Healthcare providers face mounting pressure to maintain financial stability while delivering exceptional patient care. The complexity of medical billing, insurance verification, claims processing, and reimbursement management requires sophisticated healthcare rcm solutions that can handle multiple touchpoints across the revenue cycle. As reimbursement models evolve and regulatory requirements become more stringent, practices of all sizes must adopt comprehensive strategies to optimize their financial operations and ensure sustainable growth.
Understanding the Core Components of Revenue Cycle Management
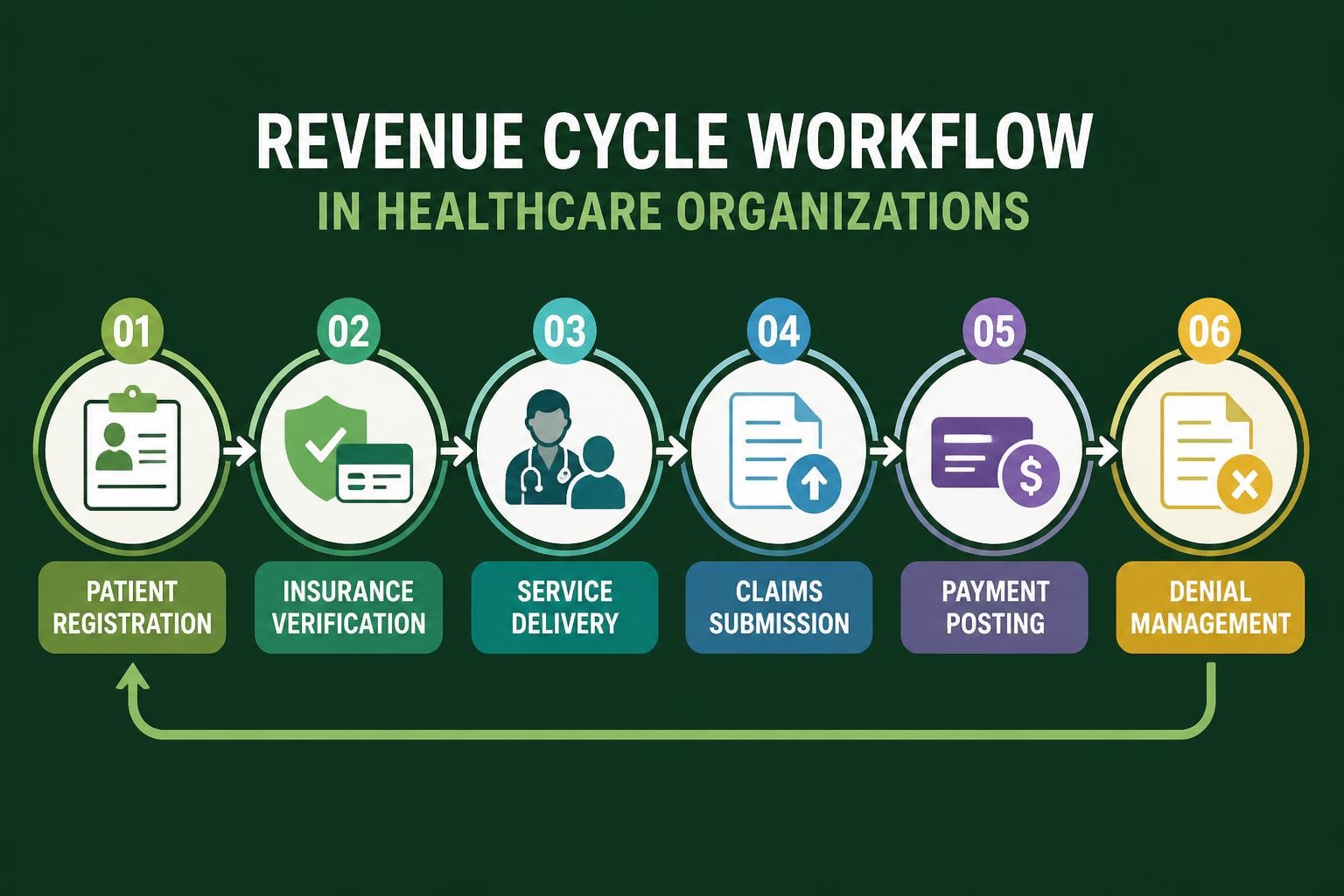
Revenue cycle management encompasses every administrative and clinical function that contributes to capturing, managing, and collecting patient service revenue. The process begins the moment a patient schedules an appointment and continues through final payment reconciliation. Healthcare revenue cycle management involves coordination between multiple departments, technology systems, and external partners.
Patient Access and Registration
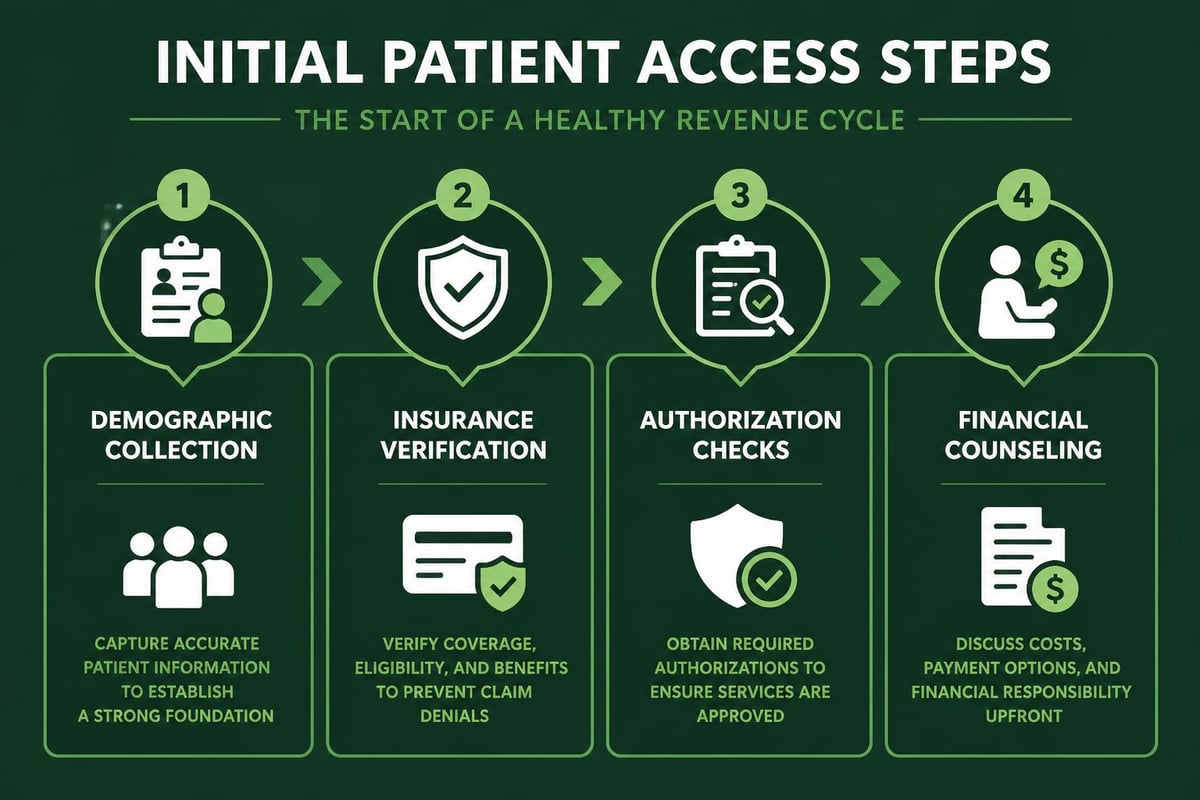
The foundation of effective healthcare rcm solutions starts with accurate patient information collection. This critical first step determines the success of all downstream processes.
Key elements of patient access include:
- Demographic information verification
- Insurance coverage confirmation
- Co-payment and deductible collection
- Patient consent documentation
- Authorization requirements identification
Front-end revenue cycle management sets the tone for the entire billing process. When registration staff collect complete and accurate information, the likelihood of claim denials decreases significantly. Many practices now leverage eligibility verification services to automate insurance coverage checks and reduce manual errors.
Medical Coding and Charge Capture
Accurate medical coding translates clinical services into standardized codes that payers recognize and reimburse. This process requires extensive knowledge of CPT, ICD-10, and HCPCS coding systems.
Proper charge capture ensures that every billable service receives appropriate documentation and coding. Missing charges represent lost revenue that practices can never recover. Healthcare rcm solutions must include robust charge capture mechanisms that integrate with electronic health record systems and provide real-time feedback to clinical staff.
| Coding Type | Purpose | Common Challenges |
|---|---|---|
| CPT Codes | Procedure and service descriptions | Selecting appropriate specificity level |
| ICD-10 Codes | Diagnosis documentation | Medical necessity justification |
| HCPCS Codes | Supplies and equipment | Limited payer coverage policies |
| Modifiers | Service detail clarification | Incorrect modifier application |
Skilled coders serve as the bridge between clinical documentation and financial reimbursement. They must stay current with coding updates, payer policies, and regulatory changes that impact proper code assignment.
Claims Submission and Processing Strategies
Submitting clean claims on the first attempt dramatically improves cash flow and reduces administrative burden. Healthcare rcm solutions must incorporate thorough claim scrubbing processes that identify errors before submission to payers.
Electronic Claims Management
Electronic claim submission has become the industry standard, offering faster processing times and reduced error rates compared to paper submissions. Medical claim submission services leverage sophisticated software platforms that validate claim data against payer-specific requirements.
Modern claims management systems check for:
- Missing or invalid information fields
- Coding inconsistencies and contradictions
- Medical necessity documentation gaps
- Duplicate claim submissions
- Prior authorization compliance
The American Hospital Association emphasizes that successful revenue cycle management requires seamless integration between clinical and financial systems. This integration allows for real-time data exchange that supports accurate claim creation and submission.
Payer Communication and Follow-Up
Maintaining open communication channels with insurance companies helps resolve claim issues quickly and prevents unnecessary denials. Effective healthcare rcm solutions include structured processes for tracking claim status and following up on delayed payments.
Practices should establish specific timelines for claim follow-up activities. Generally, claims should be checked 7-10 days after submission to confirm receipt and processing status. Any claims remaining unpaid after 30 days require intensive investigation and outreach.
Denial Management and Appeals Processes
Even with the best prevention strategies, claim denials remain an inevitable part of healthcare billing. The difference between financially successful practices and struggling ones often lies in how effectively they manage and overturn denials.
Common Denial Categories
Understanding denial patterns helps practices address root causes and prevent future occurrences. Healthcare rcm solutions should include comprehensive denial tracking and reporting capabilities.
Frequent denial reasons include:
- Registration and eligibility errors
- Authorization and referral deficiencies
- Coding inaccuracies or lack of specificity
- Medical necessity documentation gaps
- Timely filing violations
- Duplicate claim submissions
The denial management process requires systematic analysis of each rejection to determine whether the denial warrants an appeal or represents a write-off opportunity. Not all denials deserve equal attention, and practices must prioritize high-value claims that offer the best return on investment for appeal efforts.
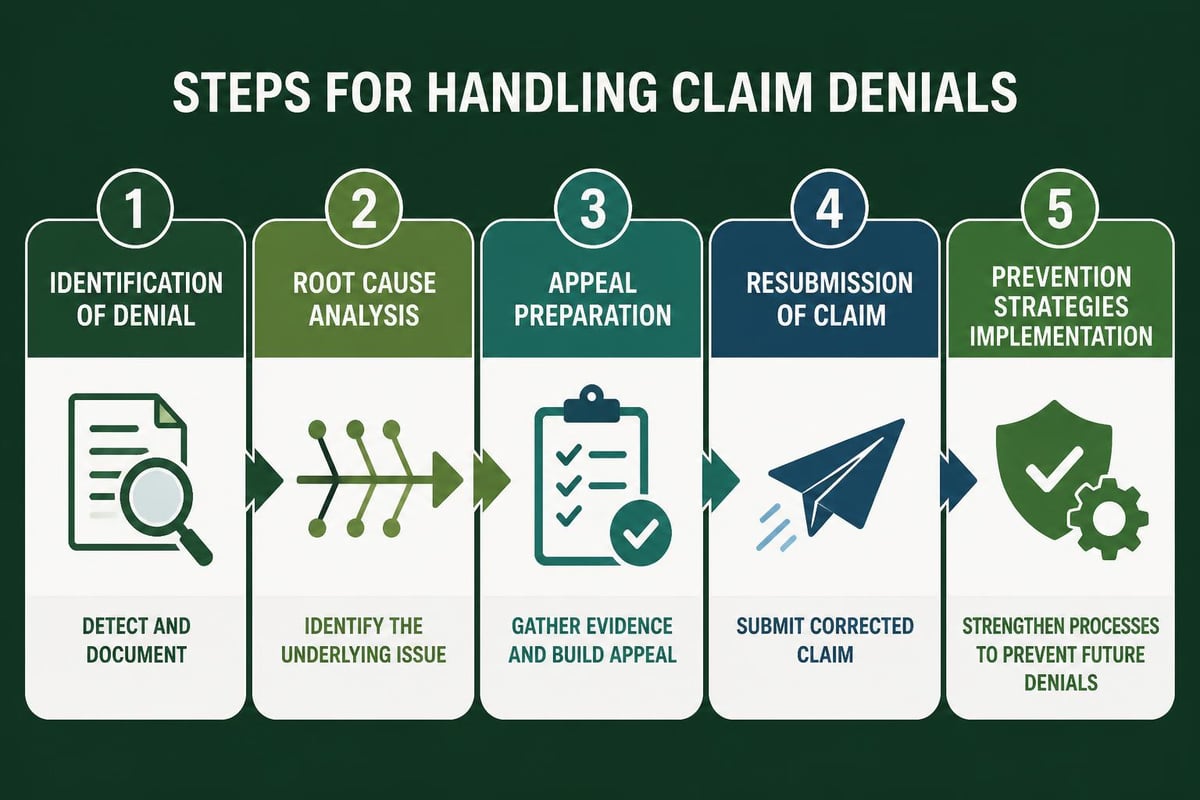
Building an Effective Appeals Strategy
Successful appeals require compelling documentation that addresses the specific denial reason cited by the payer. Generic appeal letters rarely succeed in overturning denials.
Appeals should include:
- Clear identification of the claim in question
- Specific denial reason and code
- Detailed explanation addressing the denial
- Supporting clinical documentation
- Relevant policy or contract language
- Requested action and timeline
Organizations that implement dedicated denial management services often see significant improvements in their appeal success rates and overall revenue recovery.
Payment Posting and Reconciliation
Accurate payment posting ensures that patient accounts reflect all payments, adjustments, and outstanding balances. This seemingly simple task requires attention to detail and understanding of complex payer remittance rules.
Electronic Remittance Advice Processing
Electronic remittance advice (ERA) documents provide detailed payment information from insurance companies. Healthcare rcm solutions that automate ERA processing reduce manual data entry and accelerate the payment posting timeline.
Payment posting staff must understand contractual adjustments, coordination of benefits, and patient responsibility calculations. Errors in these areas can lead to incorrect patient statements and collection challenges.
| Payment Component | Description | Action Required |
|---|---|---|
| Paid Amount | Insurance payment received | Post to patient account |
| Contractual Adjustment | Write-off per contract | Apply adjustment code |
| Deductible | Patient responsibility | Bill patient |
| Co-insurance | Patient percentage share | Bill patient |
| Denied Amount | Claim rejection | Route to denial management |
The RCM process relies on accurate payment posting to maintain clean accounts receivable and generate appropriate patient statements. Any discrepancies between expected and received payments require investigation and resolution.
Patient Collections and Statements
With increasing patient financial responsibility through high-deductible health plans, collecting patient portions has become a critical revenue cycle function. Healthcare rcm solutions must support flexible payment options and clear communication with patients about their financial obligations.
Effective patient collection strategies include upfront payment estimation, point-of-service collections, and convenient payment plans. Practices that prioritize transparency and offer multiple payment channels typically achieve higher collection rates than those relying solely on traditional billing statements.
Technology Integration and Automation
Modern healthcare rcm solutions leverage advanced technology to streamline workflows, reduce manual tasks, and improve accuracy across the revenue cycle. Revenue cycle management software continues to evolve with artificial intelligence and machine learning capabilities that predict denial risks and optimize billing processes.
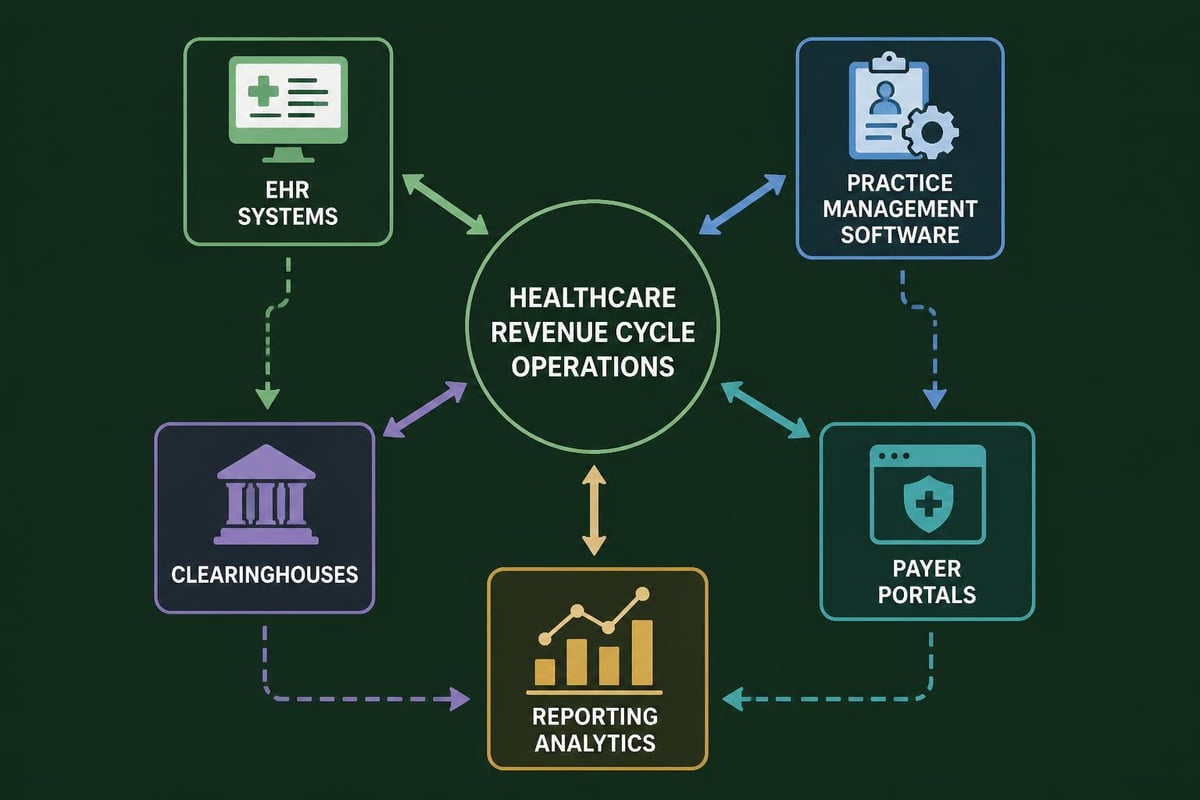
Practice Management System Integration
Seamless integration between practice management systems, electronic health records, and billing platforms eliminates duplicate data entry and reduces errors. Healthcare organizations benefit from unified systems that share information across clinical and financial functions.
Integration capabilities to prioritize include:
- Real-time eligibility verification
- Automated charge capture from clinical documentation
- Electronic claim submission and tracking
- ERA auto-posting functionality
- Patient portal payment processing
Organizations using integrated systems report fewer billing errors, faster reimbursement cycles, and improved staff productivity compared to those managing disconnected platforms.
Analytics and Performance Monitoring
Data-driven decision-making separates high-performing practices from average ones. Healthcare rcm solutions should provide comprehensive reporting and analytics that track key performance indicators and identify improvement opportunities.
Essential metrics to monitor include:
- Days in accounts receivable
- Clean claim rate
- Denial rate by payer and reason
- Collection rate
- Net collection percentage
- Cost to collect
Regular performance review allows practices to identify trends, benchmark against industry standards, and implement targeted improvements. Organizations that establish monthly or quarterly review cycles maintain better financial health than those conducting sporadic assessments.
Compliance and Regulatory Considerations
Healthcare providers operate in one of the most heavily regulated industries, with strict requirements governing patient privacy, billing practices, and documentation standards. Effective healthcare rcm solutions incorporate compliance safeguards throughout all processes.
HIPAA Compliance Requirements
The Health Insurance Portability and Accountability Act establishes strict standards for protecting patient health information. Revenue cycle operations handle sensitive data daily, requiring robust security measures and staff training.
HIPAA compliance in RCM includes:
- Access controls limiting data exposure
- Encryption of electronic transmissions
- Audit trails tracking system access
- Business associate agreements with vendors
- Regular security risk assessments
- Staff training and awareness programs
Violations can result in significant penalties and reputational damage. Organizations must maintain comprehensive compliance programs that address both technical safeguards and operational policies.
Coding and Billing Regulations
Federal and state regulations govern proper coding and billing practices. Understanding these requirements prevents inadvertent violations that could trigger audits or fraud investigations.
Key regulatory considerations include:
- Anti-kickback statute compliance
- Stark Law self-referral prohibitions
- False Claims Act requirements
- National Correct Coding Initiative edits
- Local coverage determination policies
Staying current with regulatory changes requires ongoing education and system updates. Healthcare rcm solutions should include compliance alerts and documentation requirements that help providers maintain adherence to current standards.
Outsourcing Versus In-House Management
Healthcare organizations face critical decisions about whether to manage revenue cycle functions internally or partner with external service providers. Both approaches offer distinct advantages depending on practice size, specialty, and strategic priorities.
Benefits of Professional RCM Services
Many practices find that partnering with experienced revenue cycle management providers delivers superior financial results compared to internal operations. Specialized firms bring expertise, technology, and economies of scale that smaller practices struggle to replicate.
| Consideration | In-House | Outsourced Services |
|---|---|---|
| Initial Investment | High (staff, systems, training) | Low (service fees only) |
| Scalability | Limited by staff capacity | Flexible to volume changes |
| Expertise | Dependent on staff knowledge | Access to specialists |
| Technology | Must purchase and maintain | Included in services |
| Focus | Divided between clinical and billing | Practice focuses on patient care |
Organizations utilizing medical billing services often report improved collection rates, reduced denial rates, and decreased administrative burden on clinical staff. These improvements allow providers to focus on patient care while financial experts handle billing complexities.
Evaluating Service Providers
Selecting the right revenue cycle management partner requires careful evaluation of capabilities, experience, and cultural fit. Practices should conduct thorough due diligence before making this important decision.
Questions to ask potential providers:
- What is your experience in our specialty?
- How do you handle HIPAA compliance and data security?
- What technology platforms do you use?
- How do you measure and report performance?
- What is your fee structure and pricing model?
- Can you provide references from similar practices?
The best partnerships involve transparent communication, regular performance reviews, and alignment on goals and expectations. Organizations should view their RCM provider as a strategic partner rather than simply a vendor relationship.
Specialty-Specific Considerations
Different medical specialties face unique revenue cycle challenges that require tailored approaches. Healthcare rcm solutions must account for specialty-specific coding requirements, payer policies, and reimbursement models.
High-Complexity Specialties
Certain specialties involve particularly complex billing scenarios that demand specialized expertise. Cardiology, oncology, and surgical practices often deal with high-dollar claims, extensive documentation requirements, and intricate coding rules.
These specialties benefit from RCM providers with specific experience and knowledge in their field. Generic billing approaches often miss important nuances that impact reimbursement and compliance.
Primary Care and Multi-Specialty Practices
Primary care practices face different challenges, including high patient volumes, diverse payer mixes, and value-based payment model participation. Healthcare rcm solutions for these organizations must handle large transaction volumes efficiently while supporting quality reporting requirements.
Multi-specialty practices add another layer of complexity with different coding systems, payer contracts, and workflow requirements across departments. Unified RCM platforms that accommodate specialty variations while maintaining consistent processes deliver the best results.
Future Trends in Revenue Cycle Management
The healthcare industry continues to evolve rapidly, with emerging trends reshaping how organizations approach revenue cycle management. Staying ahead of these changes positions practices for long-term success.
Value-Based Care Integration
The shift from fee-for-service to value-based reimbursement models fundamentally changes revenue cycle requirements. Healthcare rcm solutions must now track quality metrics, coordinate care across settings, and document outcomes in addition to traditional billing functions.
Value-based contracts require:
- Quality measure reporting capabilities
- Population health management tools
- Risk stratification and analytics
- Care coordination documentation
- Alternative payment model reconciliation
Organizations participating in accountable care organizations, bundled payments, or other alternative payment models need RCM systems that support both traditional and value-based reimbursement tracking.
Artificial Intelligence and Automation
Artificial intelligence applications in revenue cycle management continue to expand, offering opportunities for significant efficiency gains. Predictive analytics can identify claims at high risk for denial before submission, allowing for proactive intervention.
Machine learning algorithms improve over time, learning from historical data to optimize coding accuracy, predict payment patterns, and prioritize work queues. As these technologies mature, they will increasingly handle routine tasks while human experts focus on complex exceptions and strategic decisions.
Patient Financial Experience
Consumerism in healthcare continues to grow, with patients expecting the same convenient, transparent financial experiences they receive in other industries. Healthcare rcm solutions must evolve to meet these expectations through user-friendly patient portals, mobile payment options, and clear cost estimates.
Organizations that prioritize patient financial experience see benefits beyond improved collections. Patient satisfaction scores increase when billing processes are transparent and convenient, contributing to better online reviews and referral patterns.
Key Performance Indicators for Success
Measuring revenue cycle performance provides objective data for identifying strengths and improvement opportunities. Healthcare rcm solutions should support comprehensive tracking of metrics that drive financial success.
Financial Metrics
Core financial KPIs reveal the overall health of revenue cycle operations and highlight areas requiring attention.
Critical financial indicators include:
- Days in A/R: Measures how quickly practice collects payments
- Net collection rate: Percentage of collectible revenue actually received
- Charge lag: Time between service delivery and charge entry
- Payment lag: Time between claim submission and payment receipt
- Bad debt percentage: Uncollectible patient balances written off
Organizations should establish baseline measurements and set improvement targets for each metric. Regular monitoring allows for early identification of negative trends before they significantly impact cash flow.
Operational Metrics
Operational KPIs track process efficiency and quality, providing insights into workflow effectiveness and staff productivity.
Important operational measures include:
- Clean claim rate (target: >95%)
- Denial rate (target: <5%)
- Appeal success rate (target: >50%)
- Point-of-service collection rate
- Patient statement effectiveness
Benchmarking these metrics against industry standards helps organizations assess their performance relative to peers and identify best practices worth adopting.
Building a Culture of Revenue Excellence
Technology and processes matter, but organizational culture ultimately determines revenue cycle success. Healthcare rcm solutions work best when supported by teams committed to continuous improvement and financial responsibility.
Staff Training and Development
Investing in ongoing education ensures staff maintain current knowledge of coding updates, payer policies, and regulatory requirements. Regular training sessions, certification support, and professional development opportunities demonstrate organizational commitment to employee growth.
Cross-training team members across multiple revenue cycle functions builds flexibility and deeper understanding of how individual actions impact overall performance. When front desk staff understand how registration errors affect downstream billing, they become more diligent about data accuracy.
Collaboration Between Clinical and Financial Teams
Breaking down silos between clinical and administrative functions improves revenue cycle outcomes. Physicians and clinical staff who understand coding and documentation requirements provide better support for accurate billing.
Regular meetings between clinical leaders and revenue cycle management teams facilitate communication about documentation improvements, coding updates, and payer policy changes. This collaboration ensures clinical decisions consider both quality of care and financial implications.
Optimizing healthcare revenue cycle management requires comprehensive strategies that address every touchpoint from patient registration through final payment reconciliation. By implementing robust processes, leveraging advanced technology, and maintaining focus on key performance metrics, healthcare organizations can achieve sustainable financial success while continuing to deliver exceptional patient care. Greenhive Billing Solutions provides comprehensive revenue cycle management services specifically designed to help healthcare providers maximize reimbursements, reduce denials, and streamline operations, allowing your practice to focus on what matters most: delivering quality patient care.