Healthcare providers today face mounting pressure to optimize financial performance while maintaining quality patient care. The complexity of medical billing, insurance verification, and claims processing demands solutions that deliver results quickly and accurately. Rapid RCM solutions have emerged as critical tools for practices seeking to reduce payment delays, minimize denials, and improve overall revenue cycle efficiency. By implementing streamlined processes and leveraging specialized expertise, healthcare organizations can transform their financial operations and achieve sustainable growth.
Understanding the Foundation of Rapid RCM Solutions
Rapid RCM solutions represent a comprehensive approach to revenue cycle management that prioritizes speed, accuracy, and continuous improvement. Unlike traditional billing methods that often involve lengthy processing times and manual interventions, these solutions focus on accelerating every stage of the revenue cycle.
The core principle behind rapid RCM solutions involves eliminating bottlenecks that slow down cash flow. From patient registration through final payment collection, each touchpoint receives attention to ensure maximum efficiency. This approach recognizes that delays at any stage create compounding problems downstream.
Key Components That Drive Rapid Processing
Several fundamental elements work together to create truly rapid RCM solutions:
- Automated eligibility verification that confirms insurance coverage before services
- Real-time claim scrubbing to identify and correct errors before submission
- Accelerated charge entry processes that reduce lag time between service delivery and billing
- Proactive denial management systems that address rejections immediately
- Streamlined payment posting that updates accounts within hours, not days
Healthcare organizations implementing comprehensive revenue cycle management services recognize that speed without accuracy creates additional problems. The goal involves achieving both simultaneously through systematic process improvement.
The Business Impact of Accelerated Revenue Cycle Operations
Financial performance metrics improve dramatically when healthcare practices adopt rapid RCM solutions. Days in accounts receivable drop significantly, often from 45-60 days to 30-35 days or less. This acceleration releases capital that practices can reinvest in equipment, staff, or facility improvements.
Clean claim rates represent another critical metric affected by rapid processing. Traditional billing operations often achieve clean claim rates between 75-85%, while optimized rapid RCM solutions push this figure above 95%. Each percentage point improvement translates directly into reduced rework and faster payments.
Measuring the Financial Benefits
| Metric | Traditional RCM | Rapid RCM Solutions | Improvement |
|---|---|---|---|
| Days in A/R | 45-60 days | 30-35 days | 25-42% faster |
| Clean Claim Rate | 75-85% | 95-98% | 12-23% higher |
| Denial Rate | 8-12% | 2-4% | 67-75% reduction |
| Collection Rate | 92-94% | 97-99% | 3-7% increase |
The revenue impact extends beyond simple acceleration. Practices using rapid RCM solutions experience fewer write-offs due to timely filing limits. When claims move through the system quickly, they reach payers well before deadlines expire. This seemingly simple improvement prevents thousands of dollars in lost revenue annually.
Denial management processes become significantly more effective when integrated into rapid RCM solutions. Rather than addressing denials weeks after occurrence, rapid systems flag and resolve issues within days.
Technology Enablement in Rapid Revenue Cycle Management
Modern rapid RCM solutions leverage technology platforms that previous generations of billing operations never accessed. AI-powered solutions can transform revenue cycle management by analyzing patterns in claims data, predicting denials before they occur, and recommending corrective actions.
However, technology alone doesn't create rapid RCM solutions. The human expertise to interpret data, make strategic decisions, and handle complex cases remains essential. The most effective approaches combine automated efficiency with skilled professional judgment.
Integration Capabilities That Matter
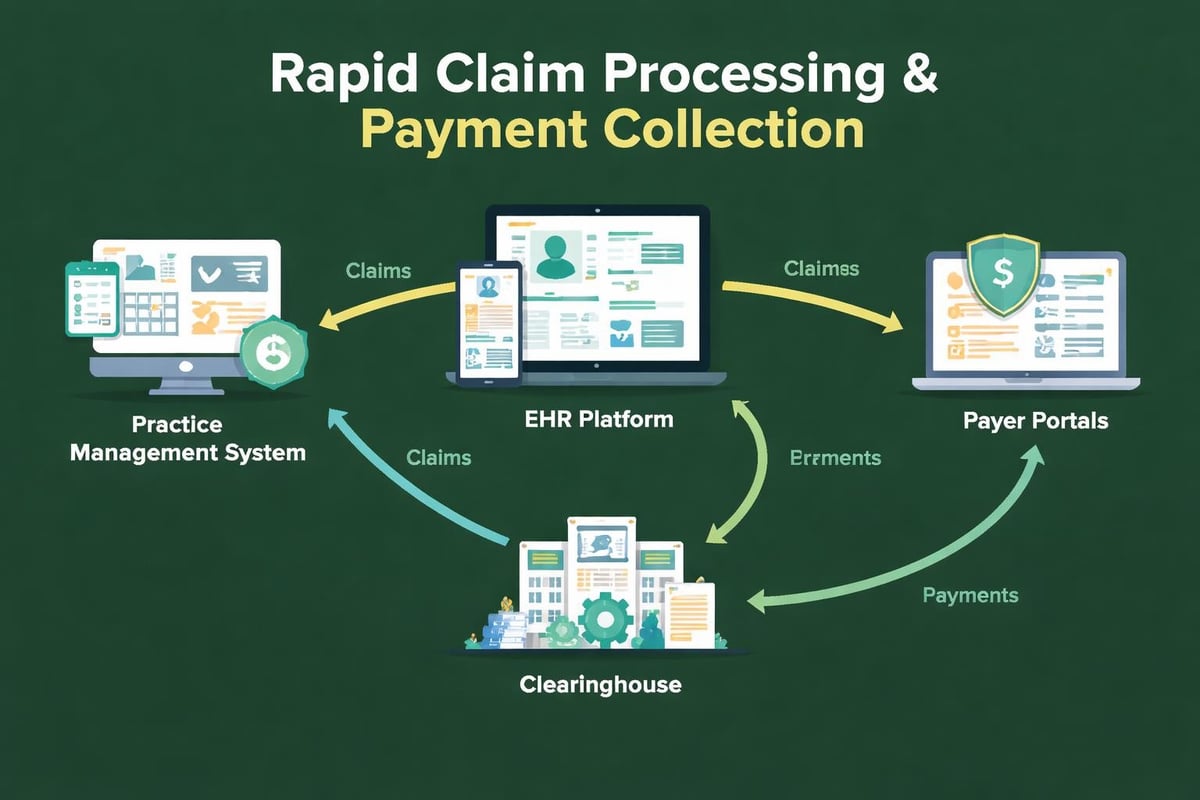
Rapid RCM solutions require seamless integration across multiple systems:
- Electronic Health Records (EHR) that capture complete documentation supporting claims
- Practice Management Systems that schedule appointments and track patient encounters
- Clearinghouse Connections that facilitate rapid claim transmission and status updates
- Payer Portals that enable real-time eligibility checks and claim status verification
- Payment Processing Platforms that accept and reconcile patient payments efficiently
Organizations exploring specialized RCM solutions for various healthcare providers discover that customization based on specialty-specific requirements significantly impacts results. Cardiology practices face different coding challenges than dermatology clinics, and rapid RCM solutions must adapt accordingly.
Building Operational Excellence Through Process Optimization
Achieving rapid results requires more than implementing new technology or hiring additional staff. The underlying processes must support speed while maintaining compliance and accuracy. Process optimization begins with mapping current workflows to identify delay points, redundancies, and error sources.
Charge entry represents a critical process area where rapid RCM solutions make substantial impact. Many practices experience 3-5 day delays between service delivery and charge entry, directly extending the entire revenue cycle. Efficient charge entry in medical billing requires standardized procedures, clear documentation requirements, and immediate feedback loops when information gaps exist.
Workflow Design for Maximum Velocity
Effective rapid RCM solutions organize work based on logical processing sequences rather than departmental boundaries. Claims move continuously through verification, coding, submission, and follow-up stages without waiting in queues between departments.
Daily work prioritization ensures that high-value claims receive immediate attention. A $15,000 surgical claim shouldn't wait behind routine office visits simply because it arrived later in the queue. Strategic prioritization accelerates cash flow by focusing resources where they generate greatest return.
Quality checkpoints positioned at critical junctures catch errors before they cause delays:
- Pre-submission claim scrubbing identifies coding inconsistencies
- Eligibility verification confirms coverage before appointment dates
- Charge audits ensure documentation supports billed services
- Payment posting reviews detect underpayments requiring appeals
Organizations implementing these checkpoints within rapid RCM solutions reduce overall processing time by preventing costly rework cycles.
Staff Training and Knowledge Management for Sustained Performance
Even the most sophisticated rapid RCM solutions depend on knowledgeable staff executing processes correctly. Continuous training ensures team members stay current with changing payer requirements, coding updates, and regulatory modifications.
Specialty-specific knowledge becomes particularly important for practices in fields with complex billing requirements. Understanding the nuances of revenue coding for different service types prevents submission errors that delay payments.
Creating a Culture of Continuous Improvement
Rapid RCM solutions thrive in environments where staff members actively seek improvement opportunities. Regular performance reviews examining individual and team metrics identify training needs and process enhancement opportunities.
Knowledge sharing systems capture expertise from experienced team members and make it accessible to newer staff. When a biller discovers an effective approach for handling a specific payer's requirements, that knowledge should benefit the entire team immediately.
| Training Focus Area | Frequency | Impact on Rapid RCM |
|---|---|---|
| Payer Policy Updates | Monthly | Reduces denials 15-25% |
| Coding Changes | Quarterly | Improves accuracy 10-18% |
| Technology Features | As Released | Accelerates processing 8-12% |
| Compliance Requirements | Quarterly | Prevents costly violations |
Understanding clean claims in medical billing requires ongoing education as payer requirements evolve. What constituted a clean claim last year may require additional documentation today.
Managing Denials Within Rapid RCM Frameworks
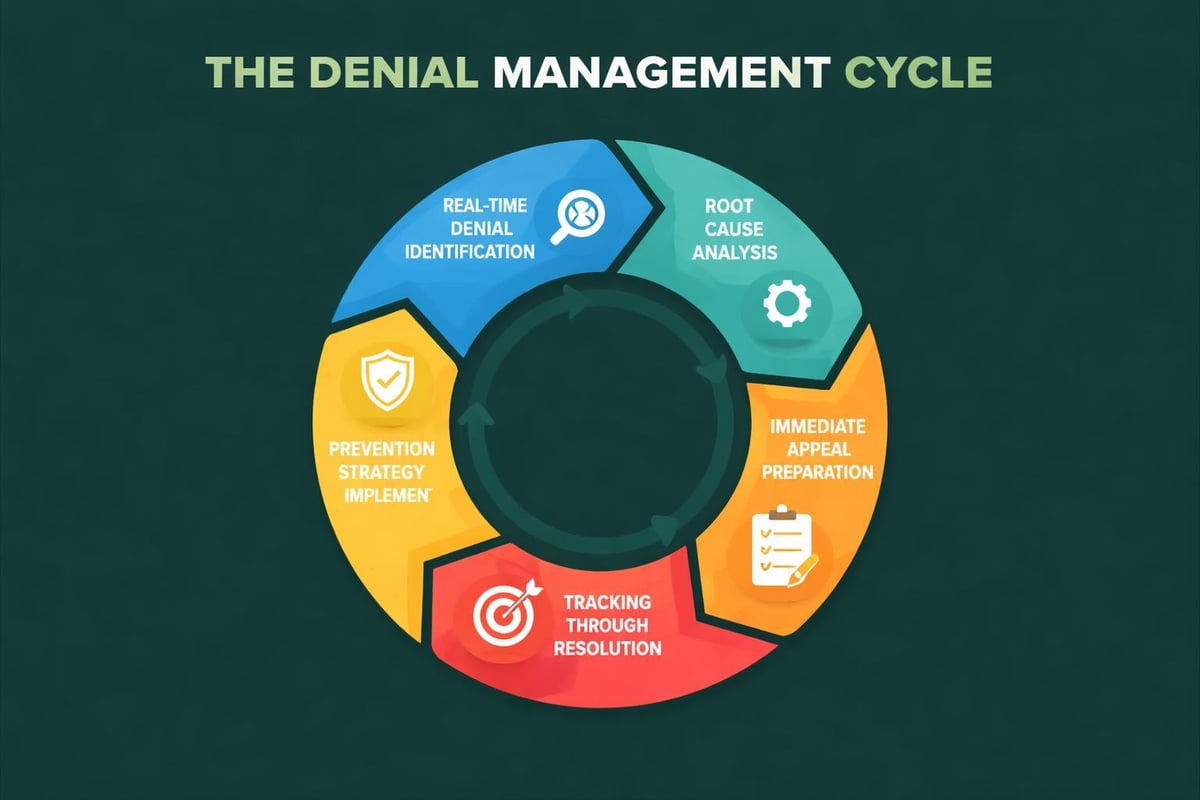
Denial management represents both a challenge and an opportunity within rapid RCM solutions. While prevention remains the primary goal, effective rapid response to denials that do occur separates high-performing operations from average ones.
The time between denial notification and appeal submission directly impacts success rates. Appeals filed within 48-72 hours of denial notification achieve approval rates 20-30% higher than appeals filed after two weeks. This reality makes rapid denial management a critical revenue protection strategy.
Denial Prevention Through Predictive Analytics
Advanced rapid RCM solutions incorporate predictive analytics that identify claims likely to face denials before submission. By analyzing historical denial patterns, these systems flag claims sharing characteristics with previously denied submissions.
Common denial triggers include:
- Missing or incorrect authorization numbers
- Services provided outside covered dates
- Non-covered diagnosis and procedure combinations
- Incorrect patient demographic information
- Billing errors such as duplicate claim submissions
When rapid RCM solutions identify potential issues before submission, staff can address problems proactively rather than reactively. This shift from defense to offense dramatically improves financial outcomes.
How denial management in medical billing improves cash flow becomes evident when practices track dollars recovered through effective appeals processes. Top-performing organizations recover 60-70% of initially denied claim amounts through systematic appeal procedures.
Selecting and Implementing Rapid RCM Solutions for Your Practice
Healthcare providers evaluating rapid RCM solutions face numerous options ranging from internal process improvements to outsourced service partnerships. The optimal choice depends on practice size, specialty focus, current performance levels, and available resources.
Small practices often benefit most from partnering with specialized service providers offering rapid RCM solutions. These partnerships provide access to expertise, technology, and economies of scale that individual practices cannot develop independently. Comprehensive RCM services tailored to practice needs enable even small organizations to achieve performance comparable to large health systems.
Implementation Roadmap for Success
Successful rapid RCM solution implementation follows a structured approach:
- Current State Assessment documenting existing workflows, metrics, and pain points
- Gap Analysis identifying specific areas where rapid solutions will generate greatest impact
- Solution Design creating customized workflows incorporating best practices and rapid processing principles
- Pilot Testing validating approaches with limited scope before full deployment
- Full Implementation rolling out solutions systematically across all revenue cycle functions
- Performance Monitoring tracking metrics to ensure sustained improvement and identify optimization opportunities
The implementation timeline varies based on practice complexity and solution scope. Smaller practices with straightforward billing may complete implementation within 60-90 days, while larger multi-specialty organizations often require 120-180 days for comprehensive deployment.
Revenue Cycle Analytics Driving Continuous Acceleration
Data visibility forms the foundation of effective rapid RCM solutions. Without clear metrics revealing performance across all revenue cycle stages, identifying improvement opportunities becomes guesswork rather than strategic analysis.
Comprehensive analytics dashboards track key performance indicators in real-time, enabling rapid response to emerging issues. When clean claim rates drop or days in accounts receivable increase, immediate investigation prevents small problems from becoming major disruptions.
Critical Metrics for Rapid RCM Monitoring
Performance tracking should encompass both efficiency and effectiveness measures:
Efficiency Metrics:
- Time from service delivery to claim submission
- Claim processing velocity through submission pipeline
- Payment posting turnaround time
- Denial response time from notification to appeal
Effectiveness Metrics:
- Clean claim submission rates by payer and service type
- First-pass resolution rates for submitted claims
- Appeal success rates and recovered revenue
- Net collection rates adjusted for contractual allowances
Organizations implementing healthcare revenue cycle analytics gain insights enabling proactive management rather than reactive firefighting. Trending data reveals patterns that predict future challenges, allowing preventive action before problems impact cash flow.
Compliance and Security Within Rapid Processing Environments
Accelerating revenue cycle operations never justifies compromising compliance or patient data security. Rapid RCM solutions must incorporate robust safeguards ensuring HIPAA compliance, accurate coding practices, and ethical billing standards.
Speed sometimes creates pressure to skip verification steps or shortcut established protocols. Effective rapid RCM solutions design workflows that achieve velocity through efficiency rather than corner-cutting. Automated verification processes run faster than manual reviews while maintaining accuracy and compliance.
Regular compliance audits ensure rapid RCM solutions maintain regulatory adherence as processes evolve. Understanding medical billing costs includes recognizing that compliance violations carry severe financial penalties far exceeding any short-term gains from questionable practices.
Security Protocols for Protected Health Information
Rapid processing requires multiple team members accessing patient information across various systems. Access controls, encryption standards, and audit trails protect sensitive data throughout the revenue cycle.
Security measures essential for rapid RCM solutions include:
- Role-based access limiting data visibility to job requirements
- Multi-factor authentication preventing unauthorized system access
- Encrypted data transmission across all platforms and connections
- Comprehensive audit logging tracking all PHI access and modifications
- Regular security training reinforcing proper data handling procedures
Healthcare providers exploring physician RCM solutions should verify that potential partners demonstrate documented security practices and compliance certifications.
Future Trends Shaping Rapid RCM Solutions
The healthcare revenue cycle management landscape continues evolving as technology advances and payer requirements change. Artificial intelligence and machine learning increasingly influence rapid RCM solutions, automating tasks that previously required human judgment.
Predictive analytics capabilities expand beyond simple denial prediction to comprehensive revenue forecasting. Advanced systems analyze scheduled procedures, historical payment patterns, and payer behavior to project cash flow with remarkable accuracy. This visibility enables better financial planning and resource allocation.
Automation extends into patient communication, with intelligent systems sending personalized payment reminders, offering convenient payment options, and answering common billing questions without staff intervention. These capabilities reduce administrative burden while improving patient satisfaction and collection rates.
AI-driven RCM software designed to automate and assist represents the next generation of rapid solutions, though human expertise remains essential for complex cases, strategic decisions, and patient relationship management.
Interoperability improvements enable seamless data exchange between disparate systems, reducing manual data entry and associated errors. As health information exchanges mature, rapid RCM solutions increasingly access comprehensive patient records supporting accurate coding and complete claim submission.
The regulatory environment continues shifting, with value-based care models creating new billing complexities. Rapid RCM solutions must adapt to these changes while maintaining processing speed and accuracy. Organizations partnering with experienced service providers gain advantage through expertise navigating evolving requirements.
Optimizing Patient Financial Experience Through Rapid Solutions
Rapid RCM solutions benefit patients as well as providers. Faster claim processing produces quicker insurance adjudication, reducing patient uncertainty about financial responsibility. Clear, timely communication about balances due improves patient satisfaction and collection rates.
Transparent pricing information provided before service delivery, enabled by rapid eligibility verification and benefit checks, allows patients to make informed decisions. This transparency builds trust and reduces disputes over unexpected bills.
Payment plan options integrated into rapid RCM solutions make healthcare expenses manageable for patients facing high deductibles. Rather than demanding full payment immediately, flexible arrangements maintain positive patient relationships while ensuring eventual collection.
Self-service portals allowing patients to view statements, make payments, and communicate about billing questions reduce administrative phone volume while providing convenience patients appreciate. These platforms integrate with rapid RCM solutions to ensure information accuracy and real-time account updates.
Understanding what adjustments on medical bills mean and communicating this clearly to patients prevents confusion and payment delays. Rapid RCM solutions should include patient-friendly statement designs and proactive communication about insurance processing.
Healthcare providers seeking sustainable financial performance must embrace rapid RCM solutions that accelerate cash flow while maintaining accuracy and compliance. The combination of optimized workflows, advanced technology, specialized expertise, and continuous improvement creates transformational results. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to enhance efficiency, reduce denials, and maximize reimbursements for healthcare practices across the United States. Our experienced team works within your existing systems to implement rapid processing strategies tailored to your specialty and practice needs, ensuring you achieve optimal financial performance while focusing on patient care.