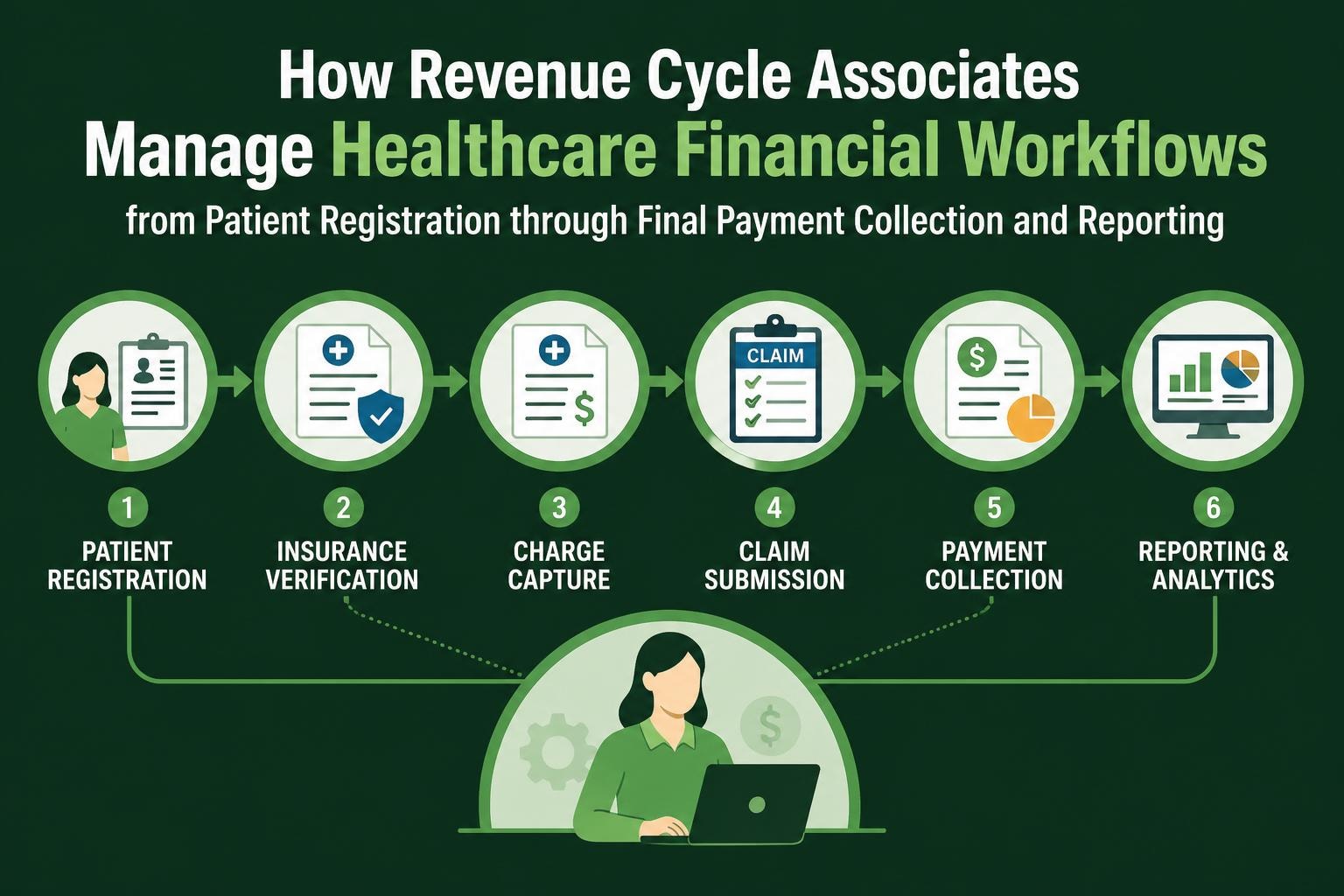
Revenue cycle associates represent the operational backbone of healthcare financial management, executing critical tasks that transform clinical services into collected revenue. These professionals work across multiple touchpoints in the billing lifecycle, from patient registration and insurance verification through claims submission, payment posting, and denial resolution. Their expertise directly influences cash flow velocity, collection rates, and overall financial health for medical practices, hospitals, and healthcare systems nationwide.
Understanding the Core Functions of Revenue Cycle Associates
Revenue cycle associates perform specialized duties that require both technical knowledge and analytical skills. These professionals handle the detailed work of medical billing, coding verification, and accounts receivable management that keeps revenue flowing consistently.
Patient Registration and Data Accuracy
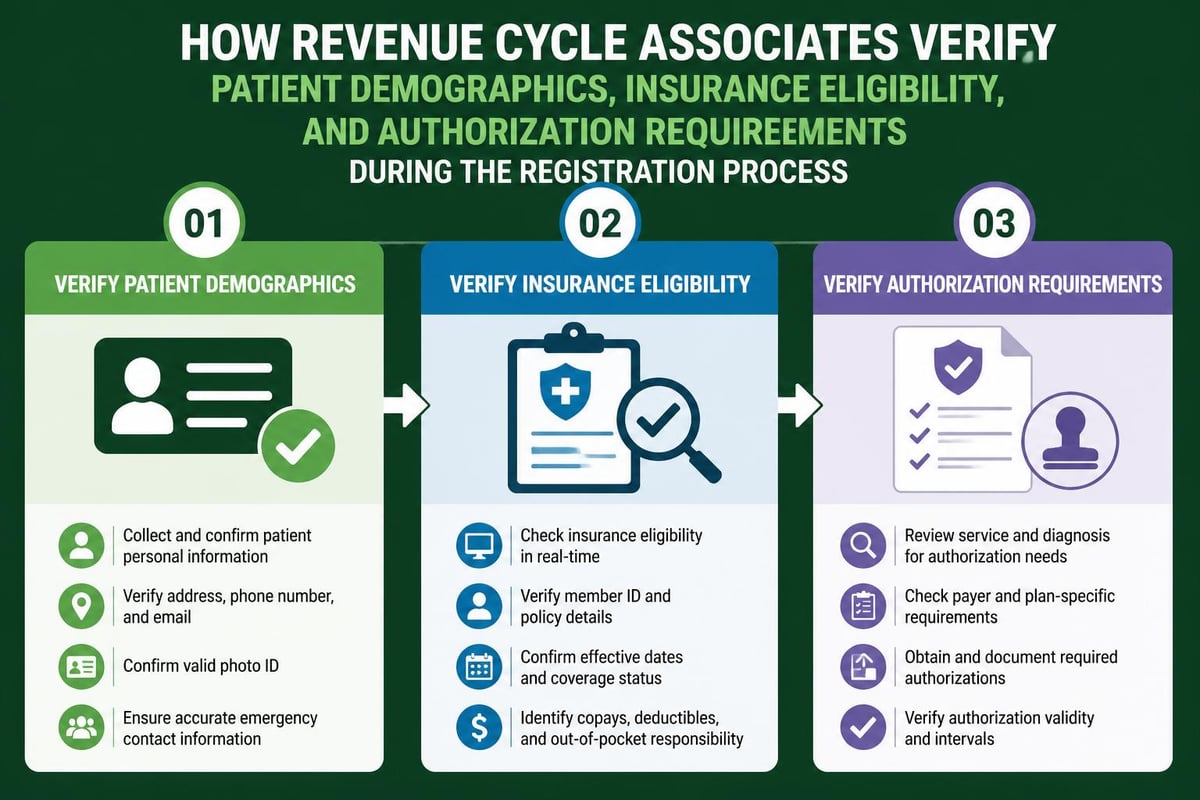
The revenue cycle begins with accurate patient information collection. Revenue cycle associates verify demographic details, insurance coverage, and eligibility status during the registration phase. This foundational work prevents downstream claim denials caused by incorrect patient identifiers, inactive insurance policies, or missing authorization requirements.
Data accuracy at this stage reduces claim rejection rates by 30-40% according to industry benchmarks. Associates cross-reference patient information against insurance databases, confirm coverage effective dates, and document any secondary or tertiary insurance policies. This thorough verification process establishes clean claims from the outset.
Claims Processing and Submission
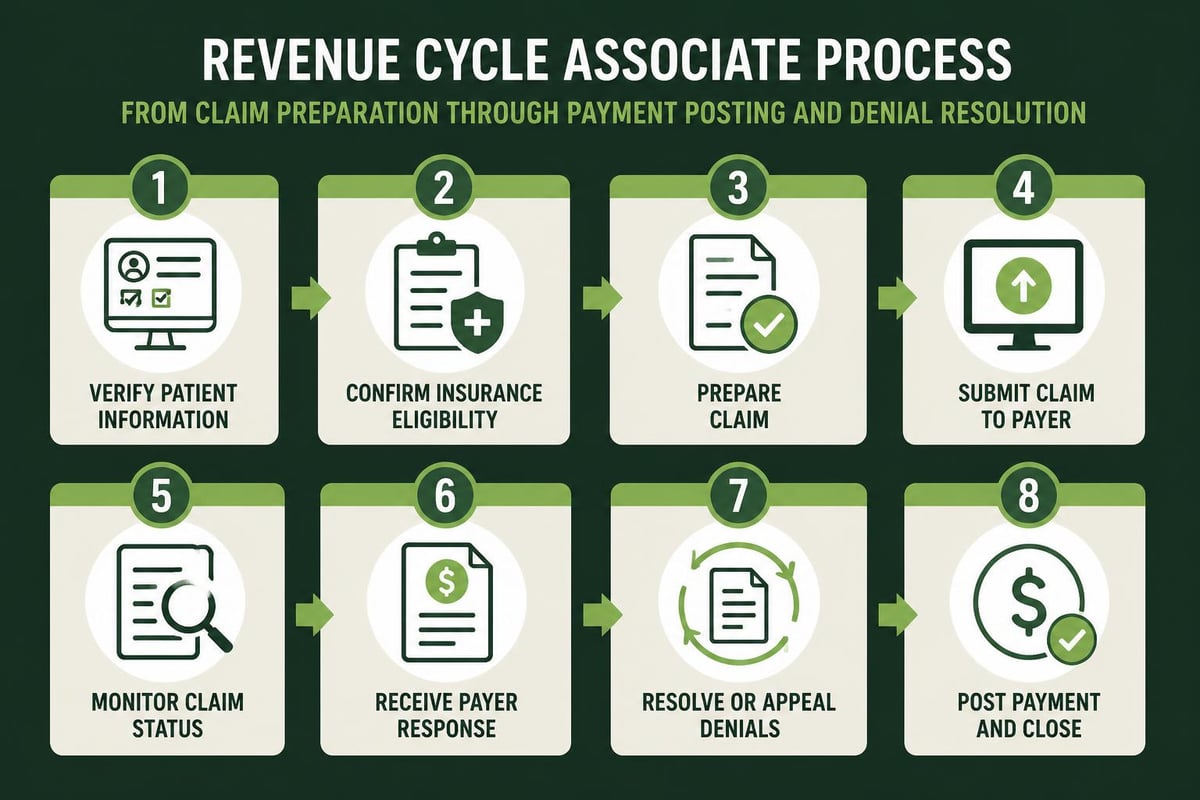
Revenue cycle associates prepare and submit claims to insurance payers following strict compliance protocols. They review charge capture documentation, validate procedure codes against diagnosis codes, and ensure modifier usage follows payer-specific guidelines. Each claim undergoes quality checks before electronic submission.
Key responsibilities in claims processing include:
- Reviewing superbills and charge tickets for completeness
- Assigning appropriate CPT and ICD-10 codes
- Applying modifiers to prevent bundling or incorrect reimbursement
- Scrubbing claims through automated editing software
- Transmitting claims via clearinghouses or direct payer portals
- Tracking claim status and following up on pending submissions
Associates monitor submission deadlines carefully, as timely filing limits vary by payer and can range from 90 days to one year from the date of service. Missing these deadlines results in automatic claim denials and lost revenue that cannot be recovered.
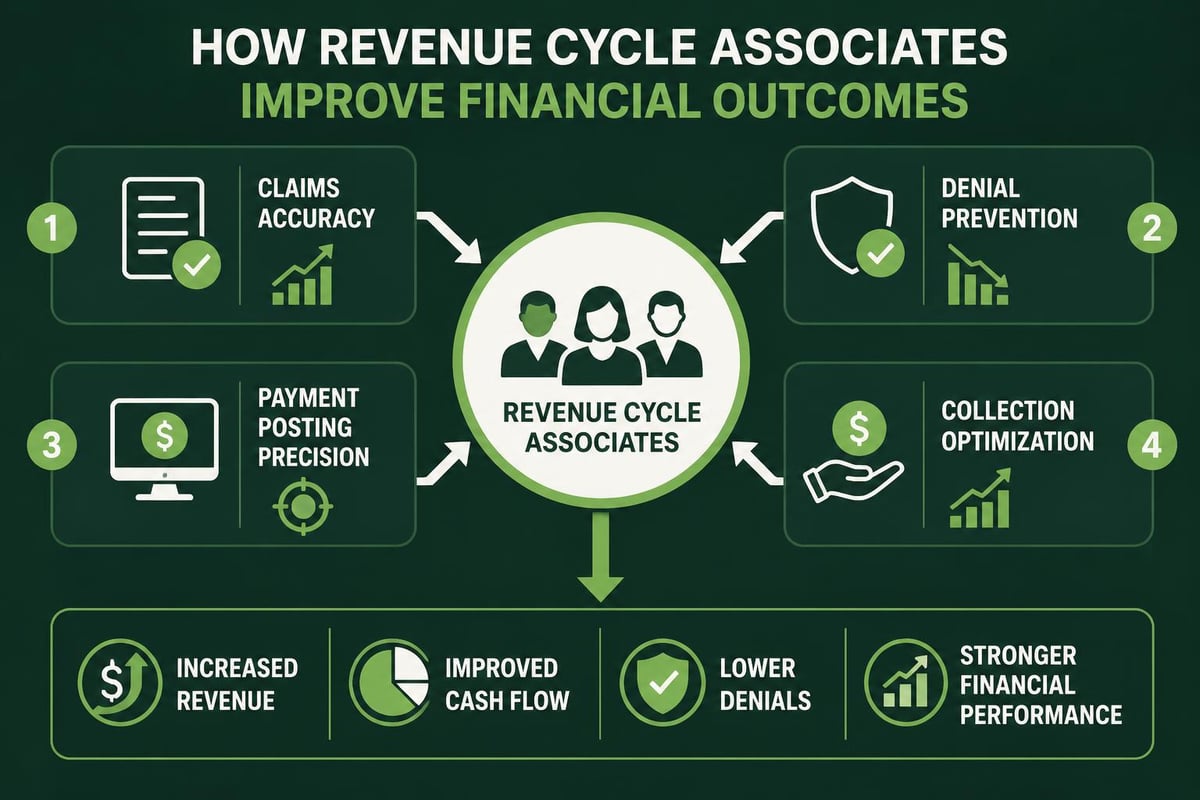
The Strategic Impact of Revenue Cycle Associates on Financial Performance
Beyond transactional tasks, revenue cycle associates contribute strategic value through performance monitoring, problem identification, and process improvement. Their daily work generates insights that inform broader revenue cycle optimization initiatives.
Denial Management and Appeals
When claims face denials or rejections, revenue cycle associates serve as the first line of response. They analyze denial reasons, categorize issues by root cause, and determine appropriate next steps. Common denial categories include:
| Denial Type | Common Causes | Resolution Approach |
|---|---|---|
| Registration Errors | Incorrect patient information, inactive insurance | Correct data and resubmit |
| Authorization Issues | Missing pre-authorization, expired authorization | Obtain authorization retroactively or appeal |
| Coding Problems | Unbundling, lack of medical necessity | Review documentation, add modifiers, appeal with clinical notes |
| Timely Filing | Missed submission deadlines | Appeal with proof of timely submission or write off |
| Duplicate Claims | Multiple submissions for same service | Void duplicate and confirm single payment |
Revenue cycle associates who excel at denial management in medical billing recover 60-70% of initially denied claims through systematic appeals and resubmission processes. This recovery work directly protects practice revenue and improves net collection rates.
Payment Posting and Reconciliation
Accurate payment posting ensures financial records reflect actual cash collected. Revenue cycle associates post payments from insurance remittances, patient payments, and electronic fund transfers while applying contractual adjustments correctly.
This detailed work requires associates to:
- Match payments to specific claims and charges
- Apply contractual write-offs per fee schedule agreements
- Identify underpayments or incorrect reimbursement amounts
- Post patient responsibility amounts for secondary billing
- Flag discrepancies for investigation
Understanding healthcare revenue cycle analytics helps associates identify payment patterns, payer-specific issues, and opportunities for contract renegotiation based on reimbursement trends.
Essential Skills and Qualifications for Revenue Cycle Associates
Successful revenue cycle associates combine technical proficiency with problem-solving abilities and attention to detail. Healthcare organizations seek candidates with specific competencies that enable high performance in this demanding role.
Technical Knowledge Requirements
Medical billing knowledge forms the foundation of revenue cycle work. Associates must understand CPT coding, ICD-10 diagnosis coding, HCPCS codes, and modifier application. Familiarity with different types of medical coding enables associates to spot coding errors before claim submission.
Additionally, revenue cycle associates need working knowledge of:
- Insurance verification procedures and eligibility systems
- Claims submission platforms and clearinghouse operations
- Electronic remittance advice (ERA) and explanation of benefits (EOB) interpretation
- Practice management and billing software systems
- HIPAA privacy and security regulations
- Payer-specific billing requirements and policies
Many healthcare employers prefer candidates with certifications such as Certified Revenue Cycle Representative (CRCR), Certified Professional Biller (CPB), or Certified Medical Reimbursement Specialist (CMRS). These credentials demonstrate commitment to professional standards and ongoing education.
Analytical and Communication Capabilities
Revenue cycle associates analyze complex billing scenarios daily, requiring strong critical thinking skills. They must determine why claims were denied, what documentation supports appeals, and how to prevent similar issues in the future. Pattern recognition helps identify systemic problems that affect multiple claims.
Effective communication proves equally important. Associates interact with:
- Clinical staff who provide documentation and clarification
- Patients who have billing questions or payment concerns
- Insurance representatives during claim status inquiries
- Management teams requiring performance reports
- Collection agencies handling aged accounts
Clear, professional communication resolves issues faster and maintains positive relationships across all stakeholders. Following revenue cycle management best practices includes establishing communication protocols that keep all parties informed throughout the billing cycle.
How Revenue Cycle Associates Adapt to Industry Changes
Healthcare billing continuously evolves with regulatory updates, payer policy changes, and technological advancements. Revenue cycle associates must stay current with industry developments to maintain billing accuracy and compliance.
Regulatory Compliance and Updates
Federal and state regulations governing healthcare billing change frequently. Revenue cycle associates monitor updates to:
- Medicare and Medicaid billing policies
- Commercial payer contracts and fee schedules
- Coding guideline revisions from AMA and CMS
- Privacy regulations under HIPAA and state laws
- Telehealth billing requirements and restrictions
Understanding these changes prevents compliance violations that lead to claim denials, payment recoupments, or audit penalties. Associates who participate in continuing education through webinars, industry publications, and professional associations maintain their expertise as requirements evolve.
Technology Integration and Automation
Modern revenue cycle operations increasingly rely on automated systems for claims scrubbing, eligibility verification, and payment posting. Revenue cycle associates work alongside these technologies, handling exceptions, complex scenarios, and cases requiring human judgment.
Automation handles routine tasks such as:
- Real-time eligibility verification through API connections
- Automated claim scrubbing against payer edit rules
- Electronic remittance advice downloads and auto-posting
- Denial trend reporting and root cause analysis
- Patient statement generation and delivery
Associates focus their expertise on cases that automation flags for review, complex denial appeals, and patient account resolution. This human-technology partnership optimizes both efficiency and accuracy across the revenue cycle.
Building High-Performance Revenue Cycle Teams
Healthcare organizations that invest in their revenue cycle associates through training, tools, and performance management achieve superior financial results. Strategic approaches to team development maximize the impact these professionals deliver.
Structured Training and Development Programs
Comprehensive onboarding prepares new revenue cycle associates for success. Effective training programs include:
- Foundation Phase: Introduction to practice management systems, payer portals, and billing workflows
- Skill Building: Hands-on training in claims processing, denial management, and payment posting with supervision
- Specialization: Deep-dive training on specific payer requirements, specialty-specific billing rules, or complex procedures
- Quality Assurance: Regular claim audits, feedback sessions, and accuracy scorecards
- Continuous Learning: Monthly updates on coding changes, payer policy modifications, and process improvements
Organizations that maintain documented training protocols and competency assessments reduce billing errors by 25-35% compared to those with informal training approaches. Ongoing education through industry resources like revenue cycle management best practices guides keeps teams informed about emerging standards.
Performance Metrics and Accountability
Clear performance expectations help revenue cycle associates understand priorities and track their contributions. Key performance indicators for these roles typically include:
| Metric | Target Range | Impact on Revenue Cycle |
|---|---|---|
| First Pass Resolution Rate | 95-98% | Reduces rework and accelerates cash flow |
| Days in A/R | <30 days | Indicates efficient collection processes |
| Clean Claim Rate | 90-95% | Minimizes denials and delays |
| Denial Recovery Rate | 60-75% | Recovers revenue from rejected claims |
| Collection Rate | >95% | Measures effectiveness of total revenue capture |
| Coding Accuracy | 98%+ | Prevents compliance issues and claim rejections |
Regular performance reviews with constructive feedback help associates improve continuously. Recognition programs that reward high performers reinforce quality work and reduce turnover in these critical positions.
The Business Value Revenue Cycle Associates Deliver
Healthcare providers face mounting financial pressures from declining reimbursement rates, rising operational costs, and increasing patient responsibility amounts. Revenue cycle associates directly address these challenges through diligent execution of billing processes that maximize legitimate revenue collection.
Cash Flow Optimization
Consistent cash flow enables healthcare organizations to meet payroll, invest in equipment, and expand services. Revenue cycle associates accelerate cash collection by:
- Submitting claims within 24-48 hours of service delivery
- Following up on unpaid claims at regular intervals
- Resolving patient accounts promptly through flexible payment options
- Identifying and correcting billing errors before they delay payment
Practices with dedicated revenue cycle associates typically collect 8-12% more of their gross charges compared to those with inconsistent billing processes. This revenue improvement comes from reduced write-offs, better payer contract compliance, and higher patient collection rates.
Reduction in Revenue Leakage
Revenue leakage occurs when healthcare providers fail to bill for all services rendered, accept incorrect payment amounts, or write off collectable balances prematurely. Revenue cycle associates prevent leakage through:
- Comprehensive charge capture review
- Payment variance analysis against fee schedules
- Underpayment identification and payer follow-up
- Patient responsibility verification and collection
Understanding net revenue management helps associates distinguish between legitimate contractual adjustments and underpayments requiring correction. This distinction protects practice revenue and ensures payers reimburse according to contracted rates.
Specialized Knowledge for Different Healthcare Settings
Revenue cycle associates working in different healthcare environments develop specialized expertise matching their practice settings. The billing complexities vary significantly between outpatient clinics, hospitals, specialty practices, and urgent care facilities.
Outpatient and Physician Practice Billing
Physician practices require revenue cycle associates familiar with evaluation and management coding, preventive care billing, and commercial insurance contracts. Common responsibilities include:
- Coding office visits using appropriate E/M levels
- Billing annual wellness visits with age-specific requirements
- Managing modifier 25 for significant, separately identifiable services
- Coordinating billing for ancillary services like laboratory or radiology
Associates working in specialty practices develop deep knowledge of procedure-specific coding and documentation requirements for their specialty area, whether cardiology, orthopedics, gastroenterology, or other fields.
Hospital and Institutional Billing
Hospital revenue cycle associates work with more complex billing scenarios involving inpatient admissions, observation status, and facility fee billing. Their expertise includes:
- DRG assignment and MS-DRG validation
- Revenue code application for facility charges
- UB-04 claim form completion
- Medicare wage index and geographic adjustments
- Outlier payment calculations
Understanding hospital revenue cycle management principles helps these associates navigate the unique challenges of institutional billing and reimbursement.
Urgent Care and Immediate Care Settings
Urgent care centers present distinct billing scenarios that revenue cycle associates must master. These include:
- Place of service designations specific to urgent care
- Time-of-service payment collection strategies
- Workers' compensation and auto accident billing
- Integration of ancillary services like X-rays and laboratory testing
Revenue cycle associates in urgent care revenue cycle management handle high patient volumes with diverse payer mixes, requiring efficiency combined with accuracy.
Technology Tools That Empower Revenue Cycle Associates
Modern revenue cycle associates leverage sophisticated software platforms and digital tools that enhance their productivity and accuracy. These technologies streamline workflows and provide real-time data for decision-making.
Practice Management and Billing Systems
Comprehensive practice management systems serve as the central hub for revenue cycle operations. These platforms enable associates to:
- Schedule appointments and register patients
- Verify insurance eligibility in real-time
- Generate superbills and charge tickets
- Submit claims electronically
- Post payments and adjustments
- Generate accounts receivable aging reports
Integration between scheduling, clinical documentation, and billing functions reduces duplicate data entry and improves charge capture. Associates working with well-integrated systems process 30-40% more claims daily compared to those using disconnected platforms.
Clearinghouses and Claim Scrubbing Tools
Clearinghouses provide the infrastructure for electronic claim submission to multiple payers through a single connection point. Revenue cycle associates benefit from clearinghouse features including:
- Automated claim validation against payer-specific rules
- Real-time eligibility verification
- Electronic remittance advice retrieval
- Claim status tracking and reporting
- Error identification before claim submission
Advanced scrubbing technology catches 85-90% of potential claim errors before submission, allowing associates to correct issues proactively rather than managing denials reactively.
Reporting and Analytics Platforms
Data-driven decision-making requires robust reporting capabilities. Revenue cycle associates use analytics tools to:
- Monitor key performance indicators daily
- Identify denial trends by payer, provider, or service type
- Track collection patterns and payment timelines
- Measure productivity across team members
- Benchmark performance against industry standards
Organizations implementing comprehensive revenue cycle process in healthcare analytics empower their associates to spot opportunities for improvement and measure the impact of process changes.
Career Development Pathways for Revenue Cycle Associates
Revenue cycle associates who demonstrate strong performance and continue developing their skills can advance into leadership positions within revenue cycle management. Multiple career progression options exist within healthcare finance.
Advancement Opportunities
Professional growth paths for revenue cycle associates include:
- Senior Revenue Cycle Associate: Handling complex accounts, mentoring junior team members, and specializing in denial appeals
- Revenue Cycle Team Lead: Supervising small teams, conducting quality audits, and coordinating workflow distribution
- Revenue Cycle Analyst: Focusing on data analysis, performance reporting, and process improvement initiatives
- Revenue Cycle Manager: Overseeing entire billing operations, managing staff, and implementing strategic initiatives
- Director of Revenue Cycle: Leading organization-wide revenue cycle strategy, vendor management, and financial optimization
Each advancement level requires additional competencies in leadership, strategic thinking, and financial analysis beyond foundational billing skills.
Professional Certifications and Education
Pursuing relevant certifications demonstrates expertise and commitment to professional development. Valuable credentials for revenue cycle associates include:
- Certified Revenue Cycle Representative (CRCR) from AAHAM
- Certified Professional Biller (CPB) from AAPC
- Certified Medical Reimbursement Specialist (CMRS) from AHA
- Certified Healthcare Access Associate (CHAA) from NAHAM
- Certified Professional Coder (CPC) from AAPC
Associates who combine billing expertise with coding certifications become particularly valuable, as they understand both the clinical documentation and reimbursement aspects of revenue cycle management. Implementing best practices in revenue cycle management becomes more effective when staff possess comprehensive credentials.
Outsourcing Considerations for Revenue Cycle Associate Functions
Many healthcare organizations evaluate whether to maintain in-house revenue cycle teams or partner with specialized service providers. Understanding the advantages of each approach helps practices make informed decisions aligned with their operational goals.
Benefits of Specialized Revenue Cycle Service Providers
Healthcare providers partnering with experienced revenue cycle management companies gain access to:
- Dedicated expertise: Teams of revenue cycle associates with specialized training and certifications
- Scalability: Flexible staffing that adjusts to patient volume fluctuations
- Technology access: Enterprise-grade billing systems and analytics platforms without capital investment
- Compliance assurance: Regular training updates and audit protocols maintaining regulatory compliance
- Performance guarantees: Service level agreements defining expected collection rates and turnaround times
Providers who collaborate with established revenue cycle management partners often see collection rate improvements of 5-15% within the first six months of engagement. The combination of experienced revenue cycle associates and optimized processes drives measurable financial improvement.
Hybrid Models Combining Internal and External Resources
Some healthcare organizations adopt hybrid approaches that maintain core revenue cycle functions internally while outsourcing specific components. Common hybrid configurations include:
- In-house patient registration and eligibility verification with outsourced claims processing
- Internal front-end revenue cycle with external denial management specialists
- On-site coding with outsourced payment posting and accounts receivable follow-up
These models allow practices to retain control over patient-facing interactions while leveraging external expertise for specialized or high-volume back-end processes. Revenue cycle associates in hybrid environments often coordinate between internal clinical staff and external billing teams, requiring strong communication and project management skills.
Critical Success Factors for Revenue Cycle Associate Excellence
Healthcare organizations seeking to maximize the value their revenue cycle associates deliver should focus on several critical enablers that drive superior performance across billing operations.
Clear Process Documentation and Workflows
Standardized procedures ensure consistency across revenue cycle operations regardless of which associate handles specific tasks. Comprehensive process documentation should cover:
- Step-by-step workflows for common billing scenarios
- Payer-specific requirements and submission guidelines
- Escalation procedures for complex issues
- Quality checkpoints and approval requirements
- Communication protocols with clinical and administrative staff
Organizations with well-documented processes reduce training time by 40-50% and maintain billing accuracy even during staff transitions or periods of high turnover.
Investment in Continuous Improvement
Revenue cycle performance improves when organizations create cultures of continuous improvement. Strategies that engage revenue cycle associates in optimization efforts include:
- Regular team meetings reviewing denial trends and root causes
- Suggestion programs rewarding process improvement ideas
- Cross-training opportunities expanding skill sets
- Technology upgrades addressing workflow inefficiencies
- Benchmark comparisons against industry standards
Associates who participate in improvement initiatives develop deeper engagement with their work and contribute valuable insights from their frontline perspective. Following guidance from resources like seven revenue cycle management best practices provides frameworks for systematic enhancement efforts.
Recognition and Retention Programs
Experienced revenue cycle associates represent significant value to healthcare organizations. The knowledge they accumulate about practice-specific billing requirements, payer relationships, and documentation standards cannot be easily replaced. Retention strategies that reduce turnover include:
- Competitive compensation benchmarked against market rates
- Performance bonuses tied to collection metrics
- Professional development funding for certifications and training
- Career advancement opportunities within revenue cycle leadership
- Work-life balance initiatives including flexible scheduling options
Organizations investing in retention typically maintain staff tenure of 5+ years, compared to industry averages of 2-3 years for revenue cycle positions. This continuity translates directly into superior billing performance and reduced operational costs.
Revenue cycle associates form the operational foundation of healthcare financial success, executing the detailed work that transforms clinical services into collected revenue. Their expertise in claims processing, denial management, payment posting, and patient account resolution directly impacts cash flow, collection rates, and organizational financial health. Healthcare providers who invest in skilled revenue cycle teams through comprehensive training, performance management, and continuous improvement initiatives achieve measurably superior financial outcomes. Greenhive Billing Solutions provides comprehensive revenue cycle management services delivered by experienced professionals who bring specialized expertise across all aspects of healthcare billing and reimbursement. Our dedicated teams work as extensions of your practice, combining technical knowledge with proven processes to maximize collections, reduce denials, and streamline your revenue cycle operations.