Healthcare providers face mounting pressure to deliver exceptional patient care while managing complex administrative responsibilities. The financial backbone of any medical practice relies on efficient billing operations, yet many organizations struggle with claim denials, coding errors, and delayed reimbursements. As the healthcare landscape becomes increasingly complex with evolving regulations and payer requirements, more practices are discovering the strategic advantages of partnering with specialized revenue cycle management providers. Understanding the benefits of outsourcing medical billing can transform how healthcare organizations approach their financial operations and patient care delivery.
Financial Performance Enhancement Through Specialized Expertise
Medical billing requires specialized knowledge that extends far beyond basic data entry. The nuances of CPT codes, modifier applications, and payer-specific requirements demand constant education and expertise. When healthcare providers partner with dedicated billing professionals, they gain access to teams who focus exclusively on revenue cycle optimization.
Outsourced billing partners bring several financial advantages:
- Reduced overhead costs associated with hiring, training, and retaining in-house billing staff
- Elimination of expenses for billing software, hardware, and infrastructure maintenance
- Scalable pricing models that align costs with actual collections
- Faster payment cycles through optimized claim submission processes
The cost structure shifts from fixed expenses to variable costs tied directly to practice performance. This alignment creates a partnership model where the billing service provider shares a vested interest in maximizing reimbursements and minimizing denials.

Revenue Optimization and Cash Flow Improvement
One of the most significant benefits of outsourcing medical billing centers on improved cash flow management. Specialized billing teams implement systematic processes that accelerate payment cycles and reduce accounts receivable days. Professional billing companies maintain dedicated staff for follow-up on outstanding claims, ensuring that payments don't languish in payer queues.
These teams understand the specific timelines and requirements for each insurance carrier, enabling them to submit clean claims on the first attempt. The result is a measurable improvement in days in accounts receivable and a healthier revenue stream. Healthcare providers who previously waited 45-60 days for reimbursements often see that timeline reduced to 30-35 days with professional billing support.
Compliance Assurance and Risk Mitigation
Healthcare compliance extends across multiple regulatory frameworks, from HIPAA privacy requirements to Medicare billing regulations and state-specific mandates. Maintaining compliance demands continuous education, policy updates, and procedural adjustments. The benefits of outsourcing medical billing include partnering with organizations that specialize in ensuring regulatory compliance and protecting patient data.
Professional billing companies invest heavily in compliance infrastructure, including:
- Regular staff training on updated regulations and payer policies
- Secure, HIPAA-compliant technology platforms with encryption and access controls
- Documented procedures and audit trails for all billing activities
- Quality assurance programs that identify and correct potential compliance issues
The risk of compliance violations carries severe financial and reputational consequences. Outsourcing transfers much of this risk to specialized partners who maintain dedicated compliance teams and stay current with regulatory changes.
Technology Access Without Capital Investment
Modern revenue cycle management relies on sophisticated software platforms that integrate with electronic health records, track claims in real-time, and provide analytical insights into practice performance. The capital investment required for these systems often exceeds what individual practices can reasonably allocate.
Understanding what billing and coding specialists require includes recognizing their need for advanced tools. Outsourced billing providers deploy enterprise-grade technology solutions without requiring practices to purchase or maintain these systems. Healthcare providers gain access to claim scrubbing software, automated denial tracking, real-time reporting dashboards, and electronic remittance advice processing.
| Technology Benefit | In-House Challenge | Outsourced Solution |
|---|---|---|
| Software Updates | Manual updates, potential downtime | Automatic updates, zero practice disruption |
| System Integration | Complex IT requirements | Seamless EHR integration managed by vendor |
| Data Security | Requires dedicated IT security staff | Enterprise-level security protocols included |
| Reporting Analytics | Limited to software capabilities | Comprehensive dashboards and custom reports |
Error Reduction and Claim Accuracy
Billing errors represent one of the costliest challenges in healthcare revenue cycle management. Incorrect coding, missing information, and documentation gaps lead to claim denials that require time-consuming appeals and resubmissions. The benefits of outsourcing medical billing become evident when examining error rates and first-pass claim acceptance.
Professional billing teams implement multi-level quality checks before claim submission. Each claim undergoes review for:
- Accurate demographic and insurance information
- Proper CPT and ICD code assignment
- Required modifier application and documentation support
- Payer-specific formatting and submission requirements
This systematic approach significantly reduces rejection rates. While in-house billing departments might experience denial rates of 10-15%, specialized billing companies typically maintain denial rates below 5%. The improvement in patient satisfaction follows naturally as billing errors decrease and patients receive accurate statements.
Denial Management Expertise
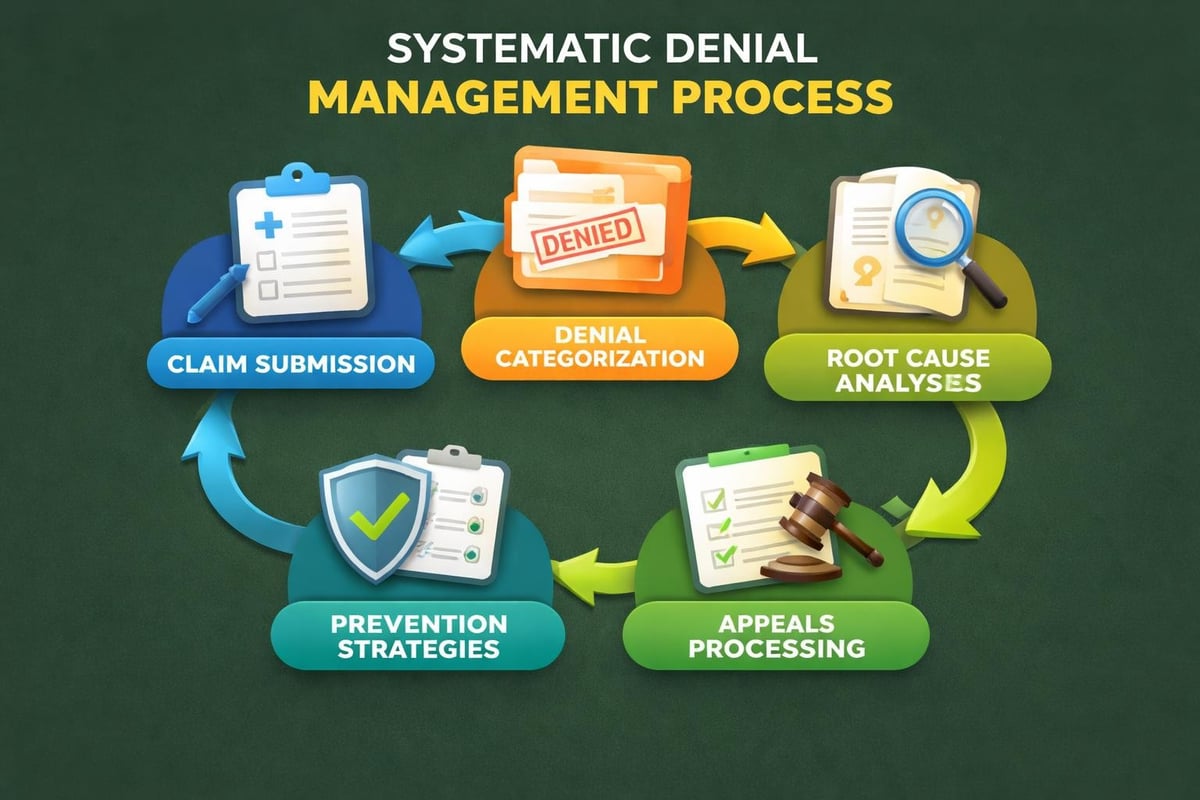
When denials do occur, specialized handling makes the difference between recovered revenue and write-offs. Professional billing services maintain dedicated denial management teams who understand payer-specific appeal processes and requirements. These specialists track denial patterns, identify root causes, and implement corrective measures to prevent recurrence.
Effective denial management in medical billing requires systematic tracking and analysis. Outsourced providers categorize denials, measure trends, and provide actionable insights that help practices address underlying issues. This proactive approach transforms denial management from reactive firefighting into strategic revenue protection.
Focus Restoration on Patient Care
Administrative burden diverts attention and resources from patient care activities. When physicians and clinical staff spend time addressing billing questions, following up on unpaid claims, or troubleshooting coding issues, patient care quality suffers. The strategic benefits of outsourcing medical billing extend beyond financial metrics to practice culture and patient experience.
Outsourcing frees healthcare providers to concentrate on:
- Extended patient consultation time without administrative interruptions
- Clinical skill development and continuing medical education
- Practice growth initiatives and service expansion
- Patient relationship building and satisfaction improvement
This shift in focus often yields measurable improvements in patient outcomes and satisfaction scores. Providers report reduced stress levels and improved work-life balance when billing responsibilities transfer to specialized partners.
Scalability and Practice Growth Support
Healthcare practices experience fluctuating volumes due to seasonal patterns, practice growth, or service line expansion. Maintaining an in-house billing department sized for peak periods results in inefficiency during slower months. Conversely, understaffing during busy periods creates backlogs and delayed reimbursements.
The benefits of outsourcing medical billing include inherent scalability that adjusts to practice needs. Professional billing companies staff multiple clients and can reallocate resources to accommodate volume changes without requiring practices to hire or lay off employees. This flexibility becomes particularly valuable during:
- New provider onboarding and credential processing
- Service line expansion into new specialties or procedures
- Seasonal patient volume variations
- Practice acquisitions or merger integrations
Credential Management and Payer Enrollment
Adding new providers or expanding into new payer networks requires navigating complex credentialing processes. Top medical billing companies often include credential management services that handle provider enrollment, maintain updated information across all payer systems, and track revalidation requirements.
This support accelerates new provider revenue generation and ensures existing providers maintain active status across all contracted payers. The administrative burden of managing multiple payer portals, tracking expiration dates, and completing revalidation applications transfers to billing partners who maintain dedicated credentialing specialists.
Performance Transparency and Data-Driven Insights
One common concern about outsourcing centers on visibility into billing operations. Modern billing partnerships address this through comprehensive reporting and transparent communication. The benefits of outsourcing medical billing include access to sophisticated reporting tools and real-time dashboards that provide deeper insights than many in-house operations generate.
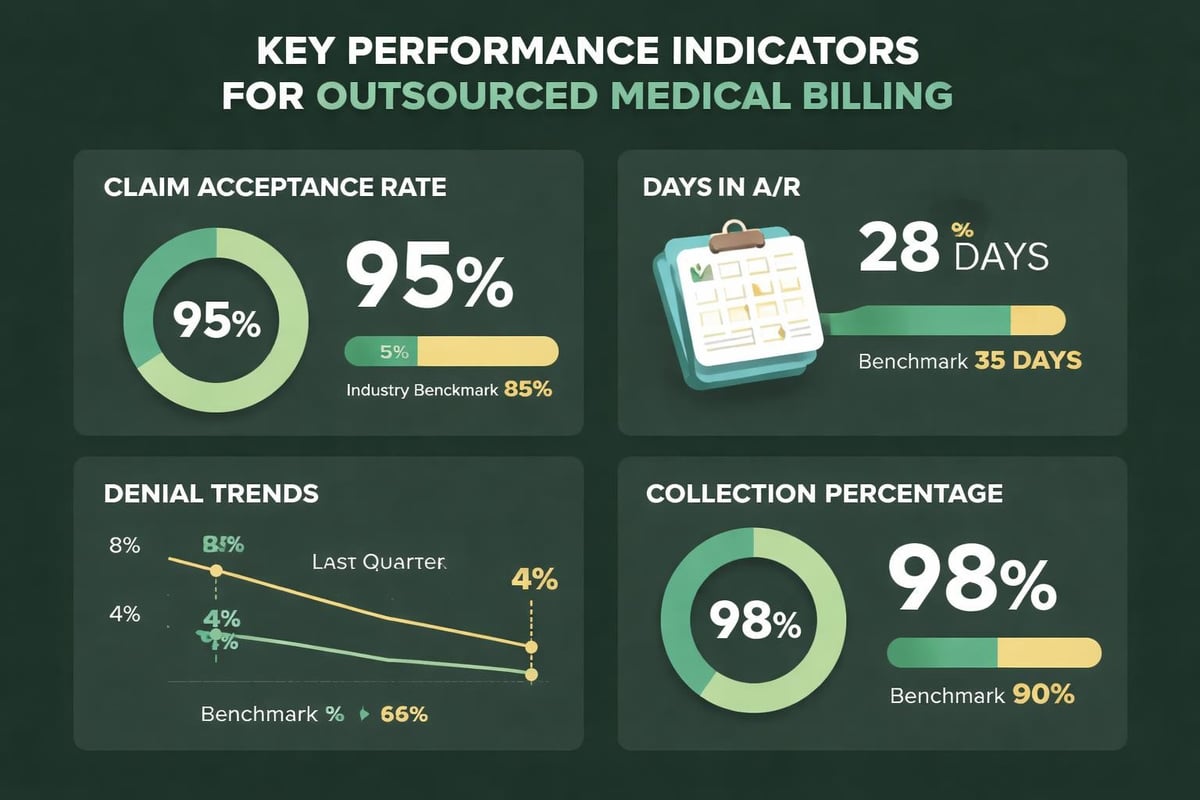
Professional billing services deliver regular reports covering:
- Claims submission volumes and acceptance rates
- Payment posting timelines and collection percentages
- Denial trends with category breakdowns and root cause analysis
- Accounts receivable aging with specific payer performance metrics
- Revenue cycle key performance indicators benchmarked against industry standards
This transparency enables healthcare administrators to identify opportunities, address concerns promptly, and make informed strategic decisions about practice operations.
| Key Performance Indicator | Measurement Frequency | Strategic Value |
|---|---|---|
| Days in Accounts Receivable | Weekly/Monthly | Cash flow health assessment |
| First-Pass Claim Acceptance | Daily/Weekly | Billing accuracy monitoring |
| Denial Rate by Category | Monthly | Process improvement targeting |
| Net Collection Rate | Monthly/Quarterly | Overall revenue cycle efficiency |
| Patient Payment Collection | Monthly | Front-office effectiveness |
Expertise Across Multiple Specialties and Payer Types
Medical specialties each carry unique coding requirements, documentation standards, and payer rules. A cardiology practice faces different billing challenges than a pediatric clinic or orthopedic surgery center. In-house billing staff typically develop expertise in their specific practice specialty but may struggle when practices expand services or add new providers with different specialties.
Professional billing companies serve diverse healthcare providers across multiple specialties, developing broad expertise that benefits individual clients. This cross-specialty knowledge proves particularly valuable for:
- Multi-specialty group practices with varied service lines
- Primary care practices offering diverse procedures and services
- Specialty practices expanding into ancillary services
- Urgent care centers treating wide-ranging conditions
The breadth of experience means billing teams have likely encountered and resolved similar challenges faced by other providers in the same specialty. This collective knowledge base accelerates problem resolution and improves billing accuracy.
Payer-Specific Knowledge and Relationships
Each insurance carrier implements unique policies, submission requirements, and payment methodologies. Medicare follows different rules than commercial payers, while Medicaid programs vary significantly across states. Understanding revenue codes in medical billing and different types of medical coding requires constant education as payers update policies.
Professional billing services maintain dedicated payer relations teams who communicate directly with insurance carriers to resolve claim issues, clarify policy questions, and negotiate payment disputes. These established relationships often expedite issue resolution compared to individual practice staff contacting payer call centers.
Staff Turnover Elimination and Knowledge Retention
Healthcare practices frequently struggle with billing staff turnover, which disrupts operations and creates knowledge gaps. The time and expense required to recruit, hire, and train replacement billing staff compounds the challenge. New employees require several months to reach full productivity, during which claim backlogs accumulate and errors increase.
The benefits of outsourcing medical billing eliminate this vulnerability entirely. Billing companies maintain depth in staffing and cross-train team members to ensure continuity. When individual team members leave, the company redistributes workload among existing staff while recruiting replacements. Healthcare practices experience no disruption or knowledge loss.
This continuity extends to institutional knowledge about specific practice patterns, common procedures, and provider preferences. Billing companies document processes and maintain detailed client profiles that preserve critical information regardless of staff changes.
Strategic Partnership for Long-Term Success
Modern healthcare delivery requires strategic focus on patient outcomes, value-based care initiatives, and operational efficiency. Administrative functions like billing, while critical, distract from these strategic priorities. The comprehensive benefits of outsourcing medical billing position healthcare providers for sustainable success by enabling leadership focus on practice vision rather than billing operations.
Professional billing partnerships function as extensions of practice teams, aligned toward common goals of financial health and operational excellence. These relationships provide healthcare organizations with access to expert knowledge and improved compliance that would be difficult to replicate internally.
The transition to outsourced billing represents a strategic decision with implications extending across practice operations, financial performance, and patient care quality. Healthcare providers who evaluate their revenue cycle management approach should consider not just immediate cost savings, but the comprehensive operational advantages that specialized billing partners deliver. From faster payment processing and reduced errors to compliance assurance and scalability, the case for outsourcing continues to strengthen as healthcare complexity increases.
Understanding the revenue cycle process in healthcare helps providers recognize where specialized expertise delivers maximum value. The decision to outsource reflects recognition that billing excellence requires dedicated focus, specialized knowledge, and significant resource investment that many practices can better allocate toward direct patient care activities.
Healthcare providers who embrace outsourcing discover that the benefits of outsourcing medical billing extend far beyond simple cost reduction, encompassing improved cash flow, enhanced compliance, and restored focus on patient care. By partnering with dedicated revenue cycle management specialists, practices position themselves for sustainable financial health and operational excellence. Greenhive Billing Solutions delivers comprehensive medical billing and revenue cycle management services designed to maximize reimbursements, streamline operations, and free healthcare providers to focus on what matters most: exceptional patient care.

