Healthcare providers face mounting pressure to deliver quality patient care while navigating increasingly complex administrative requirements. Among these challenges, prior authorization stands out as one of the most time-consuming and resource-intensive processes. Prior auth services have emerged as a critical solution for practices seeking to reduce claim denials, expedite treatment approvals, and maintain healthy cash flow. For revenue cycle management professionals, understanding how specialized prior auth services function and deliver value is essential to improving overall financial performance.
Understanding Prior Authorization in Healthcare Operations
Prior authorization represents a utilization management process where insurance companies require approval before covering specific medical services, procedures, medications, or equipment. This administrative step serves as a cost-control mechanism for payers, ensuring that proposed treatments meet medical necessity criteria and align with coverage policies.
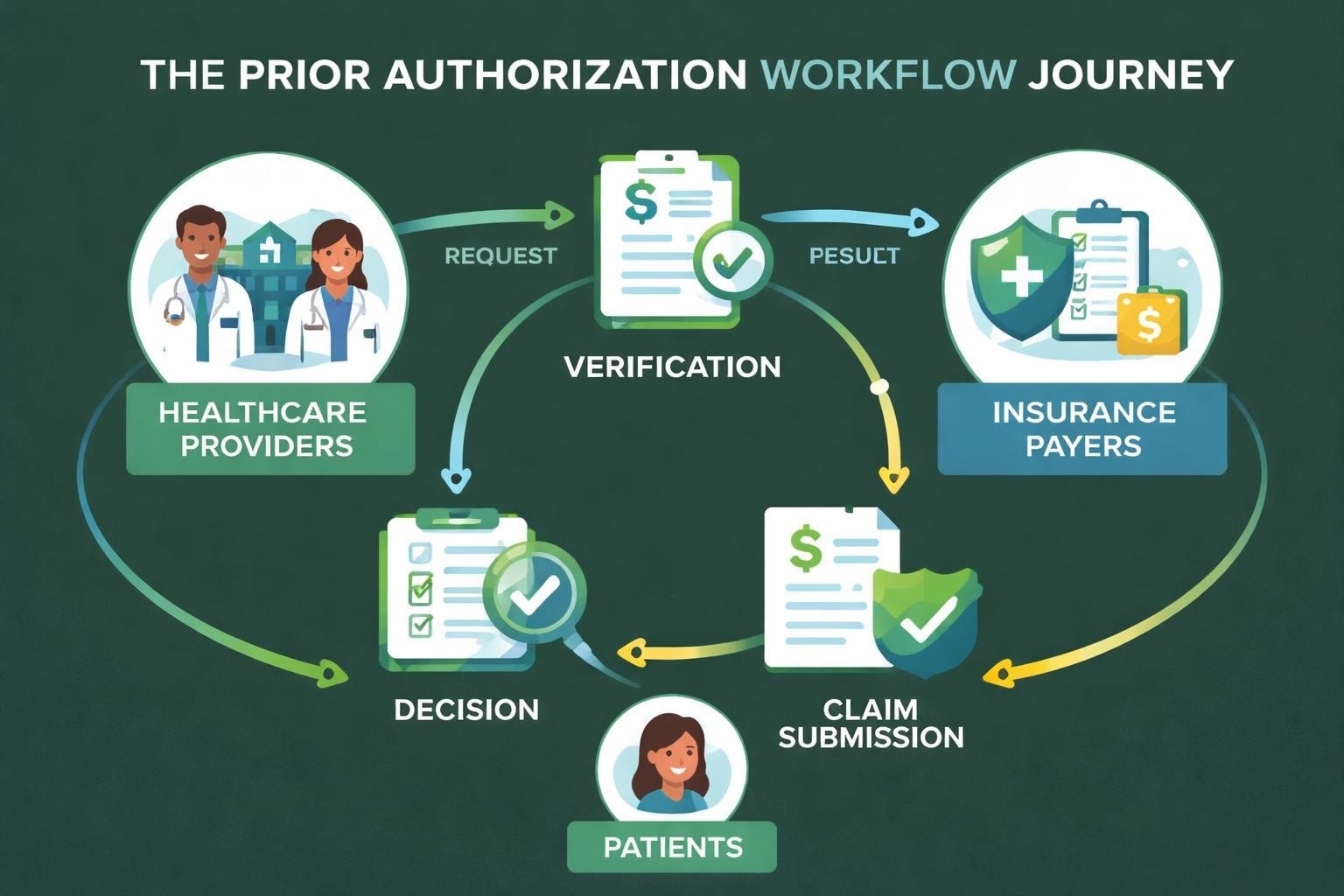
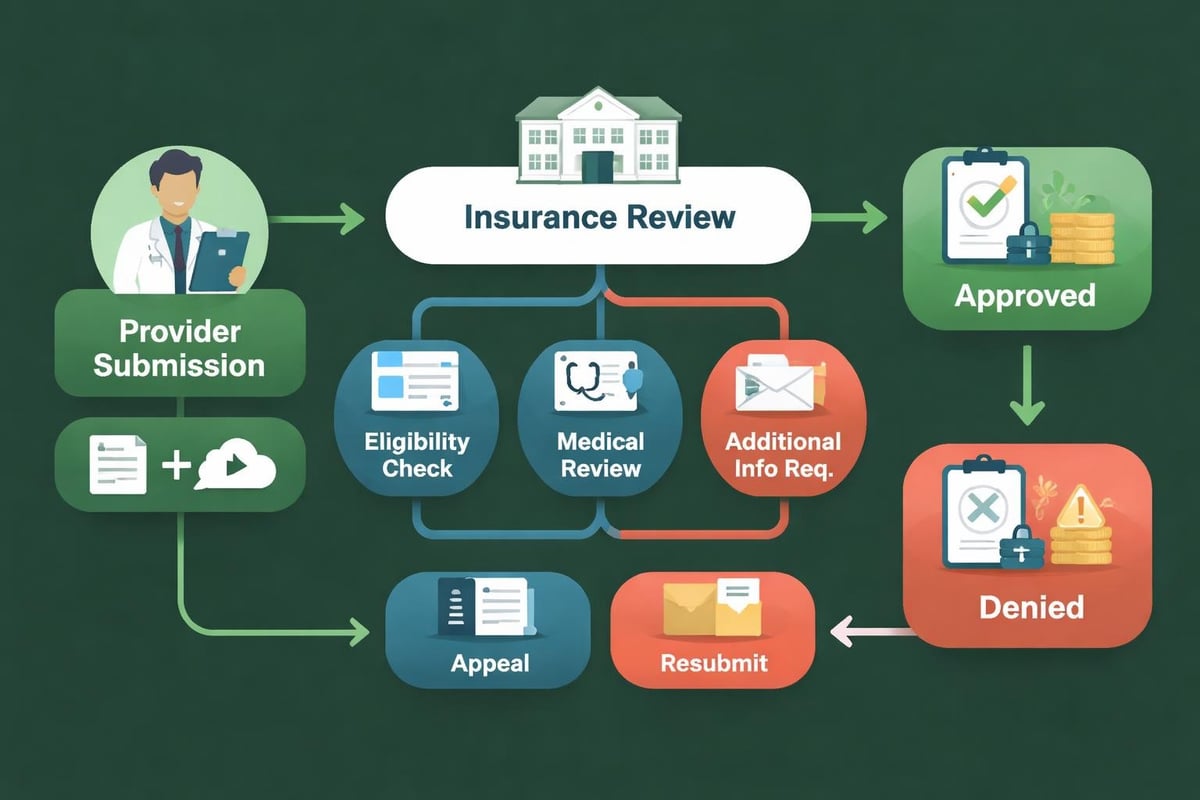
The process typically involves multiple steps and stakeholders. Healthcare providers must submit detailed clinical documentation justifying the requested service. Insurance reviewers evaluate this information against established guidelines. The decision then flows back through the system to the provider and patient. Each step creates opportunities for delays, errors, and denials that directly impact practice revenue.
Modern healthcare demands have made prior authorization increasingly burdensome. According to research from medical associations, physicians and their staff spend an average of two business days per week completing prior authorization requirements. This administrative burden diverts resources away from patient care and creates operational bottlenecks that affect the entire revenue cycle.
The Business Impact of Prior Authorization Challenges
Practices that handle prior authorization internally often encounter significant operational costs and revenue disruptions. Staff members must navigate varying requirements across multiple insurance carriers, each with distinct forms, documentation standards, and submission processes. This complexity leads to several measurable business challenges:
- Extended treatment delays that affect patient satisfaction and outcomes
- High denial rates due to incomplete or improperly submitted requests
- Increased administrative costs from redundant work and resubmissions
- Cash flow disruptions when procedures cannot proceed without approval
- Staff burnout from repetitive, time-consuming authorization tasks
The financial implications extend beyond direct costs. When prior authorization requirements expand to new service categories, practices must quickly adapt their workflows or face mounting claim denials. For smaller practices with limited administrative staff, these requirements can become particularly overwhelming.
How Prior Auth Services Deliver Value to Healthcare Practices
Professional prior auth services provide specialized expertise and dedicated resources to manage the authorization process on behalf of healthcare providers. These services operate as an extension of the practice, handling submissions from initial request through final approval or appeal.
A comprehensive prior auth service manages multiple critical functions simultaneously. The service team verifies insurance coverage and determines which services require prior authorization. They gather necessary clinical documentation and translate provider notes into language that meets payer requirements. The team then submits requests through appropriate channels and monitors status until resolution.
Key Components of Effective Prior Authorization Services
| Service Component | Function | Business Benefit |
|---|---|---|
| Coverage Verification | Confirms insurance status and authorization requirements | Reduces claim denials from coverage issues |
| Clinical Documentation Review | Ensures submissions include all required supporting information | Improves first-pass approval rates |
| Multi-Payer Management | Handles varying requirements across insurance carriers | Eliminates need for internal expertise on each payer |
| Status Tracking | Monitors pending requests and follows up proactively | Prevents approval delays from oversight |
| Appeal Management | Handles denials with clinical justification and resubmission | Recovers revenue from initially denied services |
The value proposition centers on efficiency and expertise. Experienced prior auth professionals understand payer-specific requirements and maintain current knowledge of changing policies. This specialization translates directly into higher approval rates and faster turnaround times compared to internal staff managing authorizations alongside other responsibilities.
Organizations providing denial management in medical billing recognize that proactive prior authorization management serves as the first line of defense against preventable claim rejections.
Integrating Prior Auth Services Into Revenue Cycle Management
Prior auth services function most effectively when integrated seamlessly with broader revenue cycle operations. This integration ensures that authorization status informs scheduling, billing, and collections processes throughout the patient encounter.
The integration begins at patient registration and scheduling. When appointment coordinators understand authorization requirements upfront, they can initiate the process before the scheduled service date. This proactive approach prevents last-minute cancellations and revenue delays.
Step-by-Step Prior Authorization Process Integration
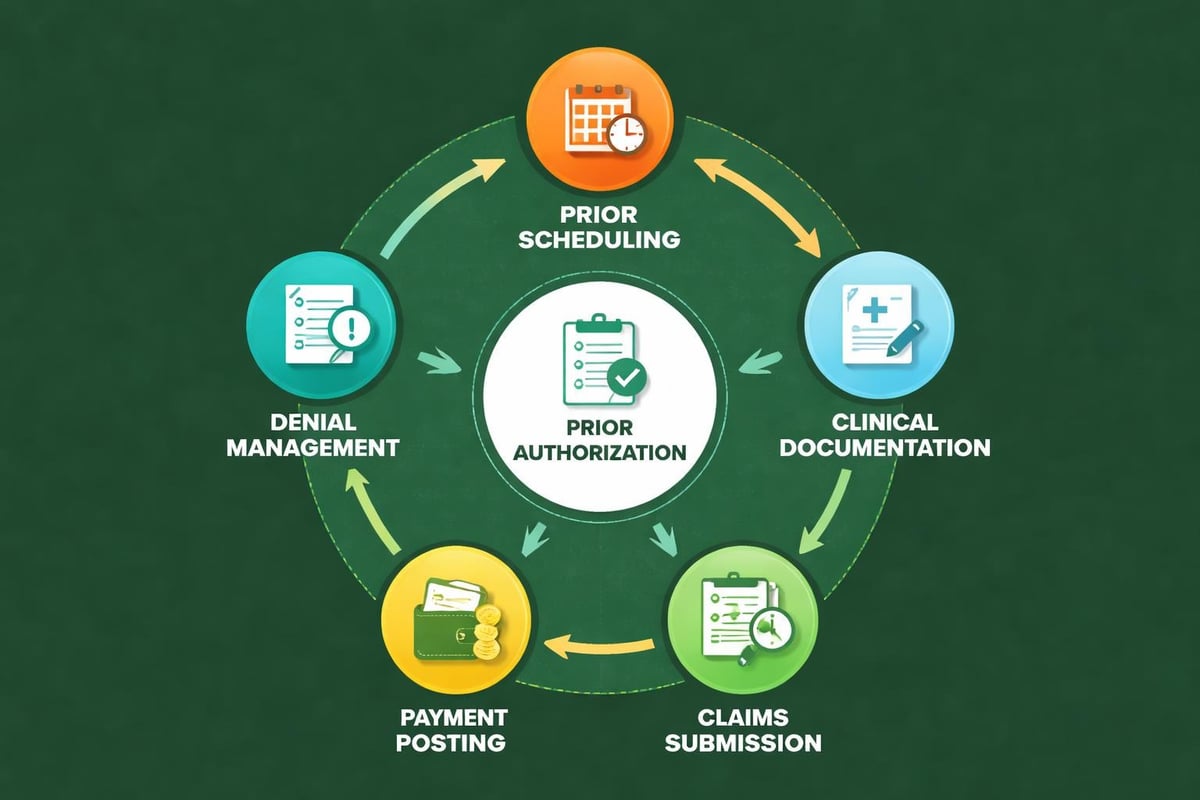
Step 1: Patient scheduling triggers insurance verification and prior auth requirement check
Step 2: Clinical staff receives notification of required documentation for pending authorization
Step 3: Prior auth team submits request with complete clinical justification to appropriate payer
Step 4: Status updates flow to scheduling and billing teams for treatment planning
Step 5: Approved authorizations attach to patient accounts for accurate claim submission
Step 6: Denied requests immediately route to appeals process while clinical team receives notification
This systematic approach creates accountability at each stage while maintaining visibility across departments. When authorization status remains uncertain as the service date approaches, scheduling teams can make informed decisions about rescheduling or patient communication.
The connection between prior auth services and clean claims cannot be overstated. A clean claim in medical billing includes proper authorization documentation, significantly increasing the likelihood of first-pass payment. Practices that prioritize authorization management see measurable improvements in days in accounts receivable and overall collection rates.
Technology and Prior Authorization Service Delivery
While prior auth services rely on human expertise, technology platforms enable efficient operation at scale. Service providers leverage specialized software to manage workflows, track authorization status, and communicate with both payers and providers.
Electronic prior authorization systems have evolved significantly in recent years. Many insurance carriers now offer portals for direct submission and real-time status checking. Some platforms, as described in resources about healthcare technology automation, enable automated request generation based on clinical data already captured in electronic health records.
Prior auth service teams utilize these platforms while adding critical oversight and intervention. Automated systems excel at routine requests with straightforward criteria but often struggle with complex cases requiring clinical judgment and narrative justification. Professional services combine technology efficiency with human expertise to optimize outcomes.
Technology Features That Enhance Prior Authorization Outcomes
- Real-time eligibility checking that identifies authorization requirements before service scheduling
- Payer portal integration enabling direct submission and status tracking across multiple carriers
- Documentation repositories maintaining clinical notes and supporting materials for quick retrieval
- Automated status monitoring with alerts for pending expirations or required follow-up actions
- Analytics dashboards showing approval rates, turnaround times, and denial patterns by payer and service type
These technological capabilities support prior auth teams but do not replace the need for skilled professionals. Understanding medical coding and billing fundamentals remains essential for translating clinical services into language that satisfies payer requirements.
Recent developments show promising changes on the horizon. Major insurers have announced plans to reduce prior authorization burdens, potentially streamlining requirements for certain service categories. However, healthcare providers should maintain robust authorization processes even as policies evolve, since requirements vary significantly across payers and continue changing.
Measuring Prior Authorization Service Performance
Healthcare organizations evaluating prior auth services should establish clear performance metrics aligned with business objectives. These measurements provide visibility into service effectiveness and identify opportunities for continuous improvement.
Key performance indicators fall into several categories addressing different aspects of authorization management. Speed metrics measure how quickly authorizations move from request to approval. Quality metrics assess accuracy and completeness of submissions. Financial metrics connect authorization performance to revenue outcomes.
| Metric Category | Specific Measurements | Target Benchmarks |
|---|---|---|
| Speed | Average turnaround time from request to approval | Under 48 hours for routine requests |
| Quality | First-pass approval rate | Above 90% |
| Quality | Denial rate requiring appeal | Below 5% |
| Financial | Revenue impact from prevented denials | Measured quarterly |
| Financial | Cost per authorization | Compared to internal processing costs |
Organizations should track these metrics monthly and review trends quarterly. Declining approval rates may signal changing payer policies requiring updated submission approaches. Increasing turnaround times might indicate staffing needs or process bottlenecks requiring attention.
The relationship between authorization performance and overall revenue cycle health becomes evident through these measurements. Practices with efficient prior auth services typically demonstrate shorter days in accounts receivable and higher clean claim rates. These improvements directly enhance cash flow and reduce the administrative burden on billing staff.
For practices managing their own billing operations or working with revenue cycle management partners, prior authorization metrics should integrate with broader financial reporting to provide complete visibility into revenue cycle performance.
Selecting Prior Auth Services for Your Practice
Healthcare organizations considering outsourced prior auth services should evaluate potential partners across multiple dimensions. The right service provider aligns with practice size, specialty requirements, payer mix, and existing technology infrastructure.
Specialty expertise stands as a critical selection factor. Prior authorization requirements vary significantly between specialties, with radiology, oncology, and orthopedics facing particularly complex approval processes. Service providers with deep experience in your specialty understand common denial reasons and optimal documentation approaches for your specific services.
Essential Questions When Evaluating Prior Auth Service Providers
- What is your team's experience with our specialty and most common procedures?
- How do you integrate with our practice management and electronic health record systems?
- What is your average turnaround time for routine versus complex authorization requests?
- How do you handle urgent or expedited authorization needs?
- What reporting and analytics do you provide to track authorization performance?
- How is your team structured, and who will serve as our primary point of contact?
- What happens when authorizations are denied, and what is your appeal success rate?
Service providers should demonstrate clear processes for handling each stage of authorization management. They should explain how they stay current with changing payer policies and maintain compliance with HIPAA and other regulatory requirements.
Cost structure represents another important consideration. Some prior auth services charge per authorization, while others use monthly retainer models based on practice volume. Understanding the total cost and comparing it to internal processing expenses helps quantify return on investment.
Organizations should also assess how potential prior auth services align with their broader revenue cycle strategy. For practices using comprehensive revenue cycle management services, prior authorization should integrate seamlessly with billing, coding, and claims management functions.
Overcoming Common Prior Authorization Challenges
Even with professional prior auth services, healthcare organizations encounter persistent challenges that require strategic solutions. Understanding these common obstacles and their resolutions helps practices maximize authorization success rates.
Incomplete clinical documentation remains the leading cause of authorization delays. Payers require specific clinical information to evaluate medical necessity, yet provider notes may not capture all required elements. Prior auth services address this challenge by providing clear documentation checklists to clinical staff and identifying missing information before submission.
Payer policy changes create another frequent challenge. Insurance carriers regularly update their prior authorization requirements, sometimes without adequate advance notice to providers. Professional services monitor these changes and adjust submission processes accordingly, preventing denials from outdated approaches.
State-specific regulations add complexity to authorization management. Resources like state healthcare advocate guidance provide valuable information about patient rights and provider obligations, which vary by jurisdiction. Prior auth services with multi-state experience navigate these differences effectively.
Communication breakdowns between departments disrupt authorization workflows. When clinical staff, schedulers, and billing teams operate in silos, critical information may not flow appropriately. Integrated prior auth services establish communication protocols ensuring all stakeholders receive timely updates on authorization status.
Solutions for Persistent Authorization Issues
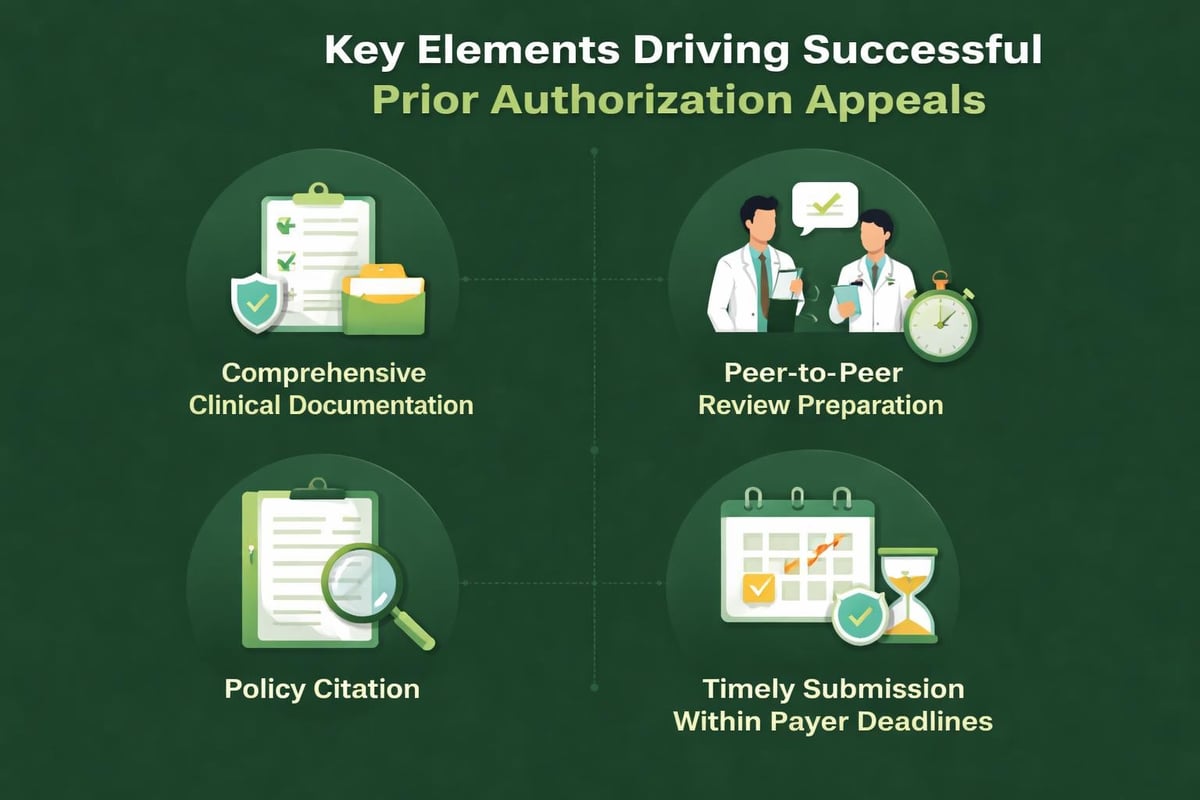
Implement standardized clinical templates that capture payer-required information during patient encounters
Establish regular payer policy review processes to identify requirement changes before they cause denials
Create escalation protocols for urgent authorizations requiring expedited processing
Maintain comprehensive appeal documentation showing patterns in payer denials that may warrant policy discussions
Develop strong payer relationships through professional interactions and data-driven discussions about approval processes
These solutions require consistent execution and ongoing refinement. Organizations leveraging prior auth services benefit from the provider's established best practices while tailoring approaches to practice-specific needs.
The Centers for Medicare & Medicaid Services continues evaluating prior authorization requirements across service categories, indicating ongoing evolution in this space. Practices must remain adaptable while maintaining core authorization management competencies.
Prior Authorization and Patient Experience
While prior auth services primarily aim to optimize administrative efficiency and financial outcomes, they significantly impact patient experience. Delays in authorization directly affect when patients receive needed care, creating frustration and potentially compromising health outcomes.
Professional prior auth services improve patient experience through faster approval turnaround and proactive communication. When patients schedule services requiring authorization, they receive clear information about the approval process and realistic timelines. This transparency reduces anxiety and allows patients to plan accordingly.
Authorization denials create particularly difficult patient situations. Patients who have scheduled procedures may face unexpected delays or financial responsibility if insurance denies coverage. Prior auth services minimize these situations through high approval rates and swift appeal processes when denials occur.
The broader healthcare industry recognizes authorization burden as a patient care issue. Recent industry commitments to reform prior authorization processes reflect growing acknowledgment that excessive administrative requirements interfere with timely care delivery.
Healthcare organizations should consider patient experience metrics when evaluating prior auth service performance. Treatment delays attributable to authorization issues, patient complaints about approval processes, and procedure cancellations due to authorization problems all provide valuable feedback on service effectiveness.
For practices prioritizing patient satisfaction alongside financial performance, professional prior auth services offer dual benefits. They reduce administrative burden on practice staff while ensuring patients experience minimal disruption in accessing needed care.
Building a Sustainable Prior Authorization Strategy
Long-term success with prior authorization management requires strategic planning beyond simply outsourcing the function. Healthcare organizations should develop comprehensive approaches that leverage prior auth services while building internal capabilities and maintaining oversight.
A sustainable strategy begins with clear policies defining when authorization requests initiate and who holds responsibility for key decisions. These policies should specify how urgent situations receive expedited handling and establish protocols for communicating authorization status to patients.
Staff education represents another critical component. While prior auth services handle submission and follow-up, clinical and administrative staff must understand documentation requirements and authorization timelines. Regular training ensures team members capture necessary information during patient encounters and schedule services appropriately.
Technology investment supports long-term authorization efficiency. Practice management systems should flag services requiring authorization during scheduling. Electronic health records should facilitate easy extraction of clinical documentation for authorization submissions. These integrations reduce manual work and minimize errors.
Organizations should also establish regular review processes assessing prior auth service performance and identifying improvement opportunities. Quarterly business reviews with service providers should examine approval rates, turnaround times, denial patterns, and financial impact. These discussions ensure continuous optimization and alignment with evolving practice needs.
Understanding how prior authorization fits within the complete revenue cycle provides essential context. Organizations focused on revenue cycle process optimization recognize that authorization management connects directly to charge capture, claims submission, and payment posting. Success in one area supports performance across the entire cycle.
Prior auth services address one of healthcare's most persistent administrative challenges by combining specialized expertise with efficient processes that accelerate approvals and reduce denials. For healthcare providers seeking to optimize revenue cycle performance while maintaining focus on patient care, professional authorization management delivers measurable value through improved cash flow, reduced administrative burden, and enhanced patient satisfaction. Greenhive Billing Solutions provides comprehensive prior authorization services integrated with complete revenue cycle management support, helping practices across the United States maximize reimbursements while streamlining operations through expert handling of insurance requirements and transparent communication at every step.