Healthcare providers throughout Florida face increasingly complex billing challenges that directly impact their financial stability and operational efficiency. From navigating intricate insurance requirements to maintaining compliance with state and federal regulations, managing revenue cycle operations demands specialized expertise and dedicated resources. Medical billing services florida providers rely on must deliver accuracy, transparency, and measurable results while adapting to the unique regulatory landscape of the Sunshine State.
Florida's diverse healthcare ecosystem-spanning major metropolitan areas like Miami, Tampa, and Jacksonville to rural communities-presents distinct challenges for medical practices. Provider organizations must balance patient care with administrative demands, making strategic partnerships with experienced billing teams essential for sustainable growth and profitability.
Understanding Florida's Medical Billing Landscape
Florida's healthcare industry operates under a complex framework of state and federal regulations that directly affect billing practices. The state's unique insurance market, combined with a large Medicare population and specific Medicaid requirements, creates layers of compliance considerations that practices must navigate successfully.
State-Specific Regulatory Requirements
Medical billing services florida practitioners choose must demonstrate thorough knowledge of state regulations. The Florida Department of Health establishes guidelines that impact billing practices, including requirements for provider licensure, patient privacy protections, and documentation standards. These regulations complement federal HIPAA requirements while adding state-specific nuances.
Florida's regulatory environment includes several critical components:
- Provider enrollment and credentialing requirements that vary by payer
- State-specific modifier usage for certain procedures
- Unique documentation standards for particular service categories
- Compliance with Florida's patient access to healthcare records laws
- Adherence to state-mandated billing transparency requirements
The Florida Medicaid program presents its own set of billing procedures and compliance requirements. Providers serving Medicaid beneficiaries must understand prior authorization protocols, covered services limitations, and specific billing formats that differ from commercial insurance or Medicare requirements.

Insurance Payer Mix Challenges
Florida's insurance landscape includes major commercial carriers, Medicare Advantage plans, traditional Medicare, Medicaid managed care organizations, and self-pay patients. Each payer category requires distinct billing approaches, timely filing deadlines, and documentation standards.
Understanding payer-specific requirements becomes critical when working with organizations like Florida Blue, the state's Blue Cross Blue Shield plan. Their billing requirements, pre-authorization processes, and claims submission protocols demand attention to detail and consistent adherence to their guidelines.
| Payer Type | Key Billing Considerations | Average Processing Time |
|---|---|---|
| Medicare Traditional | CMS guidelines, modifier requirements, LCD/NCD policies | 14-30 days |
| Medicare Advantage | Prior authorization, network requirements, varied plan designs | 21-45 days |
| Commercial Insurance | Credentialing, contract terms, plan-specific coding requirements | 30-60 days |
| Florida Medicaid | Program limitations, managed care coordination, specific billing formats | 30-90 days |
Essential Services Provided by Florida Medical Billing Companies
Comprehensive medical billing services florida providers need extend far beyond simple claims submission. Professional billing partners deliver integrated solutions that address every stage of the revenue cycle, from patient registration through final payment posting.
Claims Processing and Submission
Accurate claims processing forms the foundation of successful revenue cycle management. Professional billing services utilize industry-standard software platforms to:
- Scrub claims for errors before submission
- Apply correct CPT and ICD-10 codes based on documentation
- Attach necessary modifiers according to payer requirements
- Submit electronic claims through secure clearinghouses
- Track claim status through adjudication
Understanding what is a CPT code for insurance becomes essential for accurate billing. Current Procedural Terminology codes, maintained by the American Medical Association, describe medical procedures and services, forming the language healthcare providers use to communicate with payers.
The claims submission process requires meticulous attention to detail at every step. Experienced billing professionals verify patient demographics, insurance coverage, and service documentation before claim creation. They understand that a single error-whether a transposed digit in a policy number or an incorrect modifier-can delay payment by weeks or result in outright denial.
Insurance Eligibility Verification
Verifying patient insurance coverage before service delivery prevents denied claims and billing disputes. Professional eligibility verification services confirm active coverage, identify coverage limitations, determine patient financial responsibility, verify prior authorization requirements, and check for coordination of benefits situations.
This proactive approach significantly reduces claim denials related to eligibility issues. When verification occurs before appointments, practices can collect appropriate copayments, discuss payment options with patients, and avoid providing services that insurance won't cover.
Real-time eligibility verification has become standard practice among leading medical billing services florida providers employ. This technology allows immediate confirmation of coverage status, deductible amounts, and copayment requirements, enabling front-desk staff to have informed financial conversations with patients.
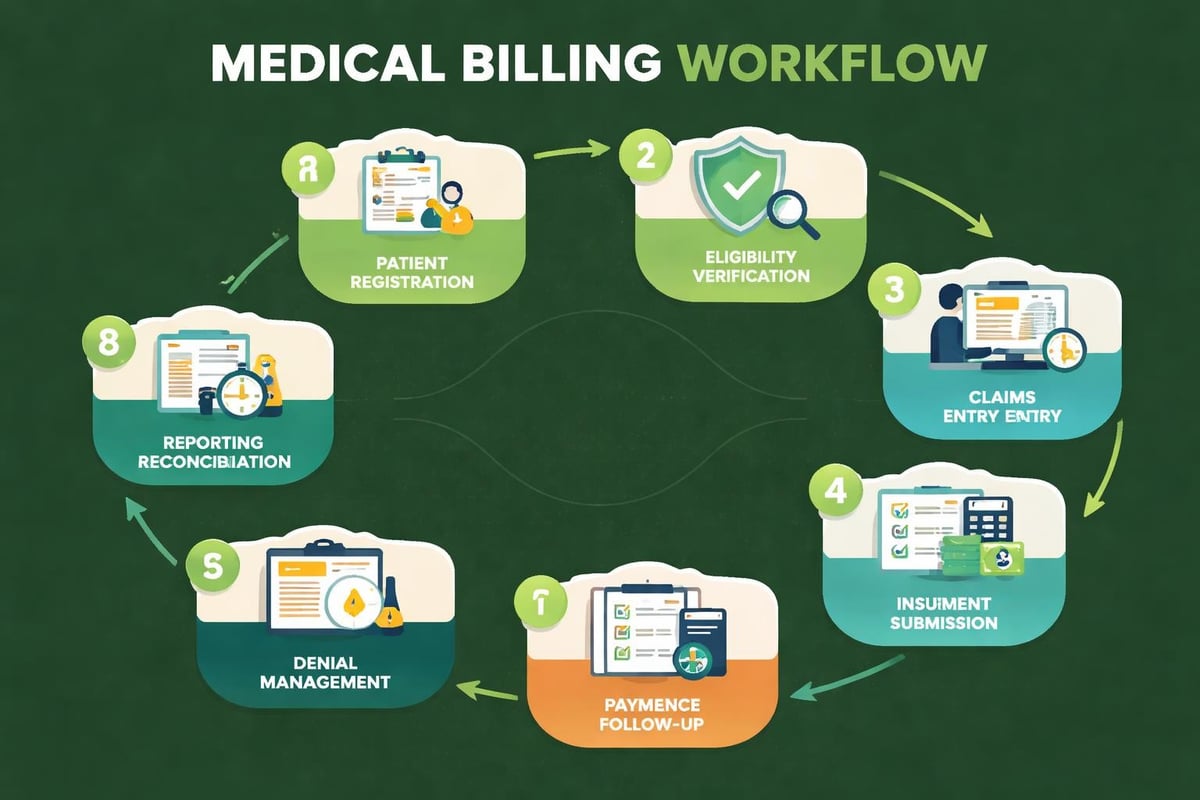
Denial Management and Appeals
Even well-prepared claims face denials. Effective denial management in medical billing transforms these setbacks into recovered revenue through systematic appeal processes.
Professional denial management includes five critical steps:
- Denial categorization and root cause analysis to identify patterns and systemic issues
- Priority assignment based on claim value and appeal deadline
- Documentation gathering to support appeal arguments with clinical evidence
- Appeal letter preparation addressing specific denial reasons with payer policy citations
- Resubmission tracking to ensure appeals receive appropriate consideration
Understanding types of modifiers in medical billing proves particularly valuable during appeals. Modifiers provide additional information about performed services, and their correct application often determines whether claims receive payment or denial.
Benefits of Outsourcing Medical Billing in Florida
Healthcare practices face a critical decision: maintain in-house billing operations or partner with specialized medical billing services florida offers. This choice significantly impacts financial performance, operational efficiency, and compliance risk management.
Financial Performance Improvements
Outsourcing billing operations typically delivers measurable financial benefits within the first few months of implementation. Practices experience increased clean claim rates, with professional billing services achieving 95-98% accuracy compared to industry averages of 75-85% for in-house operations.
Revenue improvements stem from multiple sources:
- Faster claim submission reducing days in accounts receivable
- Higher first-pass acceptance rates minimizing denial-related delays
- Systematic follow-up on unpaid claims preventing write-offs
- Expert denial management recovering previously lost revenue
- Accurate coding maximizing appropriate reimbursement
The healthcare revenue cycle management industry has developed sophisticated methodologies for optimizing every revenue cycle component. Professional billing teams apply these best practices consistently, delivering results that individual practices struggle to achieve independently.
Operational Efficiency and Cost Savings
Maintaining in-house billing departments requires significant infrastructure investment. Practices must budget for competitive salaries, employee benefits, continuing education, billing software licensing, hardware and IT support, and office space and equipment.
Medical billing services florida practices partner with typically operate on a percentage-of-collections model, aligning incentives between provider and billing company. This arrangement transforms fixed overhead costs into variable expenses that scale with practice revenue.
| Cost Category | In-House Billing | Outsourced Billing |
|---|---|---|
| Staff Salaries | $35,000-$55,000 per FTE | Included in service fee |
| Benefits (30%) | $10,500-$16,500 per FTE | Not applicable |
| Software/Systems | $500-$2,000 monthly | Included in service fee |
| Training/Education | $1,000-$3,000 annually | Provider responsibility |
| Space/Equipment | $300-$800 monthly | Not required |
Beyond direct cost savings, outsourcing frees practice management and clinical staff to focus on core competencies. Physicians can dedicate attention to patient care rather than billing disputes, while administrative leaders concentrate on strategic initiatives like service line development or patient experience improvements.
Compliance and Risk Mitigation
The regulatory complexity surrounding medical billing creates substantial compliance risk for healthcare providers. Coding errors, documentation deficiencies, or billing irregularities can trigger audits, recoupment demands, or even fraud investigations.
Professional medical billing services florida providers trust maintain expertise in current compliance requirements. Their teams receive ongoing training in regulatory updates, coding changes, and payer policy modifications. This specialized knowledge helps practices avoid common compliance pitfalls.
The Healthcare Financial Management Association provides resources and education on compliance best practices, which leading billing services incorporate into their operational protocols. This commitment to compliance protects providers from financial and legal risks while ensuring ethical billing practices.
Selecting the Right Medical Billing Partner in Florida
Choosing medical billing services florida practices can trust requires careful evaluation of multiple factors. The right partnership delivers not just technical competence but also cultural alignment and communication transparency.
Key Evaluation Criteria
When assessing potential billing partners, practices should examine several critical areas. Experience with your specialty matters significantly, as billing requirements vary substantially between primary care, surgical specialties, behavioral health, and other practice types. A billing company experienced in your specialty understands typical procedures, common denial reasons, and specialty-specific coding nuances.
Technology infrastructure deserves close scrutiny. Quality billing services utilize robust practice management systems, maintain secure data transmission protocols, provide real-time reporting capabilities, integrate with existing EHR systems, and employ automated workflow tools for efficiency.
Transparency in communication and reporting separates exceptional billing partners from mediocre ones. Providers should expect regular performance reports, accessible account managers, prompt responses to inquiries, and clear explanations of billing metrics and trends.
Questions to Ask Prospective Billing Services
Due diligence requires asking direct questions about operations, performance, and service delivery. Consider these essential inquiries:
- What is your average first-pass acceptance rate for claims?
- How quickly do you submit clean claims after service delivery?
- What percentage of denied claims do you successfully appeal?
- How do you stay current with coding updates and regulatory changes?
- What reporting do you provide, and how frequently?
- How do you handle patient billing inquiries and payment posting?
- What are your contract terms, including termination provisions?
- Can you provide references from practices similar to ours?
Understanding contractual adjustment in medical billing helps practices evaluate how billing services manage write-offs and negotiate with payers. Experienced billing partners understand these adjustments and work to minimize their impact on practice revenue.
Implementation and Transition Process
Transitioning to new medical billing services florida practices select requires careful planning and execution. Successful implementations follow structured approaches that minimize disruption to revenue flow.
A typical implementation timeline spans 6-12 weeks and includes:
- Initial assessment and data gathering where the billing service reviews current operations, identifies improvement opportunities, and collects necessary practice information
- System configuration and integration involving software setup, clearinghouse connections, and EHR interface establishment
- Staff training on new workflows, communication protocols, and responsibilities that remain with practice personnel
- Parallel processing period where both old and new systems operate simultaneously to ensure continuity
- Full transition with ongoing monitoring and performance optimization
Practices should maintain realistic expectations during transitions. Initial months may show temporary disruptions as new processes stabilize, but well-managed implementations quickly demonstrate improvement in key performance indicators.
Technology and Innovation in Florida Medical Billing
The medical billing industry continues evolving through technological advancement and process innovation. Leading medical billing services florida providers employ leverage these developments to deliver superior results.
Automation and Artificial Intelligence
Modern billing operations increasingly incorporate automation tools that reduce manual tasks and improve accuracy. Automated eligibility verification, claim scrubbing algorithms, payment posting automation, denial pattern analysis, and patient communication systems all contribute to operational efficiency.
Artificial intelligence applications in medical billing continue expanding. Machine learning algorithms identify coding patterns, predict claim denial likelihood, optimize billing workflows, and detect potential compliance issues before submission.
These technologies don't replace human expertise but augment it. Experienced billing professionals apply clinical knowledge and critical thinking to complex situations while automation handles routine tasks with speed and consistency.
Data Analytics and Performance Monitoring
Sophisticated reporting capabilities transform billing data into actionable insights. Professional billing services provide practices with comprehensive analytics on key performance indicators, payer-specific trends, denial reasons and patterns, provider productivity metrics, and patient payment behavior.
Understanding what are adjustments on medical bills becomes clearer through detailed reporting. Analytics reveal how different adjustment categories affect net revenue, enabling practices to make informed decisions about payer contracts and service line profitability.
Dashboard metrics typically include:
- Days in accounts receivable
- Clean claim rate
- Net collection rate
- Denial rate by reason and payer
- Average reimbursement per procedure
- Patient responsibility collection percentage
Regular review of these metrics enables continuous improvement. Practices and their billing partners collaborate to address identified issues, capitalize on opportunities, and optimize overall revenue cycle performance.
Specialty-Specific Billing Considerations in Florida
Different medical specialties face unique billing challenges that require specialized expertise. Medical billing services florida practices select should demonstrate competency in relevant specialty areas.
Primary Care and Family Medicine
Primary care practices typically handle high patient volumes with diverse insurance coverage. Their billing challenges include complex coding for evaluation and management services, preventive care billing requirements, chronic care management documentation, and coordination of benefits for patients with multiple coverages.
Understanding annual wellness visit CPT code by age proves essential for primary care billing. These preventive services require specific coding based on whether visits represent initial or subsequent wellness exams, and proper billing ensures both patient and provider receive appropriate benefits.
Surgical Specialties
Surgical practices face billing complexity related to global surgical packages, modifier application for multiple procedures, assistant surgeon billing, and implant and supply documentation. Common errors with modifier 59 frequently affect surgical billing, as this modifier indicates distinct procedural services. Incorrect application triggers denials or potential compliance concerns.
Behavioral Health and Mental Health Services
Mental health providers navigate unique billing requirements including telehealth service coding, crisis intervention billing, group therapy documentation, and coordination with managed behavioral health organizations.
The American Academy of Professional Coders offers specialized training in behavioral health coding, recognizing the distinct knowledge requirements for accurate billing in this specialty. Professional billing services serving mental health providers should demonstrate this specialized expertise.
Future Trends in Florida Medical Billing
The medical billing landscape continues evolving in response to regulatory changes, technological advancement, and market pressures. Practices benefit from understanding emerging trends that will shape future operations.
Value-Based Care Impact
Healthcare payment models increasingly incorporate quality metrics and outcome measurements rather than simple fee-for-service structures. This shift affects billing practices through alternative payment model reporting, quality measure documentation requirements, risk adjustment coding accuracy, and bundled payment arrangements.
Medical billing services florida providers partner with must adapt to these evolving models. Expertise in value-based care billing becomes essential as more payer contracts incorporate quality incentives and shared savings arrangements.
Regulatory Environment Changes
Healthcare regulation remains dynamic, with frequent updates to coding systems, coverage policies, and compliance requirements. Professional billing services maintain awareness of regulatory developments and implement necessary changes promptly.
Recent regulatory focus areas include telehealth service expansion and billing rules, price transparency requirements, prior authorization reform initiatives, and documentation standards for specific service categories.
Patient Financial Responsibility
Growing patient cost-sharing through high-deductible health plans shifts more financial responsibility to patients themselves. This trend requires billing services to enhance patient communication capabilities, offer flexible payment arrangements, implement point-of-service collection strategies, and provide clear, understandable billing statements.
Successful practices recognize that patient collections require different approaches than insurance billing. Medical billing services florida practices trust increasingly incorporate patient-focused financial services alongside traditional insurance billing operations.
Measuring Success with Medical Billing Services
Establishing clear performance expectations and measurement criteria ensures billing partnerships deliver promised value. Practices should implement systematic monitoring of key performance indicators.
Critical Performance Metrics
Effective measurement focuses on metrics that directly impact practice financial health and operational efficiency. Essential KPIs include:
| Metric | Target Range | Significance |
|---|---|---|
| Days in A/R | 30-40 days | Cash flow and collection efficiency |
| Clean Claim Rate | 95-98% | Submission accuracy and denial prevention |
| Net Collection Rate | 95-99% | Overall revenue cycle effectiveness |
| Denial Rate | 5-10% | Claim quality and payer relationship health |
| Cost to Collect | 3-7% of collections | Operational efficiency |
Regular monitoring of these metrics enables early identification of issues and opportunities. Practices should receive monthly reports detailing performance against established targets, along with explanatory analysis for any significant variances.
Continuous Improvement Processes
Superior billing partnerships incorporate ongoing optimization rather than static service delivery. This approach includes regular performance reviews, process refinement based on data analysis, proactive identification of revenue opportunities, and collaborative problem-solving between practice and billing service.
How denial management in medical billing improves cash flow demonstrates the importance of systematic approaches to common challenges. Rather than accepting denials as inevitable, professional billing services analyze patterns, address root causes, and implement preventive measures that reduce future occurrences.
Return on Investment Calculation
Evaluating billing service ROI requires comparing total costs against measurable financial improvements. Practices should consider revenue increase from improved collections, cost savings from eliminated in-house operations, time savings for clinical and administrative staff, reduced compliance risk, and faster cash conversion cycles.
Most practices implementing professional medical billing services florida offers experience positive ROI within 3-6 months. The combination of increased collections and reduced operational costs typically outweighs service fees, while additional benefits like improved compliance and staff satisfaction provide value beyond simple financial calculations.
Common Pitfalls to Avoid
Even with professional billing support, practices can undermine their own success through common mistakes. Awareness of these pitfalls enables proactive prevention.
Documentation Deficiencies
Inadequate clinical documentation remains the leading cause of denied claims and compliance risk. Billing services can only code and bill based on documented services. Practices must ensure complete encounter documentation, specific diagnosis coding support, medical necessity justification, and procedure details supporting billed codes.
Understanding different types of medical coding helps providers recognize what documentation coders need. ICD-10 diagnostic coding, CPT procedural coding, and HCPCS supply coding each require specific documentation elements.
Communication Gaps
Successful billing partnerships require ongoing communication between practice and billing service. Common communication failures include delayed notification of insurance changes, failure to forward payer correspondence, incomplete information about denied claims, and lack of coordination on patient billing issues.
Establishing clear communication protocols prevents these problems. Practices should designate specific contacts for billing service communication, schedule regular meetings to review performance and issues, create systems for forwarding relevant information promptly, and maintain documentation of billing-related decisions and communications.
Unrealistic Expectations
While professional billing services deliver substantial improvements, practices sometimes maintain unrealistic expectations. Understanding industry norms helps set appropriate goals. No billing service achieves 100% collection of billed charges due to contractual adjustments, patient bad debt, and legitimate denials. Similarly, some claim denials are inevitable regardless of submission quality, and payment timing depends partly on payer processing speeds beyond billing service control.
Experienced medical billing services florida practices work with set realistic targets based on specialty, payer mix, and practice characteristics. They provide transparent reporting that distinguishes between controllable factors and external variables affecting revenue cycle performance.
Florida healthcare providers face complex billing challenges that require specialized expertise, sophisticated technology, and dedicated focus. Professional medical billing services deliver measurable improvements in revenue cycle performance while allowing practices to concentrate on patient care and strategic growth. By selecting experienced partners who understand Florida's unique regulatory environment and payer landscape, practices position themselves for financial stability and operational excellence. Greenhive Billing Solutions provides comprehensive revenue cycle management services designed specifically for healthcare providers seeking to optimize their billing operations, improve collections, and maintain compliance across all aspects of the revenue cycle.