Provider billing represents the backbone of financial sustainability for healthcare organizations across the United States. This complex process encompasses everything from patient registration and insurance verification to claim submission and payment collection. When executed effectively, provider billing ensures that healthcare practices receive appropriate compensation for the services they deliver, maintaining cash flow and supporting continued patient care. Understanding the intricacies of this system has become increasingly critical as payer requirements evolve, regulatory standards tighten, and reimbursement models shift toward value-based care.
Understanding the Provider Billing Process
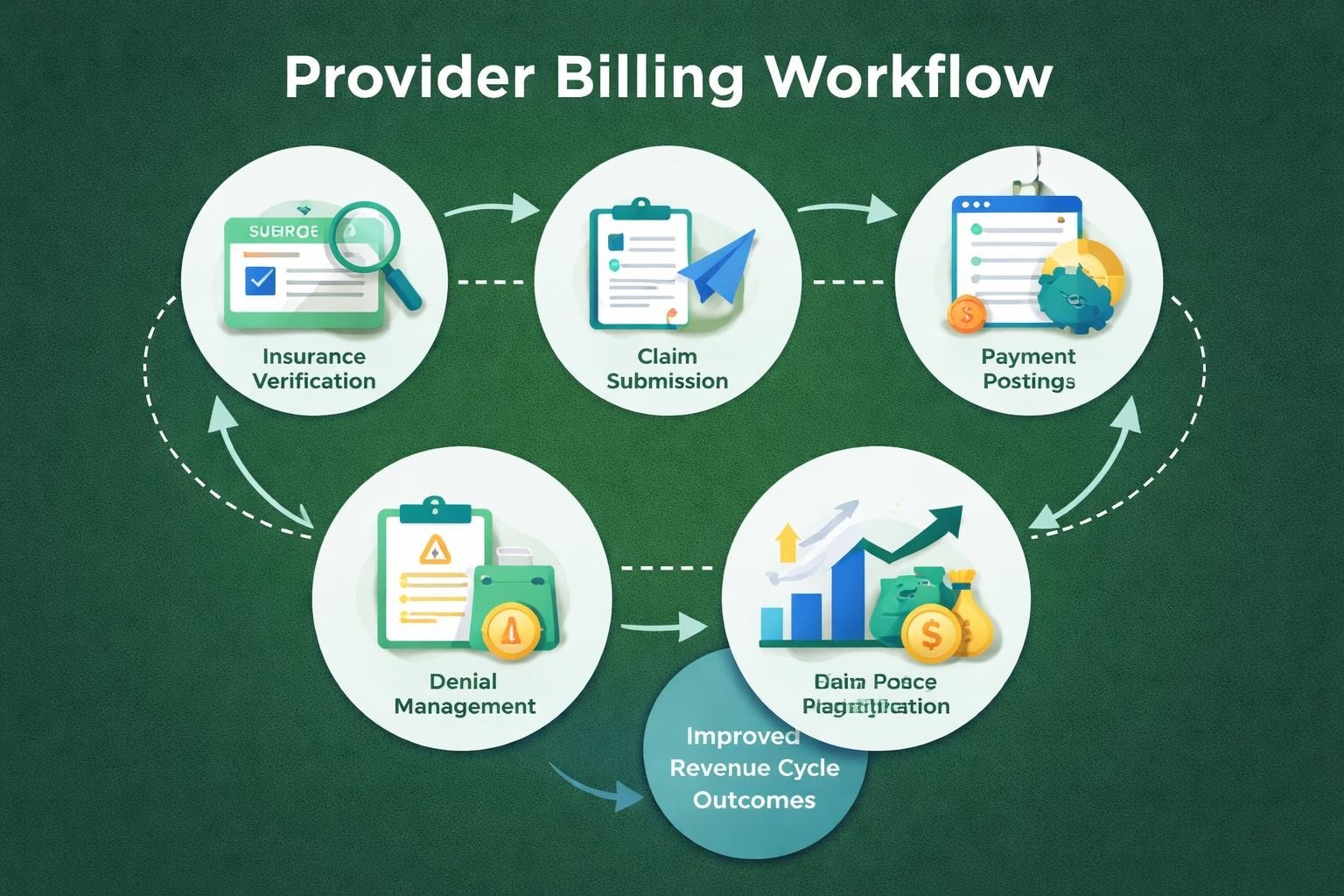
Provider billing involves a systematic approach to translating healthcare services into billable claims that insurance companies and patients can process for payment. This workflow begins the moment a patient schedules an appointment and continues through final payment reconciliation.
The initial phase requires accurate patient demographic information and insurance details. Front-office staff must verify eligibility and benefits before services are rendered, preventing downstream payment issues. Insurance eligibility verification confirms active coverage, identifies copayment requirements, and determines whether prior authorization is necessary for specific procedures.
Following the patient encounter, clinical documentation must support the services provided. Physicians and clinical staff generate notes that accurately reflect diagnoses, treatments, and medical necessity. This documentation becomes the foundation for accurate coding and compliant claim submission.
Key Components of Effective Provider Billing
Several interconnected elements work together to create a successful provider billing operation:
- Accurate patient registration capturing complete demographic and insurance information
- Real-time insurance verification to confirm coverage and benefits before service delivery
- Precise medical coding using current ICD-10, CPT, and HCPCS code sets
- Timely claim submission meeting payer deadlines and format requirements
- Proactive denial management addressing rejected claims quickly and systematically
- Consistent payment posting recording all payments, adjustments, and patient balances accurately
Each component requires specialized knowledge and attention to detail. A breakdown at any stage can delay reimbursement, increase administrative costs, and strain practice resources. Healthcare organizations implementing comprehensive medical billing services typically experience improved claim acceptance rates and faster payment cycles.
Common Provider Billing Challenges
Healthcare practices face numerous obstacles in their billing operations. Claim denials represent one of the most significant challenges, with industry data showing that 5-10% of all claims are initially denied. These denials stem from various sources including coding errors, missing documentation, eligibility issues, and timely filing violations.
Coding accuracy remains a persistent concern. The transition to ICD-10 expanded the diagnosis code set dramatically, requiring coders to select from thousands of specific codes. Selecting an inappropriate code or failing to support medical necessity can result in claim rejection or reduced reimbursement. Organizations benefit from implementing medical coding services staffed by certified professionals who stay current with coding updates and payer-specific requirements.
Regulatory Compliance and Documentation
Provider billing must comply with numerous federal and state regulations. The Centers for Medicare & Medicaid Services establishes compliance standards that govern coverage, coding, and billing practices for government payers. Private insurance companies maintain their own requirements, creating a complex landscape of rules that billing staff must navigate.
Documentation deficiencies create significant billing challenges. Claims lacking proper supporting documentation face automatic denial, requiring appeals and resubmission. Clinical staff must document the medical necessity for services, justify the level of care provided, and maintain records that meet both regulatory standards and payer requirements.
| Challenge Type | Impact on Revenue | Common Solutions |
|---|---|---|
| Claim Denials | 5-10% revenue loss | Denial tracking, root cause analysis, staff training |
| Coding Errors | Reduced reimbursement | Regular audits, certified coders, ongoing education |
| Insurance Verification Failures | Increased bad debt | Real-time eligibility checks, benefit verification |
| Timely Filing Violations | Complete claim rejection | Claim tracking systems, submission calendars |
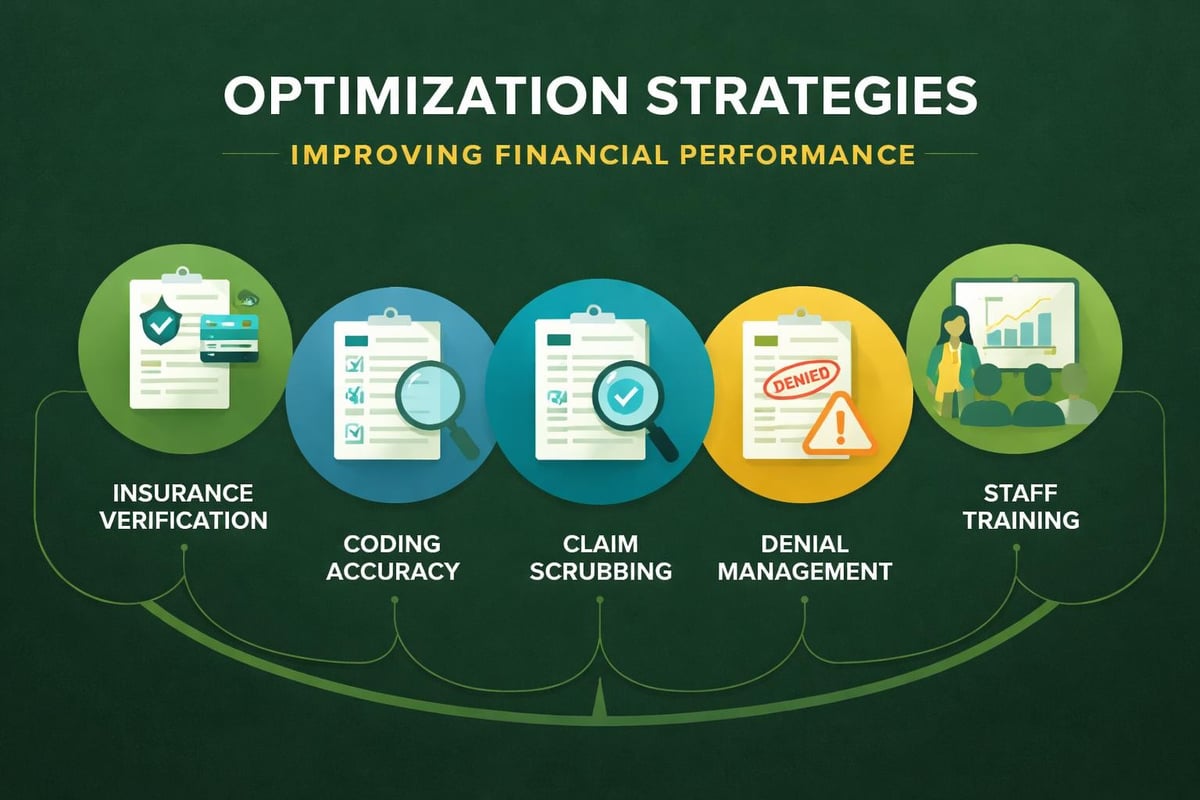
Best Practices for Provider Billing Optimization
Implementing proven strategies strengthens provider billing performance and accelerates revenue collection. Healthcare organizations should establish clear processes, invest in staff training, and leverage technology to reduce errors and improve efficiency.
1. Verify Insurance Eligibility at Every Encounter
Never assume that insurance coverage remains unchanged from previous visits. Patients switch plans, lose coverage, or modify their benefits regularly. Eligibility verification services performed before each appointment prevent claim denials related to inactive coverage or ineligible services.
2. Implement Front-End Controls
Catching errors before claim submission saves time and resources. Front-end controls include real-time eligibility verification, automated coding edits, and claim scrubbing technology that identifies potential issues. These preventive measures reduce denial rates significantly.
3. Maintain Coding Accuracy Through Continuous Education
Medical coding requirements evolve constantly. Annual CPT updates, quarterly ICD-10 revisions, and changing payer policies require ongoing staff education. Medical coding best practices emphasize the importance of certified coders, regular training sessions, and access to current coding resources.
4. Establish Robust Denial Management Processes
Denied claims require immediate attention to preserve revenue. Effective denial management in medical billing involves tracking denial patterns, identifying root causes, implementing corrective actions, and appealing unjustified denials. Organizations should designate specific staff members to manage denials and establish performance metrics to monitor resolution rates.
5. Enhance Communication with Payers and Patients
Clear, professional communication reduces billing disputes and accelerates payment. When contacting insurance companies, maintain detailed records of all interactions including representative names, reference numbers, and outcomes. Patient communication requires sensitivity and clarity, explaining financial responsibilities without medical jargon. The dos and don’ts of billing communication provide valuable guidance for maintaining positive relationships while pursuing payment.
Technology's Role in Provider Billing
Modern provider billing relies heavily on technology solutions that automate routine tasks, reduce errors, and provide real-time visibility into revenue cycle performance. Practice management systems, electronic health records, and specialized billing software work together to streamline operations.
Essential Technology Features
Healthcare organizations should seek billing technology offering these capabilities:
- Automated eligibility verification connecting to payer databases in real-time
- Integrated coding assistance suggesting appropriate codes based on documentation
- Electronic claim submission supporting multiple payer formats and requirements
- Denial tracking and reporting identifying patterns and monitoring resolution progress
- Revenue cycle analytics measuring key performance indicators and financial metrics
Many smaller practices struggle to maintain in-house technology infrastructure. Medical billing services for small practices provide access to enterprise-level technology without the capital investment, allowing practices to benefit from advanced systems while focusing clinical resources on patient care.
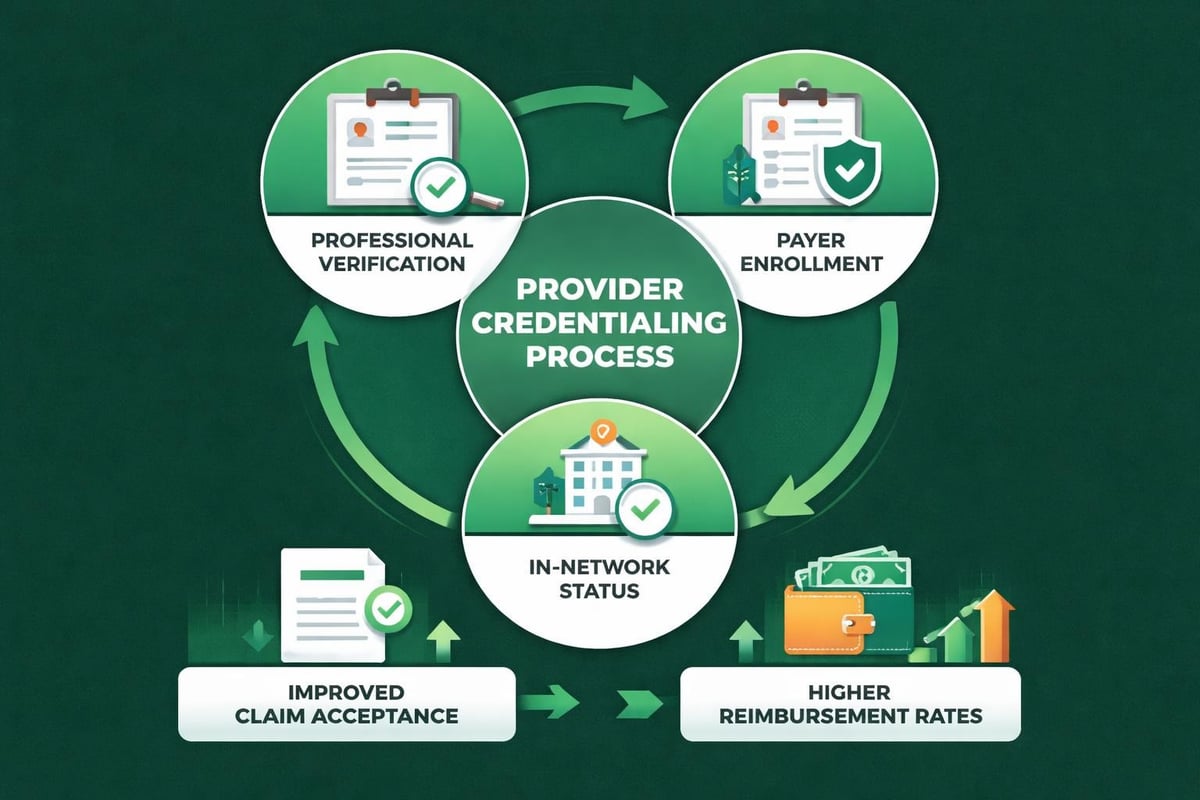
Credentialing and Network Participation
Provider billing success depends partly on proper credentialing and network participation. Physicians and facilities must complete credentialing with insurance companies before submitting claims as in-network providers. This process verifies professional qualifications, licensure, and malpractice coverage.
Credentialing delays can postpone revenue for months. Provider credentialing best practices emphasize starting the process early, maintaining current documentation, and tracking application status closely. Organizations offering medical credentialing services manage this complex process, ensuring providers can bill insurance companies without interruption.
Network participation agreements establish reimbursement rates and billing requirements for specific payers. Understanding contracted rates helps practices verify correct payment amounts and identify underpayments requiring correction.
Measuring Provider Billing Performance
Healthcare organizations must monitor specific metrics to evaluate billing performance and identify improvement opportunities. Key performance indicators provide objective data showing whether revenue cycle operations meet industry standards.
| Metric | Industry Benchmark | Significance |
|---|---|---|
| Clean Claim Rate | 95% or higher | Percentage of claims paid on first submission |
| Days in A/R | 30-40 days | Average time from service to payment |
| Denial Rate | Less than 5% | Percentage of claims initially denied |
| Collection Rate | 95% or higher | Percentage of expected revenue actually collected |
| Cost to Collect | 3-5% of collections | Administrative expense per dollar collected |
Tracking these metrics monthly reveals trends and highlights areas requiring attention. A declining clean claim rate might indicate coding issues or inadequate documentation. Rising days in accounts receivable could signal claim submission delays or ineffective follow-up processes.
Compliance Considerations in Provider Billing
Healthcare billing operates under strict regulatory oversight. The False Claims Act, Anti-Kickback Statute, Stark Law, and HIPAA all impose requirements on billing practices. Violations can result in substantial penalties, exclusion from federal programs, and criminal prosecution in severe cases.
Billing compliance programs should include these elements:
- Written policies and procedures documenting proper billing practices
- Regular compliance training for all revenue cycle staff
- Internal audits reviewing coding accuracy and billing practices
- Clear reporting mechanisms for suspected compliance violations
- Prompt investigation and correction of identified issues
The American Hospital Association’s patient billing guidelines offer a framework for establishing ethical billing practices that protect both organizations and patients. Healthcare providers should also consult resources like billing compliance guidance to ensure their practices align with current standards.
Prior Authorization Management
Many insurance companies require prior authorization for specific services, procedures, and medications. Obtaining authorization before service delivery prevents claim denials and reduces patient financial liability. However, the authorization process can be time-consuming and administratively burdensome.
Effective prior authorization management requires dedicated staff who understand payer-specific requirements and maintain detailed tracking systems. Missing authorization deadlines or failing to obtain necessary approvals creates billing complications that can delay or prevent payment entirely. Organizations offering prior authorization services handle this complex process, reducing administrative burden on clinical staff.
Streamlining Authorization Workflows
Healthcare practices can improve authorization efficiency through these strategies:
- Identifying services requiring authorization during scheduling
- Submitting authorization requests immediately upon scheduling
- Maintaining organized tracking systems for all pending authorizations
- Following up proactively on pending requests
- Communicating authorization status to clinical and billing teams
Revenue Cycle Integration
Provider billing does not operate in isolation. It represents one component of the broader revenue cycle, connecting to patient access, clinical documentation, charge capture, and collections. Optimizing billing performance requires coordination across all revenue cycle functions.
Healthcare revenue cycle management encompasses the entire financial process from patient pre-registration through final payment. Organizations achieving superior financial performance integrate their revenue cycle functions, ensuring seamless information flow between departments and minimizing handoff errors.
Strong revenue cycle performance depends on collaboration between clinical and administrative staff. Physicians must understand how documentation affects coding and reimbursement. Billing staff need access to clinical expertise when researching denials or responding to payer inquiries. This collaboration creates a culture where all team members recognize their role in financial sustainability.
Selecting Provider Billing Partners
Many healthcare organizations choose to outsource provider billing functions to specialized companies. This decision allows practices to focus clinical resources on patient care while leveraging billing expertise and technology investments maintained by revenue cycle management firms.
When evaluating potential billing partners, healthcare organizations should assess these factors:
Experience and Specialization: Does the billing company understand your specialty's unique coding requirements and payer relationships? Specialty-specific expertise produces better results than general billing knowledge.
Technology Capabilities: What systems does the billing company use? How will they integrate with your existing practice management and EHR systems? Seamless integration prevents duplicate data entry and reduces errors.
Transparency and Reporting: How frequently will you receive performance reports? What metrics will they track? Access to real-time data helps practices monitor financial performance and identify issues quickly.
Compliance and Security: How does the billing company protect patient information? What compliance certifications and audits do they maintain? HIPAA compliance and data security must be non-negotiable requirements.
Organizations researching top medical billing companies should request references, review performance guarantees, and clearly understand pricing structures before making commitments.
Patient Financial Responsibility
The shift toward high-deductible health plans has increased patient financial responsibility significantly. Collecting patient portions requires different strategies than pursuing insurance payment. Provider billing systems must accommodate payment plans, patient statements, and multiple payment methods.
Transparent communication about financial responsibility improves collection rates. Discussing costs before service delivery, explaining insurance benefits clearly, and offering payment options reduces surprise bills and patient complaints. Best practices for billing communication emphasize compassion and clarity when addressing patient financial concerns.
Organizations should establish clear financial policies covering:
- When and how to collect patient payments
- Payment plan eligibility and terms
- Financial assistance programs for qualifying patients
- Collection agency referral criteria
- Write-off policies for uncollectible balances
Documentation and Medical Necessity
Insurance companies pay for medically necessary services supported by appropriate documentation. Proving medical necessity requires clinical documentation that clearly explains why specific services were required for the patient's condition. Vague or incomplete documentation creates claim denial risk even when services were appropriate.
Clinical staff should document these elements for every patient encounter:
- Chief complaint and history of present illness establishing the reason for the visit
- Relevant medical history providing context for treatment decisions
- Physical examination findings supporting diagnoses and treatment plans
- Assessment and diagnoses using specific, accurate terminology
- Treatment plans and follow-up recommendations demonstrating appropriate care
Coders translate this documentation into billable codes, but they cannot create information that clinical staff failed to record. Regular feedback between coding and clinical teams improves documentation quality over time, supporting both compliance and optimal reimbursement.
The Future of Provider Billing
Provider billing continues to evolve alongside healthcare delivery models and payment structures. Value-based care models tie reimbursement to quality metrics and patient outcomes rather than service volume. These models require enhanced data tracking, quality reporting, and risk adjustment capabilities.
Artificial intelligence and machine learning technologies are beginning to impact provider billing operations. These tools can predict denial likelihood, suggest optimal coding, and identify revenue opportunities that human reviewers might miss. However, technology complements rather than replaces skilled billing professionals who bring judgment and expertise to complex situations.
Regulatory changes remain constant in healthcare. Billing professionals must stay informed about legislative developments, new payer policies, and emerging compliance requirements. Organizations investing in ongoing education and professional development position themselves to adapt quickly as the industry evolves.
Mastering provider billing requires expertise across coding, compliance, technology, and payer relationships, with performance directly impacting healthcare organizations' financial sustainability. Whether managing billing in-house or seeking specialized support, practices must prioritize accuracy, efficiency, and regulatory compliance to maximize reimbursements while maintaining positive patient relationships. Greenhive Billing Solutions delivers comprehensive revenue cycle management services specifically designed for healthcare providers, offering insurance eligibility verification, claims processing, denial management, and transparent reporting that improves financial performance. Our team of experienced professionals ensures HIPAA compliance while streamlining your billing operations and maximizing reimbursements across all payer types.