Healthcare providers face mounting pressure to maintain financial stability while delivering quality patient care. Managing the complete financial lifecycle of patient encounters requires specialized expertise, efficient processes, and constant adaptation to regulatory changes. Revenue cycle management services have become essential for medical practices seeking to optimize reimbursements, reduce administrative burdens, and focus resources on clinical excellence. These comprehensive solutions address every financial touchpoint from initial patient contact through final payment reconciliation, ensuring maximum revenue capture while maintaining compliance with industry standards.
Understanding Revenue Cycle Management Services
Revenue cycle management services encompass the entire financial process that healthcare providers use to track patient care episodes from registration and appointment scheduling to the final payment of a balance. This systematic approach ensures that every billable service is properly documented, coded, submitted, and reimbursed. The Healthcare Financial Management Association recognizes revenue cycle management as a critical function that directly impacts a healthcare organization's financial performance and sustainability.
The scope of these services extends beyond simple billing operations. They include patient registration, insurance eligibility verification, charge capture, medical coding, claims submission, payment posting, denial management, and patient collections. Each component must function seamlessly to prevent revenue leakage and maintain steady cash flow.
Components of Comprehensive RCM Services
Professional revenue cycle management services address multiple operational areas simultaneously. Rather than treating billing as an isolated function, these services integrate financial and clinical workflows to create efficiency throughout the practice.
Core service components include:
- Patient registration and demographic verification to ensure accurate information from the first encounter
- Insurance eligibility verification to confirm coverage before services are rendered
- Medical coding and charge capture to translate clinical documentation into billable claims
- Claims submission and tracking to expedite reimbursement and identify issues early
- Payment posting and reconciliation to maintain accurate financial records
- Denial management and appeals to recover revenue from rejected claims
- Patient billing and collections to manage self-pay balances professionally
These interconnected services work together to minimize claim rejections, accelerate payment cycles, and reduce administrative overhead for healthcare providers.
The Business Case for Outsourcing RCM Services
Healthcare practices increasingly recognize that managing revenue cycles internally diverts resources from patient care and requires significant infrastructure investment. According to TechTarget research, a significant percentage of revenue cycle leaders now outsource outpatient services to specialized providers, reflecting growing confidence in the B2B service model.
Outsourced revenue cycle management services deliver measurable financial benefits while reducing operational complexity. Practices gain access to dedicated professionals who stay current with coding updates, payer requirements, and regulatory changes without requiring internal training programs or staff expansion.
Cost Efficiency and Predictability
In-house billing departments require substantial fixed costs including salaries, benefits, software licenses, office space, and ongoing training. These expenses persist regardless of practice volume or collection rates. Revenue cycle management services typically operate on performance-based models, aligning costs directly with collections and creating financial predictability.
Financial advantages include:
- Reduced fixed overhead by eliminating full-time billing staff positions
- Elimination of software licensing fees and technology maintenance costs
- Scalability that adjusts to practice growth without hiring delays
- Performance-based pricing that ties expenses to actual collections
Practices also avoid the hidden costs of employee turnover, which disrupts billing operations and requires expensive recruitment and training cycles. Specialized service providers maintain consistent teams with deep expertise across multiple specialties.
Key Performance Metrics in RCM Services
Measuring the effectiveness of revenue cycle management services requires tracking specific key performance indicators that reveal operational health and financial performance. These metrics provide objective evidence of service quality and identify opportunities for continuous improvement.
| Metric | Target Range | Impact |
|---|---|---|
| First-pass claim acceptance rate | 95-98% | Reduces rework and accelerates payment |
| Days in accounts receivable | 30-40 days | Improves cash flow and working capital |
| Net collection rate | 95-99% | Maximizes revenue realization |
| Claim denial rate | 5-10% | Minimizes revenue leakage |
| Cost to collect | 3-5% of collections | Ensures operational efficiency |
Professional service providers deliver transparent reporting on these metrics, enabling healthcare organizations to monitor performance and make data-driven decisions. The reporting and analytics capabilities of quality RCM partners provide visibility into financial operations that many practices lack with internal billing.
Denial Management Performance
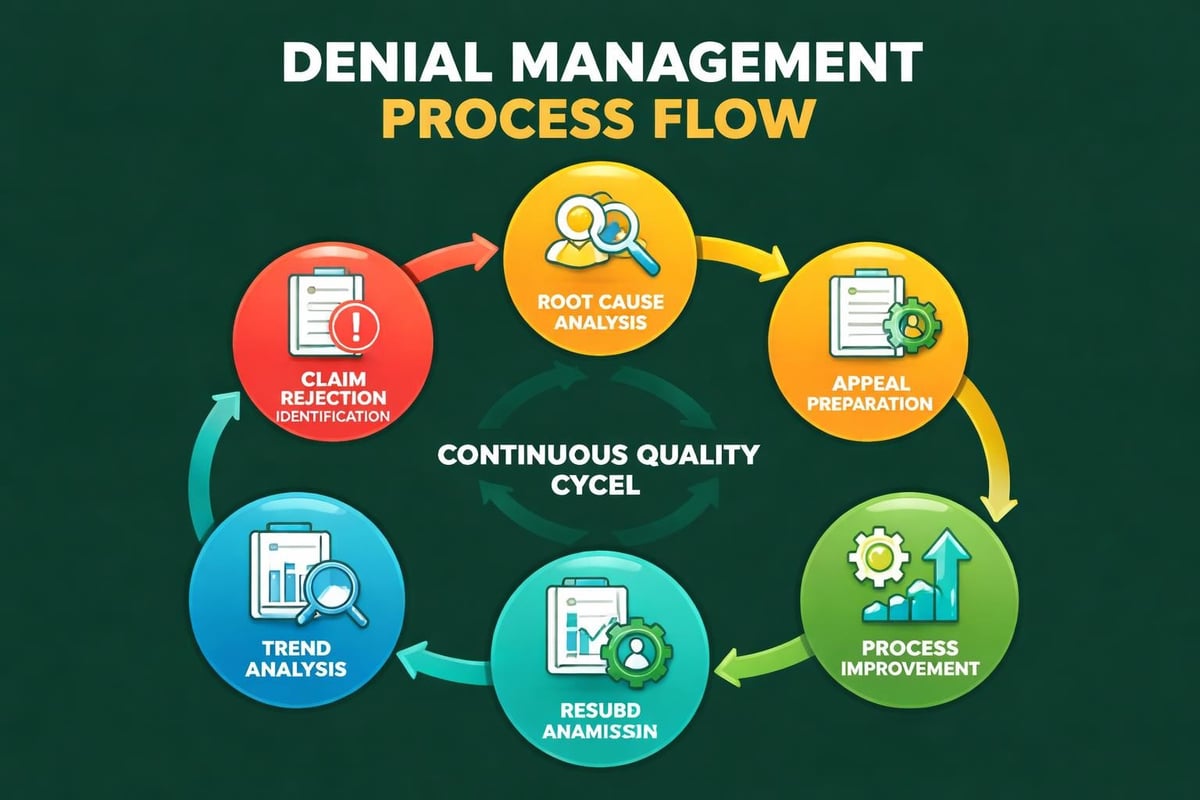
Denial rates serve as a critical indicator of RCM service quality. Every denied claim represents delayed or lost revenue and requires additional resources to resolve. Effective denial management services systematically identify denial patterns, address root causes, and implement preventive measures.
Professional RCM teams analyze denial data to identify trends across payers, procedure codes, and denial reasons. This intelligence allows them to adjust front-end processes, improve documentation requirements, and train clinical staff on capture requirements that prevent future denials.
Technology Integration and Adaptability
Modern revenue cycle management services leverage sophisticated technology platforms to automate workflows, reduce errors, and accelerate processing. However, the most effective B2B service providers demonstrate flexibility in working with client-owned systems rather than requiring proprietary software adoption.
This adaptability proves particularly valuable for practices that have invested in practice management systems or electronic health records with integrated billing capabilities. Rather than abandoning these investments, professional RCM services work within existing technology ecosystems, complementing practice systems with specialized expertise and dedicated resources.
Working with Client Systems
Experienced revenue cycle management professionals adapt to diverse software environments including industry-standard platforms used across healthcare. This flexibility eliminates the disruption and expense of system migrations while allowing practices to maintain familiar workflows.
Service providers train their teams on multiple platforms and stay current with software updates and feature enhancements. This expertise ensures that practices maximize their technology investments while benefiting from specialized billing knowledge that internal staff may lack.
When evaluating best medical billing software for small business needs, practices should consider how potential RCM partners integrate with different platforms. The ability to work seamlessly with existing systems reduces implementation timelines and maintains operational continuity.
Specialty-Specific RCM Expertise
Different medical specialties face unique billing challenges, coding requirements, and payer policies. Generalist billing approaches often miss specialty-specific nuances that impact reimbursement rates and claim acceptance. Revenue cycle management services with specialty expertise deliver superior results by understanding the specific requirements of each practice type.
Specialty considerations include:
- Cardiology practices require expertise in complex procedure coding, modifier usage for diagnostic and interventional services, and familiarity with cardiac-specific payer policies
- Primary care providers need efficient workflows for high-volume encounters, annual wellness visits, and preventive service billing
- Surgical specialties demand precise coding for procedures, appropriate bundling and unbundling decisions, and skilled global period management
- Diagnostic centers benefit from specialized knowledge of imaging codes, technical versus professional component billing, and radiology-specific compliance requirements
Professional service providers develop specialty-specific teams with concentrated experience in particular medical fields. This specialization ensures faster claims processing, higher acceptance rates, and better denial resolution compared to generalist approaches. For instance, cardiology medical billing requires understanding of cardiovascular-specific codes and documentation requirements that differ significantly from other specialties.
Compliance and Risk Management
Healthcare billing operates within a complex regulatory environment that exposes practices to significant compliance risks. Revenue cycle management services provide critical protection by implementing controls, maintaining current knowledge of regulatory requirements, and ensuring consistent adherence to billing standards.
HIPAA Compliance and Data Security
Patient financial information requires the same rigorous protection as clinical records under HIPAA privacy and security rules. Professional RCM service providers implement comprehensive safeguards including encryption, access controls, audit logging, and staff training to protect sensitive data throughout the revenue cycle.
| Security Measure | Protection Provided | Compliance Requirement |
|---|---|---|
| Data encryption in transit and at rest | Prevents unauthorized access to patient information | HIPAA Security Rule |
| Role-based access controls | Limits data exposure to minimum necessary | HIPAA Privacy Rule |
| Regular security audits | Identifies vulnerabilities before breaches occur | HIPAA Security Rule |
| Business associate agreements | Establishes legal framework for data handling | HIPAA Privacy Rule |
| Staff training programs | Ensures workforce understands compliance obligations | HIPAA Security Rule |
These protections extend beyond basic compliance to risk management that protects practices from costly data breaches, regulatory penalties, and reputational damage. Service providers maintain comprehensive policies and procedures that meet or exceed industry standards.
Front-End Revenue Cycle Optimization
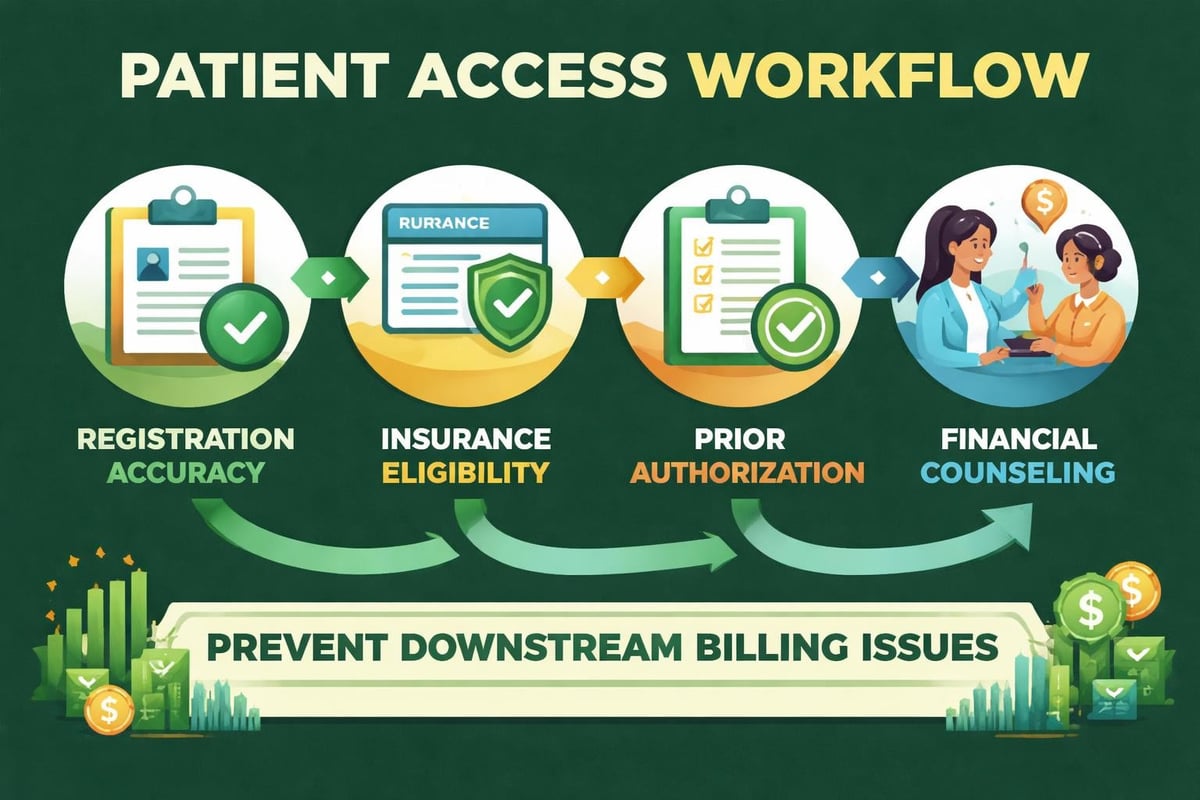
While many practices focus on back-end billing and collections, professional revenue cycle management services recognize that effective revenue capture begins at the patient's first contact. Front-end processes including registration, insurance verification, and authorization management directly impact claim acceptance rates and payment speed.
Insurance Verification and Authorization
Verifying insurance coverage before service delivery prevents claim denials, reduces patient balance disputes, and accelerates reimbursement. Eligibility verification services confirm active coverage, identify coordination of benefits issues, and determine patient financial responsibility before appointments.
Step-by-step verification process:
- Collect accurate insurance information during scheduling to ensure eligibility checks use correct payer details
- Verify coverage electronically through payer portals or clearinghouses to confirm active benefits
- Identify authorization requirements specific to the planned services and payer policies
- Submit prior authorizations when required, tracking approval status before scheduled appointments
- Communicate financial responsibility to patients, establishing clear expectations for copays, deductibles, and coinsurance
These proactive measures prevent the majority of preventable denials and create transparency around patient financial obligations. When patients understand their responsibility before service delivery, collection rates improve significantly.
Professional prior authorization services streamline this complex process, managing documentation requirements, payer communications, and appeal processes when authorizations are initially denied.
Medical Coding Accuracy and Compliance
Accurate medical coding forms the foundation of successful revenue cycle management. Coding errors create claim denials, trigger audits, delay payments, and potentially expose practices to fraud allegations. Professional medical coding services ensure that clinical documentation translates into precise, compliant codes that support maximum appropriate reimbursement.
Current Procedural Terminology and Diagnosis Coding
Professional coders maintain certification in current procedural terminology (CPT) and diagnosis coding systems, staying current with annual updates and payer-specific interpretations. This expertise proves particularly valuable as coding systems grow more complex and payer audits intensify.
The transition to ICD-10 dramatically increased diagnosis code specificity requirements, making professional coding expertise more valuable than ever. Revenue cycle management services employ certified coders who understand the clinical documentation necessary to support specific code selections and can communicate effectively with providers about documentation improvement.
Quality coding services also conduct regular audits to identify patterns, ensure compliance, and provide education that improves provider documentation. These medical coding audit services protect practices from compliance risks while optimizing reimbursement.
Claims Management and Submission
Once coding is complete, efficient claims management ensures rapid submission, proactive tracking, and quick resolution of issues. Professional revenue cycle management services leverage automated clearinghouses, electronic claim submission, and real-time claim status tracking to accelerate the payment cycle.
Electronic Claims Processing
Electronic claim submission offers significant advantages over paper claims including faster processing, immediate acknowledgment of receipt, and automated error checking that identifies issues before payer adjudication. Professional medical claim submission services optimize electronic workflows to maximize these benefits.
Electronic submission advantages:
- Submission to acknowledgment typically occurs within 24-48 hours compared to weeks for paper claims
- Real-time claim scrubbing identifies errors before submission, reducing rejection rates
- Electronic remittance advice streamlines payment posting and reconciliation
- Reduced postage and printing costs eliminate paper claim expenses
- Automated tracking provides visibility into claim status throughout the adjudication process
Professional service providers maintain direct connections with major payers and utilize sophisticated clearinghouses that route claims optimally based on payer requirements and historical performance data.
Payment Posting and Reconciliation
Accurate payment posting creates the financial foundation for practice management, providing visibility into collections, outstanding balances, and payer performance. Professional payment posting services ensure that every payment is recorded correctly, allocated appropriately, and reconciled against expected reimbursement.
Manual payment posting creates opportunities for errors that corrupt financial data and obscure practice performance. Automated posting from electronic remittance advice eliminates transcription errors while accelerating processing. However, experienced professionals must still review posting for accuracy and identify discrepancies that require investigation.
| Payment Type | Posting Complexity | Key Considerations |
|---|---|---|
| Insurance payments via ERA | Low to moderate | Automated posting with exception review |
| Insurance payments via paper EOB | Moderate to high | Manual entry with verification requirements |
| Patient payments | Low to moderate | Allocation to correct balances and services |
| Contractual adjustments | Moderate | Verification against contract terms |
| Denial and rejection postings | High | Categorization for tracking and appeal workflows |
Professional RCM services reconcile payments against expected amounts based on contract terms, identifying underpayments that require appeals and ensuring practices receive full contractual reimbursement.
Patient Financial Engagement
The shift toward high-deductible health plans has dramatically increased patient financial responsibility, making patient collections a larger component of practice revenue. Professional revenue cycle management services implement patient-friendly billing practices that improve collection rates while maintaining positive patient relationships.
Clear, timely communication about financial responsibility sets appropriate expectations and increases the likelihood of payment. Transparent billing statements that clearly explain charges, insurance payments, and patient balances reduce confusion and disputes.
Patient Payment Options and Flexibility
Modern patients expect convenient payment options including online portals, automated payment plans, and multiple payment methods. Revenue cycle management services implement patient-friendly payment technologies that accommodate these preferences while maintaining security and compliance.
Offering payment plans for large balances improves collection rates by making obligations manageable. Rather than writing off large patient balances as uncollectible, structured payment arrangements recover revenue over time while demonstrating flexibility that patients appreciate.
Professional services also implement appropriate collection escalation processes that balance revenue recovery with patient satisfaction. Rather than immediately engaging aggressive collection agencies, phased communication strategies often resolve balances while preserving patient relationships.
Selecting Revenue Cycle Management Services
Healthcare providers evaluating revenue cycle management services should consider multiple factors beyond basic pricing. The right partnership delivers not just cost savings but operational improvements, compliance protection, and strategic guidance that supports long-term practice growth.
Evaluation criteria should include:
- Specialty experience relevant to your practice type and patient mix
- Technology compatibility with existing practice management and EHR systems
- Transparent reporting providing visibility into key performance metrics
- Compliance programs demonstrating HIPAA adherence and audit preparedness
- Communication protocols ensuring responsive support and collaborative problem-solving
- Performance guarantees or benchmarks establishing clear service expectations
- Transition planning minimizing disruption during implementation
- Scalability supporting practice growth without service degradation
According to research on revenue cycle management market trends, the sector continues evolving with technological advances and changing regulatory requirements. Partnering with service providers that invest in continuous improvement positions practices for long-term success.
When evaluating potential partners, request references from similar practices and investigate their experience with your specific payer mix. The healthcare RCM vendor landscape includes numerous providers, making thorough due diligence essential.
Implementation and Transition Management
Transitioning to outsourced revenue cycle management services requires careful planning to maintain cash flow continuity and prevent claim processing delays. Professional service providers follow structured implementation methodologies that minimize disruption while establishing efficient ongoing operations.
Step-by-step transition process:
- Conduct comprehensive assessment of current billing operations, identifying processes, systems, and performance baselines
- Develop detailed transition plan establishing timelines, responsibilities, and communication protocols
- Configure system access and security implementing appropriate permissions and ensuring HIPAA compliance
- Transfer knowledge and documentation providing service teams with payer contracts, fee schedules, and practice-specific requirements
- Execute parallel processing period running dual operations briefly to ensure accuracy before full transition
- Monitor performance metrics closely during the initial period, addressing issues quickly to prevent revenue disruption
- Establish ongoing communication cadence creating regular touchpoints for performance review and strategic planning
The transition period typically spans 30-90 days depending on practice size and complexity. During this time, maintaining open communication between clinical staff, administrative personnel, and RCM service teams ensures smooth workflow integration.
Professional service providers assign dedicated implementation specialists who guide practices through each phase, addressing concerns and adjusting processes based on early performance data. This structured approach minimizes the revenue cycle disruption that can occur during billing transitions.
Regional Considerations and Practice Location
While revenue cycle management processes follow standard frameworks, regional variations in payer mix, state regulations, and competitive dynamics require location-specific expertise. Practices benefit from working with service providers who understand regional healthcare markets and maintain relationships with local payers.
For example, medical billing services in California must navigate Medi-Cal requirements and the state's unique managed care environment. Similarly, medical billing coding in Arizona requires familiarity with AHCCCS and Arizona-specific commercial payer policies.
Regional expertise extends beyond simple geographic knowledge to understanding local provider communities, payer negotiation dynamics, and state regulatory requirements that impact billing operations. This localized knowledge complements national expertise to deliver optimal results.
Optimizing revenue cycle performance requires specialized expertise, dedicated resources, and continuous adaptation to regulatory and payer changes. By partnering with experienced professionals who understand the complete financial lifecycle of patient encounters, healthcare providers can improve cash flow, reduce administrative burdens, and focus resources on clinical excellence. Greenhive Billing Solutions delivers comprehensive revenue cycle management services tailored to healthcare providers across the United States, combining HIPAA-compliant operations with transparent communication and performance-focused processes designed to maximize reimbursements while streamlining practice operations.