Healthcare providers face increasing pressure to maintain financial stability while delivering quality patient care. The complexity of medical billing, insurance verification, and claims processing demands a strategic approach that goes beyond simple transaction management. Claims care RCM represents a comprehensive methodology that integrates every aspect of the revenue cycle into a cohesive system designed to maximize reimbursements, reduce denials, and streamline administrative workflows. For practices of all sizes, understanding and implementing effective claims care strategies has become essential to long-term viability and growth.
Understanding the Foundation of Claims Care RCM
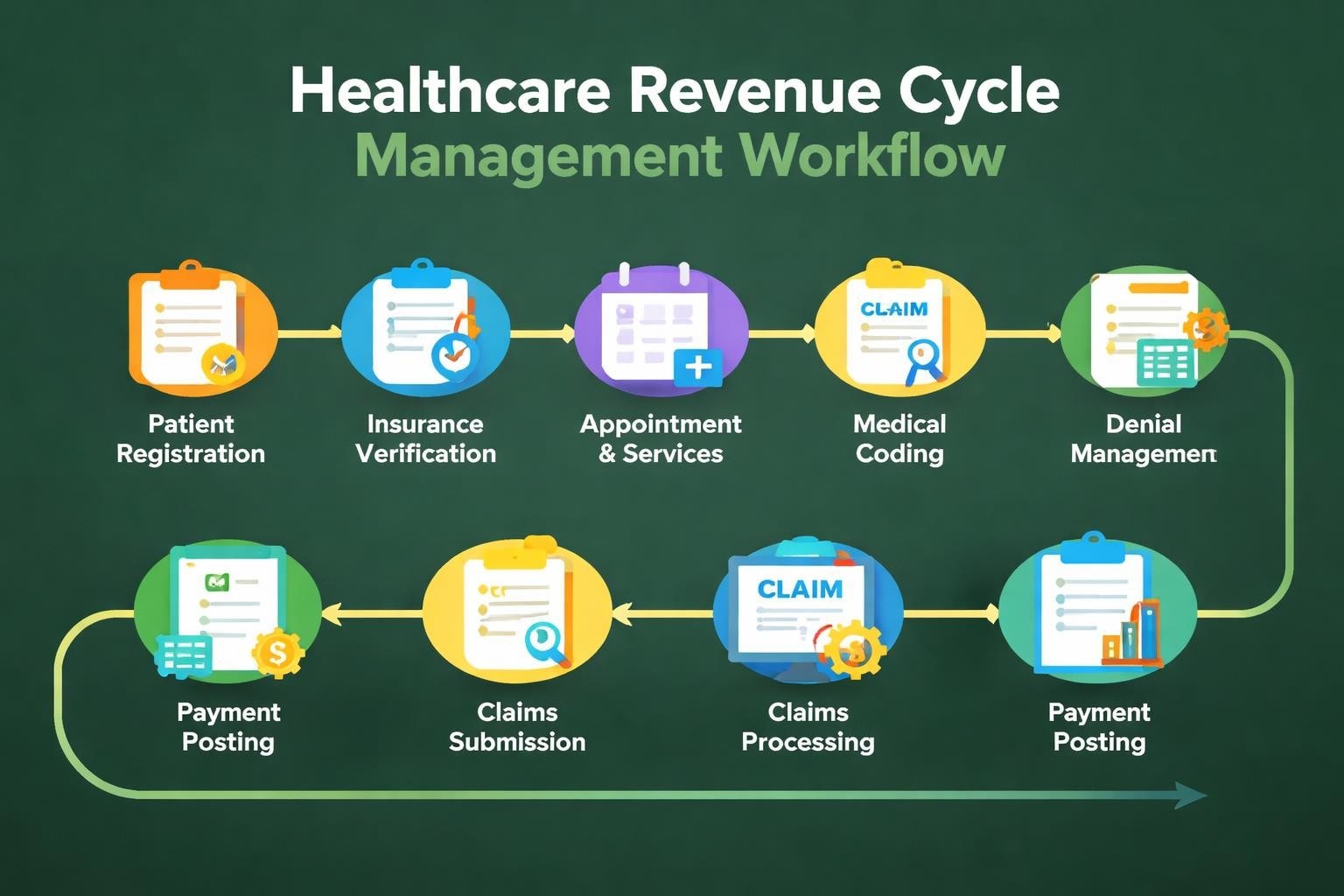
Claims care RCM encompasses the entire lifecycle of patient revenue management, from the moment an appointment is scheduled through final payment reconciliation. This holistic approach recognizes that each stage of the revenue cycle directly impacts financial outcomes and operational efficiency.
The foundation of effective claims care begins with accurate patient data collection and insurance verification. Before services are rendered, healthcare providers must confirm coverage details, understand benefit limitations, and identify any prior authorization requirements. This upfront diligence prevents downstream complications that lead to claim denials and delayed payments.
Core Components of Effective Claims Management
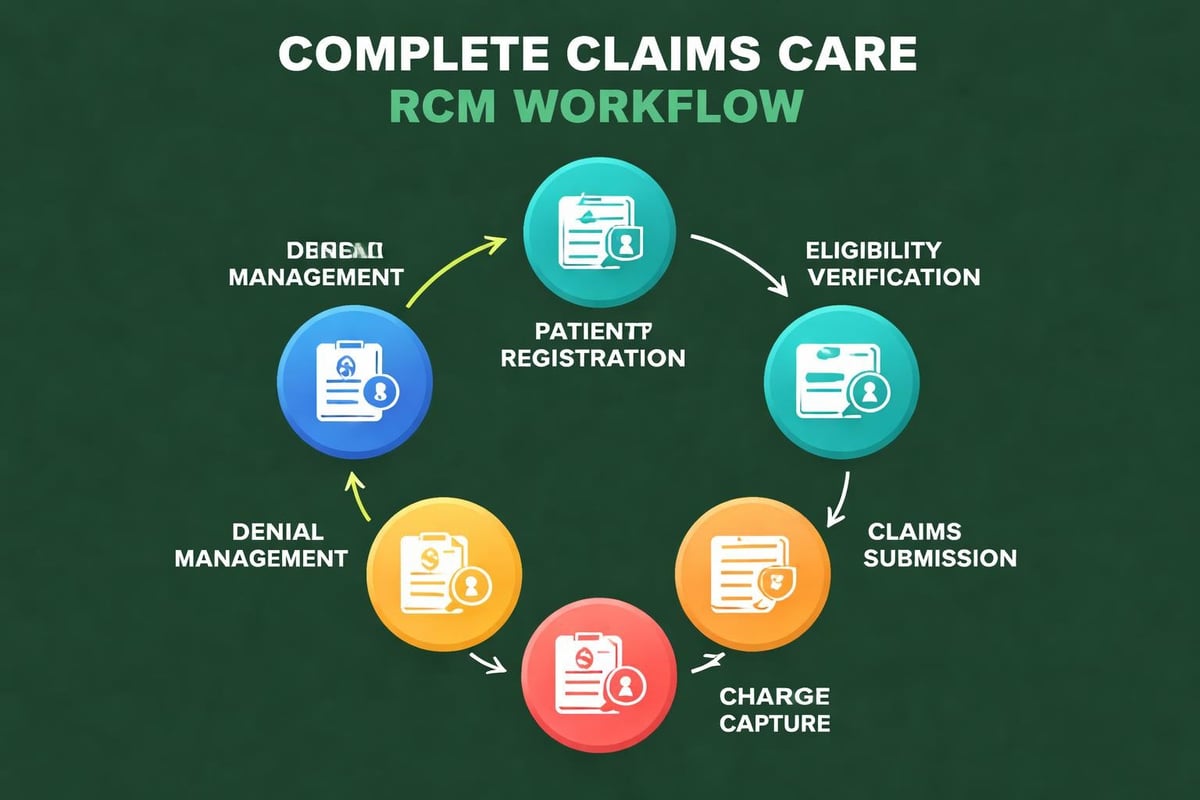
Successfully managing claims requires attention to multiple interdependent elements that work together to ensure clean submissions and prompt reimbursements:
- Patient registration accuracy establishes the data foundation for all subsequent billing activities
- Real-time eligibility verification confirms coverage and identifies potential payment issues before service delivery
- Charge capture precision ensures all billable services are documented and coded correctly
- Claims scrubbing technology catches errors before submission to payers
- Denial tracking systems identify patterns and enable process improvements
- Payment posting efficiency maintains accurate accounts receivable records
According to revenue cycle management best practices, achieving clean claims rates above 95% requires systematic attention to each of these components. Organizations that treat claims care as an integrated system rather than isolated tasks consistently outperform those with fragmented approaches.
Strategic Approaches to Claims Processing
Claims care RCM demands a proactive rather than reactive mindset. Healthcare providers who excel in revenue cycle management implement strategies that prevent problems before they occur rather than simply addressing issues after denials arrive.
Pre-Submission Verification Protocols
Implementing comprehensive verification protocols before claims submission dramatically reduces denial rates and accelerates payment cycles. These protocols should include systematic checks at multiple points in the workflow.
Step 1: Verify patient demographic information against insurance records to ensure exact matches across all data fields.
Step 2: Confirm coverage eligibility and benefit details specific to the planned procedures or services.
Step 3: Review medical necessity documentation to ensure clinical notes support the proposed billing codes.
Step 4: Cross-reference procedure codes with payer-specific coverage policies and local coverage determinations.
Step 5: Validate that all required modifiers are applied correctly to prevent bundling errors or inappropriate denials.
Organizations that follow structured verification processes report significantly higher first-pass payment rates and reduced administrative costs associated with rework and appeals. The investment in front-end accuracy yields substantial returns through improved cash flow and reduced days in accounts receivable.
Technology Integration in Claims Care Systems
Modern claims care RCM relies heavily on technology to manage the volume and complexity of healthcare billing. However, technology alone does not guarantee success. The human expertise required to configure systems, interpret results, and make strategic decisions remains irreplaceable.
Advanced revenue cycle platforms integrate with electronic health records, practice management systems, and clearinghouse networks to create seamless data flows. These integrations eliminate manual data entry, reduce transcription errors, and enable real-time status monitoring throughout the claims lifecycle.
| Technology Component | Primary Function | Impact on Claims Care |
|---|---|---|
| Claims Scrubbing Software | Pre-submission error detection | Reduces denial rates by 30-50% |
| Eligibility Verification Systems | Real-time coverage confirmation | Prevents eligibility-related denials |
| Denial Management Platforms | Pattern analysis and tracking | Identifies systemic issues for correction |
| Payment Posting Automation | Reconciliation and posting | Accelerates cash application and reduces errors |
| Analytics Dashboards | Performance monitoring | Enables data-driven decision making |
Healthcare providers often partner with specialized RCM service providers who bring both technological capabilities and deep industry expertise. These partnerships allow practices to leverage enterprise-grade systems without the capital investment and ongoing maintenance requirements of in-house infrastructure.
Understanding healthcare revenue cycle analytics enables organizations to identify performance gaps and prioritize improvement initiatives based on quantifiable data rather than assumptions.
Denial Management as a Claims Care Priority
Denial management represents one of the most critical aspects of claims care RCM. Even organizations with strong front-end processes experience denials due to changing payer policies, coding updates, and the inherent complexity of medical billing regulations.
Building a Systematic Denial Response Framework
Effective denial management requires both immediate response capabilities and long-term strategic improvements. Organizations must address individual denials while simultaneously analyzing patterns to prevent future occurrences.
The most successful denial management programs categorize denials by type, root cause, and preventability. This classification enables targeted interventions that address underlying issues rather than simply treating symptoms.
- Clinical denials related to medical necessity require documentation improvements and better clinical-billing communication
- Technical denials stemming from coding errors indicate the need for coder training or technology upgrades
- Eligibility denials suggest weaknesses in front-end verification processes
- Timely filing denials point to workflow bottlenecks or insufficient claim tracking
Organizations should establish clear metrics for denial management performance, including denial rate by category, appeal success rate, and average time to resolution. Regular review of these metrics against industry benchmarks identifies opportunities for improvement and demonstrates the value of denial management investments.
Specialized denial management services provide expertise in appeals writing, payer negotiations, and systematic root cause analysis that many practices struggle to maintain in-house.

Optimizing the Claims Submission Process
Claims submission represents the moment when all upstream revenue cycle activities converge into a single transaction with the payer. The quality of claims submission directly determines payment speed, denial rates, and overall revenue cycle performance.
Clean Claims Standards and Achievement
The industry standard for clean claims-those submitted without errors requiring additional information or correction-stands at 95% or higher. Achieving this benchmark requires disciplined processes and continuous quality monitoring.
Clean claims standards encompass multiple dimensions beyond simple data accuracy. Claims must include appropriate supporting documentation, comply with payer-specific formatting requirements, and reflect current coding guidelines. The definition of a clean claim varies somewhat by payer, making it essential to understand individual payer requirements.
Healthcare providers should implement systematic claim review processes before electronic submission. Automated scrubbing catches many technical errors, but human review remains necessary for complex cases involving unusual circumstances or multiple procedures.
According to comprehensive RCM solutions, organizations that invest in robust claims submission processes see dramatic improvements in days in accounts receivable and overall collection rates. The correlation between clean claim rates and financial performance is consistently documented across healthcare settings.
Patient Financial Responsibility and Collections
The shift toward high-deductible health plans has fundamentally changed the revenue cycle landscape. Patient financial responsibility now represents a larger percentage of practice revenue than ever before, requiring new approaches to collections and patient financial engagement.
Claims care RCM must now address two payers for virtually every encounter: the insurance company and the patient. Managing these dual payment sources requires different strategies, communication approaches, and technology solutions.
Strategies for Patient Payment Collection
Healthcare providers face unique challenges in patient collections due to the sensitive nature of medical services and the complexity of explaining financial responsibility. Effective patient collection strategies balance financial necessity with relationship preservation.
Transparent communication about costs before service delivery sets appropriate expectations and improves collection rates. Patients who understand their financial responsibility upfront are more likely to pay promptly and less likely to dispute charges.
Multiple payment options increase the likelihood of successful collections. Offering payment plans, online payment portals, and automated payment arrangements accommodates different patient preferences and financial situations. Organizations report collection rate improvements of 20-30% when implementing comprehensive patient payment strategies.
The integration of patient financial counseling into the revenue cycle workflow helps patients navigate complex insurance benefits and identify potential assistance programs. This supportive approach to collections maintains positive patient relationships while improving financial outcomes.
Compliance and Regulatory Considerations
Claims care RCM operates within a highly regulated environment where compliance failures carry significant financial and legal consequences. Healthcare providers must navigate federal regulations, state-specific requirements, and individual payer policies while maintaining efficient workflows.
HIPAA compliance governs all aspects of patient data handling throughout the revenue cycle. From initial registration through final payment posting, every touchpoint must protect patient privacy and maintain data security. Regular staff training, robust access controls, and comprehensive audit trails form the foundation of HIPAA-compliant claims care processes.
| Regulatory Area | Key Requirements | RCM Impact |
|---|---|---|
| HIPAA Privacy | Protected health information safeguards | Affects data sharing and communication protocols |
| HIPAA Security | Technical and administrative controls | Requires secure systems and staff training |
| False Claims Act | Accurate billing and documentation | Demands precise coding and claim review |
| Stark Law | Physician self-referral restrictions | Influences billing relationships and arrangements |
| Anti-Kickback Statute | Prohibited financial relationships | Affects RCM vendor relationships and incentives |
Understanding revenue cycle management fundamentals provides context for how regulatory requirements shape industry practices and technological solutions.

Leveraging Professional RCM Service Partnerships
Many healthcare providers partner with specialized RCM service organizations to access expertise, technology, and operational capacity that would be difficult to maintain in-house. These partnerships allow practices to focus on clinical excellence while ensuring financial performance through expert revenue cycle management.
Professional RCM services bring several distinct advantages to claims care processes. Teams of certified coders stay current with coding updates and payer-specific requirements. Billing specialists develop deep knowledge of individual payer policies and effective appeal strategies. Technology platforms provide capabilities that would require significant capital investment for individual practices.
The B2B RCM services model recognizes that healthcare providers need flexible partnerships that adapt to their specific circumstances. Service providers work with existing practice management systems, integrate with established workflows, and scale services based on practice volume and complexity.
Organizations considering RCM partnerships should evaluate potential providers based on several critical factors:
- Industry experience and specialization in relevant medical specialties
- Technology capabilities and integration flexibility
- Performance guarantees and transparent reporting
- HIPAA compliance and data security practices
- Communication protocols and accessibility
Successful partnerships begin with clear expectations regarding performance metrics, communication frequency, and decision-making authority. Regular performance reviews ensure alignment and provide opportunities to refine processes based on results.
Services such as medical claim submission and eligibility verification delivered by experienced teams often achieve superior results compared to in-house operations, particularly for smaller practices with limited specialized staffing.
Metrics and Performance Monitoring
Effective claims care RCM requires continuous performance monitoring through well-defined metrics that provide actionable insights. Organizations cannot improve what they do not measure, making metric selection and tracking essential to revenue cycle excellence.
Essential KPIs for Claims Care Success
Key performance indicators should reflect both process efficiency and financial outcomes. Leading indicators predict future performance, while lagging indicators confirm results and identify trends.
Clean claim rate measures the percentage of claims accepted by payers without additional information requests or corrections. This fundamental metric directly correlates with payment speed and administrative costs.
First-pass resolution rate tracks claims paid upon initial submission without denials or requests for additional information. Higher rates indicate effective front-end processes and accurate claim preparation.
Days in accounts receivable calculates the average time between service delivery and payment receipt. This metric reveals collection efficiency and identifies potential workflow bottlenecks.
Denial rate by category breaks down denials by type to identify systematic issues requiring process improvements or staff training.
Net collection rate compares actual collections to allowable reimbursement, revealing the organization's effectiveness at capturing available revenue.
Benchmark data from industry sources helps contextualize performance metrics and identify improvement opportunities. Organizations should compare their performance against both national benchmarks and specialty-specific standards to gain meaningful insights.
Regular review of reporting analytics enables data-driven decision making and strategic resource allocation across the revenue cycle.
Staff Training and Development
The human element of claims care RCM cannot be overlooked despite increasing automation. Well-trained staff who understand both technical requirements and the broader context of revenue cycle management drive superior results.
Comprehensive training programs address multiple dimensions of claims care competency. Technical skills in coding, billing software operation, and payer portal navigation form the foundation. However, analytical skills for problem-solving, communication abilities for patient and payer interactions, and attention to detail also prove essential.
Ongoing education keeps staff current with regulatory changes, coding updates, and evolving payer policies. The healthcare billing landscape changes constantly, requiring continuous learning to maintain effectiveness. Organizations that invest in staff development through regular training sessions, certification support, and access to industry resources consistently outperform those with static knowledge bases.
Cross-training creates operational resilience by ensuring multiple team members can perform critical functions. This redundancy prevents workflow disruptions during absences and provides coverage during volume spikes or staffing transitions.
Professional development opportunities improve retention by demonstrating organizational investment in employee growth. In an industry facing significant workforce challenges, retention of experienced billing staff provides competitive advantage through preserved institutional knowledge and established payer relationships.
Future Trends Shaping Claims Care RCM
The revenue cycle management landscape continues to evolve rapidly, driven by technological innovation, regulatory changes, and shifting payment models. Healthcare providers must anticipate these trends to position themselves for long-term success.
Artificial intelligence and machine learning are increasingly integrated into claims care processes. These technologies identify patterns in denial data, predict claim outcomes, and automate routine tasks with growing sophistication. However, human oversight remains essential for complex cases and strategic decision-making.
Value-based payment models require expanded claims care capabilities beyond traditional fee-for-service billing. Organizations must track quality metrics, manage shared savings calculations, and coordinate data across multiple systems. Claims care RCM is evolving to support these alternative payment methodologies while maintaining excellence in traditional billing.
Price transparency regulations are changing patient financial interactions by requiring upfront cost estimates for many services. Revenue cycle teams must develop new capabilities for accurate cost projection and patient communication to comply with these requirements.
Interoperability standards promise improved data exchange between systems, reducing manual data entry and enabling more automated workflows. As these standards mature and achieve broader adoption, claims care processes will become more streamlined and less prone to transcription errors.
Understanding the complexities of healthcare claims management helps organizations prepare for ongoing industry evolution and maintain competitive positioning.
Integration Across the Revenue Cycle
Claims care RCM achieves optimal results when integrated seamlessly with all other revenue cycle functions. Siloed approaches that treat claims processing as isolated from scheduling, coding, and collections miss opportunities for synergy and efficiency gains.
Effective integration begins with unified data systems that eliminate duplicate entry and ensure consistency across all touchpoints. When registration staff enter patient information once and that data flows automatically to coding, billing, and collections systems, accuracy improves and efficiency increases.
Communication protocols between departments enable rapid problem resolution and continuous improvement. Regular meetings between clinical, coding, and billing staff identify documentation issues, clarify coding questions, and align practices with payer requirements.
Technology platforms that support end-to-end revenue cycle management provide the infrastructure for integration. These systems connect scheduling, clinical documentation, coding, billing, and collections into cohesive workflows with built-in checkpoints and quality controls.
Organizations benefit from viewing claims care not as a distinct department but as a central component of an integrated revenue cycle ecosystem. This perspective encourages collaboration, shared accountability for outcomes, and strategic alignment across all revenue-related functions.
Mastering claims care RCM requires strategic vision, operational excellence, and continuous adaptation to industry changes. Healthcare providers who implement comprehensive approaches to claims management, denial prevention, and performance monitoring achieve superior financial outcomes while maintaining focus on patient care. Greenhive Billing Solutions delivers expert revenue cycle management services that optimize every aspect of the claims process, from initial eligibility verification through final payment posting. Our experienced team works seamlessly with your existing systems to improve clean claim rates, reduce denials, and accelerate reimbursements, allowing you to concentrate on what matters most: delivering exceptional patient care.