Healthcare organizations across the United States face mounting pressure to optimize their financial operations while maintaining quality patient care. Optum revenue cycle management has emerged as a leading solution that addresses these challenges through comprehensive, technology-driven approaches. Understanding how major players like Optum structure their RCM services provides valuable insights for healthcare providers seeking to enhance their own revenue cycle performance, whether through outsourcing partnerships or by adopting proven industry methodologies.
Understanding Optum Revenue Cycle Management Solutions
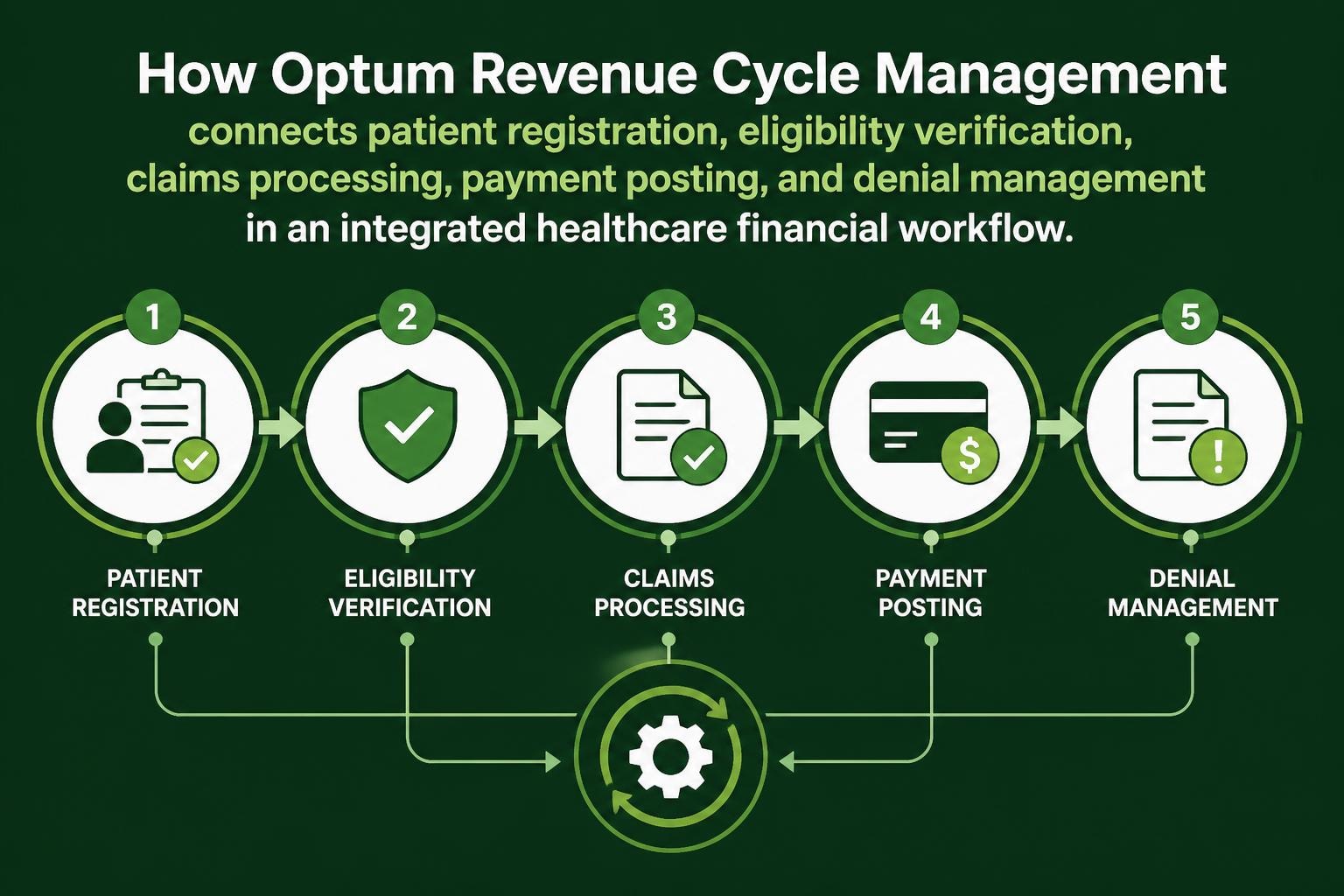
Optum revenue cycle management represents a comprehensive approach to healthcare financial operations, encompassing everything from patient registration through final payment collection. The Optum RCM platform integrates multiple touchpoints across the revenue cycle to create seamless workflows that reduce administrative burden while maximizing reimbursement.
Healthcare providers partnering with full-service RCM organizations gain access to similar capabilities that mirror the sophisticated systems employed by industry leaders. These services typically include:
- Patient access and registration management
- Insurance eligibility verification and benefits discovery
- Medical coding and charge capture
- Claims submission and management
- Payment posting and reconciliation
- Denial management and appeals processing
- Patient billing and collections
- Analytics and reporting
The Technology Foundation
Modern optum revenue cycle management relies heavily on advanced technology platforms that automate routine tasks and provide real-time visibility into financial performance. The introduction of AI-powered platforms like Optum Integrity One demonstrates the industry's shift toward intelligent automation that improves clinical documentation and coding accuracy while reducing administrative workload.
Healthcare providers working with specialized RCM service providers benefit from teams that utilize industry-standard platforms and adapt to existing client systems. This flexibility ensures continuity while introducing best-practice workflows that drive measurable improvements in key performance indicators.
Key Components of Effective Revenue Cycle Management
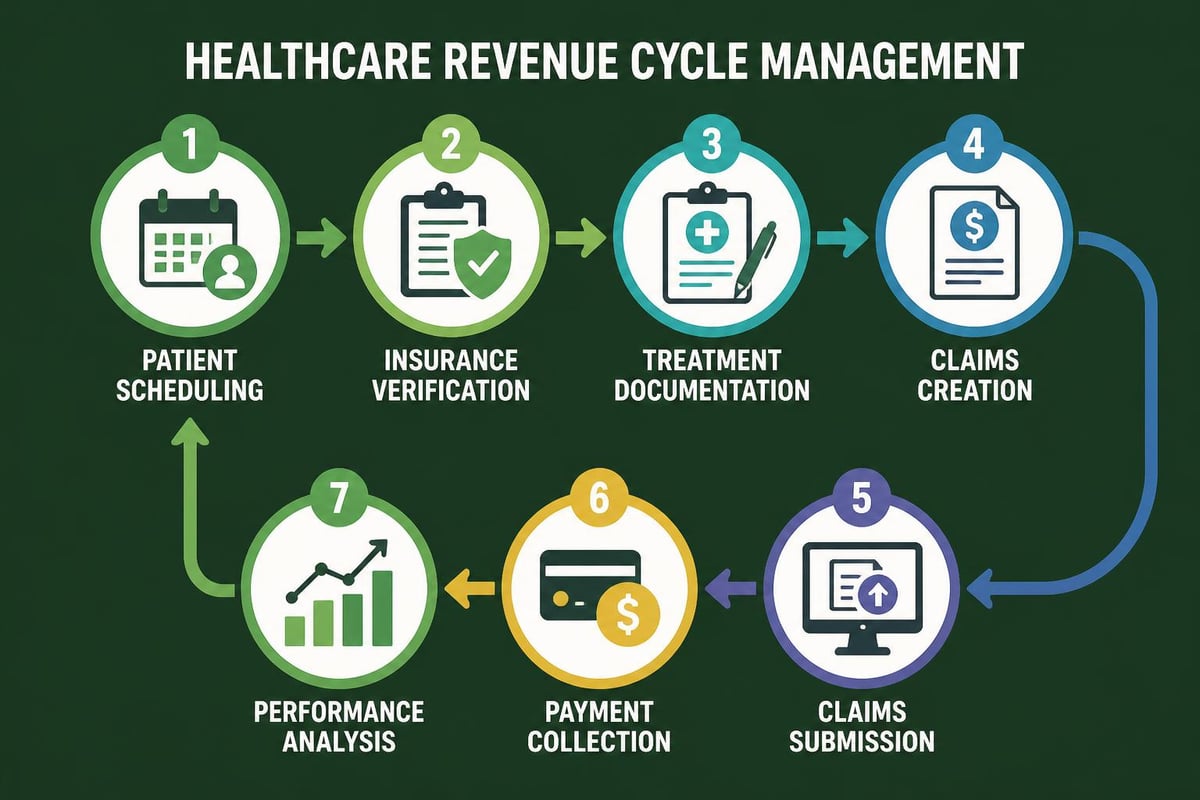
Breaking down optum revenue cycle management into its core components reveals the intricate processes that determine financial success for healthcare organizations. Each stage requires precise execution and coordination to prevent revenue leakage and ensure optimal reimbursement.
Front-End Revenue Cycle Operations
The front-end of the revenue cycle establishes the foundation for successful claims processing. Patient registration accuracy directly impacts downstream processes, making this initial touchpoint critical for financial performance.
Patient Registration Best Practices:
- Verify patient demographic information at every encounter
- Confirm insurance coverage through real-time eligibility verification services
- Collect accurate insurance card copies and identification
- Estimate patient financial responsibility upfront
- Secure payment arrangements before service delivery
Organizations that implement robust front-end processes experience significantly fewer claim denials and accelerated payment cycles. Insurance verification best practices emphasize the importance of confirming coverage before services are rendered, preventing costly rework and payment delays.
Mid-Cycle Charge Capture and Coding
The mid-cycle phase transforms clinical documentation into billable charges through accurate medical coding. Optum revenue cycle management systems emphasize the critical link between clinical documentation quality and proper code assignment.
| Documentation Element | Impact on Revenue | Optimization Strategy |
|---|---|---|
| Clinical specificity | Supports appropriate code levels | Provider education and feedback |
| Procedure detail | Enables complete charge capture | Automated charge reconciliation |
| Medical necessity | Prevents claim denials | Real-time coding guidance |
| Modifier usage | Ensures proper reimbursement | Regular coding audits |
Healthcare providers must ensure their medical coding services maintain current knowledge of coding guidelines and payer-specific requirements. This expertise prevents undercoding that leaves money on the table and overcoding that triggers audits and compliance issues.
Back-End Claims and Collections
The back-end revenue cycle encompasses claims submission through final payment collection. Back-end RCM best practices focus on clean claims submission, proactive denial management, and strategic accounts receivable follow-up.
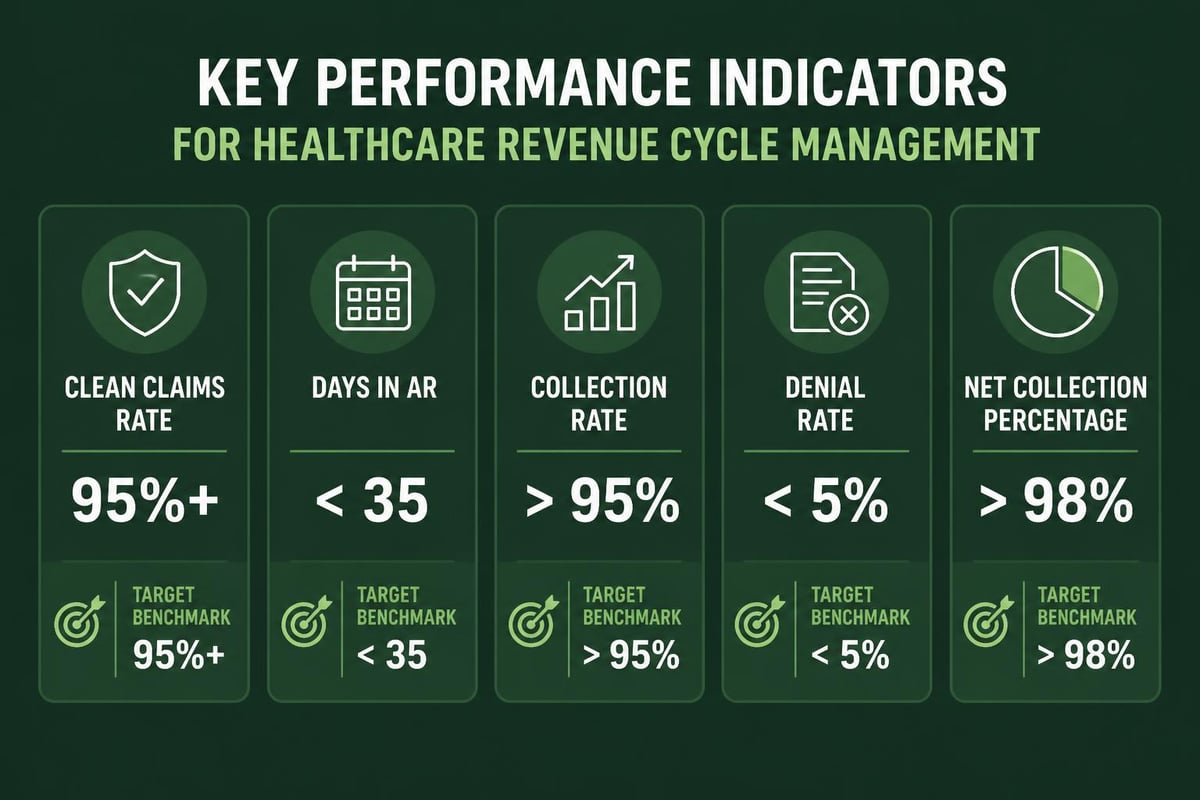
Critical back-end metrics include:
- Clean claims rate (target: 95% or higher)
- First-pass resolution rate
- Days in accounts receivable
- Collection rates by payer category
- Denial rates by denial reason
Professional RCM service providers continuously monitor these metrics and implement corrective actions when performance deviates from established benchmarks. This data-driven approach ensures sustained financial health and identifies opportunities for process improvement.
Advanced Strategies in Optum Revenue Cycle Management
Beyond foundational processes, optum revenue cycle management incorporates sophisticated strategies that address complex billing scenarios and optimize reimbursement across diverse payer contracts. Healthcare organizations implementing these advanced approaches gain competitive advantages in an increasingly challenging financial environment.
Denial Management and Prevention
Effective denial management represents one of the highest-value opportunities in revenue cycle optimization. Rather than simply working denials reactively, leading RCM approaches emphasize prevention through root cause analysis and systematic process improvements.
The comprehensive approach to denial management in medical billing includes both preventive and corrective strategies. Organizations should track denial patterns by:
- Payer
- Denial reason code
- Provider or location
- Service type
- Time period
This analytical foundation enables targeted interventions that address systemic issues rather than individual claim problems. For instance, recurring eligibility denials might indicate the need for enhanced front-end verification processes, while medical necessity denials could signal documentation improvement opportunities.
Prior Authorization Management
Prior authorization requirements continue to expand across commercial and government payers, creating administrative challenges that impact both revenue cycle efficiency and patient satisfaction. Optum revenue cycle management systems integrate prior authorization services into front-end workflows, ensuring requirements are identified and fulfilled before service delivery.
Effective prior authorization workflows include:
- Automated identification of services requiring authorization
- Real-time status tracking and follow-up
- Appeals processes for denied authorizations
- Provider communication and coordination
- Documentation of authorization details in billing systems
Organizations that streamline prior authorization processes reduce claim denials, accelerate time-to-payment, and improve patient access to necessary services.
Contract Management and Optimization
Understanding payer contracts and ensuring accurate reimbursement according to contracted rates requires sophisticated contract management capabilities. Many healthcare providers discover significant underpayment issues when they implement comprehensive contract modeling and payment variance analysis.
| Contract Analysis Component | Purpose | Revenue Impact |
|---|---|---|
| Fee schedule modeling | Establish expected reimbursement | Identifies underpayments |
| Payment variance reporting | Compare actual to expected payments | Quantifies discrepancies |
| Contract term tracking | Monitor contract compliance | Prevents revenue leakage |
| Renegotiation analytics | Support rate negotiations | Improves future contracts |
Professional RCM services include contract management capabilities that protect provider revenue and ensure payers honor their contractual obligations. This oversight function becomes particularly valuable as contract complexity increases and payer payment methodologies evolve.
Technology and Automation in Modern RCM
The integration of advanced technology distinguishes modern optum revenue cycle management from traditional billing services. Automation, artificial intelligence, and predictive analytics transform RCM from a transactional function into a strategic capability that drives organizational performance.
Artificial Intelligence Applications
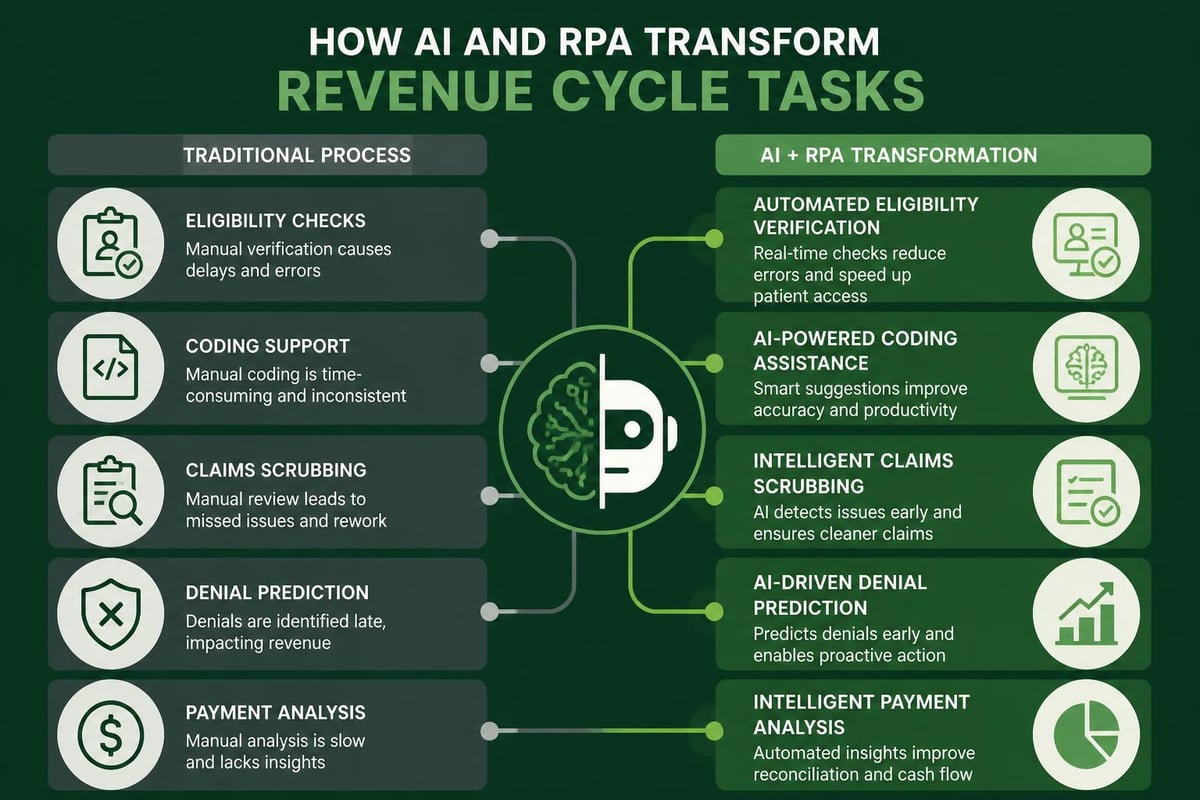
AI applications in revenue cycle management extend beyond simple rule-based automation to encompass machine learning algorithms that improve over time. These intelligent systems analyze patterns across millions of transactions to identify opportunities and risks that human reviewers might miss.
Current AI applications include:
- Predictive denial modeling
- Automated coding assistance
- Payment variance detection
- Patient payment propensity scoring
- Resource allocation optimization
Organizations leveraging AI-enhanced RCM services benefit from these capabilities without requiring internal technology investments. Experienced RCM service providers integrate these tools into their operational workflows, delivering improved results through technology-enabled processes.
Robotic Process Automation
Robotic process automation (RPA) handles high-volume, repetitive tasks with greater speed and accuracy than manual processing. Common RCM applications include eligibility verification, claim status checks, payment posting, and routine correspondence.
The benefits of RPA in revenue cycle management include:
- Increased productivity: Bots work 24/7 without breaks
- Improved accuracy: Eliminates manual data entry errors
- Cost efficiency: Reduces labor costs for routine tasks
- Scalability: Easily handles volume fluctuations
- Staff satisfaction: Frees staff for higher-value work
Healthcare providers partnering with full-service RCM organizations access these automation benefits through the service provider's technology infrastructure. This approach delivers automation advantages without internal IT overhead or capital investment.
Performance Metrics and Continuous Improvement
Optum revenue cycle management emphasizes data-driven performance management through comprehensive metrics and analytics. Healthcare organizations must establish clear benchmarks and monitoring processes to evaluate RCM effectiveness and identify improvement opportunities.
Essential RCM Key Performance Indicators
Tracking the right metrics provides visibility into revenue cycle health and highlights areas requiring attention. Revenue cycle management best practices recommend monitoring both operational efficiency metrics and financial performance indicators.
Operational Efficiency Metrics:
- Point-of-service cash collection rate
- Registration error rate
- Coding productivity (charts per day)
- Clean claims rate
- Claim submission lag time
- Denial rate (by reason and payer)
- Denial overturn rate
- A/R days outstanding
- Collection rate (net and gross)
Financial Performance Indicators:
- Net collection rate
- Cost to collect
- Revenue per encounter
- Bad debt percentage
- Contractual adjustment accuracy
- Payment variance rate
Organizations should establish metric baselines, set improvement targets, and implement regular performance review cycles. This disciplined approach to performance management ensures sustained focus on revenue cycle optimization.
Benchmarking and Comparative Analysis
Understanding how your revenue cycle performance compares to industry standards provides context for improvement initiatives. While specific benchmarks vary by specialty and practice setting, general industry standards offer useful reference points.
| Metric | Industry Standard | High-Performing Organizations |
|---|---|---|
| Clean Claims Rate | 90-95% | 98%+ |
| Days in A/R | 35-45 days | <30 days |
| Denial Rate | 5-10% | <3% |
| Net Collection Rate | 95-98% | 99%+ |
| Cost to Collect | 3-5% | <2.5% |
Healthcare providers working with specialized revenue cycle management services benefit from the provider's cross-client visibility and industry benchmarking capabilities. This comparative perspective helps identify performance gaps and prioritize improvement initiatives.
Regulatory Compliance and Risk Management
Maintaining compliance with evolving healthcare regulations represents a critical dimension of optum revenue cycle management. Organizations must balance aggressive revenue optimization with strict adherence to billing rules, coding guidelines, and documentation requirements.
HIPAA Compliance in Revenue Cycle Operations
Revenue cycle processes involve extensive handling of protected health information (PHI), making HIPAA compliance essential. RCM service providers must implement comprehensive safeguards including:
- Access controls and user authentication
- Encryption of data in transit and at rest
- Business associate agreements with all vendors
- Staff training on privacy and security requirements
- Incident response and breach notification procedures
- Regular risk assessments and security audits
Healthcare providers should verify that any RCM partner maintains robust compliance programs and undergoes regular third-party security assessments. This due diligence protects patient privacy and minimizes organizational risk.
Coding Compliance and Audit Preparedness
Proper medical coding serves as the foundation for compliant billing, yet coding errors remain a common source of compliance risk. Organizations must implement multiple layers of quality assurance to ensure coding accuracy.
Coding compliance strategies include:
- Regular coding audits by certified professionals
- Ongoing coder education and certification maintenance
- Documentation improvement programs for providers
- Pre-bill coding review for high-risk services
- Post-payment audits to identify patterns
- Corrective action plans for identified issues
Professional medical coding audit services provide objective assessments of coding accuracy and compliance risk. These audits identify both undercoding that reduces revenue and overcoding that creates compliance exposure.
Implementation Considerations for Healthcare Providers
Healthcare organizations evaluating optum revenue cycle management approaches or considering RCM service partnerships must carefully assess their current state, identify gaps, and select solutions that align with their specific needs and circumstances.
Build vs. Buy Analysis
The fundamental decision facing many healthcare providers involves whether to build internal RCM capabilities or partner with specialized service providers. This analysis should consider multiple dimensions beyond simple cost comparison.
Factors favoring internal RCM operations:
- Very large practice size with scale advantages
- Unique billing requirements or workflows
- Strong existing RCM infrastructure and expertise
- Desire for direct staff oversight and control
- Integration with other internal systems
Factors favoring outsourced RCM services:
- Small to medium practice size
- Difficulty recruiting and retaining billing staff
- Inconsistent RCM performance
- Limited technology budget
- Need for rapid performance improvement
- Desire to focus on clinical operations
Many healthcare providers find that partnering with experienced RCM service providers offers the optimal balance of performance, cost efficiency, and operational focus. Organizations like Greenhive Billing Solutions deliver comprehensive RCM services that combine expert staff with industry-leading technology platforms.
Transition Planning and Change Management
Successfully implementing new optum revenue cycle management approaches or transitioning to an RCM service provider requires careful planning and change management. Poor transitions create payment disruptions, staff confusion, and patient dissatisfaction.
Critical transition elements include:
- Detailed process documentation and gap analysis
- Data migration planning and validation
- Staff communication and training programs
- Parallel operations during transition period
- Performance monitoring and issue resolution
- Ongoing optimization after go-live
Healthcare providers should establish clear success criteria, define roles and responsibilities, and maintain open communication throughout the transition process. This structured approach minimizes disruption and accelerates time to value.
Ongoing Partnership Management
Whether implementing internal improvements based on industry best practices or working with an external RCM service provider, ongoing performance management ensures sustained results. Regular communication, metric review, and continuous improvement efforts maintain momentum and prevent performance degradation.
Effective partnership management includes quarterly business reviews, monthly operational meetings, regular reporting cadences, and collaborative problem-solving when issues arise. This collaborative approach maximizes the value of RCM investments and supports long-term financial health.
Optum revenue cycle management demonstrates how comprehensive, technology-enabled approaches can transform healthcare financial operations and deliver measurable performance improvements. Healthcare providers seeking similar results should evaluate their current RCM performance, identify improvement opportunities, and consider how specialized expertise and proven methodologies can accelerate their progress. Greenhive Billing Solutions provides comprehensive revenue cycle management services designed to enhance financial performance, reduce administrative burden, and ensure maximum reimbursements for healthcare practices throughout the United States. Our experienced team works seamlessly with your existing systems to deliver the expertise and results your organization deserves.