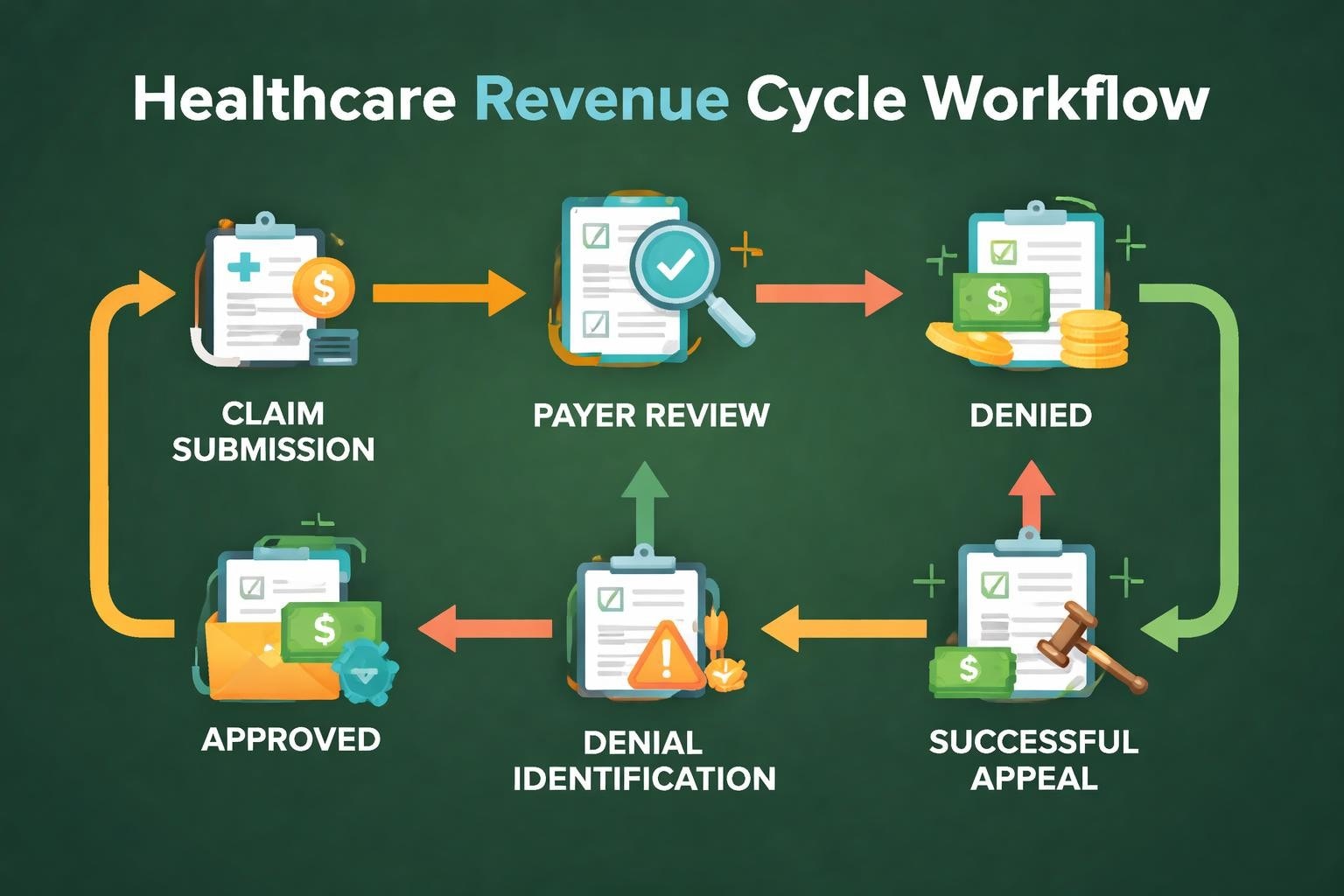
Healthcare providers face a persistent challenge that directly impacts their bottom line: claim denials. With denial rates averaging between 5% and 10% across the industry, the financial stakes have never been higher. Denial management healthcare represents a systematic approach to identifying, correcting, and preventing claim denials before they erode revenue and strain operational resources. For medical practices, hospitals, and healthcare organizations, mastering this critical component of revenue cycle management is no longer optional-it's essential for financial sustainability and operational excellence.
Understanding the Financial Impact of Denial Management Healthcare
Claim denials cost the healthcare industry billions of dollars annually. When a payer rejects a claim, the financial consequences extend far beyond the initial denial amount.
The true cost includes staff time spent investigating denials, resubmitting corrected claims, and managing appeals processes. According to industry research on denial management practices, healthcare organizations typically recover only 63% of denied claims, leaving substantial revenue on the table.
Key financial impacts include:
- Direct revenue loss from unrecovered denials
- Increased administrative costs for rework and appeals
- Delayed cash flow affecting operational budgets
- Resource reallocation from patient care to billing operations
- Potential patient satisfaction issues due to billing confusion
The average cost to rework a single denied claim ranges from $25 to $117, depending on complexity. For a practice processing thousands of claims monthly, these costs accumulate rapidly. Effective denial management healthcare strategies focus on both recovering denied claims and preventing future denials through root cause analysis.

Common Reasons Healthcare Claims Get Denied
Understanding why claims get denied is the foundation of effective denial management healthcare. Payers reject claims for numerous reasons, but certain patterns emerge consistently across specialties.
| Denial Category | Common Causes | Prevention Strategy |
|---|---|---|
| Registration Errors | Incorrect patient demographics, misspelled names, wrong dates of birth | Implement front-end verification processes |
| Eligibility Issues | Expired coverage, inactive policies, out-of-network providers | Verify eligibility in real-time before services |
| Coding Problems | Incorrect CPT/ICD codes, unbundling errors, lack of medical necessity | Ensure certified coders review all claims |
| Authorization Gaps | Missing prior authorizations, expired authorizations | Track authorization requirements by payer |
| Documentation Deficiencies | Incomplete medical records, missing signatures, insufficient notes | Establish documentation standards and audits |
Registration and eligibility errors account for approximately 27% of all claim denials. These preventable mistakes occur at the front end of the revenue cycle and are entirely avoidable with proper eligibility verification services.
Coding-related denials represent another significant category. Medical necessity denials occur when documentation doesn't support the level of service billed or when services don't meet payer criteria. These denials require clinical review and often involve appeals with supporting medical records.
Building a Comprehensive Denial Management Healthcare Framework
An effective denial management healthcare program requires structured processes, dedicated resources, and ongoing performance monitoring. Organizations that treat denial management as a strategic priority consistently outperform those with reactive approaches.
Step 1: Establish Denial Tracking and Categorization Systems
The first step involves implementing systems to capture every denial, regardless of amount. Many practices focus only on high-dollar denials, missing patterns that emerge from smaller, recurring issues.
Create standardized denial categories aligned with your practice's needs. Track denials by payer, denial reason code, service type, provider, and date of service. This granular data reveals trends that inform prevention strategies.
Step 2: Assign Ownership and Accountability
Designate specific team members responsible for denial management activities. Clear ownership ensures denials don't fall through the cracks and establishes accountability for recovery rates.
Consider creating specialized roles:
- Denial analysts who investigate root causes
- Appeals specialists who prepare and submit appeals documentation
- Front-end prevention coordinators who address registration and eligibility issues
- Coding quality reviewers who analyze coding-related denials
Step 3: Develop Standard Operating Procedures for Appeals
Time is critical in denial management healthcare. Most payers impose strict deadlines for appeals, typically 90 to 180 days from the denial date. Develop standardized processes for denial management that ensure timely, complete appeals submissions.
Your procedures should specify:
- Initial denial review protocols
- Documentation requirements for each denial type
- Appeal letter templates and submission formats
- Escalation pathways for complex denials
- Follow-up schedules and tracking mechanisms
Step 4: Implement Performance Metrics and Reporting
What gets measured gets managed. Establish key performance indicators (KPIs) that provide visibility into denial management healthcare effectiveness.
| Metric | Calculation | Target Range |
|---|---|---|
| Denial Rate | (Denied claims / Total claims) × 100 | < 5% |
| Overturn Rate | (Appeals won / Total appeals) × 100 | > 65% |
| Days in AR for Denials | Average age of denied claims | < 30 days |
| Prevention Rate | Reduction in repeat denials quarter-over-quarter | Increasing trend |
| Net Collection Rate | (Payments / [Charges – Adjustments]) × 100 | > 95% |
Regular reporting keeps denial management visible to leadership and drives continuous improvement initiatives.
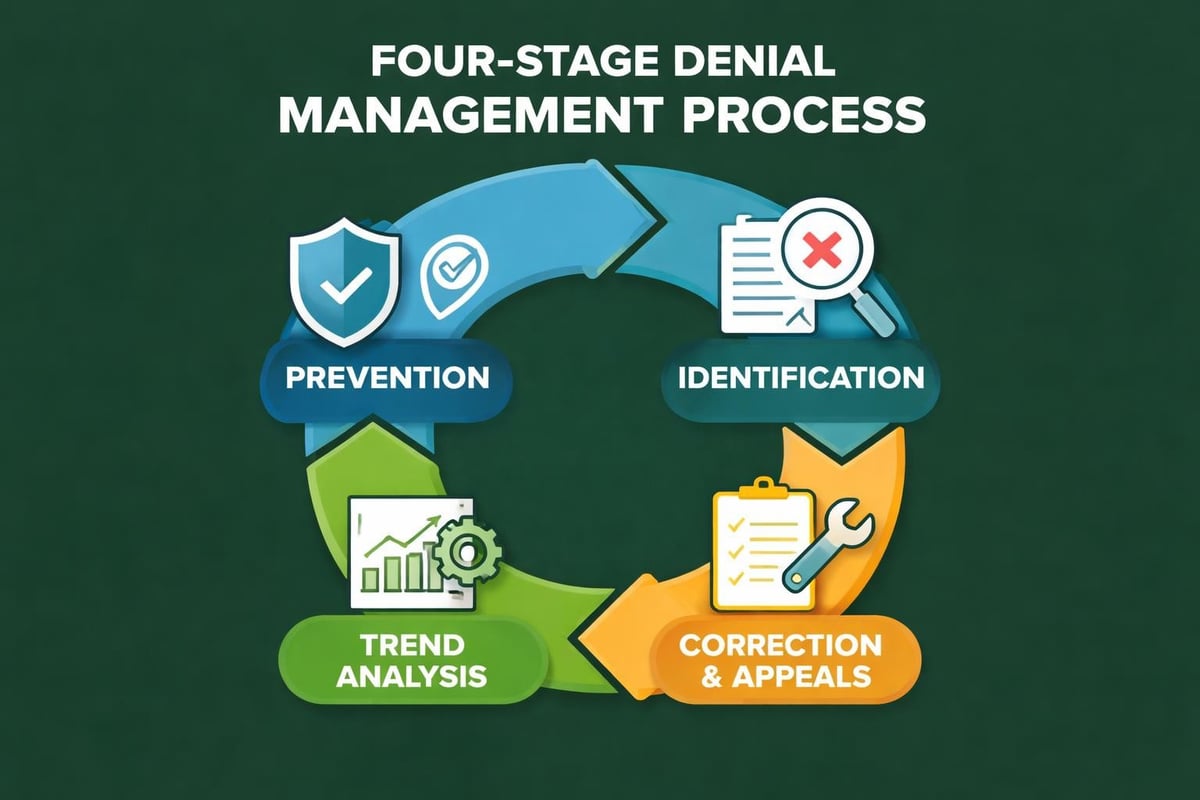
Prevention-Focused Strategies in Denial Management Healthcare
While recovering denied claims is important, preventing denials in the first place delivers greater financial impact. Proactive denial management shifts resources from costly rework to value-adding activities.
Front-End Revenue Cycle Optimization
The majority of preventable denials originate during patient registration and scheduling. Investing in front-end processes yields substantial returns.
Implement these prevention tactics:
- Real-time eligibility verification for every appointment
- Automated insurance card scanning to reduce data entry errors
- Pre-service authorization tracking and management
- Patient liability estimation and collection at time of service
- Demographic data validation against payer databases
Many healthcare organizations partner with specialized medical billing services that have established verification workflows and payer relationships to streamline these processes.
Clinical Documentation Improvement Programs
Physicians and clinical staff don't always document with billing requirements in mind. Bridging this gap between clinical care and billing documentation is essential for denial prevention.
Establish collaborative relationships between clinical and revenue cycle teams. Provide ongoing education about documentation requirements, medical necessity criteria, and common denial triggers. Consider implementing concurrent documentation reviews for high-risk services or procedures.
Coding Quality Assurance Initiatives
Coding accuracy directly impacts claim acceptance rates. Establish quality assurance programs that review coding accuracy before claim submission.
Regular coding audits should examine:
- Appropriate use of evaluation and management levels
- Correct application of modifiers
- Proper bundling and unbundling practices
- Diagnosis code specificity and sequencing
- Alignment between procedures and supporting diagnoses
Pre-submission claim scrubbing identifies errors before payers see them, dramatically reducing denial rates.
Technology and Automation in Denial Management Healthcare
Modern denial management healthcare relies heavily on technology solutions that automate repetitive tasks, identify patterns, and accelerate workflows. While Greenhive Billing Solutions doesn't provide software products, our team leverages industry-standard platforms to deliver comprehensive denial management services.
Automated Denial Tracking and Workflow Management
Manual denial tracking in spreadsheets is inefficient and error-prone. Automated systems capture denials directly from electronic remittance advice (ERA) files, categorize them according to reason codes, and route them to appropriate staff members.
These platforms maintain complete denial histories, track appeal deadlines, and generate work queues prioritized by financial impact and time sensitivity. Automation ensures nothing gets overlooked and provides real-time visibility into denial inventory.
Predictive Analytics and Pattern Recognition
Advanced analytics identify denial trends before they become systemic problems. By analyzing historical denial data, these tools predict which claims are likely to be denied based on specific characteristics.
For example, analytics might reveal that a particular payer consistently denies certain procedure codes when billed with specific diagnosis combinations. Armed with this insight, you can adjust documentation, coding, or authorization processes to prevent future denials.
Integration Across Revenue Cycle Systems
Effective denial management healthcare requires data flow between multiple systems: practice management software, electronic health records, clearinghouses, and payer portals. Integration eliminates manual data transfers and ensures consistency across platforms.
Experienced revenue cycle management teams work within your existing technology infrastructure, optimizing workflows without requiring new software investments.

Payer-Specific Strategies for Denial Management Healthcare
Different payers have different rules, documentation requirements, and approval criteria. Generic denial management approaches miss opportunities for payer-specific optimization.
Understanding Payer Contracts and Policies
Review your contracts with major payers to understand their specific requirements. Pay attention to:
- Authorization requirements by service category
- Documentation standards for different procedure types
- Timely filing limits for initial claims and appeals
- Appeal processes and required supporting materials
- Bundling and unbundling rules specific to each payer
Maintaining payer policy manuals and updating them regularly prevents denials based on policy changes.
Building Payer Relationships
Establishing relationships with payer representatives can expedite appeals and clarify ambiguous requirements. Regular communication with payer networks helps you stay informed about policy updates and emerging denial trends.
For complex denials or unusual circumstances, direct conversations with payer medical directors often resolve issues more efficiently than written appeals.
Medicare and Medicaid Considerations
Government payers have unique requirements that differ from commercial insurance. Medicare Administrative Contractors (MACs) publish Local Coverage Determinations (LCDs) and National Coverage Determinations (NCDs) that specify coverage criteria for services.
Medicaid programs vary by state, with different eligibility requirements, covered services, and billing procedures. Understanding these nuances is critical for practices serving Medicare and Medicaid populations.
Training and Staff Development for Denial Management Healthcare Success
Technology and processes are important, but people drive denial management healthcare outcomes. Investing in staff training and development yields measurable improvements in denial rates and recovery percentages.
Cross-Functional Education Programs
Denial prevention requires collaboration across departments. Develop training programs that educate:
- Front desk staff on registration accuracy and insurance verification
- Clinical staff on documentation requirements and medical necessity
- Coding professionals on payer-specific guidelines and emerging code sets
- Billing staff on claim submission requirements and denial analysis
- Leadership on denial metrics and their financial implications
Comprehensive training on denial management practices ensures everyone understands their role in prevention and recovery.
Certification and Continuing Education
Encourage staff to pursue relevant certifications in medical coding, billing, and revenue cycle management. Certified professionals stay current with industry changes and bring specialized expertise to denial management efforts.
Support ongoing education through:
- Industry conference attendance
- Webinar participation on coding and billing topics
- Professional association memberships
- Internal knowledge-sharing sessions
- Regular updates on payer policy changes
Creating a Culture of Continuous Improvement
The most successful denial management healthcare programs foster cultures where staff proactively identify improvement opportunities. Encourage team members to suggest process enhancements and recognize contributions that reduce denials or improve recovery rates.
Regular team meetings focused on denial trends create opportunities for collaborative problem-solving and knowledge sharing across the organization.
Measuring Success and ROI in Denial Management Healthcare
Demonstrating the value of denial management healthcare investments requires quantifiable metrics that connect activities to financial outcomes.
Key Performance Indicators Beyond Denial Rate
While denial rate is important, it doesn't tell the complete story. Track these additional metrics:
Prevention Metrics:
- First-pass resolution rate (claims paid on first submission)
- Clean claim rate (claims submitted without errors)
- Pre-submission error detection rate
- Authorization approval rate
Recovery Metrics:
- Denial recovery rate by category
- Average time to appeal submission
- Appeal success rate by denial type
- Recovered revenue as percentage of denied amounts
Financial Metrics:
- Net collection rate improvement
- Days in accounts receivable
- Cost per claim processed
- Return on investment for denial management programs
Benchmarking Against Industry Standards
Compare your performance against industry benchmarks to identify improvement opportunities. Healthcare denial management research provides comparative data across specialties and practice sizes.
If your denial rate exceeds industry averages, investigate root causes and implement targeted interventions. If you're performing well, look for opportunities to further optimize and share best practices across your organization.
Calculating Return on Investment
Quantify the financial impact of denial management healthcare initiatives by comparing:
- Revenue recovered from previously denied claims
- Revenue preserved through denial prevention
- Administrative cost reductions from process improvements
- Staff time redirected from rework to value-adding activities
For practices considering outsourced denial management services, calculate the cost of internal denial management against the recovery rates and efficiency gains from specialized providers.
Outsourced Versus In-House Denial Management Healthcare
Healthcare organizations face a strategic decision about whether to manage denials internally or partner with specialized revenue cycle management companies. Each approach has distinct advantages depending on practice size, resources, and strategic priorities.
When In-House Management Makes Sense
Larger organizations with sufficient volume may justify dedicated denial management staff. In-house teams offer:
- Direct control over processes and timelines
- Immediate access to clinical staff for documentation questions
- Deep knowledge of practice-specific workflows and preferences
- Integration with existing revenue cycle teams
However, maintaining in-house expertise requires ongoing investments in training, technology, and staff retention.
Benefits of Specialized Revenue Cycle Partners
Many practices find that partnering with experienced revenue cycle management providers delivers superior results at lower total cost. Specialized teams bring:
- Dedicated expertise in denial identification and appeals
- Established relationships with major payers
- Scalable resources that flex with claim volume
- Advanced technology platforms without capital investment
- Performance-based accountability for recovery rates
Outsourced partners handle the full denial management healthcare lifecycle, from initial identification through final appeal, allowing internal staff to focus on patient care and strategic initiatives.
Hybrid Approaches
Some organizations adopt hybrid models, maintaining oversight and high-level strategy internally while outsourcing day-to-day denial management operations. This approach combines control with specialized expertise and can be particularly effective for practices in transition or growth phases.
Effective denial management healthcare transforms revenue cycle performance by recovering lost revenue and preventing future denials through systematic process improvements. Healthcare organizations that prioritize denial management see measurable improvements in cash flow, operational efficiency, and financial sustainability. Greenhive Billing Solutions partners with healthcare providers nationwide to deliver comprehensive denial management in medical billing, combining specialized expertise with proven processes to maximize claim acceptance and recovery rates. Contact Greenhive Billing Solutions to learn how our tailored revenue cycle management services can strengthen your practice's financial performance.