Understanding what is ABN in medical billing is fundamental for healthcare providers who serve Medicare beneficiaries. An Advance Beneficiary Notice (ABN) is a standardized notification that Medicare providers must issue to beneficiaries before delivering items or services that Medicare is likely to deny. This document protects both the provider and the patient by establishing financial responsibility upfront and ensuring informed consent. Revenue cycle management teams must grasp the nuances of ABN implementation to maintain compliance, reduce claim denials, and secure appropriate reimbursement for services rendered.
The Fundamental Purpose of ABN in Medical Billing
What is ABN in medical billing at its core? The Advance Beneficiary Notice serves as a critical communication tool between healthcare providers and Medicare beneficiaries. When a provider believes Medicare may not cover a particular service or item, the ABN informs the patient of this potential denial before the service is delivered. This advance notification allows the beneficiary to make an informed decision about whether to proceed with the service and accept financial responsibility.
The official CMS guidelines on ABN usage specify that the notice must be provided in writing using the standardized CMS Form R-131. This form has been designed to ensure clarity and consistency across all Medicare providers. Without a properly executed ABN, providers may be unable to bill the beneficiary for services that Medicare denies, resulting in significant revenue loss.
Protecting Provider Revenue and Patient Rights
The dual protection offered by ABNs benefits both parties in the healthcare transaction. For providers, a valid ABN creates a legal pathway to collect payment from the beneficiary when Medicare denies coverage. For patients, the notice ensures they receive clear information about potential out-of-pocket costs before committing to a service. This transparency strengthens the provider-patient relationship while maintaining financial accountability.
When Healthcare Providers Must Issue an ABN
Determining when to issue an ABN requires careful analysis of Medicare coverage policies and individual patient circumstances. Providers must issue an ABN when they have reason to believe that Medicare will deny payment for a service that is normally covered by Medicare but may be denied in a specific instance. This differs significantly from services that Medicare never covers, which do not require an ABN.
Common scenarios requiring an ABN include:
- Services exceeding Medicare frequency limitations
- Diagnostic tests deemed not medically necessary for the patient's condition
- Treatments that fail to meet Medicare's coverage criteria
- Upgrade equipment or supplies when standard options suffice
- Routine screening procedures performed more frequently than Medicare allows
The comprehensive guide from AAPC emphasizes that providers should not issue ABNs as a routine practice for all services. Overusing ABNs can create unnecessary administrative burden and patient confusion. Instead, providers should base ABN issuance on specific, documented reasons for expecting Medicare denial.
Services That Never Require an ABN
Understanding what is ABN in medical billing also means knowing when not to use it. Medicare provides clear guidance on services excluded from ABN requirements. Services that are never covered by Medicare, such as cosmetic procedures or services deemed experimental, do not require an ABN because patients should already understand these are non-covered benefits.
Similarly, providers cannot use ABNs for services covered under Medicare Advantage plans, as these plans operate under different rules. Emergency or urgent care services also fall outside ABN requirements, as patients cannot reasonably be expected to make informed financial decisions in crisis situations.
The Standardized CMS ABN Form Requirements
The official ABN form, known as Form CMS-R-131, follows a specific format mandated by the Centers for Medicare & Medicaid Services. This standardization ensures consistency across all healthcare settings and helps beneficiaries recognize legitimate notices. The form must include several mandatory elements to be considered valid and enforceable.
Essential components of a valid ABN:
- Patient and provider identification information
- Detailed description of the service or item in question
- Clear explanation of why Medicare may deny coverage
- Estimated cost of the service or item
- Beneficiary's decision and signature
- Date of issuance
The notice must be provided in the beneficiary's preferred language when possible, and providers must maintain signed copies in patient records. The timing of ABN delivery is equally critical. According to Medicare Claims Processing Manual guidelines, the ABN must be issued sufficiently in advance of the service to allow the beneficiary adequate time to consider their options and make an informed decision.
| ABN Component | Requirement | Purpose |
|---|---|---|
| Service Description | Must be specific and understandable | Ensures patient knows exactly what service may not be covered |
| Reason for Expected Denial | Clear Medicare policy reference | Provides justification for the notice |
| Cost Estimate | Reasonable good faith estimate | Allows patient to assess financial impact |
| Beneficiary Options | Three clear choices provided | Enables informed decision-making |
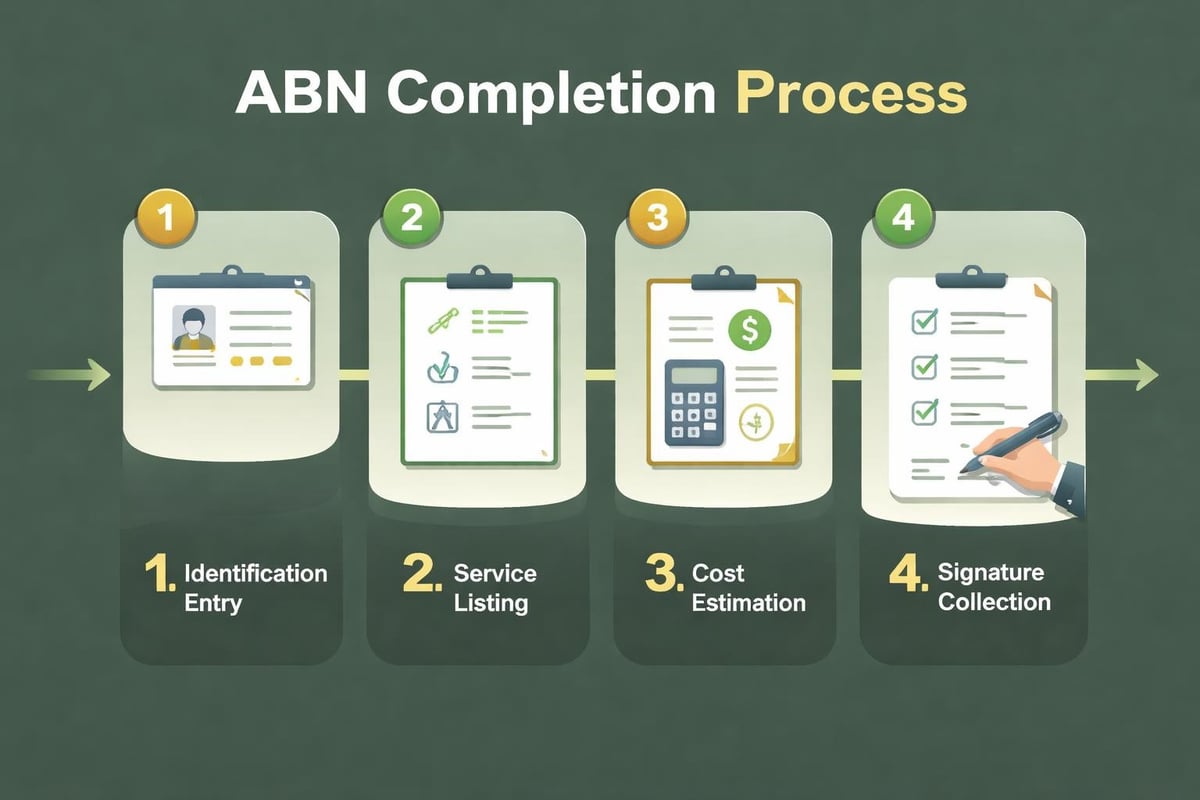
Completing the ABN: Step-by-Step Process
For revenue cycle management teams supporting healthcare providers, understanding the proper ABN completion process prevents costly errors and protects provider revenue. The standardized form includes specific sections that must be completed accurately to ensure compliance and enforceability.
Step 1: Enter Accurate Identifying Information
Begin by recording the beneficiary's name, Medicare number, and the date the notice is provided. The provider's name and contact information must also be clearly stated. This information establishes the parties involved and creates a documented timeline.
Step 2: List Services and Reasons for Expected Denial
In the designated section, describe each service or item that may be denied. Use language the patient can understand rather than technical medical terminology. For each service, explain specifically why Medicare may not pay. Reference the relevant Medicare policy, frequency limitation, or medical necessity standard that applies.
Step 3: Provide Accurate Cost Estimates
Healthcare providers must include a reasonable estimate of what the service will cost if the patient chooses to proceed. Mastering the CMS ABN requires providers to base estimates on current fee schedules and actual charges. Significant discrepancies between estimated and actual costs can undermine the notice's validity.
Step 4: Present Beneficiary Options Clearly
The ABN presents three options to the beneficiary. Option 1 allows the patient to receive the service and accept financial responsibility if Medicare denies payment. Option 2 lets the patient decline the service entirely. Option 3 permits the patient to receive the service and have a claim submitted to Medicare, with the understanding they may owe payment if Medicare denies coverage. The beneficiary must select one option and sign the form.
Step 5: Obtain Signature and Maintain Records
The beneficiary or their authorized representative must sign and date the ABN. Providers must retain the signed original or a copy for their records. This documentation proves the notice was properly delivered and acknowledged, which is essential for successful denial management services when claims are rejected.
Common ABN Errors That Lead to Revenue Loss
Despite the standardized format, providers frequently make mistakes when implementing ABN procedures. These errors can result in denied claims that cannot be billed to the patient, creating significant revenue leakage. Revenue cycle management professionals must identify and correct these issues systematically.
Frequent ABN mistakes include:
- Issuing the notice too close to the service date, leaving insufficient decision time
- Providing vague or incomplete service descriptions
- Failing to obtain the beneficiary's signature or dating the form incorrectly
- Using outdated versions of the ABN form
- Issuing ABNs for services that never require them
- Estimating costs inaccurately or omitting cost information entirely
- Not maintaining proper documentation in patient records
According to resources on correct ABN usage, one of the most damaging errors occurs when providers issue an ABN but fail to submit the claim to Medicare first. Even when the beneficiary signs Option 1 agreeing to pay, providers must still submit a claim to Medicare and receive a formal denial before billing the patient directly. Skipping this step violates Medicare regulations and can result in compliance penalties.
Avoiding ABN Overuse and Underuse
Finding the appropriate balance in ABN issuance protects both compliance and patient relationships. Issuing ABNs for every service creates administrative inefficiency and may alarm patients unnecessarily. Conversely, failing to issue ABNs when needed exposes providers to financial risk.
Effective medical billing services incorporate systematic ABN review processes. These processes analyze each service against current Medicare coverage policies, local coverage determinations, and the patient's specific clinical circumstances. This analysis determines whether an ABN is warranted before the patient arrives for service.
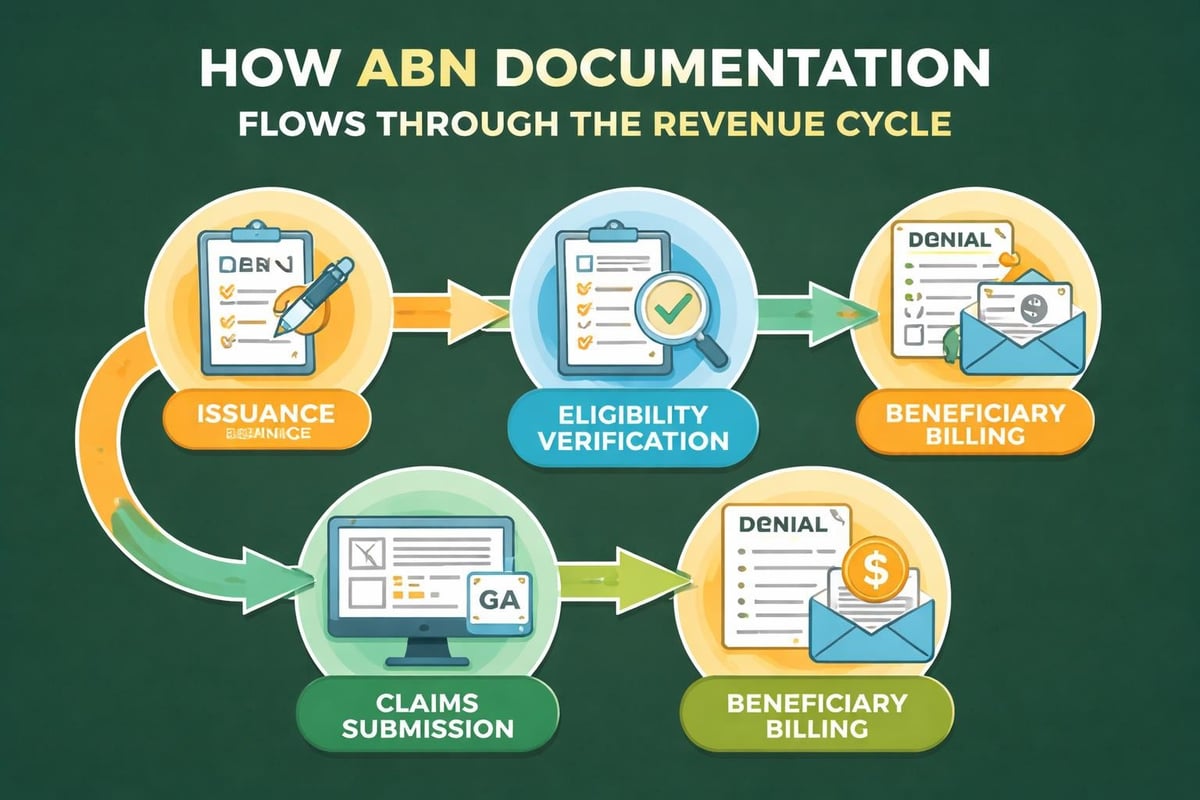
The ABN's Impact on Claims Processing and Reimbursement
Understanding what is ABN in medical billing extends beyond the initial notice to encompass the entire claims lifecycle. When an ABN is properly executed and Medicare subsequently denies the claim, the provider has established the right to bill the beneficiary for the service. This process requires specific coding and documentation on the claim form itself.
Providers must append modifier GA (waiver of liability statement issued as required by payer policy) to claim line items when a valid ABN is on file. This modifier informs Medicare that the beneficiary was notified in advance of potential non-coverage and agreed to accept financial responsibility. Without this modifier, Medicare's systems may process the claim differently and potentially hold the provider liable.
| Modifier | Usage Scenario | Impact on Claim |
|---|---|---|
| GA | Valid ABN on file | Allows provider to bill beneficiary if Medicare denies |
| GX | Service statutorily excluded, ABN issued voluntarily | Claim denied; informational only |
| GZ | Service expected to be denied, no ABN issued | Claim denied; provider assumes financial responsibility |
The relationship between ABNs and claims processing cannot be overstated. Revenue cycle teams must track ABN documentation meticulously and ensure coding specialists have access to this information when submitting claims. A missing ABN or incorrectly applied modifier can transform a collectible balance into a write-off.
Coordination with Eligibility Verification
The ABN process intersects significantly with eligibility verification services. Before determining whether an ABN is necessary, providers must verify the patient's current Medicare coverage, including any applicable frequency limitations or previous service utilization. This verification informs the provider's decision about expected coverage.
When eligibility systems indicate a service may exceed frequency limits or conflict with coverage criteria, the revenue cycle team should flag the account for ABN issuance. This proactive approach prevents post-service disputes and protects revenue collection.
Training Staff on Proper ABN Implementation
For healthcare organizations, successful ABN management requires comprehensive staff training across multiple departments. Front desk personnel, clinical staff, billing specialists, and revenue cycle managers all play distinct roles in the ABN process. Each team member must understand their responsibilities and how their actions affect overall compliance.
Key training elements for different roles:
- Front office staff: Recognizing triggers that require ABN issuance and scheduling adequate time for notice delivery
- Clinical providers: Understanding Medicare coverage policies and medical necessity standards that inform ABN decisions
- Billing specialists: Applying correct modifiers, tracking ABN documentation, and processing denied claims appropriately
- Revenue cycle managers: Auditing ABN compliance, monitoring denial patterns, and implementing process improvements
Organizations working with revenue cycle management partners benefit from external expertise in ABN compliance. Professional RCM teams bring specialized knowledge of Medicare policies and systematic approaches to ABN workflow integration.
Creating ABN Workflow Documentation
Standardized workflows ensure consistent ABN handling across the organization. These workflows should document decision trees for determining when ABNs are required, templates for common ABN scenarios, and clear escalation paths when staff are uncertain about ABN necessity.
The workflow should specify timing requirements, such as issuing ABNs at least one business day before the scheduled service when possible. It should also address how to handle situations where the patient arrives for service and an ABN becomes necessary unexpectedly.
ABN Compliance and Audit Preparedness
Medicare auditors routinely examine ABN practices during compliance reviews and post-payment audits. Providers must maintain meticulous documentation demonstrating proper ABN issuance, beneficiary acknowledgment, and appropriate billing practices. The importance of ABN compliance becomes evident during these audits, as improper ABN usage can trigger significant financial penalties and mandatory refunds.
Audit-ready ABN documentation includes the signed ABN form, evidence of timely delivery, documentation in the patient's medical record, and proof that the claim was submitted to Medicare before billing the beneficiary. Revenue cycle teams should conduct internal audits regularly to identify compliance gaps before external reviewers discover them.
Critical audit focus areas:
- Completeness of ABN forms with all required elements
- Appropriate use of modifiers GA, GX, and GZ
- Documentation of service medical necessity or lack thereof
- Timing of ABN issuance relative to service delivery
- Accuracy of cost estimates compared to actual charges
- Proper submission of claims to Medicare prior to beneficiary billing
Organizations offering medical coding audit services can provide objective assessments of ABN compliance and recommend corrective actions. These audits identify patterns of improper ABN usage and help organizations implement preventive measures.
Responding to ABN-Related Denials
When Medicare denies a claim and an ABN is on file, the provider must follow specific procedures for beneficiary billing. The denial explanation from Medicare should reference the reason for non-coverage, which should align with the reason documented on the ABN. If the beneficiary selected Option 1 on the ABN, the provider may bill them directly for the service.
However, if discrepancies exist between the ABN's stated reason and Medicare's actual denial reason, the provider may face challenges collecting from the beneficiary. This scenario highlights the importance of accurate ABN completion based on thorough knowledge of Medicare policies.
Technology Solutions for ABN Management
Modern healthcare organizations increasingly rely on technology to streamline ABN workflows and improve compliance. Electronic health record systems can integrate ABN templates, trigger alerts when services may require ABNs, and maintain digital copies of signed notices. Practice management systems can flag accounts with pending ABNs and ensure appropriate modifiers are applied during claims submission.
Advanced revenue cycle management platforms offer sophisticated ABN tracking capabilities. These systems can analyze historical denial patterns to predict when ABNs should be issued, calculate accurate cost estimates based on fee schedules, and generate compliance reports for audit purposes. While Greenhive Billing Solutions does not provide software products, our experienced team works seamlessly with client-owned systems and industry-standard platforms to optimize ABN management processes.
| Technology Feature | Benefit | Implementation Consideration |
|---|---|---|
| Automated ABN triggers | Reduces missed ABN opportunities | Requires regular policy updates |
| Electronic signature capture | Improves documentation efficiency | Must ensure legal validity |
| Integrated cost estimators | Provides accurate patient estimates | Needs current fee schedule data |
| Compliance reporting dashboards | Enables proactive audit preparation | Requires staff training on metrics |
Integration with Patient Portals
Patient portals offer opportunities to deliver ABNs electronically and obtain digital acknowledgments. This approach can improve patient convenience and documentation accuracy while reducing paper waste. However, providers must ensure electronic ABN delivery meets CMS requirements for adequate advance notice and patient understanding.
The portal must present the ABN in a format that ensures the beneficiary reads and comprehends the notice before acknowledging it. Simple click-through acceptance may not satisfy CMS standards for informed consent. Best practices include requiring the beneficiary to view each section of the ABN before proceeding and providing clear instructions throughout the digital form.
Financial Impact of Effective ABN Management
The financial implications of proper ABN implementation extend far beyond individual claims. Organizations that systematically manage ABNs experience reduced write-offs, fewer compliance penalties, and improved cash flow predictability. Conversely, poor ABN practices create multiple revenue risks.
When providers fail to issue required ABNs, they assume financial responsibility for denied services regardless of whether Medicare's denial was predictable. This liability can accumulate significantly over time, particularly for high-cost services or procedures with frequent medical necessity denials. The LinkedIn guide on ABN impact describes how strategic ABN management contributes to overall financial health.
Measuring ABN program effectiveness:
- Track the percentage of services requiring ABNs that receive proper documentation
- Monitor denial rates for services where ABNs should have been issued
- Calculate collection rates on beneficiary balances with valid ABNs
- Measure staff compliance with ABN issuance protocols
- Analyze patient satisfaction scores related to ABN communication
Revenue cycle analytics should incorporate ABN metrics to identify improvement opportunities. Practices with high rates of ABN-related write-offs may need enhanced staff training, updated policy references, or improved clinical documentation to support medical necessity determinations.
Calculating the Cost of ABN Non-Compliance
Healthcare organizations should quantify the financial impact of ABN failures to justify investment in improved processes and technology. This calculation includes direct revenue loss from services that cannot be collected from Medicare or the beneficiary, plus potential refunds required if services were incorrectly billed to the beneficiary without proper ABN documentation.
Additional costs may include administrative time spent appealing denials, responding to beneficiary complaints, and addressing compliance audit findings. Organizations facing repeated ABN violations may also experience increased audit scrutiny and reputational damage that affects patient retention and referral relationships.
ABN Considerations for Different Healthcare Settings
Understanding what is ABN in medical billing requires recognizing how different practice settings face unique ABN challenges. Hospital outpatient departments, physician practices, durable medical equipment suppliers, and skilled nursing facilities all encounter distinct scenarios requiring ABN customization while maintaining core compliance principles.
Physician practices frequently issue ABNs for diagnostic testing that may not meet medical necessity criteria or for services exceeding frequency limitations. For example, routine screening procedures performed more frequently than Medicare coverage allows typically require an ABN. Practices must stay current on Local Coverage Determinations that specify when common services may be denied.
Durable medical equipment suppliers face ABN requirements when beneficiaries request upgraded equipment features beyond Medicare's standard coverage. The ABN must clearly distinguish between the standard covered equipment and the upgraded features the beneficiary wishes to obtain at their own expense.
Specialty-Specific ABN Scenarios
Certain medical specialties encounter ABN situations more frequently than others. Orthopedic practices may issue ABNs for certain therapeutic injections that exceed Medicare frequency limits. Dermatology practices often need ABNs for cosmetic procedures or for treating multiple skin lesions when Medicare coverage limits apply. Cardiology practices may require ABNs for certain diagnostic studies performed more frequently than coverage policies allow.
Each specialty should develop standardized ABN templates for their most common scenarios, incorporating specific Medicare policy references and accurate cost estimates based on their fee schedules. This preparation enables efficient ABN issuance without compromising compliance.
Proper ABN management protects healthcare providers from significant revenue loss while ensuring Medicare beneficiaries make informed decisions about their care. By understanding what is ABN in medical billing and implementing systematic compliance processes, healthcare organizations can navigate Medicare's complex coverage landscape with confidence. Greenhive Billing Solutions provides comprehensive revenue cycle management services that incorporate expert ABN handling, claims processing, and denial management to maximize reimbursements while maintaining full regulatory compliance. Our experienced team works with your existing systems to streamline operations and improve your practice's financial performance.

