Healthcare providers face mounting pressure to maximize revenue while managing complex payer contracts, regulatory requirements, and operational costs. Net revenue management has emerged as a critical discipline that goes beyond traditional billing practices to optimize every dollar earned from patient services. For healthcare organizations, understanding and implementing net revenue management strategies can mean the difference between financial stability and revenue leakage that threatens sustainability.
Understanding Net Revenue Management in Healthcare Revenue Cycles
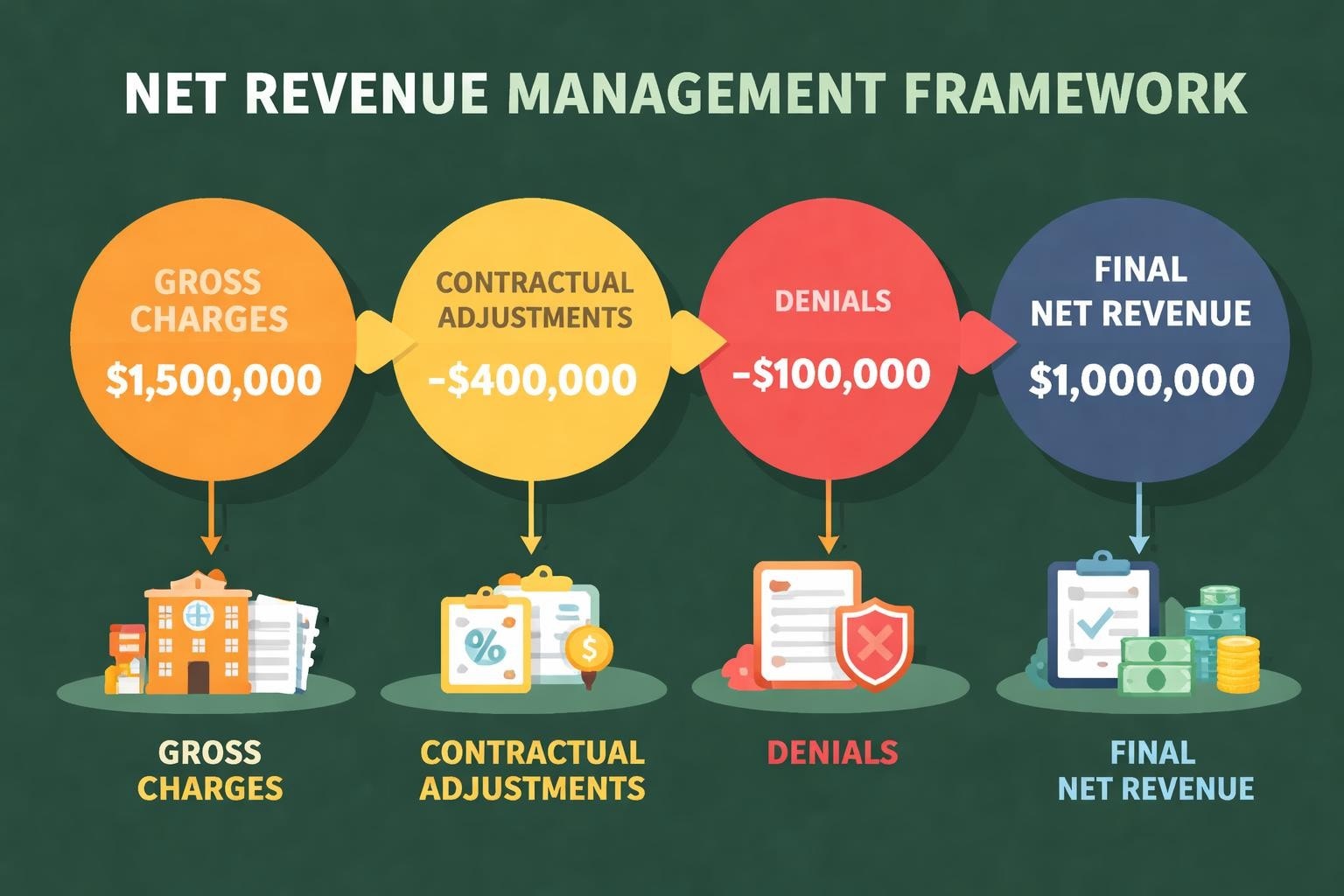
Net revenue management represents a comprehensive approach to maximizing the actual revenue healthcare providers receive after all deductions, adjustments, and write-offs. Unlike gross revenue, which reflects the total charges submitted, net revenue reflects the real financial picture after contractual adjustments, denials, bad debt, and other reductions.
Understanding net revenue management requires recognizing that it encompasses every touchpoint in the revenue cycle, from accurate charge capture and coding through claims submission, payment posting, and denial management. The discipline focuses on identifying and eliminating revenue leakage while optimizing reimbursement rates through strategic contract management and operational excellence.
The Critical Components of Net Revenue Management
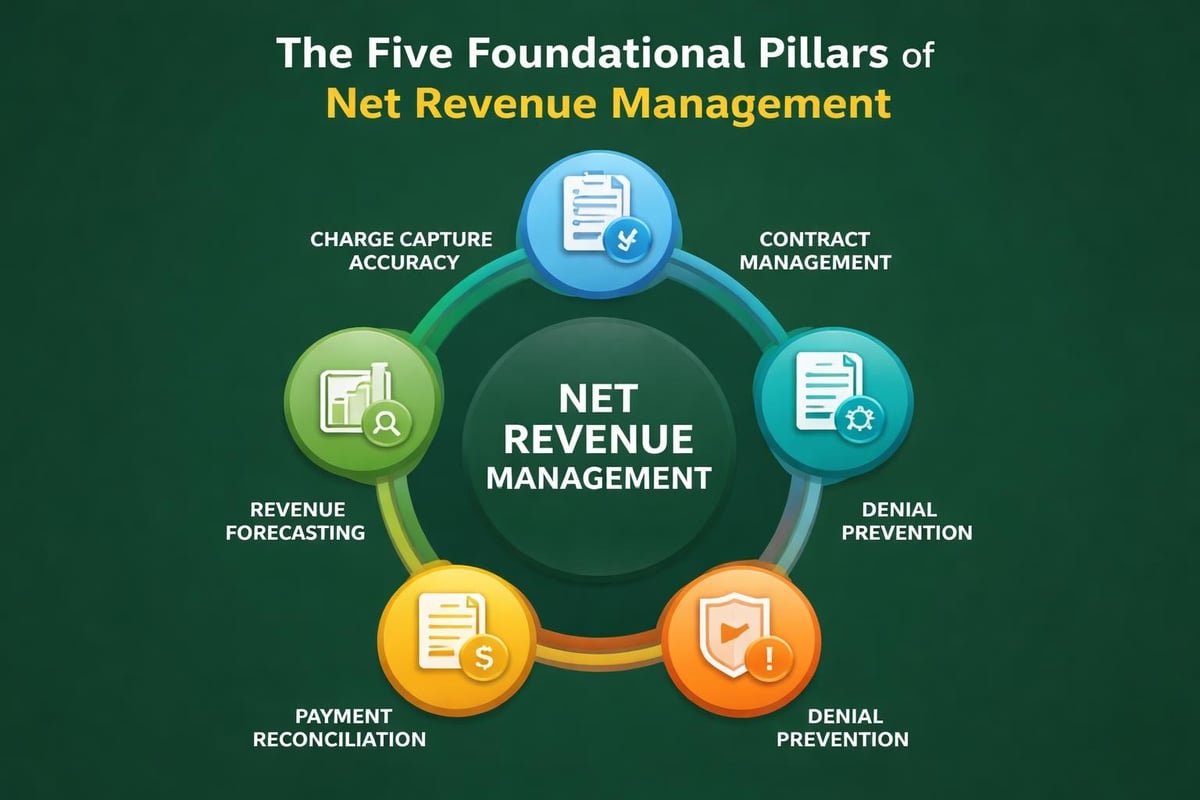
Healthcare organizations must address several interconnected elements to implement effective net revenue management strategies:
- Charge capture integrity: Ensuring all services rendered are accurately documented and billed
- Contract optimization: Negotiating favorable payer agreements and monitoring compliance
- Denial prevention: Identifying root causes of claim rejections before submission
- Payment variance analysis: Tracking discrepancies between expected and actual reimbursements
- Revenue forecasting: Predicting net collections based on historical performance and payer mix
These components work together to create a comprehensive framework that protects revenue at every stage. When healthcare providers optimize their revenue cycle management, they gain visibility into financial performance and can make data-driven decisions about resource allocation and strategic planning.
Strategic Pricing and Contract Management
Net revenue management demands sophisticated approaches to pricing strategy and payer negotiations. Healthcare providers must understand their true cost of service delivery, competitive market positioning, and payer-specific reimbursement patterns to maximize net collections.
Analyzing Payer Mix and Reimbursement Patterns
Different payers reimburse at vastly different rates for identical services. Commercial insurers typically pay significantly higher rates than government programs, while self-pay patients present unique collection challenges. Effective net revenue management requires detailed analysis of:
| Payer Category | Average Reimbursement Rate | Collection Timeline | Denial Rate |
|---|---|---|---|
| Commercial Insurance | 135-160% of Medicare | 30-45 days | 8-12% |
| Medicare | 100% (baseline) | 14-21 days | 3-5% |
| Medicaid | 60-80% of Medicare | 45-60 days | 10-15% |
| Self-Pay | Variable (20-40% collected) | 60-120+ days | N/A |
Understanding these patterns allows healthcare organizations to forecast net revenue more accurately and identify opportunities for improvement. For example, reducing denial rates for commercial payers by just two percentage points can significantly impact overall net collections.
Contract Negotiation and Performance Monitoring
Strategic contract management forms the backbone of net revenue management. Healthcare providers should regularly review payer contracts to ensure reimbursement rates align with market standards and cost structures. This includes:
Rate negotiation leverage points:
- Volume commitments and exclusivity agreements
- Quality metrics and outcome-based incentives
- Timeliness of claims processing and payment
- Administrative burden and documentation requirements
Beyond initial negotiations, implementing robust denial management processes helps identify when payers fail to honor contractual obligations. Regular contract compliance audits reveal underpayments that can be recovered through appeals and reconciliation processes.
Operational Excellence in Revenue Capture
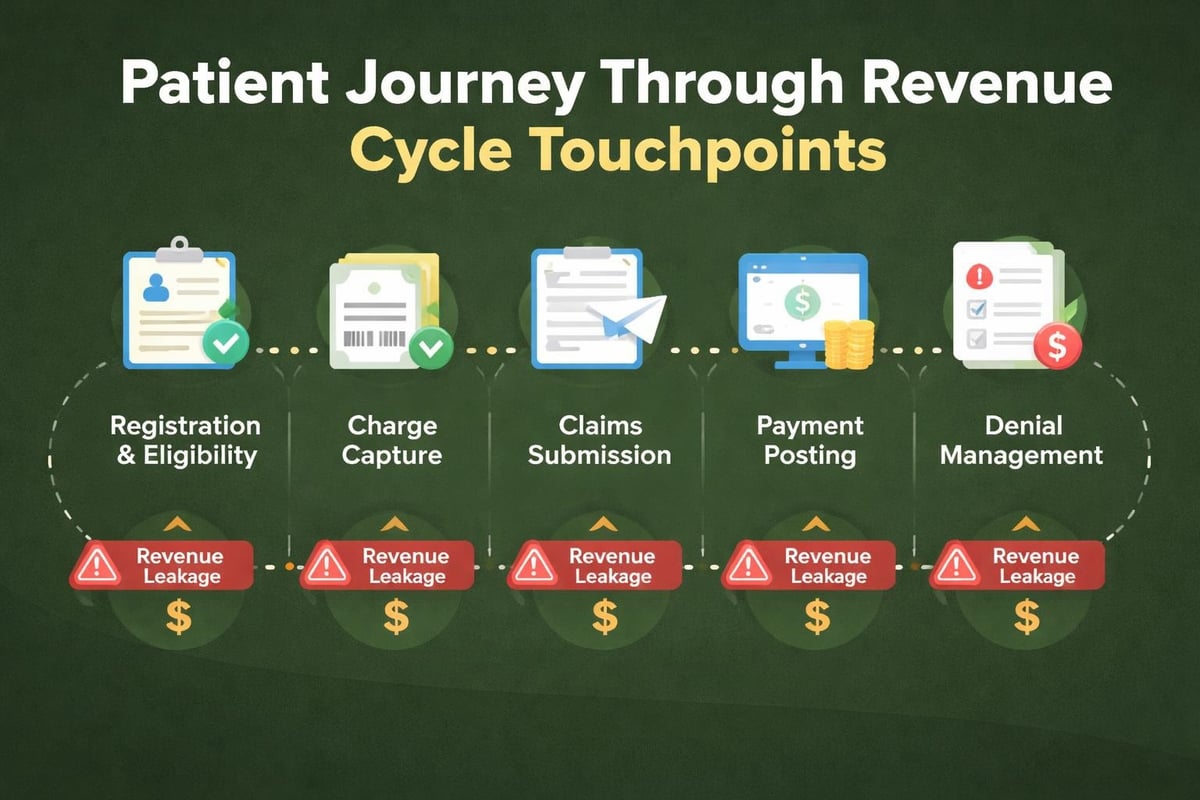
Net revenue management extends to every operational process that impacts financial performance. From front-desk registration through final payment posting, each step presents opportunities to protect or lose revenue.
Front-End Revenue Cycle Optimization
The revenue cycle begins long before claims submission. Front-end processes directly impact net revenue through:
- Insurance verification accuracy: Confirming coverage and benefits prevents downstream denials
- Patient demographic accuracy: Correct information ensures claims reach the right payer
- Authorization management: Obtaining required approvals before service delivery
- Point-of-service collections: Collecting deductibles and copayments at the time of service
- Financial counseling: Helping patients understand their obligations and payment options
Healthcare providers partnering with dental care specialists like Dental Plus Clinic understand that front-end accuracy becomes especially critical when managing diverse service lines and patient populations across multiple locations. Each registration error or missed authorization creates downstream revenue cycle disruptions that reduce net collections.
Charge Capture and Coding Excellence
Accurate charge capture and medical coding directly determine the difference between gross charges and net revenue. Undercoding leaves money on the table, while overcoding triggers denials and compliance risks.
Understanding revenue coding fundamentals helps organizations implement controls that ensure:
- All billable services are captured in the medical record
- Documentation supports the level of service billed
- Codes reflect the most specific diagnosis and procedure information
- Modifiers are applied correctly to maximize appropriate reimbursement
- Charges are submitted within payer-specific filing deadlines
Regular coding audits identify patterns of missed charges or coding errors that systematically reduce net revenue. For example, facilities might discover they consistently fail to bill for specific supplies or services, representing thousands of dollars in monthly revenue leakage.
Technology and Data Analytics in Net Revenue Management
Modern net revenue management relies heavily on technology platforms and data analytics to identify opportunities and monitor performance. Healthcare organizations need sophisticated tools to track the dozens of metrics that impact financial outcomes.
Key Performance Indicators for Net Revenue
Effective net revenue management strategy requires monitoring specific metrics that reveal financial health:
| Metric | Target Range | Impact on Net Revenue |
|---|---|---|
| Clean Claim Rate | >95% | Reduces rework and accelerates payment |
| Days in A/R | <40 days | Improves cash flow and reduces bad debt |
| Net Collection Rate | >95% | Measures actual collections vs. expected |
| Denial Rate | <5% | Directly impacts revenue realization |
| Cost to Collect | <3% of collections | Ensures operational efficiency |
These metrics provide early warning signs when net revenue performance deteriorates. For instance, increasing days in accounts receivable might indicate payer payment delays, coding issues causing denials, or insufficient follow-up on outstanding claims.
Predictive Analytics and Revenue Forecasting
Advanced analytics enable healthcare organizations to predict net revenue with greater accuracy by analyzing historical patterns, payer behavior, and seasonal variations. Predictive models can forecast:
- Expected net collections by payer and service line
- Denial probability for specific claim types
- Optimal staffing levels for billing operations
- Contract performance against benchmarks
- Revenue impact of proposed operational changes
These insights allow financial leaders to make proactive decisions rather than reacting to revenue shortfalls after they occur. Revenue cycle analytics platforms integrate data from practice management systems, electronic health records, and clearinghouses to provide comprehensive visibility into net revenue performance.
Denial Management as a Net Revenue Strategy
Claim denials represent one of the most significant threats to net revenue in healthcare. Industry studies suggest that 5-10% of all claims are initially denied, with many organizations failing to rework and recover this revenue.
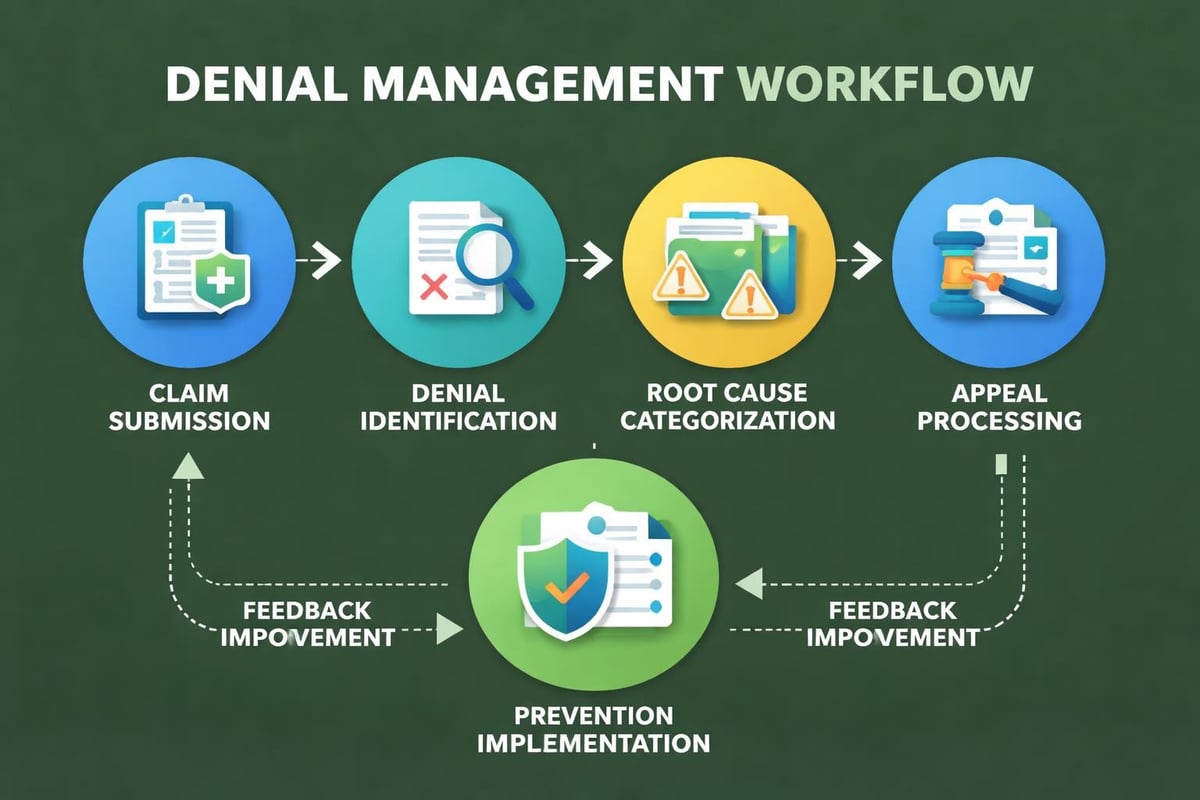
Root Cause Analysis and Prevention
Effective net revenue management requires understanding why denials occur and implementing systematic prevention strategies. Common denial categories include:
- Eligibility and registration errors: Patient not covered on date of service
- Authorization failures: Missing precertification for procedures
- Coding and documentation issues: Unsupported level of service or medical necessity
- Timely filing violations: Claims submitted after payer deadlines
- Duplicate claims: Same service billed multiple times
Learning how denial management improves cash flow helps organizations prioritize prevention over appeals. While appeals can recover denied revenue, prevention eliminates the cost and delay associated with rework.
Building an Effective Appeals Process
Despite prevention efforts, some denials are inevitable. Net revenue management requires robust appeals processes that maximize recovery rates:
- Prioritize high-value denials: Focus resources on claims with significant dollar amounts
- Track payer-specific patterns: Identify systemic denial trends by insurance company
- Document appeal rationale: Provide clear clinical and contractual justification
- Meet appeal deadlines: Payers impose strict timeframes that cannot be extended
- Monitor appeal outcomes: Track success rates and adjust strategies accordingly
Healthcare organizations should calculate their denial recovery rate (dollars recovered divided by dollars denied) as a key net revenue management metric. Recovery rates below 60% suggest opportunities to improve appeal effectiveness or redirect resources to prevention.
Compliance and Regulatory Considerations
Net revenue management must operate within strict regulatory boundaries. Aggressive billing practices that violate compliance standards can result in penalties, audits, and reputational damage that far exceed any short-term revenue gains.
Billing Compliance Fundamentals
Healthcare organizations must balance revenue optimization with compliance requirements:
Critical compliance areas:
- Medicare and Medicaid billing regulations
- HIPAA privacy and security standards
- Stark Law and Anti-Kickback Statute provisions
- False Claims Act prohibitions
- State-specific insurance regulations
Understanding clean claims in medical billing ensures that optimization efforts focus on legitimate opportunities rather than questionable practices. Clean claims that meet all payer requirements process faster, reduce denials, and minimize compliance risk.
Audit Preparedness and Documentation
Net revenue management strategies should include regular internal audits that identify potential compliance issues before external auditors discover them. Comprehensive documentation protects revenue during audits by demonstrating:
- Medical necessity for services rendered
- Appropriate level of service based on documentation
- Compliance with payer-specific billing requirements
- Proper use of modifiers and billing codes
- Timely and accurate charge capture processes
Organizations facing audits can protect net revenue by maintaining organized documentation, responding promptly to information requests, and engaging compliance experts when needed. Proactive compliance reduces the risk of payment recoupments that can devastate net revenue performance.
Service Line Analysis and Profitability Management
Not all healthcare services contribute equally to net revenue. Strategic net revenue management requires understanding which service lines generate positive margins and which consume resources without adequate financial return.
Calculating True Service Line Profitability
Healthcare organizations should analyze net revenue by service line, considering both direct and indirect costs:
| Service Line | Gross Revenue | Contractual Adjustments | Net Revenue | Direct Costs | Contribution Margin |
|---|---|---|---|---|---|
| Primary Care | $500,000 | $200,000 (40%) | $300,000 | $240,000 | $60,000 (20%) |
| Specialty Surgery | $800,000 | $240,000 (30%) | $560,000 | $350,000 | $210,000 (37.5%) |
| Imaging Services | $350,000 | $140,000 (40%) | $210,000 | $180,000 | $30,000 (14.3%) |
| Laboratory Services | $200,000 | $80,000 (40%) | $120,000 | $95,000 | $25,000 (20.8%) |
This analysis reveals which services drive net revenue performance and deserve additional investment versus those that may require operational improvements or strategic reconsideration.
Resource Allocation Based on Net Revenue Performance
Organizations can optimize net revenue by directing resources toward high-performing service lines while addressing underperformance in others. Strategies include:
- Expanding capacity for services with strong contribution margins
- Renegotiating payer contracts for services with excessive adjustments
- Implementing efficiency improvements to reduce direct costs
- Evaluating whether to continue offering unprofitable services
- Cross-training staff to support multiple service lines flexibly
Healthcare providers should regularly review their revenue cycle processes to ensure resource allocation aligns with strategic priorities and net revenue optimization goals.
Staff Training and Performance Management
Net revenue management succeeds only when staff members understand their role in protecting revenue and possess the skills to execute effectively. From registration specialists to billing coordinators, every team member impacts financial outcomes.
Building a Revenue-Focused Culture
Organizations with strong net revenue performance cultivate cultures where staff understand the financial impact of their work. This requires:
- Regular training on billing requirements and payer policies
- Clear performance metrics tied to revenue cycle outcomes
- Recognition programs for accuracy and productivity achievements
- Open communication about financial performance and goals
- Continuous improvement processes that engage frontline staff
When registration staff understand how insurance verification prevents denials, they approach their work with greater attention to detail. When coders recognize how documentation impacts reimbursement, they proactively communicate with providers about improvement opportunities.
Performance Metrics for Revenue Cycle Staff
Different roles require different performance metrics aligned with net revenue management objectives:
Registration and scheduling:
- Insurance verification completion rate
- Demographic accuracy rate
- Authorization obtainment rate
- Point-of-service collection percentage
Coding and charge capture:
- Coding accuracy rate
- Average days to code encounters
- Query response time
- Charge lag days
Claims and follow-up:
- Clean claim submission rate
- Days to submit claims
- Denial resolution rate
- A/R over 90 days percentage
These metrics create accountability for revenue cycle performance while identifying training needs and process improvement opportunities.
Partnering with Revenue Cycle Management Experts
Many healthcare organizations lack the internal expertise or resources to optimize net revenue management independently. Strategic partnerships with specialized revenue cycle management companies provide access to industry best practices, experienced staff, and proven processes.
Evaluating Revenue Cycle Management Partners
Healthcare providers should carefully assess potential revenue cycle management partners based on several criteria:
- Industry expertise and healthcare specialization
- Technology platforms and reporting capabilities
- Transparency in performance metrics and communication
- Compliance with HIPAA and regulatory requirements
- References from similar organizations
- Pricing structure aligned with performance outcomes
Organizations exploring partnerships should understand that effective revenue cycle management companies bring deep expertise in areas like medical billing for behavioral health and other specialized practice areas, along with the infrastructure to scale operations as practice needs evolve.
Measuring Partnership Success
Net revenue management partnerships should deliver measurable improvements across key performance indicators. Healthcare organizations should establish baseline metrics before engagement and track progress monthly:
- Increased net collection rate
- Reduced days in A/R
- Lower denial rates
- Improved clean claim rates
- Decreased cost to collect
- Enhanced revenue cycle transparency
Regular performance reviews ensure partnerships continue delivering value and identify opportunities for further optimization. Successful partnerships function as extensions of internal teams, providing expertise while respecting the unique needs of each healthcare organization.
Net revenue management represents the intersection of clinical excellence, operational efficiency, and financial strategy in healthcare. By implementing comprehensive approaches that address pricing, operations, technology, compliance, and staff performance, healthcare organizations can maximize the revenue they earn from patient care. Greenhive Billing Solutions specializes in helping healthcare providers across the United States optimize their revenue cycles through expert medical billing, claims processing, denial management, and comprehensive revenue cycle services. Our team delivers transparent, HIPAA-compliant solutions that improve financial performance while allowing providers to focus on patient care.