Managing financial operations in healthcare requires precision, expertise, and strategic oversight. Healthcare accounts receivable represents one of the most critical components of financial sustainability for medical practices, hospitals, and healthcare facilities. The complexity of insurance verification, claims processing, and payment collection creates challenges that directly impact cash flow and operational efficiency. Understanding how to optimize these processes determines whether a practice thrives or struggles financially.
Understanding Healthcare Accounts Receivable Fundamentals
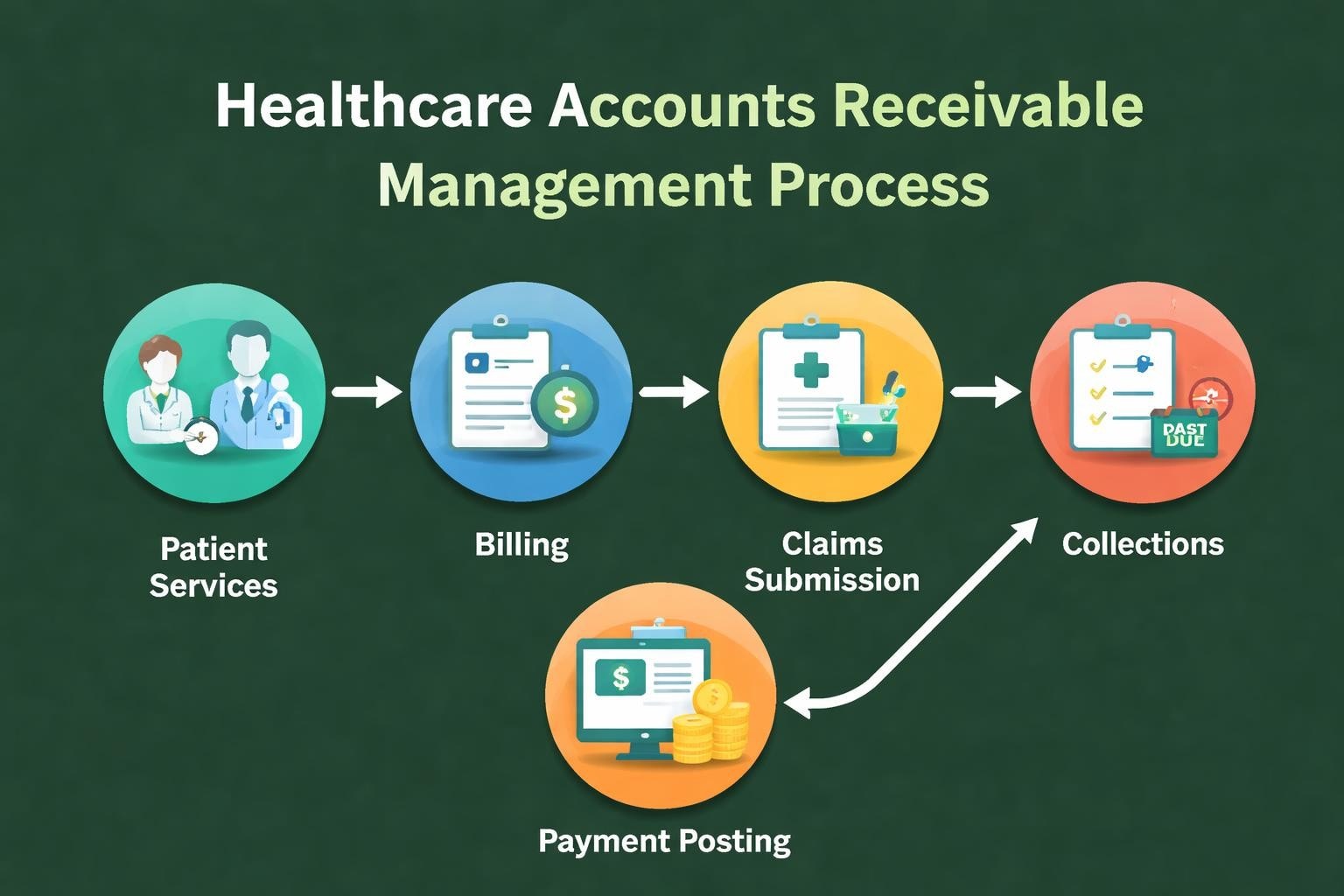
Healthcare accounts receivable encompasses all outstanding payments owed to medical providers for services rendered. This includes balances from insurance companies, government payers, and patients themselves. Unlike other industries where payment collection follows straightforward paths, healthcare receivables involve multiple layers of verification, coding, submission, and follow-up.
The timeline for collecting these receivables varies significantly based on payer type, claim complexity, and administrative efficiency. Medicare and Medicaid claims typically process within 14-30 days when submitted correctly, while commercial insurance claims may take 30-60 days or longer. Patient responsibility portions often extend collection timelines even further, particularly when practices lack robust patient payment policies.
Key Components of Receivables Management
Effective management requires attention to several interconnected elements. Each component plays a vital role in ensuring timely reimbursement and maintaining healthy cash flow.
Front-end operations set the foundation for successful collections. This includes patient registration accuracy, insurance eligibility verification, and authorization procurement. When front-desk staff capture complete demographic and insurance information, downstream processes run more smoothly. Verifying insurance eligibility before services reduces claim denials and accelerates payment cycles.
Mid-cycle processes involve charge capture, medical coding, and claims submission. Certified coders translate clinical documentation into standardized codes that payers recognize and reimburse. Accurate coding directly correlates with clean claim rates-the percentage of claims paid on first submission without errors or additional documentation requests.
Back-end operations focus on payment posting, denial management, and patient billing. This phase requires systematic follow-up on unpaid claims, appeals processing for denials, and patient collections strategies. Practices that excel at back-end operations maintain detailed workflows and assign specific staff members to monitor aging accounts.

Common Challenges That Disrupt Cash Flow
Healthcare providers face numerous obstacles when managing accounts receivable. Recognizing these challenges represents the first step toward implementing effective solutions.
Claim denials rank among the most significant issues impacting healthcare accounts receivable performance. According to industry research, the average denial rate ranges from 5% to 10%, though some practices experience rates exceeding 15%. Each denied claim requires additional staff time to investigate, correct, and resubmit. Understanding denial management in medical billing helps practices reduce these costly errors and recover revenue more efficiently.
Incomplete documentation creates another major barrier. When clinical notes lack specificity or fail to support billed services, payers reject claims or request additional information. These delays extend days in accounts receivable and increase administrative burden. Training clinical staff on documentation requirements aligned with coding guidelines minimizes these issues.
Patient collections have grown increasingly challenging as high-deductible health plans shift more financial responsibility to consumers. Many patients cannot afford large balances, leading to extended payment plans or write-offs. Common mistakes in healthcare accounts receivable management include failing to collect patient portions at time of service and lacking clear payment policies.
Technology Integration Gaps
Outdated systems or lack of integration between electronic health records (EHR), practice management software, and billing platforms creates inefficiencies. Manual data entry between systems increases error rates and slows processing times. Modern revenue cycle management requires seamless technology integration that automates routine tasks and provides real-time visibility into receivables status.
Staff members working with disconnected systems spend valuable time on redundant data entry rather than focusing on high-value activities like denial appeals or patient communication. This inefficiency directly impacts the bottom line through both lost revenue and increased operational costs.
Best Practices for Optimizing Collections
Implementing structured processes and proven methodologies transforms healthcare accounts receivable performance. These strategies address both preventive measures and corrective actions.
Establishing Clear Front-End Protocols
Step 1: Implement real-time eligibility verification for every patient encounter. This confirms coverage status, identifies patient responsibility amounts, and flags authorization requirements before services occur.
Step 2: Train registration staff on the importance of complete and accurate data collection. Every field in the patient registration system serves a purpose in the billing cycle. Missing or incorrect information creates downstream problems.
Step 3: Develop pre-service collection policies that outline when and how to collect patient portions. Studies show that collecting patient responsibility at time of service increases collection rates by 30-40% compared to post-service billing.
Step 4: Create authorization workflows for procedures and services requiring payer approval. Tracking authorization status prevents denials related to lack of pre-certification.
Optimizing Mid-Cycle Operations
Charge capture accuracy ensures that providers receive payment for all services rendered. Regular audits comparing scheduled appointments against billed services identify potential revenue leakage. Many practices discover 2-5% revenue loss from unbilled services during these reviews.
Clean claims in medical billing require precise coding based on complete documentation. Investing in ongoing coder education and implementing coding audits maintains high accuracy rates. Clean claim rates above 95% indicate excellent coding quality and process control.
Claim scrubbing technology identifies errors before submission to payers. These automated systems check for common mistakes like invalid code combinations, missing modifiers, or demographic mismatches. Addressing issues before submission significantly reduces denial rates.
| Metric | Industry Average | Best-in-Class |
|---|---|---|
| Clean Claim Rate | 75-85% | 95%+ |
| First-Pass Resolution | 80-85% | 92%+ |
| Days in AR | 45-50 days | <35 days |
| Denial Rate | 8-12% | <5% |
Strengthening Back-End Processes
Systematic denial management requires categorizing denials by reason code, identifying patterns, and implementing corrective actions. Effective denial management strategies focus on prevention rather than solely on appeals. Root cause analysis reveals whether denials stem from registration errors, coding issues, or payer policy changes.
Payment posting accuracy ensures proper credit allocation and identifies underpayments. Automated electronic remittance advice (ERA) processing reduces manual posting time while improving accuracy. Staff members can focus on variance analysis rather than data entry.
Aging accounts require prioritized attention based on balance size and collectability. Establishing workflows that automatically assign follow-up tasks based on aging categories ensures consistent attention to all outstanding balances. Best practices for managing accounts receivable in healthcare emphasize regular work queues and accountability measures.
Monitoring Key Performance Indicators
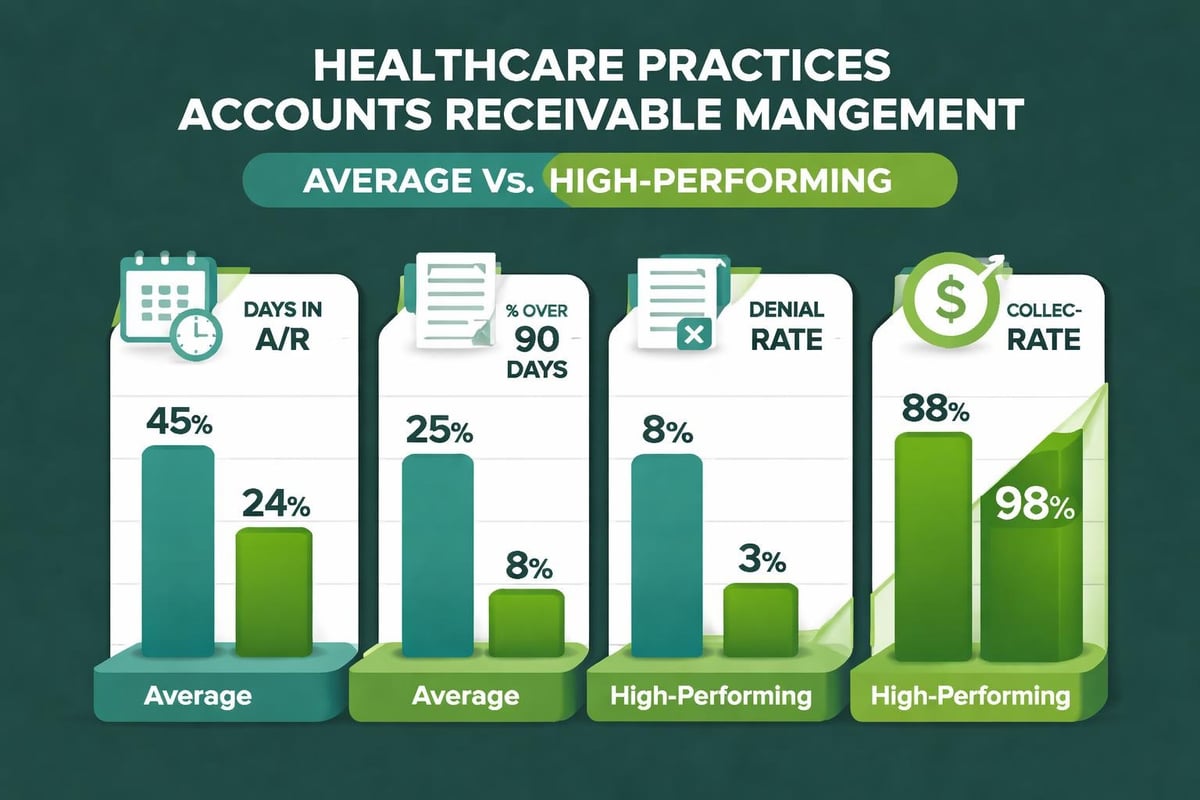
Data-driven management separates high-performing practices from those struggling with cash flow challenges. Regular monitoring of specific metrics provides early warning signs of emerging problems and validates improvement initiatives.
Days in accounts receivable measures the average time between service delivery and payment receipt. This calculation divides total accounts receivable by average daily charges. Lower numbers indicate faster payment cycles and healthier cash flow. Industry benchmarks vary by specialty, but most successful practices maintain days in AR below 40.
Accounts receivable aging categorizes outstanding balances by time periods: 0-30 days, 31-60 days, 61-90 days, 91-120 days, and over 120 days. The percentage of receivables in each category reveals collection effectiveness. High percentages in older categories signal collection problems requiring immediate attention.
Net collection rate compares actual collections against expected reimbursement after contractual adjustments. This metric reveals the percentage of collectible revenue actually received. Strong performers achieve net collection rates of 95% or higher, while struggling practices may see rates below 90%.
Understanding Revenue Cycle Velocity
Beyond static metrics, analyzing trends reveals whether initiatives improve performance over time. Month-over-month comparisons identify seasonal patterns and measure the impact of process changes. Revenue cycle analytics in healthcare enables data-driven decision making and resource allocation.
Segmenting metrics by payer type, service line, or provider reveals specific areas requiring attention. One insurance carrier might consistently process claims slower than others, indicating opportunities for payer relationship management. Certain service lines might demonstrate higher denial rates, suggesting focused coding education needs.
- Gross collection rate: Total payments divided by total charges
- Adjusted collection rate: Payments divided by (charges minus contractual adjustments)
- Point-of-service collections: Patient payments collected before or at service delivery
- Cost to collect: Total collection costs divided by total collections
Technology Solutions That Drive Results
Modern healthcare accounts receivable management depends heavily on technology platforms that automate routine tasks, reduce errors, and provide actionable insights. Strategic technology selection and implementation create competitive advantages.
Integrated Revenue Cycle Platforms
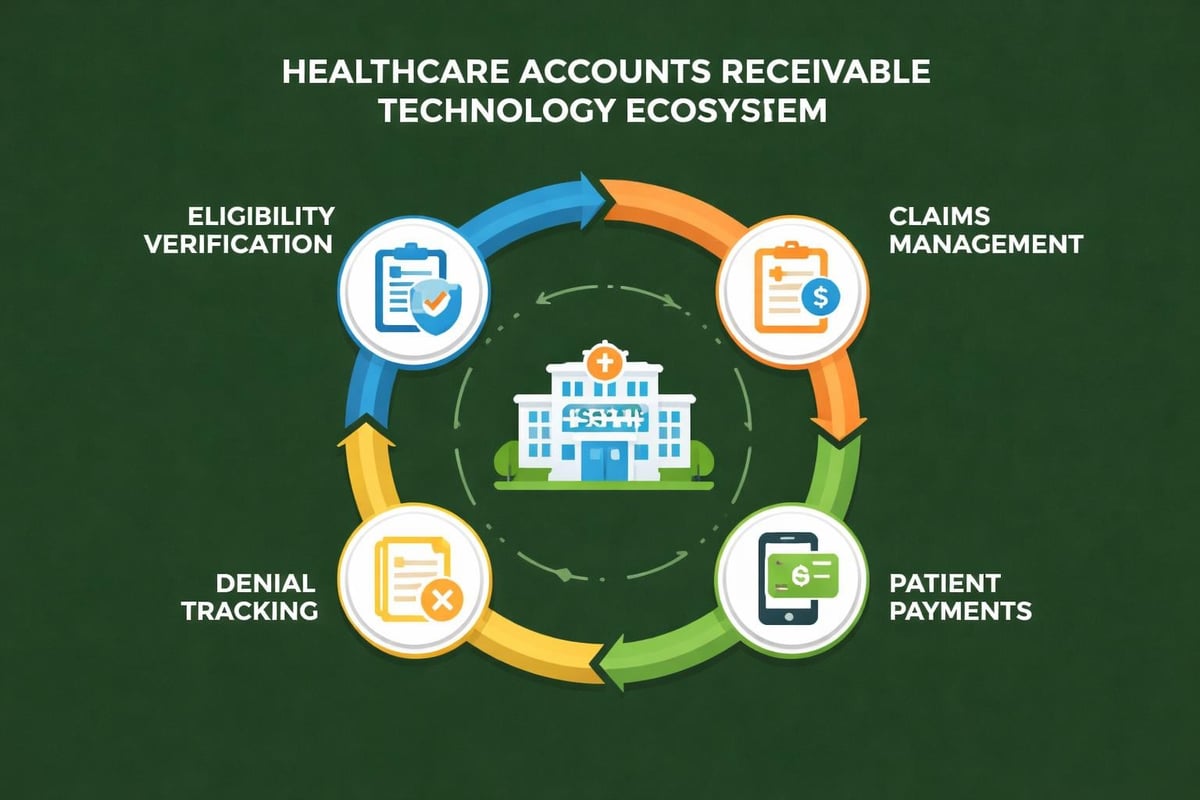
Comprehensive platforms connect clinical documentation, coding, billing, and collections within unified systems. This integration eliminates manual handoffs and ensures data consistency throughout the revenue cycle. Revenue cycle management tools streamline workflows and improve visibility across all operational stages.
These systems typically include modules for eligibility verification, charge capture, claims management, denial tracking, and patient payment processing. Real-time dashboards display current performance against targets, enabling rapid response to emerging issues.
Artificial intelligence and machine learning capabilities enhance traditional automation. These technologies identify patterns in denial data, predict claim outcomes before submission, and recommend optimal coding selections based on documentation. Early adopters report significant improvements in clean claim rates and reduced denial volumes.
Specialized Applications
Denial management software tracks every denied claim from identification through resolution. These applications categorize denials, assign work queues, monitor appeal deadlines, and measure recovery rates. Analytics identify root causes and trending patterns that inform preventive strategies.
Patient engagement platforms facilitate communication regarding financial responsibility. Automated appointment reminders include estimated patient portions, payment portals enable online transactions, and text messaging options increase accessibility. Best practices outlined by industry experts emphasize the importance of clear patient communication in improving collection rates.
Eligibility verification tools automate insurance checks and flag coverage issues before services occur. Real-time verification reduces claim denials related to eligibility while improving patient registration efficiency. These systems integrate with scheduling platforms to check coverage when appointments are booked.
Staff Training and Development Priorities
Technology alone cannot optimize healthcare accounts receivable performance. Skilled staff members who understand revenue cycle complexities and payer requirements drive sustainable improvements.
Clinical documentation specialists bridge the gap between providers and coders. These professionals educate physicians on documentation requirements that support accurate coding and reduce queries. When clinical notes clearly describe medical necessity, severity, and specificity, coding accuracy improves dramatically.
Billing specialists require ongoing education about payer policy changes, coding updates, and regulatory requirements. Annual CPT and ICD-10 code revisions demand continuous learning. Understanding various revenue coding requirements ensures compliance while maximizing appropriate reimbursement.
Patient financial counselors need training in communication strategies that balance empathy with firm collection policies. These staff members explain benefits, discuss payment options, and establish payment plans. Their effectiveness directly impacts patient satisfaction scores and collection rates.
Creating Cross-Functional Understanding
Revenue cycle success requires collaboration between clinical, administrative, and financial teams. Regular meetings that include representatives from each area foster shared understanding of how individual roles impact overall performance. When registration staff understand how incomplete information causes claim denials, they become more diligent about data accuracy.
Case study discussions reviewing specific denied claims or collection challenges provide valuable learning opportunities. Teams analyze what went wrong, identify prevention strategies, and implement process improvements. Common pitfalls in healthcare accounts receivable often stem from siloed operations lacking cross-functional communication.
Payer Contract Management Considerations
Understanding contractual relationships with insurance companies influences healthcare accounts receivable strategies. Fee schedules, payment terms, and claim filing deadlines vary significantly across payers.
Credentialing maintenance ensures uninterrupted billing capabilities. Expired credentials result in claim denials and payment delays. Establishing credentialing calendars with renewal reminders prevents these avoidable issues. Revenue cycle best practices emphasize proactive credential management as foundational to financial stability.
Contract analysis reveals whether actual payments align with contracted rates. Regular audits comparing remittances against fee schedules identify underpayments requiring correction. Many practices discover 1-3% revenue recovery through systematic contract compliance monitoring.
Timely filing limits vary by payer, ranging from 90 days to one year after service dates. Missing these deadlines results in complete payment denials regardless of claim validity. Tracking submission dates and payer-specific requirements prevents these costly errors.
| Payer Type | Typical Filing Limit | Average Payment Time |
|---|---|---|
| Medicare | 12 months | 14-21 days |
| Medicaid | 12 months (varies by state) | 21-30 days |
| Commercial | 90-180 days | 30-45 days |
| Workers' Compensation | 12 months | 45-60 days |
Outsourcing Versus In-House Management
Healthcare organizations face strategic decisions about whether to manage accounts receivable internally or partner with specialized service providers. Each approach offers distinct advantages depending on practice size, resources, and expertise.
In-house management provides direct control over revenue cycle operations and immediate access to billing staff. Larger organizations with sufficient volume to support dedicated teams often prefer this approach. However, recruiting and retaining qualified billing professionals presents ongoing challenges, particularly in competitive labor markets.
Outsourced solutions leverage specialized expertise and economies of scale. Working with experienced revenue cycle management partners provides access to advanced technology, certified coders, and established best practices without capital investment. Service providers assume responsibility for staffing, training, and performance outcomes.
Hybrid models combine internal oversight with external support for specific functions. Some practices maintain front-end operations in-house while outsourcing complex denial management or patient collections. This approach balances control with specialized expertise where most needed.
Evaluation Criteria for Service Providers
Organizations considering outsourcing should evaluate potential partners across multiple dimensions. HIPAA compliance represents a non-negotiable requirement, as billing partners access protected health information. Comprehensive security protocols and business associate agreements protect patient privacy and organizational liability.
Technology capabilities determine operational efficiency and reporting quality. Modern platforms should offer real-time access to financial data, customizable reports, and integration with existing practice management systems. Implementing appropriate billing software solutions enables transparency and accountability.
Industry specialization matters significantly. Medical billing requirements vary substantially across specialties. Partners with relevant experience understand specialty-specific coding nuances, common denial patterns, and payer relationships. This expertise translates directly into improved collection rates.
Compliance and Regulatory Considerations
Healthcare accounts receivable management operates within extensive regulatory frameworks. Maintaining compliance protects organizations from financial penalties, legal liability, and reputational damage.
HIPAA requirements govern how patient financial information is stored, transmitted, and accessed. Billing operations must implement appropriate safeguards including encryption, access controls, and audit trails. Regular risk assessments identify vulnerabilities requiring remediation.
Stark Law and Anti-Kickback Statute regulations influence financial relationships between providers and referral sources. Billing arrangements must avoid structures that could be construed as payment for referrals. Legal review of service agreements ensures compliance with these complex requirements.
Fair Debt Collection Practices Act (FDCPA) applies to patient collections, particularly when organizations use third-party collection agencies. Understanding prohibited practices prevents violations that trigger patient complaints and regulatory scrutiny. Strategies for managing accounts receivable must balance effective collections with respectful patient interactions.
State-Specific Regulations
Individual states impose additional requirements affecting billing operations. Some states mandate specific notice periods before sending accounts to collections or limit interest rates on patient balances. Multistate organizations must navigate varying requirements across jurisdictions.
Surprise billing regulations enacted at federal and state levels impact how practices bill patients for out-of-network services. Understanding good faith estimate requirements and dispute resolution processes ensures compliance while protecting revenue.
Patient-Centric Collection Approaches
Modern healthcare accounts receivable strategies recognize that patients represent both consumers and customers. Positive financial experiences influence patient satisfaction, retention, and reputation.
Price transparency initiatives empower patients to understand costs before receiving services. Providing good faith estimates for common procedures, explaining insurance coverage, and discussing payment expectations builds trust. Transparency reduces billing disputes and improves collection rates.
Flexible payment options acknowledge financial challenges many patients face. Offering payment plans with reasonable terms increases the likelihood of full balance recovery compared to demanding immediate payment. Digital payment portals provide convenient 24/7 access that aligns with consumer preferences.
Financial assistance programs support patients who qualify based on income and resources. Establishing clear policies for charity care and discounts demonstrates community commitment while ensuring consistent application of assistance criteria. Proper documentation protects these write-offs during audits.
Communication strategies should emphasize clarity and empathy. Understanding healthcare accounts receivable challenges helps staff members explain complex billing situations in accessible terms. Training financial counselors in de-escalation techniques and problem-solving approaches improves patient interactions.
Measuring Return on Investment
Healthcare organizations investing in revenue cycle improvements must quantify financial impact to justify continued resource allocation. Comprehensive measurement examines both direct revenue gains and operational efficiency improvements.
Revenue increase calculations compare collections before and after implementing new processes or technologies. Tracking metrics like net collection rate, days in AR, and denial rates reveals whether initiatives achieve intended outcomes. Successful implementations typically demonstrate measurable improvement within 90-120 days.
Cost reduction analysis examines staffing efficiency, write-off percentages, and administrative expenses. Automation that reduces manual tasks enables staff reallocation to higher-value activities. Comprehensive healthcare revenue cycle management approaches optimize both revenue and cost structures.
Opportunity cost assessment considers what financial resources tied up in accounts receivable could achieve if collected more quickly. Faster collection cycles improve cash flow available for practice investments, debt reduction, or operational expenses. This liquidity advantage provides strategic flexibility beyond simple revenue metrics.
Long-Term Strategic Value
Beyond immediate financial metrics, effective healthcare accounts receivable management creates sustainable competitive advantages. Practices known for billing accuracy and respectful collection approaches attract and retain patients. Provider satisfaction improves when administrative burdens decrease, reducing turnover and recruitment costs.
Strong revenue cycle performance enables strategic investments in clinical programs, technology upgrades, and facility improvements. Financial stability positions organizations to weather industry changes including regulatory shifts, payer policy modifications, and reimbursement pressures.
Optimizing healthcare accounts receivable requires comprehensive strategies addressing technology, processes, staff capabilities, and patient relationships. Successful organizations implement systematic approaches that prevent denials, accelerate collections, and maintain compliance while delivering positive patient experiences. When practices struggle with revenue cycle challenges or lack internal expertise to achieve best-in-class performance, partnering with specialized providers offers proven solutions. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to maximize reimbursements, improve cash flow, and streamline operations for healthcare providers nationwide. Our experienced team combines industry expertise with transparent communication to help practices achieve their financial goals while maintaining focus on patient care.