Healthcare providers face mounting pressure to maintain financial stability while delivering exceptional patient care. Revenue cycle solutions healthcare organizations implement today directly impact their ability to survive and thrive in an increasingly complex reimbursement environment. From initial patient registration through final payment collection, every step in the revenue cycle presents opportunities for optimization and potential pitfalls that can drain resources. Understanding how comprehensive revenue cycle management transforms operational efficiency and financial performance has become essential for practices of all sizes.
Understanding Revenue Cycle Solutions for Healthcare Organizations
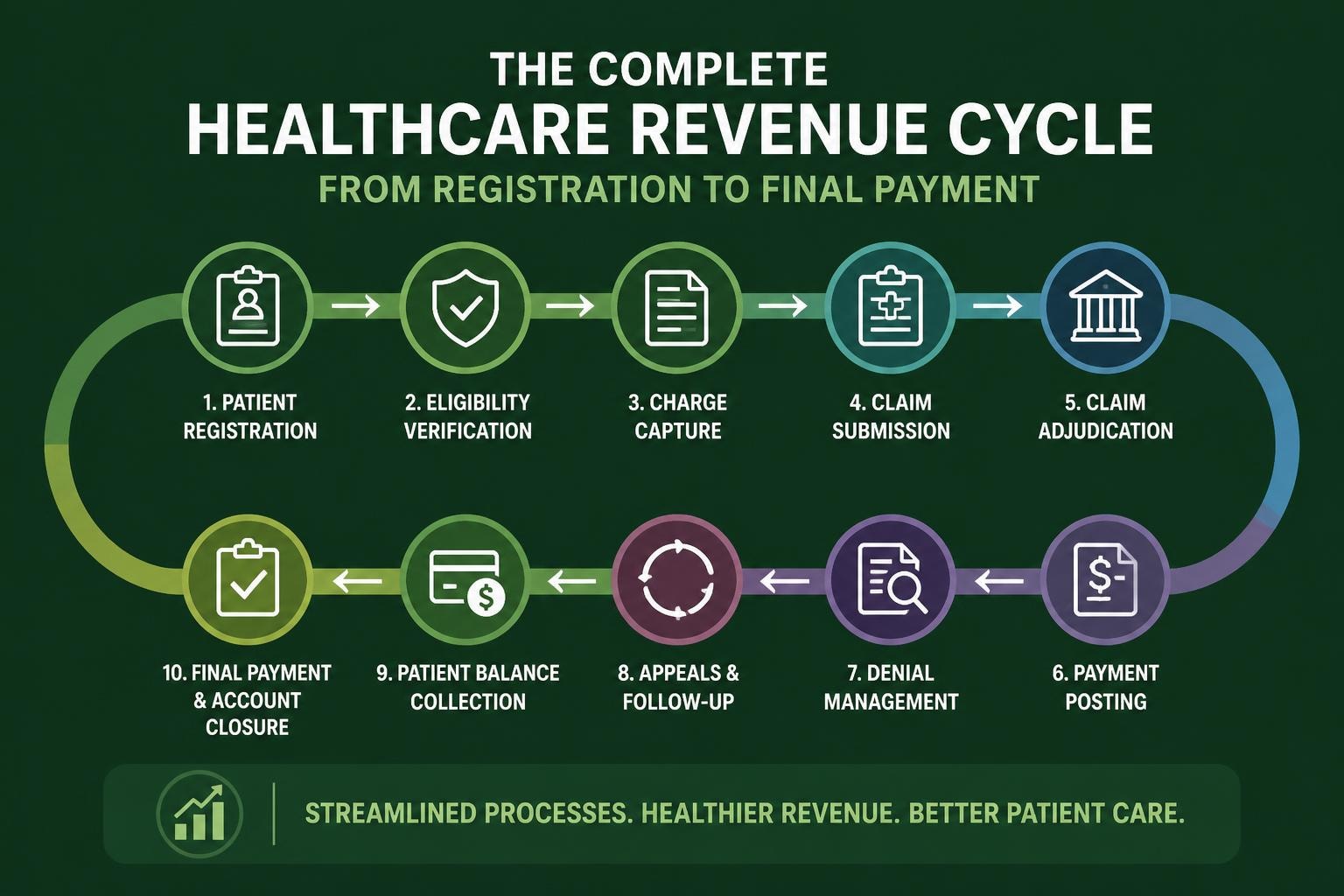
Revenue cycle solutions healthcare providers depend on encompass far more than simple billing services. These comprehensive systems address every touchpoint where financial transactions occur within a healthcare organization. According to research on revenue cycle components, the cycle begins before patients even receive care and continues until all balances are fully resolved.
Core Components of Effective Revenue Cycle Management
The foundation of successful revenue cycle solutions healthcare practices implement starts with patient access services. This critical first phase includes:
- Insurance eligibility verification and benefits confirmation
- Prior authorization management and approval tracking
- Patient demographic data collection and validation
- Financial counseling and payment arrangement setup
- Registration accuracy checks and error prevention
Eligibility verification alone can prevent thousands of dollars in denied claims when performed correctly. Eligibility verification services establish the groundwork for clean claims submission by confirming coverage details before services are rendered.
The Middle Revenue Cycle: Charge Capture and Coding
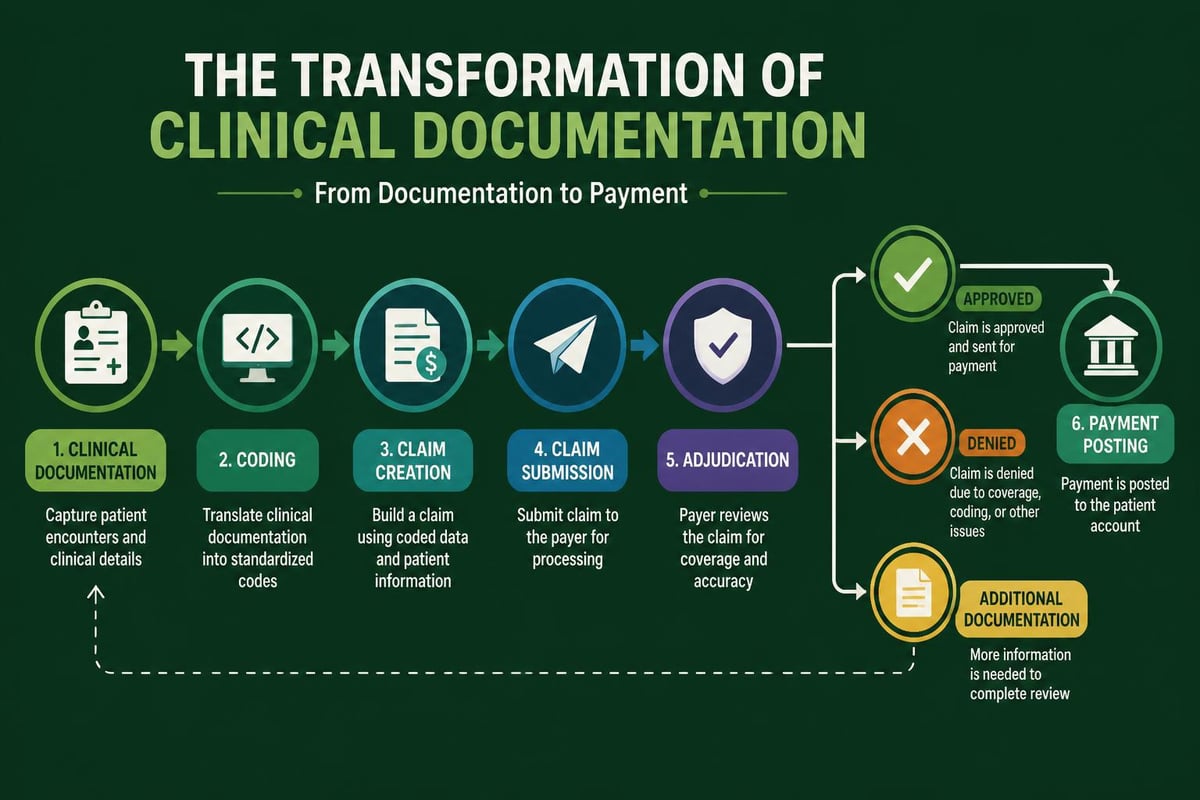
Once patient care is delivered, the middle revenue cycle phase transforms clinical documentation into billable claims. This segment requires precise medical coding and comprehensive charge capture processes.
Medical coding specialists translate provider documentation into standardized procedure codes (CPT) and diagnosis codes (ICD-10). The accuracy of this translation determines whether claims are paid, denied, or require additional information. Medical coding services ensure that documentation supports the codes submitted, reducing audit risk and maximizing appropriate reimbursement.
| Revenue Cycle Phase | Key Activities | Common Challenges |
|---|---|---|
| Front-End | Registration, eligibility verification, authorization | Incomplete patient data, coverage changes |
| Middle | Charge capture, coding, claim creation | Documentation gaps, coding errors |
| Back-End | Claim submission, payment posting, collections | Denials, underpayments, patient balances |
Technology-Driven Revenue Cycle Solutions Healthcare Providers Need
Modern revenue cycle solutions healthcare organizations utilize increasingly rely on sophisticated technology platforms. The American Hospital Association emphasizes that automation alone cannot solve revenue cycle challenges without proper integration of people, processes, and technology working in harmony.
Practice Management and Billing Systems
Practice management systems serve as the operational backbone for revenue cycle solutions healthcare practices implement. These platforms handle:
- Appointment scheduling coordinated with provider availability
- Patient registration workflows that capture complete demographic information
- Charge entry interfaces connecting to electronic health records
- Claim scrubbing tools that identify errors before submission
- Payment posting modules tracking all revenue sources
Integration between these systems eliminates data silos that create inefficiencies. When patient information flows seamlessly from registration through billing, the likelihood of errors decreases substantially.
Advanced Analytics and Reporting Tools
Data-driven decision-making separates high-performing revenue cycle operations from struggling ones. Reporting and analytics capabilities provide visibility into key performance indicators that reveal both strengths and weaknesses in revenue cycle performance.
Revenue cycle dashboards should track metrics including:
- Days in accounts receivable (A/R)
- First-pass claim acceptance rates
- Denial rates by payer and denial reason
- Collection rates for patient responsibility amounts
- Net collection percentages across all payer categories
These metrics illuminate exactly where revenue cycle solutions healthcare providers implement are succeeding or require adjustment.
Managing Claim Denials Through Comprehensive Solutions
Claim denials represent one of the most significant obstacles to healthy cash flow for healthcare organizations. Revenue cycle solutions healthcare practices adopt must include robust denial management strategies that both prevent denials and resolve them efficiently when they occur.
Prevention-Focused Denial Management
The most effective approach to denials addresses root causes before claims are ever submitted. Denial management services should incorporate preventive measures such as:
- Real-time eligibility verification at every patient encounter
- Pre-submission claim scrubbing with automated error detection
- Coding quality audits identifying patterns of incorrect code usage
- Authorization tracking systems preventing services without proper approval
- Documentation improvement programs ensuring medical necessity support
Proactive prevention costs significantly less than reactive denial resolution. Each denied claim requires staff time to research, correct, and resubmit, creating inefficiencies that drain resources.
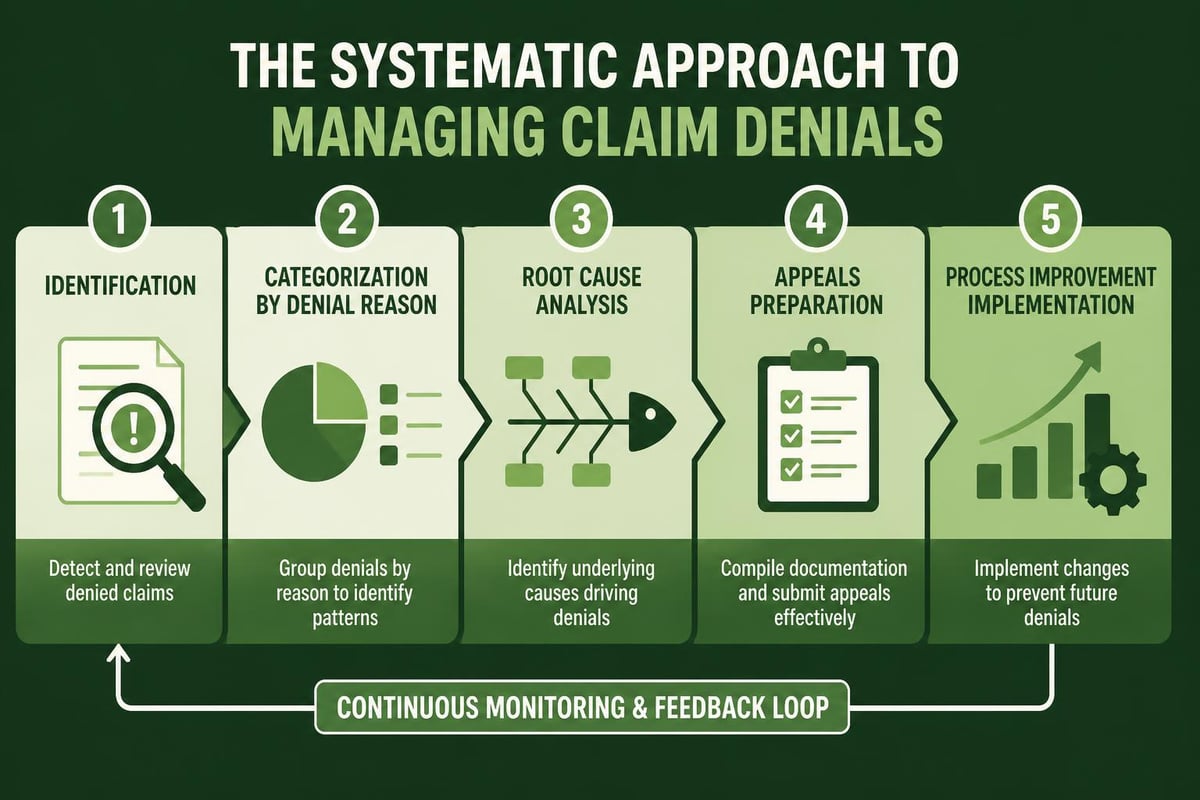
Resolution and Appeals Process
When denials do occur, rapid response determines recovery success rates. Effective revenue cycle solutions healthcare organizations employ include structured appeals processes with defined timeframes and responsibility assignments.
The denial resolution workflow should follow these steps:
- Immediate identification of denied claims through automated alerts
- Categorization by denial reason and payer requirements
- Priority assignment based on dollar value and appeal deadline
- Research and documentation gathering supporting evidence
- Appeal submission with complete justification and required attachments
- Follow-up tracking ensuring timely payer response
Understanding how denial management improves cash flow helps practices prioritize this crucial revenue cycle component.
Optimizing Patient Financial Responsibility Collections
The shift toward high-deductible health plans has dramatically increased the portion of revenue that healthcare providers must collect directly from patients. Revenue cycle solutions healthcare practices implement must now address patient collections with the same sophistication traditionally reserved for insurance claims.
Upfront Payment Estimation and Collection
Transparency in patient financial responsibility builds trust while improving collection rates. Before services are rendered, patients should receive accurate estimates of their out-of-pocket costs based on:
- Verified insurance benefits and remaining deductible amounts
- Specific procedures or services planned
- Historical payment patterns from the same payer
- Negotiated contract rates with the patient's insurance plan
Collecting patient responsibility amounts at the time of service yields significantly higher recovery rates than billing after the fact. Many practices now require payment of estimated amounts before scheduling elective procedures.
Payment Plan Options and Financial Counseling
Not all patients can pay their full balance immediately. Revenue cycle solutions healthcare providers implement should include flexible payment arrangements that make healthcare accessible while ensuring eventual payment.
Financial counseling services help patients understand:
- Total charges and insurance coverage details
- Available payment plan options with manageable installment amounts
- Charity care or financial assistance programs for qualifying patients
- Third-party financing options for larger balances
By addressing financial concerns proactively, practices reduce bad debt write-offs and maintain positive patient relationships.
Compliance and Regulatory Considerations
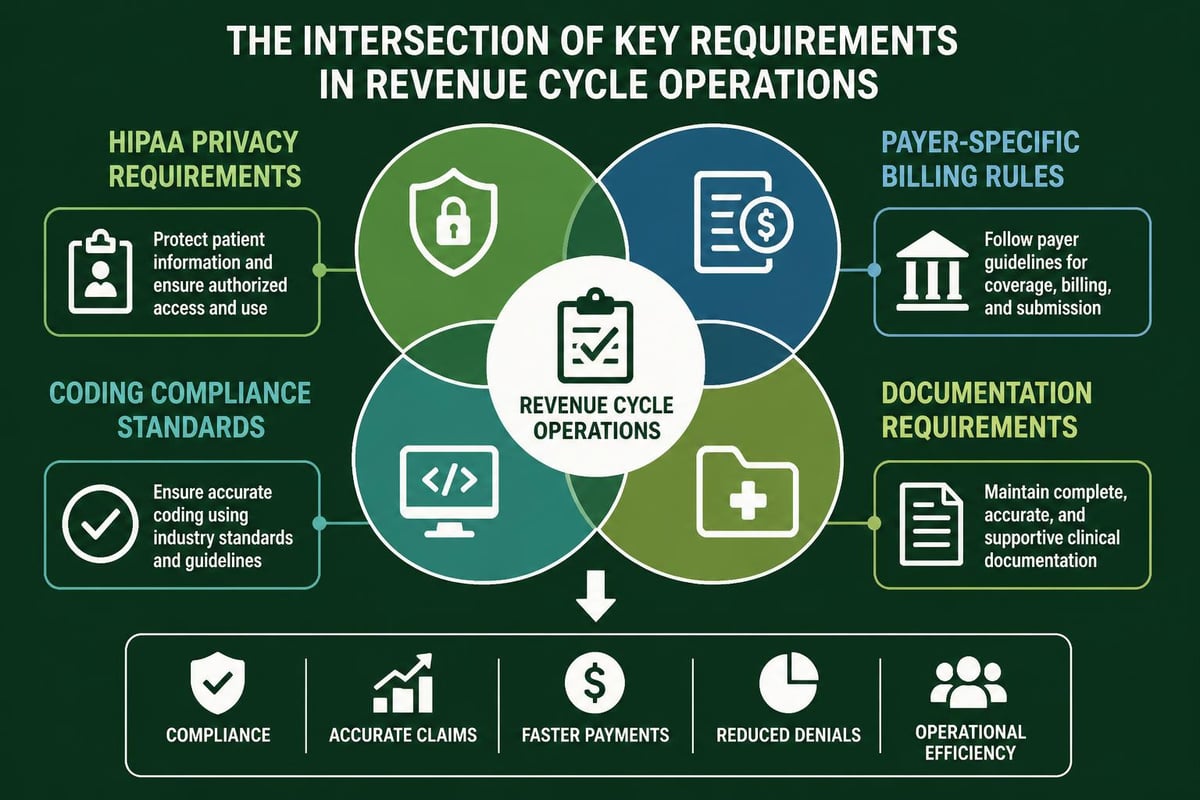
Revenue cycle solutions healthcare organizations depend on must maintain strict adherence to evolving regulatory requirements. Compliance failures result in denied claims, audits, and potential penalties that devastate practice finances.
HIPAA Security and Privacy Requirements
All revenue cycle operations involve protected health information (PHI) that falls under HIPAA regulations. Billing and collections activities require:
- Secure transmission of electronic claims and remittances
- Encrypted storage of patient financial and medical data
- Access controls limiting information visibility to authorized personnel
- Business associate agreements with all third-party service providers
- Regular security risk assessments and mitigation strategies
Outsourced revenue cycle solutions healthcare practices utilize must demonstrate comprehensive HIPAA compliance through documented policies, technical safeguards, and staff training programs.
Payer-Specific Requirements and Contract Terms
Each insurance payer establishes unique billing requirements, timely filing deadlines, and contract terms that govern reimbursement. Revenue cycle solutions healthcare providers implement must accommodate these variations through:
| Payer Type | Key Compliance Areas | Common Requirements |
|---|---|---|
| Medicare | Medical necessity, modifier usage | LCD/NCD adherence, MIPS reporting |
| Medicaid | State-specific billing rules | Prior authorization, spend-down tracking |
| Commercial | Contract terms, negotiated rates | Credentialing, timely filing (90-180 days) |
The American Hospital Association’s resources on revenue cycle management provide valuable guidance on navigating these complex regulatory requirements.
Selecting the Right Revenue Cycle Solutions Healthcare Partner
For many healthcare providers, managing the complete revenue cycle in-house stretches resources beyond capacity. Partnering with specialized revenue cycle management services allows practices to focus on patient care while experts handle complex billing operations.
Evaluating Service Provider Capabilities
When assessing potential revenue cycle solutions healthcare partners, providers should examine:
- Experience in your specialty, understanding unique coding and billing requirements
- Technology platforms the service provider utilizes and system integration capabilities
- Transparency in reporting, providing regular access to performance metrics and financial data
- Compliance certifications demonstrating adherence to HIPAA and industry standards
- Communication protocols ensuring your team stays informed of important issues
Medical billing services should function as an extension of your practice, not simply a vendor relationship.
Key Performance Indicators for Outsourced RCM
Accountability drives success in outsourced revenue cycle relationships. Establish clear performance expectations with measurable benchmarks:
- Clean claim rate above 95% on first submission
- Days in A/R maintained below 40 days
- Net collection rate exceeding 95% of expected reimbursement
- Denial rate below 5% of total claims submitted
- Response time for claim follow-up within 7 days of denial
Regular performance reviews ensure revenue cycle solutions healthcare practices have implemented continue delivering expected results.
Specialty-Specific Revenue Cycle Considerations
Different medical specialties face unique revenue cycle challenges requiring tailored solutions. Revenue cycle solutions healthcare providers need must address specialty-specific requirements including procedure complexity, payer mix, and documentation standards.
High-Volume Primary Care Practices
Primary care practices handle diverse patient populations with varying insurance coverage. Their revenue cycle challenges include:
- Managing large numbers of low-reimbursement encounters efficiently
- Coordinating care management programs with value-based payment models
- Processing numerous medication refills and minor procedure charges
- Handling wellness visits with complex preventive care coding rules
Efficiency and automation become critical for primary care revenue cycle success. Medical billing services for small practices must scale operations appropriately.
Specialty Practices With Complex Procedures
Specialties like cardiology, orthopedics, and gastroenterology face different challenges:
- Higher reimbursement per encounter requiring more detailed coding
- Complex modifier usage determining appropriate payment levels
- Frequent prior authorization requirements for expensive procedures
- Detailed documentation standards supporting medical necessity
- Higher audit risk due to procedure costs and complexity
These practices benefit from revenue cycle specialists with deep knowledge of specialty-specific requirements and payer policies.
Integration of Revenue Cycle With Clinical Operations
The most effective revenue cycle solutions healthcare organizations implement bridge the gap between clinical and financial operations. TechTarget’s exploration of revenue cycle technologies highlights how integrated systems optimize overall organizational performance.
Clinical Documentation Improvement Programs
Physician documentation drives coding accuracy and reimbursement appropriateness. Clinical documentation improvement (CDI) initiatives connect clinical care with revenue cycle outcomes by:
- Training providers on documentation requirements for common diagnoses
- Implementing templates that prompt complete information capture
- Conducting concurrent reviews identifying documentation gaps before billing
- Providing feedback to physicians on documentation quality and specificity
- Aligning documentation with quality reporting and value-based care metrics
Strong CDI programs protect practices from audits while ensuring maximum appropriate reimbursement for services provided.
Care Coordination and Authorization Management
Prior authorization services exemplify the intersection of clinical and revenue cycle operations. Obtaining authorizations requires:
- Clinical staff providing detailed procedure plans and medical justification
- Revenue cycle teams navigating payer-specific authorization portals
- Communication loops ensuring all parties know authorization status
- Tracking systems preventing services from proceeding without approval
- Appeals processes when initial authorization requests are denied
Coordinated authorization management prevents denied claims and schedule disruptions that frustrate both patients and providers.
Measuring Revenue Cycle Performance Success
Continuous improvement requires consistent measurement of revenue cycle outcomes. Revenue cycle solutions healthcare practices implement should include comprehensive performance tracking across all cycle phases.
Financial Performance Metrics
Core financial indicators reveal overall revenue cycle health:
- Gross collection rate: Total payments divided by total charges
- Net collection rate: Total payments divided by allowed amounts
- Cost to collect: Operating expenses as percentage of collections
- Cash collection per encounter: Average payment received per patient visit
- Point-of-service collections: Percentage of patient responsibility collected at visit
These metrics provide different perspectives on financial performance, each revealing specific strengths or improvement opportunities.
Operational Efficiency Indicators
Beyond financial outcomes, operational metrics identify process bottlenecks:
| Metric | Target Benchmark | What It Reveals |
|---|---|---|
| Claim submission lag | Under 3 days from service date | Charge capture and coding efficiency |
| First-pass resolution rate | Above 90% | Claim accuracy and clean claim percentage |
| Denial resolution time | Under 15 days | Denial management effectiveness |
| A/R over 90 days | Below 15% of total A/R | Collection follow-up processes |
Monitoring these indicators helps prioritize improvement initiatives that deliver meaningful impact.
Future Trends in Revenue Cycle Solutions Healthcare
The healthcare reimbursement landscape continues evolving rapidly. Revenue cycle solutions healthcare providers adopt must anticipate emerging trends including:
Value-Based Care and Alternative Payment Models
The shift from fee-for-service to value-based reimbursement fundamentally changes revenue cycle requirements. Practices must now track:
- Quality measure performance tied to bonus payments
- Patient outcome data demonstrating care effectiveness
- Care coordination activities often unreimbursed under traditional models
- Risk adjustment coding accurately reflecting patient complexity
- Shared savings calculations from accountable care arrangements
Revenue cycle systems must evolve beyond simple fee-for-service billing to capture and report these additional data elements.
Artificial Intelligence and Machine Learning Applications
AI-powered revenue cycle solutions healthcare organizations increasingly adopt include:
- Predictive analytics identifying claims likely to deny before submission
- Intelligent coding assistance suggesting appropriate procedure codes
- Automated payment posting recognizing and applying complex remittances
- Chatbots handling routine patient billing inquiries
- Pattern recognition detecting potential fraud or compliance issues
These technologies enhance human expertise rather than replacing skilled revenue cycle professionals.
Patient Experience and Consumer-Friendly Billing
Modern patients expect consumer-grade experiences from healthcare billing. Revenue cycle solutions healthcare practices implement must include:
- Mobile-responsive payment portals accessible from any device
- Clear, understandable billing statements avoiding medical jargon
- Multiple payment options including digital wallets and payment plans
- Proactive communication about upcoming bills and payment due dates
- Self-service account management reducing phone call volume
Patient satisfaction with billing processes impacts overall practice reputation and collection success rates.
Training and Staff Development for Revenue Cycle Excellence
Technology and processes alone cannot ensure revenue cycle success. The people executing these processes require ongoing training and development. Revenue cycle solutions healthcare practices depend on must include comprehensive staff education covering:
Regulatory Updates and Industry Changes
Healthcare regulations change constantly, requiring continuous education:
- Annual coding updates for CPT and ICD-10 code sets
- New payer policies and coverage determination changes
- HIPAA modifications and emerging privacy requirements
- State-specific billing regulations and Medicaid policy updates
- Fraud and abuse prevention including OIG guidance
Regular training sessions keep staff current on requirements affecting their daily responsibilities.
Technology Proficiency and System Optimization
Staff must fully utilize available technology features. Training should address:
- Advanced system features beyond basic functionality
- Reporting tools for monitoring individual and team performance
- Workflow customization adapting systems to practice preferences
- Integration capabilities connecting multiple platforms seamlessly
- Troubleshooting techniques resolving common technical issues
Investing in staff development maximizes the return on technology investments.
Building a Sustainable Revenue Cycle Strategy
Long-term revenue cycle success requires strategic planning beyond addressing immediate challenges. Revenue cycle solutions healthcare organizations implement should align with broader practice goals including growth plans, specialty focus changes, and financial objectives.
Strategic Planning Elements
Comprehensive revenue cycle strategy addresses:
- Capacity planning ensuring adequate resources for projected volume
- Payer mix optimization negotiating favorable contract terms
- Service line expansion preparing billing operations for new procedures
- Compliance monitoring proactively addressing regulatory risks
- Disaster recovery planning protecting revenue cycle operations from disruptions
Regular strategic reviews ensure revenue cycle operations support overall practice objectives rather than functioning in isolation.
Continuous Process Improvement
Net revenue management requires ongoing refinement of processes and procedures. Establish improvement cycles that:
- Identify underperforming areas through data analysis
- Research best practices and alternative approaches
- Implement changes on a pilot basis before full rollout
- Measure results and adjust as needed
- Standardize successful improvements across all processes
This iterative approach drives incremental gains that compound over time into substantial performance improvements.
Healthcare providers implementing comprehensive revenue cycle solutions position themselves for financial stability and sustainable growth in an increasingly complex reimbursement environment. From front-end eligibility verification through final payment collection, every touchpoint presents opportunities for optimization that directly impact practice profitability. Whether managing revenue cycle operations internally or partnering with specialized services, the key lies in combining technology, skilled professionals, and proven processes into an integrated system. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to maximize reimbursements, reduce denials, and streamline operations for healthcare providers nationwide. Our experienced team handles everything from eligibility verification through denial management, allowing your practice to focus on delivering exceptional patient care while we optimize your financial performance.