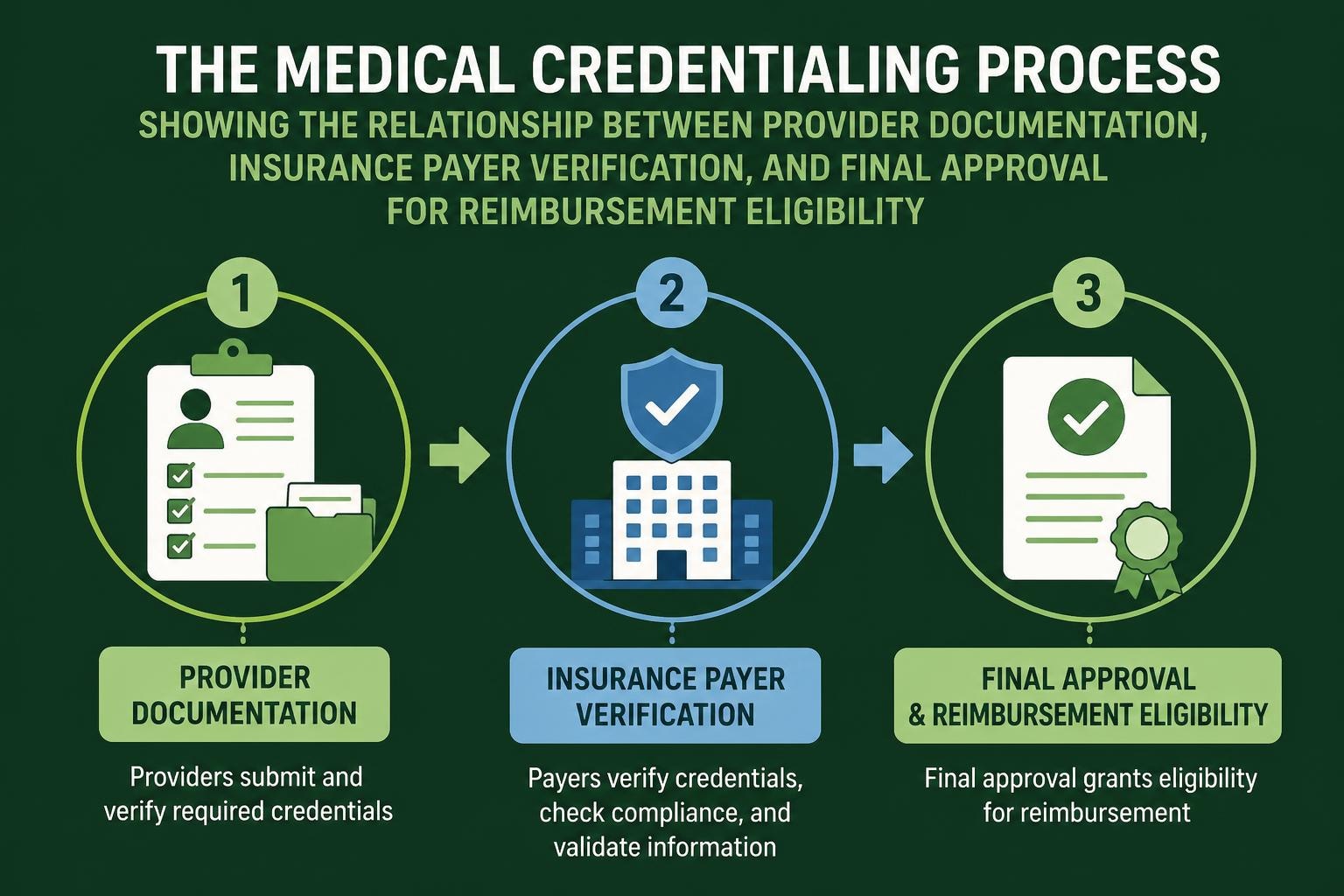
Medical credentialing serves as the foundation for healthcare providers to establish their legitimacy, demonstrate qualifications, and secure contracts with insurance payers. This comprehensive verification process validates the education, training, licensure, and professional history of physicians, nurse practitioners, and other healthcare professionals before they can deliver care and receive reimbursement. For healthcare practices aiming to maintain compliance and optimize their revenue cycle, understanding the nuances of this critical process is essential to avoiding costly delays and ensuring seamless operations.
Understanding the Medical Credentialing Process
Medical credentialing represents a systematic approach to verifying and evaluating the qualifications of healthcare providers. Insurance companies, hospitals, and healthcare facilities require this rigorous evaluation before granting privileges or network participation.
The process involves collecting extensive documentation including medical degrees, board certifications, state licenses, malpractice insurance, work history, and references. Credentialing specialists then verify each credential through primary sources such as medical schools, licensing boards, and certification organizations.
Why Medical Credentialing Matters for Revenue Cycle Performance
Without proper credentialing, healthcare providers cannot bill insurance companies for services rendered. This directly impacts cash flow and revenue generation, making credentialing a critical component of revenue cycle management.
Key financial implications include:
- Delayed revenue until credentialing completes
- Inability to accept insurance patients
- Reduced patient volume and market reach
- Potential denials for non-credentialed providers
- Limited network participation opportunities
The timeline for completing medical credentialing typically ranges from 90 to 180 days, though complex applications or incomplete documentation can extend this period significantly. This comprehensive guide outlines the medical credentialing process with detailed timelines and requirements that practices should anticipate.
Essential Components of Provider Credentialing
Documentation Requirements
Medical credentialing demands meticulous attention to documentation accuracy and completeness. Providers must gather and maintain current versions of multiple credentials simultaneously.
| Document Type | Typical Validity Period | Renewal Considerations |
|---|---|---|
| State Medical License | 1-2 years | Varies by state regulation |
| Board Certification | 10 years | Some require ongoing MOC |
| DEA Registration | 3 years | Federal requirement for prescribers |
| Malpractice Insurance | Annual | Coverage limits must meet requirements |
| CAQH Profile | Ongoing | Update within 120 days of changes |
Primary Source Verification Standards
Credentialing organizations cannot accept provider-supplied documents at face value. They must conduct primary source verification by contacting the original issuing institution directly.
This verification extends to:
- Medical school graduation confirmation
- Residency and fellowship training verification
- Board certification status checks
- State license validation through licensing boards
- National Practitioner Data Bank queries
- Medicare and Medicaid sanctions screening
Third-party verification services streamline this process by maintaining relationships with primary sources and automating verification workflows. However, avoiding common physician credentialing pitfalls requires vigilance throughout every verification step.
Step-by-Step Medical Credentialing Workflow
Step 1: Obtain National Provider Identifier (NPI)
The NPI serves as the unique identification number for healthcare providers across all insurance transactions. Providers must apply through the National Plan and Provider Enumeration System (NPPES) before initiating other credentialing activities.
Step 2: Complete CAQH ProView Enrollment
The Council for Affordable Quality Healthcare (CAQH) ProView database allows providers to maintain a centralized credential file that multiple payers can access. This universal application reduces redundant data entry across different insurance networks.
Step 3: State Medical License Verification
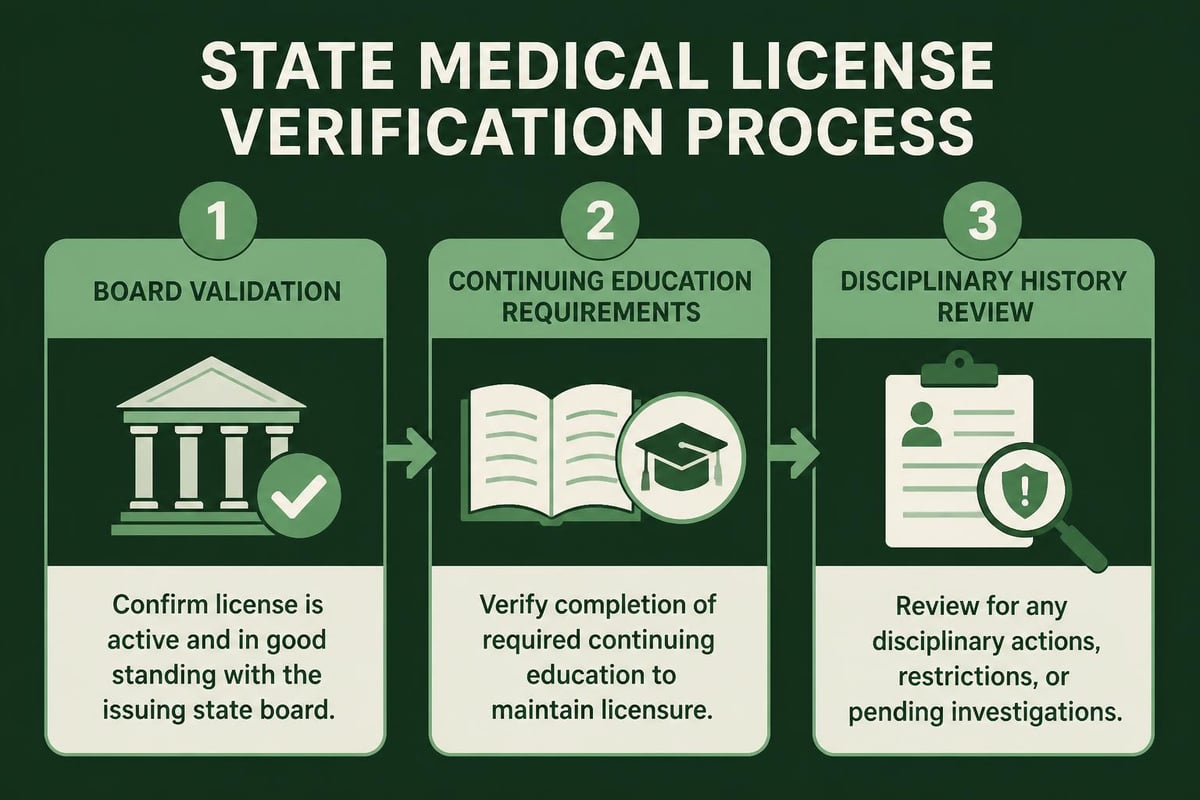
Credentialing specialists verify state licenses directly with medical boards, confirming active status, expiration dates, and any disciplinary actions or restrictions.
Step 4: Insurance Payer Applications
Each insurance company maintains its own credentialing application with specific requirements and formats. Providers must complete separate applications for Medicare, Medicaid, and commercial payers.
Step 5: Hospital Privileges and Affiliations
Hospital credentialing runs parallel to payer credentialing and often includes additional peer references and competency assessments. These privileges must be verified as part of the overall credentialing package.
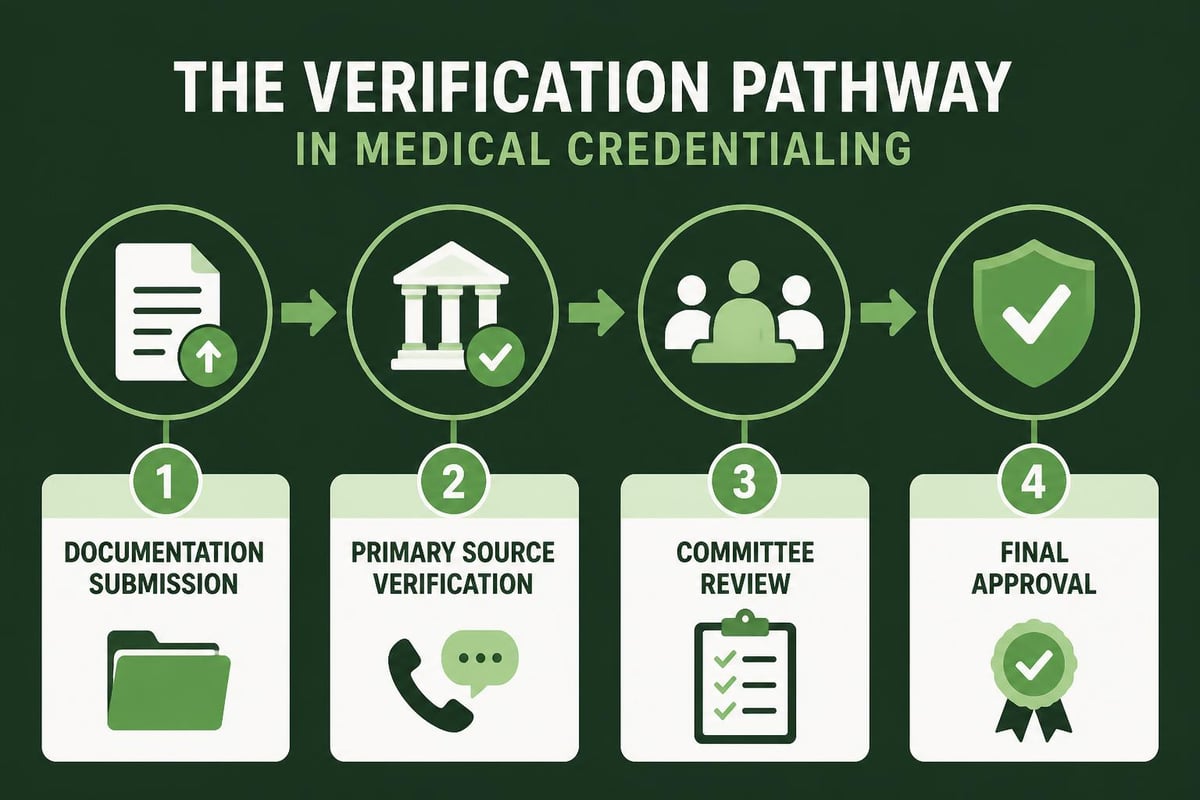
Step 6: Credentialing Committee Review
Applications undergo review by credentialing committees who evaluate all documentation, verification results, and professional qualifications before making approval decisions.
Step 7: Final Approval and Network Participation
Upon approval, providers receive notification of their effective date for network participation and can begin submitting claims for reimbursement.
Common Credentialing Challenges and Solutions
Incomplete or Outdated Documentation
The most frequent obstacle in medical credentialing stems from missing or expired credentials. Providers often underestimate the breadth of documentation required or fail to track expiration dates across multiple credentials.
Solutions for documentation management:
- Implement 90-day renewal reminders for all credentials
- Maintain digital copies with clear organization systems
- Verify information accuracy before submission
- Keep detailed logs of credential expiration dates
- Establish redundant tracking mechanisms
Communication Gaps Between Providers and Payers
Credentialing delays frequently result from poor communication channels or unresponsive verification sources. When verification requests go unanswered, applications stall indefinitely.
Proactive follow-up protocols and relationships with credentialing specialists at payer organizations help overcome these barriers. For practices struggling with these administrative burdens, specialized credentialing services can manage the entire process and maintain consistent communication.
Disciplinary Actions and Red Flags
Any history of malpractice claims, license suspensions, or professional sanctions requires detailed explanation and supporting documentation. Transparency and thorough documentation of remedial actions prove essential when addressing historical concerns.
Best Practices for Streamlined Medical Credentialing
Implementing systematic approaches to credentialing reduces processing time and minimizes errors. Healthcare practices that treat credentialing as an ongoing process rather than a one-time event achieve better outcomes and fewer disruptions.
Centralized Credential Management
Maintaining a centralized repository for all provider credentials creates a single source of truth. This approach to clinician credentialing ensures that updates flow consistently across all applications and verification requests.
Benefits include:
- Reduced duplication of effort
- Faster response to verification requests
- Improved accuracy across applications
- Simplified audit and compliance processes
- Better visibility into credential status
Automation and Technology Integration
Modern credentialing platforms automate routine tasks such as expiration tracking, verification request submission, and status monitoring. These systems integrate with CAQH ProView and payer portals to synchronize data automatically.
| Manual Process | Automated Solution | Time Savings |
|---|---|---|
| Tracking expiration dates | Automated alerts and notifications | 75% reduction |
| Completing redundant forms | Data population from central database | 60% reduction |
| Following up on verifications | Automated status checks and reminders | 50% reduction |
| Document collection | Provider self-service portals | 40% reduction |
Ongoing Monitoring and Maintenance
Medical credentialing never truly ends. Continuous monitoring ensures credentials remain current and compliant while detecting issues before they impact practice operations or reimbursement capabilities.
Managing credentialing effectively requires dedicated staff time or outsourced expertise to handle the ongoing administrative requirements. This becomes particularly important as practices expand provider rosters or add new service locations.
Integration with Broader Revenue Cycle Operations
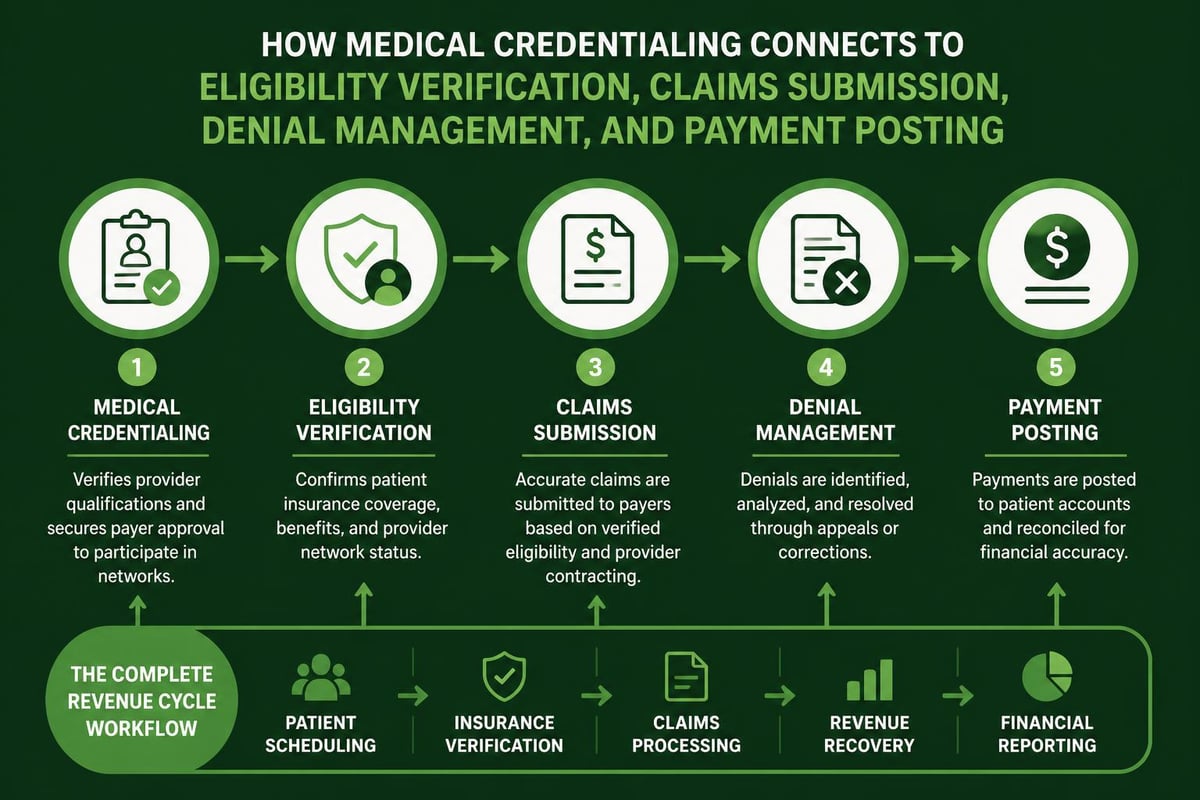
Medical credentialing functions as the gateway to all downstream revenue cycle activities. Without proper credentialing, even perfect eligibility verification and claims submission cannot generate reimbursement.
Credentialing and Denial Management
Credentialing issues frequently surface during claim processing as denials. Non-covered providers, expired credentials, or missing network participation generate denial codes that interrupt revenue flow.
Effective denial management requires identifying whether credentialing gaps contributed to rejections. Addressing these root causes prevents recurring denials and improves clean claim rates.
Timeline Planning for New Providers
Healthcare practices hiring new providers must initiate credentialing immediately to avoid revenue gaps. The standard 120-180 day credentialing timeline means new providers often cannot bill insurance for months after joining a practice.
Strategic planning steps:
- Start credentialing before the provider's start date
- Prepare all documentation in advance
- Submit applications to multiple payers simultaneously
- Track application status weekly
- Prepare for initial cash-pay or delayed billing periods
Organizations can reference credentialing best practices to establish systematic onboarding protocols that minimize revenue disruption when adding providers.
Credentialing for Different Provider Types
Physicians and Advanced Practice Providers
Medical doctors and doctors of osteopathic medicine undergo the most comprehensive credentialing review. Board certifications, fellowship training, and hospital privileges receive particular scrutiny during evaluation.
Nurse practitioners and physician assistants follow similar processes but may require additional documentation regarding collaborative practice agreements or supervision arrangements depending on state regulations.
Allied Health Professionals
Physical therapists, occupational therapists, mental health counselors, and other allied health providers face specialty-specific credentialing requirements. Professional association certifications and state-level practice acts govern their credential verification processes.
Group Practice Considerations
When credentialing multiple providers within a group practice, coordinated applications and batch processing can improve efficiency. However, each provider still requires individual verification and approval regardless of their organizational affiliation.
Regulatory Compliance in Medical Credentialing
Healthcare regulations mandate specific credentialing standards that organizations must follow to maintain compliance and avoid penalties.
The Joint Commission Standards
Accredited hospitals and healthcare facilities must adhere to Joint Commission credentialing and privileging standards. These requirements specify verification timeframes, reappointment cycles, and documentation retention policies.
CMS Enrollment Requirements
Medicare enrollment through the Provider Enrollment, Chain, and Ownership System (PECOS) creates additional credentialing layers for providers serving Medicare beneficiaries. State Medicaid programs maintain separate enrollment systems with unique requirements.
NCQA Credentialing Verification
Health plans accredited by the National Committee for Quality Assurance (NCQA) must follow standardized credentialing and recredentialing processes. These guidelines establish minimum verification standards and maximum processing timeframes.
Re-Credentialing and Ongoing Requirements
Medical credentialing requires periodic renewal, typically every 24 to 36 months depending on payer policies. Re-credentialing follows similar verification processes but may focus primarily on changes since the last review.
Re-credentialing triggers include:
- Standard renewal cycle completion
- Changes in practice location or specialty
- Addition of new licenses or certifications
- Updates to malpractice coverage
- Modifications to group affiliations
Proactive re-credentialing prevents lapses in network participation that could disrupt patient care and revenue flow. Practices should initiate re-credentialing processes at least 90 days before current credentials expire.
Measuring Credentialing Success
Healthcare organizations should track key performance indicators to assess credentialing efficiency and identify improvement opportunities.
| Metric | Industry Benchmark | Improvement Strategies |
|---|---|---|
| Average credentialing time | 90-120 days | Streamline document collection |
| Application error rate | Less than 5% | Implement quality review checkpoints |
| Re-credentialing on-time rate | Greater than 95% | Automated expiration tracking |
| Primary source verification time | 30-45 days | Establish verification relationships |
| Provider satisfaction score | 4.0+ out of 5.0 | Improve communication and transparency |
Regular assessment of these metrics reveals bottlenecks and opportunities for process enhancement. Comparing performance against benchmarks helps practices understand where they excel and where additional resources might improve outcomes.
Cost Considerations and Resource Allocation
Medical credentialing requires significant investment in staff time, technology platforms, and verification services. Understanding these costs helps practices make informed decisions about in-house versus outsourced credentialing management.
Internal Credentialing Costs
Dedicated credentialing staff salaries, benefits, and ongoing training represent the primary expense for in-house operations. Additional costs include:
- CAQH ProView fees
- Primary source verification services
- Credentialing software subscriptions
- Background check services
- Continuing education for credentialing specialists
Outsourced Credentialing Economics
Many healthcare practices partner with specialized credentialing service providers to reduce administrative burden and improve processing efficiency. These arrangements typically involve per-provider fees or monthly retainer agreements that cover all credentialing activities.
The introduction to medical credentialing for new practices highlights how outsourcing can accelerate initial enrollment while allowing practices to focus on clinical operations and patient care.
Medical credentialing forms the essential foundation that enables healthcare providers to participate in insurance networks and receive timely reimbursement for services rendered. By implementing systematic processes, leveraging technology solutions, and maintaining ongoing compliance, practices can minimize delays and optimize their credentialing operations. Greenhive Billing Solutions supports healthcare providers throughout the entire revenue cycle, including comprehensive credentialing management that ensures your providers maintain current credentials and uninterrupted network participation. Our experienced team handles the administrative complexities so you can focus on delivering exceptional patient care while maximizing your practice's financial performance.