The financial stability of healthcare organizations depends heavily on efficiently managing every stage of patient care billing, from initial registration through final payment collection. The healthcare revenue cycle management process represents the backbone of practice sustainability, encompassing all administrative and clinical functions that contribute to capturing, managing, and collecting patient service revenue. Understanding this complex process enables healthcare providers to optimize operations, reduce claim denials, and ensure consistent cash flow while maintaining compliance with evolving regulatory requirements.
Understanding the Healthcare Revenue Cycle Management Process
The healthcare revenue cycle management process begins the moment a patient schedules an appointment and continues until the practice receives full payment for services rendered. This comprehensive workflow integrates clinical documentation, accurate coding, timely claim submission, and persistent follow-up to maximize reimbursement.
Healthcare providers face mounting pressure to maintain financial viability while delivering quality care. The Healthcare Financial Management Association provides comprehensive resources that highlight how effective revenue cycle management directly impacts organizational sustainability. Every touchpoint in this process represents an opportunity to either enhance or hinder revenue capture.
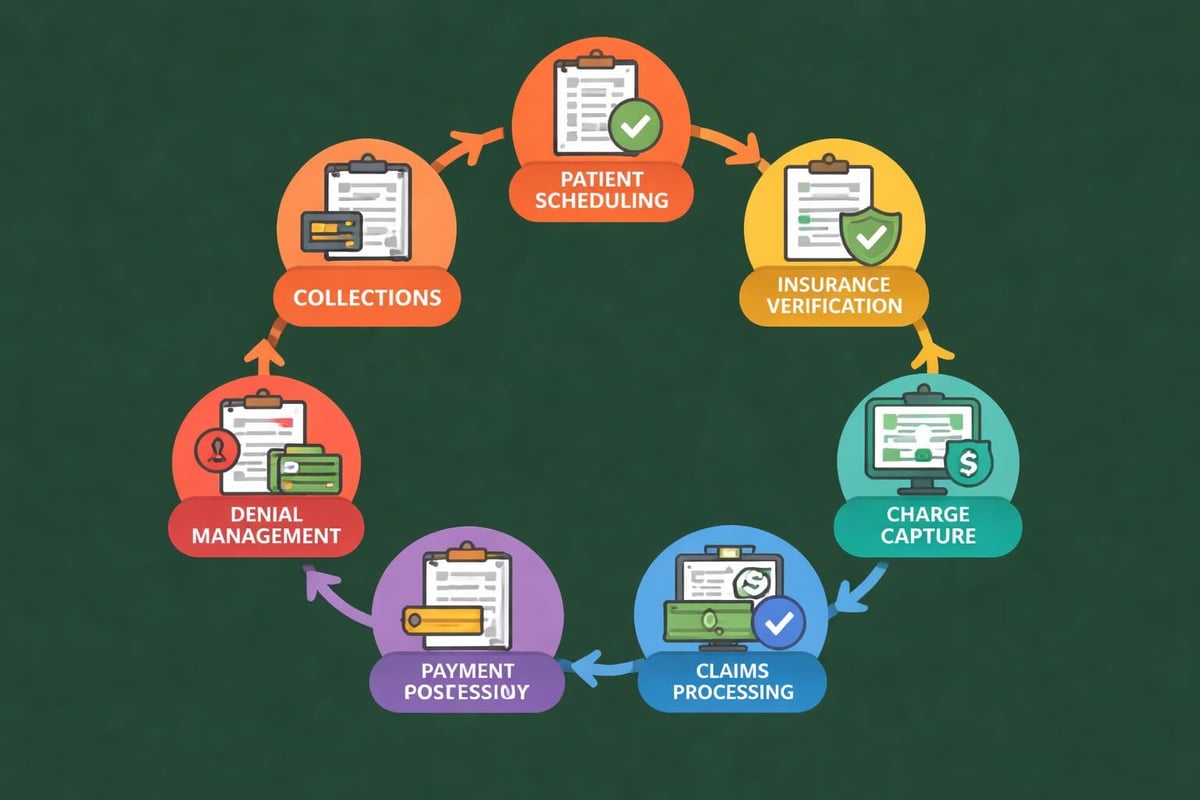
The cycle encompasses several critical phases:
- Pre-registration and scheduling
- Patient check-in and insurance verification
- Charge capture and medical coding
- Claims submission and adjudication
- Payment posting and reconciliation
- Denial management and appeals
- Patient billing and collections
Organizations that master these interconnected stages experience fewer billing errors, reduced days in accounts receivable, and improved patient satisfaction. Conversely, weaknesses at any single point can create bottlenecks that cascade throughout the entire revenue stream.
Front-End Revenue Cycle Components
Front-end processes establish the foundation for successful reimbursement. These patient-facing activities occur before or during the clinical encounter and directly influence downstream billing accuracy.
Patient Registration and Demographic Verification
Accurate patient information collection represents the first critical step in the healthcare revenue cycle management process. Registration staff must capture complete demographic data, including current addresses, contact information, and emergency contacts. Even minor errors at this stage can lead to claim rejections weeks later.
Essential registration elements include:
- Complete patient name with correct spelling
- Date of birth and Social Security number
- Current residential and mailing addresses
- Emergency contact information
- Primary care physician details
- Referring provider information when applicable
Healthcare practices that implement electronic registration systems often experience higher data accuracy rates compared to manual paper-based processes. These systems can incorporate validation rules that flag incomplete or inconsistent information before the patient encounter begins.
Insurance Eligibility and Benefits Verification
Verifying insurance coverage before service delivery prevents unexpected denials and reduces patient billing surprises. The eligibility verification process confirms active coverage, identifies patient financial responsibility, and determines authorization requirements.
| Verification Element | Information Obtained | Impact on Revenue |
|---|---|---|
| Coverage Status | Active/Inactive policy | Prevents service to uninsured patients |
| Benefits Level | Copay, deductible, coinsurance | Accurate patient estimates |
| Authorization Requirements | Prior approval needs | Avoids preventable denials |
| Network Status | In/out of network | Determines reimbursement rates |
Real-time eligibility verification has become standard practice for efficient organizations. This technology queries payer systems instantly, providing immediate confirmation of coverage details. Practices should verify benefits at scheduling and again at check-in to catch any coverage changes.
Prior Authorization Management
Many procedures, medications, and specialized services require payer approval before delivery. The prior authorization process involves submitting clinical documentation that justifies medical necessity according to payer criteria.
Delayed or denied authorizations directly impact both revenue timing and patient access to care. Organizations must track authorization status diligently, follow up on pending requests, and maintain systematic workflows that prevent services from occurring without required approvals.
Mid-Cycle Revenue Management Activities
Mid-cycle processes translate clinical services into billable charges and prepare claims for submission. Accuracy during these stages determines whether practices receive appropriate reimbursement for services rendered.
Charge Capture and Documentation
Providers must document all billable services comprehensively and submit charges promptly. Charge capture systems should integrate with electronic health records to automatically generate charges based on documented procedures and diagnoses.
Common charge capture challenges include:
- Missed charges – Services provided but not billed
- Delayed submissions – Charges entered days after service dates
- Incomplete documentation – Insufficient detail to support billing
- Code mismatches – Procedures not supported by documented diagnoses
Healthcare organizations lose significant revenue annually due to charge capture failures. Implementing systematic charge reconciliation processes helps identify and recover these missed opportunities before filing deadlines expire.
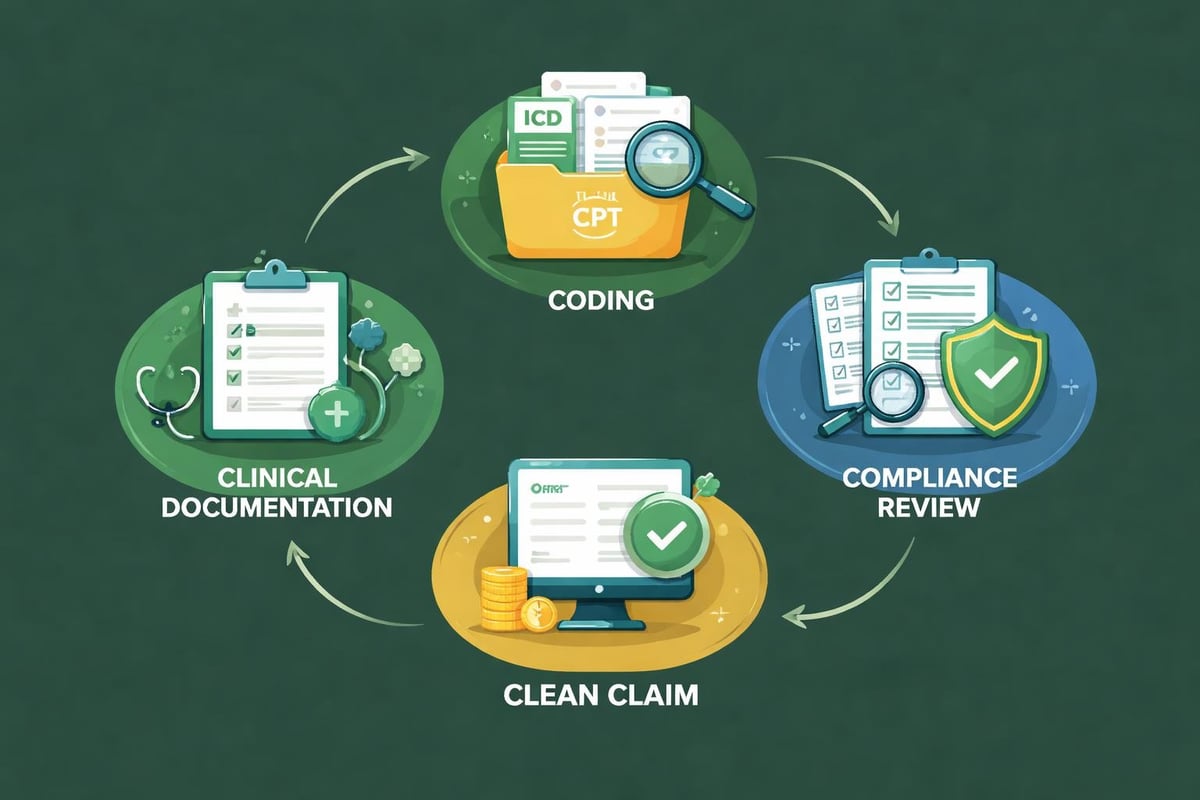
Medical Coding Excellence
Professional medical coders translate clinical documentation into standardized codes that payers recognize and reimburse. This critical function within the healthcare revenue cycle management process requires extensive knowledge of CPT, ICD-10, and HCPCS code sets along with payer-specific billing rules.
Medical coding services must ensure codes accurately reflect documented services while maximizing appropriate reimbursement. Coding errors represent a leading cause of claim denials and compliance risks.
Coding accuracy depends on:
- Complete and legible clinical documentation
- Current knowledge of annual code updates
- Understanding of payer coverage policies
- Appropriate modifier application
- Compliance with medical necessity requirements
Organizations should implement regular coding audits to identify patterns of errors and provide targeted education to both coders and providers. The comprehensive guide to revenue cycle management emphasizes how coding quality directly correlates with clean claim rates.
Claims Submission and Management
Timely and accurate claim submission ensures steady cash flow. The healthcare revenue cycle management process depends on electronic claims transmission to most payers, with careful attention to formatting requirements and submission deadlines.
Electronic Claims Processing
Electronic claim submission has largely replaced paper billing, offering faster processing times and immediate feedback on submission errors. Clearinghouses serve as intermediaries that scrub claims for common errors before transmission to payers.
Modern claim submission services incorporate real-time claim status tracking that provides visibility throughout the adjudication process. This transparency enables faster identification of issues and reduces days in accounts receivable.
| Submission Method | Processing Time | Error Detection | Cost Efficiency |
|---|---|---|---|
| Electronic (EDI) | 7-14 days | Immediate validation | High |
| Paper | 30-45 days | Manual review only | Low |
| Portal Entry | 14-21 days | Basic validation | Medium |
Healthcare practices should target clean claim rates above 95% to optimize revenue flow. Claims requiring rework consume staff time, delay payments, and increase the risk of timely filing denials.
Claims Adjudication Monitoring
After submission, payers review claims for coverage eligibility, coding accuracy, medical necessity, and contract compliance. This adjudication process results in payment, denial, or requests for additional information.
Proactive monitoring of claim status prevents aging receivables and identifies systematic issues requiring correction. Organizations should establish protocols for following up on claims that remain unpaid beyond expected timeframes.
Payment Posting and Reconciliation
Accurate payment posting maintains reliable accounts receivable records and identifies underpayments or overpayments requiring correction. This component of the healthcare revenue cycle management process requires detailed attention to remittance advice interpretation.
Electronic Remittance Advice Processing
Electronic Remittance Advice (ERA) files contain detailed payment information that explains how payers adjudicated each claim. Understanding what is ERA in medical billing enables efficient payment posting and variance analysis.
Payment posting services must reconcile payments against expected reimbursement, identify adjustment reasons, and flag discrepancies for review. This process reveals patterns such as consistent underpayment for specific codes or payers.
Key posting activities include:
- Matching payments to billed charges
- Recording contractual adjustments
- Identifying patient responsibility amounts
- Flagging short payments for follow-up
- Applying payments to correct patient accounts
Automation has transformed payment posting efficiency, with modern systems automatically applying electronic payments according to remittance details. However, human oversight remains essential for identifying anomalies and ensuring posting accuracy.
Contractual Adjustment Analysis
Understanding contractual adjustments in medical billing helps practices verify that payers reimburse according to negotiated contracts. These write-offs represent the difference between billed charges and contracted rates.
Regular contract compliance analysis identifies payers that consistently underpay or incorrectly apply contract terms. Organizations should maintain current fee schedules for all payers and systematically verify that payments align with contract provisions.

Denial Management and Appeals
Despite best efforts, claim denials occur regularly within the healthcare revenue cycle management process. Effective denial management strategies minimize revenue leakage and identify opportunities for process improvement.
Denial Root Cause Analysis
How denial management in medical billing improves cash flow begins with understanding why claims face rejection. Denials typically fall into preventable categories that systematic process improvements can address.
Common denial categories include:
- Registration errors – Incorrect patient demographics or insurance information
- Authorization failures – Missing or expired prior authorizations
- Coding issues – Incorrect codes or missing modifiers
- Medical necessity – Insufficient documentation to support service
- Timely filing – Claims submitted beyond payer deadlines
- Duplicate billing – Same service billed multiple times
- Coordination of benefits – Incorrect primary/secondary payer sequencing
Tracking denial patterns by category, payer, provider, and service type reveals systematic issues requiring targeted interventions. Organizations should calculate denial rates and establish benchmarks for acceptable performance levels.
Strategic Appeals Management
Denied claims with merit deserve systematic appeal efforts to recover appropriate reimbursement. The appeals process requires gathering supporting documentation, crafting persuasive arguments, and adhering to payer-specific appeal procedures and deadlines.
First-level appeals often involve simple claim corrections and resubmission. More complex denials may require detailed clinical documentation, medical necessity justification, or contract interpretation arguments. Practices must weigh the cost of appeal efforts against potential recovery amounts when prioritizing work.
Successful denial management incorporates feedback loops that translate denial patterns into front-end process improvements. Resources such as the seven steps of revenue cycle management emphasize this continuous improvement approach.
Patient Financial Responsibility and Collections
Increasing patient financial responsibility through high-deductible health plans has elevated the importance of patient collections within the healthcare revenue cycle management process. Organizations must balance compassionate patient interactions with necessary revenue collection.
Point-of-Service Collections
Collecting patient payments at the time of service significantly improves collection rates compared to billing after care delivery. Practices should provide accurate cost estimates during scheduling and verification, then collect copays, deductibles, and estimated patient portions at check-in.
Effective point-of-service collection requires:
- Accurate benefit verification providing reliable estimates
- Staff training on professional payment discussions
- Multiple payment options including cards and payment plans
- Clear financial policies communicated before service
- Technology supporting secure payment processing
Patient-friendly payment options such as automated payment plans can improve collection rates while maintaining positive patient relationships. Transparency about costs before services renders helps patients plan financially and reduces surprise billing complaints.
Patient Statement Management
When balances remain after insurance processing, clear and timely patient statements facilitate payment. Statements should clearly explain services rendered, insurance payments applied, and remaining patient responsibility.
The healthcare revenue cycle management process includes systematic statement generation cycles with appropriate follow-up intervals. Practices typically send multiple statements at 30-day intervals before escalating collection efforts.
Modern patient portals enable patients to view balances, review explanation of benefits, and make payments online at their convenience. These self-service tools reduce administrative burden while improving patient satisfaction and payment speed.
Technology and Automation in Revenue Cycle Operations
Technology transformation has fundamentally changed how organizations execute the healthcare revenue cycle management process. Automation eliminates manual tasks, reduces errors, and provides real-time visibility into performance metrics.
Practice Management and Billing Systems
Integrated practice management systems serve as the operational hub for revenue cycle activities. These platforms manage scheduling, registration, charge capture, claim submission, payment posting, and reporting within unified databases.
While specialized revenue cycle management companies like Greenhive Billing Solutions don't provide software products, experienced teams work seamlessly with client-owned systems and adapt to existing technology platforms. This flexibility ensures practices benefit from expert revenue cycle management without requiring system changes.
Analytics and Performance Monitoring
Reporting and analytics capabilities transform raw data into actionable insights that guide operational improvements. Key performance indicators provide objective measures of revenue cycle health.
| Metric | Benchmark Target | Significance |
|---|---|---|
| Clean Claim Rate | >95% | First-pass acceptance without rework |
| Days in A/R | <40 days | Speed of payment collection |
| Denial Rate | <5% | Claim quality and accuracy |
| Collection Rate | >95% | Effectiveness of total collections |
| Cost to Collect | <3% of collections | Operational efficiency |
Regular performance monitoring identifies trends requiring attention before they significantly impact cash flow. Organizations should establish dashboards that provide real-time visibility into critical metrics.
Compliance and Regulatory Considerations
The healthcare revenue cycle management process operates within a complex regulatory environment requiring strict compliance with federal and state requirements. Organizations must balance revenue optimization with adherence to billing regulations and privacy protections.
HIPAA Compliance in Revenue Cycle Operations
Protected health information flows throughout revenue cycle processes, requiring robust safeguards to prevent unauthorized disclosure. Staff handling patient data must receive regular HIPAA training and follow established protocols for secure information handling.
The importance of compliance and auditing in revenue cycle management cannot be overstated. Organizations face significant penalties for privacy breaches, making comprehensive compliance programs essential.
Fraud and Abuse Prevention
Billing practices must comply with False Claims Act provisions and anti-kickback statutes. Regular internal audits help identify unintentional billing errors before they attract regulatory scrutiny or qui tam actions.
Compliance program elements include:
- Written policies and procedures
- Regular coding and billing audits
- Staff education and training
- Monitoring and reporting systems
- Response and correction protocols
- Open lines of communication for concerns
Partnering with experienced revenue cycle management providers ensures access to compliance expertise and systematic audit processes that protect organizational integrity.
Optimizing Revenue Cycle Performance
Continuous improvement mindsets separate high-performing organizations from those struggling with revenue cycle challenges. The healthcare revenue cycle management process benefits from systematic evaluation and strategic enhancement initiatives.
Staff Training and Development
Revenue cycle staff require ongoing education to maintain current knowledge of coding updates, payer policy changes, and regulatory requirements. Investment in professional development pays dividends through improved accuracy and efficiency.
Organizations should provide both formal training programs and regular updates on specific topics. Cross-training staff across multiple revenue cycle functions builds operational resilience and deepens understanding of how individual roles impact overall performance.
Process Standardization
Standardized workflows reduce variation and ensure consistent execution of revenue cycle tasks. Documented procedures provide reference materials for staff and establish accountability standards.
Organizations should regularly review and update standard operating procedures to incorporate best practices and lessons learned from denial analysis and performance metrics. Best practices in healthcare revenue cycle management emphasize systematic process documentation and adherence.
Outsourcing Strategic Partnerships
Many healthcare organizations partner with specialized revenue cycle management companies to access expertise, technology, and economies of scale unavailable internally. These partnerships enable providers to focus on clinical care while ensuring professional management of complex billing operations.
When evaluating outsourcing options, practices should consider provider experience in their specific specialty, technology capabilities, reporting transparency, and cultural fit. Successful partnerships involve collaborative relationships with aligned incentives focused on maximizing appropriate reimbursement.
Specialty-Specific Revenue Cycle Considerations
Different medical specialties face unique revenue cycle challenges requiring tailored approaches. Understanding specialty-specific requirements ensures optimal reimbursement for specialized services.
High-Volume Versus Complex Billing
Primary care practices typically process high volumes of relatively straightforward claims with standard evaluation and management codes. Surgical specialties face more complex coding with procedure combinations, modifiers, and global period considerations.
Specialty-specific expertise proves essential for complex billing scenarios. For example, cardiology medical billing requires understanding of cardiac procedure bundling rules and appropriate modifier application for distinct procedural services.
Value-Based Care Impact
The shift toward value-based reimbursement models adds complexity to the healthcare revenue cycle management process. Organizations participating in quality programs must track additional metrics, submit supplementary data, and manage performance-based payment adjustments.
Revenue cycle teams need visibility into quality measure performance to understand how these programs impact total reimbursement. Integration between clinical quality systems and billing platforms facilitates this comprehensive financial view.
Mastering the healthcare revenue cycle management process requires sustained attention to detail, continuous process improvement, and strategic use of technology and expertise. Organizations that excel across all revenue cycle stages experience improved cash flow, reduced administrative burden, and enhanced ability to focus on quality patient care. Greenhive Billing Solutions provides comprehensive revenue cycle management services that help healthcare providers optimize every stage of the billing process, from initial patient registration through final payment collection, ensuring maximum appropriate reimbursement while maintaining full regulatory compliance.

