Selecting the right rcm vendor represents one of the most critical decisions healthcare providers face in optimizing their financial operations. The revenue cycle encompasses everything from patient registration and insurance verification to claims processing and payment collection, and partnering with the wrong vendor can lead to decreased cash flow, increased denials, and administrative burdens. With the healthcare revenue cycle management market continuously evolving, understanding how to evaluate and select a vendor that aligns with your practice's specific needs has never been more important for long-term financial sustainability.
Understanding What an RCM Vendor Brings to Your Practice
An rcm vendor provides specialized services and expertise designed to streamline your revenue cycle operations. These partnerships extend beyond simple billing services to encompass comprehensive solutions that address every stage of the revenue cycle. Healthcare providers who work with experienced vendors gain access to dedicated teams trained in the latest coding updates, payer requirements, and regulatory compliance standards.
Core Service Offerings
When evaluating potential partners, you'll encounter vendors offering various service models. Some provide end-to-end revenue cycle management, while others specialize in specific components.
Comprehensive RCM vendors typically offer:
- Patient eligibility verification and benefits confirmation
- Medical coding and charge capture services
- Claims submission and tracking
- Payment posting and reconciliation
- Denial management and appeals
- Patient billing and collections
- Reporting and analytics
The most effective partnerships develop when vendors integrate seamlessly with your existing workflows. Understanding revenue cycle management fundamentals helps providers recognize which services will deliver the greatest impact for their specific practice type and patient population.
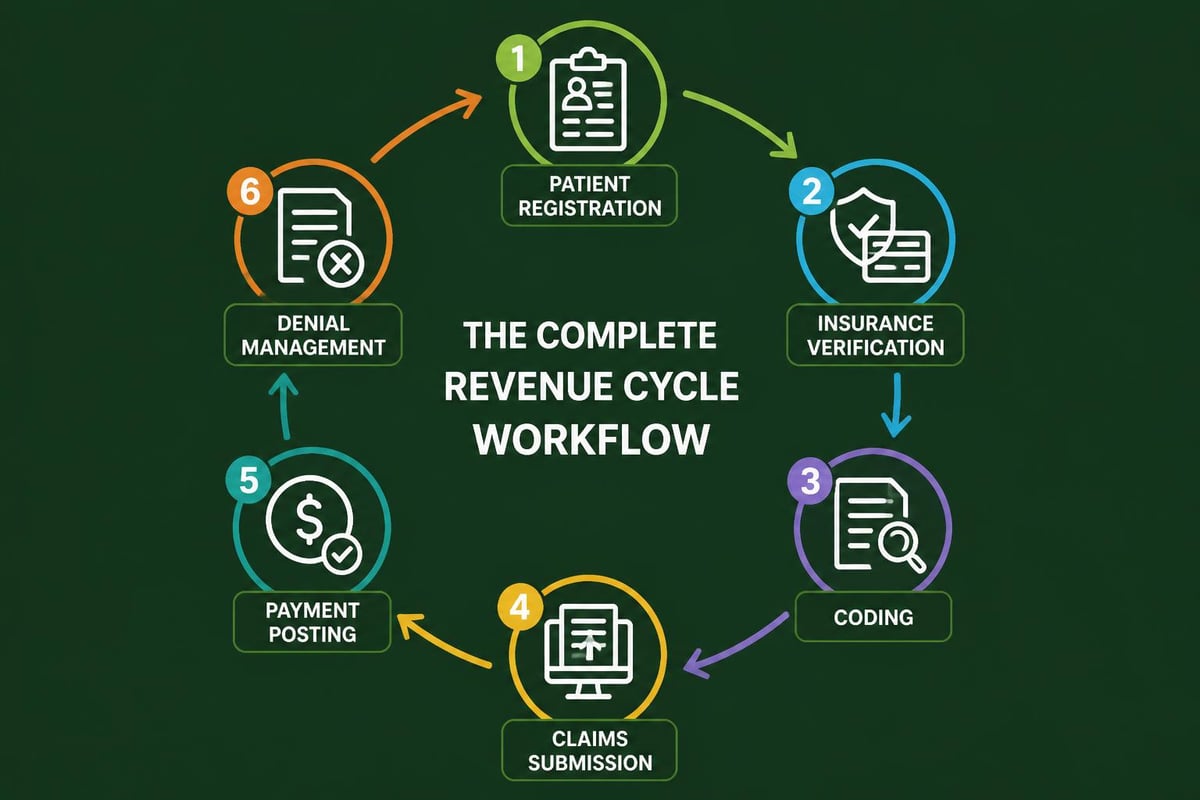
Technology and Integration Capabilities
Modern rcm vendor relationships depend heavily on technology infrastructure. The vendor's ability to integrate with your electronic health record (EHR) system determines how efficiently data flows between clinical and financial operations. Practices using advanced EHR platforms need vendors who can leverage these systems rather than creating duplicate data entry requirements.
| Integration Type | Benefits | Considerations |
|---|---|---|
| Direct EHR Integration | Automated charge capture, reduced errors | Requires compatible systems |
| API Connections | Real-time data exchange, scalability | Technical setup complexity |
| Manual Data Transfer | Works with any system | Higher error rates, slower processing |
| Portal-Based Access | Secure information sharing | May require duplicate entry |
The current landscape of RCM software shows increasing emphasis on integrated solutions that eliminate siloed operations. Providers should prioritize vendors who demonstrate technical proficiency with their existing technology stack.
Evaluating Performance Metrics and Vendor Capabilities
Selecting an rcm vendor requires objective assessment of their track record and capabilities. Performance metrics provide quantifiable evidence of a vendor's effectiveness in managing revenue cycles for practices similar to yours.
Key Performance Indicators to Review
Financial Performance Metrics:
- Clean claim rate – The percentage of claims accepted on first submission without errors
- Days in accounts receivable – Average time between service delivery and payment collection
- Collection rate – Percentage of expected revenue actually collected
- Denial rate – Percentage of claims initially denied by payers
- Cost to collect – Operational expenses as a percentage of revenue collected
Research from KLAS rankings of top revenue cycle management vendors demonstrates that high-performing vendors consistently maintain clean claim rates above 95% and keep accounts receivable below industry benchmarks. Request specific performance data from prospective vendors, ideally with references from clients in your specialty.
Specialty-Specific Expertise
Not all rcm vendor partners possess equal expertise across medical specialties. Cardiology practices face different coding complexities and payer requirements than pediatric clinics or surgical centers. Vendors with demonstrated experience in your specialty bring valuable knowledge of procedure-specific coding nuances, common denial reasons, and payer policies affecting your revenue.
Practices focusing on physician revenue cycle management benefit from vendors who understand the unique challenges physician groups encounter, including multispecialty billing, complex modifier usage, and physician credentialing requirements.
Compliance and Security Standards
Healthcare providers bear ultimate responsibility for protecting patient information and maintaining regulatory compliance, even when outsourcing revenue cycle functions. Your rcm vendor becomes an extension of your organization, requiring the same rigorous adherence to privacy and security standards you maintain internally.
HIPAA Compliance Requirements
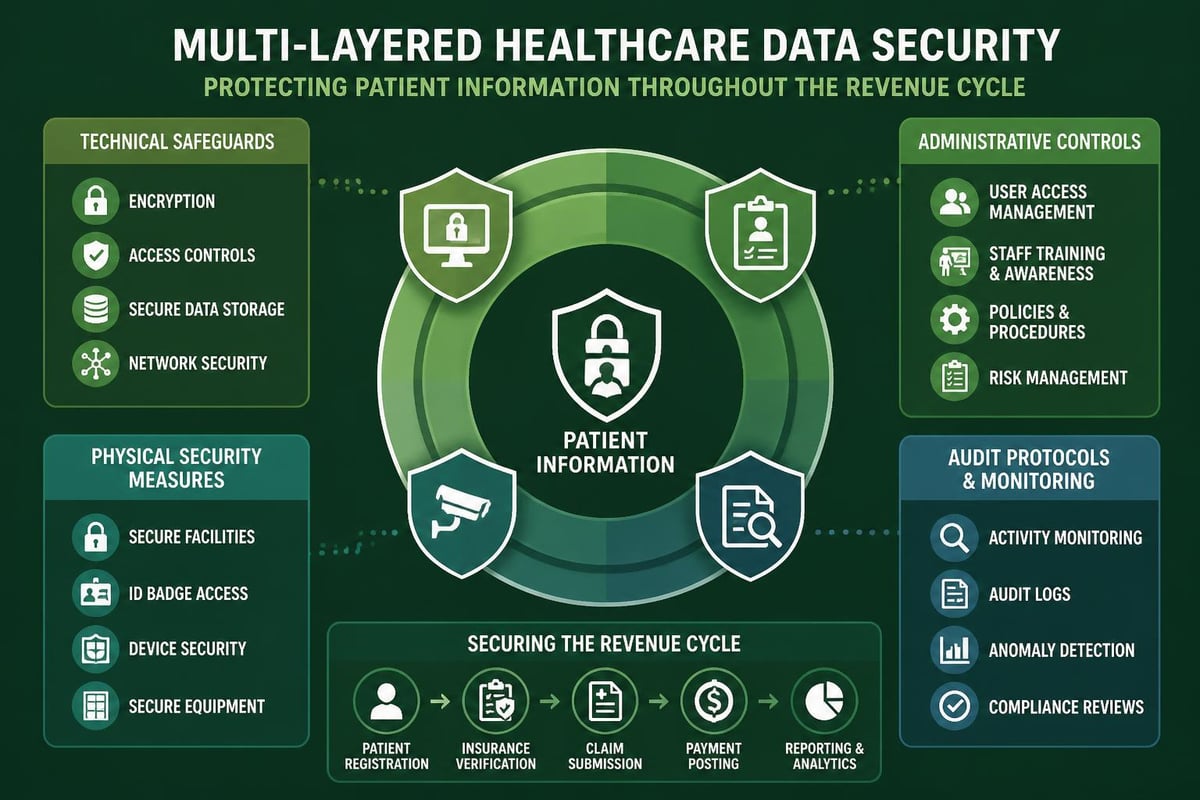
Every vendor handling protected health information (PHI) must demonstrate comprehensive HIPAA compliance programs. This includes technical safeguards, administrative policies, and physical security measures protecting patient data.
Essential compliance elements include:
- Business Associate Agreements (BAAs) clearly defining responsibilities
- Regular security audits and vulnerability assessments
- Employee training programs on PHI handling
- Incident response protocols for potential breaches
- Encryption for data transmission and storage
- Access controls limiting information to authorized personnel
Beyond basic compliance, leading vendors proactively monitor regulatory changes and update their processes accordingly. They provide transparent documentation of their security measures and willingly participate in your compliance audits.
Audit Support and Documentation
Revenue cycle operations generate extensive documentation that may be subject to payer audits, government investigations, or legal proceedings. Your rcm vendor should maintain organized, accessible records supporting every claim submitted on your behalf.
Strong vendors provide detailed audit trails showing who accessed patient accounts, what changes were made, and when actions occurred. This documentation proves essential during denial management processes and appeals requiring substantiation of medical necessity or proper coding.
Technology Platform Assessment
The technology infrastructure your rcm vendor employs directly impacts operational efficiency and your ability to access real-time financial data. Outdated systems create bottlenecks, while modern platforms enable proactive revenue cycle management.
System Features and Functionality
| Feature Category | Must-Have Capabilities | Advanced Capabilities |
|---|---|---|
| Eligibility Verification | Real-time benefit checks | Predictive coverage analysis |
| Claims Management | Electronic submission, tracking | Automated scrubbing, predictive analytics |
| Denial Management | Reason code tracking, appeal workflows | AI-powered denial prediction |
| Reporting | Standard financial reports | Customizable dashboards, trend analysis |
| Patient Engagement | Online billing statements | Payment plans, price estimation tools |
Modern platforms leverage automation to reduce manual tasks and minimize errors. Understanding back-end revenue cycle best practices reveals how technology streamlines claims processing, accelerates payment posting, and identifies revenue leakage before it impacts cash flow.
Reporting and Analytics Capabilities
Transparent, actionable reporting distinguishes exceptional rcm vendor partnerships from mediocre ones. You need visibility into every aspect of your revenue cycle performance, from individual claim status to aggregate financial trends.
Comprehensive reporting includes denial analysis identifying patterns by payer, procedure code, or denial reason. This intelligence enables targeted improvements addressing root causes rather than symptoms. Vendors offering healthcare revenue cycle analytics empower practices to make data-driven decisions optimizing financial performance.
Real-time dashboards provide immediate visibility into key metrics without waiting for monthly reports. Practice managers should be able to monitor daily charge entry, outstanding accounts receivable aging, and collection trends to identify issues requiring immediate attention.
Cost Structure and Contract Considerations
Understanding the financial relationship with your rcm vendor requires careful analysis of pricing models and contract terms. The least expensive option rarely delivers the best value when considering long-term financial performance.
Common Pricing Models
Percentage-based pricing charges a percentage of collections, typically ranging from 4% to 10% depending on specialty, claim volume, and services provided. This model aligns vendor incentives with your financial success, as they earn more when you collect more revenue.
Fixed-fee arrangements charge a set monthly amount regardless of collection volume. These contracts provide predictable expenses but may not incentivize maximum collection efforts.
Per-claim pricing charges for each claim submitted, which can work well for practices with consistent claim volumes but may become expensive during high-volume periods.
Hybrid models combine elements of multiple approaches, such as a base fee plus a lower collection percentage. These arrangements can balance cost predictability with performance incentives.
Contract Terms and Flexibility
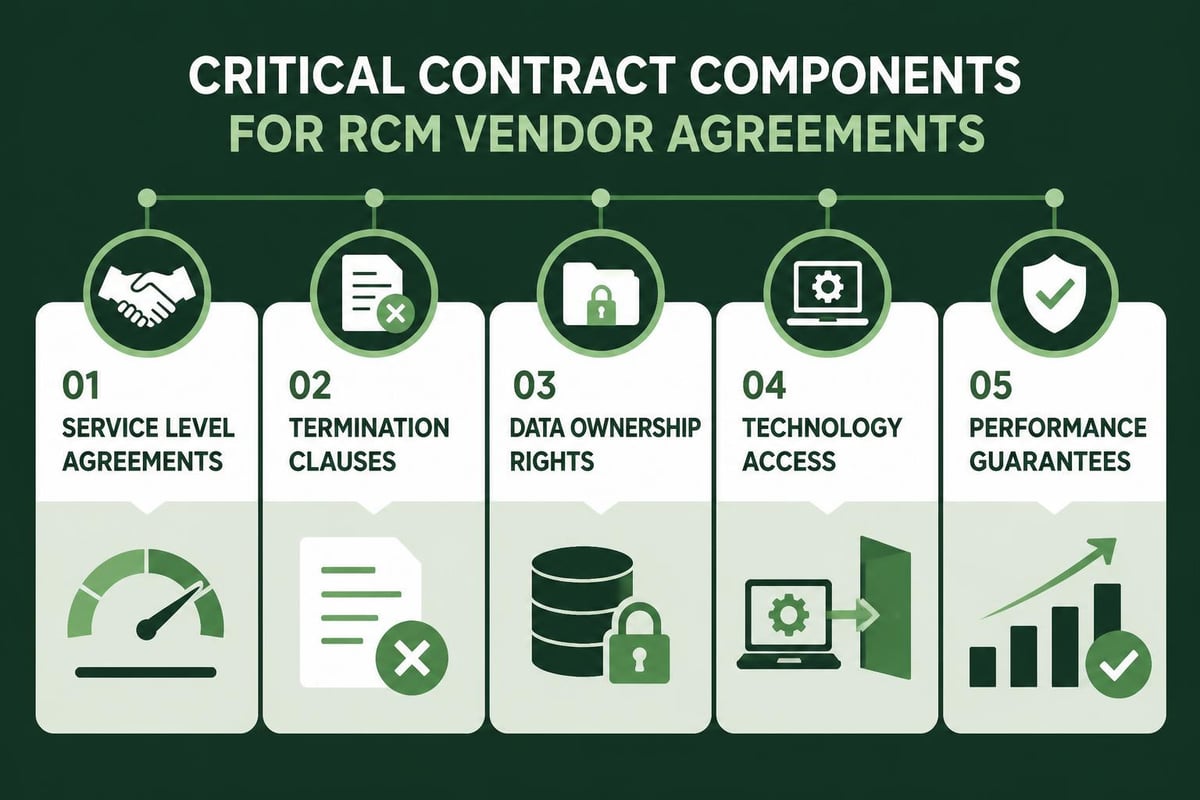
Contract length, termination provisions, and service level agreements significantly impact your relationship flexibility. Avoid long-term contracts without clear performance guarantees or reasonable exit provisions.
Key contract elements to negotiate:
- Performance guarantees with specific metrics and consequences
- Data ownership and accessibility provisions
- Transition assistance if changing vendors
- Fee structure clarity including any additional charges
- Service scope definitions preventing surprise billing
- Technology access during and after the contract
Some practices benefit from exploring net revenue management strategies that optimize overall revenue performance rather than focusing solely on gross collections. Your vendor should demonstrate understanding of how contractual adjustments, write-offs, and payer mix affect your bottom line.
Implementation and Transition Planning
Successfully partnering with an rcm vendor depends on smooth implementation and knowledge transfer. The transition period tests vendor capabilities and reveals how they'll perform long-term.
Step-by-Step Implementation Process
Step 1: Discovery and Planning
The vendor conducts a comprehensive assessment of your current processes, technology systems, and performance baseline. This phase establishes realistic timelines and identifies potential challenges.
Step 2: System Integration and Testing
Technical teams configure connections between your EHR and the vendor's platform. Thorough testing ensures data flows correctly and all functionality operates as expected.
Step 3: Training and Knowledge Transfer
Your staff receives training on new workflows, communication protocols, and system access. The vendor should document processes clearly and provide ongoing training resources.
Step 4: Parallel Processing Period
Many implementations include a period where both your internal team and the vendor process claims simultaneously, allowing verification that the vendor's work meets quality standards before full transition.
Step 5: Go-Live and Monitoring
The vendor assumes full responsibility for revenue cycle functions while closely monitoring performance metrics. Frequent communication during this period addresses any issues immediately.
Managing Change Within Your Practice
Staff members may resist outsourcing functions they previously handled internally. Successful transitions require clear communication about how the rcm vendor partnership benefits the practice and individual team members.
Providers should maintain involvement in revenue cycle oversight even when outsourcing operational tasks. Understanding revenue cycle billing processes enables you to ask informed questions and recognize when vendor performance falls short of expectations.
Ongoing Vendor Management and Optimization
Establishing a relationship with an rcm vendor marks the beginning, not the end, of revenue cycle optimization. Continuous monitoring, communication, and improvement ensure the partnership delivers sustained value.
Communication Protocols and Accountability
Regular meetings with your vendor team maintain alignment and address emerging issues. Effective partnerships include scheduled review sessions examining performance metrics, discussing payer policy changes, and identifying improvement opportunities.
| Meeting Type | Frequency | Focus Areas |
|---|---|---|
| Operational Status | Weekly | Claim status, urgent issues, payer communications |
| Performance Review | Monthly | KPI analysis, denial trends, collection rates |
| Strategic Planning | Quarterly | Process improvements, technology updates, contract review |
| Executive Summary | Annual | Year-over-year performance, contract renewal, strategic goals |
Accountability mechanisms ensure vendors maintain promised service levels. Establish clear escalation procedures for unresolved issues and document vendor responsiveness to concerns.
Continuous Improvement Initiatives
Leading vendors don't simply maintain baseline performance but actively seek opportunities to enhance results. They should present improvement initiatives based on data analysis and industry best practices.
For practices offering specialized services, vendors should understand unique billing requirements. For example, practices providing annual wellness visits need vendors familiar with age-specific coding requirements and documentation standards.
Revenue cycle best practices evolve as payer requirements change and new technologies emerge. Your vendor should proactively communicate industry changes affecting your revenue and recommend process adjustments maintaining optimal performance.
Vendor Comparison and Selection Framework
Choosing between multiple qualified rcm vendor candidates requires systematic evaluation preventing costly mistakes. Structured comparison frameworks ensure you consider all relevant factors before making this important decision.
Creating Your Evaluation Scorecard
Develop a weighted scorecard assigning point values to criteria based on their importance to your practice. This objective approach prevents emotional decisions and documents your selection rationale.
Sample Evaluation Categories:
- Technical Capabilities (25%) – System features, integration options, reporting tools
- Performance Track Record (25%) – Clean claim rates, collection rates, references
- Compliance and Security (20%) – HIPAA programs, audit capabilities, certifications
- Cost Structure (15%) – Pricing model, contract terms, hidden fees
- Implementation Support (10%) – Transition planning, training, timeline
- Communication and Service (5%) – Responsiveness, dedicated account management
Resources like user reviews of top RCM vendors provide valuable insights into real-world vendor performance beyond marketing materials. Contact references from practices similar to yours in size, specialty, and geographic location.
Red Flags to Avoid
Certain warning signs during the vendor evaluation process signal potential problems that may emerge after contract signing.
Be cautious of vendors who:
- Promise unrealistic results without understanding your current performance
- Refuse to provide client references or performance data
- Lack experience with your specialty or EHR system
- Offer significantly lower pricing than competitors without explanation
- Present vague or confusing contract terms
- Demonstrate poor communication during the sales process
- Cannot clearly explain their technology infrastructure
- Show unwilling to negotiate contract terms or service guarantees
Some practices find value in consulting resources about the best medical billing companies to understand market standards and competitive offerings.
Specialty-Specific Vendor Considerations
Different medical specialties face unique revenue cycle challenges requiring specialized vendor expertise. Understanding these nuances helps you select an rcm vendor prepared to address your specific needs.
High-Volume Specialties
Primary care practices, urgent care centers, and other high-volume providers need vendors who can efficiently process large claim volumes while maintaining accuracy. Automation capabilities become especially important for these practices.
Vendors serving urgent care revenue cycle management needs should understand after-hours coding requirements, multiple diagnosis management, and the high percentage of self-pay patients typical in urgent care settings.
Complex Procedural Specialties
Surgical specialties, interventional radiology, and other procedure-intensive practices require vendors with deep coding expertise. These specialties frequently use complex modifiers, bundle procedures correctly, and navigate medical necessity requirements.
Understanding clean claim requirements becomes critical when procedures involve multiple components that must be coded precisely to avoid denials and payment delays.
Behavioral Health and Mental Health Services
Behavioral health practices encounter unique payer requirements, authorization processes, and documentation standards. Vendors serving this specialty need familiarity with medical billing for behavioral health including telehealth billing, session coding, and state-specific Medicaid requirements.
Selecting the right rcm vendor fundamentally impacts your practice's financial health and operational efficiency. By systematically evaluating vendor capabilities, technology platforms, compliance standards, and specialty expertise, healthcare providers position themselves for successful partnerships that optimize revenue cycle performance. Greenhive Billing Solutions delivers comprehensive revenue cycle management services specifically tailored for healthcare providers, combining experienced professionals with industry-standard technology to improve clean claim rates, accelerate collections, and ensure HIPAA compliance. Our transparent communication and proven track record help practices across the United States maximize reimbursements while focusing on patient care.