Healthcare providers face mounting pressure to maintain financial stability while delivering exceptional patient care. At the heart of this challenge lies the claim processing system in healthcare, a critical component that determines whether practices receive timely, accurate reimbursement for services rendered. Understanding how these systems function, the challenges they present, and strategies for optimization can dramatically impact a practice's bottom line. For revenue cycle management professionals and healthcare administrators, mastering claim processing workflows represents one of the most direct paths to improved financial performance.
Understanding the Claim Processing System in Healthcare
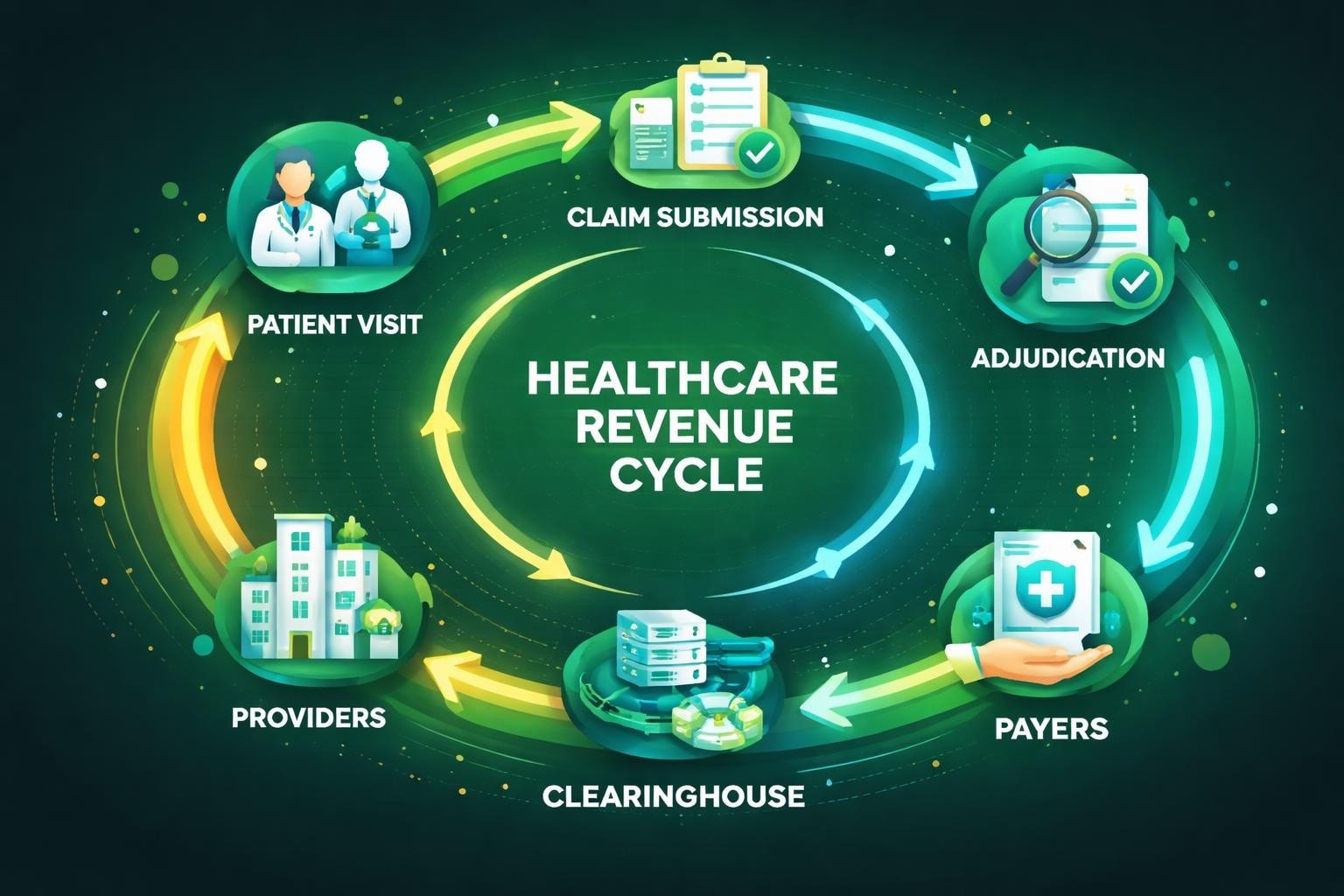
A claim processing system in healthcare encompasses the entire lifecycle of a medical claim, from initial service documentation through final payment or denial resolution. This complex ecosystem involves multiple stakeholders, including healthcare providers, billing specialists, insurance companies, clearinghouses, and regulatory bodies. Each entity plays a specific role in ensuring that claims are submitted accurately, reviewed thoroughly, and paid appropriately.
The primary objective of any effective claim processing system is to translate clinical services into standardized billing codes that payers can evaluate and reimburse. This translation requires precise documentation, coding expertise, and compliance with ever-changing payer requirements. When executed properly, the system facilitates smooth cash flow and minimizes administrative burden. When mismanaged, it leads to payment delays, denials, and revenue loss.
Core Components of Modern Claim Processing
Modern claim processing relies on several interconnected components that work together to move claims from submission to payment:
- Patient registration and insurance verification establish eligibility before services are rendered
- Charge capture and coding translate clinical documentation into billable services
- Claims submission delivers formatted claims to the appropriate payers
- Adjudication allows payers to review and determine payment amounts
- Payment posting and reconciliation record received payments against outstanding balances
- Denial management addresses rejected claims and initiates appeals when necessary
Understanding each component helps practices identify bottlenecks and implement targeted improvements. The American Medical Association provides comprehensive resources on claims processing best practices that healthcare providers can leverage to strengthen their revenue cycle operations.
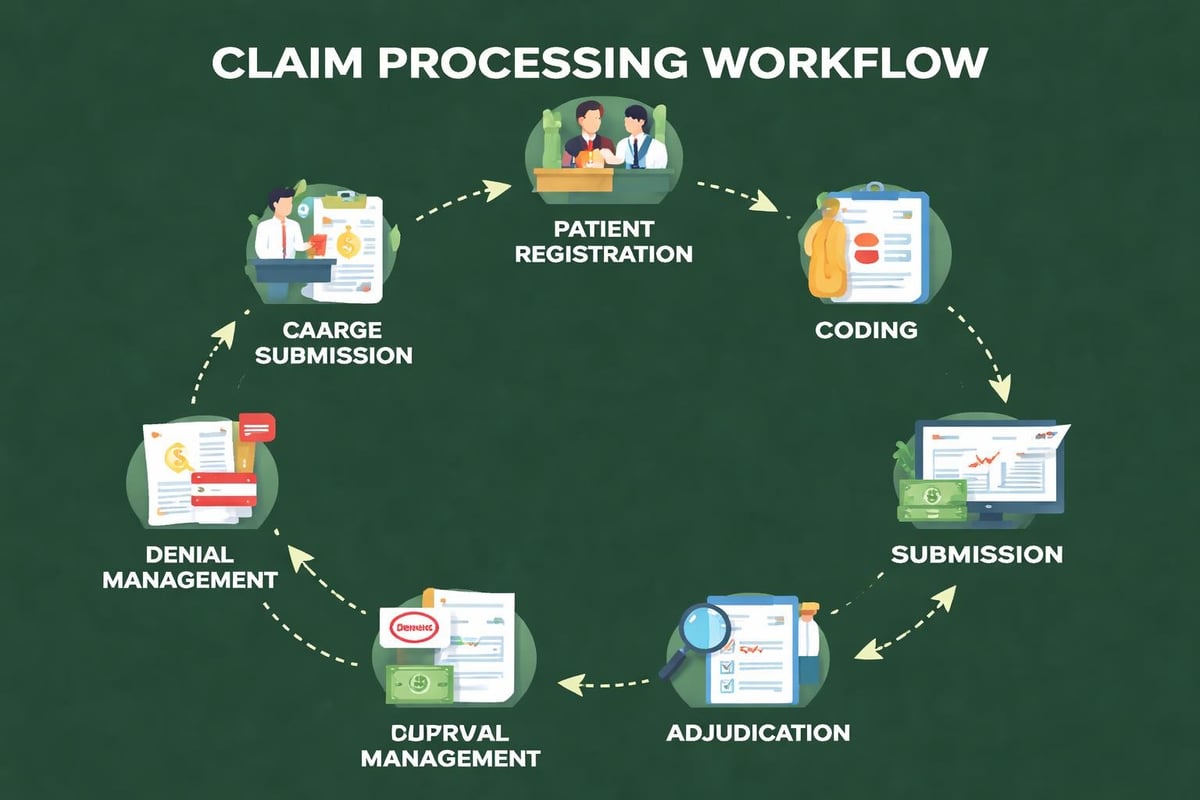
Critical Stages in the Claims Processing Workflow
The claim processing system in healthcare follows a sequential workflow, though many activities occur simultaneously or require iteration when issues arise. Each stage demands attention to detail and adherence to established protocols.
Stage 1: Pre-Service Preparation
Before any claim enters the processing system, foundational work must occur. Insurance verification confirms patient coverage, benefit levels, and authorization requirements. This step prevents downstream denials related to eligibility or coverage limitations. Front-end accuracy directly correlates with back-end success rates.
Demographic data collection ensures that patient information matches payer records exactly. Even minor discrepancies in name spelling, date of birth, or insurance identification numbers can trigger automatic rejections. Establishing standardized data collection protocols minimizes these preventable errors.
Stage 2: Documentation and Coding
Clinical documentation provides the source material for medical coding professionals who assign procedure and diagnosis codes. The specificity and completeness of provider documentation directly impact coding accuracy. Understanding what is a billing and coding specialist reveals why these professionals serve as crucial intermediaries between clinical care and financial reimbursement.
Proper code selection requires knowledge of current procedural terminology, ICD-10 diagnosis codes, and payer-specific billing rules. Modifiers add nuance to procedures, clarifying circumstances that affect reimbursement. Incorrect modifier usage represents a common source of denials that experienced billing teams proactively address.
Stage 3: Claim Scrubbing and Submission
Before submission, claims undergo scrubbing to identify potential errors or missing information. Automated systems check for common mistakes like invalid code combinations, missing referral numbers, or incomplete provider credentials. This quality control step significantly reduces the rate of immediate rejections.
Claims are then transmitted electronically to payers or clearinghouses. Electronic submission has become the standard, offering faster processing times and automated acknowledgment receipts. The claims processing workflow has evolved substantially with technological advancement, enabling real-time tracking and status updates.
Stage 4: Payer Adjudication
Once received, payers adjudicate claims by reviewing submitted information against coverage policies, contracted rates, and medical necessity criteria. This process determines whether claims are approved, partially paid, or denied. Adjudication timelines vary by payer and claim complexity, ranging from days to several weeks.
| Adjudication Outcome | Meaning | Next Steps |
|---|---|---|
| Paid in Full | Claim approved at submitted amount | Post payment and close claim |
| Partially Paid | Some charges reduced or denied | Review explanation of benefits, appeal if warranted |
| Denied | Entire claim rejected | Analyze denial reason, correct and resubmit or appeal |
| Pending | Additional information requested | Provide requested documentation promptly |
Understanding adjudication patterns helps practices anticipate cash flow and identify systematic issues requiring policy-level interventions.
Stage 5: Payment and Reconciliation
Approved claims generate remittance advice documents detailing payment amounts, adjustments, and denials. Electronic remittance advice (ERA) streamlines payment posting processes, reducing manual entry errors and accelerating reconciliation. Payment posting updates patient accounts and provides data for financial reporting.
Reconciliation compares expected payments against received amounts, identifying discrepancies that require investigation. Contractual adjustments, underpayments, and bundling issues surface during this analysis. Regular reconciliation prevents revenue leakage and ensures contractual compliance.
Common Challenges in Claim Processing Systems
Despite technological advances, the claim processing system in healthcare continues to present significant challenges that impact practice profitability and operational efficiency. Recognizing these obstacles enables proactive mitigation strategies.
Denial Management Complexity
Claim denials represent one of the most costly challenges in healthcare revenue cycles. Denial rates averaging 5-10% may seem manageable, but they translate into substantial lost revenue when left unaddressed. Denial management in medical billing requires dedicated resources to analyze root causes, correct errors, and submit appeals within tight timeframes.
Common denial categories include:
- Registration and eligibility errors stemming from incorrect patient information
- Authorization failures when required pre-approvals are not obtained
- Coding inaccuracies involving incorrect or unsupported procedure codes
- Timely filing violations when claims are submitted after payer deadlines
- Medical necessity denials when documentation fails to justify services
Each category demands different resolution approaches. Front-end prevention proves more cost-effective than back-end correction, making staff training and process improvements essential investments.
Payer-Specific Requirements
Different insurance companies maintain unique billing requirements, creating complexity for practices serving diverse patient populations. What one payer accepts, another may reject. Fee schedules, coverage policies, and documentation standards vary significantly across commercial, Medicare, and Medicaid payers.
Maintaining current knowledge of these requirements strains administrative resources, particularly for smaller practices. Centralized reference materials, regular training updates, and experienced billing staff help navigate this variability. Professional revenue cycle management services bring expertise across multiple payer types, reducing the learning curve for individual practices.

Technology's Role in Modern Claim Processing
Technology has fundamentally transformed the claim processing system in healthcare, introducing automation, artificial intelligence, and advanced analytics that enhance accuracy and efficiency. These innovations address traditional pain points while creating new opportunities for optimization.
Automation and Artificial Intelligence
Automated systems now handle routine tasks that previously required extensive manual effort. Claim scrubbing software identifies errors before submission, reducing rejection rates. Robotic process automation manages repetitive data entry tasks, freeing staff for higher-value activities. According to recent analyses of claims processing automation, advanced optical character recognition and AI-driven validation can significantly improve accuracy rates.
Artificial intelligence applications extend beyond basic automation. Machine learning algorithms analyze historical claim data to predict denial likelihood, enabling preemptive corrections. Natural language processing extracts relevant information from unstructured clinical notes, supporting more accurate code assignment. These technologies continue evolving, offering increasingly sophisticated support for revenue cycle operations.
Integration and Interoperability
Modern practice management systems integrate claim processing functions with electronic health records, scheduling platforms, and patient accounting systems. This integration eliminates duplicate data entry, ensures consistency across platforms, and provides comprehensive visibility into the revenue cycle.
Interoperability standards like HL7 and FHIR facilitate data exchange between disparate systems, enabling seamless information flow. Real-time eligibility verification, electronic prior authorization, and automated claim status inquiries all depend on robust integration capabilities. Practices benefit most when technology vendors prioritize open standards and collaborative ecosystems.
Best Practices for Optimizing Claim Processing
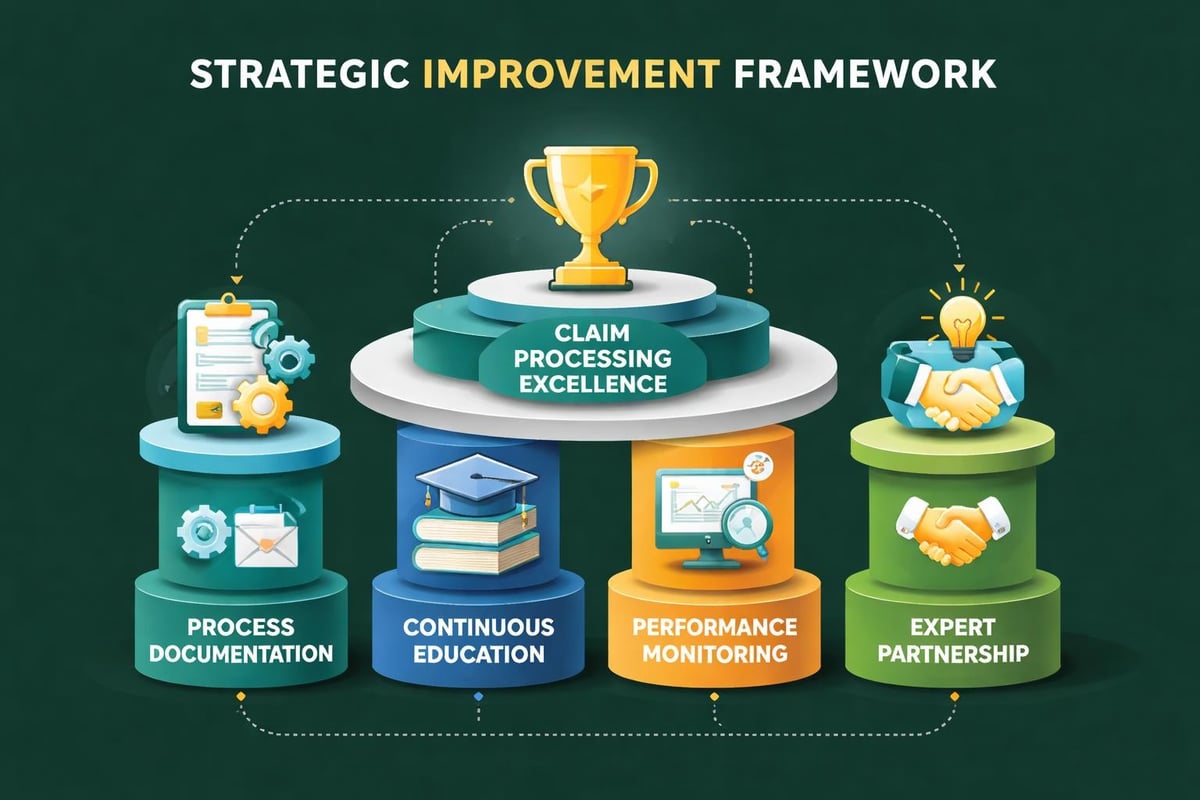
Healthcare providers seeking to enhance their claim processing system in healthcare should implement proven best practices that address both operational efficiency and financial performance. Strategic improvements compound over time, yielding substantial returns.
Establish Clear Process Documentation
Written protocols for each stage of the claims process create consistency and facilitate staff training. Standard operating procedures should address:
- Insurance verification timing and documentation requirements
- Coding quality assurance checkpoints and review criteria
- Claim submission schedules and batch processing protocols
- Payment posting rules and variance investigation triggers
- Denial tracking, analysis, and appeal procedures
Documentation enables quality monitoring and continuous improvement. When processes exist only as tribal knowledge, staff turnover disrupts operations and introduces errors.
Invest in Continuous Education
The regulatory environment, coding guidelines, and payer policies change frequently. Staff education programs keep billing teams current with evolving requirements. Professional certifications demonstrate competency and commitment to best practices.
Training should extend beyond billing specialists to include clinical staff whose documentation drives accurate coding. Physicians and advanced practice providers benefit from understanding how their charting directly impacts reimbursement. Collaborative education sessions build mutual appreciation for each role's contribution to revenue cycle success.
Monitor Key Performance Indicators
Data-driven management requires tracking metrics that reveal system performance and highlight improvement opportunities. Essential key performance indicators include:
| Metric | Target Range | Significance |
|---|---|---|
| First-pass acceptance rate | >95% | Measures clean claim submission quality |
| Days in accounts receivable | <40 days | Indicates collection efficiency |
| Denial rate | <5% | Reflects prevention effectiveness |
| Appeal success rate | >50% | Shows denial management competency |
| Net collection rate | >95% | Demonstrates overall revenue capture |
Regular reporting and trend analysis enable proactive intervention before minor issues become major problems. Benchmarking against industry standards provides context for performance evaluation.
Leverage Professional Expertise
Many healthcare practices find that partnering with specialized revenue cycle management services provides advantages over maintaining entirely in-house operations. Professional billing companies bring economies of scale, specialized expertise, and technology investments that individual practices struggle to replicate.
These partnerships work particularly well when service providers adapt to existing practice management systems rather than requiring wholesale platform changes. The flexibility to integrate with best medical billing software for small business environments ensures practices retain familiar workflows while gaining expert support.
Regulatory Compliance in Claim Processing
The claim processing system in healthcare operates within a complex regulatory framework that governs privacy, fraud prevention, and billing practices. Compliance failures carry significant financial and legal consequences, making regulatory adherence non-negotiable.
HIPAA Requirements
The Health Insurance Portability and Accountability Act establishes standards for protecting patient health information during transmission, storage, and processing. Claim processing involves sharing protected health information with payers and clearinghouses, requiring appropriate safeguards.
Business associate agreements formalize relationships with third-party vendors who access patient data. Encryption protocols protect electronic transmissions. Access controls limit information exposure to authorized personnel. Regular security risk assessments identify vulnerabilities requiring remediation.
Anti-Fraud Provisions
Federal and state regulations prohibit fraudulent billing practices, including upcoding, unbundling, and billing for services not rendered. The False Claims Act imposes substantial penalties for knowing submission of fraudulent claims. Compliance programs establish internal controls that prevent violations and detect problems early.
Documentation requirements serve anti-fraud objectives by ensuring that billed services are medically necessary and appropriately supported. Regular audits of coding accuracy and billing patterns identify potential compliance risks. Education programs ensure staff understand prohibited practices and reporting obligations.
Timely Filing and Coordination of Benefits
Payer contracts specify timeframes for claim submission, typically ranging from 90 to 365 days from the date of service. Missing these deadlines results in automatic denials with limited appeal rights. Tracking submission dates and understanding different types of medical coding deadlines prevents costly timing errors.
When patients have multiple insurance policies, coordination of benefits rules determine primary and secondary payer responsibilities. Proper sequencing ensures maximum reimbursement while avoiding duplicate payments. Claims submitted to the wrong payer first may face rejection and timing complications.
Financial Impact of Effective Claim Processing
The efficiency and accuracy of a claim processing system in healthcare directly correlates with practice financial health. Improvements in this area generate measurable returns through multiple mechanisms.
Revenue Acceleration
Faster claim submission and resolution compress the cash conversion cycle, accelerating revenue recognition. Practices that submit clean claims promptly receive payment weeks earlier than those with error-prone processes. This timing difference impacts working capital availability and reduces financing needs.
Electronic submission, automated eligibility verification, and real-time claim status monitoring all contribute to acceleration. Eliminating paper-based workflows and manual interventions removes delays inherent in traditional approaches.
Cost Reduction
Claim processing errors consume staff time through rework, phone calls to payers, and manual corrections. Each claim that requires resubmission carries hidden costs in labor and opportunity expense. Prevention through front-end accuracy costs less than back-end correction.
Automation reduces the staffing hours required per claim processed. While technology investments require upfront capital, the ongoing operational savings typically justify these expenditures. Scalability improves as practices grow without proportional increases in administrative headcount.
Revenue Preservation
Denial prevention and effective appeal management preserve revenue that would otherwise be lost. Given that some denied claims are never successfully recovered, improving first-pass acceptance rates directly protects earnings. Even when appeals succeed, the delay and effort represent inefficiency.
Understanding how denial management in medical billing improves cash flow demonstrates the substantial financial impact of systematic denial prevention and resolution strategies. Practices that excel in these areas consistently outperform peers in overall revenue cycle metrics.
Selecting the Right Support for Your Practice
Healthcare providers evaluating their claim processing system in healthcare often face decisions about resource allocation, technology investment, and whether to outsource certain functions. These choices depend on practice size, specialty, growth trajectory, and internal capabilities.
In-House vs. Outsourced Operations
Building internal billing expertise provides direct control and deep practice-specific knowledge. Staff familiarity with providers, typical procedures, and patient populations can enhance accuracy. However, recruiting, training, and retaining qualified billing professionals challenges many practices, particularly in competitive labor markets.
Outsourcing to professional revenue cycle management companies offers access to specialized expertise, proven processes, and advanced technology without capital investment. The Centers for Medicare & Medicaid Services processing architecture illustrates the complexity involved, which specialized service providers navigate daily across hundreds of clients.
The optimal approach often combines internal oversight with external execution, maintaining strategic control while leveraging specialized operational support.
Technology Platform Considerations
Whether managing claims internally or through partners, the underlying technology platform significantly impacts performance. Essential capabilities include:
- Real-time eligibility verification to prevent coverage issues
- Integrated coding reference tools supporting accurate charge capture
- Automated claim scrubbing identifying errors before submission
- Comprehensive reporting for performance monitoring and trend analysis
- Seamless electronic remittance advice posting reducing manual effort
Practices should evaluate platforms based on specialty-specific features, user experience, vendor support quality, and integration capabilities with existing systems. Resources like healthcare claims management software comparisons provide valuable perspectives on available solutions.
Service Provider Evaluation Criteria
When considering outsourced support, practices should assess potential partners across multiple dimensions:
- Experience in your specialty and understanding of specific billing requirements
- Technology platform flexibility and ability to adapt to your existing systems
- Transparency in reporting and communication practices
- Compliance credentials including HIPAA certification and audit results
- Performance guarantees and accountability for results
The most successful partnerships feature collaborative relationships where providers and revenue cycle management teams function as integrated extensions of the practice. Service models that emphasize education and process improvement deliver greater long-term value than transactional arrangements focused solely on claim volume.
Emerging Trends Shaping Future Claim Processing
The claim processing system in healthcare continues evolving in response to technological innovation, regulatory changes, and market pressures. Forward-thinking practices monitor these trends to position themselves advantageously.
Predictive Analytics and Machine Learning
Advanced analytics applications increasingly leverage historical claim data to predict outcomes and optimize strategies. Machine learning models identify patterns associated with denials, enabling proactive intervention. Predictive algorithms forecast cash flow based on claim submission patterns and historical collection rates.
These capabilities move revenue cycle management from reactive to proactive, shifting effort from problem correction to problem prevention. Research on AI in healthcare claims processing highlights the expanding role of artificial intelligence across the revenue cycle.
Value-Based Care and Alternative Payment Models
As healthcare shifts from fee-for-service toward value-based reimbursement, claim processing systems must adapt. Bundled payments, shared savings arrangements, and quality incentives require different workflows than traditional claim submission. Tracking quality metrics, coordinating across care episodes, and managing complex contract terms demands enhanced capabilities.
Practices participating in alternative payment models need technology and expertise supporting these non-traditional reimbursement mechanisms. Revenue cycle management becomes more complex but also more strategic in optimizing outcomes under these arrangements.
Increased Transparency and Patient Responsibility
Rising patient cost-sharing through high-deductible health plans shifts collection responsibility from insurers to patients. This trend requires enhanced point-of-service collection capabilities, patient-friendly billing statements, and flexible payment options. The claim processing system must accommodate split payment scenarios where insurers and patients each bear portions of total charges.
Transparency initiatives, including advance cost estimates and benefit explanations, demand real-time access to payer contracts and coverage details. Meeting these expectations requires sophisticated technology integration and staff training on patient communication.
Optimizing your claim processing system in healthcare requires strategic focus, specialized expertise, and ongoing commitment to excellence. The financial and operational benefits of improvement span accelerated revenue, reduced costs, and enhanced compliance. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed to maximize reimbursement while minimizing administrative burden for healthcare providers. Our experienced team works seamlessly with your existing systems, providing the expertise and support needed to transform your claims processing performance and strengthen your practice's financial foundation.