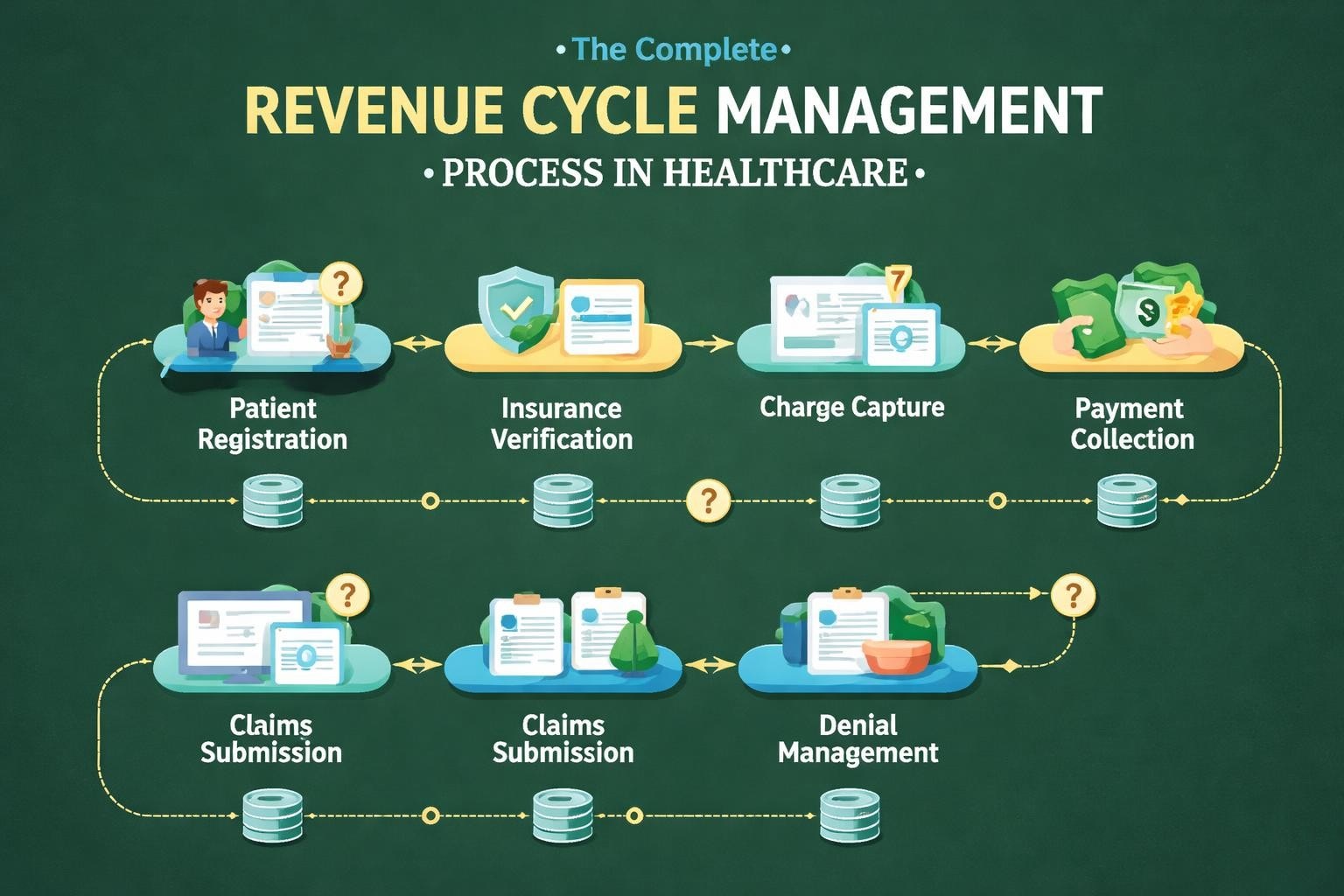
The revenue cycle management process represents the financial backbone of every healthcare organization, yet many providers struggle to optimize this critical workflow. Understanding the rcm cycle healthcare framework enables medical practices to maximize reimbursements, reduce claim denials, and maintain healthy cash flow. This comprehensive guide explores each stage of the revenue cycle, identifies common challenges, and provides actionable strategies that healthcare providers can implement to improve their financial performance.
Understanding the Fundamental Stages of RCM Cycle Healthcare
The rcm cycle healthcare encompasses all administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue. According to the Healthcare Financial Management Association, this process begins before a patient enters your facility and continues until all claims are fully adjudicated and paid.
Pre-Service Activities That Set the Foundation
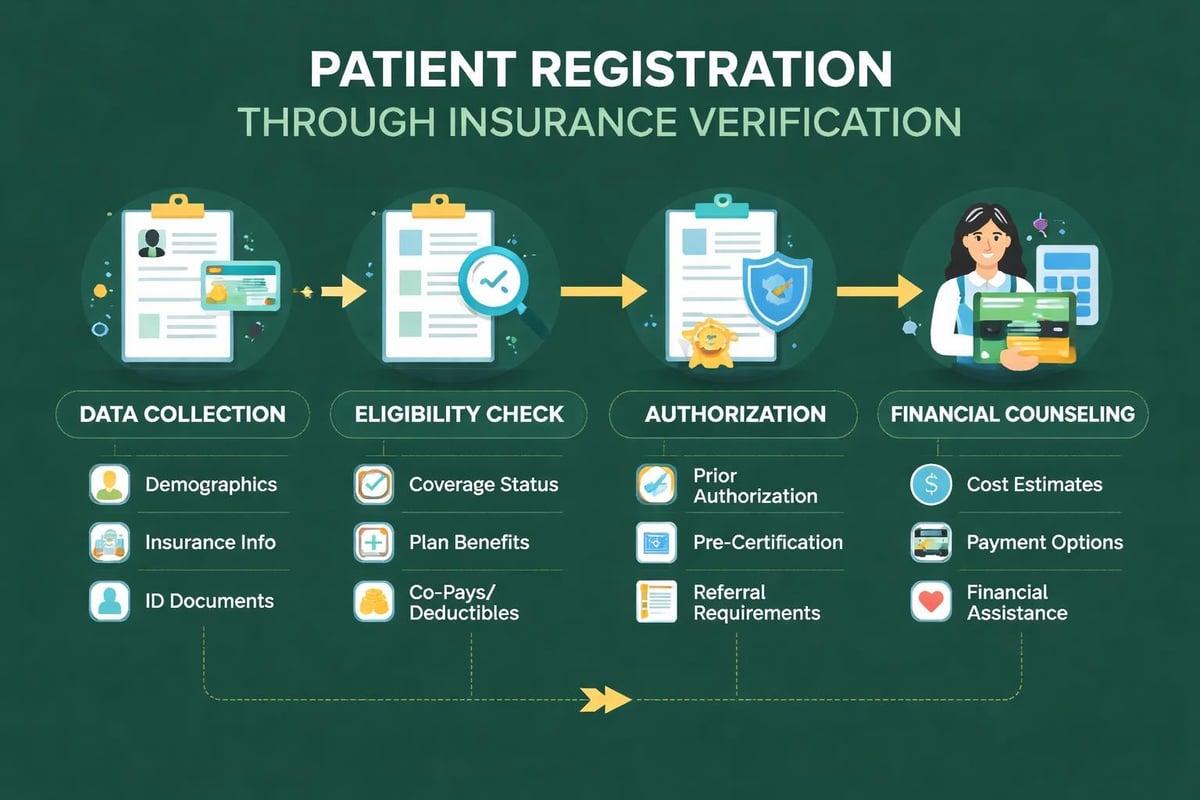
Patient registration represents the first critical touchpoint in the revenue cycle. During this phase, your staff collects demographic information, insurance details, and medical history. Accuracy at this stage directly impacts downstream processes.
Insurance verification and eligibility confirmation must occur before services are rendered. This step prevents claim denials related to inactive coverage or incorrect policy information. When your team verifies benefits in advance, they can also determine:
- Patient financial responsibility including deductibles and copayments
- Coverage limitations and exclusions
- Prior authorization requirements for specific procedures
- Out-of-network status and associated implications
Prior authorization has become increasingly complex, requiring dedicated staff resources. Healthcare Finance News reports that authorization delays significantly impact revenue cycle performance across all practice sizes.
Financial counseling during pre-service activities helps patients understand their payment obligations. Transparent conversations about costs improve collection rates and patient satisfaction simultaneously.
Service Delivery and Clinical Documentation Excellence
Clinical encounters generate the documentation that supports medical billing and coding. The quality and completeness of this documentation determine reimbursement levels and compliance with regulatory standards.
Charge Capture and Code Assignment
Charge capture ensures that all billable services are recorded accurately. Missing charges represent lost revenue that many practices never recover. Implementing systematic charge entry in medical billing processes minimizes revenue leakage.
Medical coding translates clinical documentation into standardized codes using CPT, ICD-10, and HCPCS systems. Professional coders must possess current knowledge of coding guidelines and payer-specific requirements. Understanding different types of medical coding helps providers select appropriate expertise for their specialty.
| Coding System | Primary Purpose | Update Frequency |
|---|---|---|
| CPT | Procedures and services | Annual |
| ICD-10-CM | Diagnoses | Annual |
| HCPCS Level II | Supplies and equipment | Quarterly |
| Revenue Codes | Hospital billing categories | As needed |
Compliance with coding regulations protects practices from audit risk and payment clawbacks. The connection between clinical documentation and code selection requires ongoing education for both clinical and billing staff.
Claims Management and Submission Protocols
Clean claims submission represents a critical efficiency metric within the rcm cycle healthcare framework. A clean claim in medical billing contains no errors or missing information that would trigger automatic rejection.
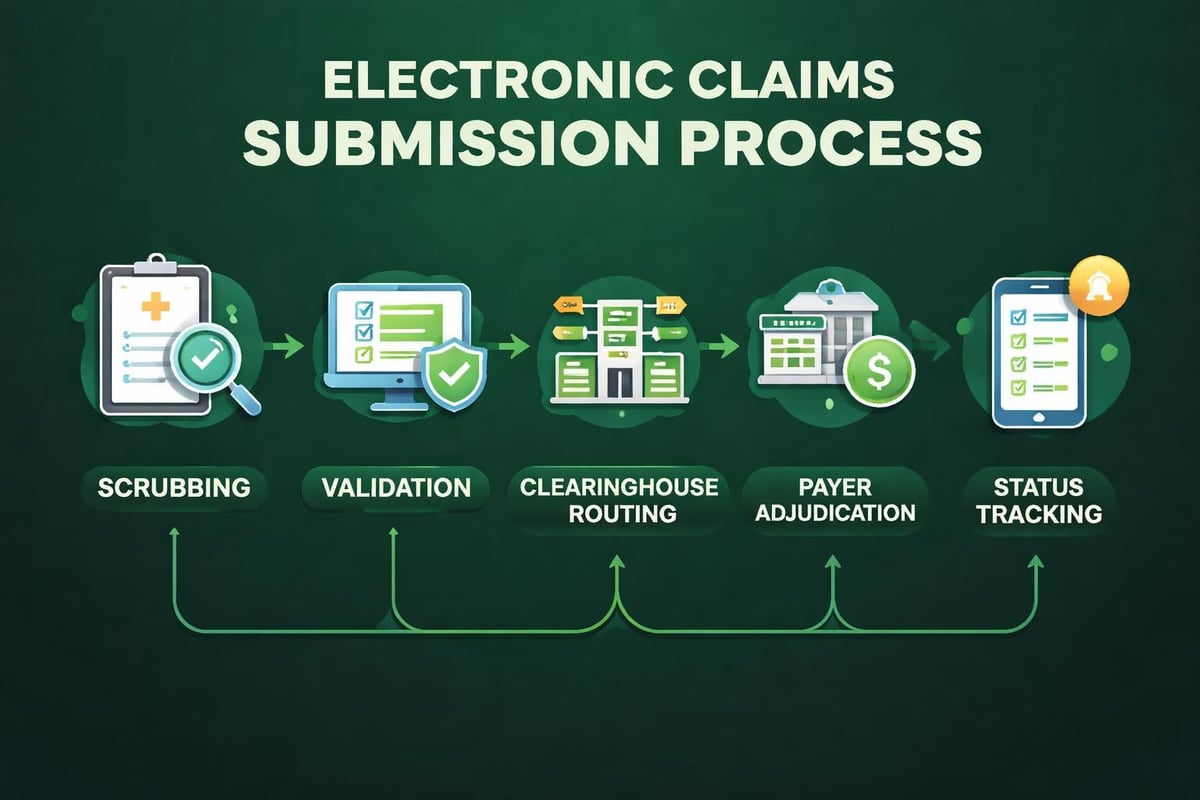
Claim Scrubbing and Quality Checks
Automated claim scrubbing identifies potential errors before submission to payers. These systems check for:
- Missing or invalid National Provider Identifier (NPI) numbers
- Incorrect date formats or service date logic errors
- Diagnosis and procedure code compatibility issues
- Duplicate claim submissions
Manual review processes supplement automated scrubbing for complex claims or high-value services. This dual-layer approach significantly reduces rejection rates.
Electronic claim submission through clearinghouses accelerates the payment cycle compared to paper submissions. Most payers now require electronic transactions, making EDI infrastructure essential for modern practices.
Tracking claim status from submission through adjudication prevents delays and identifies problems early. Many billing systems integrate real-time eligibility and claim status checking capabilities.
Payment Posting and Reconciliation Procedures
Accurate payment posting maintains the integrity of your practice's financial records. This stage of the rcm cycle healthcare requires attention to detail and systematic processes that match payments to specific claims and patient accounts.
Electronic Remittance Advice Processing
Understanding what is ERA in medical billing revolutionizes payment posting efficiency. Electronic Remittance Advice files contain detailed payment information that can be automatically posted to practice management systems.
Payment variances require investigation and proper accounting. The most common payment adjustments include:
- Contractual adjustments reflecting negotiated rate differences between billed charges and allowed amounts
- Deductible and coinsurance amounts transferred to patient responsibility
- Coordination of benefits adjustments when multiple payers cover services
- Timely filing denials when claims exceed submission deadlines
Learning why contractual adjustment in medical billing remains essential helps staff accurately process payer payments and maintain compliant accounting practices.
Reconciliation processes ensure that all payments are properly allocated and that accounts receivable aging reports reflect accurate outstanding balances. Regular reconciliation identifies discrepancies early, preventing larger problems from developing.
Denial Management and Appeals Strategy
Denial management represents one of the most significant opportunities for revenue recovery within the rcm cycle healthcare framework. TechTarget’s analysis of healthcare RCM emphasizes that effective denial management can recover 60-90% of denied claims when processes are optimized.
Root Cause Analysis and Prevention
Tracking denial reasons provides actionable data for process improvement. Common denial categories include:
- Registration and eligibility errors
- Authorization and precertification failures
- Coding and documentation deficiencies
- Timely filing violations
- Medical necessity determinations
Implementing denial management in medical billing processes that focus on prevention rather than just correction yields better financial outcomes. Prevention strategies target the root causes identified through denial analysis.
| Denial Type | Primary Cause | Prevention Strategy |
|---|---|---|
| Registration errors | Incomplete patient data | Real-time verification systems |
| Authorization denials | Missing pre-approvals | Automated tracking workflows |
| Coding errors | Documentation gaps | Provider education programs |
| Medical necessity | Insufficient support | Enhanced clinical documentation |
Appeals require timely submission with supporting documentation that addresses the specific denial reason. Successful appeals staff understand payer policies, coverage guidelines, and effective communication strategies.
Patient Financial Responsibility and Collections
Patient responsibility has grown substantially as high-deductible health plans become more prevalent. Effective patient collections require a balanced approach that maintains positive relationships while securing payment.
Point-of-Service Collections
Collecting payments at the time of service significantly improves collection rates compared to billing after services are rendered. Staff training on financial conversations helps team members discuss payment expectations professionally and compassionately.
Price transparency regulations now require providers to offer good-faith estimates for services. Providing accurate cost information upfront builds trust and facilitates payment discussions.
Payment plan options make healthcare more accessible while ensuring revenue collection. Establishing clear policies for:
- Minimum monthly payment amounts
- Interest rates and finance charges (where applicable)
- Default and write-off thresholds
- Third-party financing partnerships
Self-service payment portals improve convenience for patients and reduce administrative burden on staff. Online payment options should include multiple payment methods and provide receipts automatically.

Technology Integration Across the Revenue Cycle
Modern rcm cycle healthcare depends on integrated technology platforms that connect clinical and financial systems. Interoperability between your electronic health record (EHR), practice management system, and billing platform eliminates redundant data entry and reduces errors.
Analytics and Performance Monitoring
Revenue cycle analytics provide visibility into performance metrics that drive decision-making. Key performance indicators include:
- Days in accounts receivable measuring the average time from service to payment
- Clean claim rate indicating the percentage of claims accepted on first submission
- Collection rate showing the percentage of expected revenue actually collected
- Denial rate tracking the percentage of claims denied by payers
- Cost to collect measuring the operational expense per dollar collected
Dashboard reporting delivers real-time insights that enable proactive management rather than reactive problem-solving. Understanding healthcare revenue cycle analytics helps practices identify trends and opportunities.
Artificial intelligence and machine learning applications now assist with coding validation, denial prediction, and payment estimation. These technologies augment human expertise rather than replacing the judgment and relationship skills that experienced revenue cycle professionals provide.
Compliance and Regulatory Considerations
HIPAA compliance governs every aspect of the rcm cycle healthcare process. Protected health information (PHI) security requirements apply to billing communications, payment posting, collections activities, and all other revenue cycle functions.
Documentation and Audit Preparedness
Maintaining comprehensive audit trails protects practices during payer audits and regulatory reviews. Documentation requirements include:
- Medical necessity support for all billed services
- Signed advance beneficiary notices (ABNs) when applicable
- Authorization approvals and supporting correspondence
- Appeal submissions and outcomes
- Collection activity logs demonstrating compliance with Fair Debt Collection Practices Act
Regular internal audits identify compliance risks before external auditors discover them. Proactive compliance programs cost significantly less than post-audit remediation and penalties.
Payer contract compliance ensures that your billing practices align with negotiated terms. Contract management systems help track multiple payer agreements, fee schedules, and special billing requirements.
Staff Training and Revenue Cycle Expertise
The human element remains central to effective revenue cycle management despite technological advances. Staff expertise directly impacts financial performance across all stages of the rcm cycle healthcare process.
Continuous Education Requirements
Medical billing regulations, coding guidelines, and payer policies change frequently. Ongoing education keeps staff current with:
- Annual CPT and ICD-10 updates
- New payer coverage policies
- Emerging compliance requirements
- Technology platform enhancements
Professional certifications demonstrate competency and commitment to excellence. Certified Professional Coders (CPC), Certified Revenue Cycle Representatives (CRCR), and other credentials validate specialized knowledge.
Cross-training team members across multiple revenue cycle functions builds organizational resilience and improves process understanding. Staff who comprehend how their work impacts downstream activities make better decisions and collaborate more effectively.
Optimizing Revenue Cycle Performance for Specialty Practices
Different medical specialties face unique revenue cycle challenges that require tailored approaches. Surgical practices manage complex authorization requirements and bundled payment arrangements. Primary care practices handle high patient volumes with diverse payer mixes. Behavioral health providers navigate medical billing for behavioral health complexities including carve-out benefits and session limits.
Specialty-Specific Considerations
Understanding your specialty's particular challenges enables targeted process improvements. For instance, urgent care revenue cycle management requires rapid charge capture and billing for walk-in patients with unknown insurance status.
Ambulatory surgery centers coordinate facility and professional billing while managing complex implant and supply charges. Hospital-based practices navigate place-of-service coding rules and split-billing arrangements.
Telemedicine has introduced new billing scenarios with evolving coverage policies and technology requirements. Staying current with telehealth billing regulations ensures compliant claims and appropriate reimbursement.
| Specialty | Key RCM Challenge | Mitigation Strategy |
|---|---|---|
| Surgery | Authorization complexity | Dedicated pre-cert staff |
| Primary Care | High volume processing | Workflow automation |
| Behavioral Health | Carve-out benefits | Specialized verification |
| Urgent Care | Unknown insurance | Point-of-service verification |
Strategic Partnerships and Outsourcing Decisions
Many healthcare providers partner with specialized revenue cycle management companies to enhance performance while allowing clinical staff to focus on patient care. Evaluating revenue cycle billing service providers requires careful consideration of expertise, technology, transparency, and cultural fit.
Building Effective RCM Partnerships
Successful outsourcing relationships begin with clear expectations and detailed service level agreements. Define specific performance metrics, reporting requirements, communication protocols, and escalation procedures.
Technology integration capabilities determine how seamlessly an RCM partner can work with your existing systems. API connections, data exchange formats, and reporting dashboards should align with your operational needs.
Transparency in processes and pricing builds trust and enables effective collaboration. Understanding how your RCM partner operates, makes decisions, and handles exceptions ensures alignment with your practice values and standards.
Regular performance reviews keep partnerships productive and identify improvement opportunities. Quarterly business reviews should examine metrics, discuss challenges, celebrate successes, and plan strategic initiatives.
Mastering the rcm cycle healthcare process requires ongoing attention to people, processes, and technology across every stage from patient registration through final payment collection. When you optimize each component and ensure seamless integration between stages, your practice achieves better financial performance, reduced administrative burden, and improved patient satisfaction. Greenhive Billing Solutions provides comprehensive revenue cycle management services that address every aspect of this complex process, from insurance verification and claims processing through denial management and patient collections, helping healthcare providers across the United States maximize reimbursements while maintaining HIPAA compliance and operational efficiency.