Health insurance claim rejections represent one of the most significant financial challenges facing healthcare providers today. When insurance companies refuse to process claims, the revenue cycle grinds to a halt, creating cash flow disruptions that can threaten practice stability. Understanding the root causes of rejected claims health insurance scenarios and implementing preventative measures has become essential for maintaining financial health in medical practices. Unlike denials, which occur after adjudication, rejections happen at the front end when claims fail to meet basic submission requirements, making them both frustrating and entirely preventable with proper procedures.
Understanding Rejected Claims Health Insurance Fundamentals
The distinction between rejections and denials often confuses healthcare providers, yet this difference determines how claims are addressed. Rejections occur when a claim contains errors that prevent it from entering the payer's adjudication system. These claims never receive formal review because they fail fundamental data validation checks.
Common rejection triggers include incorrect patient demographic information, invalid insurance identification numbers, missing or mismatched procedure codes, and formatting errors. The claim essentially bounces back to the provider, requiring correction and resubmission. Time sensitivity becomes critical because the original service date remains unchanged, and providers must work within filing deadline constraints.
Denials, conversely, indicate that a payer reviewed the claim and determined it does not meet coverage criteria or medical necessity requirements. The internal appeals process becomes necessary for overturning denials, while rejections simply need correction and resubmission.
Financial Impact of Rejected Claims
Revenue disruption from rejected claims health insurance situations extends beyond delayed payments. Each rejection triggers additional administrative costs as staff members investigate errors, correct information, and resubmit claims. The cumulative effect drains resources and diverts attention from patient care.
| Impact Category | Financial Consequence | Operational Effect |
|---|---|---|
| Delayed Revenue | 30-60 day payment delays | Cash flow disruption |
| Administrative Costs | $25-50 per rework claim | Increased overhead |
| Lost Claims | 3-5% never resubmitted | Permanent revenue loss |
| Staff Time | 15-30 minutes per correction | Reduced productivity |
Research indicates that practices lose significant revenue simply because rejected claims never get corrected and resubmitted. Staff overwhelm, poor tracking systems, and approaching filing deadlines contribute to this permanent revenue leakage.
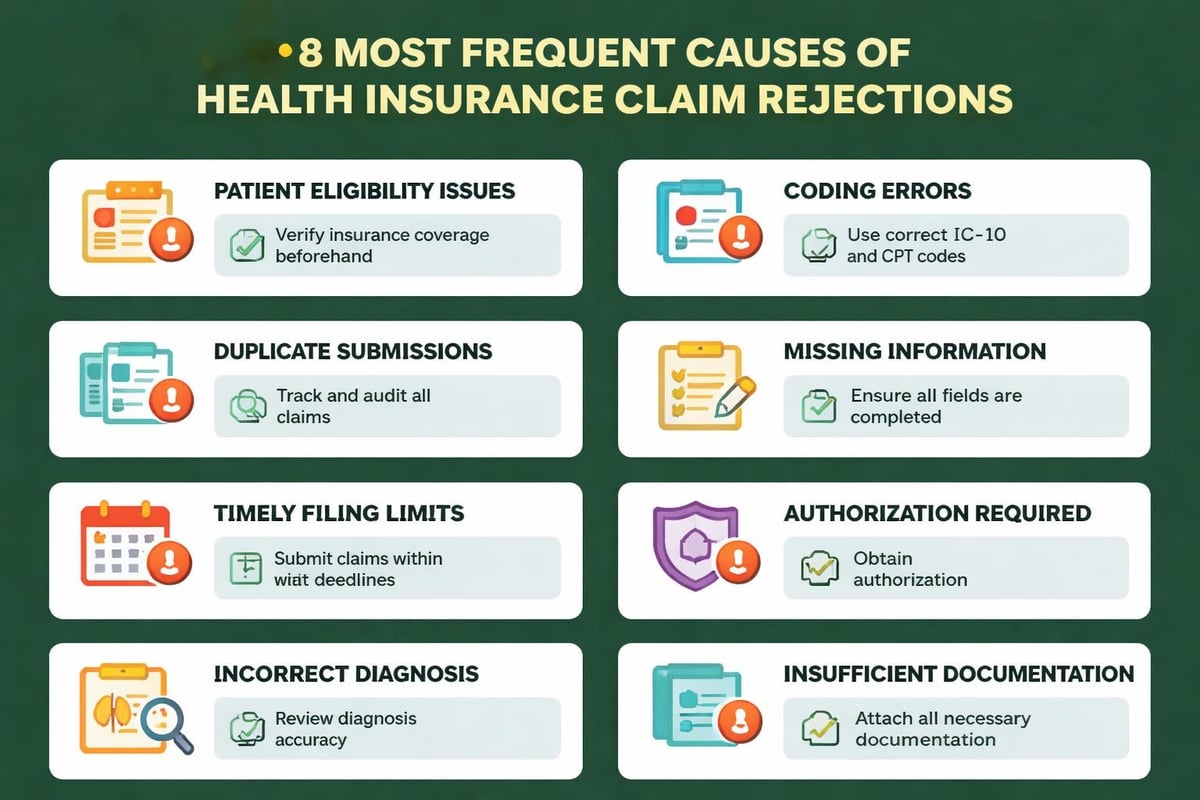
Primary Causes Behind Rejected Claims Health Insurance
Identifying why claims get rejected provides the foundation for prevention strategies. Healthcare providers face recurring patterns of rejection that, once recognized, become manageable through systematic process improvements.
Patient Eligibility and Registration Errors
Inaccurate patient information stands as the leading cause of claim rejections. Even minor discrepancies between the information submitted and what appears in the payer's database trigger automatic rejections. Common problems include:
- Misspelled patient names or transposed letters
- Incorrect date of birth entries
- Outdated insurance policy numbers
- Wrong subscriber information for dependent coverage
- Expired insurance coverage submitted as active
Front desk registration procedures directly determine whether these errors occur. When staff members fail to verify insurance cards, update demographic information, or confirm coverage status, rejected claims health insurance problems multiply exponentially. Implementing robust eligibility verification services eliminates most of these preventable errors before claims submission.
Coding Inaccuracies and Mismatches
Medical coding errors create substantial rejection volumes across all specialties. Incorrect CPT codes, outdated ICD-10 codes, and mismatched diagnosis-to-procedure relationships all trigger immediate rejections. Code specificity requirements have increased dramatically, making general or non-specific codes unacceptable for many payers.
Modifier misuse represents another frequent coding issue. When providers fail to append necessary modifiers or use incorrect ones, claims get rejected for lacking proper documentation of circumstances. Understanding types of modifiers in medical billing helps prevent these technical rejections.
Duplicate Claims Submission
Submitting the same claim multiple times creates automatic rejections marked as duplicates. This often happens when practices lack proper tracking systems or when anxious staff members resubmit claims without verifying whether the original submission is still in process. Payer systems flag duplicate submissions immediately, rejecting all subsequent versions.
Prevention Strategies for Rejected Claims Health Insurance
Building a proactive approach to claim submission requires systematic changes across multiple operational areas. Healthcare providers who implement comprehensive prevention measures see rejection rates drop from industry averages of 15-20% to below 5%.
Step 1: Implement Front-End Verification Protocols
Establish verification procedures that confirm patient eligibility before services are rendered. Staff should:
- Scan and verify insurance cards at every visit
- Confirm active coverage status through real-time eligibility checks
- Document any coverage changes or updates immediately
- Verify patient demographic information matches insurance records
- Identify and communicate patient financial responsibility upfront
Real-time verification technology has transformed this process, allowing front desk personnel to confirm coverage instantly rather than discovering issues after claim submission. When practices prioritize verification, rejected claims health insurance incidents decrease substantially.
Step 2: Strengthen Coding Accuracy
Invest in ongoing coder education and implement quality assurance checks before claim submission. Code validation software can catch errors automatically, flagging issues like:
- Invalid code combinations
- Missing diagnosis codes
- Incorrect code sequencing
- Outdated or deleted codes
- Insufficient code specificity
Regular coding audits identify patterns in errors, allowing targeted training to address specific weaknesses. Partnering with experienced medical coding services provides additional quality oversight and ensures compliance with evolving coding requirements.
Step 3: Establish Claim Scrubbing Procedures
Deploy claim scrubbing technology that reviews every claim against payer-specific requirements before submission. These systems check hundreds of data points, identifying potential rejection triggers that human reviewers might miss. Automated scrubbing catches:
- Missing required fields
- Invalid provider or facility identifiers
- Incorrect claim form types
- Authorization number discrepancies
- Billing limit violations
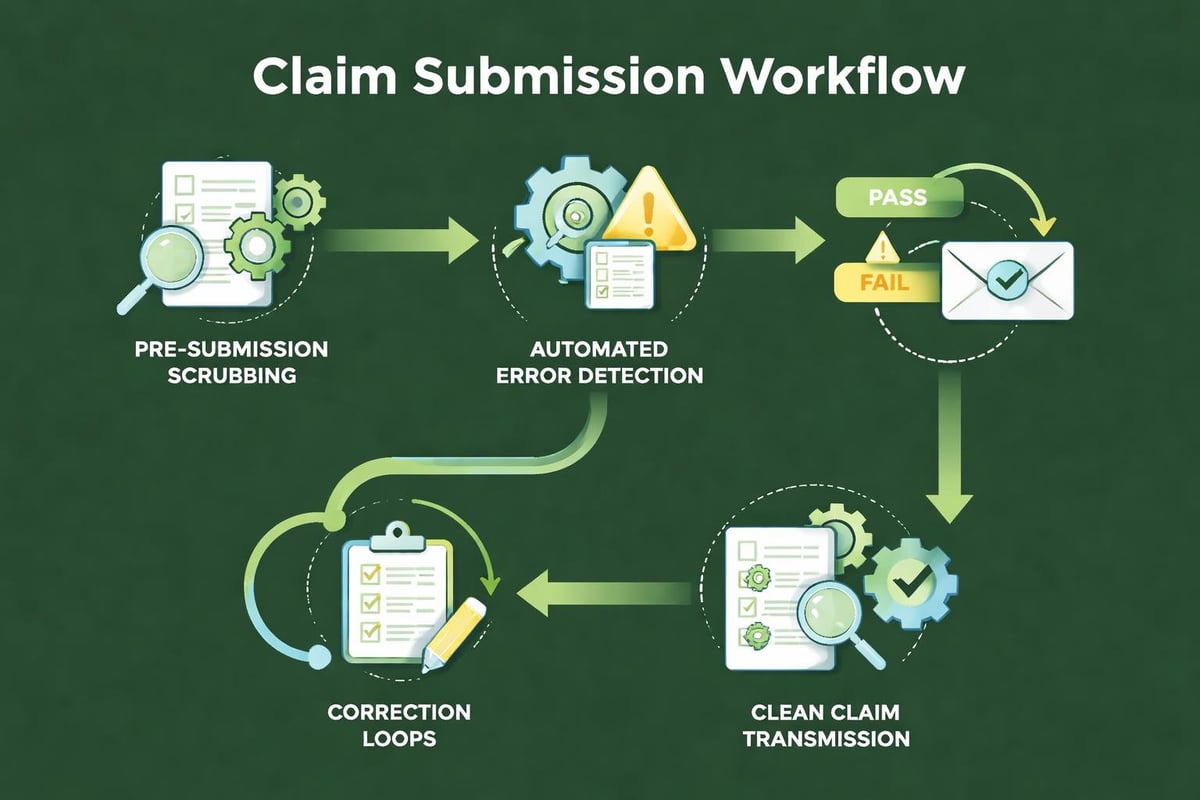
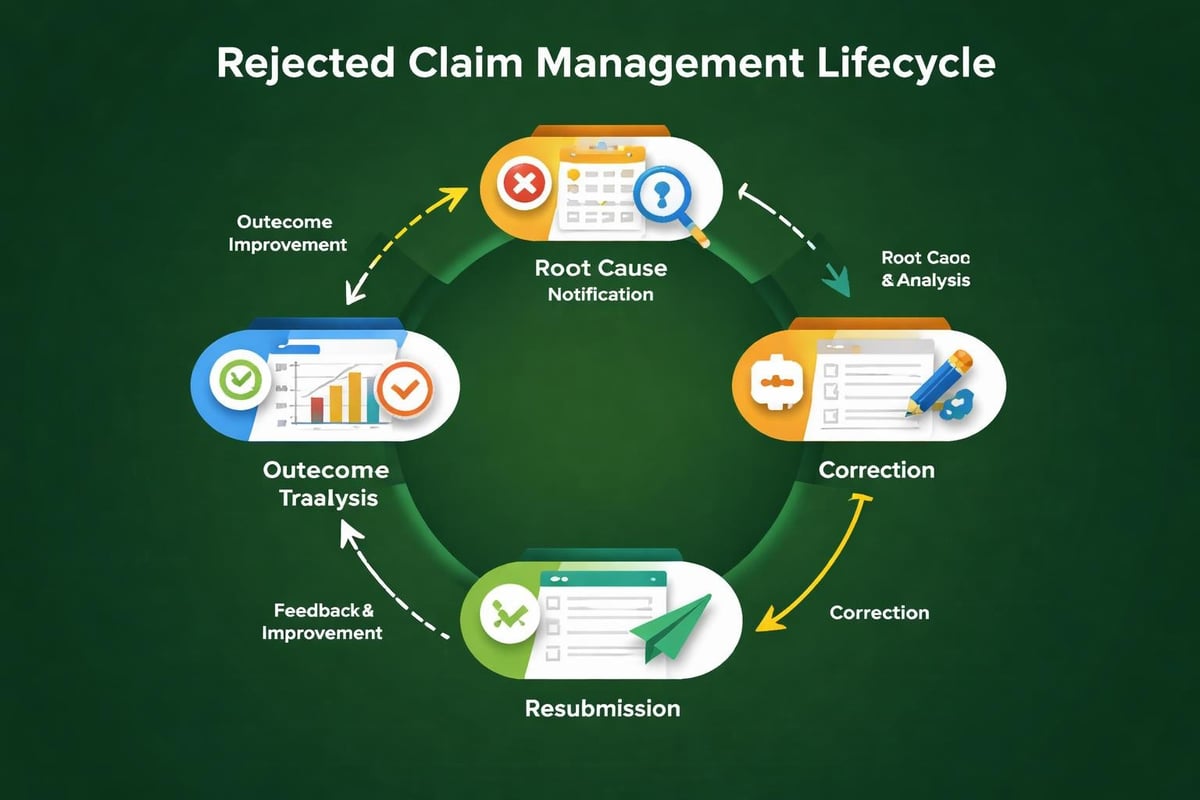
Managing Rejected Claims Health Insurance Efficiently
Even with strong prevention measures, some rejections will occur. How practices respond determines whether these rejections cause minimal disruption or significant revenue delays.
Building an Effective Tracking System
Comprehensive tracking ensures no rejected claim falls through organizational cracks. Modern practice management systems should flag rejections immediately upon receipt, routing them to appropriate staff for resolution. Key tracking elements include:
| Tracking Component | Purpose | Critical Data |
|---|---|---|
| Rejection Date | Timeline monitoring | Date rejection received |
| Rejection Reason | Error identification | Specific payer code/message |
| Assigned Staff | Accountability | Who is correcting |
| Correction Status | Progress monitoring | Current resolution stage |
| Resubmission Date | Deadline tracking | When corrected claim sent |
Establishing clear ownership for rejected claim resolution prevents the common scenario where multiple staff members assume someone else is handling the problem. Designating specific team members for rejection management improves response times and resolution rates.
Analyzing Rejection Patterns
Monthly rejection analysis reveals systemic problems requiring process changes rather than individual claim corrections. Track rejections by:
- Rejection reason codes
- Specific payers
- Individual providers
- Service types
- Front desk personnel
When particular payers consistently reject claims for specific reasons, investigate their unique requirements. Payer-specific training and customized claim templates reduce these predictable rejections. Resources like Consumer Reports’ appeal guidance provide insights into payer behavior patterns.
Technology Solutions for Reducing Rejections
Healthcare technology has evolved to address rejected claims health insurance challenges through automation and real-time validation. Practices that leverage these tools report dramatic improvements in clean claim rates.
Integrated Practice Management Systems
Modern practice management platforms connect registration, scheduling, coding, and billing functions, ensuring data consistency across all claim elements. When demographic information changes in one area, the system updates all connected modules automatically, preventing the common problem of outdated information in billing records.
Integration with payer systems allows real-time eligibility verification and benefit checks, eliminating assumptions about coverage. These systems also maintain current fee schedules and coding updates, reducing rejections from outdated information.
Clearinghouse Services and Pre-Claim Validation
Clearinghouses serve as intermediaries between providers and payers, offering value-added services beyond simple claim transmission. Advanced clearinghouses provide:
- Pre-submission validation against payer-specific rules
- Error correction recommendations with specific guidance
- Rejection resolution support from experienced staff
- Detailed reporting on submission success rates
- Electronic remittance advice integration for payment posting
Quality clearinghouses reduce rejected claims health insurance scenarios by catching errors before claims reach payers, allowing corrections without triggering formal rejections. The feedback loop helps practices identify and resolve recurring problems systematically.
Artificial Intelligence and Machine Learning Applications
Emerging AI solutions analyze historical claim data to predict rejection probability before submission. These systems learn from past rejections, identifying subtle patterns that indicate likely problems. Predictive analytics flag high-risk claims for manual review, concentrating quality assurance efforts where they provide maximum value.
Machine learning algorithms also optimize coding selection based on documentation, suggesting the most appropriate and specific codes while flagging potential mismatches between diagnoses and procedures.
Staff Training and Competency Development
Technology alone cannot solve rejected claims health insurance problems without skilled staff who understand proper procedures and payer requirements. Investing in team development produces measurable returns through improved claim quality.
Cross-Functional Training Programs
Breaking down operational silos helps staff understand how their work affects downstream processes. Front desk personnel who understand coding and billing requirements collect better information during registration. Coders who appreciate payer adjudication nuances make better code selections. Billers who know clinical workflows communicate more effectively with providers about documentation needs.
Regular training sessions should cover:
- Current coding updates and guidelines
- Payer-specific submission requirements
- Common rejection scenarios and solutions
- Documentation improvement strategies
- Technology system updates and features
Bringing team members together for shared learning builds communication and creates problem-solving partnerships that reduce errors across departmental boundaries.
Certification and Continuing Education
Encouraging professional certification demonstrates commitment to excellence while building staff expertise. Certified coders make fewer errors, understand complex scenarios better, and stay current with evolving requirements through mandatory continuing education.
Supporting staff attendance at professional conferences and workshops provides exposure to industry best practices and emerging trends. The knowledge gained translates directly into improved claim quality and reduced rejection rates.
Payer-Specific Strategies and Requirements
Each insurance payer maintains unique submission requirements, coverage policies, and processing rules. Healthcare providers who tailor their processes to accommodate these variations see significantly lower rejection rates than those using generic approaches.
Building Payer Requirement Documentation
Creating detailed reference guides for major payers helps staff submit clean claims consistently. These guides should document:
- Required authorization procedures
- Covered service limitations
- Specific coding preferences
- Claim form requirements
- Supporting documentation needs
- Timely filing deadlines
Maintaining current payer information requires regular communication with insurance representatives and monitoring payer bulletins announcing policy changes. Many rejections occur when practices continue using outdated procedures after payers implement new requirements.
Medicare and Medicaid Considerations
Government payers maintain particularly strict submission standards with detailed technical requirements. Medicare claims demand precise adherence to National Coverage Determinations and Local Coverage Determinations. Understanding CMS guidance on appeals helps providers navigate both rejections and denials effectively.
Medicaid programs vary significantly by state, with each maintaining distinct requirements for eligibility verification, service authorization, and claim submission. Providers serving Medicaid populations must stay current with state-specific policies to avoid preventable rejected claims health insurance scenarios.
Documentation Excellence and Medical Necessity
Insufficient or unclear documentation underlies many claim problems, even when coding is technically correct. Insurance companies increasingly scrutinize medical necessity, requiring comprehensive documentation to support the services billed.
Linking Documentation to Coding
The connection between provider documentation and assigned codes must be clear and unambiguous. Coders need complete information about:
- Patient presentation and chief complaint
- Examination findings supporting diagnosis
- Treatment provided and medical decision-making
- Follow-up plans and continuing care needs
When documentation lacks specificity, coders cannot assign the detailed codes that payers require, resulting in either rejected claims or downcoded payments. Training providers on documentation standards aligned with coding requirements creates the foundation for clean claims.
Templates and Documentation Aids
Electronic health record templates guide providers toward complete documentation while ensuring all required elements appear in clinical notes. Well-designed templates prompt for information needed to support specific procedures and diagnoses, reducing the common problem of incomplete documentation discovered only after claim submission.
However, templates must allow flexibility for individualized patient care and clinical judgment. Over-reliance on generic templates produces documentation that fails to support medical necessity for complex or unusual cases.
Revenue Cycle Integration and Coordination
Addressing rejected claims health insurance requires viewing revenue cycle operations holistically rather than as isolated functions. When registration, clinical documentation, coding, billing, and collections work as integrated processes, claim quality improves dramatically.
Process Mapping and Gap Analysis
Understanding current workflows reveals bottlenecks, redundancies, and gaps that contribute to claim problems. Comprehensive process mapping should trace each claim from patient scheduling through final payment, identifying every handoff and decision point.
Gap analysis highlights where information gets lost, procedures are inconsistent, or quality checks are lacking. Common gaps include:
- Missing feedback loops where billing doesn't inform registration about recurring errors
- Inconsistent verification procedures across different staff members
- Inadequate quality assurance before claim submission
- Poor communication between clinical and administrative teams
Implementing structured communication protocols and regular cross-functional meetings addresses these gaps, creating smoother workflows with fewer errors. Organizations that invest in comprehensive denial management services often discover broader revenue cycle improvements beyond just managing denials.
Performance Metrics and Accountability
Measuring key performance indicators provides objective data about claim quality and identifies improvement opportunities. Essential metrics include:
| Metric | Target | Improvement Action |
|---|---|---|
| Clean Claim Rate | >95% | Below 95% requires process review |
| Rejection Rate | <5% | Identify top rejection reasons monthly |
| Days in A/R | <30 | Accelerate claim submission and follow-up |
| Resubmission Time | <7 days | Improve rejection workflow efficiency |
| Collection Rate | >95% | Address denials and patient collections |
Regular reporting creates accountability and focuses improvement efforts on areas with greatest impact. When staff understand how their performance affects overall outcomes, engagement with quality improvement initiatives increases substantially.
Outsourcing Considerations for Rejected Claims Health Insurance
Many healthcare providers recognize that managing the complexities of modern revenue cycle operations exceeds their internal capabilities and resources. Partnering with specialized revenue cycle management services provides access to expertise, technology, and dedicated resources that reduce rejected claims health insurance problems while allowing clinical staff to focus on patient care.
Evaluating Revenue Cycle Management Partners
Not all billing services deliver equivalent value. Healthcare providers should evaluate potential partners based on:
- Industry experience with similar practice types and specialties
- Technology capabilities including modern systems and integration options
- Transparency in reporting and communication practices
- Compliance expertise with HIPAA and payer regulations
- Performance guarantees and measurable outcome commitments
Quality revenue cycle management providers function as true partners, offering strategic guidance alongside operational execution. They bring deep payer knowledge, coding expertise, and established workflows that prevent rejections rather than simply correcting them after occurrence.
Services That Address Rejection Prevention
Comprehensive revenue cycle management encompasses multiple services that collectively minimize rejected claims health insurance scenarios. Medical claim submission services ensure every claim meets payer requirements before submission, while ongoing eligibility verification confirms coverage before services are rendered.
Professional billing services maintain current knowledge of payer policy changes, coding updates, and compliance requirements, adapting submission procedures proactively rather than reactively discovering problems through rejections. This forward-looking approach protects revenue and accelerates collections.
Continuous Improvement and Future Preparedness
The healthcare reimbursement landscape continues evolving, with payers implementing increasingly sophisticated claim processing systems and stricter submission requirements. Healthcare providers must embrace continuous improvement cultures that anticipate changes and adapt proactively.
Staying Current with Industry Changes
Regular monitoring of industry publications, payer communications, and regulatory updates helps practices stay ahead of changes affecting claim submission. Resources like WebMD’s appeal guidance and Experian’s prevention strategies provide valuable insights into evolving best practices.
Professional association membership connects providers with peers facing similar challenges, creating opportunities to learn about effective solutions and emerging trends. Sharing knowledge within professional communities accelerates learning and helps practices avoid common pitfalls.
Building Organizational Resilience
Healthcare organizations that view rejected claims health insurance challenges as opportunities for systematic improvement build resilience that extends beyond billing operations. Process discipline, data-driven decision making, and continuous learning create capabilities that benefit all organizational functions.
Investing in staff development, technology infrastructure, and operational excellence positions practices for long-term success regardless of how reimbursement models evolve. The skills and systems that prevent claim rejections also support value-based care initiatives, quality reporting requirements, and patient satisfaction improvements.
Reducing rejected claims health insurance incidents requires systematic approaches that address root causes rather than symptoms, combining strong processes, skilled staff, appropriate technology, and ongoing quality improvement. Healthcare providers who implement comprehensive prevention strategies protect revenue, improve cash flow, and create operational efficiency that supports their primary mission of patient care. Greenhive Billing Solutions specializes in helping healthcare providers eliminate claim rejections through expert revenue cycle management services including eligibility verification, claims processing, coding excellence, and denial management, all delivered with HIPAA compliance and transparent communication that ensures maximum reimbursements and financial stability for practices nationwide.

