Healthcare providers face mounting pressure to maintain financial stability while delivering quality patient care. Understanding the rcm cycle has become critical for practices seeking to optimize revenue flow and reduce administrative burden. This comprehensive framework encompasses every financial interaction from initial patient contact through final payment, creating a seamless process that directly impacts your bottom line. For healthcare organizations partnering with revenue cycle management service providers, mastering these fundamentals ensures better collaboration and maximized reimbursements.
Understanding the RCM Cycle Framework
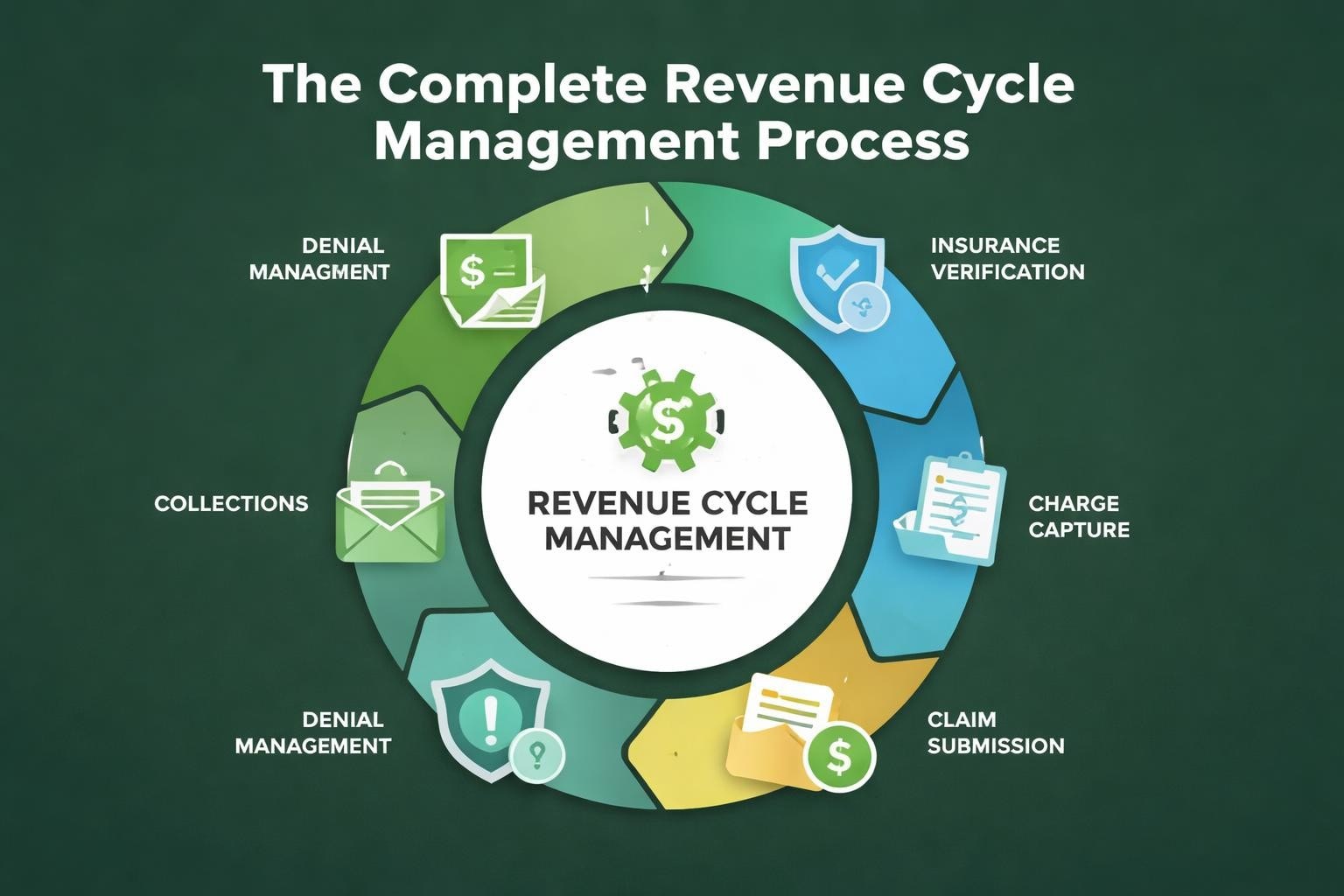
The rcm cycle represents the complete financial journey of a patient encounter within a healthcare organization. This cyclical process begins the moment a patient schedules an appointment and continues through billing, payment collection, and account reconciliation. Unlike linear workflows, the revenue cycle operates as a continuous loop where each phase influences subsequent stages and overall financial performance.
Healthcare providers rely on this framework to track revenue generation, identify bottlenecks, and measure operational efficiency. According to the Healthcare Financial Management Association’s overview of RCM, organizations that optimize their revenue cycle processes see significant improvements in days in accounts receivable and clean claim rates. The cycle encompasses both clinical and administrative functions, requiring coordination across multiple departments.
Key Components of an Effective Revenue Cycle
A well-structured rcm cycle includes several interdependent components that work together to ensure financial success:
- Patient access and registration with accurate demographic and insurance information
- Insurance verification and authorization to confirm coverage before service delivery
- Charge capture and coding that translates clinical services into billable procedures
- Claims submission following payer-specific requirements and timelines
- Payment posting and reconciliation for both insurance and patient payments
- Denial management and appeals to recover rejected claims
- Patient billing and collections for outstanding balances
Each component requires specific expertise and attention to detail. Missing information during registration can cascade into claim denials weeks later, while coding errors lead to underpayment or compliance issues.
The Front-End Revenue Cycle Process
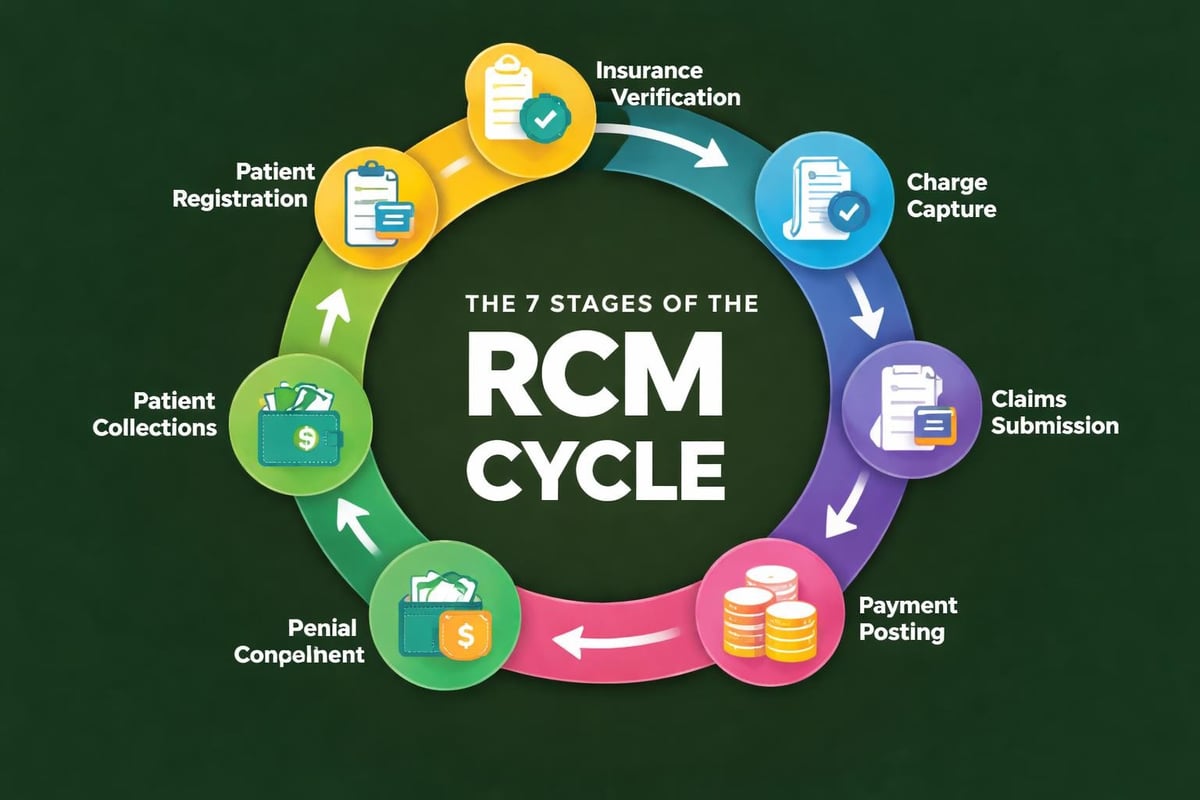
Front-end operations set the foundation for successful revenue capture. This phase encompasses all activities occurring before or during patient service delivery, making it crucial for preventing downstream revenue leakage.
Patient Registration and Demographic Accuracy
Patient registration represents the first critical touchpoint in the rcm cycle. Collecting complete and accurate demographic information prevents claim rejections and delays. Registration staff must verify patient identity, confirm contact information, and document insurance details with precision.
Common front-end challenges include incomplete forms, outdated insurance information, and data entry errors. These issues contribute to an estimated 80% of claim denials according to TechTarget’s comprehensive definition of revenue cycle management. Implementing standardized registration protocols and staff training reduces these preventable errors.
Insurance Verification and Eligibility Confirmation
Verifying insurance coverage before service delivery protects both providers and patients from unexpected financial responsibility. This step confirms active coverage, identifies co-pays and deductibles, and determines whether prior authorization is required for planned procedures.
Real-time eligibility verification has become the industry standard, allowing practices to confirm coverage instantly rather than waiting days for manual verification. Professional revenue cycle management services handle this time-intensive process, ensuring that practices can verify medical insurance efficiently without burdening clinical staff.
| Verification Element | Purpose | Impact of Errors |
|---|---|---|
| Coverage Status | Confirms active policy | Denied claims, patient disputes |
| Benefit Limitations | Identifies service restrictions | Unexpected patient liability |
| Prior Authorization | Secures payer approval | Claim denials, delayed payment |
| Co-pay Requirements | Determines patient responsibility | Collection challenges |
Mid-Cycle Revenue Management
The mid-cycle phase bridges clinical service delivery with financial transactions. This segment of the rcm cycle focuses on accurate documentation, proper coding, and timely claim submission.
Charge Capture and Documentation
Charge capture ensures that all billable services receive proper documentation and coding. Missed charges represent direct revenue loss, while undercoding leaves money on the table. Healthcare providers must establish robust processes to capture every eligible service, from routine office visits to complex procedures.
Charge entry in medical billing requires meticulous attention to detail and understanding of documentation requirements. Specialized billing professionals review encounter forms, cross-reference clinical notes, and apply appropriate codes before claim creation.
Medical Coding and Compliance
Accurate medical coding translates clinical documentation into standardized codes that payers recognize and reimburse. Professional coders apply CPT, ICD-10, and HCPCS codes based on provider documentation, ensuring compliance with coding guidelines and payer policies.
The complexity of medical coding in revenue cycle management continues to increase with expanding code sets and evolving regulations. Coding errors lead to:
- Claim denials requiring rework and appeals
- Payment delays that strain cash flow
- Compliance risks including audit exposure
- Revenue leakage from undercoding
- Patient dissatisfaction due to billing confusion
Understanding what CPT codes are used for insurance in healthcare claims enables providers to optimize reimbursement while maintaining compliance.
Back-End Revenue Cycle Operations
Back-end processes focus on payment collection, denial resolution, and financial reconciliation. This phase determines how quickly and completely practices receive payment for services rendered.
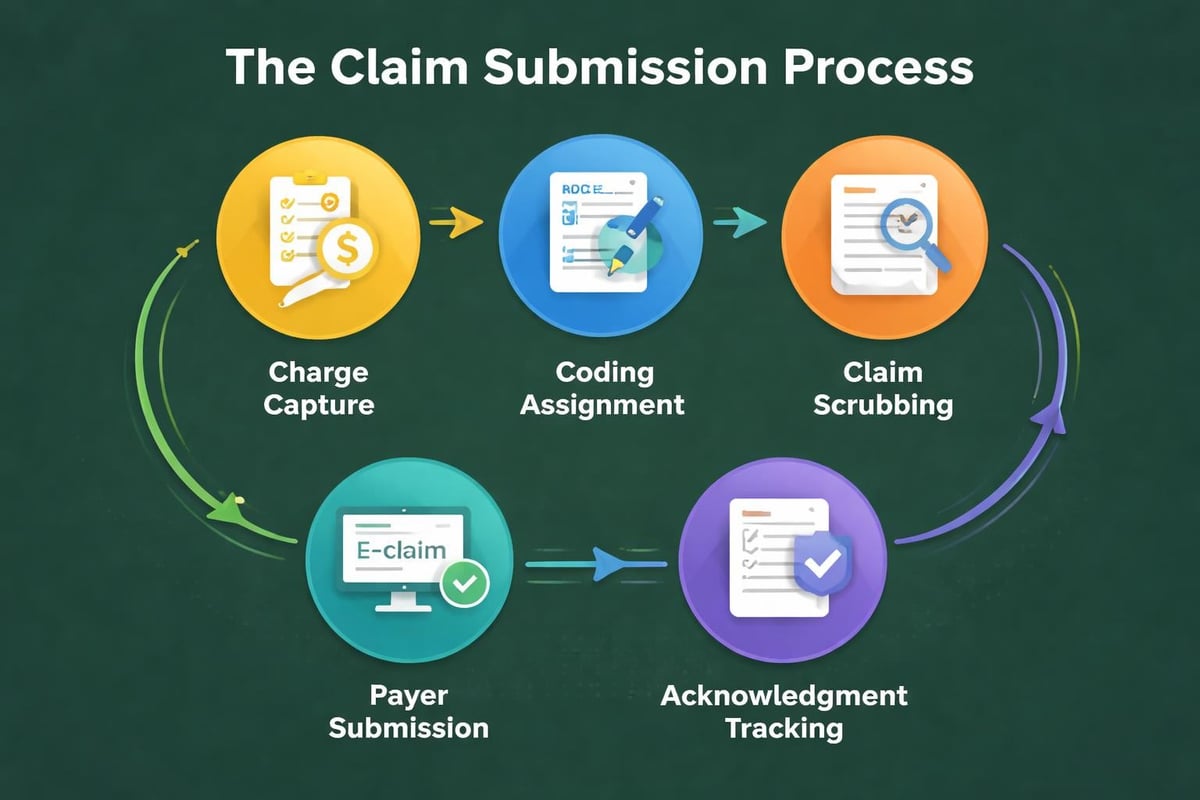
Claims Processing and Payment Posting
Once submitted, claims undergo payer adjudication where insurance companies review documentation, verify coverage, and determine payment amounts. Practices must monitor claim status, respond to payer requests promptly, and post payments accurately.
Electronic remittance advice (ERA) streamlines payment posting by providing standardized digital explanations of benefits. Understanding what ERA means in medical billing helps practices automate reconciliation and identify payment variances quickly.
Payment posting accuracy ensures financial reports reflect true receivables and revenue. Staff must reconcile payments against billed charges, post adjustments correctly, and flag discrepancies for review.
Denial Management and Appeals
Denial management represents a critical component of the rcm cycle that directly impacts revenue recovery. Insurance denials occur for numerous reasons, from simple administrative errors to complex medical necessity disputes. Effective denial management requires:
- Systematic denial tracking to identify patterns and root causes
- Timely appeals submission within payer-specific deadlines
- Strong documentation supporting medical necessity and coverage
- Process improvements addressing recurring denial reasons
Organizations implementing robust denial management in medical billing recover 60-70% of denied claims through appeals. Professional revenue cycle services bring expertise in payer policies and appeals processes that maximize recovery rates.
| Denial Category | Common Causes | Resolution Strategy |
|---|---|---|
| Technical | Missing information, coding errors | Correct and resubmit |
| Authorization | Lack of prior approval | Retroactive authorization or appeal |
| Medical Necessity | Insufficient documentation | Clinical appeal with supporting notes |
| Timely Filing | Missed submission deadlines | Process review and prevention |
Patient Financial Responsibility
Patient collections have grown substantially as high-deductible health plans shift more cost responsibility to consumers. Managing patient balances requires clear communication, convenient payment options, and professional collection practices.
Patient Billing and Communication
Transparent billing statements help patients understand their financial responsibility and encourage timely payment. Effective patient billing includes:
- Clear itemization of services rendered
- Explanation of insurance adjustments and payments
- Outstanding balance displayed prominently
- Multiple payment options including online portals
- Payment plan availability for larger balances
Many patients struggle to understand adjustments on medical bills and how insurance processing affects their responsibility. Educational communication reduces confusion and disputes.
Collection Strategies and Patient Relations
Balancing revenue collection with patient satisfaction requires strategic approaches that maintain relationships while securing payment. Professional collection practices include:
- Pre-service estimates for scheduled procedures
- Point-of-service collection for known co-pays and deductibles
- Payment plans for balances exceeding patient capacity
- Multiple communication channels (mail, phone, email, text)
- Compliance with FDCPA regulations and ethical standards
Revenue cycle billing professionals understand how to navigate sensitive financial conversations while preserving the patient-provider relationship that drives long-term practice success.
Optimizing Your RCM Cycle Performance
Continuous improvement separates high-performing revenue cycles from those plagued by inefficiency and revenue leakage. Healthcare providers should regularly assess performance metrics and implement targeted improvements.
Key Performance Indicators
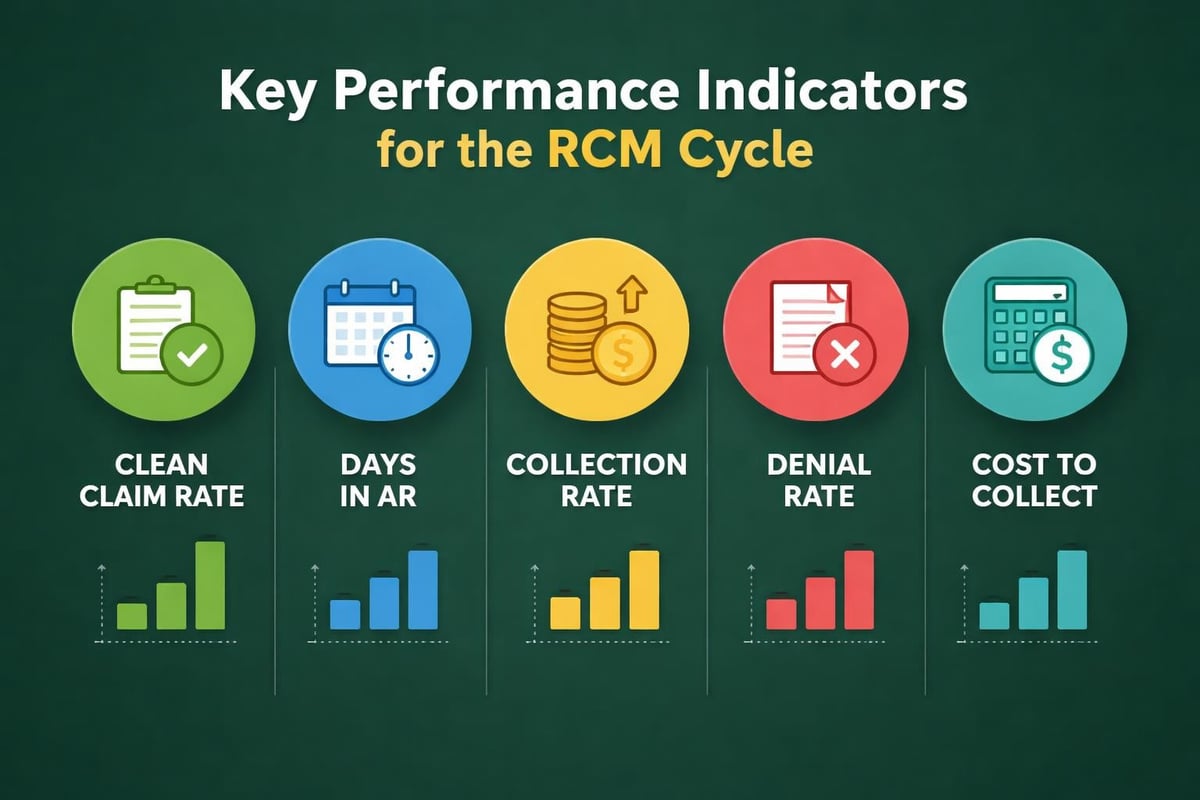
Measuring rcm cycle effectiveness requires tracking specific metrics that reveal operational health:
| Metric | Target Range | Significance |
|---|---|---|
| Clean Claim Rate | 95-98% | Claims accepted without rework |
| Days in AR | 30-40 days | Speed of revenue collection |
| Collection Rate | >95% | Effectiveness capturing net revenue |
| Denial Rate | <5% | Quality of submission processes |
| Cost to Collect | <3% of revenue | Operational efficiency |
Organizations tracking these metrics identify improvement opportunities and benchmark against industry standards. Healthcare revenue cycle analytics provide actionable insights that drive strategic decisions.
Best Practices for Revenue Cycle Excellence
Industry leaders implement proven strategies that optimize the rcm cycle across all phases. Experian Health’s guide to revenue cycle management best practices emphasizes standardization and technology adoption.
Front-End Best Practices:
- Real-time insurance verification at scheduling
- Patient financial counseling before service
- Automated eligibility checking systems
- Staff training on documentation requirements
Mid-Cycle Best Practices:
- Regular coding audits and feedback
- Charge capture reviews to prevent leakage
- Claim scrubbing before submission
- Specialized expertise for complex procedures
Back-End Best Practices:
- Denial tracking and trending analysis
- Automated payment posting with ERA integration
- Dedicated denial management workflows
- Patient-friendly billing statements and portals
Technology and the Modern RCM Cycle
Technology integration has transformed revenue cycle management from manual, paper-intensive processes to streamlined digital workflows. Modern practices leverage sophisticated platforms that automate routine tasks and provide real-time visibility into financial performance.
Revenue Cycle Management Systems
Comprehensive RCM platforms integrate with electronic health records, practice management systems, and clearinghouses to create seamless data flow. These systems automate eligibility verification, claim scrubbing, payment posting, and reporting functions that previously required substantial manual effort.
Healthcare providers partnering with professional revenue cycle management services benefit from expertise across top medical billing software platforms without capital investment in technology infrastructure. Service providers maintain current systems and adapt to client preferences.
Automation and Artificial Intelligence
Emerging technologies bring new capabilities to the rcm cycle:
- Automated coding suggestions based on clinical documentation
- Predictive analytics identifying denial risks before submission
- Intelligent claim routing to appropriate payers
- Chatbots handling routine patient billing inquiries
- Machine learning detecting patterns in denials and underpayments
While technology enhances efficiency, human expertise remains essential for complex coding decisions, appeal writing, and patient communication. The optimal approach combines technological capabilities with skilled professionals who understand healthcare reimbursement nuances.
Specialty-Specific Revenue Cycle Considerations
Different medical specialties face unique rcm cycle challenges requiring tailored approaches. Understanding specialty-specific requirements ensures optimal revenue capture and compliance.
Behavioral Health Revenue Cycle Management
Mental health and substance abuse treatment providers navigate complex coverage limitations, prior authorization requirements, and stigma-related billing sensitivities. Medical billing for behavioral health requires specialized knowledge of mental health parity laws and behavioral health-specific coding.
Behavioral health organizations often encounter higher denial rates due to medical necessity documentation requirements and session limit policies. Professional billing services with behavioral health expertise improve reimbursement outcomes through proper documentation guidance and effective appeals.
Urgent Care Revenue Cycle Challenges
Urgent care centers face unique revenue cycle pressures including high patient volumes, walk-in encounters without pre-registration, and frequent out-of-network scenarios. Urgent care revenue cycle management demands efficient front-end processes and expertise navigating varied payer contracts.
Point-of-service collection becomes critical in urgent care settings where patients may not return for future visits. Streamlined registration and real-time eligibility checking enable staff to collect appropriate co-pays and estimate patient responsibility accurately.
Primary Care and Physician RCM
Primary care practices balance high patient volumes with complex coding requirements for evaluation and management services, preventive care, and chronic disease management. Physician RCM encompasses everything from wellness visit coding to understanding contractual adjustments from multiple payer contracts.
Understanding why contractual adjustments in medical billing remain essential helps practices accurately forecast revenue and negotiate favorable payer contracts.
Common RCM Cycle Challenges and Solutions
Healthcare providers across all specialties encounter recurring obstacles that impede revenue cycle performance. Identifying these challenges enables targeted interventions that improve financial outcomes.
Staffing and Expertise Gaps
Recruiting and retaining qualified billing and coding staff presents ongoing challenges, particularly for smaller practices. The specialized knowledge required for effective revenue cycle management extends beyond basic billing skills to include:
- Current procedural and diagnostic coding systems
- Payer-specific policies and claim requirements
- Compliance regulations and documentation standards
- Denial management and appeals processes
- Patient communication and collection strategies
Many practices find that partnering with specialized revenue cycle management services addresses expertise gaps while reducing overhead associated with staff recruitment, training, and turnover.
Payer Complexity and Policy Changes
Insurance companies continuously update policies, coverage criteria, and claim submission requirements. Staying current with these changes across multiple payers strains internal resources and increases denial risk.
Professional billing services maintain dedicated teams monitoring payer updates, analyzing policy changes, and adjusting workflows accordingly. This proactive approach prevents denials and ensures practices capitalize on reimbursement opportunities.
Compliance and Regulatory Requirements
Healthcare billing compliance encompasses numerous regulations including HIPAA privacy rules, anti-kickback statutes, and payer-specific billing requirements. Non-compliance exposes practices to audits, penalties, and reputational damage.
Organizations must balance aggressive revenue pursuit with conservative compliance practices. Understanding different types of medical coding helps providers maintain documentation standards that support both reimbursement and audit defense.
Building a Sustainable Revenue Cycle Strategy
Long-term financial health requires more than addressing immediate revenue cycle problems. Healthcare providers benefit from strategic planning that aligns revenue cycle operations with organizational goals and market dynamics.
Partnering with Revenue Cycle Management Services
Many healthcare organizations discover that outsourcing revenue cycle functions delivers superior results compared to maintaining internal billing departments. Professional services bring:
Specialized Expertise: Dedicated teams with deep knowledge across multiple specialties and payer types
Scalability: Flexible capacity that adjusts to volume fluctuations without hiring or layoffs
Technology Access: Enterprise-grade systems without capital investment
Compliance Support: Ongoing monitoring of regulatory changes and requirements
Performance Transparency: Detailed reporting and analytics for informed decision-making
The revenue cycle process in healthcare benefits from experienced professionals who understand both the clinical and financial aspects of practice operations.
Continuous Improvement Culture
High-performing revenue cycles require commitment to ongoing evaluation and enhancement. Practices should establish regular review cycles that:
- Analyze performance metrics against benchmarks and historical trends
- Identify root causes of denials, delays, and inefficiencies
- Implement corrective actions with clear accountability and timelines
- Monitor results to validate improvement effectiveness
- Share learnings across teams to prevent recurring issues
This systematic approach transforms the rcm cycle from a transactional process into a strategic advantage that supports practice growth and financial stability.
Mastering the rcm cycle requires understanding each phase's interdependencies and implementing best practices that optimize revenue capture while maintaining compliance. Healthcare providers seeking to enhance financial performance, reduce administrative burden, and ensure maximum reimbursements benefit from partnering with experienced revenue cycle management specialists. Greenhive Billing Solutions delivers comprehensive revenue cycle services tailored to your practice's unique needs, combining expert billing professionals with transparent communication and HIPAA-compliant processes. Our team adapts to your existing systems and workflows, handling everything from insurance verification through denial management so you can focus on delivering exceptional patient care.