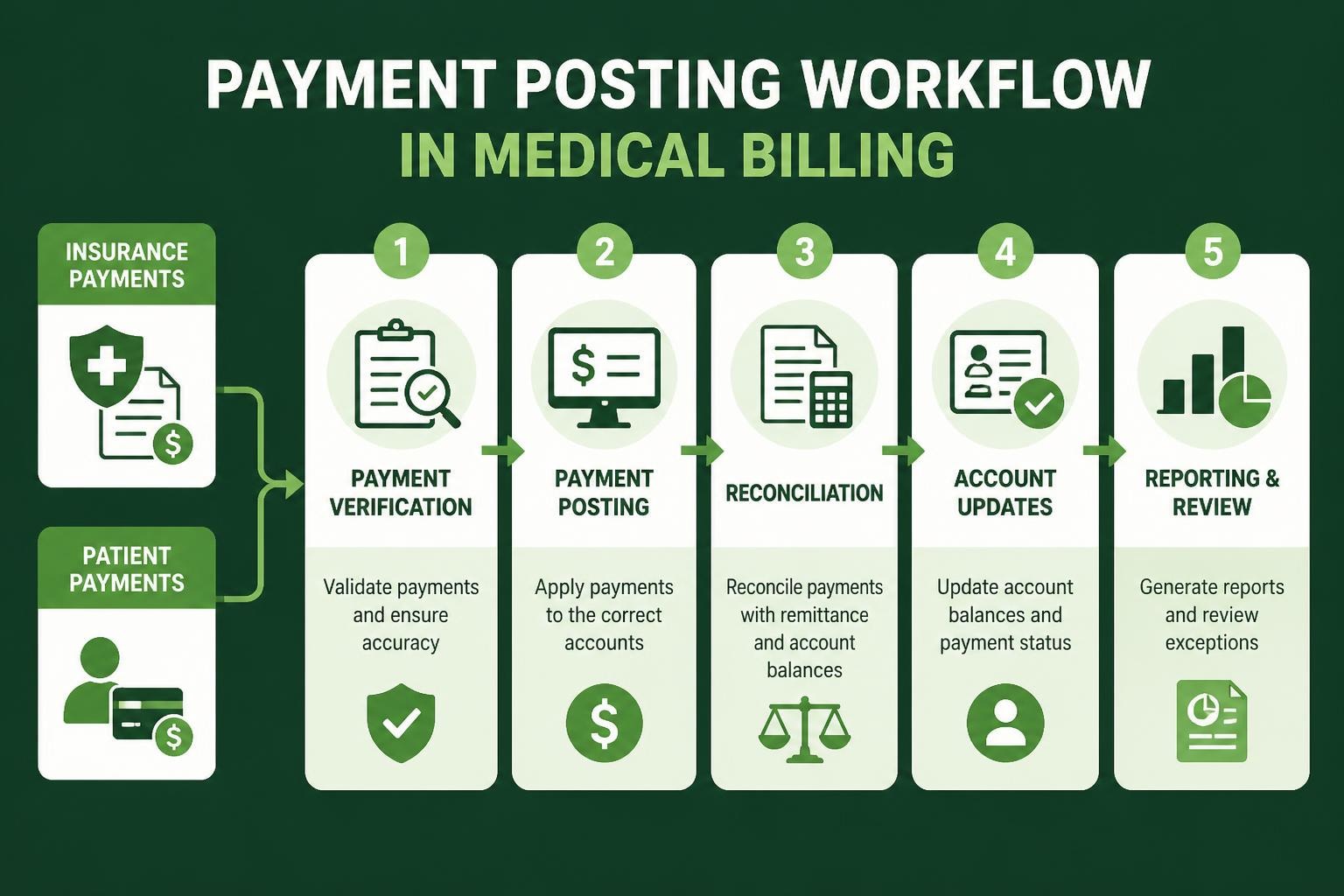
Healthcare providers face mounting pressure to maintain financial stability while delivering exceptional patient care. Within the complex ecosystem of revenue cycle management, payment posting in medical billing represents a critical checkpoint that directly impacts cash flow, financial reporting accuracy, and overall practice profitability. Every payment received-whether from insurance companies, patients, or third-party payers-must be accurately recorded, reconciled, and applied to the correct patient accounts. When this process falters, even briefly, the consequences ripple throughout the entire financial infrastructure of a healthcare organization.
Understanding the Foundation of Payment Posting
Payment posting in medical billing serves as the bridge between services rendered and revenue realized. This fundamental process involves recording all payments received by a healthcare practice and applying them to the appropriate patient accounts. The complexity extends beyond simple data entry, encompassing verification of payment amounts, identification of contractual adjustments, and recognition of denial patterns that require corrective action.
Healthcare practices receive payments through multiple channels. Insurance companies transmit electronic remittance advice (ERA) files containing payment details for multiple claims simultaneously. Patients submit copayments, deductibles, and coinsurance amounts through various methods including cash, checks, credit cards, and online portals. Third-party administrators process payments for self-insured employer plans with their own adjustment methodologies.
Each payment source requires specific handling protocols. Understanding ERA in medical billing becomes essential for practices seeking to automate portions of the posting process while maintaining accuracy. The transformation from manual paper-based posting to electronic workflows has revolutionized efficiency, yet human oversight remains indispensable for identifying discrepancies and unusual patterns.
Key Components of Effective Payment Recording
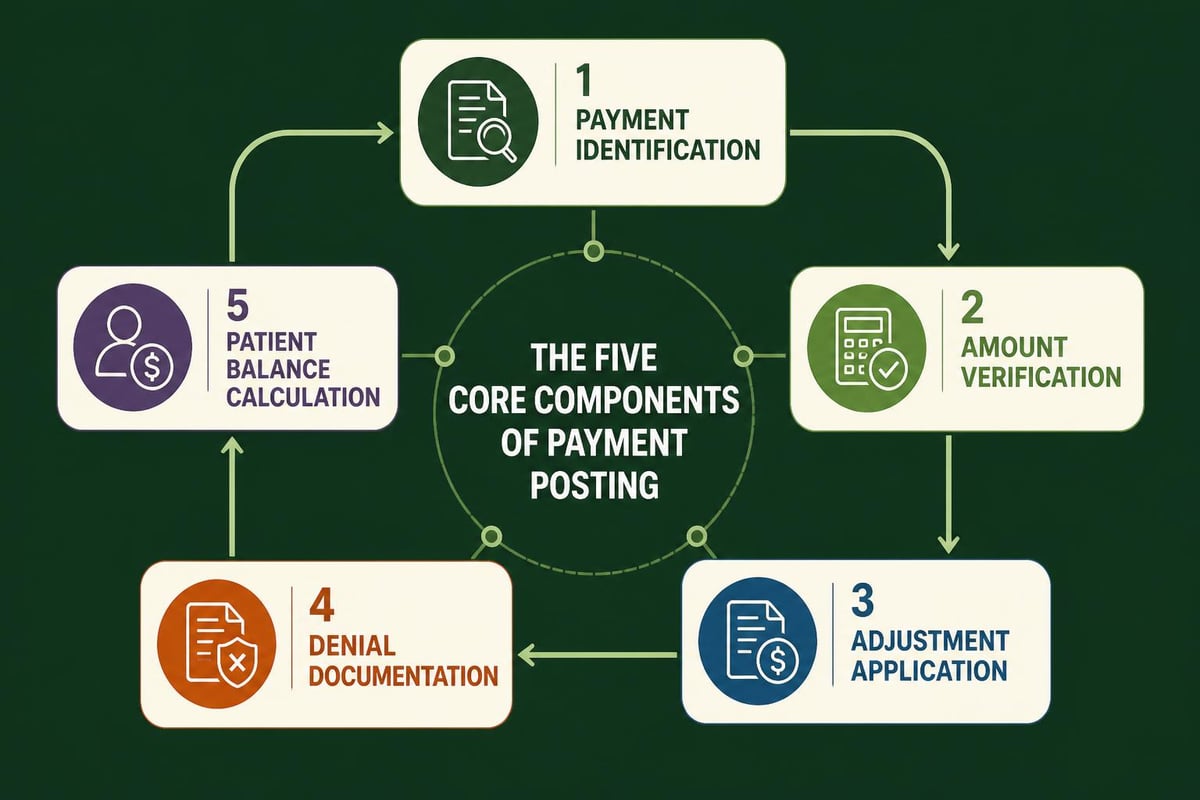
The payment posting workflow encompasses several distinct yet interconnected activities:
- Payment identification – Matching incoming payments to specific claims and patient encounters
- Amount verification – Confirming posted amounts align with contracted rates and expected reimbursement
- Adjustment application – Recording contractual adjustments, write-offs, and other balance modifications
- Denial documentation – Flagging rejected claims for appeal or corrective action
- Patient balance calculation – Determining remaining patient responsibility after insurance processing
According to CareCloud’s analysis of payment posting importance, accurate posting provides healthcare administrators with real-time financial visibility essential for operational decision-making.
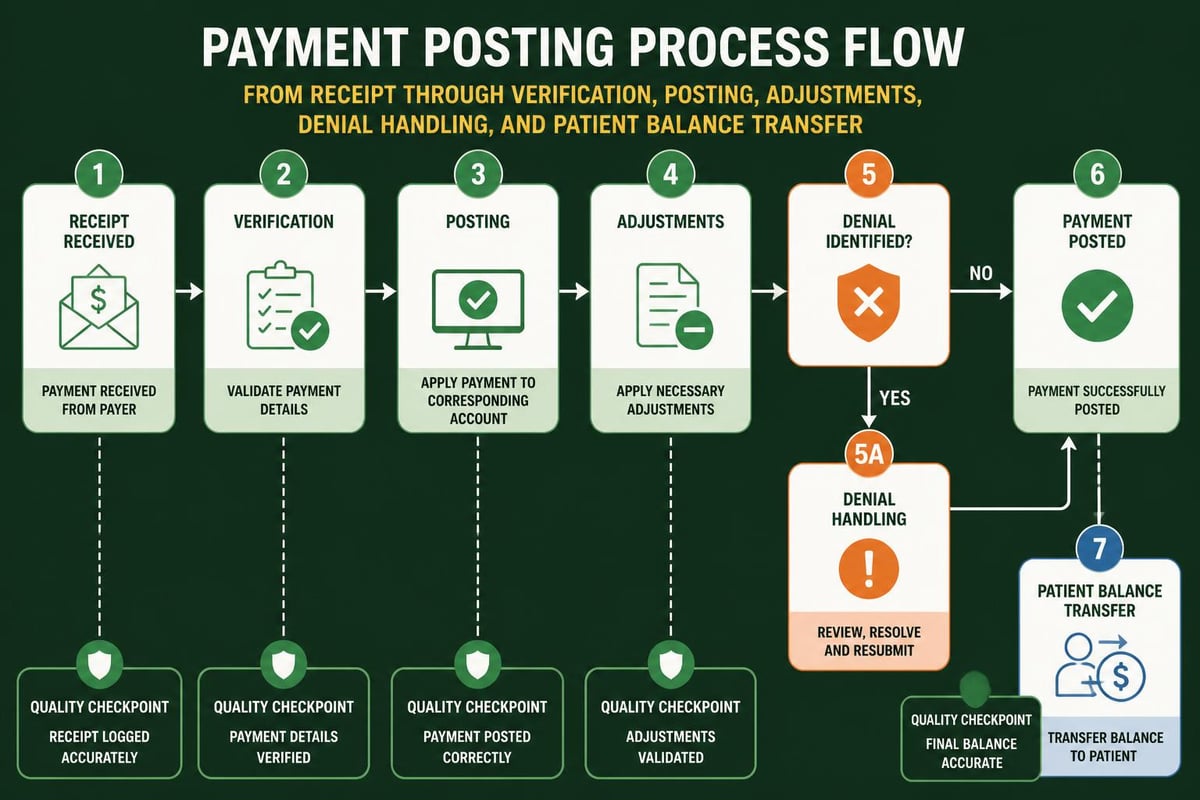
The Step-by-Step Payment Posting Process
Mastering payment posting in medical billing requires systematic execution across multiple stages. Healthcare organizations benefit from standardized workflows that reduce variability and minimize errors.
Step 1: Payment Receipt and Organization
The process begins when payments arrive at the practice through various channels. Staff must organize incoming payments by source and payment type. Electronic payments arrive with accompanying ERA files that contain detailed remittance information. Paper checks require manual matching with explanation of benefits (EOB) documents that detail payment calculations.
Practices should establish dedicated time blocks for payment processing to ensure consistent attention to this critical function. Daily posting prevents backlogs that can obscure the true financial position of the organization.
Step 2: Payment Verification Against Expected Amounts
Before posting any payment, billing staff must verify that received amounts align with contractual expectations. This verification process protects against underpayment and identifies calculation errors from payers.
| Verification Element | What to Check | Common Discrepancy |
|---|---|---|
| Contracted Rate | Matches fee schedule | Outdated rate applied |
| Patient Responsibility | Aligns with benefit structure | Incorrect deductible calculation |
| Adjustment Codes | Properly justified | Inappropriate write-offs |
| Procedure Codes | Match claim submission | Downcoding by payer |
Understanding contractual adjustments helps staff differentiate between acceptable write-offs and payment errors requiring appeal.
Step 3: Posting to Patient Accounts
Once verified, payments are posted to the practice management system. This step requires precision in selecting the correct patient, date of service, and claim number. Modern billing systems often auto-post ERA payments, but manual review remains crucial for accuracy.
The posting professional must apply payments to specific procedure codes within each claim. Insurance payments may cover multiple services from the same encounter, requiring careful allocation of funds to ensure each procedure reflects its individual reimbursement status.
Step 4: Adjustment and Write-Off Application
Understanding what adjustments on medical bills represent enables proper categorization of balance reductions. Contractual adjustments reflect the difference between billed charges and contracted rates. Non-covered service adjustments remove balances for procedures not included in the patient's benefit plan. Bad debt write-offs remove uncollectible patient balances after exhaustive collection efforts.
Each adjustment type carries different implications for financial reporting and compliance. Proper categorization ensures accurate revenue recognition and supports audit requirements.
Step 5: Denial and Rejection Handling
When payers deny or reject claims, payment posting personnel document the denial reason and route the claim for appropriate action. Denial codes provide insight into the issue, whether administrative (incorrect patient information), clinical (lack of medical necessity), or authorization-related (missing prior approval).
Effective denial management in medical billing starts with accurate documentation during payment posting. Tracking denial patterns reveals systemic issues that require process improvements or staff training.
Step 6: Patient Balance Transfer
After insurance processing completes, remaining balances transfer to patient responsibility. Accurate calculation of patient obligations requires consideration of deductibles, coinsurance percentages, copayments, and non-covered services.
The transition from insurance responsibility to patient responsibility must be clearly documented. Patients deserve transparent communication about their financial obligations, supported by accurate account records that explain how their balance was calculated.
Common Challenges in Payment Posting
Healthcare organizations encounter recurring obstacles that compromise posting accuracy and efficiency. Recognition of these challenges enables proactive mitigation strategies.
High-Volume Processing Demands
Busy practices process hundreds or thousands of payments weekly. The volume creates pressure to prioritize speed over accuracy, leading to errors that compound over time. Split payments across multiple claims, partial payments requiring follow-up, and bulk ERA files containing dozens of patients all increase complexity.
Solutions include:
- Implementing auto-posting for straightforward ERA payments
- Scheduling dedicated posting sessions to minimize interruptions
- Cross-training staff to manage volume fluctuations
- Utilizing batch processing capabilities in practice management systems
Payer-Specific Variations
Each insurance company applies unique adjustment codes, payment methodologies, and reporting formats. Staff must maintain working knowledge of multiple payer requirements simultaneously. According to DrChrono’s explanation of payment posting, these variations represent a significant training challenge for billing departments.
Creating payer-specific reference guides helps staff navigate differences efficiently. Regular review of remittance advice documents from each major payer identifies changes in payment policies before they create systematic errors.
Coordination of Benefits Complexity
Patients with multiple insurance policies require coordination of benefits (COB) processing. Primary insurance pays first according to their contract, then secondary insurance considers remaining balances. Payment posting in medical billing becomes significantly more complex when tracking multiple payers for the same service.
Staff must understand COB rules, post payments in the correct sequence, and calculate patient responsibility only after all insurance payments post. Errors in COB posting create patient billing disputes and delayed revenue recognition.
Underpayment Identification
Subtle underpayments easily escape detection amid high transaction volumes. When an insurance company pays $85 for a service contracted at $100, busy staff may overlook the $15 shortfall if they don't verify against fee schedules. Benchmark Solutions emphasizes accurate payment posting as a safeguard against revenue leakage from chronic underpayment.
| Detection Strategy | Implementation Method | Benefit |
|---|---|---|
| Automated variance reports | System alerts for payments below threshold | Flags significant discrepancies |
| Monthly fee schedule audits | Compare posted rates to contracts | Identifies systemic issues |
| Random posting quality checks | Supervisor review of sample transactions | Maintains staff accuracy |
| Payer performance tracking | Monitor average payment percentage by carrier | Reveals problematic payers |
Best Practices for Optimizing Payment Posting
Healthcare organizations that excel at payment posting in medical billing implement structured best practices that enhance accuracy, efficiency, and financial transparency.
Establish Daily Posting Protocols
Same-day or next-day posting prevents backlogs and maintains current financial records. Delayed posting obscures the practice's true financial position and creates aging account receivable problems. Daily posting discipline also accelerates patient billing, reducing collection cycles.
Implement Multi-Level Quality Controls
Quality assurance mechanisms catch errors before they impact financial reporting. Supervisory review of random posting samples, automated system edits that flag unusual transactions, and monthly reconciliation of total payments to bank deposits all contribute to data integrity.
New staff should work under heightened supervision until they demonstrate consistent accuracy. Experienced staff benefit from periodic refresher training on payer policy updates and system enhancements.
Leverage Technology Appropriately
Modern practice management systems offer sophisticated auto-posting capabilities for ERA files. When properly configured, these systems apply payments accurately while flagging exceptions for manual review. However, technology serves as a tool, not a replacement for knowledgeable staff.
The comprehensive revenue cycle management process integrates payment posting technology with other billing functions to create seamless workflows. Staff should focus their expertise on exception handling, complex cases, and continuous process improvement.
Maintain Comprehensive Documentation
Every adjustment, write-off, and balance transfer requires supporting documentation. This documentation serves multiple purposes including audit support, dispute resolution, and pattern analysis. Notes should explain the rationale for unusual transactions and reference specific policies or contracts when applying adjustments.
Documentation standards ensure consistency across staff members and facilitate training of new personnel. Clear audit trails demonstrate compliance with regulations and payer contracts.
Monitor Key Performance Indicators
Data-driven management of payment posting identifies improvement opportunities and measures progress. Relevant metrics include:
- Days in accounts receivable – Measures collection efficiency
- Payment posting lag time – Tracks processing speed
- Error rate per posting session – Quantifies accuracy
- Denial rate by payer – Identifies problematic relationships
- Contractual adjustment percentage – Monitors payer compliance
Regular review of these indicators with posting staff creates accountability and highlights training needs. Reporting and analytics capabilities transform raw posting data into actionable intelligence.

The Financial Impact of Accurate Payment Posting
Payment posting accuracy directly influences multiple aspects of practice financial health. The consequences of posting errors extend far beyond simple bookkeeping mistakes.
Cash Flow Management
Accurate, timely posting provides the foundation for reliable cash flow projections. Practice administrators depend on current accounts receivable aging reports to forecast incoming revenue and plan expenditures. When posting lags or contains errors, financial planning occurs in the dark.
Delayed payment posting artificially inflates accounts receivable, creating the illusion of pending revenue that has actually already arrived. This distortion can lead to poor financial decisions based on inaccurate data.
Compliance and Audit Readiness
Healthcare practices face regular audits from payers, government programs, and regulatory bodies. Accurate payment posting documentation demonstrates proper handling of patient funds and compliance with billing regulations. According to the American Medical Association’s guidance on coding mistakes, documentation errors create compliance vulnerabilities.
Practices must prove that patient balances accurately reflect insurance payments and contractual obligations. Auditors scrutinize adjustment applications, write-off justifications, and patient billing calculations. Clean posting records expedite audits and minimize compliance risk.
Revenue Optimization
Systematic identification of underpayments through diligent posting review recovers revenue that would otherwise be lost. Even small underpayments across hundreds of claims accumulate into significant annual amounts. Staff trained to recognize payment discrepancies protect practice profitability.
Payment posting services from specialized providers often include underpayment detection protocols that recover revenue overlooked by busy in-house staff.
Patient Satisfaction
Accurate patient balances prevent billing disputes that damage patient relationships. When insurance processing and payment posting occur correctly, patient statements clearly explain financial responsibility. Errors create frustration, time-consuming phone calls, and potential loss of patient trust.
Transparent, accurate billing supported by proper payment posting in medical billing contributes to positive patient experiences. Patients appreciate clear explanations of insurance processing and legitimate bills based on verified information.
Training and Skill Development for Posting Staff
Competent payment posting requires specialized knowledge spanning insurance regulations, payer contracts, accounting principles, and software proficiency. Healthcare organizations must invest in comprehensive training programs that develop these multifaceted skills.
Foundational Knowledge Requirements
New payment posting staff need grounding in fundamental concepts:
- Insurance Terminology – Understanding EOBs, ERAs, deductibles, coinsurance, copayments, and out-of-pocket maximums
- Contract Interpretation – Reading and applying provider-payer agreements to verify payment accuracy
- Adjustment Code Meanings – Recognizing standard reason codes and their financial implications
- System Navigation – Proficiently using the practice management software for posting and reporting
- Regulatory Compliance – Following HIPAA privacy requirements and other healthcare regulations
CapMinds’ comprehensive guide to payment posting emphasizes the breadth of knowledge required for excellence in this role.
Ongoing Education Initiatives
The healthcare payment landscape continuously evolves with payer policy changes, coding updates, and regulatory modifications. Staff require regular training to maintain current knowledge. Monthly team meetings should address recent payer correspondence, new adjustment codes, and system updates.
Cross-training creates operational flexibility and prevents knowledge concentration risks. When only one person understands complex posting scenarios, the practice becomes vulnerable to that individual's absence or departure.
Error Analysis as Learning Tool
Reviewing posting errors constructively builds staff competency. When supervisors identify mistakes, discussing the root cause and correct approach transforms errors into learning opportunities. Tracking common error types reveals training gaps requiring attention.
Creating a culture that views mistakes as improvement opportunities rather than punishable failures encourages staff to seek clarification when uncertain rather than guessing.
Integration with Broader Revenue Cycle Functions
Payment posting in medical billing does not exist in isolation. It connects intimately with upstream and downstream revenue cycle processes, creating dependencies that impact overall financial performance.
Relationship to Claims Management
Claims submission quality directly affects payment posting efficiency. Clean claims with accurate coding generate straightforward payments that post easily. Claims containing errors trigger denials that complicate posting and require corrective action. Medical claim submission services that emphasize first-pass accuracy reduce downstream posting complications.
Communication between claims staff and posting personnel creates feedback loops that improve submission quality. When posting staff notice recurring denial patterns, they should alert claims managers to address root causes.
Connection to Patient Collections
After insurance payments post and patient balances calculate, the collection process begins. Accurate posting ensures patients receive correct statements reflecting legitimate obligations. Collection staff depend on posting accuracy to confidently pursue patient balances.
When patients dispute charges, investigation often traces back to payment posting. Staff must access posting documentation to verify that insurance payments applied correctly and patient calculations followed proper methodology.
Impact on Financial Reporting
Monthly financial statements derive from posted transaction data. Revenue recognition, accounts receivable valuation, and bad debt expense all reflect the cumulative result of daily posting activities. Chief financial officers trust that posted data accurately represents the practice's financial position.
Accounting staff reconcile posted payments to bank deposits, ensuring that all received funds were properly recorded. Discrepancies indicate posting errors or potentially more serious issues like payment theft.
Outsourcing Considerations for Payment Posting
Many healthcare practices evaluate whether to maintain in-house payment posting or engage specialized service providers. This decision involves multiple factors specific to each organization's circumstances.
Benefits of Specialized Service Providers
Dedicated payment posting teams offer several advantages. They maintain current knowledge of payer policies across multiple carriers. They achieve economies of scale through high-volume processing. They provide consistent coverage without concerns about staff vacations or turnover.
Service providers typically guarantee performance standards for accuracy and turnaround time, creating accountability absent in many in-house operations. Top medical billing companies leverage specialized expertise and technology investments that individual practices cannot justify.
In-House Operation Advantages
Some practices prefer maintaining direct control over payment posting. In-house staff develop intimate knowledge of practice-specific situations and physician preferences. They integrate more naturally with front-office functions and patient interactions.
Smaller practices with manageable posting volumes may find in-house operations more cost-effective than outsourcing. The decision should consider total costs including staff salaries, benefits, training, software, and supervision against outsourcing fees.
Hybrid Approaches
Many organizations adopt hybrid models that balance internal control with external expertise. Practices might handle routine posting in-house while outsourcing complex cases, overflow volumes, or specialized functions like denial management.
Understanding the full scope of services available from RCM providers helps practices design optimal hybrid arrangements that leverage both internal and external capabilities.
Technology Evolution in Payment Posting
Technological advancement continues reshaping how healthcare organizations approach payment posting in medical billing. Modern solutions offer capabilities that dramatically improve efficiency and accuracy compared to manual processes.
Artificial intelligence and machine learning algorithms now analyze payment patterns, predict posting errors, and recommend corrections before transactions finalize. Automated systems learn from historical data to recognize payer-specific quirks and flag unusual payments for manual review.
Integration between clearinghouses, payers, and practice management systems creates seamless data flows that eliminate manual data entry for many transactions. Real-time eligibility verification before service delivery improves payment predictability and reduces posting surprises.
Mobile applications enable posting staff to work remotely while maintaining secure access to patient financial data. Cloud-based systems provide accessibility, automatic updates, and disaster recovery capabilities superior to legacy on-premise software.
Despite technological sophistication, human judgment remains essential. Technology handles routine transactions efficiently while experienced staff focus on exceptions, complex cases, and continuous process refinement. The most successful organizations blend technological capabilities with human expertise.
Accurate payment posting in medical billing forms the cornerstone of healthy practice finances, connecting every payment received to the proper patient account while maintaining compliance and transparency. Healthcare providers that prioritize posting excellence through standardized workflows, quality controls, and ongoing staff development position themselves for financial stability and growth. Greenhive Billing Solutions provides comprehensive revenue cycle management services including expert payment posting that ensures accurate financial records, maximizes reimbursements, and frees healthcare providers to focus on patient care. Our experienced team handles the complexities of payment processing with precision and transparency, supporting your practice's financial health every step of the way.