Managing the financial health of a healthcare practice requires meticulous attention to services billing processes. Whether operating a small clinic or a multi-specialty medical group, the way you handle billing for the professional services you provide directly impacts cash flow, operational efficiency, and long-term sustainability. Healthcare providers face unique challenges in services billing, from navigating complex payer requirements to ensuring accurate documentation and coding. Understanding best practices in this critical area can mean the difference between a thriving practice and one struggling with denied claims and revenue shortfalls.
Understanding Services Billing in Healthcare Revenue Cycle Management
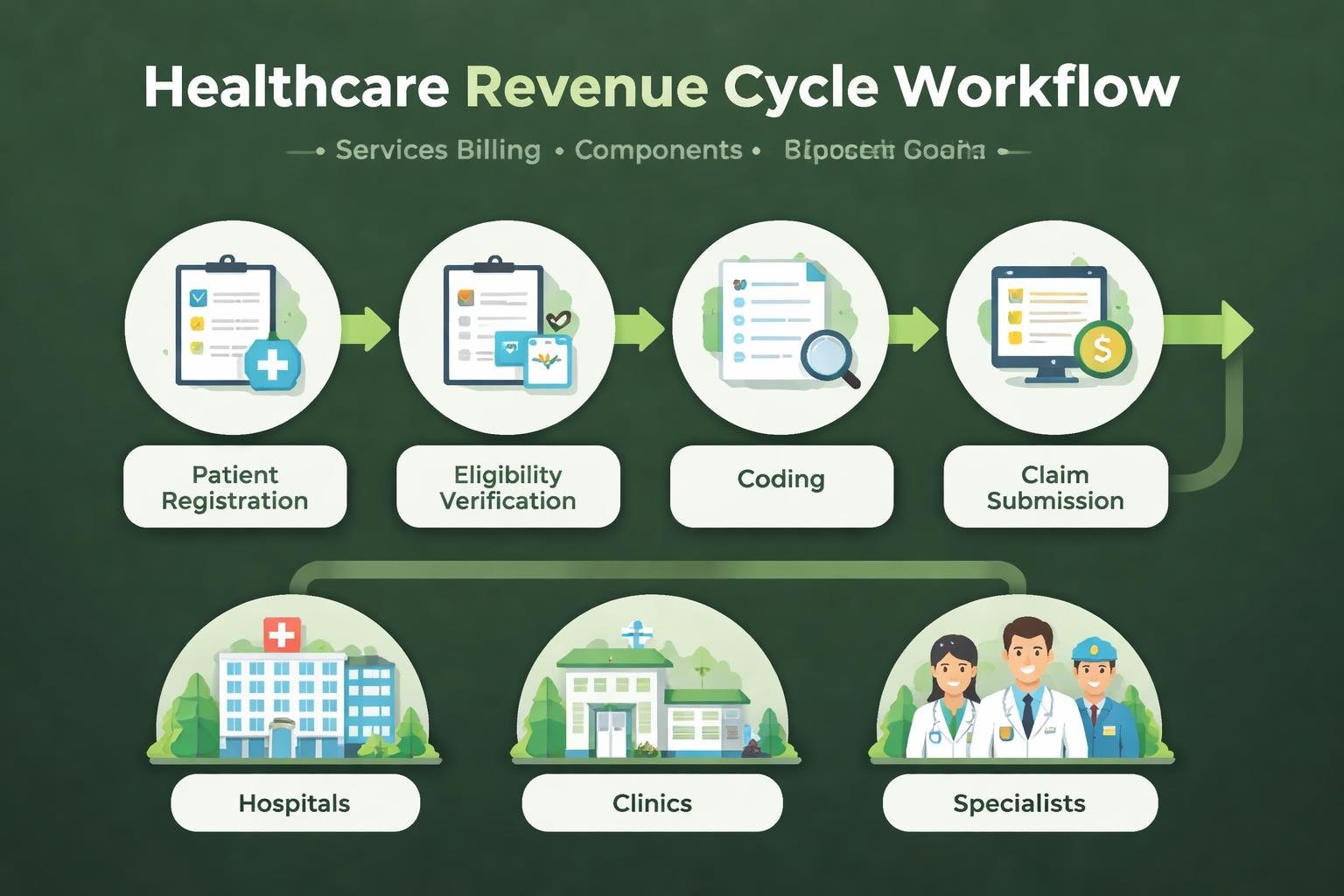
Services billing refers to the systematic process of invoicing and collecting payment for healthcare services rendered to patients. This encompasses every step from patient registration and insurance verification through claim submission, payment posting, and follow-up on outstanding balances. Unlike product-based billing, services billing requires capturing intangible care delivery through proper documentation, accurate coding, and compliant claim formatting.
Healthcare providers must navigate multiple payer types, each with distinct requirements. Medicare, Medicaid, and commercial insurers all maintain separate billing guidelines, coverage policies, and reimbursement methodologies. The Centers for Medicare & Medicaid Services provides comprehensive billing best practices that healthcare organizations should review regularly to maintain compliance.
The complexity of services billing stems from several factors:
- Variable service descriptions requiring precise CPT and HCPCS coding
- Modifier usage to communicate specific service circumstances
- Place of service indicators that affect reimbursement rates
- Medical necessity documentation requirements
- Coordination of benefits for patients with multiple insurance policies
Professional billing differs fundamentally from facility billing, though many practices handle both. Professional services billing focuses on physician work, while facility billing covers technical components and resource utilization. Understanding this distinction helps practices optimize their revenue capture strategies.
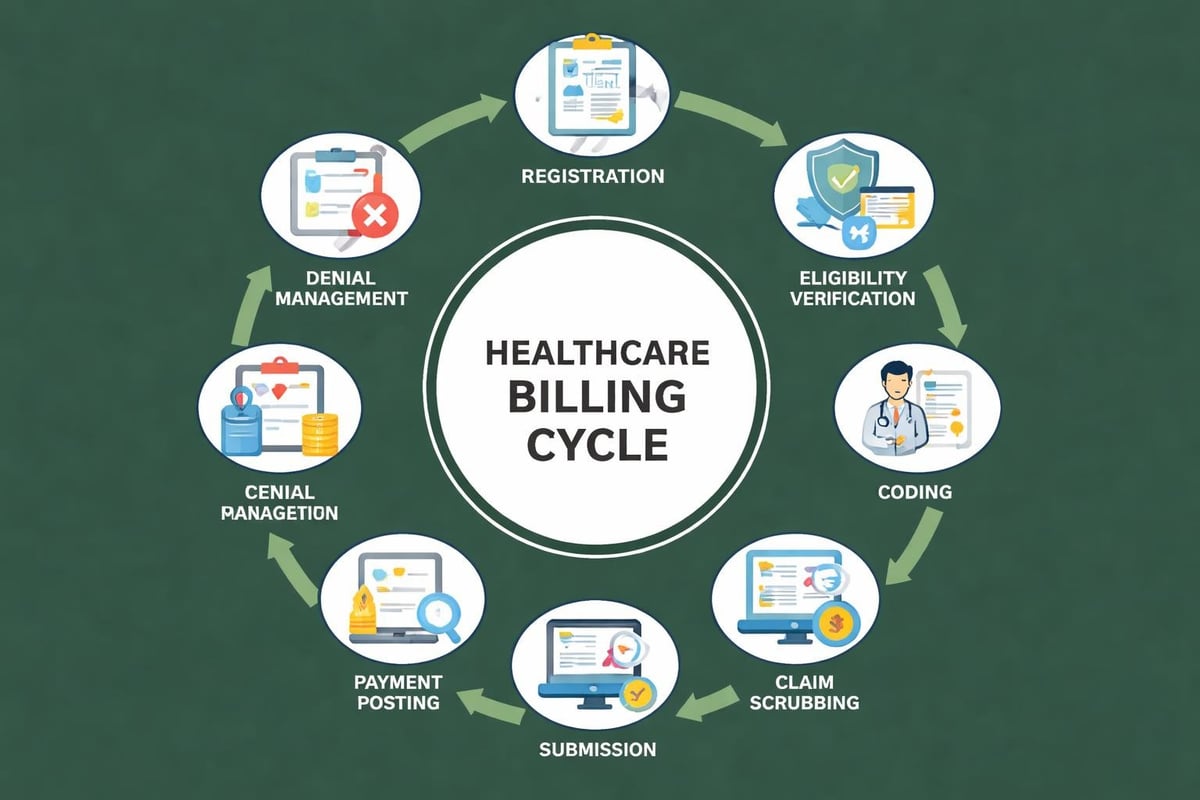
Essential Components of Effective Services Billing
Accurate Patient Registration and Demographics
The foundation of successful services billing begins at patient registration. Demographic accuracy directly correlates with claim acceptance rates. A single transposed digit in a member ID or an outdated address can result in claim denials that delay payment by weeks or months.
Front-office staff should verify the following information at every patient encounter:
- Full legal name exactly as it appears on the insurance card
- Date of birth to ensure correct patient identification
- Current contact information including phone number and address
- Insurance policy details including group number and effective dates
- Guarantor information for billing coordination
Many practices implement dual-entry systems where staff compare the insurance card to what's entered in the practice management system. This simple verification step can reduce demographic-related denials by 40-60%. Eligibility verification services form a critical component of this initial stage, confirming active coverage before services are rendered.
Comprehensive Documentation Standards
Clinical documentation serves as the legal record of care and the justification for services billed. Without thorough documentation, even correctly coded claims may face denials for lack of medical necessity. Providers should document the chief complaint, history of present illness, review of systems, examination findings, medical decision-making, and treatment plan for each encounter.
Documentation must support the level of service billed. For evaluation and management services, this means aligning documentation with the specific requirements for each CPT code level. The medical record should tell a clear story of why the patient needed care, what was done, and what the provider decided.
| Documentation Element | Billing Impact | Common Pitfall |
|---|---|---|
| Chief Complaint | Establishes medical necessity | Too vague or generic |
| History | Supports E&M level | Incomplete system reviews |
| Examination | Justifies service complexity | Copy-paste errors |
| Medical Decision Making | Determines code selection | Insufficient detail on risk |
| Treatment Plan | Shows medical necessity | Not documented at all |
Precise Medical Coding Practices
Accurate coding translates clinical documentation into standardized billing language. Professional medical coders must stay current with annual CPT updates, ICD-10-CM revisions, and payer-specific coding guidelines. The coding process requires matching diagnosis codes that demonstrate medical necessity for each procedure or service code submitted.
Diagnosis coding has become increasingly specific under ICD-10-CM, with many codes requiring laterality, encounter type, and other details. Submitting a non-specific code when a more specific option exists often triggers automated denials. Similarly, procedure coding demands attention to bundling rules, modifier requirements, and service-specific documentation needs.
Understanding different types of medical coding helps practices assign the right expertise to various coding tasks. Specialty-specific coding knowledge becomes particularly valuable for practices in fields like cardiology, orthopedics, or behavioral health where code selection complexity increases.
Services Billing Best Practices for Revenue Optimization
Front-End Revenue Cycle Excellence
Preventing claim denials starts before the claim is ever submitted. Pre-service processes including insurance verification, benefit confirmation, and prior authorization management significantly impact clean claim rates. Practices that invest in robust front-end processes typically see 15-25% improvements in first-pass claim acceptance.
Real-time eligibility verification confirms active coverage and identifies potential issues like inactive policies, termed coverage, or incorrect subscriber information. This verification should occur 24-48 hours before scheduled appointments, giving staff time to contact patients about coverage issues or collect deposits for non-covered services.
Prior authorization services help practices navigate the increasingly complex requirement landscape. Many procedures now require pre-approval, and failure to obtain authorization often results in complete claim denials with no appeal rights. Tracking authorization requirements by payer and procedure ensures nothing falls through the cracks.
Claim Submission and Scrubbing Protocols
Before claims reach payers, they should undergo comprehensive scrubbing to identify and correct errors. Automated claim scrubbing systems check hundreds of edits including:
- Valid code combinations
- Age and gender conflicts
- Missing modifiers
- Bundling violations
- Place of service inconsistencies
Clean claim rates above 95% are achievable with proper scrubbing processes. Each percentage point improvement in clean claim rates translates directly to faster payment and reduced administrative costs. Industry research from medical billing best practices guides emphasizes the importance of technology in achieving these benchmarks.
Electronic claim submission through clearinghouses provides real-time feedback on claim acceptance. Clearinghouse edits catch many errors before claims reach payers, allowing immediate correction and resubmission. This technology layer has become essential for efficient services billing operations.
Payment Posting and Reconciliation
Accurate payment posting ensures the practice accounting system reflects true accounts receivable status. Payment posting involves recording payer payments, patient payments, contractual adjustments, and other account activity. Consistency in posting methodology prevents reporting errors and enables meaningful financial analysis.
Staff should post payments to the specific service line level rather than globally to the encounter. This granular posting approach enables tracking of payment patterns by CPT code, helping identify underpayments or systematic payer errors. Payment posting services require trained personnel who understand EOB interpretation and adjustment coding.
Reconciliation compares expected reimbursement against actual payment received. Significant variances warrant investigation to determine if the payer calculated payment correctly according to the contract. Many practices leave money on the table by failing to audit payments for accuracy.
Managing Denials and Appeals in Services Billing
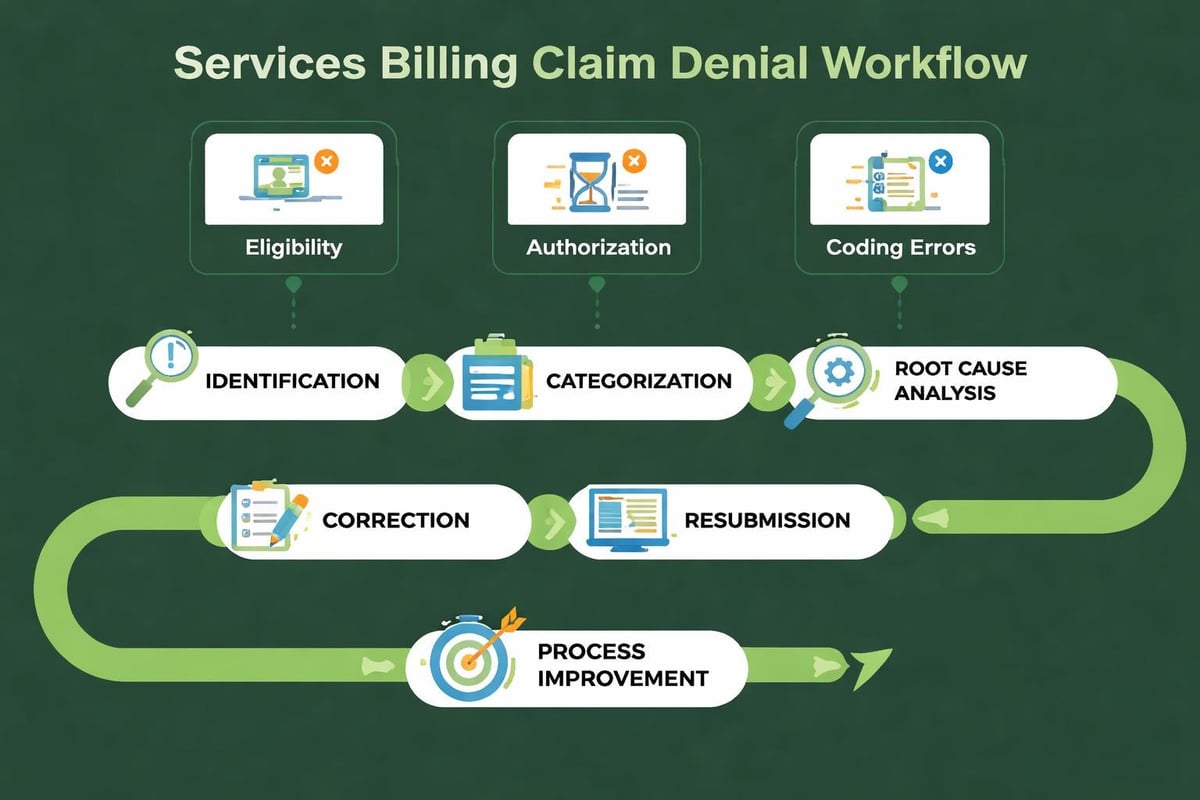
Denial Analysis and Prevention
Denial management represents one of the most critical aspects of services billing. Systematic denial tracking reveals patterns that inform process improvements. Practices should categorize denials by reason code, payer, provider, and service type to identify improvement opportunities.
Common denial categories include:
- Registration errors: Incorrect demographic information or insurance details
- Eligibility issues: Inactive coverage or termed policies
- Authorization problems: Missing or expired authorizations
- Coding errors: Invalid codes, bundling issues, or medical necessity gaps
- Timely filing: Claims submitted after payer deadlines
The most effective denial prevention strategy involves addressing root causes rather than just working individual denials. If authorization-related denials spike, the solution lies in improving front-end authorization processes, not just appealing denied claims. Denial management services focus on both claim-level resolution and systemic process improvement.
Strategic Appeals Management
Not all denials warrant appeal efforts. Practices must evaluate the cost of appeal work against the potential recovery amount. Appeals prioritization considers claim value, probability of overturn, and appeal complexity. High-dollar claims with clear documentation supporting coverage typically receive immediate appeal attention.
Effective appeals require understanding payer-specific appeal procedures, documentation requirements, and deadlines. Each payer maintains distinct appeal processes with specific forms, submission methods, and timeframes. Missing an appeal deadline typically results in permanent claim denial with no further recourse.
The appeal letter should clearly state why the denial was incorrect, cite specific policy language supporting coverage, and include relevant clinical documentation. Generic appeal templates rarely succeed. Successful appeals demonstrate thorough understanding of both clinical care and coverage policies.
Technology and Services Billing Efficiency
Practice Management and Billing Systems
Modern revenue cycle management depends on integrated technology platforms that support services billing workflows. Practice management systems coordinate scheduling, registration, charge capture, and billing functions. Integration between clinical and billing systems reduces manual data entry and associated errors.
Key technology features that support effective services billing include:
- Real-time eligibility verification integration
- Automated coding assistance and compliance checking
- Built-in claims scrubbing with payer-specific edits
- Electronic remittance advice processing
- Comprehensive reporting and analytics dashboards
While many providers rely on medical billing software owned by their practices, others partner with revenue cycle management companies that bring expertise in multiple platforms. The ability to work with existing client systems while providing expert guidance offers flexibility for practices at different technology maturity levels.
Reporting and Analytics for Continuous Improvement
Data-driven decision making separates high-performing revenue cycle operations from those struggling with inefficiency. Key performance indicators (KPIs) for services billing provide objective measures of operational health and highlight areas needing attention.
| KPI | Target Benchmark | What It Measures |
|---|---|---|
| Clean Claim Rate | >95% | Claims accepted without errors |
| Days in A/R | <30 days | Speed of payment collection |
| Collection Rate | >95% | Percentage of expected revenue collected |
| Denial Rate | <5% | Claims initially denied by payers |
| Cost to Collect | <3% of collections | Efficiency of billing operations |
Regular monitoring of these metrics enables proactive management. Trending reports show whether performance improves or deteriorates over time. Healthcare revenue cycle analytics transform raw data into actionable insights that drive process improvements.

Compliance Considerations in Services Billing
Regulatory Requirements and Billing Compliance
Healthcare services billing operates within a complex regulatory environment. HIPAA compliance governs patient information handling in all billing communications and processes. Practices must implement appropriate safeguards to protect patient data throughout the revenue cycle.
Beyond HIPAA, various state regulations affect billing operations. For example, New York regulations establish specific requirements for billing services and service bureaus. Healthcare organizations must understand applicable state laws in jurisdictions where they operate or where their billing partners are located.
Billing compliance programs should address:
- False Claims Act awareness and prevention
- Stark Law and Anti-Kickback Statute considerations
- Proper documentation supporting billed services
- Accurate coding without upcoding or unbundling
- Appropriate use of modifiers to communicate service circumstances
Regular compliance audits help identify potential issues before they become regulatory problems. Internal auditing programs demonstrate good faith compliance efforts and provide opportunities for staff education and process correction.
Fraud Prevention and Detection
While most billing errors stem from honest mistakes, practices must guard against intentional fraud. Billing compliance monitoring includes oversight of unusual billing patterns, outlier providers, and high-risk service combinations. Automated fraud detection systems flag anomalies for human review.
Common fraud red flags include consistent billing of the highest-level evaluation codes, excessive use of certain modifiers, or billing patterns that deviate significantly from peer benchmarks. Investigating these patterns often reveals training needs, documentation gaps, or occasionally, intentional overbilling requiring immediate correction.
Organizations providing billing services must maintain strict separation between coding decisions and financial incentives. Best practices from comprehensive billing and collections guides emphasize the importance of quality controls and independent oversight in preventing compliance issues.
Optimizing Services Billing Through Specialization
Specialty-Specific Billing Expertise
Different medical specialties face unique services billing challenges. Cardiology practices navigate complex procedure bundling rules and modifier requirements. Behavioral health providers manage session-based billing with authorization limitations. Surgical specialties coordinate professional and facility billing with specific global period considerations.
Specialty expertise in services billing delivers tangible value through higher collection rates and fewer denials. Billers who understand specialty-specific documentation requirements, common procedures, and payer policies identify and prevent issues that generalist billers might miss. This specialized knowledge becomes particularly valuable for practices in high-complexity specialties.
Resources like medical billing for behavioral health demonstrate how specialty-focused approaches address unique challenges. Behavioral health billing requires understanding of session timing rules, split billing scenarios, and specialty-specific authorization requirements that differ substantially from other medical specialties.
Small Practice Considerations
Small and independent practices face particular challenges in maintaining efficient services billing operations. Resource constraints limit the ability to employ multiple specialized billing staff or invest in expensive technology platforms. However, small practices can achieve excellent billing performance through focused attention to core processes.
Strategies for small practice billing success include:
- Standardizing encounter documentation templates
- Establishing clear charge capture procedures
- Implementing daily claims submission routines
- Conducting weekly accounts receivable reviews
- Partnering with experienced billing professionals
Many small practices find that specialized billing services for small practices provide access to expertise and technology that would be cost-prohibitive to develop internally. This partnership model allows practices to maintain clinical focus while ensuring revenue cycle excellence.
Building a Culture of Billing Excellence
Staff Training and Development
Effective services billing requires knowledgeable, engaged staff committed to continuous improvement. Ongoing training ensures team members stay current with changing regulations, payer policies, and coding updates. Annual CPT and ICD-10 updates alone require significant educational investment.
Training programs should address both technical skills and soft skills. Billers need coding accuracy and systems proficiency, but they also benefit from customer service training for patient interactions and problem-solving skills for denial resolution. Cross-training team members on multiple functions builds operational resilience and provides career development opportunities.
Certification programs through organizations like AAPC and AHIMA provide structured learning paths and credential verification. Billing and coding specialists with professional certifications typically demonstrate higher accuracy and productivity than uncertified staff.
Communication and Transparency
Open communication between clinical and billing teams prevents many common services billing problems. Regular meetings between providers and billing staff create opportunities to discuss documentation issues, coding questions, and payer feedback. This collaboration improves both clinical documentation and billing accuracy.
Patient communication about billing matters requires particular attention to clarity and compassion. Transparent discussions about costs, insurance coverage, and payment expectations before service delivery prevent surprises and improve collection rates. Training front-desk staff in these conversations builds patient trust while protecting practice revenue.
Payer communication skills also impact billing success. Effective appeals, authorization requests, and payment dispute resolution require clear, professional correspondence that addresses specific payer concerns with supporting documentation and policy citations.
Mastering services billing best practices enables healthcare providers to maximize revenue while maintaining compliance and delivering excellent patient care. By focusing on accurate data capture, comprehensive documentation, precise coding, and proactive denial management, practices position themselves for financial success in an increasingly complex healthcare environment. Greenhive Billing Solutions partners with healthcare providers across the United States to implement these best practices through comprehensive revenue cycle management services. Our experienced team handles eligibility verification, claims processing, denial management, and all aspects of the billing cycle, allowing providers to focus on patient care while we optimize their financial performance.