Healthcare providers face increasing pressure to maintain financial stability while delivering quality patient care. Revenue cycle management systems have emerged as critical infrastructure for medical practices seeking to optimize their billing operations and maximize reimbursements. These comprehensive solutions address every stage of the patient financial journey, from initial registration through final payment collection. Understanding how these systems function and their impact on practice profitability has become essential for healthcare administrators, physicians, and billing managers across the United States.
Understanding Revenue Cycle Management Systems
Revenue cycle management systems represent the technological and procedural framework that healthcare organizations use to track patient service revenue from initial appointment scheduling through final payment reconciliation. These systems encompass both software platforms and the processes that govern how patient data, clinical information, and financial transactions flow through an organization.
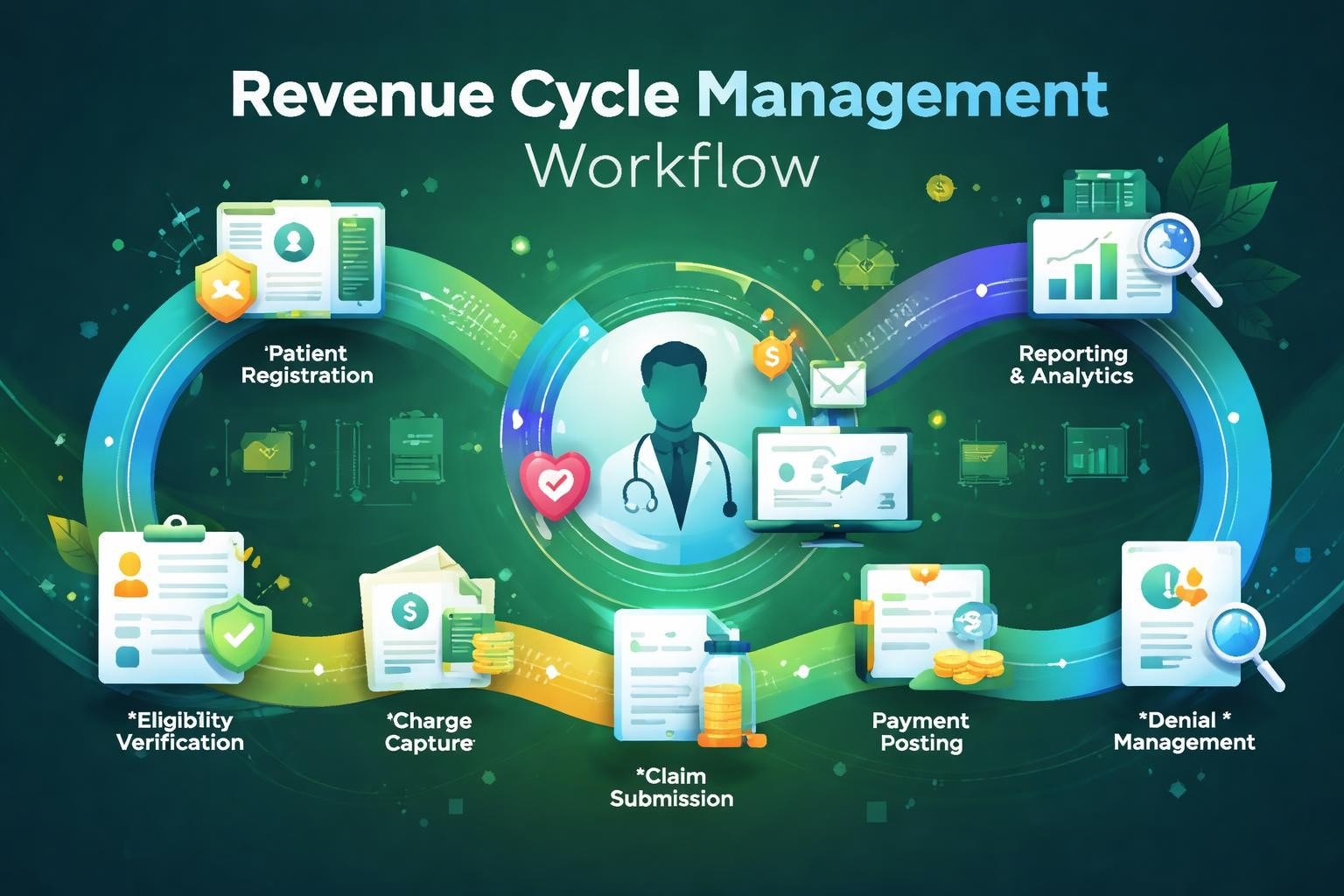
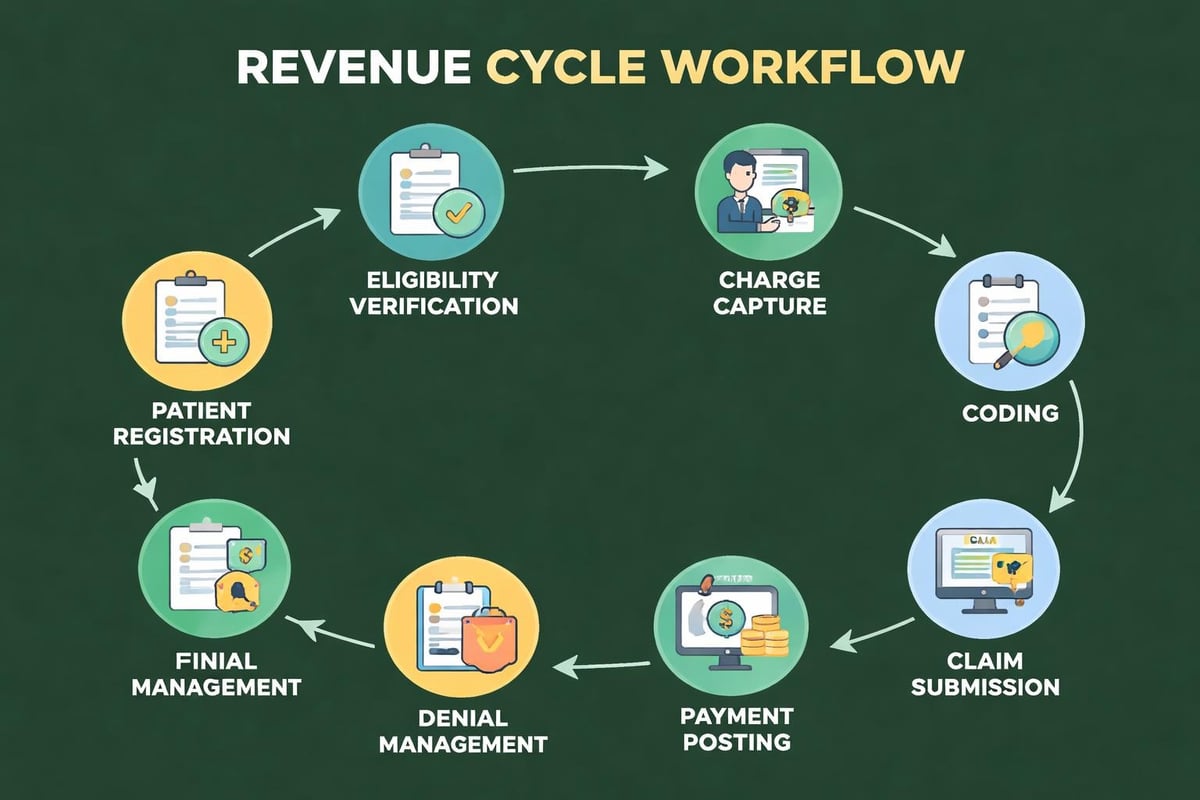
The primary function of revenue cycle management systems is to ensure accurate and timely reimbursement for medical services rendered. This involves multiple interconnected processes including patient registration, insurance verification, charge capture, coding, claim submission, payment posting, and collections. Each component must function seamlessly to prevent revenue leakage and reduce administrative burden.
Modern healthcare billing environments demand sophisticated systems capable of handling complex payer requirements, regulatory compliance mandates, and evolving reimbursement models. According to the Healthcare Financial Management Association, effective revenue cycle management directly impacts an organization's ability to maintain financial health while delivering quality care.
Core Components of Effective Systems
Revenue cycle management systems consist of several integrated modules that work together to process patient financial information. Understanding these components helps healthcare providers identify areas for improvement and optimization.
Essential system elements include:
- Patient access and registration modules
- Insurance eligibility verification tools
- Charge capture and coding interfaces
- Claims management and submission platforms
- Payment posting and reconciliation systems
- Denial management and appeals tracking
- Reporting and analytics dashboards
Each module serves a distinct purpose while contributing to the overall efficiency of the revenue cycle. Patient access components ensure accurate demographic and insurance information collection at the point of service. Verification tools confirm coverage before services are rendered, reducing the risk of claim denials. Coding interfaces help translate clinical documentation into billable procedures, while claims platforms manage the submission process to various payers.
The sophistication of revenue cycle management systems has evolved significantly to address changing healthcare reimbursement landscapes. Many organizations now implement systems that incorporate artificial intelligence and machine learning to predict claim denial risks, identify coding patterns, and automate routine tasks. These technological advancements help practices maintain competitiveness while managing operational costs.
Key Benefits for Healthcare Organizations
Implementing robust revenue cycle management systems delivers measurable advantages that extend beyond basic billing functions. Healthcare providers who invest in optimizing these systems typically experience improvements across multiple operational and financial metrics.
Financial performance improvements include:
- Reduced claim denial rates
- Faster payment cycles
- Improved cash flow predictability
- Enhanced collection rates
- Lower administrative costs
Organizations report significant reductions in days in accounts receivable when they streamline their revenue cycle processes. This acceleration means practices receive payments more quickly, improving working capital and reducing the need for external financing. The American Medical Association’s revenue cycle guide emphasizes that understanding payment mechanics is essential for maximizing reimbursement.
Beyond financial metrics, effective systems contribute to operational efficiency by reducing manual workload and minimizing errors. Staff members spend less time correcting rejected claims and can focus on higher-value activities like patient care coordination and strategic financial planning. This efficiency gain proves particularly valuable for smaller practices with limited administrative resources.
| Metric | Before Optimization | After Optimization | Improvement |
|---|---|---|---|
| Clean Claim Rate | 78% | 95% | +17% |
| Days in A/R | 48 days | 32 days | -33% |
| Denial Rate | 12% | 4% | -67% |
| Collection Rate | 94% | 98% | +4% |
These performance improvements translate directly to practice profitability. When claims are submitted correctly the first time, practices avoid costly rework and expedite payment receipt. Lower denial rates mean fewer resources dedicated to appeals and resubmissions.
Operational Efficiency Gains
Revenue cycle management systems streamline workflows by automating repetitive tasks and establishing standardized procedures across the organization. This standardization reduces variability in billing practices and ensures consistency regardless of which team member handles a particular claim.
Automation capabilities within modern systems handle tasks such as eligibility verification, claim status checking, and payment posting without manual intervention. These automated processes run continuously, processing information faster and more accurately than manual methods. Staff members receive alerts only when exceptions require human judgment or intervention.
For practices utilizing medical billing services, integration with revenue cycle management systems ensures seamless data exchange and real-time visibility into billing operations. This transparency allows providers to monitor performance metrics and identify bottlenecks before they impact cash flow.
Critical Selection Criteria for Healthcare Providers
Choosing appropriate revenue cycle management systems requires careful evaluation of organizational needs, existing infrastructure, and long-term strategic goals. Healthcare providers must consider multiple factors to ensure selected systems align with practice requirements and deliver expected returns on investment.
System Integration Capabilities
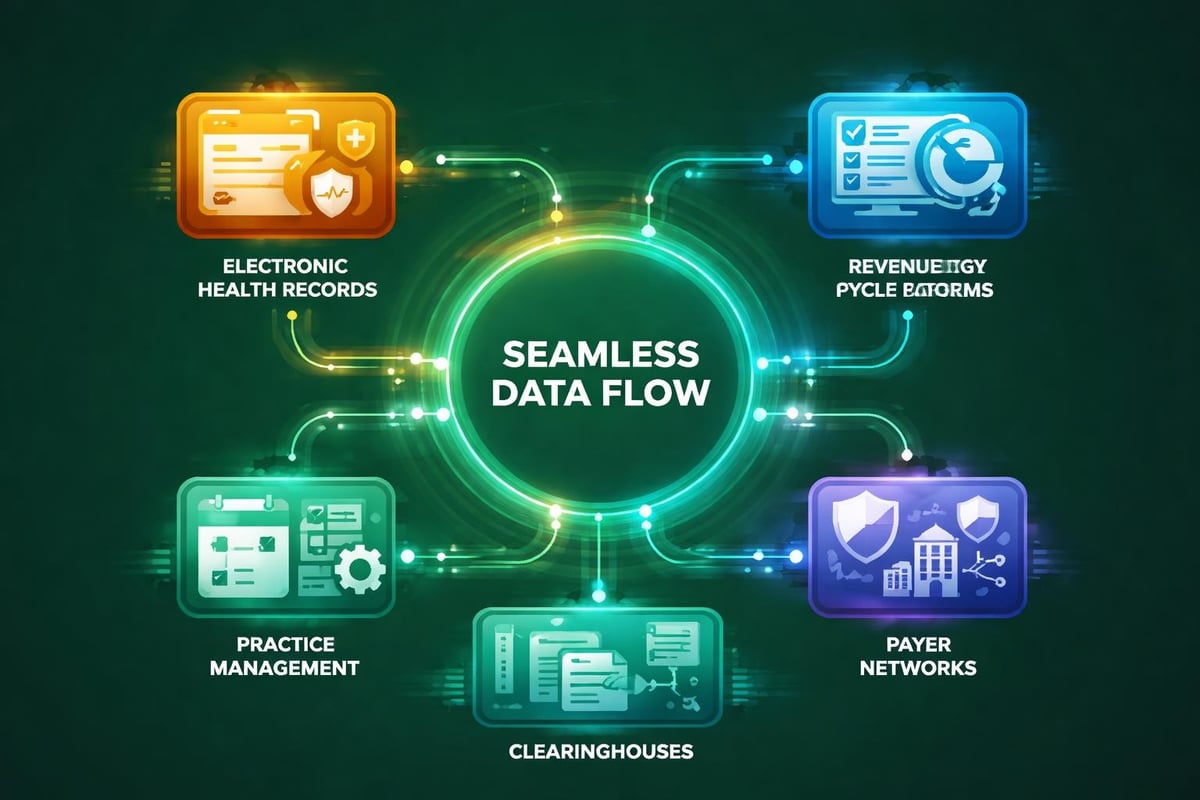
Modern medical practices use various software platforms for electronic health records, practice management, scheduling, and clinical documentation. Revenue cycle management systems must integrate seamlessly with these existing tools to avoid data silos and duplicate entry requirements.
Integration considerations include:
- Electronic health record compatibility – Systems should exchange clinical data automatically to support accurate coding and billing
- Practice management connectivity – Scheduling, registration, and demographic information must flow between platforms without manual intervention
- Payer clearinghouse connections – Direct interfaces with major clearinghouses streamline claim submission and status tracking
- Banking system integration – Payment posting becomes more efficient when systems connect directly to merchant services and lockbox providers
Practices that achieve strong integration across their technology ecosystem report fewer errors, faster processing times, and improved staff satisfaction. The ability to view patient financial information alongside clinical data provides valuable context for care delivery decisions and patient communication.
Scalability and Flexibility Requirements
Healthcare organizations evolve over time through growth, mergers, service line expansion, and regulatory changes. Revenue cycle management systems must accommodate these changes without requiring complete replacement or extensive customization.
Scalable systems handle increasing transaction volumes as patient populations grow. They support adding new providers, locations, and specialties without degrading performance. Flexible platforms adapt to changing payer requirements, new billing codes, and regulatory mandates through configuration rather than programming.
Cloud-based revenue cycle management systems offer particular advantages for scalability because they eliminate infrastructure constraints and provide automatic updates. Practices avoid capital expenditures for servers and can adjust capacity based on actual usage patterns.
| Feature | On-Premise Systems | Cloud-Based Systems |
|---|---|---|
| Initial Investment | High | Low |
| Scalability | Limited | Unlimited |
| Updates | Manual | Automatic |
| Disaster Recovery | Complex | Built-in |
| Remote Access | Difficult | Standard |
Implementation Best Practices
Successfully deploying revenue cycle management systems requires strategic planning, stakeholder engagement, and attention to change management principles. Organizations that follow structured implementation approaches achieve faster time to value and higher user adoption rates.
Planning and Preparation Phase
Before selecting or implementing systems, healthcare providers should conduct comprehensive assessments of current state operations. This evaluation identifies specific pain points, quantifies improvement opportunities, and establishes baseline metrics for measuring success.
Preparation activities include:
- Process mapping – Document current workflows to understand how work moves through the organization
- Performance baselining – Measure existing key performance indicators like denial rates, days in accounts receivable, and collection percentages
- Stakeholder identification – Determine who will use the system and how it impacts their daily responsibilities
- Requirements definition – Specify must-have features versus nice-to-have capabilities based on organizational priorities
- Budget allocation – Account for software costs, implementation services, training, and ongoing support
Thorough preparation prevents common implementation pitfalls such as scope creep, inadequate training, and poor user adoption. Organizations should involve frontline staff in requirements gathering to ensure systems support actual workflow needs rather than theoretical ideals.
Teams providing denial management services can offer valuable insights during planning phases because they understand common failure points in the revenue cycle and can recommend system features that address these challenges.
Data Migration and System Configuration
Transitioning from legacy systems to new revenue cycle management platforms requires careful data migration planning. Historical patient accounts, payer contracts, fee schedules, and other reference data must transfer accurately to maintain business continuity.
Clean data migration begins with data quality assessment and remediation. Organizations should identify duplicate records, correct formatting inconsistencies, and validate critical information before migration. This upfront investment prevents perpetuating errors into new systems and establishes strong data governance practices.
System configuration involves setting up rules, workflows, and templates that align with organizational preferences and payer requirements. Rather than accepting default settings, successful implementations customize systems to match established best practices and specialty-specific needs.
Optimizing System Performance
Implementing revenue cycle management systems represents the beginning rather than the end of the optimization journey. Healthcare organizations must continuously monitor performance, identify improvement opportunities, and refine processes to maximize system value.
Key Performance Indicators and Metrics
Effective measurement frameworks track both leading and lagging indicators across the revenue cycle. Leading indicators predict future performance and enable proactive intervention, while lagging indicators confirm historical results and validate improvement initiatives.
Critical metrics to monitor include:
- First pass resolution rate
- Clean claim percentage
- Average days in accounts receivable
- Net collection rate
- Point of service collections
- Denial rate by reason code
- Authorization approval time
- Coding accuracy percentage
Regular reporting on these metrics helps identify trends before they become significant problems. For example, an increasing denial rate for a specific payer might indicate changes in their requirements that necessitate workflow adjustments or additional staff training.
| Metric Category | Example Metrics | Target Range |
|---|---|---|
| Access | Insurance verification rate, Registration accuracy | >95% |
| Billing | Clean claim rate, Coding accuracy | >95% |
| Collections | Net collection rate, Days in A/R | >98%, <35 days |
| Denials | Denial rate, Overturn percentage | <5%, >60% |
Dashboard visualization tools within revenue cycle management systems enable stakeholders to monitor performance at a glance and drill down into specific issues when anomalies appear. Customizable dashboards should provide role-specific views so executives see high-level trends while operational staff access detailed transaction information.
Continuous Process Improvement
The most successful healthcare organizations treat revenue cycle optimization as an ongoing discipline rather than a one-time project. They establish regular review cycles to evaluate performance data, solicit staff feedback, and implement incremental improvements.
Process improvement methodologies like Lean and Six Sigma provide structured frameworks for identifying waste, reducing variation, and enhancing quality. Applied to revenue cycle operations, these approaches help eliminate non-value-added steps, standardize best practices, and reduce defects that lead to claim denials.
Staff members working directly with revenue cycle management systems often identify practical improvements that executives might overlook. Creating formal channels for capturing and evaluating these suggestions builds engagement and taps into frontline expertise.
Organizations leveraging eligibility verification services benefit from specialized expertise in one of the most critical early stages of the revenue cycle. Verification accuracy directly impacts downstream billing success and patient satisfaction.

Compliance and Security Considerations
Revenue cycle management systems process highly sensitive patient financial and health information, making security and regulatory compliance paramount concerns. Healthcare providers must ensure their systems meet stringent requirements for data protection, privacy, and auditability.
HIPAA Compliance Requirements
The Health Insurance Portability and Accountability Act establishes national standards for protecting patient health information. Revenue cycle management systems must implement administrative, physical, and technical safeguards to ensure HIPAA compliance.
Technical safeguards include encryption for data at rest and in transit, access controls that limit information viewing to authorized personnel, and audit logs that track who accessed what information and when. These protections prevent unauthorized disclosure while maintaining necessary access for legitimate business purposes.
Compliance considerations include:
- Role-based access controls
- Encryption standards
- Audit trail capabilities
- Business associate agreements
- Breach notification procedures
- Regular security assessments
Healthcare providers remain ultimately responsible for compliance even when using external systems or services. Business associate agreements formalize these relationships and specify each party's responsibilities for protecting patient information. Organizations should verify that vendors maintain appropriate certifications and undergo regular security audits.
Data Backup and Disaster Recovery
Revenue cycle interruptions due to system failures, natural disasters, or cyberattacks can devastate healthcare organizations financially. Robust backup and recovery capabilities ensure business continuity even when primary systems become unavailable.
Modern cloud-based revenue cycle management systems typically include redundant data storage across geographically dispersed data centers. This distribution protects against localized disruptions and enables rapid failover when issues occur. Organizations should verify recovery time objectives and recovery point objectives align with their business requirements.
Regular testing of backup and recovery procedures validates that systems will function as expected during actual emergencies. Many organizations discover gaps in their disaster recovery plans only when attempting real recoveries, making periodic testing essential for preparedness.
Emerging Trends and Future Developments
The revenue cycle management landscape continues evolving in response to technological innovation, regulatory changes, and shifting reimbursement models. Healthcare providers should monitor these trends to anticipate future requirements and maintain competitive advantages.
Artificial intelligence and machine learning increasingly influence revenue cycle management systems by automating complex decision-making processes. These technologies identify patterns in denial data to predict which claims face rejection risk, recommend coding options based on clinical documentation, and prioritize work queues based on revenue impact.
Robotic process automation handles repetitive tasks such as claim status checking, payment posting, and eligibility verification without human intervention. This automation frees staff to focus on exceptions that require judgment and complex problem-solving. Research from TechTarget on revenue cycle management software highlights how automation continues transforming billing operations.
Emerging capabilities include:
- Predictive analytics for denial prevention
- Natural language processing for coding assistance
- Real-time eligibility verification at point of service
- Automated prior authorization management
- Patient payment estimation and collection
- Value-based care performance tracking
Consumer engagement tools integrated with revenue cycle management systems improve patient financial experiences through transparent cost estimates, convenient payment options, and self-service account access. As patients bear increasing financial responsibility through high-deductible health plans, these capabilities become essential for maintaining collection rates.
Interoperability improvements driven by regulations like the 21st Century Cures Act facilitate data exchange between disparate systems. Enhanced interoperability reduces administrative burden, improves care coordination, and streamlines prior authorization processes that often delay or prevent payment.
Partnering With Revenue Cycle Management Experts
Many healthcare providers recognize that maintaining internal expertise across all revenue cycle functions requires significant investment in staffing, training, and technology. Partnering with specialized service providers offers an alternative approach that delivers professional expertise without the overhead of building internal capabilities.
Service providers bring experienced professionals who understand payer-specific requirements, coding guidelines, and regulatory compliance mandates. These specialists work with industry-standard tools and adapt to each organization's existing systems and workflows. The flexibility to scale services based on volume fluctuations provides cost predictability and operational efficiency.
When evaluating potential partners, healthcare organizations should assess track record, specialization in relevant practice areas, technology capabilities, and cultural fit. The right partnership extends an organization's capabilities without compromising control over patient relationships or strategic direction. Providers offering medical claim submission services can streamline one of the most critical aspects of revenue cycle operations.
Transparent communication and regular reporting ensure alignment between service providers and healthcare organizations. Detailed performance dashboards, scheduled review meetings, and collaborative problem-solving create partnerships that continuously improve rather than simply maintaining status quo operations.
Organizations utilizing comprehensive services gain access to specialized knowledge in areas like prior authorization services and payment posting services without the challenge of recruiting and retaining specialists in these disciplines.
Revenue cycle management systems form the financial backbone of modern healthcare delivery, enabling organizations to capture appropriate reimbursement while maintaining operational efficiency. As reimbursement models evolve and regulatory requirements increase in complexity, the sophistication of these systems becomes increasingly critical to practice success. Greenhive Billing Solutions delivers comprehensive revenue cycle management services that optimize every stage of the patient financial journey, from initial eligibility verification through final payment collection. Our experienced team works seamlessly with your existing systems to reduce denials, accelerate cash flow, and maximize reimbursements while maintaining strict HIPAA compliance and transparent communication.