Billing patients accurately and efficiently is one of the most critical aspects of revenue cycle management in modern healthcare. The process extends far beyond simply sending invoices-it encompasses insurance verification, transparent cost communication, regulatory compliance, and patient satisfaction. When healthcare providers implement effective billing strategies, they not only improve cash flow but also build trust with patients and reduce administrative burdens. Understanding the complexities of patient billing helps practices optimize their financial performance while maintaining positive patient relationships and staying compliant with evolving healthcare regulations.
Understanding the Patient Billing Lifecycle
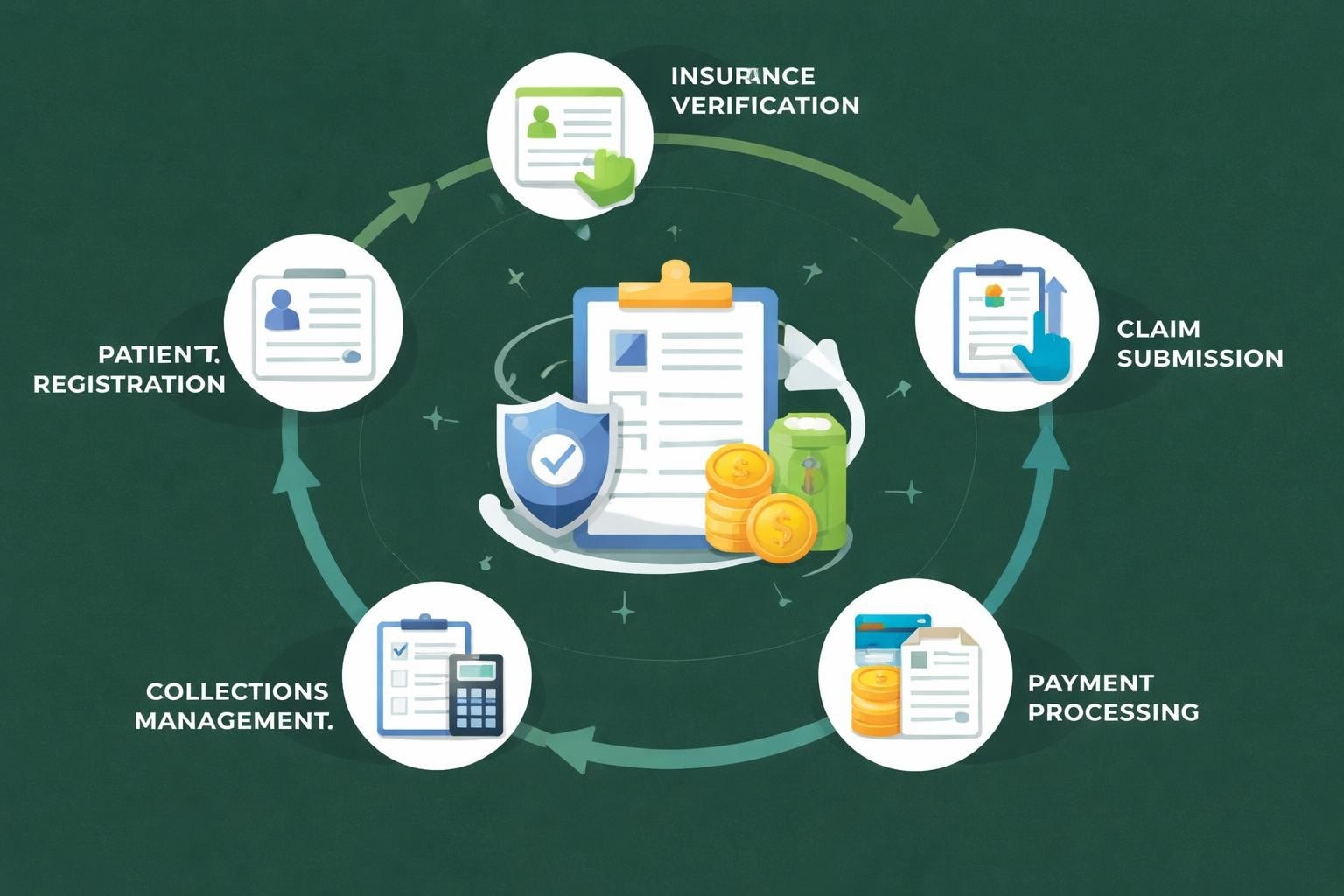
The patient billing process begins long before a patient walks through the door and continues well after treatment concludes. Every touchpoint in this lifecycle presents opportunities for optimization and potential pitfalls that can delay reimbursement.
Pre-Visit Preparation and Verification
Effective billing patients starts with thorough preparation during scheduling and registration. Front-desk staff must collect accurate demographic information, verify insurance coverage, and determine patient financial responsibility. This proactive approach prevents claim denials and surprise bills that damage patient trust.
Key pre-visit tasks include:
- Confirming insurance eligibility and coverage levels
- Verifying referral and authorization requirements
- Collecting copayments and estimated patient portions
- Updating patient contact and insurance information
- Documenting any changes in coverage or employment
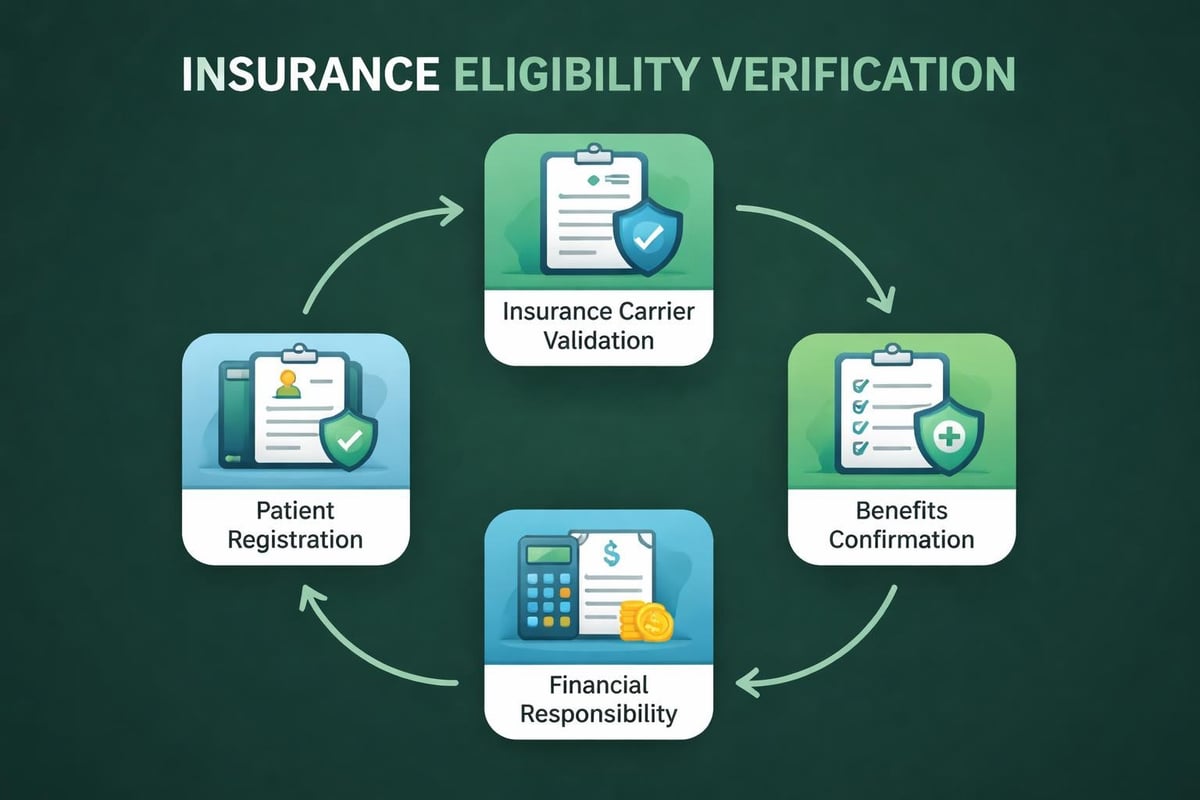
The eligibility verification services provided by specialized RCM partners can streamline this critical first step, ensuring clean claims from the outset.
Point-of-Service Collections and Transparency
Collecting payments at the point of service significantly improves collection rates and reduces accounts receivable days. However, this must be balanced with transparency and patient-friendly communication. The No Surprises Act requirements mandate that providers give patients good faith estimates for scheduled services, fundamentally changing how billing patients works in many scenarios.
| Collection Strategy | Average Success Rate | Patient Satisfaction Impact |
|---|---|---|
| Point-of-service collection | 85-95% | High (when communicated clearly) |
| Statement after service | 60-70% | Moderate |
| Collection agency | 20-30% | Low |
Healthcare providers must implement systems that calculate patient responsibility accurately based on insurance benefits, deductibles, and coinsurance. Clear communication about costs before services prevents disputes and improves the patient experience.
Compliance and Regulatory Considerations
Billing patients in healthcare involves navigating a complex web of federal and state regulations. Non-compliance can result in substantial penalties, reputation damage, and legal consequences.
HIPAA Compliance in Billing Communications
Every aspect of patient billing must protect protected health information (PHI). This includes secure transmission of statements, proper handling of payment information, and strict access controls for billing systems. Staff training on HIPAA requirements is essential to prevent breaches.
Outsourced billing partners must demonstrate robust security protocols and HIPAA compliance certifications. When evaluating medical billing services, healthcare providers should verify that vendors maintain business associate agreements and regular security audits.
Balance Billing Restrictions
The No Surprises Act and various state laws restrict balance billing for out-of-network emergency services and certain non-emergency situations. Providers must understand when balance billing is prohibited and implement safeguards to prevent violations. The American Medical Association’s guidance provides crucial information on these requirements.
Prohibited balance billing scenarios:
- Emergency services at out-of-network facilities
- Non-emergency services by out-of-network providers at in-network facilities (without proper consent)
- Post-stabilization services without transfer authorization
- Air ambulance services in most circumstances
Creating Patient-Friendly Billing Statements
Statement design significantly impacts patient understanding and payment behavior. Complex, confusing bills lead to delayed payments and increased administrative costs from patient inquiries.
Essential Statement Elements
A well-designed patient bill should clearly show the service date, provider name, procedure description in plain language, insurance payments, adjustments, and patient responsibility. Avoid medical jargon and billing codes that patients cannot understand without research.
The statement should also include:
- Clear payment due dates with consequences for late payment
- Multiple payment options including online portals, phone payments, and mail
- Contact information for billing questions with specific hours of availability
- Itemized charges that patients can review and verify
Many practices struggle with explaining adjustments on medical bills, which confuse patients who see large amounts "written off" but still owe significant balances.

Digital Billing and Patient Portals
Modern patients expect digital access to their billing information. Patient portals allow 24/7 access to statements, payment history, and the ability to make payments online. This convenience improves satisfaction and accelerates collections.
| Portal Feature | Patient Adoption Rate | Impact on Collections |
|---|---|---|
| Online bill viewing | 65-75% | Moderate |
| Online payment | 55-65% | High |
| Payment plan setup | 40-50% | High |
| Auto-pay enrollment | 25-35% | Very high |
Implementing Effective Payment Plans
Not all patients can pay their entire balance immediately. Payment plans are essential for billing patients while maintaining access to care and steady revenue flow.
Structuring Payment Arrangements
Payment plans should be tailored to patient financial situations while ensuring reasonable collection timelines. Most practices offer interest-free plans for balances paid within six to twelve months. Clear written agreements prevent misunderstandings and provide legal protection if collection becomes necessary.
Step-by-step payment plan implementation:
- Assess patient financial situation through income verification or financial assistance applications
- Calculate reasonable monthly payment based on balance and patient capacity
- Create written agreement specifying amount, frequency, and consequences of non-payment
- Set up automated payments to reduce administrative burden and missed payments
- Monitor compliance and follow up promptly on missed payments
The American Hospital Association’s billing guidelines emphasize the importance of flexible payment options as part of ethical billing practices.
Financial Assistance Programs
Many healthcare organizations maintain financial assistance policies (FAPs) that provide discounts or free care to qualifying patients. These programs fulfill community benefit requirements and prevent bad debt accumulation. Clear communication about available assistance is both ethical and financially prudent.
Claims Processing and Follow-Up
Accurate claim submission is fundamental to billing patients correctly. When insurance claims are denied or underpaid, the patient balance may be incorrect, leading to disputes and delayed payments.
Clean Claim Submission
Clean claims-those without errors or missing information-process quickly and reduce patient confusion. Key elements include accurate patient demographics, correct insurance information, appropriate diagnosis and procedure codes, and proper modifiers. Understanding different types of medical coding helps ensure claims are coded correctly from the start.
Common claim errors that affect patient billing:
- Incorrect insurance identification numbers
- Mismatched patient names or dates of birth
- Missing or invalid authorization numbers
- Incorrect place of service codes
- Bundling or unbundling errors
Specialized medical claim submission services can reduce these errors through experienced staff and advanced claim scrubbing technology.
Denial Management and Appeals
When claims are denied, prompt action protects both revenue and patient relationships. Patients should not be billed for amounts that insurance should cover. Effective denial management in medical billing identifies denial patterns, corrects root causes, and ensures successful appeals.
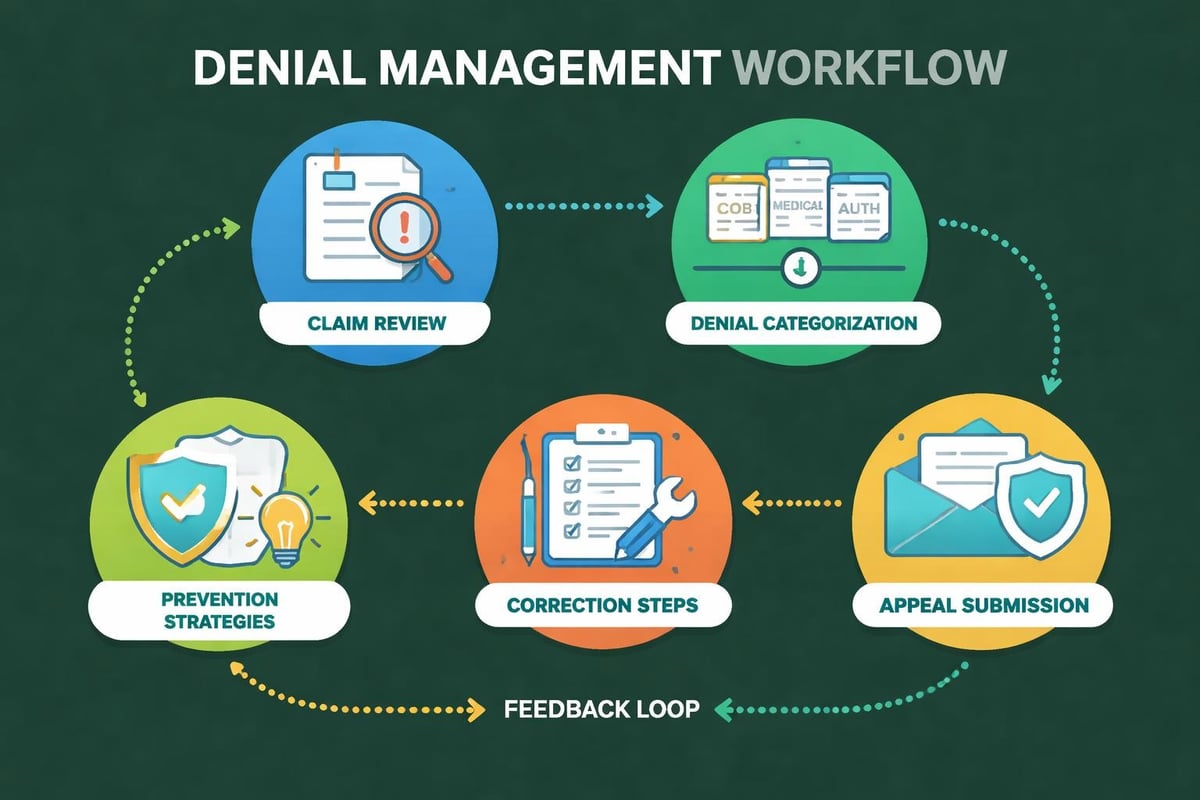
The appeals process requires detailed documentation, timely submission, and thorough knowledge of payer requirements. Many denials result from simple errors that can be corrected and resubmitted quickly, while others require formal appeals with supporting medical records.
Best Practices to Avoid Improper Billing
Improper billing damages patient trust, triggers audits, and may constitute fraud. Healthcare providers must implement safeguards to ensure billing accuracy and compliance.
Documentation and Coding Accuracy
The foundation of proper billing is complete, accurate clinical documentation that supports the codes submitted. Providers should document all services performed, medical necessity for procedures, and relevant patient history. Regular medical coding audits identify documentation gaps and coding errors before they become compliance issues.
Following best practices to avoid improper billing protects practices from penalties and maintains patient trust. This includes regular staff training, clear documentation standards, and robust compliance monitoring.
Staff Training and Education
Billing staff must understand coding guidelines, payer policies, and regulatory requirements. Regular training sessions keep teams current on changes to billing rules, new regulations, and evolving best practices. Cross-training helps ensure continuity when staff members are absent.
Essential training topics for billing teams:
- Annual CPT and ICD code updates
- Payer-specific billing requirements
- Compliance and fraud prevention
- Patient communication and conflict resolution
- Technology system updates and new features
Managing Patient Communications and Disputes
Even with perfect billing processes, questions and disputes arise. How practices handle these interactions significantly impacts patient satisfaction and collection success.
Responding to Patient Inquiries
Billing questions should receive prompt, courteous responses from knowledgeable staff. Many patient concerns stem from confusion about insurance processing, contractual adjustments in medical billing, or complex medical terminology. Staff should be empowered to explain charges clearly and adjust accounts when errors occur.
A dedicated billing phone line with specific hours and trained representatives improves the patient experience. Average hold times should be monitored and minimized, as long waits increase patient frustration.
Handling Disputes and Complaints
When patients dispute charges, practices need clear protocols for investigation and resolution. This includes reviewing the medical record, verifying coding accuracy, checking insurance processing, and comparing charges to established fee schedules. Legitimate errors should be corrected immediately with clear communication to the patient.
| Dispute Type | Resolution Time | Common Outcome |
|---|---|---|
| Duplicate billing | 1-3 days | Charge removal |
| Coding error | 3-7 days | Claim correction |
| Insurance processing error | 7-14 days | Balance adjustment |
| Service not rendered | 1-3 days | Charge removal |
Leveraging Technology for Billing Efficiency
Modern billing technology automates routine tasks, reduces errors, and provides analytics for continuous improvement. While technology doesn't replace skilled professionals, it enhances their efficiency and accuracy.
Revenue Cycle Management Systems
Comprehensive RCM platforms integrate scheduling, registration, charge capture, claims submission, payment posting, and reporting. These systems provide visibility across the entire revenue cycle and identify bottlenecks. Though practices may invest in medical billing software for small businesses or larger enterprise solutions, the key is ensuring proper implementation and staff training.
Analytics and Reporting
Data-driven decision-making improves billing performance. Healthcare revenue cycle analytics reveal trends in denial rates, collection percentages, days in accounts receivable, and patient payment behavior. Regular analysis of these metrics guides process improvements and staff training priorities.
Critical billing metrics to monitor:
- Clean claim rate (target: above 95%)
- First-pass resolution rate (target: above 85%)
- Days in accounts receivable (target: below 40 days)
- Collection rate (target: above 95% of expected reimbursement)
- Patient payment collection rate (target: above 70% within 90 days)
Outsourcing Versus In-House Billing
Healthcare organizations must decide whether to manage billing patients internally or partner with specialized RCM services. Each approach has advantages depending on practice size, specialty, and resources.
Benefits of Specialized RCM Partners
Outsourced billing services provide access to experienced professionals, advanced technology, and specialized expertise without the overhead of maintaining internal staff. For many practices, particularly smaller ones, this model improves efficiency and collections while reducing administrative burden. Medical billing services for small practices often deliver better results than understaffed internal departments.
RCM partners also adapt to changing regulations and payer requirements more quickly than individual practices can. They invest in ongoing training, technology updates, and compliance monitoring as core business functions.
When In-House Billing Makes Sense
Large practices with high volumes and standardized procedures may justify dedicated internal billing departments. These organizations can attract qualified billing professionals, invest in comprehensive technology, and maintain direct control over the billing process. The decision often depends on practice size, financial resources, and management preferences.
Regardless of the chosen model, implementing patient-friendly practices outlined by Experian’s billing recommendations improves collection rates and patient satisfaction across both approaches.
Specialty-Specific Billing Considerations
Different medical specialties face unique billing challenges that affect how they approach billing patients. Understanding these nuances improves accuracy and compliance.
Behavioral Health Billing Challenges
Mental health and substance abuse services involve specific documentation requirements, confidentiality concerns, and authorization processes. Medical billing for behavioral health requires expertise in these specialized areas to ensure proper reimbursement while protecting patient privacy.
Procedural Specialty Billing
Specialties performing procedures and surgeries face complex coding scenarios with multiple CPT codes, modifiers, and bundling rules. Understanding what constitutes a CPT code for insurance purposes and how modifiers in medical billing affect reimbursement is critical for accurate billing.
Patient Financial Responsibility and Legal Considerations
Understanding the legal framework around patient financial obligations helps practices navigate complex situations while protecting their revenue.
Patient Obligations and Rights
Patients generally have legal obligations to pay for services rendered, but numerous factors affect collectability. Patients have rights to accurate billing, clear explanations, and protection from unfair collection practices. Resources explaining whether patients must pay medical bills help both providers and patients understand these obligations.
Collection Agency Partnerships
When internal collection efforts fail, healthcare providers may engage collection agencies. These partnerships require careful vendor selection to ensure compliance with Fair Debt Collection Practices Act (FDCPA) requirements and protection of patient relationships. Clear policies determine when accounts move to collections and what percentage the agency retains.
Billing patients effectively requires balancing regulatory compliance, operational efficiency, and patient satisfaction across every stage of the revenue cycle. By implementing transparent communication, leveraging technology, maintaining compliance, and focusing on accuracy, healthcare providers can optimize collections while building patient trust. Greenhive Billing Solutions provides comprehensive revenue cycle management services that help healthcare providers navigate these complexities with experienced professionals, proven processes, and a commitment to maximizing reimbursements while maintaining HIPAA compliance and transparent patient communication.