Management billing represents a critical administrative function that transforms how healthcare organizations approach revenue cycle operations. This strategic oversight encompasses the coordination, execution, and continuous improvement of billing processes to ensure timely reimbursements and financial stability. For healthcare providers navigating increasingly complex regulatory requirements and payer protocols, effective management billing serves as the foundation for sustainable practice growth. The approach combines operational expertise with systematic process control to minimize errors, reduce claim denials, and accelerate cash flow across all service lines.
Understanding Management Billing in Healthcare Revenue Cycles
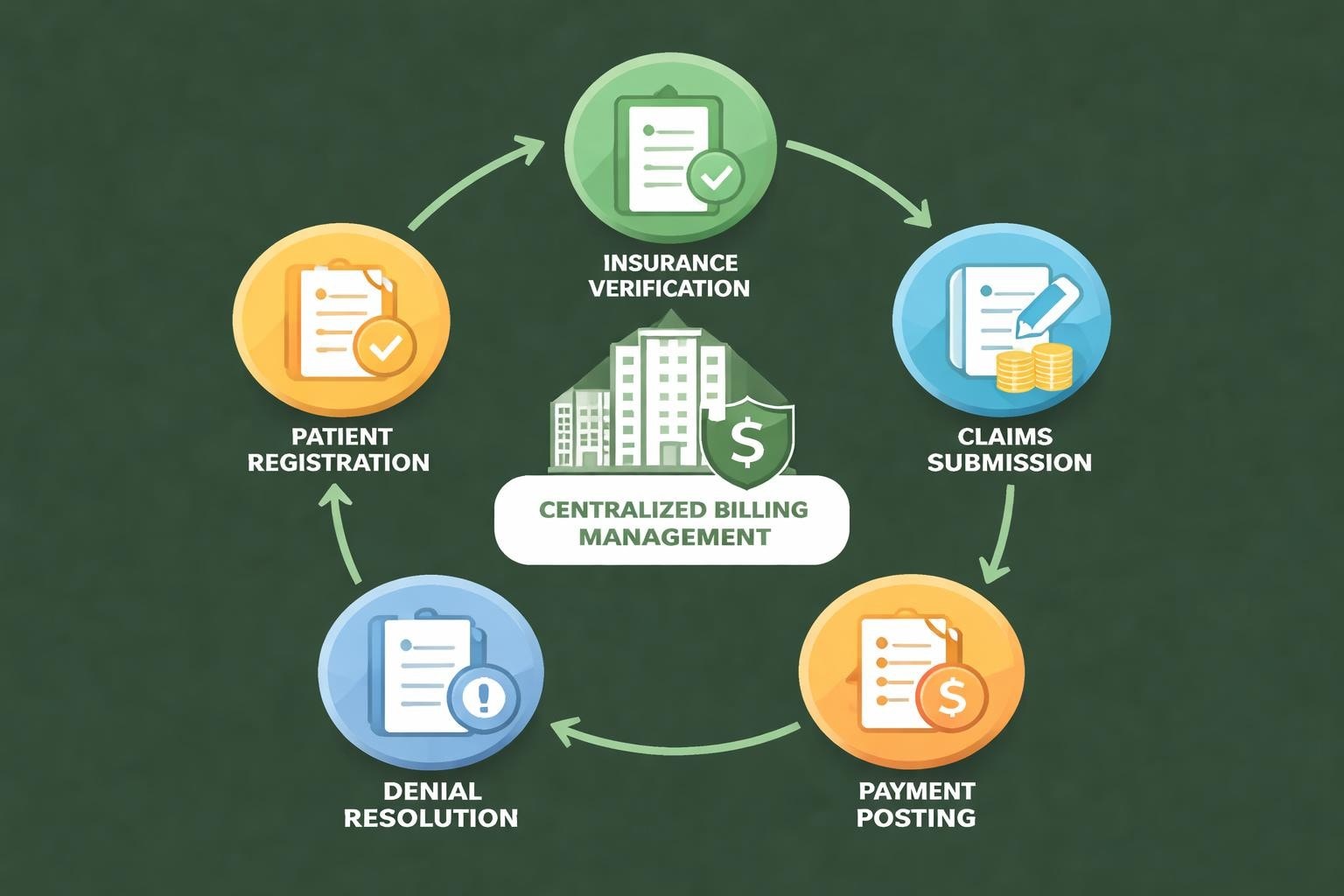
Management billing extends beyond basic invoice generation to encompass comprehensive oversight of the entire revenue cycle. This discipline involves coordinating multiple touchpoints from patient registration through final payment reconciliation. Healthcare organizations implementing robust management billing frameworks establish standardized protocols that govern how charges are captured, coded, submitted, and followed up across all payer categories.
The scope of management billing includes developing workflows that align with regulatory compliance standards while optimizing operational efficiency. Professional billing managers establish key performance indicators to measure cycle times, collection rates, and denial percentages. These metrics provide actionable intelligence for continuous process refinement.
Core Components of Effective Management Billing
Successful management billing operations rest on several foundational elements that work together to create a cohesive revenue cycle ecosystem:
- Charge capture accuracy ensuring all billable services are documented and coded correctly
- Claims scrubbing processes that identify and correct errors before submission
- Payer contract management to verify reimbursement rates and coverage requirements
- Denial tracking systems that categorize rejections and implement corrective actions
- Payment posting protocols establishing consistent application of reimbursements and adjustments
- Accounts receivable monitoring with aging reports and targeted collection strategies
Each component requires specific expertise and systematic execution. When healthcare providers implement comprehensive denial management strategies, they address one of the most costly aspects of revenue cycle performance. Management billing frameworks must also incorporate ongoing staff training to maintain competency as regulations and payer requirements evolve.

Implementing Strategic Management Billing Practices
Organizations achieve optimal results when they approach management billing as a strategic initiative rather than a purely administrative function. This perspective shift enables healthcare leaders to allocate appropriate resources and establish governance structures that support long-term financial health.
Step-by-Step Implementation Framework
Step 1: Assessment and Baseline Measurement
Begin by evaluating current billing performance across all relevant metrics including days in accounts receivable, clean claim rate, and collection percentage. Document existing workflows and identify bottlenecks or redundancies that impede efficient processing.
Step 2: Process Standardization
Develop written procedures for each billing activity from patient check-in through payment reconciliation. Standardization reduces variation and creates consistency across staff members, which directly impacts accuracy and processing speed.
Step 3: Technology Integration
Select and implement systems that automate routine tasks while providing real-time visibility into billing operations. Integration between clinical documentation and billing platforms minimizes manual data entry and reduces transcription errors.
Step 4: Staff Training and Development
Establish ongoing education programs that keep billing personnel current with coding updates, payer policy changes, and regulatory requirements. Investing in staff competency pays dividends through improved first-pass resolution rates.
Step 5: Performance Monitoring
Create dashboards that track key indicators daily or weekly, enabling rapid response to emerging issues. Regular performance reviews identify trends and inform strategic adjustments to billing protocols.
Automation and Technology in Management Billing
Modern management billing leverages technology platforms to handle high-volume, repetitive tasks while freeing skilled professionals to focus on complex problem-solving and strategic oversight. Automation represents one of the most impactful investments healthcare organizations can make to improve revenue cycle performance.
| Technology Function | Impact on Management Billing | Key Benefits |
|---|---|---|
| Eligibility Verification | Real-time insurance validation | Reduces registration errors, prevents coverage issues |
| Claims Scrubbing | Pre-submission error detection | Increases clean claim rate, accelerates reimbursement |
| Electronic Remittance | Automated payment posting | Eliminates manual posting delays, improves accuracy |
| Denial Tracking | Pattern identification and categorization | Enables root cause analysis, prevents recurring issues |
| Reporting Analytics | Performance measurement and trending | Supports data-driven decision making, identifies opportunities |
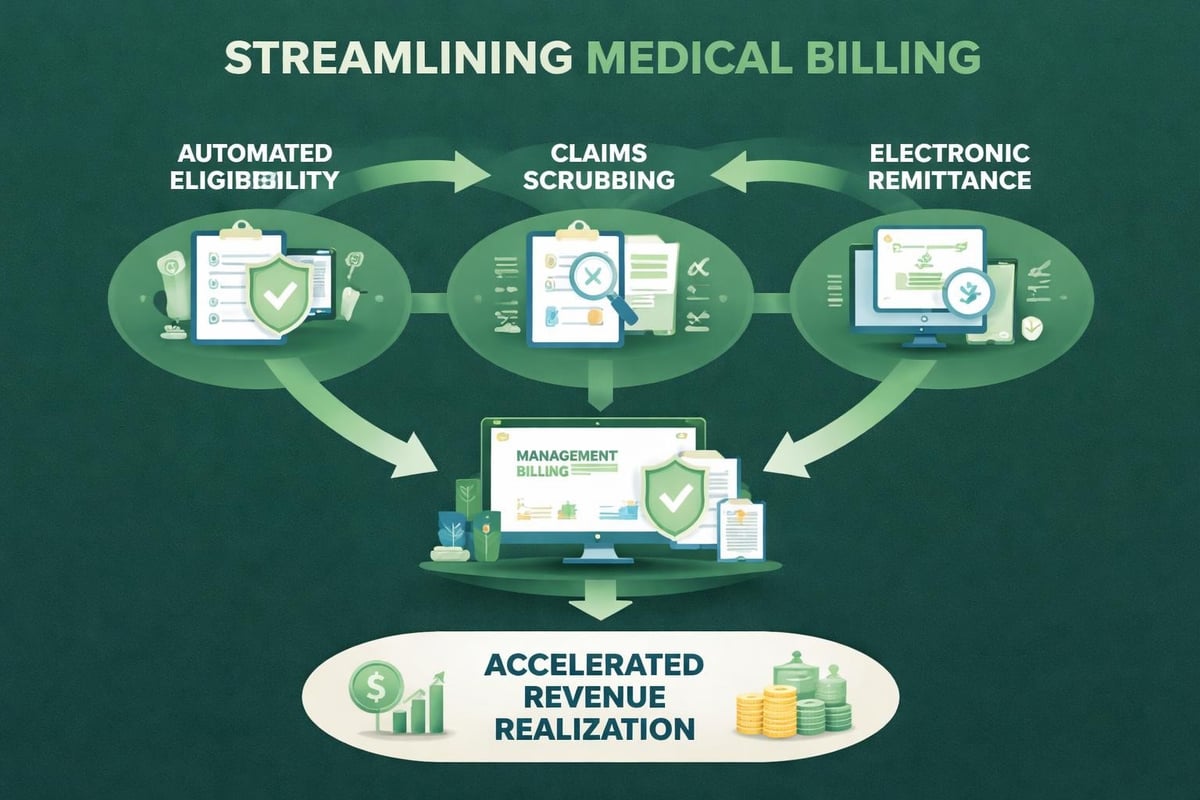
Healthcare providers implementing automated solutions experience measurable improvements in operational efficiency. According to best practices in billing and collections, organizations that adopt automated systems reduce processing costs while improving accuracy across billing operations.
The selection of appropriate technology requires careful evaluation of practice-specific needs and workflows. Revenue cycle management service providers utilize industry-standard platforms adapted to each client's unique requirements, ensuring seamless integration with existing systems.
Data Security and Compliance Considerations
Management billing technology must incorporate robust security protocols to protect sensitive patient information. HIPAA compliance requirements mandate specific safeguards for electronic protected health information throughout the billing process. Organizations implementing automated billing solutions verify that platforms include encryption, access controls, audit logging, and secure transmission capabilities.
Regular compliance audits verify that management billing practices adhere to federal regulations and payer-specific requirements. Documentation of security measures and staff training creates an essential compliance framework that protects both patients and healthcare organizations from data breaches and regulatory penalties.
Common Management Billing Challenges and Solutions
Healthcare organizations encounter predictable obstacles when establishing or refining management billing operations. Recognizing these challenges enables proactive planning and mitigation strategies that prevent revenue disruption.
Payer Complexity and Varying Requirements
Each insurance carrier maintains unique submission requirements, coverage policies, and documentation standards. This variation complicates billing operations and increases the likelihood of claim rejections when staff members lack current knowledge of payer-specific protocols.
Solution: Maintain a centralized payer policy repository that documents submission requirements, prior authorization protocols, and common rejection reasons for each major carrier. Assign staff members to monitor specific payers and distribute updates through regular team communications.
Coding Accuracy and Regulatory Changes
Medical coding systems undergo continuous updates as new procedures are developed and regulatory bodies refine classification standards. Understanding different types of medical coding becomes essential for accurate charge capture and appropriate reimbursement.
Solution: Establish relationships with coding specialists who maintain current certifications and participate in ongoing education. Implement regular auditing processes that sample coded encounters and provide feedback to improve documentation and coding precision.
Denial Management and Appeals Processing
Even well-managed billing operations experience claim denials that require systematic review and appropriate appeals. Denial management in medical billing directly impacts cash flow and requires dedicated resources to maximize recovery.
Solution: Create a denial management workflow that categorizes rejections by reason code, assigns responsibility for appeals, and tracks resolution timelines. Analyze denial patterns monthly to identify systemic issues requiring workflow modifications or additional staff training.
Financial Impact of Optimized Management Billing
The financial implications of effective management billing extend throughout healthcare organizations, influencing everything from operating capital to strategic growth initiatives. Quantifying these impacts helps leadership teams prioritize revenue cycle investments and allocate resources appropriately.
Healthcare practices implementing comprehensive management billing improvements typically observe:
- Reduced days in accounts receivable by 15-30% through faster claim processing and payment posting
- Increased clean claim rates to 95% or higher through enhanced scrubbing and coding accuracy
- Improved collection percentages with systematic follow-up on outstanding balances
- Decreased write-offs resulting from better denial management and timely appeals
- Enhanced cash flow predictability enabling better financial planning and investment decisions
These improvements translate directly to bottom-line performance. A practice collecting $5 million annually that reduces its days in accounts receivable from 45 to 35 days effectively releases approximately $400,000 in working capital that can be deployed for operational needs or strategic initiatives.
Return on Investment for Management Billing Services
Healthcare organizations evaluating whether to enhance internal capabilities or partner with specialized service providers should consider both direct costs and opportunity costs. Internal billing departments require ongoing investments in staff salaries, benefits, training, technology licenses, and facility overhead.
| Cost Category | Internal Department | Outsourced Services |
|---|---|---|
| Personnel | Salaries, benefits, taxes, turnover costs | Service fees (percentage or per-claim) |
| Technology | Software licenses, updates, maintenance | Included in service agreement |
| Training | Continuing education, certifications, conferences | Provider responsibility |
| Compliance | Audit costs, consultant fees, remediation | Provider maintains compliance |
| Scalability | Fixed costs regardless of volume | Variable costs aligned with volume |
Many healthcare providers discover that partnering with experienced revenue cycle management specialists delivers superior financial performance compared to internal operations. Professional billing services maintain specialized expertise, leverage economies of scale for technology investments, and adapt quickly to regulatory changes.
Best Practices for Sustainable Management Billing Excellence
Achieving initial improvements in billing performance represents an important milestone, but sustaining excellence requires ongoing commitment to process discipline and continuous improvement. Healthcare organizations that maintain high-performance revenue cycles embed specific practices into their operational culture.
Establishing Clear Accountability Structures
Assign specific individuals or teams responsibility for each component of the billing process. When everyone owns everything, no one takes definitive action on problems. Clear accountability ensures that issues receive prompt attention and resolution. Understanding what billing and coding specialists contribute helps organizations structure teams appropriately.
Document performance expectations for each role within the billing function. Measurable objectives create clarity about priorities and enable fair performance evaluation. Share performance data transparently so team members understand how their contributions impact overall results.
Regular Process Auditing and Refinement
Schedule quarterly reviews of billing workflows to identify inefficiencies or areas where error rates exceed acceptable thresholds. Process audits should examine both technical accuracy and operational efficiency. Common audit focus areas include charge lag time, coding accuracy rates, claim submission timelines, and payment posting delays.
Following medical billing best practices ensures that processes remain aligned with industry standards and regulatory requirements. Documentation of audit findings and implemented improvements creates an important compliance record.
Cultivating Payer Relationships
Proactive communication with insurance carriers helps resolve issues quickly and may provide advance notice of policy changes. Designated staff members should maintain regular contact with payer representatives to discuss recurring denial patterns, clarify coverage questions, and address systematic problems.
Building collaborative relationships rather than adversarial interactions facilitates faster claim resolution and may provide preferential support when complex cases require payer intervention. Document all payer communications to create a reference history for future interactions.
Investing in Ongoing Education
Healthcare billing regulations, coding standards, and payer policies evolve continuously. Organizations that prioritize staff education maintain competitive advantages through superior knowledge application. Budget for regular training opportunities including webinars, conferences, certification programs, and subscriptions to industry publications.
Cross-training team members across multiple billing functions builds operational resilience and creates career development pathways that improve retention. When staff members understand the full revenue cycle context, they make better decisions within their specific areas of responsibility.
Integration with Clinical Operations
Management billing achieves optimal effectiveness when it connects seamlessly with clinical workflows rather than operating as an isolated administrative function. This integration begins at the point of service and extends through all patient interactions.
Clinical staff members who understand the billing implications of documentation decisions create more complete records that support accurate coding and appropriate reimbursement. Front-desk personnel trained in insurance verification prevent coverage issues before services are rendered. Providers who document medical necessity thoroughly reduce denial risk for services requiring prior authorization.
Creating feedback loops between billing operations and clinical teams closes knowledge gaps that contribute to revenue leakage. When billing staff identify recurring documentation deficiencies, clinical leadership can implement targeted training to address root causes. Shared performance metrics align both functions toward common financial objectives.
Healthcare organizations implementing comprehensive revenue cycle analytics gain visibility into how clinical decisions impact financial performance. This intelligence enables more informed strategic planning around service line development, staffing models, and payer contract negotiations.
Scalability and Growth Considerations
Management billing systems must accommodate practice growth without proportional increases in administrative burden. Scalable processes and technology platforms enable healthcare organizations to expand patient volumes, add providers, or open new locations while maintaining billing performance standards.
Evaluating scalability requires examining both technical capabilities and operational workflows. Systems that require extensive manual intervention become bottlenecks as volume increases. Platforms offering workflow automation, exception-based management, and robust reporting scale more effectively across growing organizations.
Strategic planning for expansion should include revenue cycle impact assessments. New service lines may require specialized coding expertise or present unique payer contracting considerations. Geographic expansion introduces state-specific Medicaid requirements and regional payer mix variations. Addressing these factors proactively prevents revenue disruption during growth phases.
Partnership with specialized revenue cycle management providers offers inherent scalability advantages. Professional billing services accommodate volume fluctuations without requiring practices to hire additional internal staff or invest in expanded technology infrastructure. This flexibility proves particularly valuable for practices experiencing seasonal variations or rapid growth trajectories.
Effective management billing transforms healthcare revenue cycles from reactive administrative burdens into strategic advantages that support financial stability and practice growth. By implementing systematic processes, leveraging appropriate technology, and maintaining focus on continuous improvement, healthcare organizations position themselves for sustainable success in increasingly complex reimbursement environments. Greenhive Billing Solutions provides comprehensive revenue cycle management services designed specifically for healthcare providers seeking to optimize billing performance, reduce administrative burden, and maximize reimbursements through expert oversight and proven methodologies.