Credentialing is the backbone of every provider organization’s risk management, revenue, and compliance strategy. As the healthcare credentialing process becomes more complex and faces growing regulatory scrutiny, even experienced practices can struggle to keep pace. A well-managed healthcare credentialing process not only reduces operational risk but also speeds up reimbursements and safeguards compliance with industry standards. This article serves as your comprehensive roadmap, guiding healthcare professionals through credentialing essentials, a step-by-step process, common obstacles, compliance trends, and proven optimization strategies to strengthen your organization’s foundation.
Understanding Healthcare Credentialing: Foundations and Importance
Healthcare organizations rely on a robust healthcare credentialing process to verify the qualifications, training, and competency of their providers. This foundational step safeguards patient safety, reduces risk, and ensures that only qualified professionals deliver care. At its core, the healthcare credentialing process is designed to confirm that every provider meets the required standards set by regulatory bodies and payers.
Credentialing involves the thorough review and verification of a provider's education, training, licensure, work history, and board certifications. Its main objectives are to protect patients, maintain compliance, and streamline provider onboarding. However, credentialing is often confused with two related concepts:
| Process | Purpose | Frequency |
|---|---|---|
| Credentialing | Initial validation of provider qualifications | At hire/onboarding |
| Privileging | Granting specific clinical privileges | After credentialing |
| Enrollment | Registering with payers for reimbursement | After credentialing |
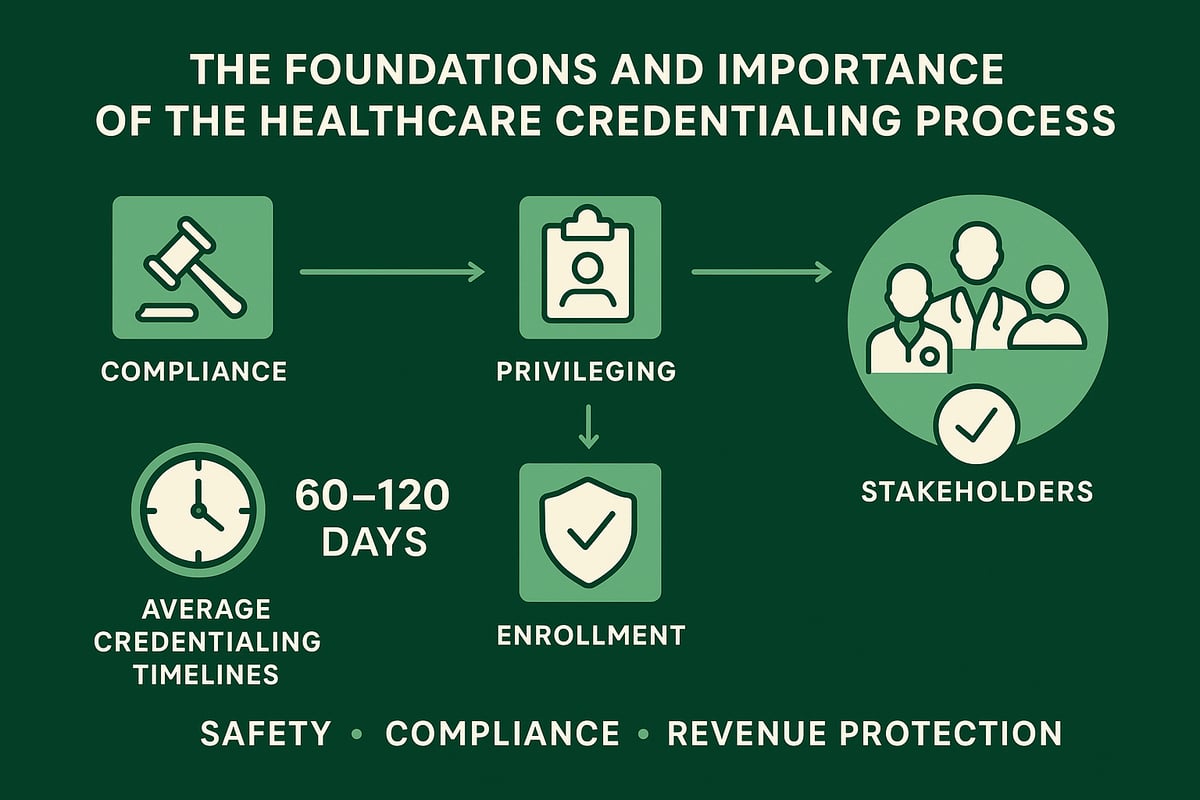
Credentialing is the first step, ensuring the provider is eligible to deliver care. Privileging grants permission to perform specific procedures within a facility. Enrollment allows providers to bill payers and receive reimbursement.
Healthcare organizations must comply with regulations from the Centers for Medicare & Medicaid Services (CMS), the National Committee for Quality Assurance (NCQA), and the Joint Commission. Each entity sets standards for the healthcare credentialing process, including timelines, documentation, and verification methods. Noncompliance can result in fines, payment denials, or even loss of accreditation.
Key stakeholders in the healthcare credentialing process include providers, payers, credentialing committees, and sometimes third-party credentialing services. Each plays a critical role in ensuring that the process is accurate and efficient.
On average, credentialing takes 60 to 120 days, but delays are common. According to industry data, up to 15 percent of applications face denials or extended processing due to missing or inaccurate information. For example, if a physician starts work before credentialing is complete and their application is denied, the clinic may lose months of revenue for services already provided.
For a deeper look at what a best-practice credentialing workflow includes, see this Medical Credentialing Services Overview.
The healthcare credentialing process not only protects patients but also keeps revenue flowing and organizations compliant. Understanding its foundations helps practices avoid costly setbacks and build a reliable provider network.
Step-by-Step Healthcare Credentialing Process
A successful healthcare credentialing process requires a clear, stepwise approach. Each stage builds on the last, ensuring accurate provider verification, regulatory compliance, and faster payer approvals. By following a structured healthcare credentialing process, organizations minimize costly errors and avoid delays that can disrupt revenue flow.

Step 1: Pre-Application Preparation
The healthcare credentialing process begins with thorough pre-application preparation. Gather all required provider documents, such as state licenses, board certifications, malpractice insurance, DEA registration, and a current CV. Double-check that every document is up to date and accurate.
Utilize a comprehensive checklist to avoid missing details. Incomplete or outdated records are a leading cause of credentialing delays. Assign a team member to verify each item for accuracy and completeness before proceeding. This proactive approach sets a strong foundation for the rest of the healthcare credentialing process.
Step 2: Application Submission
Next, select the appropriate payers and networks for your providers. Obtain the latest application forms, either directly from payer portals or via the CAQH platform. Take time to complete each form precisely, as errors can stall the healthcare credentialing process.
Common mistakes include inconsistent information, missing signatures, or outdated contact details. Use a double-review system to ensure accuracy before submission. Timely and error-free applications help maintain momentum throughout the healthcare credentialing process.
Step 3: Primary Source Verification (PSV)
Primary Source Verification, or PSV, is a regulatory cornerstone of the healthcare credentialing process. This step requires direct confirmation of a provider’s credentials from original sources. Typical verifications include medical school transcripts, state licensing boards, and the National Practitioner Data Bank.
Most payers follow strict guidelines, and incomplete PSV can halt the process. On average, PSV can take two to four weeks, depending on response times. Tracking each verification ensures nothing is missed during the healthcare credentialing process.
Step 4: Credentialing Committee Review
Once documentation and PSV are complete, the file advances to the credentialing committee review. This committee evaluates the provider’s qualifications, background, and any potential red flags. The review is a critical checkpoint in the healthcare credentialing process.
Possible outcomes include full approval, denial, or a request for additional information. Factors such as gaps in work history or malpractice claims can trigger closer scrutiny. Preparing supporting documentation in advance helps address committee concerns efficiently and keeps the healthcare credentialing process moving.
Step 5: Payer Enrollment & Contracting
After committee approval, payer enrollment and contracting become the focus. Providers must be enrolled with payers to bill and receive reimbursements. This stage involves negotiating participation agreements and understanding fee schedules.
Delays in this step can significantly impact your revenue cycle. According to Credentialing Delays Financial Impact, lengthy credentialing processes can result in substantial financial losses for practices. Streamlining payer enrollment is essential for an efficient healthcare credentialing process and optimal cash flow.
Step 6: Ongoing Monitoring & Recredentialing
The healthcare credentialing process does not end with initial approval. Ongoing monitoring is vital to ensure continued compliance. Track license expirations, monitor for sanctions, and schedule timely recredentialing cycles.
Timely updates to provider files prevent interruptions in payment or network participation. Set up alerts and periodic audits to maintain credentialing accuracy. An organized ongoing process safeguards your organization’s reputation and revenue, completing the healthcare credentialing process lifecycle.
Common Challenges in Credentialing and How to Overcome Them
The healthcare credentialing process is a vital component of provider operations, but it is often fraught with obstacles that can disrupt workflows and impact revenue. Understanding the most common challenges helps organizations proactively address issues before they escalate.

Key Challenges in the Healthcare Credentialing Process
Healthcare organizations frequently encounter several hurdles during the healthcare credentialing process:
- Incomplete or Inaccurate Documentation: Missing or incorrect provider data is a leading cause of delays.
- Communication Gaps: Providers and credentialing teams may experience miscommunication, resulting in errors or stalled applications.
- Payer Variability: Each payer has unique requirements, forms, and timelines, creating complexity and confusion.
- Regulatory Scrutiny: Increased oversight from agencies means more thorough audits and higher compliance expectations.
- Time-Sensitive Renewals: Missing license or certification renewal dates can halt reimbursements and disrupt patient care.
Real-World Impact Example:
A multi-specialty group lost three months of revenue after a provider’s state license lapsed unnoticed. Claims were denied, and re-enrollment became a lengthy process. This scenario highlights how a small oversight in the healthcare credentialing process can cause significant financial setbacks.
Credentialing Data and Denials
On average, initial credentialing can take 90 to 120 days, but delays are common. Industry data shows that nearly 15% of applications face denials or require resubmission due to incomplete information or errors. These issues directly affect the healthcare credentialing process, leading to delayed onboarding and missed revenue opportunities.
According to Denial Management in Medical Billing, credentialing errors are a major contributor to claim denials, further underscoring the importance of robust processes and oversight.
Proven Solutions to Overcome Challenges
Healthcare organizations can minimize risk and streamline the healthcare credentialing process by adopting these best practices:
- Implement Detailed Checklists: Use structured checklists for every credentialing stage to ensure all documentation is accurate and complete.
- Leverage Digital Tracking Systems: Adopt digital tools to monitor application status, renewal deadlines, and compliance alerts.
- Enhance Communication: Establish regular check-ins between providers, credentialing staff, and payers to resolve issues quickly.
- Conduct Regular Audits: Schedule internal audits to catch errors early and verify that all provider records are current.
- Standardize Processes: Create standardized workflows to handle the variability in payer requirements and keep the process consistent.
By addressing these challenges proactively, organizations can reduce delays, lower denial rates, and protect revenue streams. A streamlined healthcare credentialing process is essential for maintaining compliance, accelerating onboarding, and achieving operational efficiency.
Compliance, Regulatory Trends, and Best Practices
The healthcare credentialing process is governed by a dynamic regulatory landscape that demands vigilance and adaptability from provider organizations. Staying compliant means keeping pace with federal standards, state-specific laws, and evolving accreditation requirements. For example, HIPAA mandates secure handling of provider data, while CMS and state health agencies frequently update credentialing criteria. Notably, the NCQA Credentialing Standards Update highlights the shift toward continuous monitoring and more rigorous verification, making it critical for organizations to review their healthcare credentialing process policies regularly.
Telemedicine’s rapid growth has added complexity to the healthcare credentialing process, especially as providers seek multi-state licensure. Each state introduces unique requirements, and cross-state practice increases the need for robust verification methods. Organizations must ensure that their credentialing teams are well-versed in state-specific rules and maintain detailed records to support compliance. Multi-state licensure also intensifies the need for ongoing monitoring, as regulations can change quickly and affect provider eligibility.
Digital transformation is reshaping the healthcare credentialing process through automation, centralized databases, and even blockchain verification. The adoption of digital platforms has led to faster turnaround times and reduced manual errors. According to Credentialing Software Market Growth, the credentialing software market is expanding rapidly as more organizations embrace technology-driven solutions. While service providers can leverage these tools, it is essential to balance automation with human oversight to ensure accuracy and compliance.
Adopting best practices in the healthcare credentialing process is essential for minimizing risk and promoting regulatory readiness. Organizations should conduct regular policy reviews, invest in ongoing staff training, and integrate technology that aligns with their workflow. Checklists, digital tracking systems, and periodic internal audits can help prevent lapses. When possible, aligning credentialing schedules with annual compliance reviews streamlines processes and helps teams stay proactive.
Reviewing industry benchmarks is vital for assessing performance in the healthcare credentialing process. For example, leading organizations achieve credentialing turnaround times of 30 to 45 days, while the industry average may exceed 60 days. Clinics that implemented annual credentialing audits have reported fewer compliance issues and smoother payer interactions. By focusing on continuous improvement, organizations can ensure their credentialing operations remain efficient, secure, and compliant.
Greenhive Billing Solutions: Credentialing Support for Healthcare Providers
Navigating the healthcare credentialing process can be complex, but Greenhive Billing Solutions streamlines every step for providers and practices. Our experienced team manages initial credentialing, recredentialing, and payer enrollment, ensuring compliance and accelerating payer approvals. We work seamlessly with client-owned systems, focusing on data security and integration.
Key features include:
- Comprehensive document preparation and application tracking
- Primary source verification and compliance monitoring
- Transparent communication and real-time status updates
Practices benefit from improved accuracy, reduced administrative burden, and tailored credentialing solutions for solo practitioners, group practices, and specialty clinics. Contact Greenhive for a complimentary assessment and let us optimize your provider onboarding.
As you’ve seen throughout this guide, effective credentialing is essential to protecting your revenue, keeping your practice compliant, and ensuring a smooth onboarding experience for your providers. Navigating each step— from document collection to ongoing monitoring— can feel overwhelming, especially with new regulations and payer requirements on the horizon. That’s where expert support makes all the difference. If you’re ready to identify gaps in your current process or simply want to streamline credentialing for 2026 and beyond, let’s take the next step together. Book Your Free Consultation and see how Greenhive Billing Solutions can help your practice move forward with confidence.