Electronic Data Interchange has fundamentally transformed how healthcare organizations manage their revenue cycle operations. As healthcare providers face increasing pressure to reduce administrative costs while maintaining accuracy, edi in medical billing has emerged as a critical technology that enables faster claims processing, fewer errors, and improved cash flow. This standardized approach to exchanging healthcare information electronically between providers, payers, and clearinghouses has become the backbone of modern medical billing operations, replacing paper-based processes with efficient digital workflows that benefit all stakeholders in the healthcare ecosystem.
Understanding Electronic Data Interchange in Healthcare
EDI in medical billing refers to the computer-to-computer exchange of healthcare information using standardized formats. This technology allows healthcare providers to submit claims, verify patient eligibility, receive remittance advice, and process authorizations without manual paper handling.
The CMS electronic billing and EDI transactions framework establishes the foundation for these exchanges, ensuring consistency across the healthcare industry. When properly implemented, EDI reduces the time between service delivery and payment while minimizing the errors that commonly occur with manual data entry.
The Technical Foundation of Medical EDI
Electronic data interchange operates through HIPAA-mandated transaction sets that define specific formats for different types of healthcare communications. These standardized formats ensure that information sent from one system can be accurately interpreted by another, regardless of the software platforms involved.
The X12 format serves as the standard language for EDI transactions in healthcare. Each transaction type has a specific number designation that identifies its purpose and required data elements.
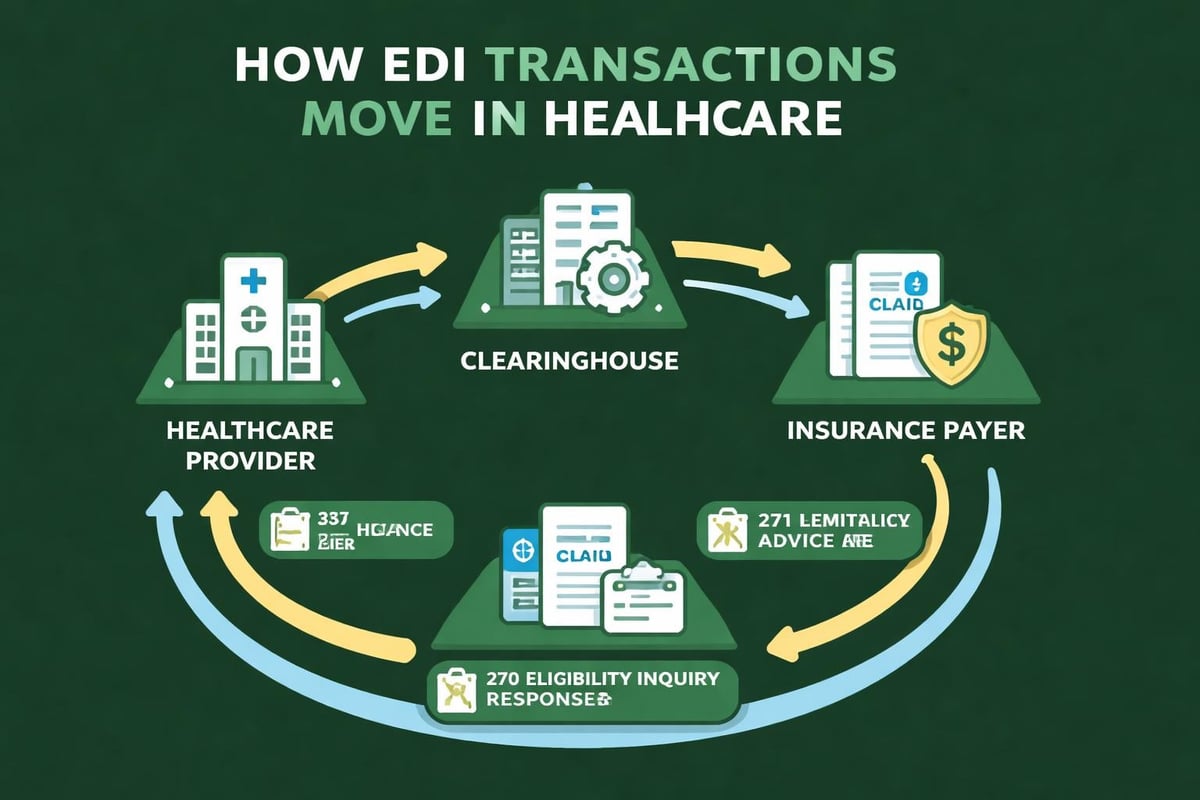
Primary EDI Transaction Types in Medical Billing
Healthcare organizations rely on several core EDI transaction types to manage their revenue cycle operations. Understanding these transactions helps practices optimize their billing workflows and reduce processing delays.
| Transaction Code | Transaction Name | Primary Purpose | Direction |
|---|---|---|---|
| 837 | Healthcare Claim | Submit professional, institutional, or dental claims | Provider to Payer |
| 835 | Electronic Remittance Advice | Receive payment information and claim adjustments | Payer to Provider |
| 270 | Eligibility Inquiry | Request patient insurance coverage details | Provider to Payer |
| 271 | Eligibility Response | Receive coverage and benefit information | Payer to Provider |
| 276 | Claim Status Request | Check on claim processing status | Provider to Payer |
| 277 | Claim Status Response | Receive claim status updates | Payer to Provider |
| 278 | Authorization Request/Response | Submit and receive prior authorization decisions | Bidirectional |
The 837 Healthcare Claim Transaction
The 837 transaction represents the electronic equivalent of paper claim forms such as the CMS-1500 or UB-04. This transaction contains all necessary information about the patient, provider, services rendered, diagnosis codes, and billing details.
Professional claims (837P) are used by physicians and other non-institutional providers. Institutional claims (837I) are submitted by hospitals and facilities. Dental claims (837D) handle dental services specifically.
Each 837 transaction undergoes validation checks at multiple points to ensure data completeness and accuracy before reaching the payer.
Electronic Remittance Advice and Payment Posting
The 835 transaction delivers detailed payment information from payers to providers. This Electronic Remittance Advice includes payment amounts, adjustment reasons, patient responsibility, and claim-level details that enable accurate payment posting.
Modern practice management systems can automatically post 835 transactions, significantly reducing the time staff spend manually entering payment information. This automation improves accuracy and allows billing teams to focus on denial management and patient inquiries.
Benefits of Implementing EDI in Medical Billing
Healthcare providers who transition to electronic data interchange experience measurable improvements across their revenue cycle operations. These benefits extend beyond simple cost savings to include enhanced accuracy, faster processing, and better compliance.
Speed and Efficiency Gains
Claims processing time drops dramatically when practices use edi in medical billing. While paper claims may take 30-45 days to process, electronic claims typically clear within 10-14 days.
Real-time eligibility verification allows front desk staff to confirm coverage before patients receive services. This immediate feedback prevents scheduling patients with inactive coverage and reduces claim denials related to eligibility issues.
Authorization requests processed electronically receive responses in hours rather than days, enabling providers to schedule procedures more quickly and improve patient satisfaction.
Error Reduction and Clean Claim Rates
EDI systems perform automated validation checks that identify errors before claims reach payers. These front-end edits catch missing information, invalid codes, and formatting issues that would trigger rejections.
- Format validation ensures all required data fields contain information
- Code validity checks confirm that diagnosis and procedure codes are current and properly formatted
- Demographic verification flags inconsistencies in patient information
- Payer-specific rules apply individual insurance company requirements
Practices implementing comprehensive EDI workflows often see their clean claim rates improve from 75-80% to over 95%, directly impacting cash flow and reducing rework.
Cost Reduction Across Operations
Electronic data interchange eliminates expenses associated with paper-based billing processes. Healthcare providers save on printing, postage, storage, and the staff time required to prepare and mail claims.
Average cost per paper claim: $2.50-$4.00
Average cost per electronic claim: $0.25-$0.75
For a practice submitting 1,000 claims monthly, this difference represents annual savings of $27,000-$39,000. These resources can be redirected toward patient care or practice growth initiatives.
Security and Compliance Considerations
The intersection of EDI healthcare transactions and HIPAA compliance creates specific security requirements that healthcare organizations must address. Protected health information transmitted electronically requires robust safeguards to prevent unauthorized access.
HIPAA Security Standards for EDI
Healthcare providers must implement both technical and administrative safeguards when using edi in medical billing. Encryption protects data during transmission, while access controls limit who can view or modify patient information.
The CMS guidelines on EDI access and privacy outline specific requirements for maintaining data security throughout the billing process.
Key security measures include:
- End-to-end encryption for all transmitted data
- User authentication with unique credentials for each system user
- Audit trails documenting all access to patient information
- Regular security assessments identifying potential vulnerabilities
- Business associate agreements with all trading partners
Trading Partner Agreements
Before exchanging EDI transactions, healthcare providers must establish trading partner agreements with clearinghouses and payers. These agreements specify technical requirements, data formats, connectivity methods, and compliance obligations.
Trading partner agreements define response times, error handling procedures, and support processes that ensure smooth operations. They also establish liability provisions and outline steps for resolving disputes.
Implementation Strategies for Healthcare Providers
Successfully deploying edi in medical billing requires careful planning and a structured approach. Healthcare organizations should assess their current workflows, select appropriate technology partners, and train staff on new processes.
Selecting Clearinghouses and Trading Partners
Clearinghouses serve as intermediaries between providers and payers, translating data formats and routing transactions to the correct destinations. When evaluating clearinghouses, practices should consider several factors:
| Evaluation Criteria | Why It Matters | Questions to Ask |
|---|---|---|
| Payer Connectivity | Direct connections reduce processing time | How many payers do you connect with directly? |
| Real-time Validation | Identifies errors before submission | What front-end edits do you perform? |
| Reporting Capabilities | Enables performance monitoring | What reporting tools are available? |
| Support Services | Resolves issues quickly | What are your support hours and response times? |
| Pricing Structure | Impacts overall costs | Are there setup fees, monthly minimums, or per-transaction charges? |
Many top medical billing companies maintain established relationships with multiple clearinghouses, allowing them to leverage optimal connections for different payer types.
Technology Integration Requirements
Practice management systems must support EDI functionality either natively or through integration with third-party solutions. The software should generate properly formatted 837 transactions, process incoming 835 remittance files, and handle eligibility verification seamlessly.
Essential integration capabilities:
- Automatic claim scrubbing before submission
- Batch and real-time transmission options
- Electronic remittance advice auto-posting
- Denial tracking and reporting
- Eligibility verification at scheduling and check-in
Healthcare providers working with revenue cycle management partners benefit from teams experienced in configuring these integrations across various software platforms.

Common Challenges and Solutions
While edi in medical billing offers significant advantages, healthcare providers may encounter obstacles during implementation and ongoing operations. Understanding these challenges helps organizations prepare appropriate responses.
Managing Payer-Specific Requirements
Despite standardization efforts, individual insurance companies often impose unique requirements beyond basic X12 format specifications. These payer-specific rules can complicate claim submission and increase rejection rates.
Effective approaches include:
- Maintaining updated payer requirement documentation
- Implementing clearinghouse solutions with payer-specific edits
- Establishing direct communication channels with payer EDI support teams
- Monitoring rejection patterns to identify recurring issues
- Conducting regular training on payer requirement changes
Understanding denial management in medical billing becomes crucial when navigating these payer variations, as systematic tracking helps identify patterns requiring process adjustments.
Staff Training and Change Management
Transitioning from paper-based processes to electronic data interchange requires staff to develop new skills and adapt to different workflows. Resistance to change can undermine implementation efforts if not addressed proactively.
Successful practices invest in comprehensive training programs that explain not just how to use new systems, but why these changes benefit both the organization and patients. Hands-on practice in test environments allows staff to build confidence before processing live transactions.
System Reliability and Backup Procedures
Healthcare providers depend on EDI systems for daily operations, making system downtime particularly disruptive. Technical issues, clearinghouse outages, or connectivity problems can halt claim submissions and eligibility verifications.
Organizations should establish backup procedures that enable operations to continue during system unavailability. This might include secondary clearinghouse connections, manual submission capabilities for urgent claims, or redundant internet connections.
Optimizing EDI Performance for Better Outcomes
After implementing edi in medical billing, healthcare providers should continuously monitor performance metrics and refine processes to maximize benefits. Regular analysis identifies improvement opportunities and ensures the technology delivers expected returns.
Key Performance Indicators to Monitor
Submission metrics track how effectively the organization uses EDI capabilities. Days in accounts receivable, clean claim rate, and average time to submission reveal workflow efficiency.
Response metrics measure payer performance and identify processing bottlenecks. Claim acknowledgment time, initial payment rate, and denial percentage by payer highlight areas requiring attention.
Financial metrics demonstrate the business impact of EDI operations. Collection rate, cost per claim, and staff productivity measurements quantify return on investment.
| Metric Category | Specific Measures | Target Benchmarks |
|---|---|---|
| Submission Quality | Clean claim rate | >95% |
| Processing Speed | Days to first submission | <2 days |
| Payer Response | Initial acceptance rate | >90% |
| Financial Impact | Days in A/R | <30 days |
| Operational Efficiency | Claims per FTE | 3,000-5,000 monthly |
Organizations leveraging healthcare revenue cycle analytics can identify trends and opportunities that manual monitoring might miss.
Continuous Process Improvement
High-performing practices treat EDI operations as ongoing initiatives rather than one-time implementations. Regular process reviews identify inefficiencies, while staff feedback reveals practical challenges that metrics might not capture.
Monthly review activities should include:
- Analyzing rejection reports to identify recurring errors
- Reviewing payer policy updates that affect claim submission
- Assessing clearinghouse performance against service level agreements
- Evaluating staff productivity and training needs
- Benchmarking performance against industry standards
The revenue cycle process in healthcare benefits from this iterative approach, as improvements in EDI operations positively impact downstream activities like payment posting and denial management.
The Role of Professional RCM Partners
Many healthcare providers choose to work with experienced revenue cycle management companies rather than managing EDI operations internally. These partnerships allow practices to access specialized expertise while focusing internal resources on patient care.
Advantages of RCM Partnership for EDI Operations
Professional billing companies maintain dedicated teams with deep knowledge of EDI standards, payer requirements, and industry best practices. They invest in robust technology infrastructure and maintain relationships with multiple clearinghouses and payers.
Benefits include:
- Reduced staffing costs and training requirements
- Access to advanced technology without capital investment
- Expertise in handling complex payer requirements
- Scalability to accommodate practice growth
- Focus on core clinical operations
RCM partners bring standardized processes refined across multiple client implementations. This experience helps avoid common pitfalls and accelerate time to optimal performance.
What to Expect from RCM EDI Services
Quality revenue cycle management providers handle the complete EDI workflow from claim generation through payment posting. They configure integrations with existing practice management systems, establish clearinghouse connections, and manage trading partner relationships.
Services typically encompass eligibility verification at scheduling, real-time claim scrubbing, electronic submission, claim status monitoring, electronic remittance processing, and denial management. Transparent reporting provides visibility into operations without requiring day-to-day involvement.
Future Developments in Medical Billing EDI
Electronic data interchange in healthcare continues evolving as technology advances and industry needs change. Healthcare providers should stay informed about emerging trends that may impact their operations and create new opportunities for efficiency gains.
FHIR and Modern Data Exchange Standards
Fast Healthcare Interoperability Resources represents a newer approach to health information exchange designed for modern web-based applications. While traditional EDI remains the standard for billing transactions, FHIR enables more flexible data sharing for other purposes.
The relationship between FHIR and established EDI standards will likely evolve, potentially creating hybrid approaches that combine the reliability of X12 transactions with the flexibility of API-based exchanges.
Artificial Intelligence and Automation
Artificial intelligence applications increasingly support EDI operations through predictive analytics, intelligent claim routing, and automated denial management. Machine learning algorithms identify patterns in rejection data, suggesting process improvements and preventing recurring errors.
These technologies enhance rather than replace edi in medical billing, adding intelligence layers that optimize existing workflows. Healthcare providers can expect continued advancement in AI capabilities that reduce manual intervention requirements.
Regulatory Changes and Industry Initiatives
Healthcare regulations continuously evolve, sometimes creating new EDI transaction requirements or modifying existing standards. The industry periodically updates X12 transaction sets to accommodate new data elements or improve existing processes.
Organizations must monitor regulatory developments and work with clearinghouses or RCM partners who track these changes and implement necessary updates proactively. The EDI support resources from CMS provide valuable information about upcoming changes affecting Medicare billing.
Strategic Considerations for Different Practice Types
The approach to implementing and managing edi in medical billing varies based on practice size, specialty, and organizational structure. Tailoring strategies to specific circumstances improves outcomes and maximizes return on investment.
Small to Mid-Size Practices
Smaller healthcare providers often lack dedicated billing staff with deep EDI expertise. These organizations typically benefit most from partnering with experienced RCM companies that provide comprehensive support without requiring internal infrastructure investment.
For practices evaluating options, understanding medical billing costs helps determine whether outsourcing or internal management delivers better value. The decision should factor in technology expenses, staffing requirements, and the opportunity cost of diverting clinical resources to billing operations.
Large Healthcare Organizations
Larger practices and healthcare systems may maintain internal billing departments but still rely on specialized technology vendors for EDI connectivity and processing. These organizations often implement sophisticated practice management systems with native EDI capabilities.
Internal teams should focus on process optimization, payer relationship management, and performance monitoring while leveraging external partners for technical infrastructure and specialized expertise in areas like behavioral health billing or other specialty-specific requirements.
Specialty-Specific Considerations
Different medical specialties encounter unique EDI challenges based on their claim characteristics and primary payer mix. Surgical specialties deal with complex authorization requirements, while primary care practices focus on high-volume claim processing efficiency.
Understanding specialty-specific nuances helps practices configure EDI workflows appropriately. For example, urgent care revenue cycle management requires different approaches than traditional office-based practices due to varying patient volumes, payer mixes, and service types.
Electronic data interchange has become indispensable for healthcare providers seeking to optimize their revenue cycle performance through faster processing, reduced errors, and improved cash flow. By understanding EDI fundamentals, implementing appropriate technology solutions, and continuously refining processes, practices can maximize the benefits this technology offers. Greenhive Billing Solutions provides comprehensive revenue cycle management services that leverage advanced EDI capabilities to help healthcare providers improve financial performance while maintaining focus on patient care. Our experienced team manages the complete billing process using industry-standard platforms, ensuring maximum reimbursements and operational efficiency for practices across the United States.