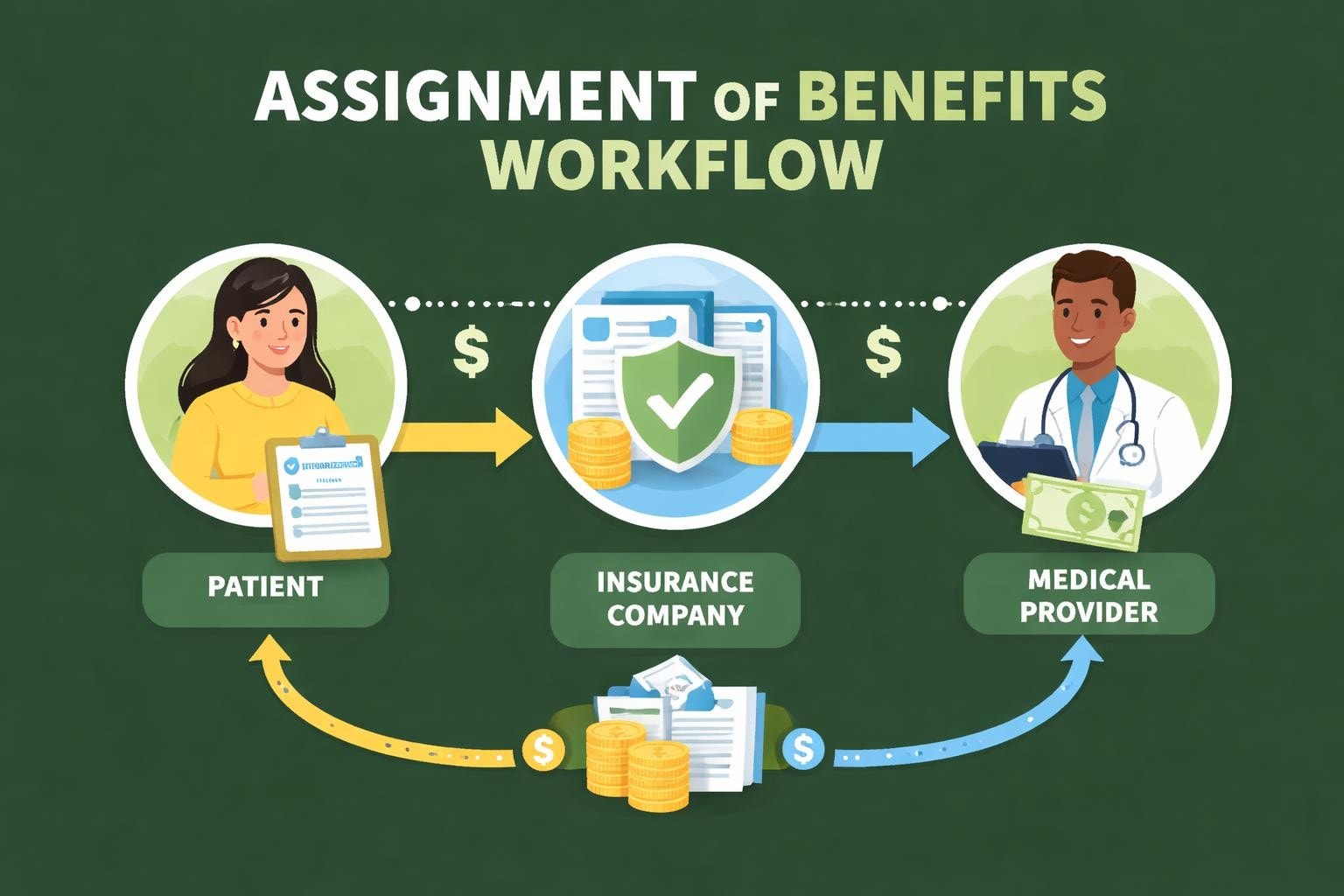
Assignment of benefits plays a fundamental role in healthcare revenue cycles, yet many providers struggle to understand its full implications for their practice operations. When patients sign an AOB authorization, they transfer their insurance payment rights directly to the healthcare provider, fundamentally changing how payments flow through the billing system. This simple administrative step can dramatically reduce collection challenges, accelerate cash flow, and minimize the burden of chasing patient payments for covered services. Understanding aob in medical billing is essential for any practice seeking to optimize their revenue cycle and maintain healthy financial operations.
Understanding Assignment of Benefits in Healthcare Revenue Cycles
Assignment of benefits represents a contractual agreement where patients authorize their insurance companies to pay healthcare providers directly for covered medical services. Rather than receiving insurance reimbursements themselves and then paying their providers, patients redirect these payments to their care team. This arrangement simplifies the payment process for everyone involved.
The concept of aob in medical billing dates back decades, emerging as insurance coverage became more prevalent in American healthcare. Initially, patients received all insurance payments and were responsible for settling their accounts with providers. This created significant administrative challenges, payment delays, and collection difficulties that threatened practice sustainability.
Modern revenue cycle management relies heavily on properly executed assignment of benefits agreements. When patients complete intake paperwork, they typically encounter AOB language either as a standalone form or integrated into broader consent documents. Most practices now consider this a standard component of patient registration.
The Legal Framework Governing AOB Agreements
State and federal regulations govern how assignment of benefits functions across different healthcare settings. The American College of Emergency Physicians outlines specific policy positions on honoring valid AOBs to ensure fair and efficient claim payments. These guidelines help standardize practices while recognizing state-level variations in enforcement and requirements.
Key regulatory considerations include:
- Patient signature requirements and consent documentation standards
- Timeframes for obtaining valid authorization before service delivery
- Insurance company obligations to honor properly executed agreements
- Provider responsibilities for maintaining compliant documentation
- State-specific laws that may impose additional requirements or restrictions
Healthcare organizations must navigate these complex regulations while ensuring their intake processes capture necessary authorizations. Practices that fail to obtain proper AOB documentation may find themselves unable to collect directly from insurers, forcing them to pursue patient payments for amounts that insurance should have covered.

How Assignment of Benefits Works in Practice
The practical application of aob in medical billing involves several coordinated steps across the revenue cycle. Understanding this workflow helps practices identify potential breakdown points and optimize their processes.
Step 1: Patient Registration and Authorization
During intake, patients review and sign AOB language authorizing direct insurance payments. This typically occurs before service delivery, though emergency departments may obtain authorization retrospectively. The signed document becomes part of the patient's permanent record.
Step 2: Insurance Verification and Benefits Confirmation
Practice staff verify coverage and benefits while confirming the insurance company will honor the AOB. Professional eligibility verification services help ensure accurate information before services are rendered, reducing the risk of payment complications.
Step 3: Service Delivery and Charge Documentation
Providers deliver care and document all services, procedures, and diagnoses. Accurate clinical documentation directly impacts subsequent billing accuracy and claim success rates.
Step 4: Claim Submission with AOB Indicator
Billing specialists prepare and submit claims to insurance companies, including specific indicators that an assignment of benefits is in effect. On CMS-1500 forms, Box 13 contains the patient's signature authorizing direct payment to the provider.
Step 5: Insurance Adjudication and Payment
The insurance company processes the claim according to coverage terms and sends payment directly to the provider rather than the patient. This direct payment arrangement is the core benefit of the AOB agreement.
Step 6: Patient Responsibility Collection
After insurance payment, any remaining patient responsibility (deductibles, copayments, coinsurance) becomes collectible from the patient. The practice pursues these amounts through standard collection procedures.
Critical Benefits for Healthcare Providers
Assignment of benefits delivers substantial operational and financial advantages that directly impact practice profitability and sustainability. These benefits extend across multiple aspects of revenue cycle management.
Improved Cash Flow and Reduced Collection Costs
Direct insurance payments arrive faster and more reliably than patient payments. Providers avoid the costly process of pursuing payments from patients who received insurance checks but failed to forward them. This streamlined approach significantly reduces days in accounts receivable.
| Metric | Without AOB | With AOB | Improvement |
|---|---|---|---|
| Average Payment Time | 45-60 days | 25-35 days | 30-40% faster |
| Collection Rate | 65-75% | 85-95% | 20-30% higher |
| Administrative Cost per Claim | $8-12 | $4-6 | 50% reduction |
Decreased Administrative Burden
When insurance companies pay providers directly, staff spend less time tracking down patient payments and reconciling accounts. Effective denial management services become more efficient when payment flows follow predictable patterns through AOB arrangements.
Administrative benefits extend to:
- Fewer patient billing inquiries and disputes
- Reduced statement generation and mailing costs
- Lower staffing requirements for collections activities
- Simplified account reconciliation processes
- Decreased write-offs from uncollectible patient balances
Enhanced Patient Satisfaction
Patients appreciate not having to manage insurance reimbursements and forward payments to providers. The simplified process reduces confusion and frustration while allowing patients to focus on their health rather than payment logistics. According to comprehensive resources on AOB, this streamlined approach benefits everyone involved in the payment process.
Implementing Effective AOB Processes
Successful aob in medical billing requires careful attention to documentation, communication, and compliance throughout the patient journey. Practices must establish standardized procedures that capture necessary authorizations while respecting patient rights and preferences.
Documentation Requirements and Best Practices
Valid assignment of benefits agreements must meet specific criteria to ensure insurance companies honor them. Practices should maintain clear policies about when and how AOB authorizations are obtained.
Essential documentation elements include:
- Patient name, date of birth, and identification number
- Clear statement authorizing direct insurance payment to provider
- Patient signature and date of signing
- Witness signature where required by state law
- Specific reference to the services or visit covered
- Language explaining patient rights and responsibilities
Many practices integrate AOB language into comprehensive consent forms that patients sign during registration. While this approach streamlines paperwork, it's crucial that patients understand what they're authorizing. Staff training should emphasize explaining these agreements in clear, accessible language.

Training Staff on AOB Procedures
Front desk personnel, registration specialists, and billing staff all need comprehensive training on assignment of benefits protocols. Each team member plays a role in ensuring proper execution and utilization of these agreements.
Registration staff training should cover:
- How to explain AOB to patients clearly and concisely
- Proper form completion and signature collection techniques
- Verification that all required fields are completed
- Procedures for handling patient questions or concerns
- Documentation standards for electronic health record systems
Billing staff require different training focused on:
- Correctly indicating AOB status on submitted claims
- Recognizing when insurance companies fail to honor valid agreements
- Appealing denials related to AOB disputes
- Understanding state-specific AOB regulations
- Coordinating with payer relations to resolve payment issues
Common Challenges and Solutions
Despite its benefits, aob in medical billing presents certain challenges that practices must navigate carefully. Understanding these potential complications helps organizations develop proactive strategies to minimize disruptions.
Patient Understanding and Consent Issues
Some patients hesitate to sign AOB authorizations because they don't understand the implications or worry about losing control over their insurance benefits. Clear communication is essential to address these concerns.
Effective patient education strategies include:
- Providing simple written explanations of AOB and its benefits
- Training staff to answer common questions confidently
- Offering examples of how the process works in practice
- Emphasizing that AOB doesn't affect their insurance coverage or rights
- Clarifying that they remain responsible for non-covered amounts
Practices should never pressure patients into signing AOB agreements they don't understand. Transparency builds trust and reduces future disputes about payment responsibilities.
Insurance Company Compliance Variations
Not all insurance companies handle AOB agreements identically. Some payers readily honor these authorizations, while others create administrative hurdles or seek technicalities to justify payment denials. Common questions about AOB often relate to payer-specific variations in processing these agreements.
Managing payer variations requires:
- Maintaining documentation of each payer's AOB requirements
- Tracking which companies frequently dispute valid authorizations
- Developing escalation procedures for problematic payers
- Building relationships with payer representatives
- Considering whether to participate with payers who consistently refuse AOB compliance
State-Specific Regulatory Differences
Different states impose varying requirements on assignment of benefits agreements. Some jurisdictions require specific language, witness signatures, or separate standalone forms rather than integrated consent documents.
State regulation variations may involve:
| Regulatory Area | Common Requirements | State Examples |
|---|---|---|
| Form Format | Standalone vs. integrated | New York, Florida |
| Signature Witnessing | Required witness signatures | California, Texas |
| Language Specificity | Mandated disclosure statements | Illinois, Pennsylvania |
| Revocation Rights | Patient ability to cancel AOB | Various states |
Working with experienced revenue cycle management partners helps practices navigate these complexities while maintaining compliance across multiple jurisdictions.
AOB and Specific Healthcare Settings
The application and importance of aob in medical billing varies across different healthcare delivery environments. Each setting faces unique considerations that affect how assignment of benefits functions.
Hospital and Emergency Department Considerations
Emergency departments face particular challenges with AOB since patients often arrive unable to provide consent. Many hospitals obtain retroactive authorization after stabilization, though this approach creates some legal complexity.
Emergency settings benefit from AOB through:
- Reduced bad debt from patients who can't pay large emergency bills
- Improved collection rates on high-dollar claims
- Better cash flow for costly emergency services
- Simplified billing for follow-up care after admission
Hospitals must balance the need for AOB authorization with emergency treatment obligations that prohibit delaying care for administrative tasks. Established policies should clarify when and how emergency departments obtain these authorizations.
Outpatient and Specialty Practice Applications
Outpatient clinics and specialty practices typically have more straightforward AOB processes since services are scheduled rather than emergent. These settings can obtain authorization during pre-registration or at check-in before service delivery.
Specialty practices particularly benefit from AOB when providing:
- High-cost procedures with significant insurance reimbursement
- Services requiring prior authorization and complex billing
- Ongoing treatment series with multiple claim submissions
- Out-of-network care where payment predictability matters
Professional medical billing services help specialty practices optimize their AOB processes while managing the unique billing requirements of their disciplines.
Technology and AOB Management
Modern practice management systems and revenue cycle platforms include functionality specifically designed to support assignment of benefits workflows. Leveraging these technological capabilities enhances efficiency and compliance.
Electronic Consent and Documentation Systems
Digital intake platforms allow patients to review and sign AOB authorizations electronically using tablets or patient portals. These systems automatically store signed documents in the appropriate records and flag missing authorizations before service delivery.
Electronic AOB management offers:
- Automatic compliance checking for required fields
- Integration with electronic health records
- Reduced paper storage and retrieval needs
- Easier audit trail maintenance
- Faster access to authorization documents during claim follow-up
Claim Submission and Payment Posting Automation
Advanced billing software automatically populates AOB indicators on electronic claims based on signed authorizations in the patient record. This automation reduces manual errors and ensures consistent claim submission practices.
Payment posting services become more efficient when systems automatically reconcile insurance payments against submitted claims with AOB indicators. Automation flags discrepancies where insurers fail to honor valid authorizations, triggering immediate follow-up.
Financial Impact on Practice Operations
The decision to consistently use aob in medical billing significantly affects practice financial performance. Quantifying these impacts helps healthcare organizations appreciate the value of robust AOB processes.
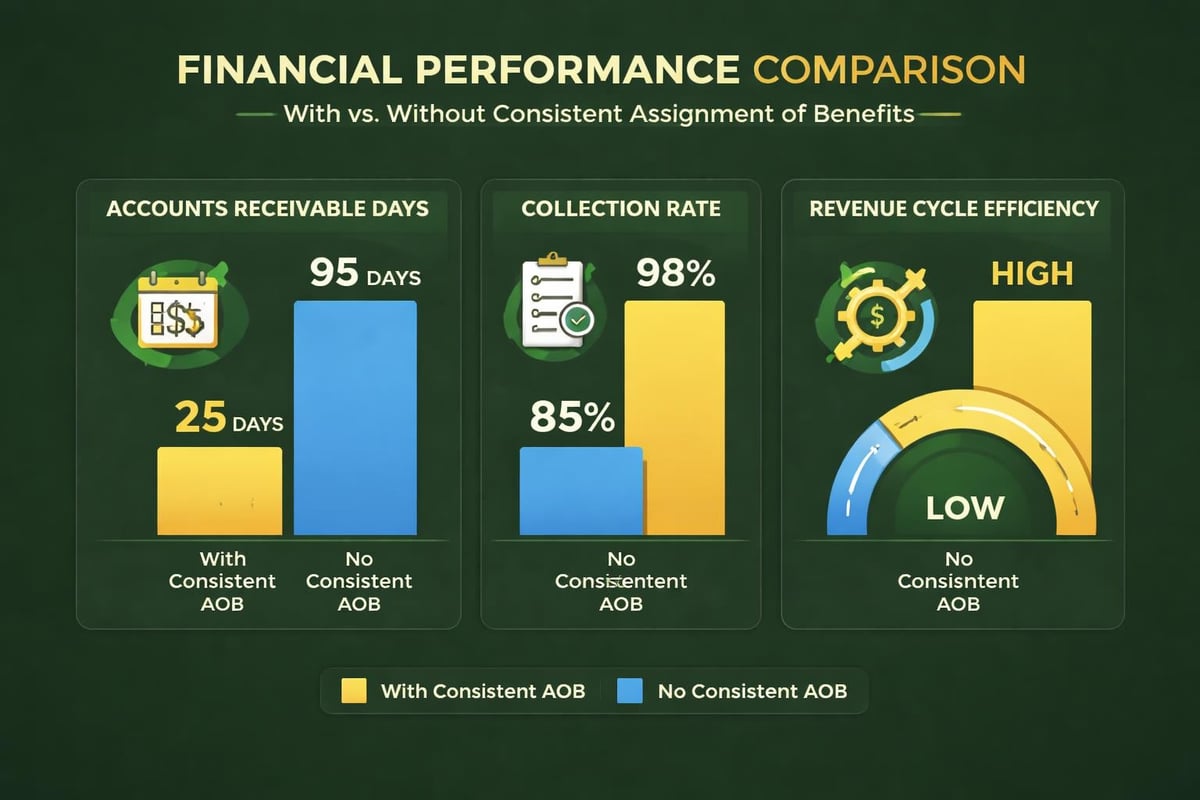
Revenue Cycle Key Performance Indicators
Practices with effective AOB utilization typically demonstrate superior performance across critical revenue cycle metrics. These improvements translate directly to bottom-line financial health.
Measurable improvements include:
- Days in accounts receivable: 15-25% reduction through faster insurance payments
- Net collection rate: 5-10% improvement from fewer uncollectible patient balances
- Cost to collect: 30-40% decrease due to reduced patient collection efforts
- Bad debt write-offs: 20-30% reduction from direct insurance payments
- Cash flow predictability: Substantially improved through consistent payment patterns
Strategic Financial Planning Benefits
Predictable insurance payment timing enables more accurate financial forecasting and cash flow management. Practice administrators can better plan for expenses, investments, and growth initiatives when revenue patterns are reliable.
Strategic advantages extend to:
- More favorable credit terms from improved financial stability
- Better negotiating position with vendors and suppliers
- Ability to invest in practice improvements and technology
- Reduced need for credit lines to cover cash flow gaps
- Enhanced practice valuation for potential buyers or partners
Best Practices for AOB Optimization
Healthcare organizations seeking to maximize the benefits of assignment of benefits should implement comprehensive strategies that address all aspects of the process. These best practices reflect proven approaches from successful practices.
Regular Process Audits and Compliance Reviews
Periodic audits ensure AOB processes remain compliant and effective as regulations and payer requirements evolve. Regular reviews identify gaps, training needs, and opportunities for improvement.
Quarterly audit activities should include:
- Random sampling of patient files to verify proper AOB documentation
- Review of claim denials related to missing or invalid authorizations
- Assessment of staff compliance with documentation protocols
- Evaluation of technology systems supporting AOB workflows
- Analysis of state regulatory changes affecting AOB requirements
Payer Relationship Management
Building strong relationships with insurance company representatives helps resolve AOB-related payment issues more quickly. Regular communication establishes practices as reliable partners who submit clean claims with proper documentation.
Effective payer engagement includes:
- Scheduled meetings with payer representatives to discuss common issues
- Participation in payer advisory councils or provider forums
- Proactive communication about claim submission process changes
- Documentation of payer-specific AOB requirements and preferences
- Escalation protocols for persistent payment problems
Healthcare revenue cycle analytics provide valuable insights into payer-specific performance, helping identify which companies consistently honor AOB agreements and which require additional attention.
Training and Education Strategies
Maintaining high-quality AOB processes requires ongoing staff education and performance monitoring. As team members change and regulations evolve, consistent training ensures everyone understands their responsibilities.
Comprehensive Onboarding Programs
New employees should receive thorough AOB training as part of their onboarding process. This foundation prevents errors and establishes proper habits from the beginning of employment.
Initial training components include:
- Legal and regulatory background on assignment of benefits
- Practice-specific policies and documentation requirements
- Hands-on practice with forms and patient interactions
- Common scenarios and appropriate responses
- Technology systems used to manage AOB processes
Continuing Education and Performance Feedback
Regular refresher training keeps staff current on evolving best practices and regulatory changes. Combining education with performance feedback helps individuals understand how their work contributes to practice success.
Effective continuing education involves:
- Monthly team meetings discussing AOB challenges and solutions
- Quarterly updates on regulatory changes affecting documentation
- Annual comprehensive training covering all aspects of the process
- Individual coaching for staff members showing documentation gaps
- Recognition programs rewarding excellence in AOB compliance
Integration with Broader Revenue Cycle Management
Assignment of benefits doesn't exist in isolation but rather functions as one component of comprehensive revenue cycle management. Understanding these connections helps optimize overall financial performance.
Coordination with Insurance Verification
Eligibility verification processes should confirm not only that patients have active coverage but also that their plans will honor AOB agreements. Some insurance products or specific benefit designs may restrict direct provider payments.
Integrated verification includes:
- Confirming payer acceptance of AOB for specific plan types
- Identifying patients whose policies require alternative payment arrangements
- Documenting verification results in the patient record
- Alerting staff when special handling is needed
- Updating payer policies as companies change AOB requirements
Claims Processing and Submission Alignment
Medical claim submission services must accurately reflect AOB status to ensure proper payment routing. Electronic claims include specific fields indicating that assignment of benefits is in effect, triggering direct provider payment.
Critical alignment points include:
- Automated population of AOB indicators from patient records
- Secondary review to catch missing authorizations before submission
- Tracking of claim status specific to AOB-related issues
- Rapid response when payers indicate AOB problems
- Documentation of all AOB-related claim communications
Denial Management Integration
When insurance companies deny claims or refuse to honor valid AOB agreements, systematic denial management processes must identify and resolve these issues quickly. Delayed response allows payer timely filing deadlines to expire, permanently reducing collectibility.
Effective denial management for AOB issues involves:
- Automated identification of denials related to missing or invalid AOB
- Rapid retrieval of signed authorization documents from patient records
- Standardized appeal letters specifically addressing AOB disputes
- Escalation procedures for payers who consistently reject valid agreements
- Tracking of resolution success rates by payer and denial reason
The Future of Assignment of Benefits
Healthcare payment models continue evolving, raising questions about how aob in medical billing will adapt to emerging trends. Understanding these developments helps practices prepare for future changes.
Value-Based Care and Alternative Payment Models
As healthcare moves toward value-based reimbursement, traditional fee-for-service billing becomes less dominant. However, assignment of benefits principles remain relevant even in bundled payment and capitation arrangements. Practices still need mechanisms to receive payments directly from payers rather than through patients.
Emerging applications include:
- Quality bonus payments directed to providers through AOB mechanisms
- Shared savings distributions from accountable care arrangements
- Episode-based payment bundles assigned to coordinating providers
- Patient-centered medical home reimbursements
- Risk-sharing arrangement settlements
Electronic Consent and Interoperability Standards
Healthcare technology standards increasingly emphasize interoperability and electronic information exchange. Future AOB processes may involve standardized electronic consent mechanisms that insurance companies can verify instantly without manual document review.
Potential developments include:
- Blockchain-based consent verification systems
- Real-time AOB validation during eligibility checks
- Standardized electronic consent formats across all payers
- Patient-controlled authorization management through health apps
- Automated renewal and update processes for ongoing care relationships
Assignment of benefits remains a fundamental component of efficient medical billing operations, directly impacting cash flow, administrative costs, and overall practice financial health. Implementing robust AOB processes requires attention to documentation, staff training, payer relationships, and technology integration across the entire revenue cycle.
Greenhive Billing Solutions brings deep expertise in comprehensive revenue cycle management, including optimized assignment of benefits processes that maximize direct insurance payments while maintaining full compliance. Our experienced team works seamlessly with your existing systems to implement best practices in AOB documentation, claim submission, and denial management. Contact us today to discover how our tailored revenue cycle services can strengthen your practice's financial performance through improved payment efficiency and reduced administrative burden.