Healthcare providers face increasing pressure to maintain financial stability while delivering quality patient care. Understanding the revenue cycle is essential for any medical practice looking to optimize cash flow, reduce claim denials, and ensure timely reimbursements. This comprehensive framework encompasses every financial interaction between providers, patients, and payers, from the moment a patient schedules an appointment until the final payment is received. For practices across the United States, mastering this process translates directly into improved financial performance and operational efficiency.
Understanding the Fundamentals of the Revenue Cycle
The revenue cycle represents the complete financial journey of a patient encounter within a healthcare organization. According to the Healthcare Financial Management Association’s comprehensive overview, this process integrates clinical, administrative, and financial functions to capture and collect patient service revenue.
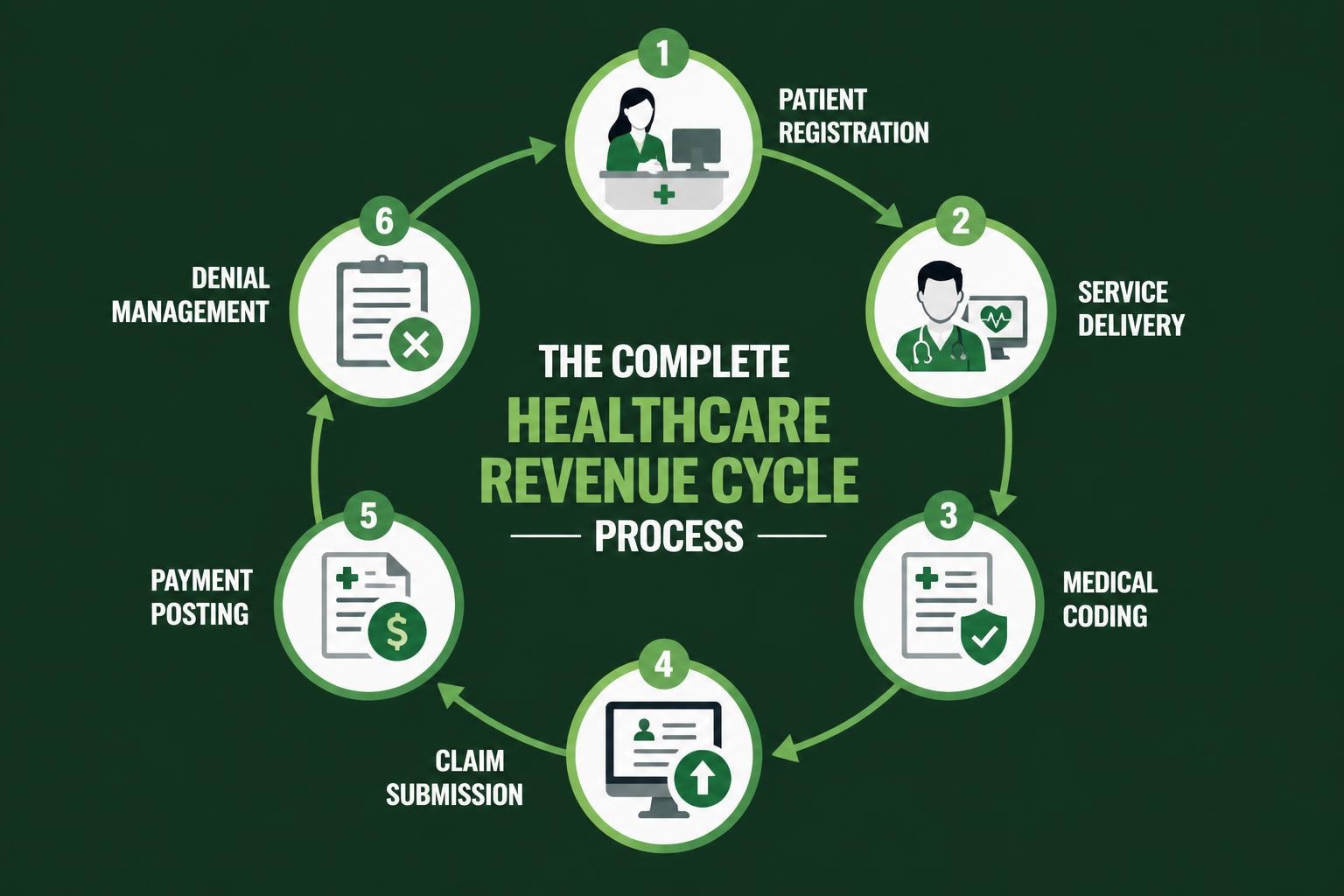
At its core, the revenue cycle includes several critical stages:
- Patient registration and insurance verification
- Medical service documentation
- Charge capture and coding
- Claims submission and adjudication
- Payment posting and reconciliation
- Patient billing and collections
- Denial management and appeals
Each stage requires precise execution to prevent revenue leakage and ensure maximum reimbursement. When one component fails, the entire cycle suffers, leading to delayed payments, increased denials, and frustrated staff members who struggle to maintain productivity.
Why the Revenue Cycle Matters for Healthcare Providers
Financial sustainability remains a top concern for medical practices of all sizes. The revenue cycle directly impacts cash flow, operating margins, and the ability to invest in new equipment, technology, and staff. Practices that optimize this process typically see faster payment cycles, reduced accounts receivable days, and improved profit margins.
Key performance indicators that measure revenue cycle efficiency include:
- Days in accounts receivable
- Clean claim rate
- Denial rate percentage
- Net collection rate
- Cost to collect per dollar
Medical practices that track these metrics consistently identify bottlenecks and opportunities for improvement. By understanding where revenue is lost or delayed, administrators can implement targeted solutions that address specific weaknesses within their operations.
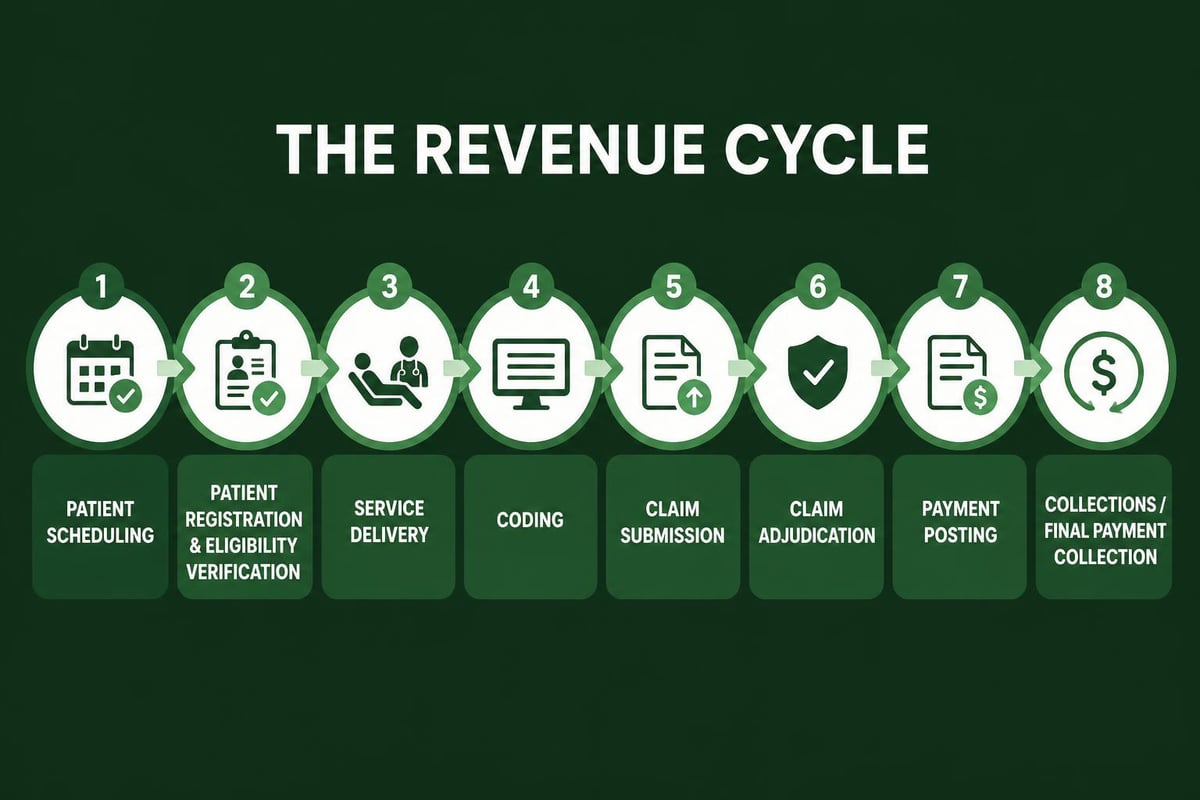
Essential Stages of the Revenue Cycle
Patient Access and Registration
The revenue cycle begins before any clinical services are provided. During patient access, staff members collect demographic information, verify insurance coverage, and determine financial responsibility. This initial stage sets the foundation for accurate billing and timely reimbursement.
Accurate patient registration prevents downstream errors that cause claim denials. When staff members verify insurance eligibility upfront through comprehensive eligibility verification services, they identify coverage issues before services are rendered, reducing the likelihood of unpaid claims.
| Patient Access Component | Impact on Revenue Cycle | Common Error |
|---|---|---|
| Demographic data collection | Ensures proper claim routing | Incorrect patient information |
| Insurance verification | Confirms coverage and benefits | Outdated insurance cards |
| Prior authorization | Prevents claim denials | Missing authorization documentation |
| Financial counseling | Improves patient collections | Unclear payment expectations |
Charge Capture and Medical Coding
After clinical services are delivered, providers must document all procedures, diagnoses, and supplies used during the patient encounter. Charge capture ensures that every billable service is recorded and assigned appropriate codes.
Medical coding translates clinical documentation into standardized codes used for billing. Certified coders review provider notes and assign CPT, ICD-10, and HCPCS codes that accurately represent the services provided. As outlined in TechTarget’s definition of revenue cycle management, this step requires both clinical knowledge and coding expertise to ensure compliance and maximize reimbursement.
Common coding challenges include:
- Incomplete or unclear provider documentation
- Selecting codes that don't support medical necessity
- Missing or incorrect modifiers
- Unbundling procedures that should be reported together
- Failing to capture all billable services
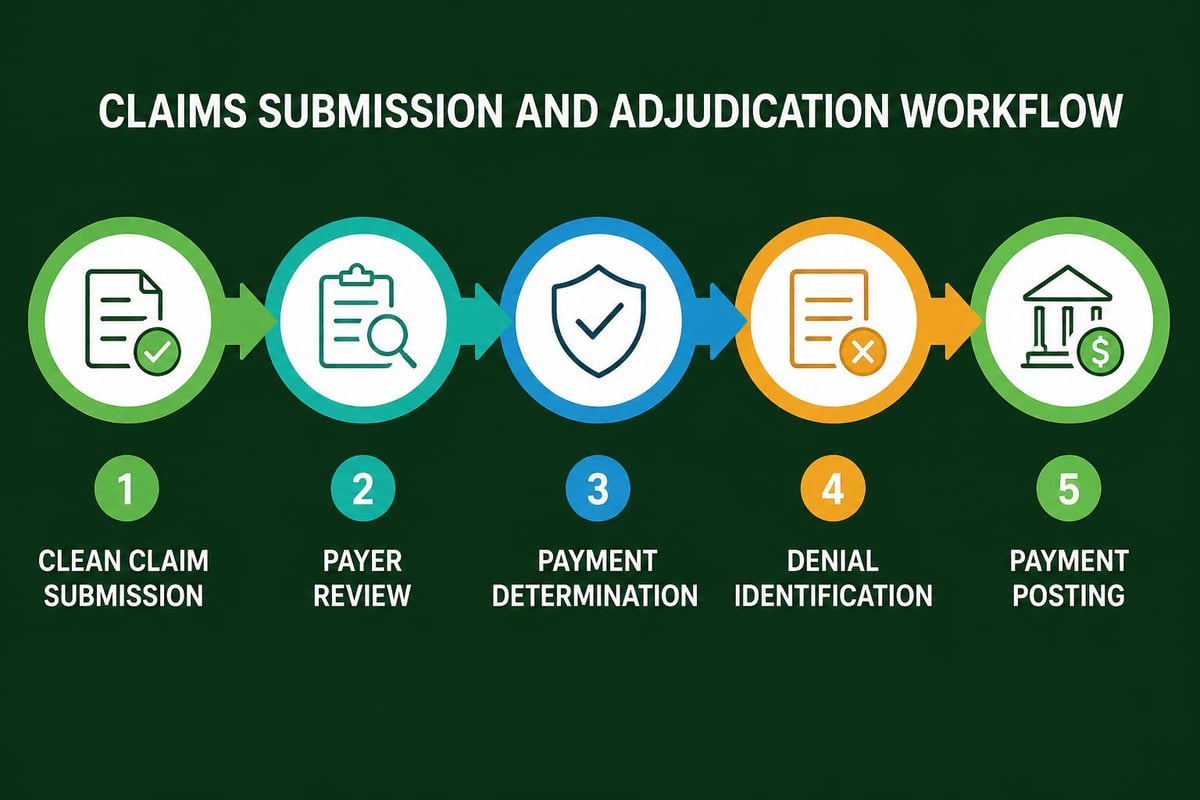
Claims Submission and Adjudication
Once charges are coded, claims are submitted to insurance payers electronically or via paper submission. Clean claims contain accurate information and meet all payer requirements, allowing for automatic processing and faster payment.
The adjudication process occurs when payers review submitted claims to determine payment amounts. Payers verify coverage, check for duplicate claims, apply contractual adjustments, and calculate patient responsibility. Through efficient medical claim submission services, practices can significantly reduce the time between service delivery and payment receipt.
Payment Posting and Reconciliation
When payers remit payment, staff members post the amounts to patient accounts and reconcile them against expected reimbursements. This stage involves reviewing explanation of benefits (EOB) statements, identifying discrepancies, and ensuring payments align with contracted rates.
Payment posting requires attention to detail and knowledge of payer contracts. Staff members must distinguish between contractual adjustments, patient responsibility, and true denials that require follow-up action. Accurate posting enables practices to identify underpayments and pursue additional reimbursement when appropriate.
Common Revenue Cycle Challenges and Strategic Solutions
High Claim Denial Rates
Claim denials represent one of the most significant challenges within the revenue cycle. Experian Health identifies complex billing processes as a primary contributor to high denial rates, which can reach 15-20% in some practices.
Top denial reasons include:
- Missing or invalid patient information
- Services not covered under the patient's plan
- Lack of prior authorization
- Coding errors or inconsistencies
- Duplicate claim submissions
- Timely filing limit violations
Effective denial management in medical billing requires systematic tracking, root cause analysis, and process improvements. Practices that implement denial prevention strategies typically reduce their denial rates by 30-50% within the first year.
Staffing Shortages and Training Gaps
The healthcare industry continues to face significant workforce challenges. Revenue cycle positions require specialized knowledge of medical terminology, coding guidelines, payer requirements, and billing regulations. Finding qualified staff members remains difficult, especially for smaller practices competing against larger health systems.
Training existing staff requires substantial time and resources. Coding guidelines change annually, payer policies evolve continuously, and regulatory requirements grow increasingly complex. Practices must invest in ongoing education to maintain staff competency and prevent costly errors.
| Challenge | Business Impact | Solution Strategy |
|---|---|---|
| Staff turnover | Increased training costs, knowledge loss | Competitive compensation, career development |
| Knowledge gaps | Higher error rates, reduced productivity | Regular training programs, certification support |
| Burnout | Decreased efficiency, quality issues | Workflow optimization, workload distribution |
| Technology adaptation | Resistance to new systems | Change management, hands-on training |
Technology Integration and Data Management
Modern revenue cycle operations depend on sophisticated software systems for billing, coding, scheduling, and reporting. However, many practices struggle with outdated technology, poor system integration, and data silos that prevent efficient workflows.
Electronic health record (EHR) systems often lack robust billing functionality, requiring separate practice management software. When systems don't communicate effectively, staff members must manually transfer information between platforms, increasing the risk of errors and duplicating effort.
Data security and HIPAA compliance add additional complexity to technology decisions. Practices must protect sensitive patient information while ensuring staff members can access the data needed to perform their jobs efficiently.
Optimizing Revenue Cycle Performance Through Best Practices
Implementing Front-End Processes That Prevent Denials
Preventing denials begins at the front desk. Staff members who verify insurance eligibility, obtain prior authorizations, and collect accurate patient information create a foundation for clean claims and faster payment.
Front-end best practices include:
- Real-time eligibility verification: Check coverage before every appointment, not just new patient visits
- Prior authorization tracking: Maintain a centralized system to monitor authorization status and expiration dates
- Point-of-service collections: Collect copayments, deductibles, and past-due balances at check-in
- Patient financial counseling: Discuss expected costs and payment options before services are rendered
- Insurance card scanning: Capture complete insurance information electronically to reduce data entry errors
Leveraging Analytics for Continuous Improvement
Data analytics transform the revenue cycle from a reactive process to a proactive performance management system. By analyzing key metrics, practices identify trends, predict future challenges, and measure the impact of improvement initiatives.
Essential revenue cycle analytics include:
- Denial trends by payer, provider, and denial reason
- Days in accounts receivable by payer category
- Clean claim rates over time
- Net collection rates by service line
- Staff productivity metrics
Practices that embrace data-driven decision making consistently outperform competitors who rely on intuition alone. Monthly scorecards keep teams focused on priority areas and create accountability for achieving financial targets.
Establishing Effective Denial Management Workflows
Managing denials requires more than simply resubmitting rejected claims. Effective programs analyze denial patterns, implement prevention strategies, and prioritize high-value appeals. Understanding how denial management improves cash flow enables practices to recover revenue that would otherwise be written off.
A comprehensive denial management program includes:
- Daily denial tracking and categorization
- Root cause analysis for recurring denial patterns
- Provider education on documentation requirements
- Timely appeal submission with supporting documentation
- Process changes to prevent future denials
- Financial impact reporting to measure program effectiveness
Successful denial management requires coordination between clinical and administrative staff. Providers must understand how their documentation affects coding and billing, while billing staff need access to clinical expertise when preparing appeals.
The Role of Outsourcing in Revenue Cycle Optimization
When to Consider Professional Revenue Cycle Services
Many healthcare providers reach a point where internal resources cannot keep pace with revenue cycle demands. Practices experiencing high denial rates, increasing days in accounts receivable, or staff burnout often benefit from partnering with specialized revenue cycle management providers.
Signs that outsourcing may be beneficial:
- Denial rates consistently exceed industry benchmarks
- Days in accounts receivable continue to climb
- Staff turnover disrupts billing operations
- Technology investments strain practice budgets
- Compliance concerns create liability risks
Professional revenue cycle management teams bring specialized expertise, advanced technology, and proven processes that improve financial performance. These partnerships allow providers to focus on patient care while experienced professionals handle complex billing and coding tasks.
Key Considerations When Selecting a Revenue Cycle Partner
Choosing the right revenue cycle partner significantly impacts practice finances and operations. Providers should evaluate potential partners based on industry experience, technology capabilities, compliance standards, and transparent communication practices.
Essential evaluation criteria include:
| Evaluation Area | Key Questions | Impact on Practice |
|---|---|---|
| Industry expertise | Do they specialize in your specialty? | Better understanding of specialty-specific requirements |
| Technology platform | What systems do they use? | Integration capabilities, reporting access |
| Compliance standards | Are they HIPAA certified? | Risk mitigation, data security |
| Transparency | How often do they report performance? | Visibility into financial operations |
| Pricing structure | Is pricing aligned with results? | Cost predictability, value alignment |
Effective partnerships require clear communication, defined expectations, and regular performance reviews. Providers should maintain oversight of their revenue cycle while leveraging partner expertise to drive continuous improvement.
Adapting the Revenue Cycle to Evolving Healthcare Dynamics
Value-Based Care and Alternative Payment Models
The healthcare industry continues shifting from fee-for-service reimbursement to value-based care models that reward quality over volume. This transition fundamentally changes how providers approach the revenue cycle, requiring new metrics, reporting capabilities, and quality tracking systems.
Alternative payment models such as bundled payments, accountable care organizations, and capitation require sophisticated data analytics to track patient outcomes, manage utilization, and demonstrate value. Practices must expand their revenue cycle capabilities beyond traditional claims processing to include quality reporting, risk adjustment, and population health management.
Regulatory Compliance and Changing Payer Requirements
Healthcare regulations evolve continuously, creating compliance challenges for revenue cycle operations. From ICD-10 code updates to new prior authorization requirements, practices must stay current with changing rules or face claim denials and potential audit penalties.
Recent regulatory changes affecting the revenue cycle:
- Price transparency requirements for hospital services
- No Surprises Act balance billing protections
- Enhanced security requirements for electronic health information
- Expanded telehealth coverage and billing guidelines
- Updated documentation requirements for evaluation and management services
Staying current with regulatory changes requires dedicated resources and ongoing education. Many practices struggle to maintain compliance while managing daily operations, making professional guidance increasingly valuable.
Patient Financial Responsibility and Collections
As high-deductible health plans become more common, patient financial responsibility continues to grow. Practices must enhance their patient collections strategies while maintaining positive patient relationships and delivering excellent care experiences.
Effective patient collections strategies include:
- Clear financial policies communicated at registration
- Cost estimates provided before scheduled services
- Multiple payment options including payment plans
- Automated payment reminders via text or email
- Online payment portals for patient convenience
Balancing collections efforts with patient satisfaction requires sensitivity and professionalism. Practices that communicate expectations clearly, offer flexible payment options, and treat patients with respect achieve higher collection rates while maintaining strong patient relationships.
Measuring Revenue Cycle Success and Setting Performance Goals
Establishing Baseline Metrics and Benchmarks
Improving the revenue cycle begins with understanding current performance. Practices should establish baseline metrics across key performance indicators, then compare results against industry benchmarks to identify areas requiring attention.
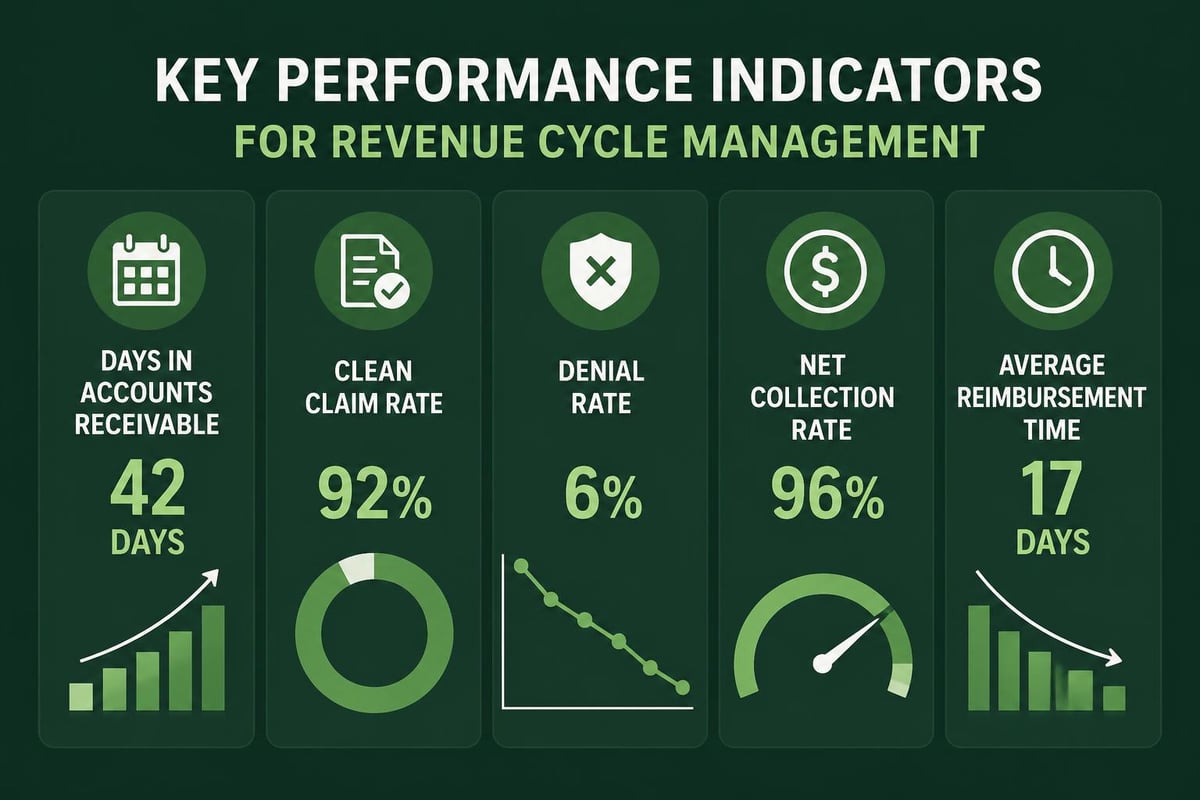
Industry benchmark targets for key metrics:
- Days in accounts receivable: 30-40 days
- Clean claim rate: 95% or higher
- Denial rate: Less than 5%
- Net collection rate: 95-99%
- Cost to collect: Less than 3% of collections
These benchmarks provide general guidance, but targets may vary based on specialty, payer mix, and geographic location. Practices should track trends over time rather than focusing exclusively on single-month results.
Creating Accountability Through Performance Reporting
Regular performance reporting keeps revenue cycle teams focused on priority areas and creates accountability for achieving financial goals. Monthly scorecards should track key metrics, highlight trends, and identify specific action items for improvement.
Effective revenue cycle scorecards include:
- Current month performance versus prior periods
- Year-to-date trends for each metric
- Comparison to established goals and benchmarks
- Top denial reasons with financial impact
- Aging accounts receivable by payer category
- Staff productivity metrics and capacity utilization
Sharing performance data with all team members creates transparency and encourages collaborative problem-solving. When staff members understand how their work impacts practice finances, they become more engaged in improvement initiatives.
Future Trends Shaping the Revenue Cycle
Artificial Intelligence and Automation
Technology continues transforming revenue cycle operations through artificial intelligence, machine learning, and robotic process automation. These tools handle repetitive tasks, identify patterns in denial data, and predict payment outcomes with increasing accuracy.
AI-powered coding assistance helps coders work more efficiently while reducing errors. Automated eligibility verification runs continuously in the background, flagging coverage changes before appointments. Predictive analytics identify claims likely to be denied, allowing staff to address issues before submission.
Patient Engagement and Digital Health Tools
Patient expectations for digital convenience continue rising. Modern patients want online scheduling, digital payment options, and mobile access to billing information. Practices that embrace patient-facing technology improve collections and enhance patient satisfaction.
Digital health tools also impact clinical documentation and charge capture. Mobile devices enable providers to document encounters at the point of care, improving accuracy and completeness. Integration between clinical and billing systems reduces manual data entry and accelerates the billing cycle.
Integrated Care Coordination and Information Sharing
Healthcare delivery increasingly involves multiple providers coordinating care across different settings. Effective care coordination requires seamless information sharing, including financial data that tracks patient responsibility, coverage details, and payment status.
Interoperability standards enable different systems to exchange data automatically, reducing administrative burden and improving accuracy. As information sharing becomes more sophisticated, revenue cycle processes will become more automated and efficient.
Mastering the revenue cycle requires comprehensive strategies that address front-end processes, coding accuracy, claims management, and denial prevention. Healthcare providers who optimize these interconnected stages achieve stronger financial performance, reduce administrative burden, and create capacity for growth. Greenhive Billing Solutions delivers comprehensive revenue cycle management services designed specifically for healthcare providers seeking to improve cash flow and operational efficiency. Our experienced team handles everything from eligibility verification to denial management, allowing your practice to focus on delivering exceptional patient care while we ensure maximum reimbursements and streamlined financial operations.