Healthcare providers across New York face mounting challenges with complex billing requirements, evolving payer regulations, and increasing administrative burdens. Medical billing companies in New York have emerged as essential partners, enabling practices to focus on patient care while ensuring accurate reimbursements and financial stability. The state's unique regulatory environment, combined with diverse payer mixes including Medicaid, Workers' Compensation, and commercial insurance, creates a landscape where specialized revenue cycle management expertise becomes invaluable. Understanding what these companies offer and how to select the right partner can transform a practice's financial performance.
The Unique Landscape of Medical Billing in New York
New York's healthcare billing environment presents distinct challenges that set it apart from other states. The combination of state-specific Medicaid regulations, Workers' Compensation requirements, and local payer policies demands specialized knowledge that many practices find difficult to maintain in-house.
Medical billing companies in New York must navigate a complex web of regulations, including strict documentation requirements and coding standards that differ from federal guidelines. The state's Medicaid program, one of the largest in the nation, has unique billing protocols and reimbursement structures that require expertise to maximize collections.

State-Specific Billing Considerations
Several factors make New York's billing landscape particularly challenging:
- Medicaid complexity: New York Medicaid includes multiple managed care plans with varying authorization and billing requirements
- Workers' Compensation regulations: Specific fee schedules and documentation standards that differ significantly from other coverage types
- No-fault insurance: Auto accident-related claims follow unique protocols under New York's no-fault insurance laws
- Prior authorization mandates: Many procedures require pre-approval through state-specific systems
According to recent industry analysis on New York medical billing challenges, providers must understand nuanced payer regulations to avoid claim denials and payment delays. This complexity has driven many practices to seek external expertise.
| Billing Challenge | Impact on Practices | Solution Required |
|---|---|---|
| State Medicaid variations | Delayed reimbursements | Specialized knowledge of NY Medicaid |
| Workers' Comp complexity | Higher denial rates | Expertise in fee schedules |
| Prior authorization delays | Treatment interruptions | Efficient authorization management |
| Payer-specific requirements | Administrative burden | Comprehensive payer knowledge |
Core Services Provided by Medical Billing Companies
Comprehensive revenue cycle management encompasses multiple interconnected processes. Medical billing companies in New York typically offer integrated services designed to optimize each stage of the billing cycle.
Claims Processing and Submission
Professional claims processing requires meticulous attention to coding accuracy, documentation requirements, and payer-specific submission protocols. Medical claim submission services ensure that claims are submitted correctly the first time, reducing the likelihood of denials or payment delays.
Effective claims submission includes:
- Accurate coding: Applying correct ICD-10, CPT, and HCPCS codes based on clinical documentation
- Electronic submission: Utilizing clearinghouses and direct payer portals for efficient transmission
- Clean claim focus: Scrubbing claims before submission to identify potential errors
- Timely filing: Ensuring claims are submitted within payer-specific deadlines
Insurance Verification and Eligibility
Eligibility verification services represent a critical first step in the revenue cycle. Verifying patient insurance coverage before services are rendered prevents downstream billing issues and reduces the risk of unpaid claims.
Real-time verification includes checking coverage status, identifying co-payments and deductibles, confirming benefit limitations, and verifying authorization requirements. This proactive approach minimizes billing surprises and improves patient satisfaction.
Denial Management and Appeals
Even with careful claim preparation, denials occur. The denial management process requires systematic analysis to identify root causes and implement corrective actions.
Medical billing companies in New York employ dedicated denial management teams that analyze rejection patterns, prepare compelling appeals with supporting documentation, track appeal status through resolution, and implement process improvements to prevent recurring denials. Research shows that effective denial management directly improves cash flow by recovering revenue that might otherwise be written off.
Technology and Automation in Medical Billing
The medical billing industry is experiencing significant transformation through technology adoption. Automation and artificial intelligence are reshaping how billing companies process claims and manage revenue cycles.
Automation Trends
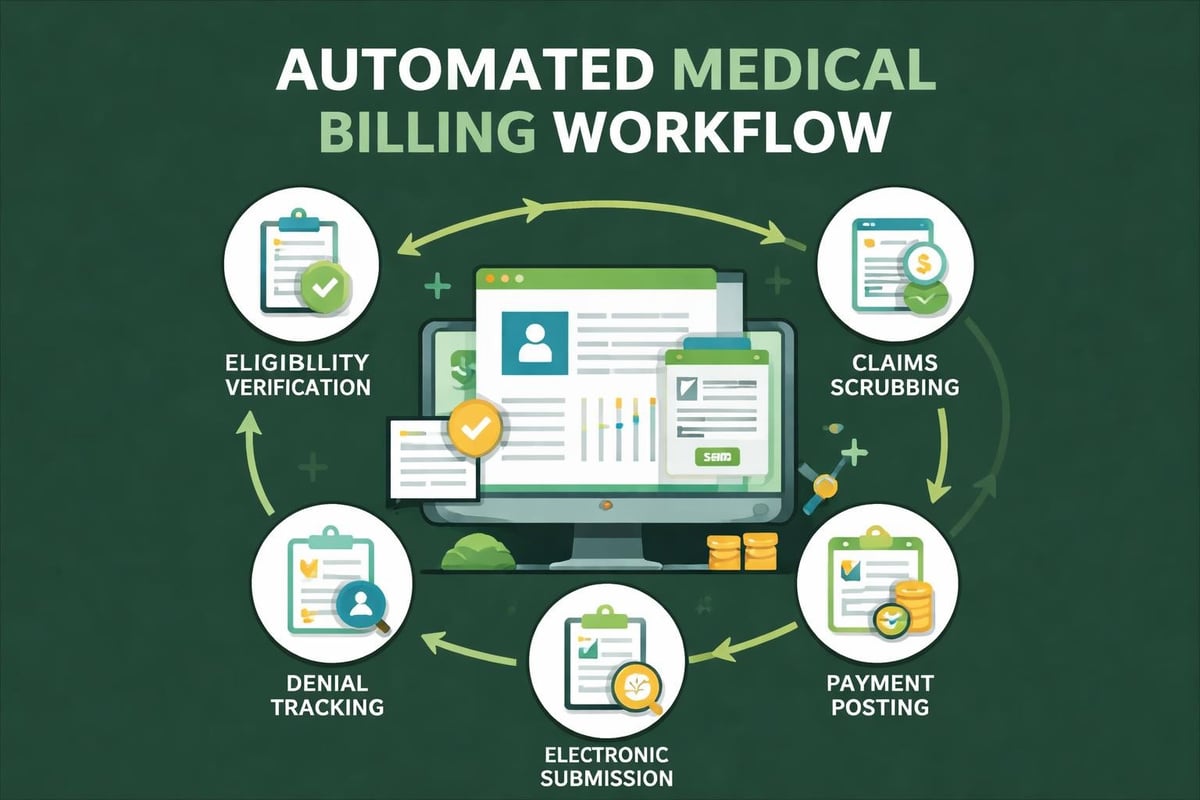
According to the 2026 state of medical billing industry report, automation has become essential for managing increasing claim volumes while maintaining accuracy. Billing companies leverage automation for eligibility verification, claims scrubbing, payment posting, and denial pattern analysis.
Advanced systems now incorporate machine learning algorithms that identify coding errors before submission, predict denial likelihood based on historical data, automate routine correspondence with payers, and optimize workflow distribution among billing staff.
Emerging Technologies
Research on Symphony for Medical Coding demonstrates how artificial intelligence systems are being developed for scalable and explainable medical coding. These innovations promise to enhance accuracy while reducing manual coding time.
Similarly, generative AI applications for surgical billing show how specialized AI can handle complex coding scenarios in specific medical specialties. These technological advances enable medical billing companies in New York to deliver higher accuracy and faster processing times.
Compliance and HIPAA Requirements
Regulatory compliance represents a non-negotiable aspect of medical billing operations. Billing companies must maintain strict adherence to HIPAA privacy and security rules, state-specific billing regulations, payer contract requirements, and federal fraud and abuse laws.
HIPAA Compliance Standards
Professional billing companies implement comprehensive safeguards including:
- Physical security: Secure facilities with controlled access
- Technical safeguards: Encrypted data transmission and storage
- Administrative controls: Staff training and documented policies
- Business associate agreements: Formal contracts outlining compliance responsibilities
The 2026 medical billing industry trends emphasize that compliance complexity continues to increase, making it essential for billing companies to maintain robust compliance programs.
Audit Preparedness
Regular internal audits help identify potential compliance gaps before they become serious issues. Billing companies should conduct coding accuracy reviews, documentation completeness checks, billing pattern analysis, and payer contract compliance verification.
Selecting the Right Medical Billing Partner
Choosing a medical billing company requires careful evaluation of multiple factors. Practices should assess capabilities, experience, and cultural fit to ensure a successful partnership.
Evaluation Criteria
| Factor | What to Look For | Why It Matters |
|---|---|---|
| Specialty expertise | Experience with your specific medical specialty | Coding and billing requirements vary significantly by specialty |
| Technology platform | Modern, integrated systems with reporting capabilities | Impacts efficiency and visibility into financial performance |
| Compliance record | Clean audit history and robust compliance programs | Protects your practice from regulatory risk |
| Communication style | Transparent reporting and responsive support | Ensures alignment and quick issue resolution |
| Pricing structure | Clear, predictable pricing with defined services | Prevents unexpected costs and budget surprises |
Questions to Ask Prospective Billing Companies
During the evaluation process, practices should inquire about specific performance metrics, staff qualifications and turnover rates, technology investments and capabilities, disaster recovery and business continuity plans, and references from similar practices.
Understanding why NYC healthcare practices are outsourcing their medical billing provides context for this decision-making process and highlights common motivations.
Performance Metrics and Accountability
Effective partnerships with medical billing companies in New York require clear performance expectations and regular monitoring. Establishing key performance indicators (KPIs) ensures accountability and enables continuous improvement.
Critical Billing Metrics
Practices should track several essential metrics:
- Clean claim rate: Percentage of claims accepted on first submission
- Days in accounts receivable: Average time from service to payment
- Collection rate: Percentage of expected reimbursement actually collected
- Denial rate: Percentage of claims initially denied
- Net collection rate: Collections divided by expected contractual reimbursement
Understanding what ERA in medical billing means helps practices leverage electronic remittance advice for faster payment reconciliation and improved accuracy.
Reporting and Transparency
Quality billing companies provide comprehensive reporting dashboards, regular performance reviews, transparent communication about challenges, and proactive recommendations for improvement. Reporting and analytics capabilities enable practices to make data-driven decisions about their revenue cycle.
Specialty-Specific Billing Considerations
Different medical specialties face unique billing challenges. Medical billing companies in New York often develop specialized expertise to address these nuances effectively.

Primary Care Billing
Primary care practices navigate complex preventive care billing, including annual wellness visit CPT codes by age, chronic care management codes, and value-based payment models. Billing companies must understand modifier usage for preventive services billed with problem-focused visits.
Specialty Practice Requirements
Specialized practices require billing expertise tailored to their procedures and common payer policies. For instance, cardiology medical billing involves complex cardiac procedures, diagnostic testing codes, and multiple procedure payment reductions that demand specific coding knowledge.
Surgical specialties benefit from understanding revenue codes in medical billing for facility billing alongside professional fee coding. The intersection of digital health services with traditional billing creates additional complexity, as explored in reimbursement billing code analysis.
Cost Structures and Return on Investment
Understanding billing company pricing models helps practices evaluate the financial impact of outsourcing. Medical billing companies in New York typically offer several pricing approaches, each with distinct advantages.
Common Pricing Models
Percentage of collections: Most common model, typically ranging from 4% to 10% of collected revenue. This aligns the billing company's success with the practice's financial performance.
Flat fee per claim: Fixed price per claim submitted, providing predictable costs regardless of claim value. This works well for practices with consistent claim volumes and values.
Monthly retainer: Fixed monthly fee for comprehensive services. Offers budget predictability but may not align incentives as directly as percentage-based models.
Calculating ROI
Practices should evaluate total cost savings from reduced staff overhead, increased collections from improved processes, reduced denial rates and faster reimbursement, and improved compliance reducing audit risk. Many practices find that professional billing services not only pay for themselves but significantly improve overall financial performance.
The Future of Medical Billing in New York
The medical billing landscape continues to evolve rapidly. Several trends are shaping the future of how medical billing companies in New York operate and deliver value.
Value-Based Care Integration
The transition from fee-for-service to value-based reimbursement models requires billing companies to track quality metrics alongside traditional billing data. This includes monitoring patient outcomes, coordinating care across providers, managing risk-based contracts, and reporting quality measures to payers.
Blockchain and Security Innovations
Emerging technologies like blockchain offer potential solutions for billing claims management, as discussed in blockchain applications in healthcare. While still evolving, these technologies promise enhanced security, reduced fraud, and streamlined claims processing.
Patient Financial Experience
Modern billing companies increasingly focus on the patient payment experience, including transparent cost estimates before services, convenient payment options and plans, clear, understandable billing statements, and compassionate collections approaches.
Transitioning to a New Billing Company
Successfully transitioning billing operations requires careful planning and execution. Practices should follow a structured approach to minimize disruption and ensure continuity.
Transition Planning Steps
- Document current processes: Create detailed documentation of existing workflows
- Set clear timelines: Establish realistic milestones for each transition phase
- Coordinate data migration: Ensure complete transfer of patient and billing records
- Train staff: Prepare your team for new processes and communication channels
- Monitor closely: Track performance metrics carefully during initial months
The transition period typically spans 60-90 days, during which practices should expect frequent communication and potential adjustments as systems and processes are refined.
Risk Mitigation
Protecting revenue during transition requires maintaining backup access to previous systems, closely monitoring days in accounts receivable, verifying successful claim submission to all payers, and maintaining clear communication channels with the billing company.
Integration with Practice Management Systems
Seamless integration between billing operations and practice management systems ensures efficiency and accuracy. Medical billing companies in New York must work effectively with various software platforms commonly used by healthcare providers.
Software Compatibility
Understanding top medical billing software options helps practices appreciate how billing companies adapt to different technological environments. Professional billing services maintain expertise across multiple platforms and can work within existing practice systems.
This flexibility allows practices to maintain their preferred workflows while benefiting from specialized billing expertise. The billing company's staff learns the practice's system rather than forcing the practice to adopt new technology.
Navigating New York's complex medical billing environment requires specialized expertise, advanced technology, and unwavering attention to compliance. Medical billing companies in New York provide healthcare providers with comprehensive revenue cycle management that improves financial performance while reducing administrative burden. Whether you're struggling with claim denials, seeking to optimize collections, or simply looking to refocus staff time on patient care, partnering with experienced billing professionals delivers measurable results. Greenhive Billing Solutions offers tailored revenue cycle management services that combine industry expertise with transparent communication, helping practices across the United States maximize reimbursements and streamline operations.

