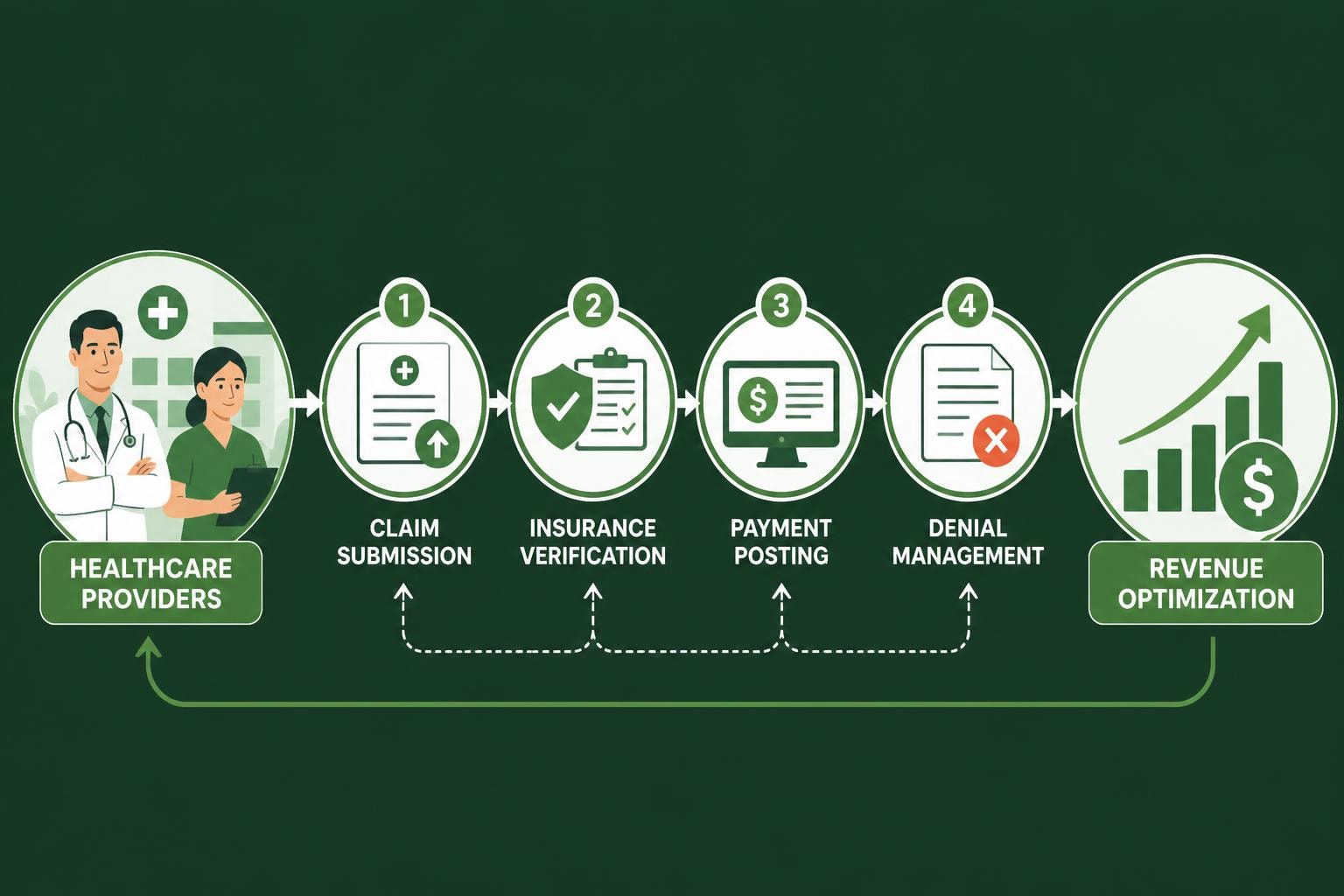
Medical billing offices serve as the financial backbone of healthcare organizations, transforming clinical documentation into revenue while navigating the complexities of insurance claims, regulatory compliance, and reimbursement cycles. These specialized departments or outsourced service providers manage every aspect of the revenue cycle, from patient registration and insurance verification to final payment posting and accounts receivable follow-up. As healthcare reimbursement models grow increasingly complex, the role of medical billing offices has expanded beyond simple claim submission to encompass sophisticated denial management, compliance monitoring, and financial analytics that directly impact provider profitability and operational sustainability.
The Core Functions of Medical Billing Offices
Medical billing offices operate as comprehensive revenue cycle hubs, coordinating multiple interconnected processes that ensure healthcare providers receive appropriate compensation for services rendered. These offices handle patient demographic verification, insurance eligibility checks, charge capture, coding review, claim submission, payment posting, and denial resolution.
The foundation of effective billing begins with accurate patient information collection and insurance eligibility verification, which prevents costly claim rejections before submission. Medical billing offices verify coverage details, copayment requirements, deductible status, and authorization needs to establish clear financial responsibility from the outset.
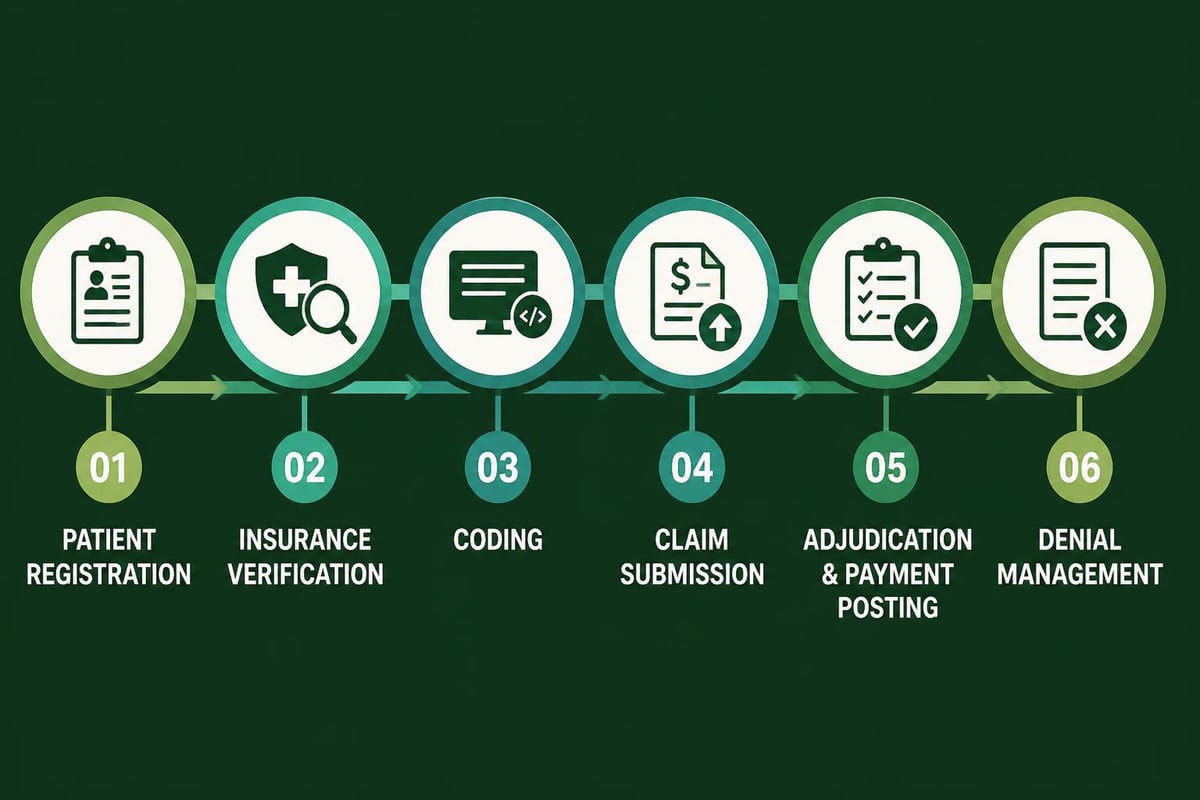
Documentation and Charge Capture
Comprehensive documentation forms the cornerstone of successful revenue cycle management. Medical billing offices work closely with clinical staff to ensure that all billable services are accurately captured and appropriately coded according to current CPT, ICD-10, and HCPCS standards.
Charge capture processes vary depending on practice size and specialty, but all medical billing offices must establish systematic protocols for:
- Reviewing clinical notes for billable procedures and diagnoses
- Verifying modifier usage for accurate service representation
- Confirming medical necessity documentation
- Ensuring timely charge entry to prevent aging issues
- Cross-referencing services with payer-specific requirements
Following medical billing best practices significantly reduces claim denials and accelerates reimbursement timelines.
Compliance Standards Governing Medical Billing Offices
Medical billing offices operate within a complex regulatory framework that includes HIPAA privacy requirements, fraud and abuse prevention laws, and payer-specific guidelines. Maintaining compliance protects healthcare organizations from financial penalties, legal liability, and reputation damage while ensuring ethical billing practices.
Understanding medical billing compliance requirements helps organizations implement effective policies and training programs. Compliance encompasses proper documentation standards, accurate coding practices, appropriate use of modifiers, and transparent communication with patients regarding financial responsibilities.
| Compliance Area | Key Requirements | Consequences of Non-Compliance |
|---|---|---|
| HIPAA Privacy | Protected health information security | Fines up to $50,000 per violation |
| Coding Accuracy | Correct CPT/ICD-10 assignment | Claim denials, audit penalties |
| Fraud Prevention | Truthful claim submission | Criminal prosecution, exclusion |
| Documentation | Medical necessity substantiation | Recoupment, legal liability |
Audit Preparedness and Internal Controls
Medical billing offices must maintain robust internal controls and audit-ready documentation systems. Regular internal audits identify coding inconsistencies, billing pattern anomalies, and compliance gaps before external reviewers discover them.
Effective audit preparation includes maintaining complete medical records, ensuring coder certification and continuing education, implementing quality assurance reviews, and documenting all billing decisions and policy interpretations. Many healthcare organizations partner with specialized providers offering medical coding audit services to identify vulnerabilities proactively.
Technology Infrastructure Supporting Medical Billing Offices
Modern medical billing offices leverage sophisticated software platforms that integrate practice management, electronic health records, clearinghouse connectivity, and financial analytics. These systems automate routine tasks, reduce manual errors, and provide real-time visibility into revenue cycle performance.
Electronic claim submission through secure clearinghouses enables rapid payer communication and automated eligibility verification. Most medical billing offices utilize integrated platforms that scrub claims for errors before submission, dramatically reducing rejection rates and accelerating payment cycles.
Advanced billing systems offer features including:
- Automated appointment reminders and patient communication
- Real-time eligibility verification at scheduling
- Integrated coding assistance and compliance checking
- Electronic remittance advice (ERA) processing
- Comprehensive reporting and analytics dashboards
- Denial tracking and workflow management
Understanding what is ERA in medical billing helps billing staff maximize automation benefits and reduce manual payment posting time.
Denial Management Strategies for Medical Billing Offices
Claim denials represent one of the most significant challenges facing medical billing offices, with industry averages indicating that 5-10% of claims experience initial denial. Effective denial management requires systematic identification, categorization, analysis, and resolution of rejected claims.
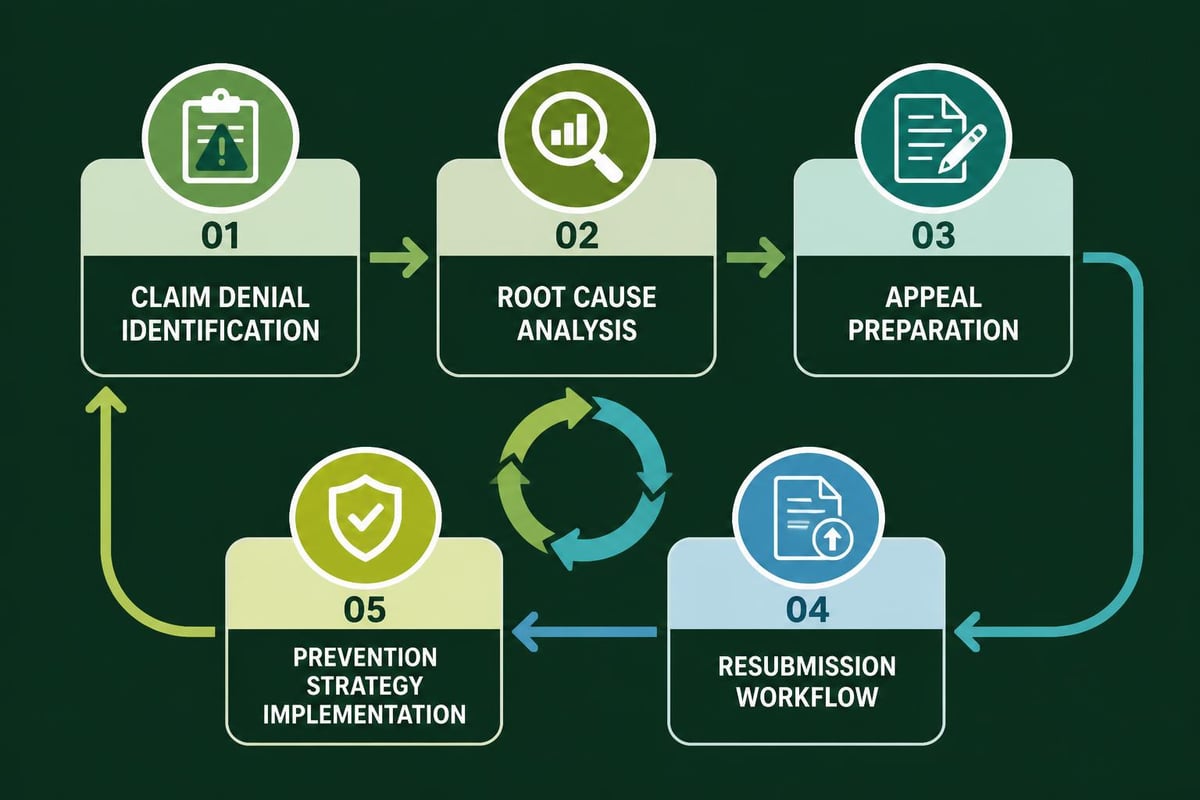
Medical billing offices must distinguish between preventable denials caused by submission errors and non-preventable denials resulting from coverage limitations or medical necessity determinations. This categorization enables targeted process improvements that address root causes rather than symptoms.
Building an Effective Denial Prevention Program
Prevention proves more cost-effective than correction when addressing claim denials. Medical billing offices should implement front-end processes that verify coverage, confirm authorization requirements, and validate coding accuracy before claim submission.
The denial management process encompasses both reactive appeals and proactive prevention strategies. Successful programs track denial reasons, measure resolution timeframes, calculate financial impact, and implement corrective actions based on data-driven insights.
Implementing best practices from the revenue cycle checklist helps medical billing offices establish comprehensive denial management workflows.
Accounts Receivable Management in Medical Billing Offices
Effective accounts receivable management directly impacts healthcare organization cash flow and financial stability. Medical billing offices monitor aging reports, follow up on outstanding claims, and implement collection strategies that balance revenue optimization with patient relationships.
Best practices for managing accounts receivable in medical billing include establishing clear follow-up protocols, prioritizing high-value claims, maintaining consistent payer communication, and implementing patient-friendly payment plans.
Key Performance Indicators for Medical Billing Offices
Successful medical billing offices track specific metrics that reveal revenue cycle health and identify improvement opportunities. These KPIs provide actionable insights into operational efficiency and financial performance.
| Metric | Target Range | What It Measures |
|---|---|---|
| Days in A/R | 30-40 days | Collection efficiency |
| Clean Claim Rate | >95% | Submission accuracy |
| Denial Rate | <5% | Quality and compliance |
| Collection Ratio | >95% | Revenue realization |
| Cost to Collect | <3% | Operational efficiency |
Medical billing offices should review these metrics monthly, comparing performance against industry benchmarks and historical trends. Significant deviations warrant immediate investigation and corrective action.
Specialized Billing Requirements by Healthcare Specialty
Different medical specialties present unique billing challenges that require specialized knowledge and process adaptations. Medical billing offices serving multiple specialties must maintain expertise across varying documentation requirements, coding conventions, and payer policies.
Cardiology practices face complex bundling rules, modifier requirements for multiple procedures, and specialized authorization protocols. Organizations seeking cardiology medical billing expertise benefit from billing professionals who understand specialty-specific nuances.
Primary care offices emphasize preventive service billing, annual wellness visit documentation, and chronic care management reimbursement. Understanding requirements like the annual wellness visit CPT code ensures appropriate revenue capture for preventive services.
Adapting Processes for Practice Size and Type
Small practices often struggle with the overhead costs of maintaining full-service in-house medical billing offices. Many discover that medical billing services for small practices provide cost-effective access to specialized expertise without the expense of dedicated staff.
Larger healthcare systems benefit from economies of scale but face challenges coordinating billing across multiple locations, specialties, and electronic systems. Centralized medical billing offices must establish standardized processes while accommodating location-specific payer contracts and operational requirements.
Staff Training and Development in Medical Billing Offices
The expertise of billing staff directly correlates with revenue cycle performance. Medical billing offices must invest in comprehensive training programs that address coding updates, regulatory changes, payer policy modifications, and technology platform enhancements.
Understanding the medical billing process from end to end enables billing staff to identify process improvement opportunities and troubleshoot issues effectively. Comprehensive training should cover patient registration, charge entry, claims submission, payment posting, denial management, and patient communication.
Professional development opportunities include:
- Certification Programs: AAPC and AHIMA credentials demonstrate coding expertise
- Payer Education: Regular updates on coverage policies and claim requirements
- Compliance Training: Annual HIPAA and fraud prevention education
- Technology Skills: Platform-specific training and workflow optimization
- Communication Techniques: Patient interaction and conflict resolution
Medical billing offices benefit from creating specialized roles focused on specific revenue cycle components, allowing staff to develop deep expertise in areas like eligibility verification, denial appeals, or payment posting.
The Future of Medical Billing Offices
Medical billing offices continue evolving in response to technological advancement, regulatory changes, and shifting reimbursement models. Artificial intelligence and machine learning applications promise to automate routine tasks, predict denial patterns, and optimize coding accuracy.
Value-based reimbursement models require medical billing offices to track quality metrics, coordinate care documentation, and demonstrate patient outcomes alongside traditional fee-for-service billing. This dual responsibility demands expanded skillsets and more sophisticated reporting capabilities.
Telehealth expansion introduces new billing scenarios, modifier requirements, and documentation standards that medical billing offices must master. The distinction between place of service codes, synchronous versus asynchronous communication, and state-specific telehealth coverage policies creates additional complexity.
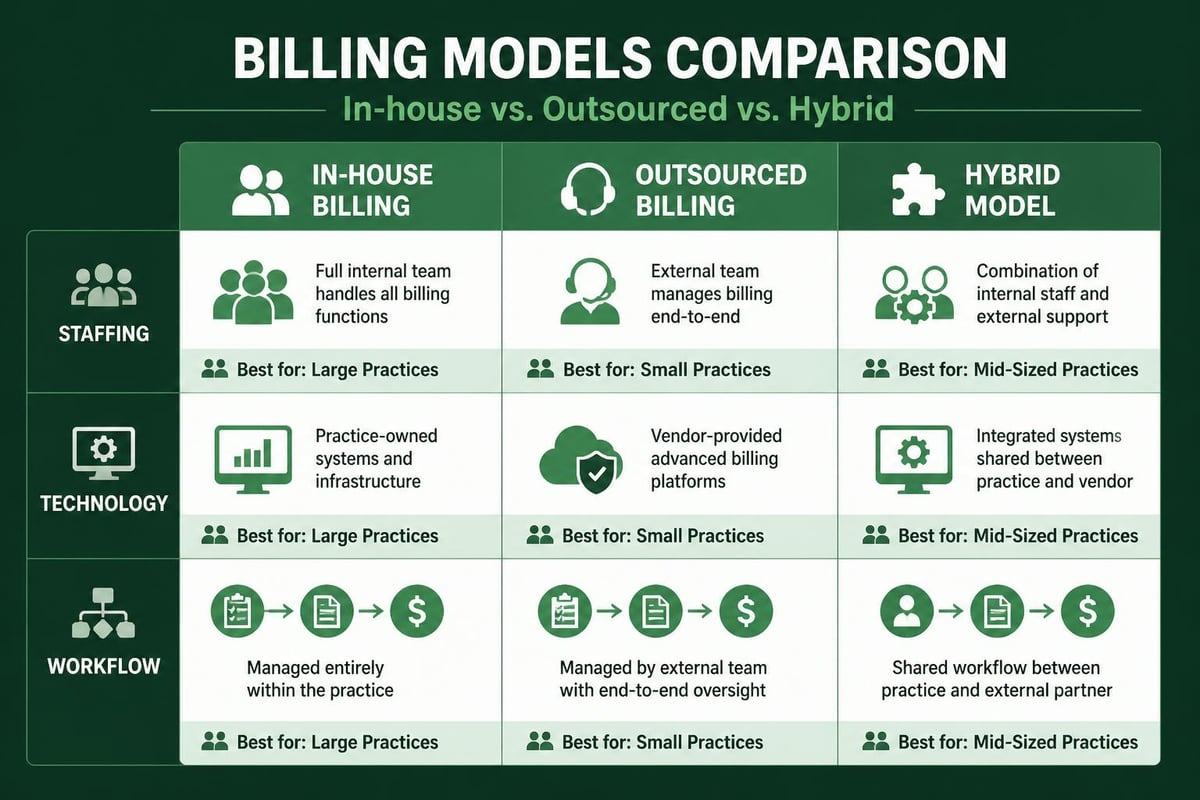
Selecting Between In-House and Outsourced Medical Billing Offices
Healthcare organizations face strategic decisions regarding whether to maintain in-house medical billing offices or partner with specialized service providers. Each approach offers distinct advantages depending on practice size, specialty focus, and operational priorities.
In-house medical billing offices provide direct oversight, immediate communication with clinical staff, and complete control over processes and priorities. Organizations with adequate volume to support dedicated billing staff often prefer maintaining internal departments.
Outsourced billing services deliver specialized expertise, scalable resources, and reduced overhead costs without capital investment in technology infrastructure. Evaluating top medical billing companies helps organizations identify partners aligned with their specific needs and values.
Critical Selection Criteria
Organizations evaluating outsourced billing partners should assess multiple factors beyond simple pricing considerations. Comprehensive evaluation includes:
- Industry experience and specialty expertise
- Technology platform capabilities and integration
- Compliance protocols and security measures
- Reporting transparency and data access
- Performance guarantees and contractual terms
- Client references and satisfaction metrics
The most successful partnerships develop when organizations clearly define expectations, establish measurable performance standards, and maintain regular communication regarding revenue cycle goals and challenges.
Geographic Considerations for Medical Billing Offices
Location impacts medical billing offices through state-specific regulations, regional payer prevalence, and local market dynamics. Practices operating in multiple states must navigate varying Medicaid programs, commercial payer networks, and regulatory requirements.
California practices contend with unique workers' compensation billing rules, while Arizona providers navigate AHCCCS requirements and tribal health program coordination. Organizations seeking medical billing services in California or medical billing coding in Arizona benefit from partners familiar with state-specific nuances.
Understanding regional payer mix helps medical billing offices prioritize credentialing efforts, optimize contracting strategies, and allocate resources effectively across different insurance programs and geographic markets.
Payment Posting Accuracy and Reconciliation
Payment posting represents a critical yet often underestimated function within medical billing offices. Accurate posting ensures proper credit application, identifies underpayments, reveals contractual adjustment patterns, and maintains clean accounts receivable aging.
Effective payment posting services reconcile remittance details against expected reimbursement, identify posting errors promptly, and maintain audit trails for financial review. Medical billing offices should implement dual verification for high-value payments and regular reconciliation between practice management systems and bank deposits.
Common payment posting challenges include managing multiple payment methods, correctly applying patient payments versus insurance payments, identifying and resolving duplicate payments, and handling coordination of benefits scenarios involving multiple payers.
Medical billing offices play an indispensable role in healthcare financial sustainability, requiring specialized expertise across coding, compliance, technology, and payer relations. Organizations seeking to optimize revenue cycle performance while maintaining compliance and operational efficiency benefit from partnering with experienced billing professionals who understand the nuances of modern healthcare reimbursement. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to maximize reimbursements, reduce administrative burden, and provide transparent financial insights that empower healthcare providers to focus on exceptional patient care while achieving sustainable financial performance.