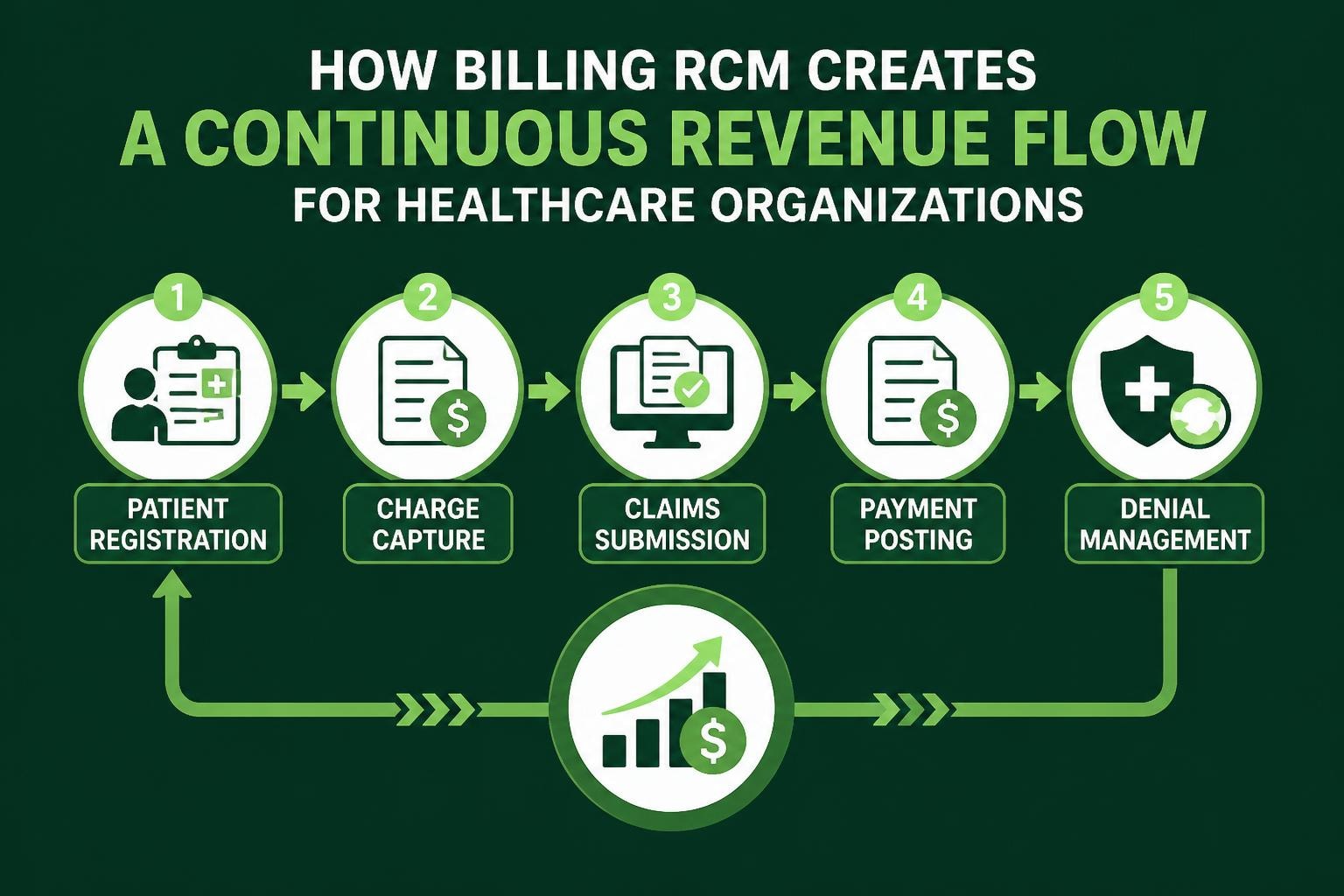
Healthcare providers face increasing pressure to maintain financial stability while delivering quality patient care. Billing RCM represents the comprehensive process that transforms clinical services into revenue, encompassing everything from patient registration through final payment collection. Understanding how billing RCM functions and implementing best practices can significantly impact a practice's bottom line, reduce administrative burden, and ensure compliance with evolving healthcare regulations.
Understanding the Core Components of Billing RCM
Billing RCM operates as an integrated system rather than isolated tasks. The revenue cycle begins the moment a patient schedules an appointment and continues until all payments are collected and reconciled.
Patient registration and eligibility verification form the foundation of effective billing RCM. Accurate demographic information and insurance verification prevent downstream errors that lead to claim denials. Many practices lose substantial revenue simply because eligibility wasn't confirmed before services were rendered.
The charge capture phase ensures every billable service is documented and coded correctly. Missing charges represent lost revenue that can never be recovered. According to research on effective physician revenue cycle management, systematic charge capture processes can identify revenue leakage points and improve financial outcomes.
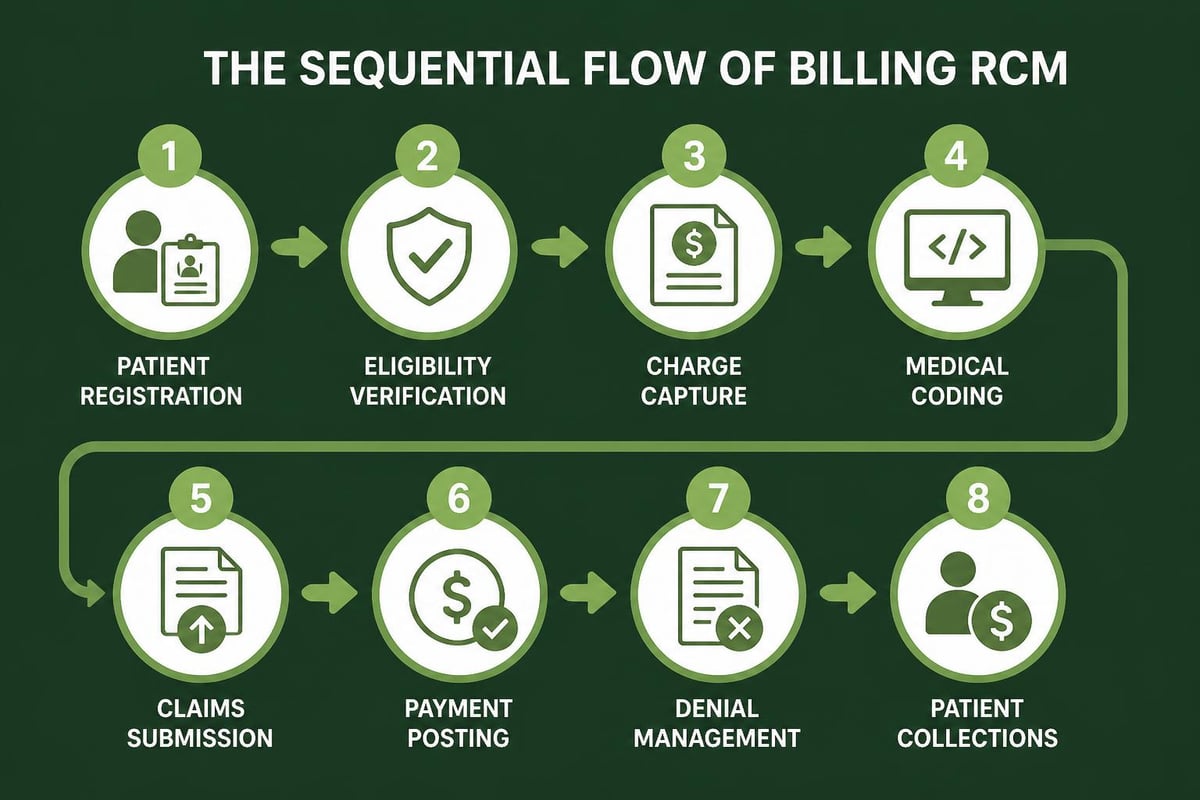
The Critical Role of Medical Coding
Medical coding translates clinical documentation into standardized codes that payers recognize and reimburse. Coders must select appropriate diagnosis codes, procedure codes, and modifiers that accurately reflect services provided.
Coding errors create significant financial consequences:
- Undercoding leaves money on the table by not capturing the full complexity of services
- Overcoding triggers audits, recoupment demands, and potential compliance violations
- Incorrect code pairing results in automatic claim rejections
- Missing modifiers causes payment delays or inappropriate denials
Staying current with different types of medical coding requirements ensures claims are submitted correctly the first time. Clean claims accelerate payment cycles and reduce administrative overhead associated with rework.
Claims Submission and Management in Billing RCM
Submitting claims represents a pivotal moment in billing RCM. Electronic claims submission has become the standard, offering faster processing and immediate acknowledgment of receipt from payers.
| Claim Type | Average Processing Time | Rejection Rate |
|---|---|---|
| Electronic Clean Claims | 14-21 days | 5-10% |
| Paper Claims | 30-45 days | 15-25% |
| Claims with Errors | 45-90+ days | 60-80% |
The Healthcare Financial Management Association emphasizes that clean claim submission rates directly correlate with revenue cycle performance. Practices achieving 95% or higher clean claim rates experience faster reimbursement and lower administrative costs.
Scrubbing Claims Before Submission
Pre-submission claim scrubbing identifies errors before claims reach payers. Automated scrubbing software checks for:
- Missing or invalid patient information
- Incorrect insurance details
- Coding errors and incompatible code combinations
- Missing authorizations or referrals
- Compliance with payer-specific requirements
Claims that pass scrubbing protocols have dramatically higher first-pass acceptance rates, reducing the time between service delivery and payment receipt.
Payment Posting and Reconciliation
Once payers process claims, they issue payments along with remittance advice explaining adjustments and denials. Payment posting involves recording these transactions accurately in the practice management system.
Electronic Remittance Advice (ERA) streamlines this process by delivering payment information in standardized electronic format. Understanding what ERA in medical billing means for operational efficiency helps practices reduce manual data entry and improve posting accuracy.
Payment variance analysis identifies patterns that indicate potential issues:
- Consistent underpayments from specific payers may signal contract problems
- Frequent denials for particular services suggest coding or documentation gaps
- High patient responsibility amounts might require better upfront collection processes
- Contractual adjustments exceeding expected amounts warrant contract review
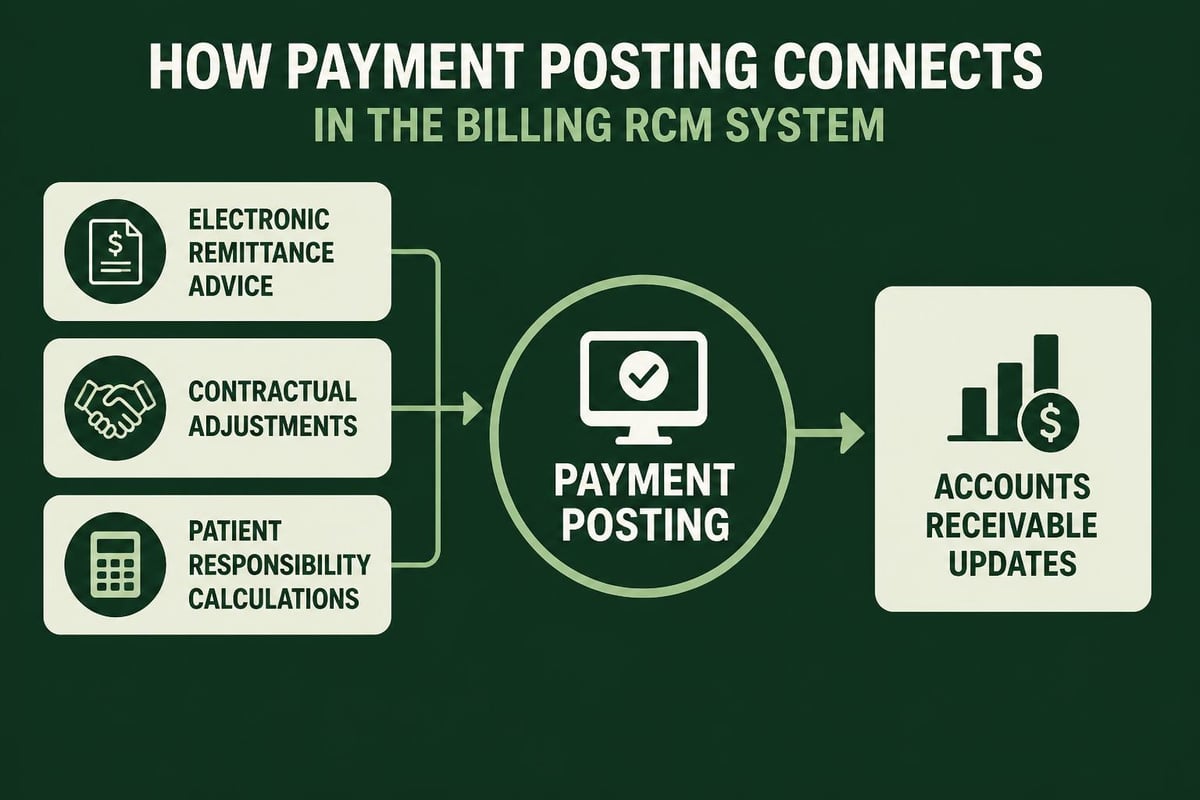
Managing Contractual Adjustments
Contractual adjustments represent the difference between billed charges and contracted rates. These adjustments are expected write-offs based on negotiated fee schedules with insurance companies.
However, excessive contractual adjustments may indicate:
- Outdated fee schedules that don't reflect current contracted rates
- Errors in contract loading within the billing system
- Underpayments being incorrectly classified as contractual
- Need for contract renegotiation with underperforming payers
Regular analysis of contractual adjustment in medical billing ensures practices maintain financial health and identify opportunities for revenue improvement.
Denial Management Within Billing RCM
Denials interrupt cash flow and create additional administrative work. Effective billing RCM includes robust denial management processes that address both prevention and resolution.
Prevention strategies focus on eliminating common denial causes:
- Verifying insurance eligibility before every appointment
- Obtaining necessary authorizations in advance
- Ensuring accurate coding and documentation
- Meeting timely filing deadlines
- Following payer-specific billing requirements
When denials occur, swift action maximizes recovery potential. The denial management in medical billing process requires systematic tracking, root cause analysis, and prompt appeals.
Building an Effective Appeals Process
Successful appeals require understanding why claims were denied and providing compelling documentation that addresses payer concerns.
Step-by-step appeal workflow:
- Categorize denials by reason code to identify patterns
- Research payer policies to understand specific requirements
- Gather supporting documentation including medical records, authorization forms, and coding references
- Write clear appeal letters that cite specific policy language
- Track appeal status and follow up within designated timeframes
- Document outcomes to inform future prevention strategies
Research on how denial management improves cash flow demonstrates that practices with dedicated denial management programs recover 60-70% of denied claims compared to less than 30% for practices without formal processes.
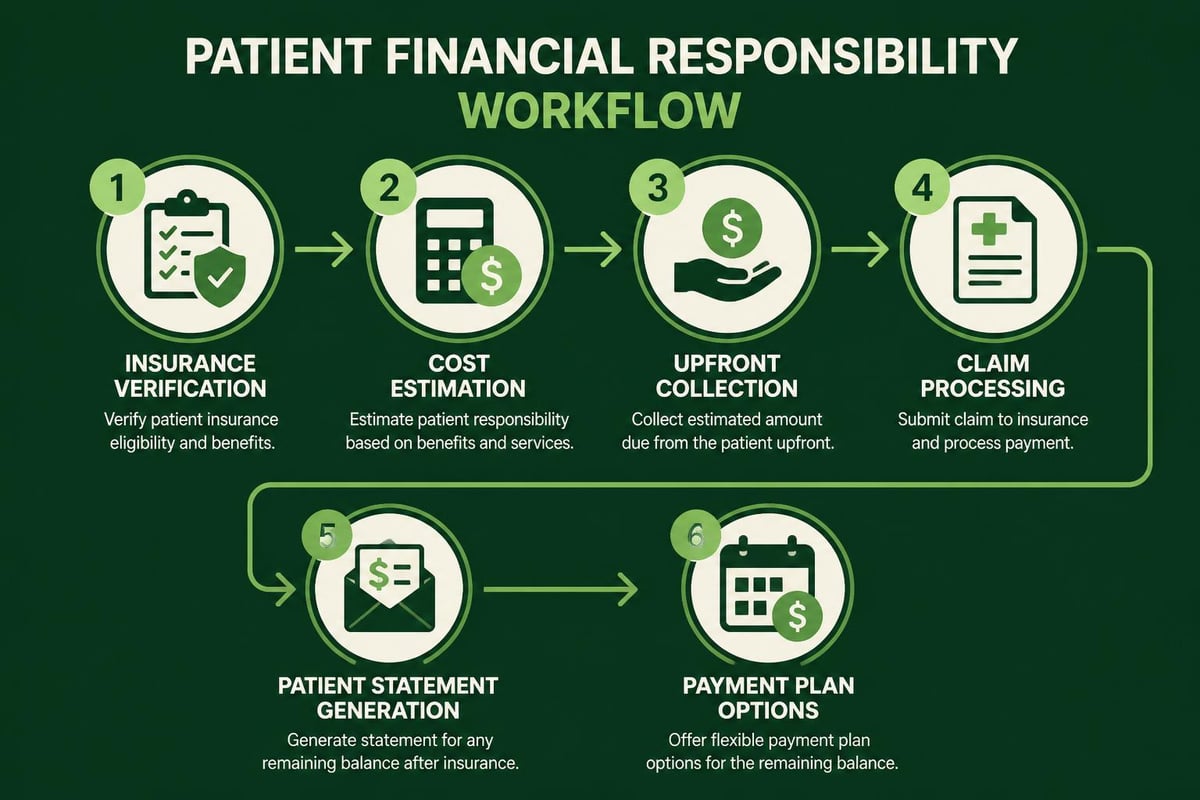
Patient Collections and Billing RCM
Patient responsibility has increased substantially due to high-deductible health plans and greater cost-sharing requirements. Collecting from patients requires different strategies than working with insurance companies.
Upfront collections prove more effective than pursuing balances after service delivery. When patients understand their financial obligations before receiving care, collection rates improve significantly.
| Collection Timing | Average Collection Rate |
|---|---|
| Point of Service | 70-80% |
| Within 30 Days | 50-60% |
| 30-60 Days | 30-40% |
| 60-90 Days | 20-25% |
| 90+ Days | Less than 10% |
Patient-Friendly Billing Practices
Transparent communication about costs and payment options improves patient satisfaction while maintaining collection rates. Offering payment plans for larger balances provides flexibility while ensuring revenue collection.
Technology solutions enable:
- Online payment portals accessible 24/7
- Automated payment reminders via text or email
- Multiple payment options including credit cards and electronic transfers
- Clear, itemized statements that patients can understand
- Secure patient portals for billing inquiries
The American Medical Association emphasizes that integrating patient collections into overall billing RCM strategy rather than treating it as a separate function yields better financial results.
Technology and Automation in Billing RCM
Modern billing RCM relies heavily on technology to manage complexity, reduce errors, and accelerate processes. Practice management systems, electronic health records, and specialized revenue cycle software work together to create integrated workflows.
Automation capabilities that enhance billing RCM performance include:
- Automated eligibility verification checks
- Real-time claim scrubbing before submission
- Electronic claims submission and status tracking
- Automated payment posting from ERA files
- Denial tracking and workflow assignment
- Reporting dashboards with key performance indicators
However, technology alone doesn't guarantee success. The expertise of billing and coding specialists who understand both clinical documentation and payer requirements remains essential.
Key Performance Indicators for Billing RCM
Measuring performance enables continuous improvement. Critical metrics include:
- Clean claim rate: Percentage of claims accepted without errors
- Days in accounts receivable: Average time from service date to payment
- Collection rate: Percentage of expected reimbursement actually collected
- Denial rate: Percentage of claims initially denied
- Cost to collect: Administrative expenses per dollar collected
Benchmarking these metrics against industry standards identifies improvement opportunities and validates the effectiveness of billing RCM processes.
Compliance and Regulatory Considerations
Billing RCM must operate within complex regulatory frameworks including HIPAA privacy and security requirements, fraud and abuse laws, and payer-specific policies.
Compliance areas requiring constant attention:
- Protected health information security during billing processes
- Proper use of modifiers and code combinations
- Accurate reporting of services actually rendered
- Appropriate unbundling or bundling of services
- Timely filing requirements for each payer
- State-specific billing regulations
Resources like the National Uniform Billing Committee provide authoritative guidance on standardized billing practices that promote compliance across healthcare settings.
Documentation Requirements
Solid documentation supports every billing decision. Medical necessity must be clearly established in the clinical record to justify the services billed. When documentation doesn't support the codes submitted, claims face denial or potential audit findings.
Physician documentation should include:
- Chief complaint and history appropriate to the service level
- Examination findings relevant to the presenting problem
- Medical decision-making that demonstrates complexity
- Treatment plan and patient instructions
- Signature and date confirming provider involvement
Understanding revenue coding requirements ensures that documentation, coding, and billing align to support compliant claims submission.
Outsourcing Versus In-House Billing RCM
Healthcare providers face decisions about whether to manage billing RCM internally or partner with specialized service providers. Each approach offers distinct advantages depending on practice size, specialty, and resources.
In-house billing RCM advantages:
- Direct control over processes and staff
- Immediate access to billing information
- No third-party fees or percentage-based costs
- Integration with clinical workflows
Outsourced billing RCM benefits:
- Access to specialized expertise and technology
- Scalability without hiring additional staff
- Reduced overhead for office space and equipment
- Performance-based accountability
- Staying current with regulatory changes
Many practices discover that comprehensive revenue cycle management services deliver better financial results than internal operations, particularly when considering the total cost of technology, training, and staffing required for effective billing RCM.
| Factor | In-House | Outsourced |
|---|---|---|
| Startup Costs | High | Low |
| Technology Updates | Practice Responsibility | Included in Service |
| Staff Training | Ongoing Expense | Provider Responsibility |
| Scalability | Requires Hiring | Immediate |
| Industry Expertise | Varies | Specialized |
Evaluating Service Providers
When considering outsourced billing RCM, providers should evaluate:
- Years of experience in their specific specialty
- Technology platforms and integration capabilities
- Reporting transparency and frequency
- Communication protocols and responsiveness
- References from similar-sized practices
- Fee structure and contract terms
Quality service providers function as true partners, offering strategic guidance beyond transaction processing.
Specialty-Specific Billing RCM Considerations
Different medical specialties face unique billing RCM challenges. Primary care practices handle high patient volumes with relatively straightforward coding, while surgical specialties navigate complex procedure coding and modifier application.
Behavioral health billing requires understanding of mental health parity laws, session-based billing, and specialized diagnosis coding. Providers offering medical billing for behavioral health services need expertise in these specialty requirements.
Hospital-based billing RCM operates with additional complexity including:
- Facility versus professional fee separation
- DRG-based inpatient reimbursement
- Outpatient prospective payment systems
- Separate billing for technical and professional components
Understanding hospital revenue cycle management specifics ensures accurate billing across all service settings.
Urgent Care Revenue Cycle Management
Urgent care centers face unique billing RCM challenges due to high patient turnover, after-hours operations, and mixed payer populations including high self-pay percentages.
Effective urgent care revenue cycle management requires:
- Rapid eligibility verification processes
- Point-of-service collection capabilities
- Accurate place of service coding
- Workers' compensation and auto accident billing expertise
- Extended business hours for billing support
The fast-paced environment demands streamlined processes that don't compromise accuracy or compliance.
Future Trends Affecting Billing RCM
Healthcare reimbursement continues evolving toward value-based models that tie payment to patient outcomes rather than service volume. This shift requires billing RCM systems capable of tracking quality metrics, managing risk-based contracts, and reporting on value measures.
Emerging billing RCM capabilities include:
- Predictive analytics identifying patients likely to become collection challenges
- Artificial intelligence detecting coding optimization opportunities
- Blockchain technology for secure, transparent claims processing
- Interoperability standards enabling seamless data exchange
- Patient engagement tools integrating billing with overall care experience
Staying ahead of these trends positions practices for success regardless of how payment models evolve. Research on revenue cycle management complexities highlights the need for both strategic and operational approaches to optimize financial performance.
Preparing for Regulatory Changes
Healthcare regulations change frequently, impacting coding requirements, billing practices, and compliance obligations. Effective billing RCM includes monitoring regulatory developments and implementing necessary adjustments promptly.
Recent areas of regulatory focus include:
- Surprise billing protections affecting out-of-network claims
- Price transparency requirements for services and charges
- Prior authorization reform to reduce administrative burden
- Telehealth billing flexibility and permanent policy decisions
- Medicare payment updates and coverage determinations
Practices must balance compliance requirements with operational efficiency, ensuring billing RCM processes adapt to new regulations without disrupting revenue flow.
Optimizing Revenue Cycle Analytics
Data-driven decision making separates high-performing billing RCM operations from average performers. Healthcare revenue cycle analytics transform raw transaction data into actionable insights.
Analytical approaches that drive improvement:
- Payer performance comparison identifying favorable and problematic relationships
- Service line profitability analysis guiding strategic decisions
- Staff productivity metrics optimizing workforce allocation
- Denial trend analysis targeting prevention efforts
- Patient payment behavior modeling improving collection strategies
Advanced analytics enable proactive management rather than reactive problem-solving, allowing practices to identify and address issues before they significantly impact revenue.
Effective billing RCM transforms the complex process of healthcare reimbursement into a streamlined operation that maximizes revenue while maintaining compliance. By focusing on accuracy, efficiency, and continuous improvement across all revenue cycle stages, healthcare providers can achieve financial stability and operational excellence. Whether managing billing RCM internally or partnering with specialized service providers, the key lies in combining technology, expertise, and proven processes that adapt to the evolving healthcare landscape. Greenhive Billing Solutions offers comprehensive revenue cycle management services designed to optimize your practice's financial performance through expert medical billing, claims processing, denial management, and transparent reporting that keeps you informed and in control.