Medical invoicing serves as the financial backbone of healthcare practices, directly impacting cash flow, operational efficiency, and patient satisfaction. This critical process encompasses far more than simply generating bills-it requires precise documentation, accurate coding, thorough insurance verification, and meticulous claim submission. For healthcare providers navigating an increasingly complex regulatory landscape, mastering medical invoicing fundamentals has become essential to maintaining financial stability while delivering quality patient care.
Understanding the Medical Invoicing Landscape
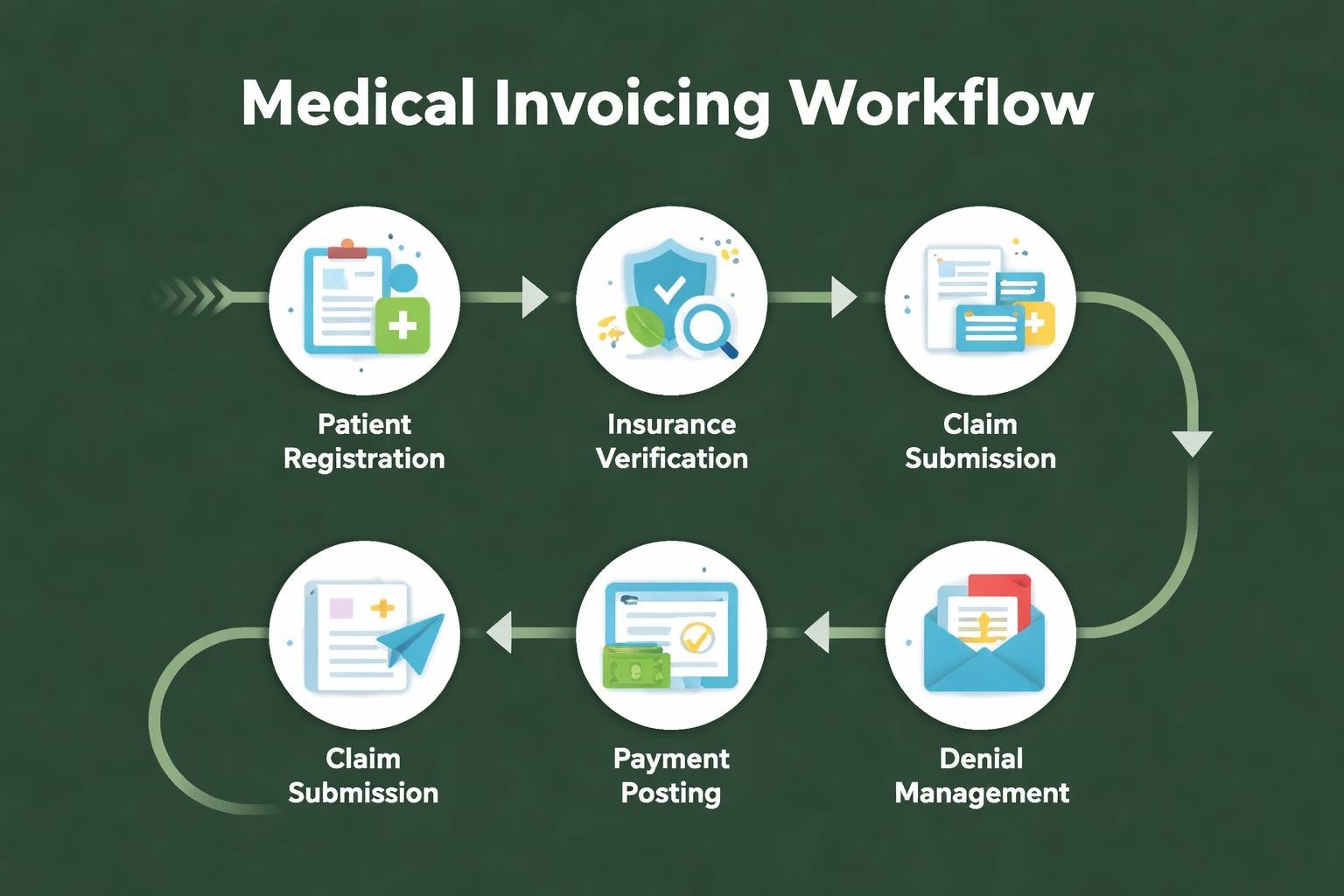
Medical invoicing represents a multifaceted process that bridges clinical services and financial reimbursement. The process begins the moment a patient schedules an appointment and continues through payment collection and reconciliation. Unlike standard commercial invoicing, healthcare billing requires adherence to strict regulatory frameworks, including HIPAA compliance, payer-specific requirements, and ever-evolving coding standards.
Healthcare providers face mounting pressure to optimize their revenue cycle management while managing increasing administrative burdens. Clean claim rates-the percentage of claims processed without requiring additional information-directly correlate with practice profitability. Research indicates that practices with higher clean claim rates experience faster reimbursements and reduced administrative overhead.
The Financial Impact of Accurate Medical Invoicing
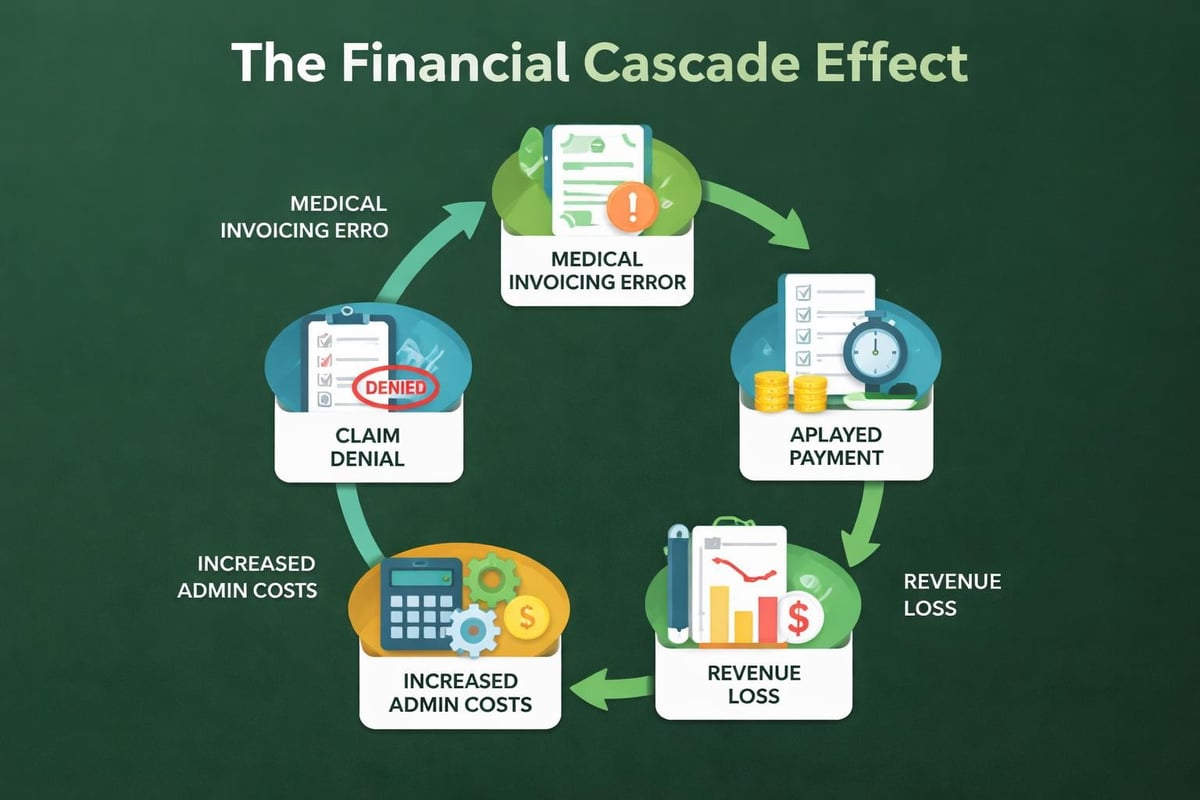
Revenue leakage represents one of the most significant challenges facing healthcare organizations today. Even minor errors in medical invoicing can cascade into substantial financial losses over time. Denied claims consume valuable staff resources, delay payments, and sometimes result in complete write-offs.
The relationship between accurate medical invoicing and practice sustainability cannot be overstated. When claims are submitted correctly the first time, practices experience improved cash flow predictability, reduced days in accounts receivable, and enhanced patient satisfaction through transparent billing processes.
Essential Components of Effective Medical Invoicing
Successful medical invoicing relies on several interconnected elements that must function seamlessly together. Understanding these components helps practices identify potential weak points in their current processes and implement targeted improvements.
Patient Information Verification
Accurate patient demographic and insurance information forms the foundation of clean claims. Before any services are rendered, front-office staff must verify and document:
- Complete patient name matching insurance card exactly
- Current address and contact information
- Active insurance coverage with correct policy numbers
- Primary and secondary insurance hierarchy
- Coordination of benefits requirements
Eligibility verification services reduce claim rejections by confirming coverage details before appointment dates. Real-time verification systems can identify coverage issues that might otherwise result in denied claims weeks after service delivery.
Precise Medical Coding
Medical coding translates clinical services into standardized codes used for billing purposes. This process requires specialized knowledge of multiple coding systems:
| Coding System | Purpose | Example |
|---|---|---|
| CPT Codes | Procedures and services | 99213 – Office visit |
| ICD-10 Codes | Diagnoses and conditions | E11.9 – Type 2 diabetes |
| HCPCS Codes | Supplies and equipment | A4253 – Blood glucose meter |
| Modifiers | Additional service details | 25 – Significant E/M service |
Staying current with annual coding updates prevents claim denials based on outdated or discontinued codes. The best practices to increase medical billing and coding accuracy emphasize continuous education and regular auditing as crucial components of coding excellence.
Five Critical Steps for Medical Invoicing Success
Implementing a systematic approach to medical invoicing dramatically improves outcomes. These five steps create a framework that minimizes errors while maximizing efficiency.
Step 1: Comprehensive Pre-Service Preparation
Before patient encounters, practices should complete thorough preparation. This includes verifying insurance eligibility, confirming prior authorization requirements, and collecting patient financial responsibilities. Understanding coverage limitations prevents surprise denials and improves patient communication regarding expected costs.
Many denials stem from services requiring prior authorization that was never obtained. Creating protocols around authorization tracking ensures compliance with payer requirements and protects revenue.
Step 2: Accurate Documentation at Point of Service
Clinical documentation must support the codes billed. Providers should document all services rendered with sufficient detail to justify the level of service coded. Proper coding practices require alignment between clinical notes and billing codes to withstand potential audits.
Electronic health record systems should facilitate documentation that naturally supports accurate coding. Templates and prompts can guide providers toward comprehensive documentation without adding excessive administrative burden.
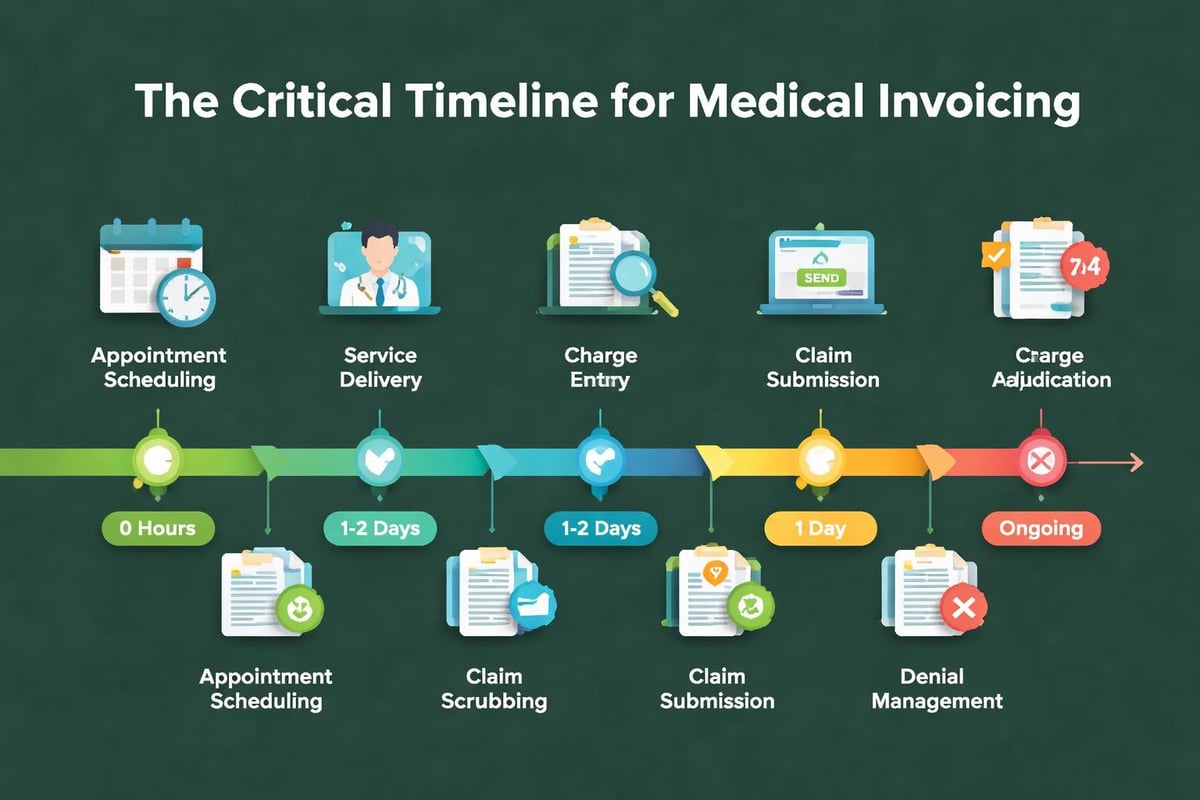
Step 3: Timely Claim Submission
Submitting claims promptly after service delivery accelerates payment cycles. Most payers impose filing deadlines, typically ranging from 90 to 365 days from the date of service. Missing these deadlines results in automatic claim denials that cannot be appealed.
Medical claim submission services ensure claims are transmitted within payer timeframes using electronic submission methods that provide immediate acknowledgment of receipt. Batch processing claims daily rather than weekly significantly improves cash flow timing.
Step 4: Proactive Denial Management
Even with excellent processes, some claim denials are inevitable. The difference between successful and struggling practices lies in how they respond to denials. Establishing dedicated denial management services ensures rejected claims receive immediate attention.
Tracking denial patterns reveals systemic issues requiring process improvements. Common denial categories include:
- Registration errors
- Coding inaccuracies
- Missing or insufficient documentation
- Timely filing violations
- Coordination of benefits issues
Step 5: Regular Performance Monitoring
What gets measured gets managed. Practices should track key performance indicators related to medical invoicing:
- Clean claim rate
- Days in accounts receivable
- Collection rate
- Denial rate by category
- Appeal success rate
- Net collection percentage
These metrics reveal process strengths and weaknesses, guiding continuous improvement efforts. Benchmarking against industry standards provides context for performance evaluation.
Compliance Considerations in Medical Invoicing
Regulatory compliance represents a non-negotiable aspect of medical invoicing. Healthcare providers must navigate complex federal and state regulations while meeting payer-specific requirements. The consequences of non-compliance extend beyond financial penalties to include potential legal liability and reputational damage.
HIPAA Requirements
Patient privacy protections under HIPAA apply throughout the medical invoicing process. Practices must implement safeguards protecting patient information during transmission, storage, and disposal. Electronic claim submissions require secure transmission methods, and paper documentation demands secure storage and compliant destruction procedures.
UCI Health’s billing compliance standards demonstrate institutional commitment to ethical billing practices. Healthcare organizations should establish comprehensive compliance programs addressing all aspects of medical invoicing.
Documentation Standards
Medical necessity documentation supports every claim submitted. Payers may request medical records during claim review, and insufficient documentation results in claim denials or recoupments. Documentation should clearly establish:
- Medical necessity for services rendered
- Appropriate level of service provided
- Clinical rationale for diagnostic testing
- Treatment plan supporting continued care
The medical billing compliance checklist provides structured guidance for maintaining audit-ready documentation practices. Regular internal audits identify documentation gaps before external auditors discover them.
Technology's Role in Modern Medical Invoicing
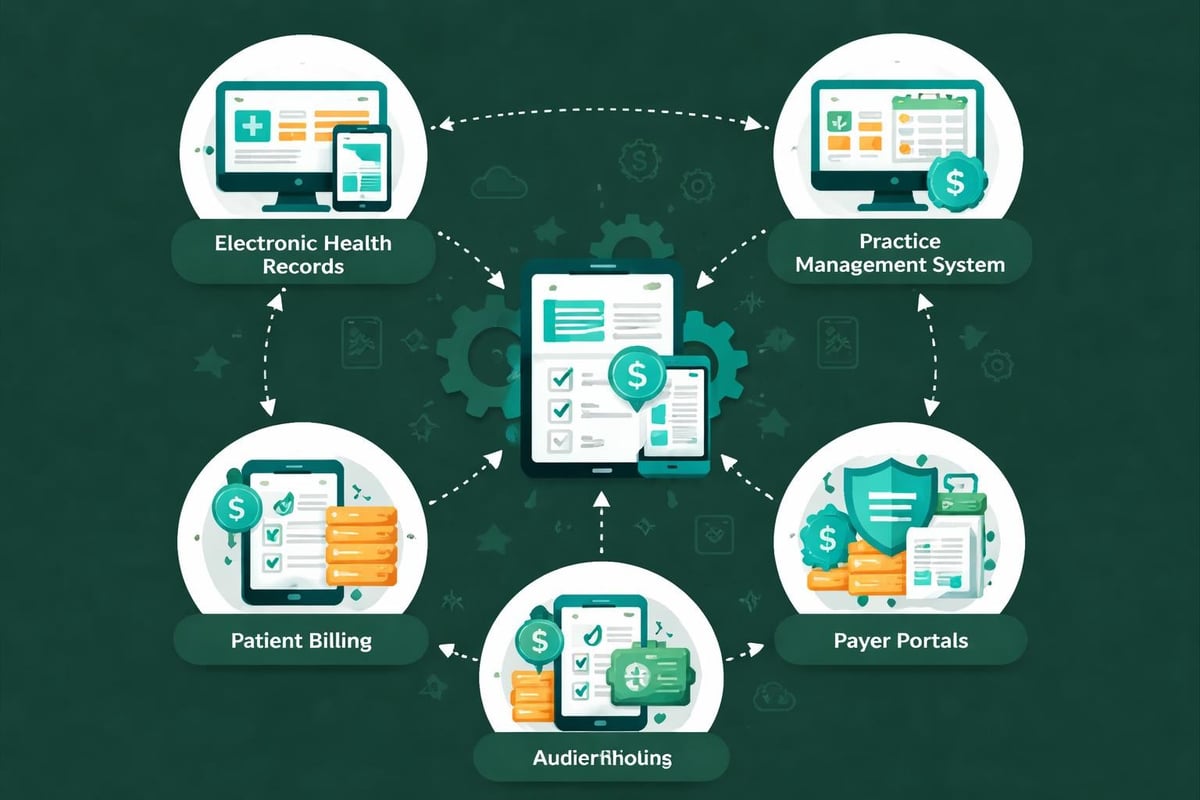
Technology has transformed medical invoicing from a paper-intensive process to a streamlined digital workflow. Modern practice management systems integrate multiple functions, reducing manual data entry and associated errors.
Electronic health records connected to billing systems eliminate duplicate data entry while ensuring clinical documentation aligns with submitted codes. Automated scrubbing tools identify potential claim errors before submission, preventing denials.
Selecting the Right Technology Solutions
Healthcare providers seeking medical billing software should evaluate solutions based on several criteria:
| Feature | Importance | Consideration |
|---|---|---|
| EHR Integration | Critical | Seamless data flow between clinical and billing systems |
| Claim Scrubbing | High | Identifies errors before submission |
| Reporting Capabilities | High | Tracks KPIs and identifies trends |
| Payer Connectivity | Critical | Electronic claim submission to multiple payers |
| User Interface | Medium | Impacts staff efficiency and training requirements |
Many successful practices partner with revenue cycle management service providers who bring expertise with multiple software platforms. These partnerships allow practices to focus on clinical care while experienced professionals handle medical invoicing complexities.
Common Medical Invoicing Mistakes and Prevention Strategies
Understanding frequent errors helps practices implement preventive measures. The most costly mistakes often stem from seemingly minor oversights that compound over time.
Patient Information Errors
Incorrect patient demographics account for a significant percentage of claim denials. Simple typos in names, transposed policy numbers, or outdated addresses trigger automatic rejections. Avoiding mistakes in medical invoices begins with rigorous front-end verification processes.
Implementing double-verification protocols where staff confirm patient information against insurance cards reduces these preventable errors. Photo documentation of insurance cards provides reference material when questions arise during claim processing.
Coding Errors
Unbundling services that should be billed together, using outdated codes, or selecting codes that don't match documented diagnoses create claim complications. Regular training on coding updates keeps staff informed about changes affecting medical invoicing accuracy.
Automated code checking systems flag potential coding conflicts before claim submission. These tools identify impossible code combinations, age-gender conflicts, and other common coding mistakes.
Incomplete Claims
Missing information delays processing even when other claim elements are accurate. Common omissions include:
- Referring provider information
- Place of service codes
- Required attachments or documentation
- Prior authorization numbers
- Coordination of benefits details
Creating claim submission checklists specific to different service types ensures completeness. Staff should verify all required fields are populated before releasing claims to clearinghouses.
Optimizing Patient Communication Around Medical Invoicing
Transparent patient communication about financial responsibilities improves collection rates and patient satisfaction. Confusion about charges, insurance coverage, and patient responsibility frequently leads to delayed payments and strained provider-patient relationships.
Providing cost estimates before services whenever possible allows patients to make informed decisions. While precise estimates prove challenging given insurance variables, ranges based on typical coverage help patients prepare financially.
Clear, itemized statements that patients can easily understand reduce billing inquiries. Avoiding excessive medical jargon and providing plain-language explanations of charges improves comprehension. Many practices find that medical billing best practices include multiple patient communication touchpoints throughout the billing cycle.
Payment Options and Financial Policies
Establishing clear financial policies communicated consistently to all patients creates predictability. These policies should address:
- Payment expectations at time of service
- Accepted payment methods
- Payment plan availability
- Financial assistance programs
- Collection procedures for delinquent accounts
Offering multiple payment options, including online portals and automated payment plans, accommodates diverse patient preferences and improves collection rates.
Staff Training and Development for Medical Invoicing Excellence
Investing in staff education yields significant returns in medical invoicing performance. The healthcare payment landscape evolves constantly, requiring ongoing learning to maintain proficiency.
Comprehensive onboarding for new billing staff should cover organizational-specific workflows alongside fundamental medical invoicing principles. Pairing new employees with experienced mentors accelerates skill development while reducing costly errors.
Regular continuing education keeps teams current on regulatory changes, payer policy updates, and emerging best practices. Medical billing compliance knowledge requires consistent reinforcement as requirements evolve.
Cross-training staff across multiple revenue cycle functions creates operational flexibility and deeper understanding of how individual roles impact overall performance. Staff who understand the complete medical invoicing workflow make more informed decisions in their specific responsibilities.
Integration of Medical Invoicing Across the Revenue Cycle
Medical invoicing doesn't exist in isolation but rather as one component of comprehensive revenue cycle management. Understanding these connections optimizes the entire financial process from patient scheduling through final payment reconciliation.
Front-end revenue cycle activities directly impact medical invoicing success. Insurance verification, authorization management, and financial counseling prevent downstream billing complications. Payment posting services connect the billing process to financial reconciliation, identifying underpayments and processing refunds when appropriate.
Denial management feeds insights back to earlier revenue cycle stages, creating continuous improvement loops. When denials reveal consistent authorization issues, front-office protocols can be adjusted to prevent future occurrences.
Metrics That Connect Medical Invoicing to Overall Performance
Tracking integrated metrics reveals how medical invoicing impacts broader organizational objectives:
- Net collection rate measuring total payments against total charges
- Cost to collect indicating efficiency of revenue cycle operations
- Point-of-service collection percentage showing front-end effectiveness
- Bad debt write-off rates identifying uncollectible accounts
These comprehensive metrics provide context beyond simple claim acceptance rates, connecting medical invoicing quality to financial sustainability.
Future Trends Shaping Medical Invoicing
The medical invoicing landscape continues evolving driven by technological advancement, regulatory changes, and shifting payment models. Forward-thinking practices prepare for these emerging trends.
Artificial intelligence and machine learning increasingly support medical invoicing processes through predictive analytics that identify high-risk claims, automated coding suggestions based on clinical documentation, and intelligent denial prediction. These technologies augment human expertise rather than replacing experienced professionals.
Value-based payment models shift focus from volume to outcomes, changing traditional medical invoicing approaches. Practices participating in bundled payments, accountable care organizations, or other alternative payment models must adapt billing processes to new reimbursement methodologies.
Patient financial responsibility continues growing with high-deductible health plans becoming more prevalent. This trend requires enhanced patient engagement strategies around medical invoicing and collection, including price transparency tools and expanded payment plan options.
The integrated approach to medical billing increasingly relies on technology platforms that connect previously siloed functions, creating end-to-end visibility across the revenue cycle.
Building a Sustainable Medical Invoicing Framework
Long-term success in medical invoicing requires systematic approaches rather than reactive problem-solving. Practices should develop standardized processes documented in comprehensive policy and procedure manuals that guide consistent execution regardless of staff turnover.
Regular process auditing identifies drift from established standards and reveals improvement opportunities. Internal audits should examine both accuracy and efficiency, ensuring processes maintain quality while optimizing resource utilization.
Benchmarking against industry standards provides objective performance assessment. Organizations can compare their metrics against specialty-specific benchmarks to identify relative strengths and weaknesses.
Continuous improvement culture encourages staff at all levels to suggest process enhancements. Front-line employees often identify inefficiencies invisible to management, and creating channels for feedback harnesses this valuable perspective.
Partnering with experienced revenue cycle management professionals provides access to specialized expertise and best practices developed across multiple healthcare organizations. These partnerships prove particularly valuable for smaller practices lacking resources for dedicated revenue cycle staff.
Mastering medical invoicing requires balancing accuracy, efficiency, compliance, and patient satisfaction across complex processes that directly impact practice financial health. By implementing systematic approaches to verification, coding, claim submission, and denial management, healthcare providers can significantly improve their revenue cycle performance. Greenhive Billing Solutions partners with healthcare practices nationwide to optimize medical invoicing processes through comprehensive revenue cycle management services, delivering improved cash flow, reduced administrative burden, and maximum reimbursements while maintaining strict HIPAA compliance and transparent communication throughout every stage of the billing process.