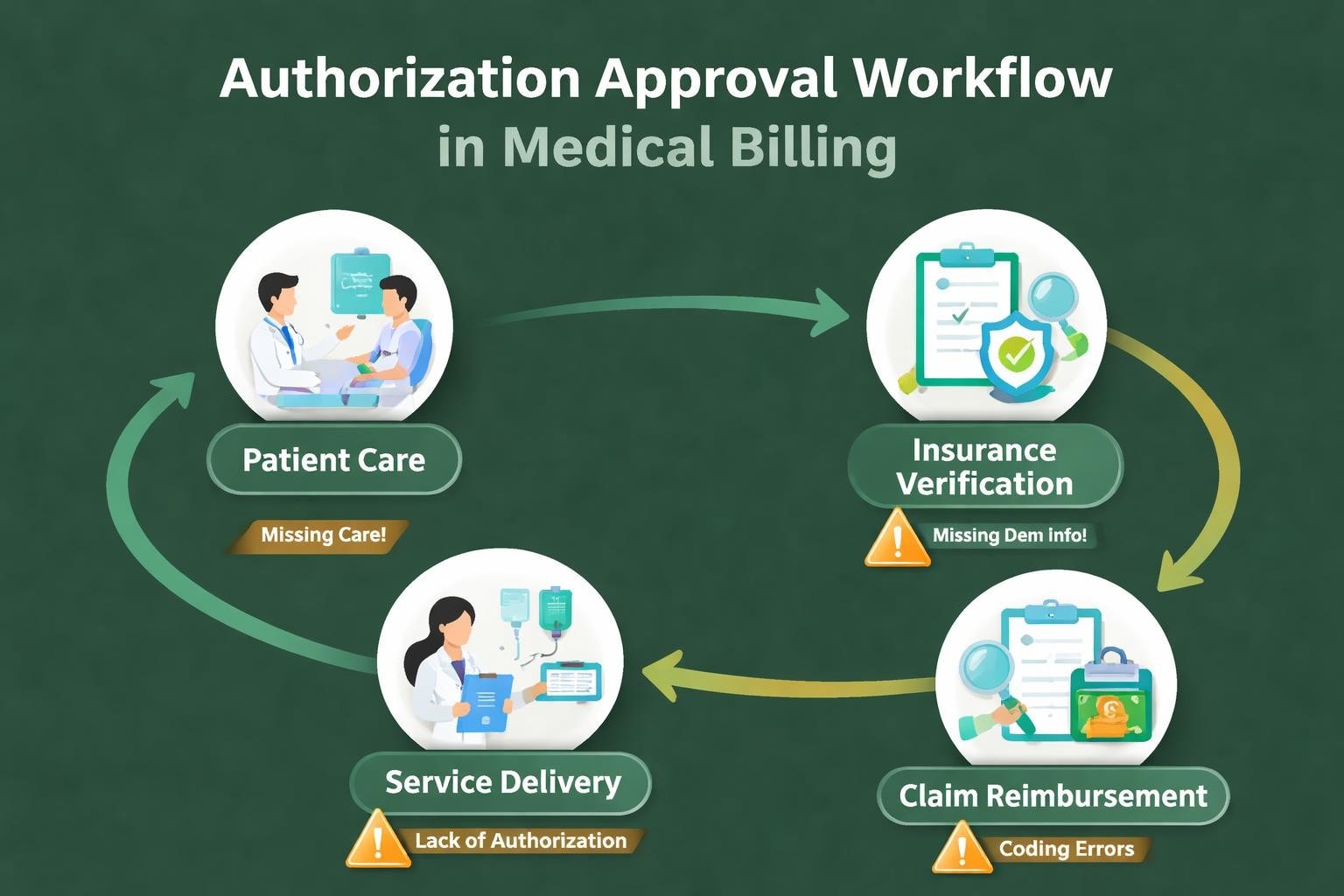
Authorization denial in medical billing represents one of the most financially damaging obstacles healthcare providers face when seeking reimbursement for services rendered. When insurance companies reject claims due to missing, incomplete, or invalid prior authorizations, practices experience immediate revenue disruption and long-term administrative burdens. Understanding the root causes, prevention strategies, and resolution methods for these denials is essential for maintaining healthy cash flow and operational efficiency. Revenue cycle management requires constant vigilance around authorization requirements, as payer policies evolve frequently and vary significantly across different insurance carriers and plan types.
Understanding Authorization Requirements in Medical Billing
Prior authorization serves as a utilization management tool that insurance companies use to determine medical necessity before approving coverage for specific services, procedures, or medications. This pre-approval process requires healthcare providers to submit clinical documentation demonstrating that proposed treatments meet payer-defined criteria for coverage. Authorization in medical billing functions as a gatekeeper mechanism that insurers employ to control costs and prevent unnecessary procedures.
The authorization process typically involves several distinct steps that providers must navigate carefully. Healthcare facilities must first identify which services require pre-approval based on payer contracts and coverage policies. Once identified, clinical staff submit authorization requests accompanied by supporting medical records, diagnostic reports, and treatment justification. Payers then review these submissions against their medical policies and either approve, deny, or request additional information.
Services That Commonly Require Prior Authorization
Different service categories trigger authorization requirements depending on payer policies and plan structures. Understanding which procedures typically need pre-approval helps practices implement preventive workflows.
High-cost diagnostic imaging procedures including MRI, CT scans, and PET scans almost universally require authorization across commercial and government payers. These expensive tests represent significant utilization management opportunities for insurers seeking to reduce unnecessary imaging expenses.
Surgical procedures and inpatient admissions constitute another major category requiring pre-authorization. Elective surgeries, especially those with alternative treatment options, face rigorous scrutiny from insurance medical directors before receiving approval.
- Specialty medications and biologics
- Durable medical equipment exceeding specific cost thresholds
- Physical therapy beyond initial evaluation visits
- Mental health and substance abuse treatment programs
- Home health services and skilled nursing facility placements

Root Causes of Authorization Denial in Medical Billing
Authorization denial in medical billing stems from multiple factors ranging from administrative oversights to clinical documentation deficiencies. Identifying these underlying causes enables practices to implement targeted prevention strategies that reduce denial rates.
Missing authorization numbers represent the most straightforward denial scenario. When providers submit claims without obtaining required pre-approval or fail to include valid authorization reference numbers, CO-15 denial codes indicate this fundamental deficiency. These denials are entirely preventable through proper workflow implementation.
Documentation and Timing Issues
Clinical documentation failures contribute significantly to authorization denials even when providers submit requests properly. Insufficient medical necessity justification, incomplete diagnostic information, or missing clinical notes give payer medical reviewers insufficient basis for approval.
Timing represents another critical factor in the authorization denial landscape. Requests submitted after service delivery typically face automatic rejection, as most payers require prospective authorization rather than retroactive approval. Similarly, authorizations obtained but expired before service dates create claim denial situations that practices must address through appeals or patient responsibility assignments.
| Denial Cause | Frequency | Prevention Strategy |
|---|---|---|
| Missing authorization number | Very High | Automated verification systems |
| Expired authorization | High | Calendar tracking and alerts |
| Service not covered | Medium | Eligibility verification upfront |
| Insufficient clinical documentation | High | Standardized submission templates |
| Wrong procedure codes | Medium | Regular coding audits |
Financial Impact of Authorization Denials on Healthcare Practices
The financial consequences of authorization denial in medical billing extend far beyond the immediate claim rejection. Practices experience direct revenue loss when services are denied, requiring either patient collection efforts or complete write-offs depending on contractual obligations and state regulations.
Administrative costs compound these direct losses substantially. Staff must invest significant time researching denial reasons, gathering additional documentation, and submitting appeals through payer-specific channels. This rework diverts resources from productive revenue cycle activities and creates bottlenecks in claim processing workflows.
Cash flow disruption occurs when expected reimbursements fail to materialize according to projected timelines. Practices relying on steady revenue streams to meet operational expenses face potential shortfalls when authorization denials create payment delays extending 30 to 90 days or longer.
Hidden Operational Costs
Beyond immediate financial metrics, authorization denials generate hidden costs that impact overall practice performance. Patient satisfaction suffers when billing complications arise from authorization issues, potentially damaging relationships and generating negative reviews. Staff morale declines when team members face repetitive denial resolution tasks that feel preventable.
Opportunity costs emerge as skilled billing professionals spend hours addressing authorization denials rather than optimizing other revenue cycle components. These professionals could instead focus on charge capture improvements, payer contract negotiations, or patient financial counseling initiatives that generate positive returns.
Prevention Strategies for Authorization Denials
Preventing authorization denial in medical billing requires comprehensive workflows that span from patient scheduling through claim submission. Proactive strategies implemented consistently across all service lines deliver measurable denial rate reductions.
Eligibility verification services form the foundation of authorization prevention programs. Real-time benefit checks performed during scheduling identify authorization requirements specific to each patient's insurance plan and service type. This upfront verification enables practices to obtain necessary approvals before appointments occur.
Step-by-Step Authorization Management Process
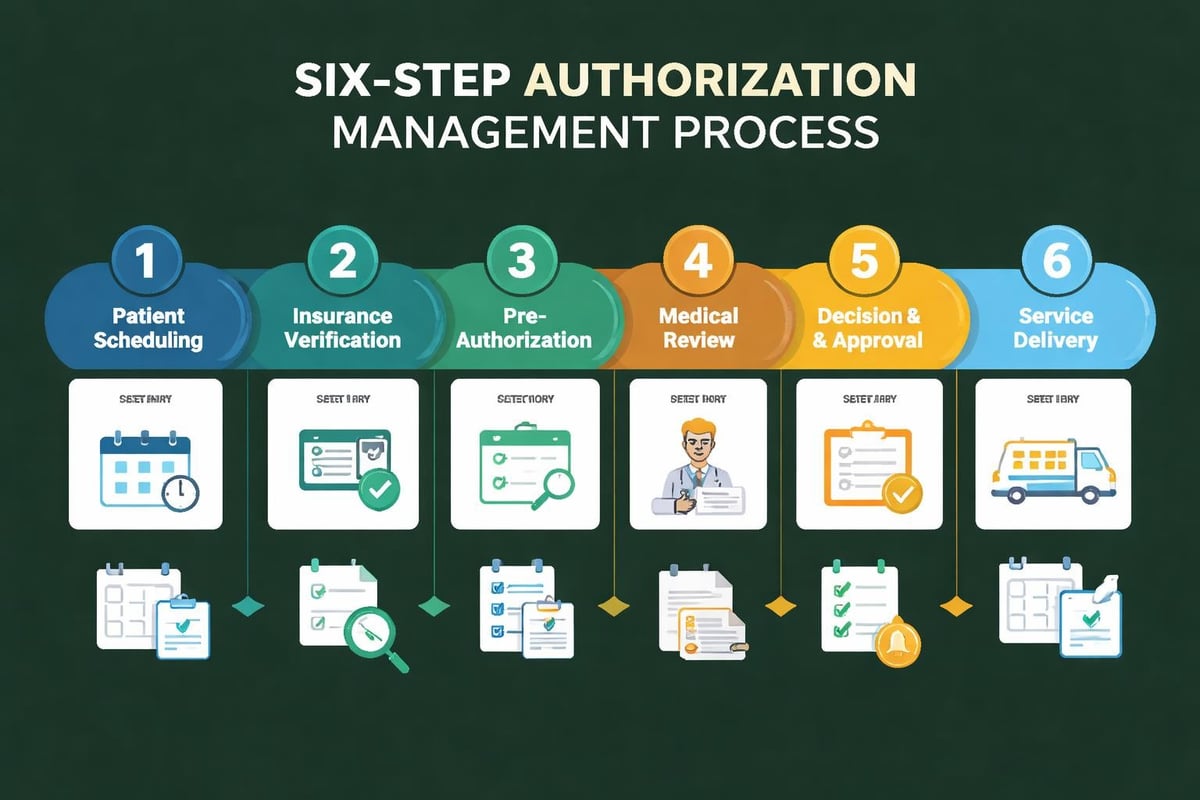
Implementing structured authorization workflows ensures consistent compliance with payer requirements across all team members and service locations.
Step 1: Schedule patient appointment and collect complete insurance information including member ID, group number, and policy effective dates.
Step 2: Verify benefits and authorization requirements through payer portals or electronic verification systems within 24 hours of scheduling.
Step 3: Submit authorization requests with comprehensive clinical documentation at least 5-7 business days before scheduled service dates.
Step 4: Follow up on pending authorization requests 48-72 hours after submission to identify any outstanding information requests.
Step 5: Document authorization approval numbers in practice management systems and link to scheduled appointments.
Step 6: Confirm authorization validity immediately before service delivery to catch any cancellations or modifications.
Technology integration amplifies prevention effectiveness by automating manual verification tasks and providing real-time alerts. Prior authorization services leverage specialized platforms that interface with multiple payer systems simultaneously, reducing staff workload while improving accuracy.
Resolving Authorization Denials Through Effective Appeals
When authorization denial in medical billing occurs despite prevention efforts, rapid response through structured appeals processes becomes essential for revenue recovery. Understanding payer-specific appeal requirements and deadlines enables practices to maximize overturn rates.
Initial appeal submissions should address the specific denial reason documented in the remittance advice. Common denial codes provide insight into whether denials stem from missing information, medical necessity questions, or procedural issues that require different resolution approaches.
Documentation Requirements for Successful Appeals
Strong appeal submissions include comprehensive clinical documentation that establishes medical necessity beyond the initial authorization request. Progress notes, diagnostic test results, specialist consultations, and evidence-based treatment guidelines strengthen the clinical rationale for covered services.
Peer-to-peer reviews offer valuable appeal escalation options when initial written appeals fail. These physician-to-physician conversations allow treating providers to explain clinical decision-making directly to insurance medical directors, often resulting in approval reversals that written documentation alone cannot achieve.
- Complete patient medical history relevant to the service
- Current clinical findings supporting treatment necessity
- Failed conservative treatment documentation when applicable
- Specialty society guidelines supporting the proposed intervention
- Comparison to payer medical policy criteria
Common Authorization Denial Scenarios and Solutions
Certain authorization denial patterns emerge repeatedly across healthcare practices regardless of specialty or payer mix. Recognizing these scenarios enables targeted intervention strategies that prevent recurrence.
Approved authorizations that still generate denials represent particularly frustrating situations for providers. These denials typically occur due to mismatches between authorized services and billed procedure codes, exceeding authorized unit limits, or services rendered outside approved date ranges.
Specialty-Specific Authorization Challenges
Different medical specialties face unique authorization denial risks based on their service patterns and payer scrutiny levels. Behavioral health providers encounter frequent authorization denials for ongoing therapy sessions beyond initial approved visit allotments. Medical billing for behavioral health requires meticulous session tracking and proactive reauthorization submissions.
Cardiology practices experience authorization challenges around diagnostic testing sequences and interventional procedures. Payers often require conservative treatment documentation before approving advanced imaging or catheterization procedures, creating potential denial scenarios when documentation gaps exist.
| Specialty | Common Authorization Issue | Solution Approach |
|---|---|---|
| Behavioral Health | Session limit exhaustion | Automated visit tracking |
| Cardiology | Diagnostic testing sequence | Protocol checklists |
| Orthopedics | Surgical medical necessity | Pre-surgical documentation review |
| Pain Management | Injection frequency limits | Treatment plan coordination |
| Oncology | Chemotherapy regimen changes | Physician attestation forms |
Staff Training and Workflow Optimization
Reducing authorization denial in medical billing requires ongoing staff education and workflow refinement. Team members across scheduling, clinical, and billing departments must understand their roles in authorization management and execute responsibilities consistently.
Regular training sessions should cover payer policy updates, common denial patterns identified through internal audits, and corrective action protocols. Creating specialty-specific authorization reference guides helps staff quickly access requirements for frequently performed procedures without researching each case individually.
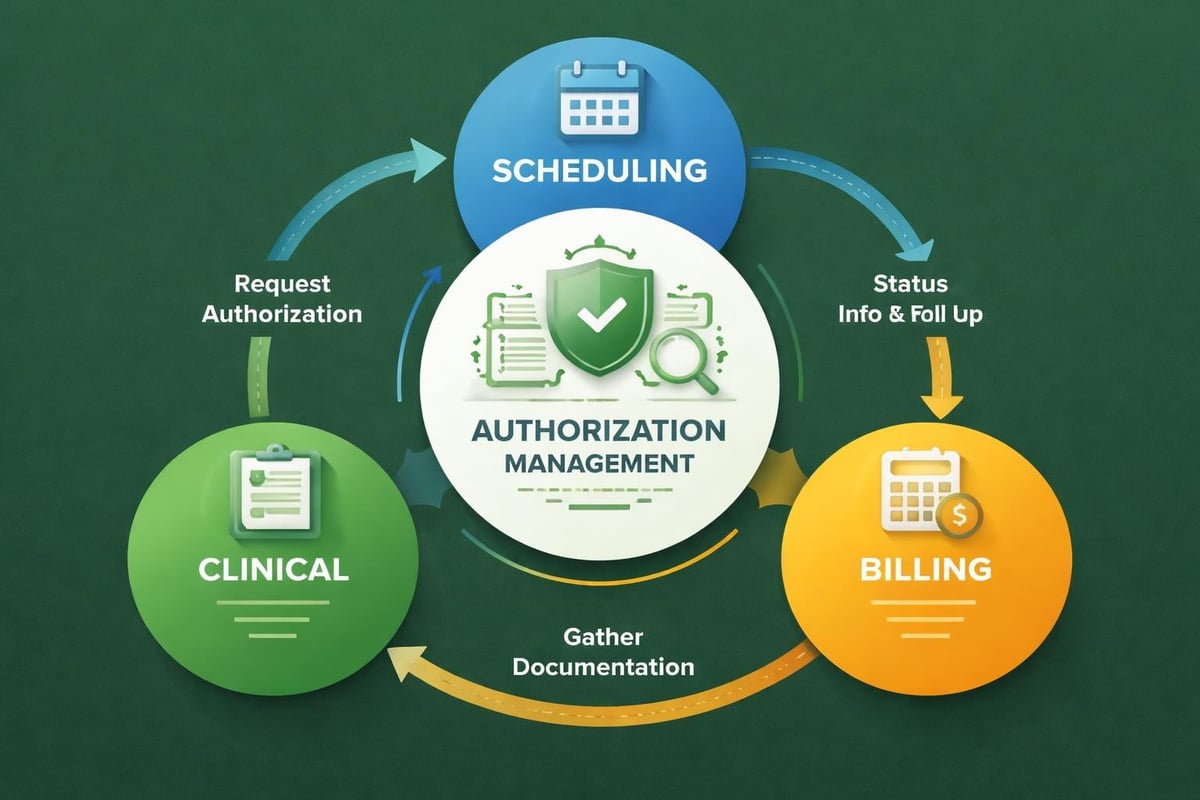
Cross-Departmental Communication Protocols
Authorization management succeeds only when information flows seamlessly between patient access, clinical care, and revenue cycle teams. Scheduling staff must alert billing teams about services scheduled that require authorization. Clinical staff must understand documentation standards that support authorization approvals and subsequent claim adjudication.
Weekly authorization status meetings bring stakeholders together to review pending requests, address outstanding information needs, and resolve authorization-related patient access barriers. These collaborative sessions identify systemic issues requiring workflow modifications rather than individual case interventions.
Standardized communication templates ensure consistent information exchange across departments. Authorization tracking spreadsheets accessible to all relevant team members provide real-time visibility into request status, approval numbers, and approved service parameters.
Technology Solutions for Authorization Management
Modern revenue cycle technology platforms offer sophisticated authorization management capabilities that reduce manual effort while improving accuracy. Electronic prior authorization systems connect directly with payer platforms, enabling real-time submission and status checking without phone calls or fax transmissions.
Artificial intelligence applications increasingly support authorization workflows through predictive analytics that identify high-risk services likely to require pre-approval. These systems analyze historical authorization patterns and automatically flag scheduled services matching denial risk profiles, prompting proactive verification.
Integration With Practice Management Systems
Seamless integration between authorization platforms and practice management systems eliminates duplicate data entry and ensures authorization information travels with patient accounts throughout the revenue cycle. Authorization numbers automatically populate claim forms, reducing keying errors that generate denials.
Calendar-based alerts notify staff when authorizations approach expiration dates for patients with ongoing treatment plans. These proactive notifications enable timely reauthorization requests that prevent service interruptions and claim denials. Denial management services often include technology implementation support to optimize system configurations for individual practice workflows.
Metrics and Performance Monitoring
Measuring authorization denial rates and tracking trends over time provides essential feedback about prevention strategy effectiveness. Practices should calculate authorization denial rates by payer, service type, and responsible staff member to identify improvement opportunities.
Key performance indicators for authorization management include authorization request turnaround time, approval rate percentage, appeal success rate, and revenue recovered through appeals. Comparing these metrics against industry benchmarks helps practices assess their relative performance and set realistic improvement goals.
Monthly dashboard reporting makes authorization performance visible to leadership and staff, creating accountability for sustained improvement. Healthcare revenue cycle analytics platforms consolidate authorization metrics alongside other denial categories, providing comprehensive revenue cycle visibility.
Continuous Improvement Through Root Cause Analysis
When authorization denials occur, conducting root cause analysis identifies whether denials stem from knowledge gaps, process failures, or external factors beyond practice control. This analytical approach transforms denials from frustrating setbacks into learning opportunities that strengthen future performance.
Quarterly review sessions examining denied cases in detail reveal patterns requiring corrective action. Perhaps certain procedure codes consistently trigger denials due to documentation deficiencies, or specific payers demonstrate particularly stringent authorization requirements that demand enhanced protocols.
Payer Contract Considerations and Negotiations
Authorization requirements specified in payer contracts significantly impact denial risk and administrative burden. During contract negotiations, practices should carefully review authorization provisions and seek favorable terms that minimize operational complexity.
Negotiating extended authorization validity periods reduces reauthorization frequency for patients requiring ongoing treatment. Requesting elimination of authorization requirements for established patient follow-up visits can substantially decrease administrative workload for primary care and specialty practices.
Contractual language clarity around authorization obligations protects practices from ambiguous requirements that create disputes during claim adjudication. Contracts should specify which procedure codes require authorization, acceptable submission timeframes, and appeal rights when authorization requests are denied.
Understanding ways to reduce denials in medical billing includes recognizing that some denial patterns stem from unreasonable contractual terms rather than practice performance deficiencies. Armed with denial data, practices can approach payer representatives with specific examples supporting requests for contract modifications during renewal negotiations.
Patient Communication About Authorization Requirements
Transparent patient communication about authorization requirements and potential delays helps manage expectations and maintain satisfaction even when approval challenges arise. Practices should inform patients during scheduling when services require pre-authorization and estimated approval timeframes.
Written financial policies should explain that authorization approval does not guarantee payment and that patients remain financially responsible for services their insurance ultimately denies. This disclosure protects practices from patient disputes when authorization approvals are later reversed or services are deemed not covered despite initial approval.
Handling Authorization Denials That Impact Patient Access
When authorization requests are denied and services cannot proceed as scheduled, compassionate patient communication becomes critical. Staff should explain denial reasons in plain language, outline appeal options the practice will pursue, and discuss alternative treatment approaches if applicable.
For non-emergent services, practices may choose to delay service delivery until appeal resolutions occur rather than exposing patients to potential financial responsibility. This patient-centered approach builds trust and demonstrates commitment to advocacy beyond immediate revenue considerations.
Offering payment plan options or financial assistance programs for patients who choose to proceed with denied services helps maintain access while protecting practice revenue. Clear advance beneficiary notices (ABNs) properly executed before service delivery establish patient financial responsibility for Medicare beneficiaries when authorization or coverage questions exist.
Authorization denial in medical billing creates significant financial and operational challenges that require comprehensive prevention strategies, efficient resolution workflows, and ongoing performance monitoring. By implementing proactive verification processes, maintaining detailed clinical documentation, and leveraging technology solutions, healthcare practices can substantially reduce authorization denial rates and accelerate revenue realization. Greenhive Billing Solutions provides comprehensive denial management and prior authorization services that help healthcare providers navigate complex payer requirements while maximizing reimbursement. Our experienced team works within your existing systems to verify coverage, obtain authorizations, and resolve denials efficiently, allowing your clinical staff to focus on patient care.