Understanding what is IPA in medical billing is essential for healthcare providers navigating the complexities of modern revenue cycle management. Independent Physician Associations, commonly known as IPAs, serve as vital intermediaries between individual healthcare practices and insurance companies, creating a framework that allows smaller providers to compete effectively in managed care environments. For practices looking to optimize their billing operations and improve reimbursement rates, grasping the role and function of IPAs becomes increasingly important in a healthcare landscape dominated by value-based care and complex payer relationships.
What IPA Stands for in Medical Billing
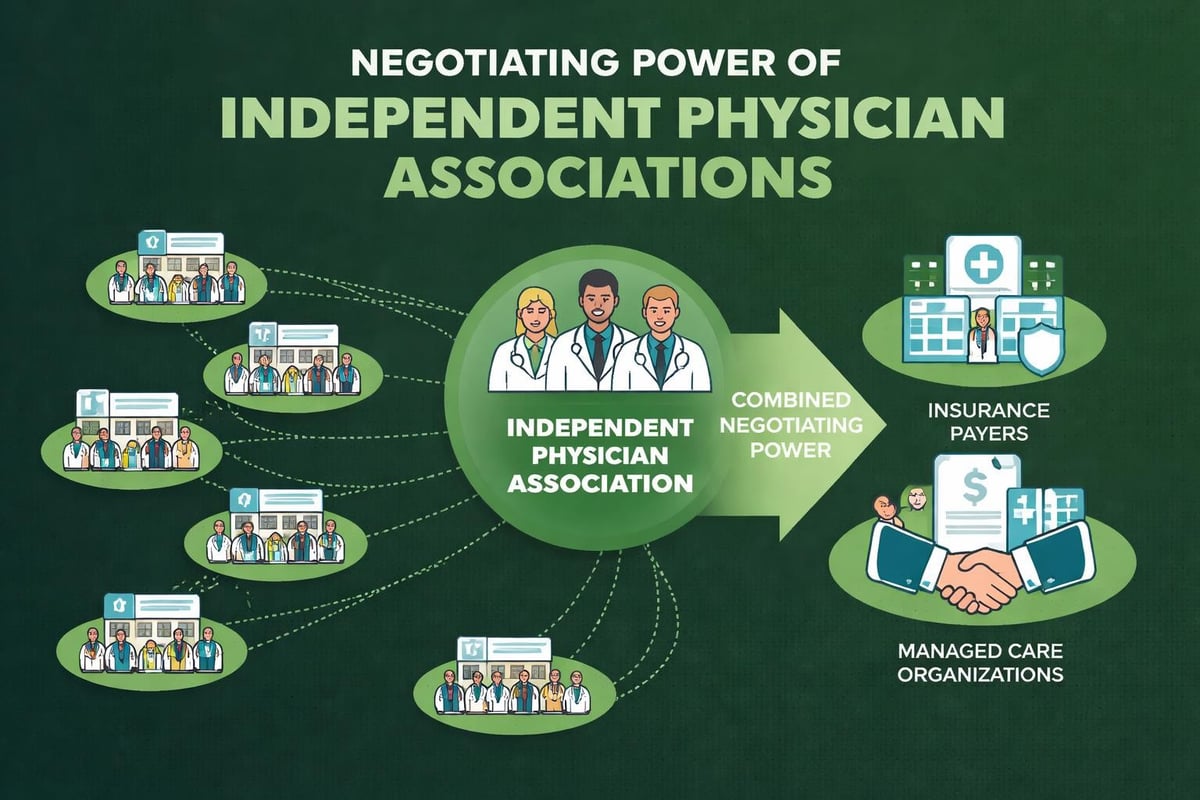
IPA stands for Independent Physician Association, a business entity that allows independent physicians and healthcare providers to collectively negotiate contracts with insurance companies while maintaining their practice autonomy. According to the American Academy of Family Physicians, these associations emerged as a response to the managed care revolution, providing solo practitioners and small group practices with bargaining power they couldn't achieve independently.
The structure allows physicians to remain in their own practices rather than becoming employees of large hospital systems or health maintenance organizations. This arrangement gives providers the financial benefits of larger networks while preserving their clinical independence and business ownership.
Core Purpose of IPAs
Independent Physician Associations serve multiple strategic functions in the healthcare ecosystem:
- Contract negotiation leverage with major insurance carriers and health plans
- Risk-sharing arrangements that distribute financial exposure across multiple providers
- Administrative support for billing, credentialing, and compliance activities
- Quality improvement initiatives that help members meet performance benchmarks
- Utilization management to control costs while maintaining care standards
By pooling resources, IPA members gain access to sophisticated infrastructure and expertise that would be cost-prohibitive for individual practices. This collective approach addresses many challenges faced by independent providers in today's competitive healthcare market.
How IPAs Function Within Revenue Cycle Management
When exploring what is IPA in medical billing from an operational perspective, it's important to understand the workflow and financial mechanisms involved. IPAs typically contract with managed care organizations, health maintenance organizations (HMOs), and preferred provider organizations (PPOs) on behalf of their physician members. These contracts establish reimbursement rates, quality metrics, and administrative requirements that directly impact how claims are processed and paid.
The Independent Practice Association model creates a distinct billing pathway that differs from traditional fee-for-service arrangements. Rather than each physician negotiating separately with payers, the IPA establishes master agreements that standardize terms across all member providers.
Payment Models and Distribution
IPAs commonly implement several payment structures that affect revenue cycle operations:
- Capitation payments where the IPA receives a fixed monthly amount per enrolled patient
- Fee-for-service arrangements with negotiated rates above standard Medicare schedules
- Shared savings programs that reward cost-effective care delivery
- Performance-based incentives tied to quality metrics and patient outcomes
- Bundled payments for episode-based care coordination
Each model requires different billing approaches and financial tracking. Medical billing services must adapt their processes to accommodate these varied payment mechanisms while ensuring accurate claim submission and proper revenue recognition.
| Payment Model | Billing Complexity | Risk Level | Revenue Predictability |
|---|---|---|---|
| Capitation | Low | High | Very High |
| Fee-for-Service | Medium | Low | Medium |
| Shared Savings | High | Medium | Low |
| Performance-Based | High | Medium | Medium |
| Bundled Payments | Very High | High | Medium |
Benefits of IPA Participation for Healthcare Providers
Understanding what is IPA in medical billing also means recognizing the tangible advantages these associations deliver to member practices. The financial and operational benefits extend throughout the entire revenue cycle, from patient registration through final payment posting.
Enhanced reimbursement rates represent one of the most immediate benefits. Individual practices rarely possess the negotiating strength to secure favorable contracts with major insurance carriers. Through collective bargaining, IPAs frequently obtain reimbursement rates 15-30% higher than what solo practitioners could negotiate independently.
Operational Advantages
Beyond better payment rates, IPA membership provides crucial infrastructure support:
- Access to centralized credentialing services that expedite provider enrollment
- Standardized billing protocols that reduce claim denials
- Shared technology platforms for claims submission and tracking
- Compliance monitoring to ensure regulatory adherence
- Expert guidance on coding updates and payer policy changes
These operational benefits directly impact the efficiency of revenue cycle management processes, reducing administrative burden and accelerating cash flow for member practices.

Risk Mitigation and Financial Stability
IPAs distribute financial risk across their entire membership base, protecting individual providers from catastrophic losses. In capitated or risk-sharing arrangements, high-cost patients are absorbed by the collective rather than devastating a single practice's finances. This risk pooling creates more predictable revenue streams and financial stability.
Denial management services become more effective within IPA frameworks because patterns of denials can be identified across multiple practices, enabling systemic solutions rather than provider-by-provider troubleshooting.
Challenges and Considerations in IPA Medical Billing
While the benefits are substantial, understanding what is IPA in medical billing requires acknowledging the complexities and potential drawbacks these arrangements introduce. The administrative requirements and financial risks demand careful evaluation before joining an IPA.
Loss of billing autonomy tops the list of concerns for many practices. IPA contracts typically mandate specific billing software, coding protocols, and submission timelines. Providers must adapt their internal processes to IPA requirements, which may conflict with established workflows or preferred systems.
Administrative Complexity
IPA participation introduces layers of administrative requirements:
- Dual reporting obligations to both the IPA and individual payers
- Compliance with IPA-specific documentation standards beyond standard requirements
- Participation in quality reporting initiatives that demand additional data collection
- Attendance at mandatory meetings and training sessions
- Adherence to utilization management protocols that may delay patient services
These obligations require dedicated staff time and resources. Smaller practices may struggle to meet IPA requirements without investing in additional administrative personnel or outsourcing to specialized medical billing services.
Financial Risk Exposure
Despite risk pooling benefits, IPA membership introduces new financial vulnerabilities. Capitated payment models shift insurance risk from payers to providers. If patient utilization exceeds projections, the IPA and its members absorb the losses. Practices accustomed to fee-for-service stability may find this uncertainty challenging.
| Risk Factor | Impact Level | Mitigation Strategy |
|---|---|---|
| Patient Over-Utilization | High | Robust utilization management |
| Coding Errors | Medium | Comprehensive training programs |
| Contract Termination | High | Diversified payer mix |
| Quality Metric Failures | Medium | Regular performance monitoring |
| Technology System Issues | Low | Redundant systems and backup |
Best Practices for Working with IPAs
For healthcare providers seeking to maximize the benefits of IPA participation, implementing strategic operational practices proves essential. Understanding what is IPA in medical billing from a practical standpoint means establishing workflows that align with IPA requirements while maintaining billing efficiency.
Clear communication channels between the practice, IPA administrators, and billing teams form the foundation of success. Regular meetings should review financial performance, address billing challenges, and discuss upcoming contract changes. This proactive communication prevents surprises and allows time for process adjustments.
Documentation and Coding Excellence
IPAs typically impose stricter documentation requirements than traditional payers because they assume financial risk. Best practices include:
- Implementing real-time coding audits before claim submission
- Training clinical staff on documentation requirements specific to IPA contracts
- Utilizing clinical decision support tools integrated with electronic health records
- Conducting quarterly reviews of coding accuracy and compliance
- Maintaining detailed encounter notes that support medical necessity
Professional medical coding services can provide the expertise needed to meet these elevated standards, reducing denial rates and protecting revenue.
Technology Integration
Successful IPA participation requires seamless technology integration. Practices must ensure their practice management and billing systems can:
- Exchange data with IPA reporting platforms efficiently
- Track patient attribution to specific IPA contracts and risk pools
- Monitor quality metrics in real-time for proactive intervention
- Generate reports that meet IPA administrative requirements
- Submit claims through IPA-designated clearinghouses or portals
Many providers partner with experienced revenue cycle management companies that maintain expertise across multiple IPA platforms and requirements, ensuring compliance without overwhelming internal staff.
IPA Impact on Claims Processing and Reimbursement
When examining what is IPA in medical billing through the lens of claims management, the differences from standard billing become apparent. Claims processing within IPA frameworks involves additional verification steps and unique coding requirements that directly affect reimbursement speed and accuracy.
Patient eligibility verification becomes more nuanced with IPA involvement. Beyond confirming active insurance coverage, billing staff must verify the patient's assignment to the specific IPA and understand which services fall under capitated payments versus fee-for-service arrangements. This distinction determines whether individual claims should be submitted or if services are covered under the monthly capitation payment.
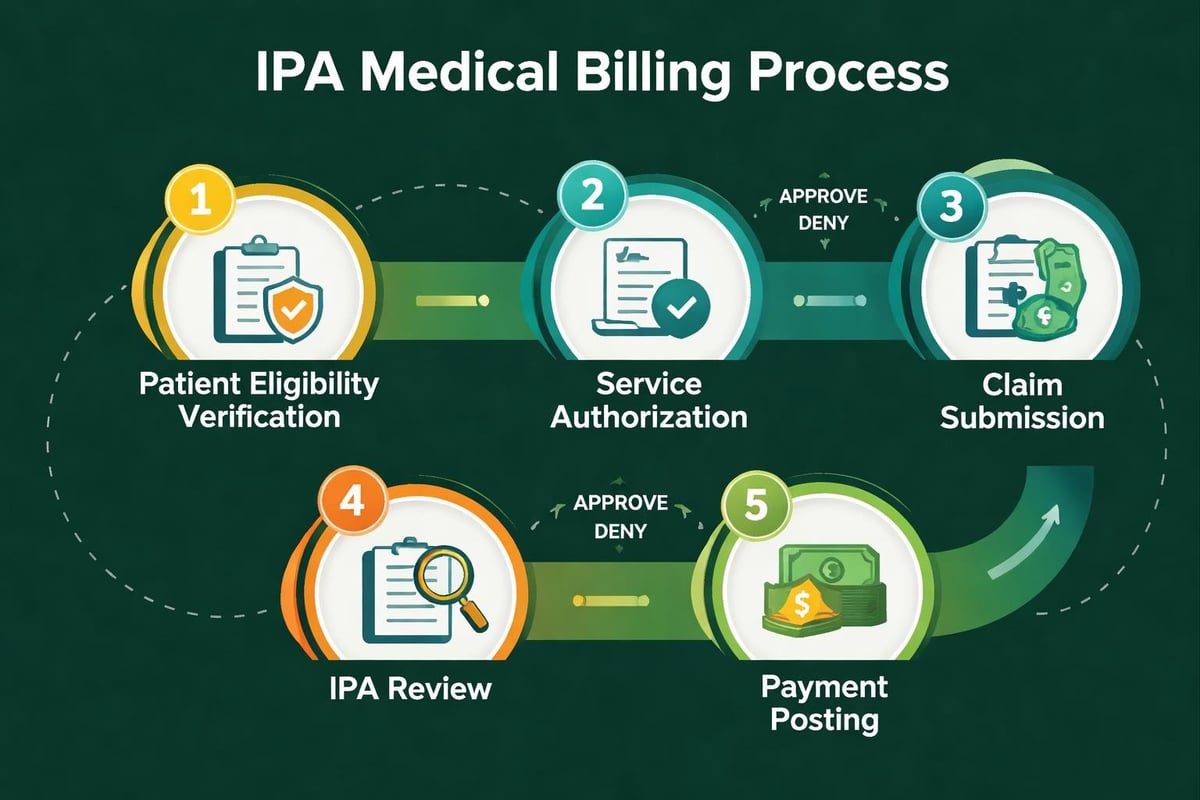
Prior Authorization Requirements
IPAs frequently implement stringent prior authorization protocols to manage utilization and control costs. These requirements often exceed those imposed by the underlying insurance carrier. Common authorization triggers include:
- Specialist referrals outside the IPA network
- High-cost diagnostic imaging and procedures
- Durable medical equipment exceeding specified thresholds
- Elective surgical procedures
- Experimental or non-formulary treatments
Prior authorization services become critical for practices within IPA networks, as failure to obtain proper authorization often results in complete claim denials with no recourse for payment.
Payment Posting and Reconciliation
Payment posting within IPA arrangements requires additional scrutiny because multiple payment sources may apply to a single patient encounter. A visit might generate:
- Capitation payment (already received monthly)
- Fee-for-service payment for services outside capitation
- Patient copayment or coinsurance
- Quality incentive payment (distributed quarterly)
Payment posting services must accurately allocate these various revenue streams to maintain clean accounts receivable and identify underpayments. Reconciliation processes should compare actual payments against contract terms to ensure the IPA and payers honor negotiated rates.
Credentialing and Provider Enrollment in IPAs
A comprehensive understanding of what is IPA in medical billing includes recognizing the credentialing complexities these associations introduce. Provider enrollment extends beyond standard payer credentialing to encompass IPA-specific requirements and ongoing maintenance obligations.
Initial credentialing for IPA participation typically involves submitting extensive documentation including professional licenses, board certifications, malpractice insurance, hospital privileges, and work history. The IPA conducts its own verification process separate from individual insurance companies, adding time to the enrollment cycle.
Ongoing Compliance Monitoring
IPA membership imposes continuous compliance obligations:
- Annual recredentialing with updated documentation
- Maintenance of minimum malpractice coverage levels
- Participation in required continuing education programs
- Adherence to quality reporting deadlines
- Cooperation with peer review processes
Professional medical credentialing services help practices navigate these requirements efficiently, preventing lapses that could interrupt IPA participation and payment eligibility.
Multi-IPA and Multi-Payer Management
Many successful practices participate in multiple IPAs simultaneously to diversify their payer mix and patient base. This strategy provides financial stability but multiplies administrative complexity. Each IPA maintains distinct contracts, protocols, and reporting requirements.
| Management Area | Single IPA | Multiple IPAs |
|---|---|---|
| Contract Terms | Simple | Complex tracking required |
| Credentialing Maintenance | Manageable | Significant administrative burden |
| Billing Protocols | Standardized | Multiple systems needed |
| Quality Reporting | Straightforward | Duplicative but non-identical |
| Financial Reconciliation | Direct | Requires sophisticated analysis |
Future Trends in IPA Medical Billing
The landscape of what is IPA in medical billing continues evolving as healthcare payment models shift toward value-based care and population health management. IPAs are adapting their structures and services to meet changing market demands and regulatory requirements.
Data analytics and population health capabilities are becoming central to IPA value propositions. Forward-thinking associations invest in sophisticated platforms that track patient outcomes, identify care gaps, and predict high-risk patients before costly interventions become necessary. These insights enable proactive care management that improves quality while controlling costs.
Technology-Driven Transformation
Emerging technologies are reshaping IPA operations:
- Artificial intelligence for predictive analytics and risk stratification
- Automated coding assistance to improve accuracy and efficiency
- Real-time eligibility verification integrated with scheduling systems
- Patient engagement platforms for care coordination and communication
- Blockchain solutions for secure, transparent claims processing
Healthcare providers evaluating IPA partnerships should assess the association's technology roadmap and investment in innovation. Organizations embracing advanced healthcare revenue cycle analytics position their members for long-term success in value-based payment environments.
Regulatory and Policy Considerations
Changes in healthcare policy significantly impact IPA operations. Recent developments include:
- Expansion of value-based payment models requiring IPA adaptation
- Enhanced quality reporting requirements through programs like MIPS and APMs
- Price transparency regulations affecting contract negotiations
- Telehealth reimbursement evolution creating new revenue opportunities
- Healthcare consolidation trends altering competitive dynamics
Staying informed about regulatory changes and their implications for IPA participation helps practices make strategic decisions about association involvement and contract terms.
Independent Physician Associations play a crucial role in modern medical billing by providing independent practitioners with the negotiating power and administrative infrastructure necessary to thrive in managed care environments. Understanding what is IPA in medical billing empowers healthcare providers to make informed decisions about participation and optimize their revenue cycle operations within these frameworks. Greenhive Billing Solutions brings specialized expertise in managing the complexities of IPA billing, credentialing, and claims processing, helping practices maximize reimbursements while maintaining compliance across multiple payer relationships. Our team adapts to your existing systems and IPA requirements, delivering comprehensive revenue cycle management that drives financial performance.

