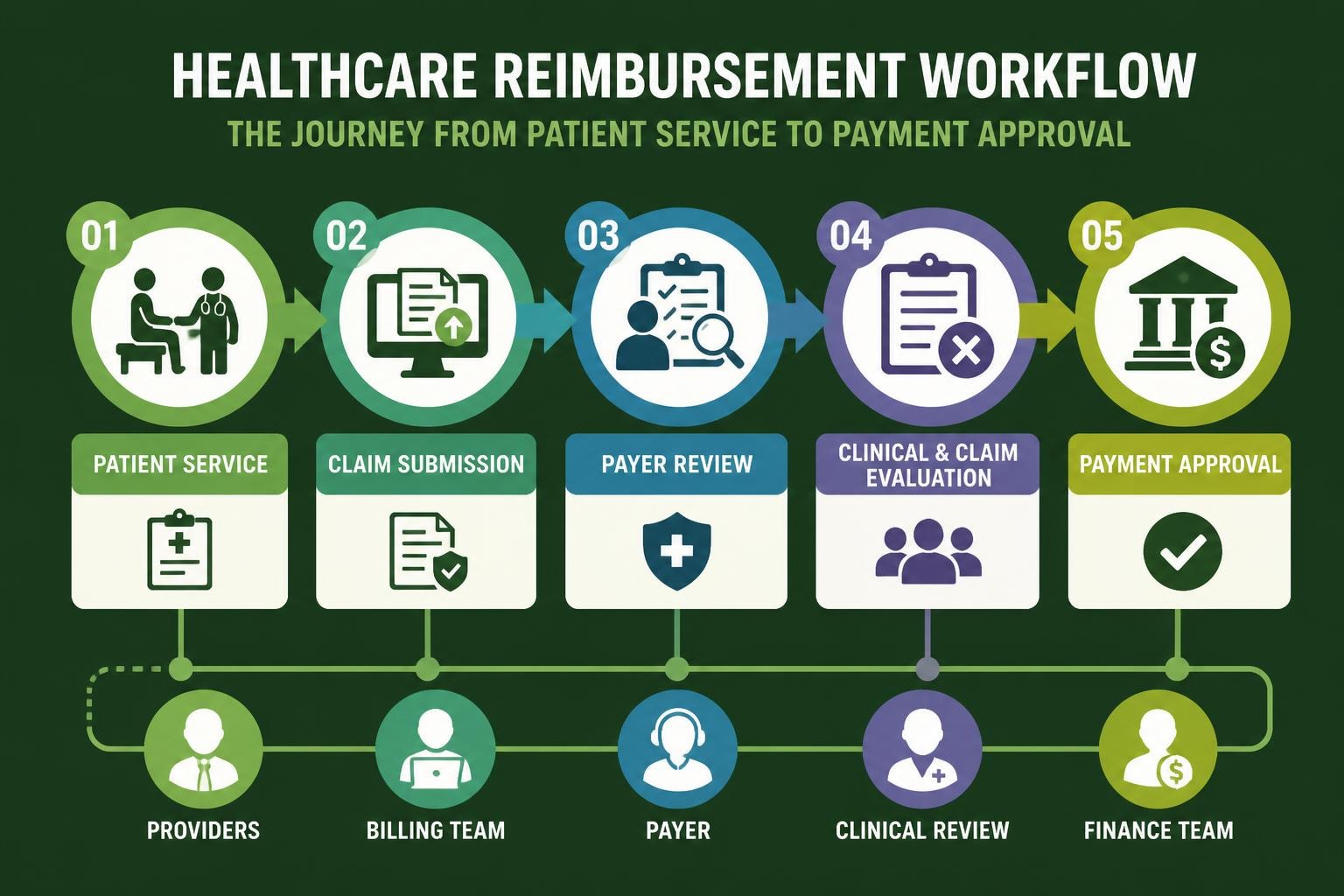
Understanding reimbursement medical processes is fundamental to maintaining a healthy revenue cycle for healthcare providers across the United States. The complexity of medical reimbursement continues to evolve as payers refine their policies, introduce new payment models, and adjust their requirements for claim submission and documentation. Healthcare practices that master these intricacies position themselves for sustainable financial success, while those that struggle often face mounting denials, delayed payments, and revenue leakage that threatens their operational viability.
Understanding Reimbursement Medical Frameworks
Reimbursement medical systems operate on the principle that healthcare providers deliver services to patients and subsequently receive payment from insurance companies, government programs, or patients themselves. This payment structure involves multiple stakeholders, each with specific requirements and expectations that must be met for successful reimbursement.
The foundation of effective reimbursement medical management begins with understanding the various payment methodologies employed by different payers. Fee-for-service models compensate providers based on individual services rendered, while value-based care arrangements tie reimbursement to quality metrics and patient outcomes. Bundled payment models combine multiple services into a single reimbursement amount, requiring careful allocation and documentation.
Major payers like Anthem outline reimbursement policies that serve as the basis for payment determinations under members' benefit plans. These policies establish the framework within which claims are evaluated, processed, and paid.
Key Components of Medical Reimbursement
Proper documentation forms the cornerstone of successful reimbursement medical outcomes. Without comprehensive clinical documentation that supports the medical necessity of services provided, even correctly coded claims face denial or downcoding. Providers must ensure that every service billed is supported by clear, detailed documentation in the patient's medical record.
The reimbursement process involves several critical elements:
- Accurate coding: Proper assignment of CPT, ICD-10, and HCPCS codes that reflect services provided
- Medical necessity: Documentation that demonstrates why services were clinically appropriate
- Payer-specific requirements: Adherence to individual payer policies and coverage guidelines
- Timely filing: Submission within payer-specified timeframes to avoid automatic denials
- Clean claim submission: Error-free claims that contain all required information
Healthcare organizations leveraging comprehensive medical billing services benefit from expertise in navigating these multifaceted requirements, ensuring that claims are positioned for successful reimbursement from the outset.
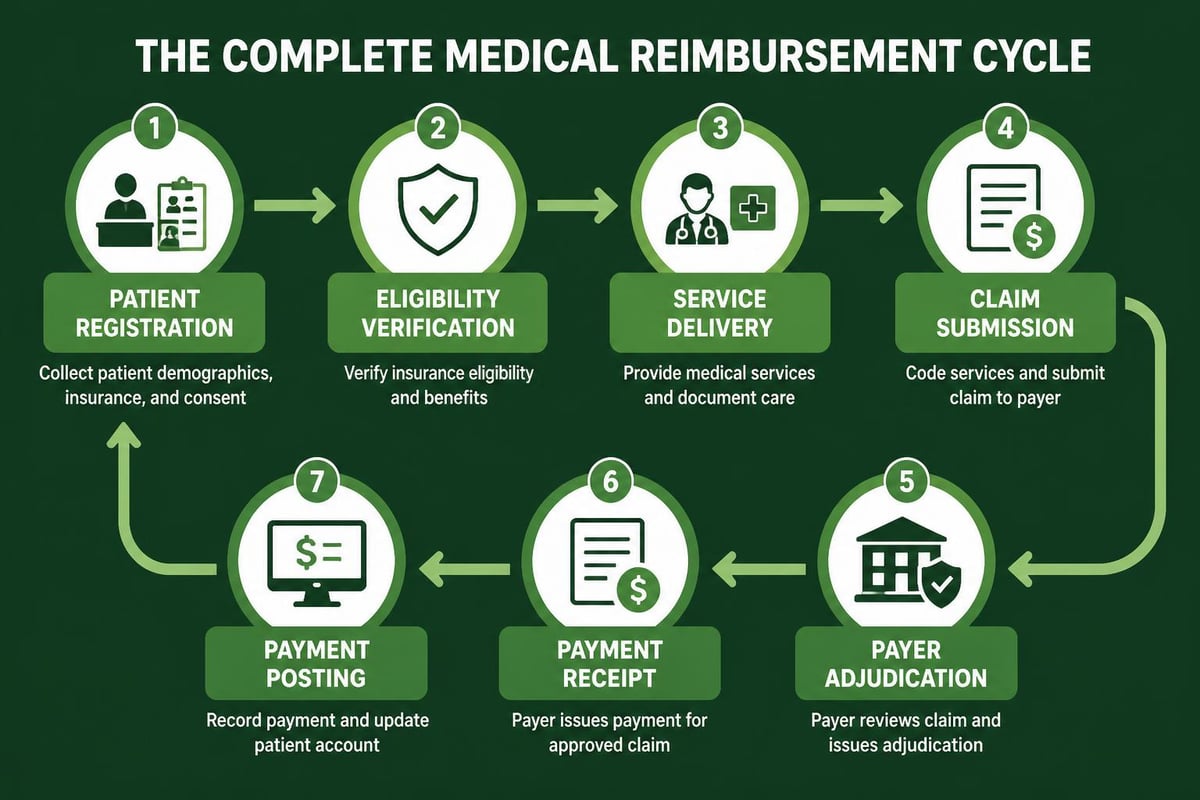
Navigating Payer-Specific Reimbursement Policies
Each insurance carrier maintains distinct reimbursement medical policies that govern how claims are processed and paid. Understanding these variations is essential for maximizing reimbursement and minimizing denials. National payers may have state-specific policy variations, while regional carriers often implement unique requirements.
Select Health’s medical coding and reimbursement policies demonstrate how payers base their guidelines on standards from CMS, CPT editorial panels, and specialty societies. These policies cover everything from basic office visits to complex surgical procedures, each with specific documentation and coding requirements.
State-Specific Variations
Reimbursement medical requirements often vary significantly by state, particularly for workers' compensation and state-funded programs. Texas medical reimbursement policies provide detailed guidelines for maximum allowable reimbursement within their workers' compensation system, establishing specific fee schedules and documentation requirements.
Providers operating in multiple states must maintain awareness of these jurisdictional differences to ensure compliant billing practices. State-specific variations may include:
- Different fee schedules: Maximum reimbursement amounts that vary by geographic location
- Unique documentation requirements: State-mandated forms or attestations
- Specific coding guidelines: State-level modifications to national coding standards
- Prior authorization thresholds: Varying dollar amounts or service types requiring pre-approval
- Appeals processes: State-specific procedures for contesting claim denials
Optimizing Claims for Maximum Reimbursement
Strategic approaches to claim submission significantly impact reimbursement medical outcomes. Providers who implement systematic quality assurance processes before claim submission experience substantially lower denial rates and faster payment cycles.
Eligibility verification services play a crucial role in preventing claim denials by confirming patient coverage, benefits, and authorization requirements before services are rendered. This proactive approach eliminates a major source of claim rejections and reduces administrative burden.
Pre-Submission Quality Checks
| Quality Check Area | Key Verification Points | Impact on Reimbursement |
|---|---|---|
| Patient Demographics | Name, DOB, policy number accuracy | Prevents identification mismatches |
| Coverage Verification | Active policy, benefit eligibility | Avoids non-covered service denials |
| Coding Accuracy | Proper CPT/ICD-10 linkage | Ensures medical necessity support |
| Modifier Application | Appropriate use of billing modifiers | Prevents bundling or duplicate denials |
| Documentation Review | Complete clinical notes | Supports medical necessity on audit |
Implementing comprehensive medical claim submission services that incorporate these quality checks ensures claims are clean before they reach the payer, dramatically improving first-pass acceptance rates.
Leveraging Technology for Reimbursement Success
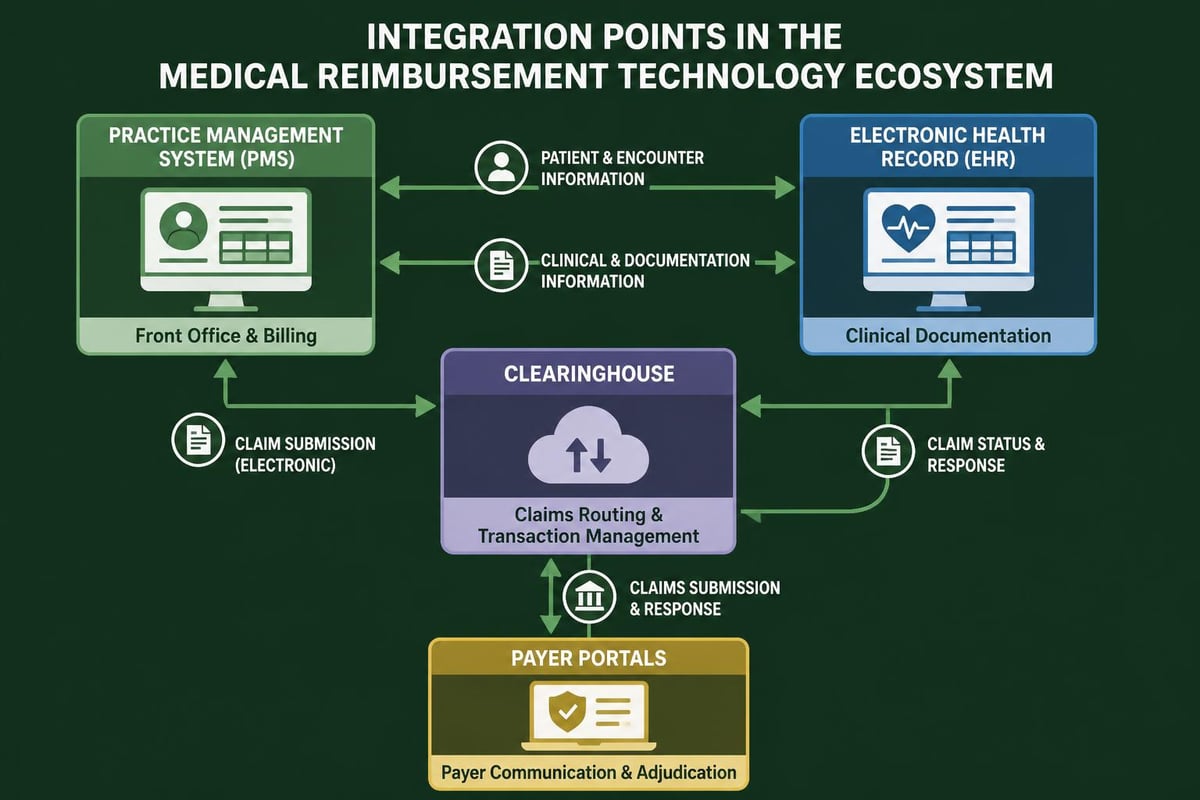
Modern revenue cycle management relies heavily on technology solutions that streamline reimbursement medical processes. Electronic claim submission, automated eligibility verification, and real-time claim status tracking have transformed how providers manage their revenue cycles.
Advanced clearinghouses provide claim scrubbing capabilities that identify errors before submission, reducing rejections and accelerating payment timelines. These systems check claims against thousands of payer-specific edits, ensuring compliance with individual carrier requirements.
Practice management and electronic health record systems must be properly configured with current fee schedules, payer contracts, and coding guidelines. Regular updates to these systems prevent reimbursement errors caused by outdated information.
Managing Denials to Protect Revenue
Even with optimal claim submission practices, reimbursement medical denials occur. How providers respond to these denials determines whether revenue is recovered or lost. Denial management requires systematic tracking, root cause analysis, and strategic appeals.
Denial management services provide specialized expertise in identifying denial patterns, developing corrective action plans, and executing effective appeals. These services recover revenue that would otherwise be written off while implementing preventive measures to reduce future denials.
Common Reimbursement Denial Categories
Understanding why denials occur enables targeted prevention strategies:
- Technical denials: Missing information, incorrect patient data, or invalid codes
- Authorization denials: Services requiring pre-authorization that was not obtained
- Medical necessity denials: Insufficient documentation to support service appropriateness
- Timely filing denials: Claims submitted after payer deadline
- Duplicate billing denials: Services appearing to be billed multiple times
- Coordination of benefits issues: Primary/secondary payer sequence errors
Each denial category requires specific corrective actions and prevention strategies. Technical denials often stem from front-end registration issues, while medical necessity denials indicate documentation improvement opportunities.
Documentation Excellence for Sustainable Reimbursement
The relationship between clinical documentation and reimbursement medical outcomes cannot be overstated. Payers increasingly scrutinize claims through prepayment audits, retrospective reviews, and medical necessity evaluations. Documentation that clearly establishes the clinical rationale for services protects reimbursement during these reviews.
Physicians and clinical staff must understand that documentation serves dual purposes: clinical communication and reimbursement support. Every service billed should have corresponding documentation that answers three fundamental questions:
- What service was provided? Detailed description of procedures, examinations, or interventions
- Why was the service necessary? Clinical indications and medical decision-making
- What was the outcome? Results, patient response, and follow-up plan
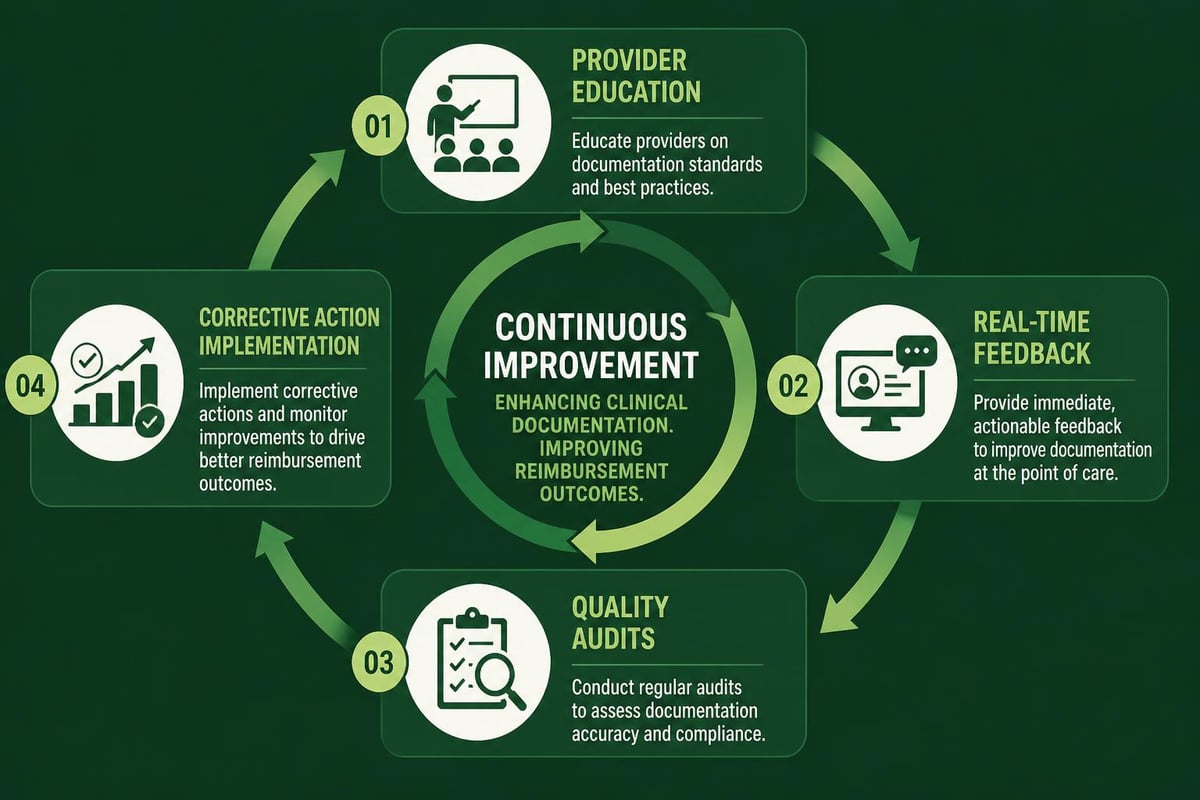
Provider Education and Compliance
Ongoing education ensures clinical staff understand reimbursement medical requirements and documentation standards. Regular training sessions should address:
| Training Topic | Frequency | Participants |
|---|---|---|
| Coding updates | Quarterly | Physicians, coders, billers |
| Payer policy changes | As released | Billing staff, clinical leadership |
| Documentation standards | Biannually | All providers |
| Compliance requirements | Annually | Entire revenue cycle team |
| Audit findings review | As needed | Affected departments |
Organizations that invest in comprehensive medical coding services benefit from certified professionals who stay current with evolving requirements and ensure coding accuracy that supports optimal reimbursement.
Contract Negotiation and Fee Schedule Management
Reimbursement medical rates are ultimately determined by contractual agreements between providers and payers. Effective contract negotiation directly impacts the revenue potential of every claim submitted under that agreement. Providers must approach contract negotiations strategically, armed with data on current reimbursement rates, service volume, and market benchmarks.
Understanding reimbursement methodologies within contracts is essential. Some payers reimburse based on a percentage of Medicare rates, while others use proprietary fee schedules or negotiated rate tables. The methodology significantly affects overall reimbursement levels and should be carefully evaluated during contract review.
Key Contract Elements Affecting Reimbursement
- Base rate structure: The fundamental payment amounts for services
- Annual rate increases: Provisions for inflation adjustments or performance-based increases
- Carve-outs: Services excluded from standard rate structures
- Outlier provisions: Additional payment mechanisms for unusually complex cases
- Stop-loss protections: Limits on provider financial exposure in bundled arrangements
- Clean claim definitions: Criteria determining when claims must be paid
- Dispute resolution: Processes for addressing reimbursement disagreements
Providers should maintain detailed records of reimbursement rates across all payers, enabling data-driven contract negotiations and identification of unfavorable agreements requiring renegotiation.
Compliance Considerations in Medical Reimbursement
Reimbursement medical activities must adhere to numerous federal and state regulations governing billing practices, documentation, and claim submission. Violations of these requirements can result in penalties, payment recoupment, or exclusion from government programs.
The False Claims Act imposes severe penalties for knowingly submitting fraudulent claims or causing improper payments from federal healthcare programs. Even unintentional errors, if systematic and significant, can trigger investigations and financial liability. Providers must implement compliance programs that prevent, detect, and correct billing errors.
Medical coding audit services provide objective assessment of coding accuracy and compliance with regulatory requirements. Regular internal audits identify risk areas before external reviewers discover them, enabling corrective action that protects reimbursement and reduces liability.
Essential Compliance Program Elements
- Written policies and procedures: Documented standards for all billing and coding activities
- Designated compliance officer: Individual responsible for oversight and coordination
- Regular training and education: Ongoing instruction on compliance requirements
- Internal monitoring and auditing: Systematic evaluation of billing practices
- Response and correction protocols: Procedures for addressing identified issues
- Open communication channels: Mechanisms for reporting potential compliance concerns
- Disciplinary guidelines: Consequences for compliance violations
Advanced Reimbursement Strategies for Specialty Practices
Different medical specialties face unique reimbursement medical challenges based on their service mix, payer relationships, and documentation requirements. Specialty-specific strategies optimize reimbursement while ensuring compliance with applicable guidelines.
Surgical specialties must navigate global period rules, modifier application for multiple procedures, and appropriate unbundling of distinct services. Medical specialties often deal with complex evaluation and management coding, chronic care management billing, and coordination of care documentation.
Understanding payer policies specific to your specialty is critical. Highmark’s reimbursement policies address claims reimbursement logic with guidelines applicable across markets but note important state-specific variations that specialty practices must understand.
Specialty-Specific Billing Considerations
| Specialty | Primary Challenges | Optimization Strategies |
|---|---|---|
| Cardiology | Complex device coding, multiple procedures | Detailed operative reports, modifier expertise |
| Orthopedics | Global periods, hardware billing | Surgery-specific documentation, implant tracking |
| Primary Care | E/M coding complexity, preventive services | Time documentation, comprehensive history |
| Radiology | Technical/professional component splits | Clear ordering documentation, medical necessity |
| Anesthesia | Time-based billing, modifiers | Accurate time tracking, concurrent case documentation |
Practices serving specialized patient populations benefit from partnering with revenue cycle management providers who understand their unique requirements and maintain expertise in specialty-specific reimbursement medical policies.
Revenue Cycle Analytics and Performance Monitoring
Data-driven decision making has become essential for optimizing reimbursement medical outcomes. Providers must track key performance indicators that reveal revenue cycle health and identify improvement opportunities.
Essential metrics for monitoring reimbursement performance include:
- Days in accounts receivable: Average time from service to payment
- First-pass claim acceptance rate: Percentage of claims paid without rework
- Denial rate: Percentage of claims initially denied
- Net collection rate: Actual collections compared to expected reimbursement
- Adjustment rate: Write-offs as percentage of gross charges
- Appeal success rate: Percentage of denied claims successfully overturned
Reporting and analytics capabilities transform raw billing data into actionable insights that drive revenue improvement. Regular review of these metrics enables proactive identification of issues before they significantly impact cash flow.
Benchmarking Against Industry Standards
Comparing your practice's reimbursement medical performance against industry benchmarks provides context for evaluation and goal-setting. While benchmarks vary by specialty, practice size, and geographic location, general targets include:
- First-pass acceptance rate above 95%
- Denial rate below 5-8%
- Days in AR under 40 days
- Net collection rate above 95%
- Bad debt write-offs under 2%
Practices falling short of these benchmarks should conduct root cause analysis to identify specific areas requiring improvement, whether in front-end processes, coding accuracy, or denial management.
The Role of Prior Authorization in Reimbursement
Prior authorization requirements have proliferated across payers, creating administrative burden while serving as a gatekeeper for reimbursement medical approvals. Services performed without required authorization typically face automatic denial, making authorization management critical to revenue protection.
Prior authorization services streamline this complex process by tracking requirements across multiple payers, submitting authorization requests with supporting documentation, and monitoring approval status. These specialized services prevent authorization-related denials while reducing administrative burden on clinical staff.
The authorization process requires meticulous attention to detail. Requests must include all payer-required information, supporting clinical documentation, and accurate coding of proposed services. Incomplete authorization requests delay approvals and may result in service postponement or denial.
Providers should maintain comprehensive tracking systems that identify which services require authorization for each payer, monitor pending authorization requests, and ensure authorizations are obtained before services are scheduled. This proactive approach eliminates a major source of preventable denials.
Navigating the complexities of reimbursement medical processes requires expertise, attention to detail, and systematic management of every revenue cycle component. Healthcare providers who master these elements position themselves for financial sustainability and growth in an increasingly challenging reimbursement environment. Greenhive Billing Solutions delivers comprehensive revenue cycle management services that optimize reimbursement outcomes through expert claim submission, denial management, and compliance oversight, enabling healthcare providers to focus on patient care while maximizing their financial performance.