Physician practices face mounting financial pressures from declining reimbursement rates, complex payer requirements, and increasing administrative burdens. Effective physician revenue cycle management serves as the financial backbone that keeps medical practices sustainable and profitable. This comprehensive process encompasses every step from patient registration through final payment collection, requiring precision, compliance expertise, and continuous optimization. Understanding and implementing robust revenue cycle strategies separates thriving practices from those struggling with cash flow challenges and mounting accounts receivable.
Understanding the Core Components of Physician Revenue Cycle Management
Physician revenue cycle management represents the financial process that healthcare facilities use to track patient care episodes from registration and appointment scheduling through final balance settlement. This systematic approach integrates clinical and administrative functions to optimize revenue capture while maintaining compliance with regulatory requirements.
The revenue cycle begins before patients even arrive at the practice. Pre-registration activities establish the foundation for successful reimbursement by collecting accurate demographic information and verifying insurance eligibility. Practices that invest in thorough eligibility verification services reduce claim denials and accelerate payment timelines.
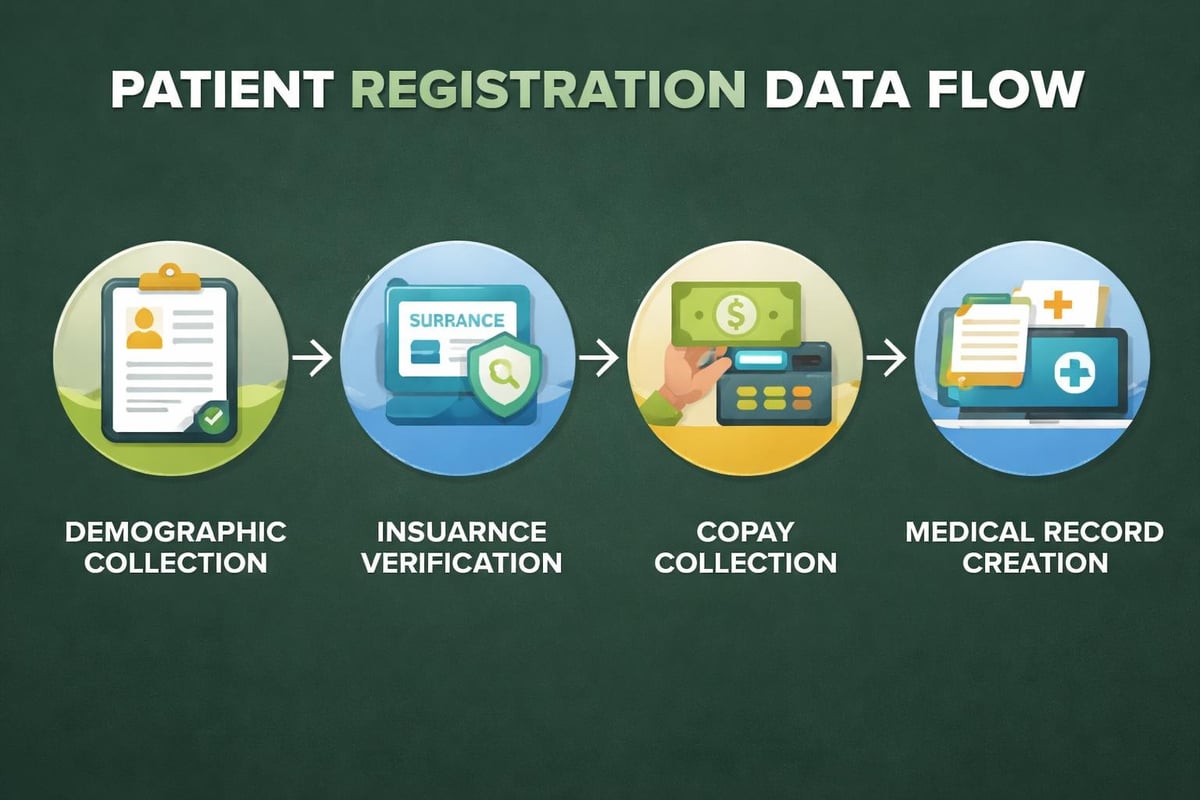
The Patient Registration Phase
Patient registration accuracy directly impacts downstream revenue cycle performance. Registration staff must collect complete and accurate information including:
- Full legal name matching insurance cards
- Current address and contact information
- Primary and secondary insurance details
- Referring physician information when applicable
- Patient responsibility estimates
Front-desk errors represent one of the most common sources of claim denials. A single transposed digit in an insurance identification number can delay payment by weeks or result in complete claim rejection. Training registration personnel on data quality standards and implementing verification protocols significantly reduces these preventable errors.
Clinical Documentation and Charge Capture Excellence
Clinical documentation serves dual purposes in physician revenue cycle management: supporting quality patient care and justifying medical necessity for reimbursement. Physicians must document services with sufficient detail to demonstrate the level of care provided while adhering to payer-specific documentation requirements.
Charge Capture Fundamentals
Charge capture represents the process of recording all billable services provided during patient encounters. The Craneware Group identifies inaccurate charge capture as one of the two biggest challenges facing healthcare providers. Missed charges translate directly to lost revenue that practices can never recover.
Effective charge capture systems include:
- Real-time service documentation at point of care
- Automated charge posting from electronic health records
- Regular charge master reviews and updates
- Provider education on documentation requirements
- Audit processes to identify missed charges
Specialty-specific considerations further complicate charge capture. Cardiology practices, for example, require different billing expertise than primary care clinics. Understanding these nuances ensures accurate coding and optimal reimbursement for specialized services.
Medical Coding Accuracy
Medical coding translates clinical documentation into standardized codes used for billing. Professional coders assign Current Procedural Terminology (CPT) codes for procedures and services, International Classification of Diseases (ICD) codes for diagnoses, and applicable modifiers to clarify service details.
Coding errors generate claim denials, payment delays, and compliance risks. Practices must balance coding conservatively to avoid fraud allegations while coding comprehensively to capture legitimate reimbursement. Partnering with experienced medical coding services helps practices navigate this complexity.
| Coding Error Type | Financial Impact | Prevention Strategy |
|---|---|---|
| Undercoding | Lost revenue, reduced reimbursement | Regular documentation training |
| Overcoding | Compliance risk, potential fraud allegations | Internal audit programs |
| Unbundling | Claim denials, payer scrutiny | Automated coding software checks |
| Missing modifiers | Reduced payment, claim rejections | Coder education on modifier usage |
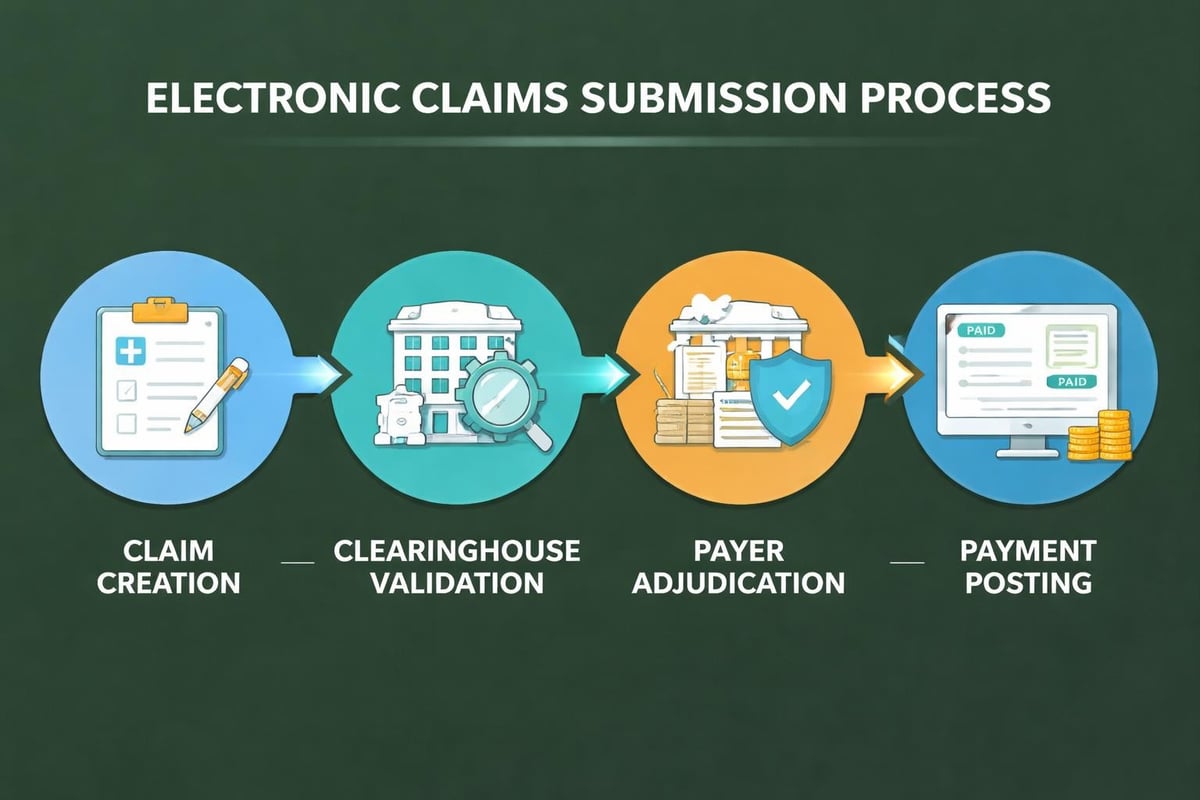
Claims Submission and Management Strategies
Claims submission represents the formal request for payment from insurance companies or government payers. This critical phase of physician revenue cycle management requires meticulous attention to payer-specific requirements, submission deadlines, and technical formatting standards.
Clean Claims Rate Optimization
The clean claims rate measures the percentage of claims accepted by payers on first submission without requiring corrections or additional information. Industry benchmarks suggest practices should achieve clean claims rates above 95%. Experian Health emphasizes automation in claims submission to reduce errors and expedite payments.
Electronic claims submission offers numerous advantages over paper claims including faster processing, immediate acknowledgment of receipt, and reduced manual handling errors. Most payers now require or strongly encourage electronic submission through clearinghouses that validate claims before forwarding to payers.
Establishing robust medical claim submission services workflows ensures consistent, timely filing that maximizes cash flow.
Payer Follow-Up Protocols
Claims don't always process smoothly even when submitted correctly. Systematic follow-up protocols identify and resolve delayed or denied claims before they age beyond filing limits. Best practices include:
- Tracking claims from submission through payment
- Following up on unpaid claims within 14 days
- Documenting all payer communications
- Escalating unresolved claims appropriately
- Monitoring payer-specific payment patterns
Denial patterns often reveal systematic issues requiring process improvements. Analyzing denial reasons helps practices address root causes rather than merely resubmitting rejected claims.
Payment Posting and Reconciliation
Payment posting involves recording payments and adjustments to patient accounts when insurance companies remit payment. This seemingly straightforward task requires careful attention to ensure accurate accounting and identify underpayments or processing errors.
Electronic Remittance Advice Processing
Electronic Remittance Advice (ERA) files contain detailed payment information from payers. Understanding what ERA in medical billing means helps practices automate payment posting while maintaining accuracy. Automated posting reduces staff time while improving data accuracy compared to manual entry from paper explanations of benefits.
Contractual adjustments represent the difference between billed charges and contracted rates. Proper posting ensures these adjustments reflect actual contract terms rather than masking underpayments. Regular contract compliance auditing protects practices from systematic underpayment.
Professional payment posting services ensure accurate account reconciliation while freeing internal staff for higher-value activities.
Denial Management and Appeals
Denial management represents one of the most critical yet often neglected aspects of physician revenue cycle management. The American Medical Association outlines eight keys to improve revenue cycle management, emphasizing the importance of addressing denials systematically.
Common Denial Categories
Understanding denial reasons enables targeted prevention strategies. Denials typically fall into several categories:
- Registration errors: Incorrect patient information or insurance details
- Authorization issues: Missing or expired prior authorizations
- Timely filing: Claims submitted after payer deadlines
- Medical necessity: Insufficient documentation supporting service need
- Coding errors: Incorrect or unsupported procedure codes
Each denial category requires different prevention and resolution approaches. Registration denials demand front-office training and verification improvements, while medical necessity denials may indicate documentation education needs for clinical staff.
Building an Effective Appeals Process
Successful appeals require organized documentation, clear communication, and persistence. Effective appeal processes include:
- Immediate review: Assess denial validity within 48 hours
- Documentation gathering: Compile supporting medical records and policies
- Appeal letter preparation: State clear rationale with supporting evidence
- Tracking and follow-up: Monitor appeal status and escalate when necessary
- Trend analysis: Identify patterns requiring systemic changes
First-level appeals often succeed when practices provide additional documentation or clarification. Practices should maintain detailed appeal templates addressing common denial reasons to streamline the process. Specialized denial management services can significantly improve appeal success rates while reducing internal workload.
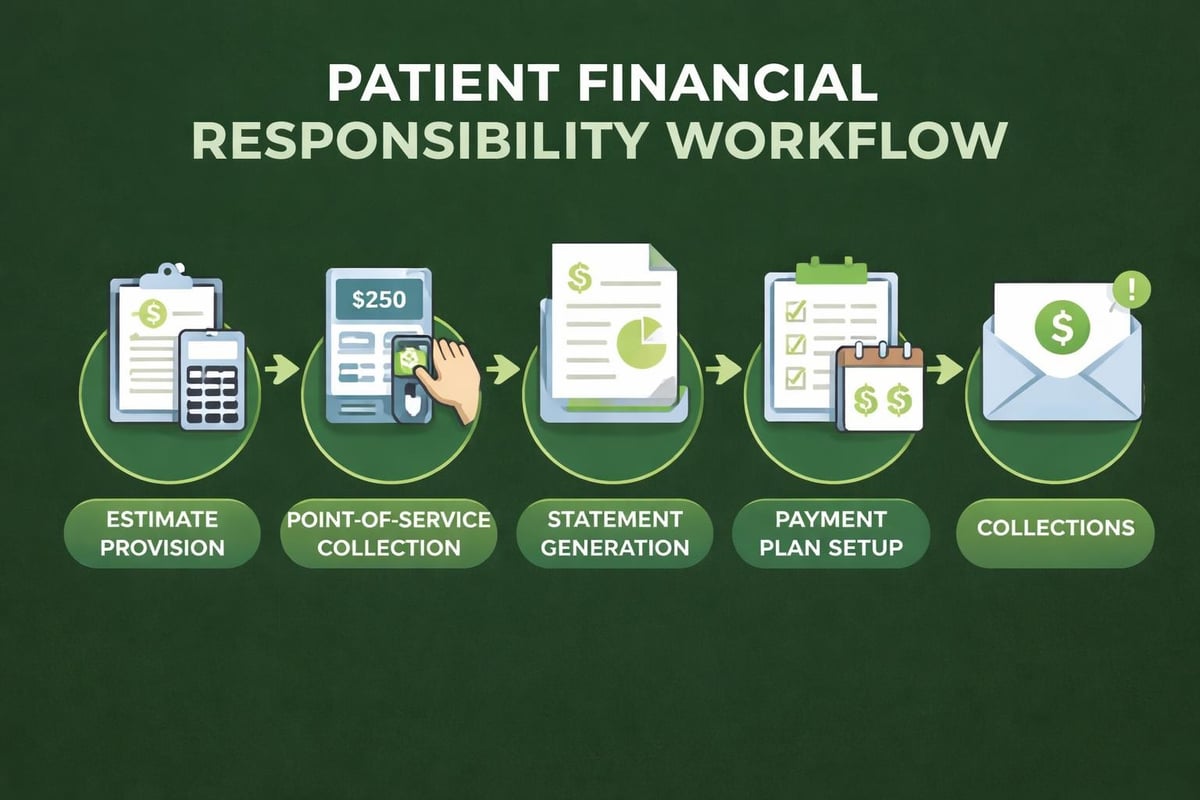
Patient Collections and Financial Counseling
Patient responsibility has increased dramatically with higher deductibles and copayments becoming standard in insurance plans. Effective patient collections represent an increasingly important component of physician revenue cycle management as patients now account for a larger portion of practice revenue.
Point-of-Service Collections
Collecting patient payments at the time of service dramatically improves collection rates compared to billing patients after the visit. Many practices now require copayment collection before seeing the patient, balancing customer service considerations with financial sustainability.
Transparent cost estimates help patients prepare financially for their visits. Providing accurate estimates of patient responsibility based on insurance benefits and deductible status demonstrates respect for patients while improving payment collection. This approach requires integrated systems that access real-time eligibility and benefit information.
Payment Plans and Financial Assistance
Not all patients can pay their full balance immediately. Offering structured payment plans makes healthcare accessible while ensuring the practice eventually receives payment. Key considerations include:
- Minimum payment thresholds
- Interest and financing charges (where legally permissible)
- Automated payment processing
- Default protocols
Financial counseling services help patients understand their bills and explore payment options including charity care programs when appropriate. This patient-centered approach improves satisfaction while optimizing collections.
Technology Integration and Automation
Modern physician revenue cycle management relies heavily on technology to improve efficiency, reduce errors, and accelerate cash flow. Coker Group emphasizes technology utilization as essential for improving revenue cycle performance in physician enterprises.
Practice Management System Optimization
Practice management systems serve as the central hub for revenue cycle operations, managing scheduling, registration, billing, and collections. Maximizing system utilization requires:
- Regular staff training on system features
- Workflow customization matching practice patterns
- Integration with clinical systems to reduce duplicate entry
- Report utilization for performance monitoring
Many practices underutilize their existing systems, manually performing tasks the software could automate. Conducting periodic system assessments identifies opportunities to improve efficiency through better technology leverage.
Reporting and Analytics
Data-driven decision making separates high-performing practices from those operating reactively. Key performance indicators for physician revenue cycle management include:
| Metric | Benchmark Target | Importance |
|---|---|---|
| Days in A/R | Under 35 days | Measures collection speed |
| Clean claims rate | Above 95% | Indicates submission quality |
| Denial rate | Below 5% | Shows process effectiveness |
| Collection rate | Above 95% | Reflects overall efficiency |
| Cost to collect | Below 3% | Measures operational efficiency |
Customized dashboards provide real-time visibility into revenue cycle performance, enabling proactive management rather than reactive problem-solving. Advanced reporting analytics capabilities transform raw data into actionable insights.
Regulatory Compliance and Risk Management
Physician revenue cycle management operates within a complex regulatory environment including HIPAA privacy requirements, Anti-Kickback Statute provisions, Stark Law restrictions, and False Claims Act implications. Compliance failures expose practices to significant financial and legal risks.
Documentation and Coding Compliance
Medical necessity documentation must support the level of service billed. Benchmark Solutions provides tips to maximize revenue cycle management, including staying informed about coding changes and maintaining documentation standards.
Internal audit programs identify compliance risks before they attract payer or government scrutiny. Regular chart reviews assess whether documentation supports billed codes and whether coding patterns align with specialty benchmarks. Outlier analysis flags providers whose coding patterns differ significantly from peers, potentially indicating undercoding, overcoding, or documentation issues.
HIPAA Compliance in Revenue Cycle Operations
Revenue cycle staff access protected health information daily, creating potential privacy and security risks. Comprehensive HIPAA compliance programs include:
- Access controls limiting system permissions to job requirements
- Regular privacy and security training
- Business associate agreements with vendors
- Breach notification protocols
- Encryption of electronic communications containing patient information
Partnering with vendors who prioritize HIPAA compliance, like top medical billing companies, provides an additional layer of security and expertise.
Outsourcing Versus In-House Management
Practices face strategic decisions about whether to manage revenue cycle operations internally or partner with specialized service providers. Each approach offers distinct advantages depending on practice size, specialty, and available resources.
Benefits of Professional Revenue Cycle Services
Specialized revenue cycle management providers bring focused expertise, dedicated resources, and proven processes that many practices cannot replicate internally. Advantages include:
- Specialized knowledge: Experts who stay current on payer policies and coding changes
- Scalability: Resources that flex with practice volume fluctuations
- Technology access: Enterprise-grade systems without capital investment
- Performance focus: Dedicated attention to revenue optimization
Small and medium practices particularly benefit from outsourcing, gaining enterprise-level capabilities without maintaining large administrative teams. Even larger practices often outsource specific functions like prior authorization services or denial management while keeping other operations internal.
Evaluating Service Providers
Selecting the right revenue cycle management partner requires careful evaluation. Important considerations include:
- Industry experience: Track record in your specialty
- Technology platform: Systems integration capabilities
- Transparency: Regular reporting and communication practices
- Compliance focus: HIPAA certification and security measures
- Performance guarantees: Metrics and accountability structures
References from existing clients provide invaluable insights into provider performance, responsiveness, and partnership quality. Practices should request references from clients of similar size and specialty.
Staff Training and Development
Whether managing revenue cycle operations internally or partnering with external providers, practice staff require ongoing education to maintain performance. True North M&A outlines challenges in healthcare revenue cycle management, many of which proper training can address.
Cross-Functional Education
Revenue cycle performance depends on coordination across multiple departments. Front-office staff need basic coding knowledge to capture charges accurately. Providers need to understand how documentation affects reimbursement. Billing staff benefit from clinical knowledge helping them identify documentation gaps requiring clarification.
Regular training sessions keep staff current on payer policy changes, coding updates, and compliance requirements. Monthly team meetings reviewing denial trends and process improvements foster continuous learning and engagement.
Performance Monitoring and Feedback
Individual accountability drives overall revenue cycle performance. Establishing clear performance expectations with regular feedback helps staff understand their contribution to practice financial health. Metrics might include:
- Registration error rates
- Charge entry timeliness
- Coding accuracy rates
- Collection effectiveness
- Patient satisfaction scores
Recognition programs celebrating achievements motivate teams and reinforce desired behaviors. Sharing success stories when the team resolves a complex denial or implements a process improvement builds culture around revenue cycle excellence.
Adapting to Value-Based Care Models
Healthcare payment models continue evolving from fee-for-service toward value-based arrangements rewarding quality and outcomes over volume. These changes require physician revenue cycle management adaptations to capture value-based payments while maintaining fee-for-service revenue.
Quality Metrics Tracking
Value-based contracts typically tie payment to quality metrics achievement. Practices must track and report various measures including:
- Clinical quality indicators specific to specialty
- Patient experience scores
- Care coordination activities
- Preventive service delivery rates
Data integration between clinical and billing systems enables automated quality reporting, reducing administrative burden while ensuring accurate payment capture for value-based contract performance.
Risk Adjustment Documentation
Risk adjustment models use patient diagnosis codes to predict expected healthcare costs, influencing payment rates in many value-based contracts. Comprehensive diagnosis documentation becomes critical for appropriate risk score calculation and payment.
Physicians must document all chronic conditions affecting patient care during each relevant encounter. This requires different thinking than traditional fee-for-service documentation focusing primarily on the visit's presenting problem.
Successful physician revenue cycle management requires coordinating numerous complex processes while maintaining compliance, optimizing efficiency, and delivering excellent patient experiences. Practices that master these fundamentals achieve better financial performance, reduced administrative stress, and improved sustainability in an increasingly challenging healthcare environment. Greenhive Billing Solutions provides comprehensive revenue cycle management services helping healthcare providers maximize reimbursements while streamlining operations, allowing physicians to focus on patient care rather than administrative complexities.

